FiveYear Outcomes of Transcatheter Aortic Valve Replacement TAVR







- Slides: 25

Five-Year Outcomes of Transcatheter Aortic Valve Replacement (TAVR) in “Inoperable” Patients With Severe Aortic Stenosis: The PARTNER Trial Samir R. Kapadia, MD On behalf of The PARTNER Trial Investigators TCT 2014 | September 13, 2014

Background • Transcatheter aortic valve replacement (TAVR) is the recommended treatment for “inoperable” patients with severe aortic stenosis (AS). • Long term clinical benefit and valve performance in this population remain unknown.

PARTNER Study Design Symptomatic Severe Aortic Stenosis Inoperable Severe Symptomatic AS with AVA< 0. 8 cm 2 (EOA index < 0. 5 cm 2/m 2), and mean gradient > 40 mm. Hg or jet velocity > 4. 0 m/s N = 358 ASSESSMENT: Transfemoral Access 1: 1 Randomization TF TAVR n = 179 V S Inoperable defined as risk of death or serious irreversible morbidity of AVR as assessed by cardiologist and two surgeons exceeding 50%. Standard Therapy n = 179 Primary Endpoint: All-Cause Mortality Over Length of Trial (Superiority) • Primary endpoint evaluated when all patients reached one year follow-up. • After primary endpoint analysis reached, patients were allowed to cross-over to TAVR.

Key End-Points for 5 Year Analysis • All-Cause Mortality • Cardiac Mortality • Re-hospitalization • Stroke • NYHA functional class • Echo-derived valve areas, transvalvular gradients, and paravalvular leak. • Mortality outcomes stratified by STS score, paravalvular leak and age.

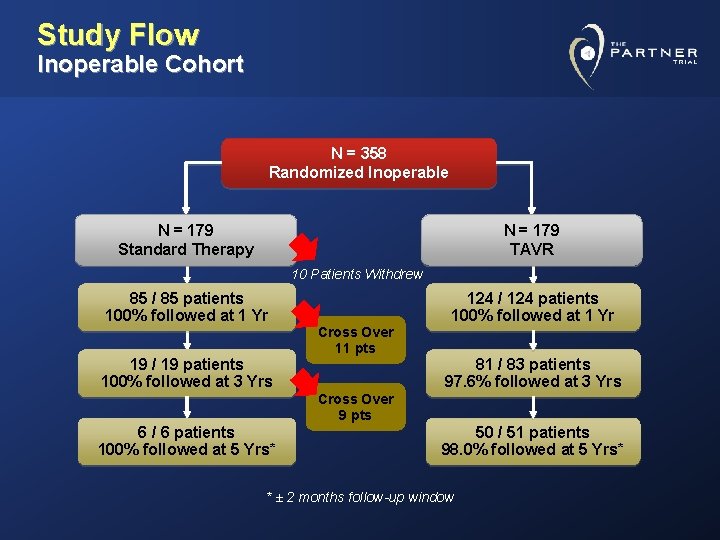
Study Flow Inoperable Cohort N = 358 Randomized Inoperable N = 179 Standard Therapy N = 179 TAVR 10 Patients Withdrew 85 / 85 patients 100% followed at 1 Yr 19 / 19 patients 100% followed at 3 Yrs Cross Over 11 pts 124 / 124 patients 100% followed at 1 Yr 81 / 83 patients 97. 6% followed at 3 Yrs Cross Over 9 pts 6 / 6 patients 100% followed at 5 Yrs* 50 / 51 patients 98. 0% followed at 5 Yrs* * ± 2 months follow-up window

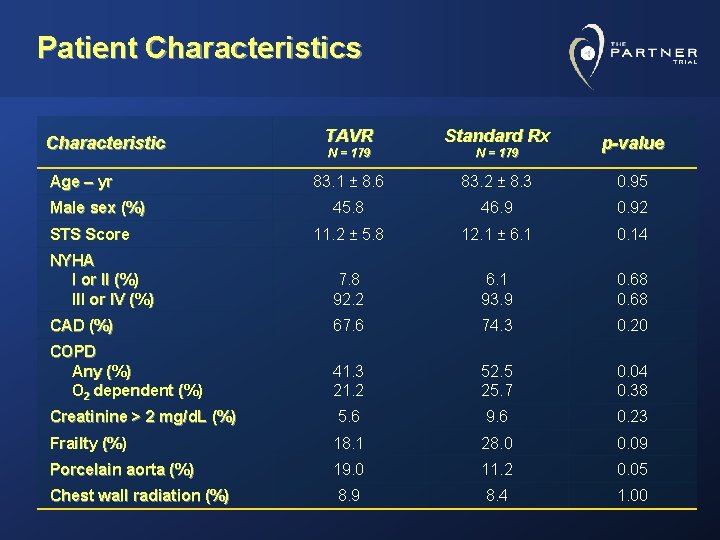
Patient Characteristics TAVR Standard Rx N = 179 83. 1 ± 8. 6 83. 2 ± 8. 3 0. 95 45. 8 46. 9 0. 92 11. 2 ± 5. 8 12. 1 ± 6. 1 0. 14 NYHA I or II (%) III or IV (%) 7. 8 92. 2 6. 1 93. 9 0. 68 CAD (%) 67. 6 74. 3 0. 20 COPD Any (%) O 2 dependent (%) 41. 3 21. 2 52. 5 25. 7 0. 04 0. 38 Creatinine > 2 mg/d. L (%) 5. 6 9. 6 0. 23 Frailty (%) 18. 1 28. 0 0. 09 Porcelain aorta (%) 19. 0 11. 2 0. 05 Chest wall radiation (%) 8. 9 8. 4 1. 00 Characteristic Age – yr Male sex (%) STS Score p-value

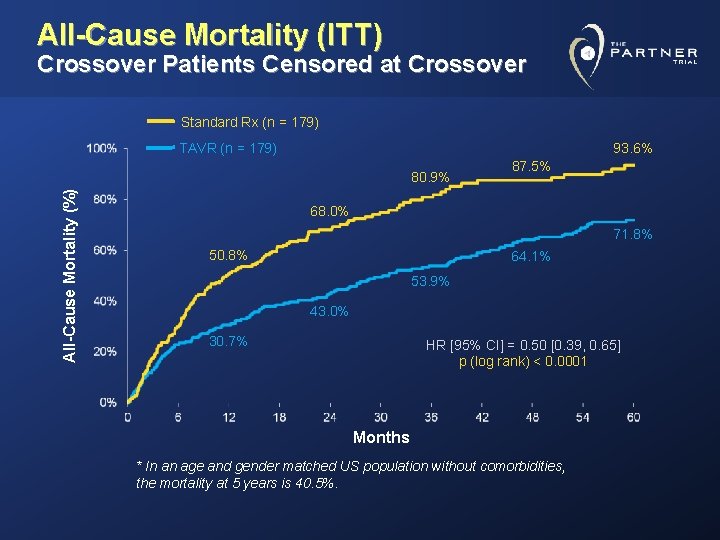
All-Cause Mortality (ITT) Crossover Patients Censored at Crossover Standard Rx (n = 179) TAVR (n = 179) 93. 6% All-Cause Mortality (%) 80. 9% 87. 5% 68. 0% 71. 8% 50. 8% 64. 1% 53. 9% 43. 0% 30. 7% HR [95% CI] = 0. 50 [0. 39, 0. 65] p (log rank) < 0. 0001 Months * In an age and gender matched US population without comorbidities, the mortality at 5 years is 40. 5%.

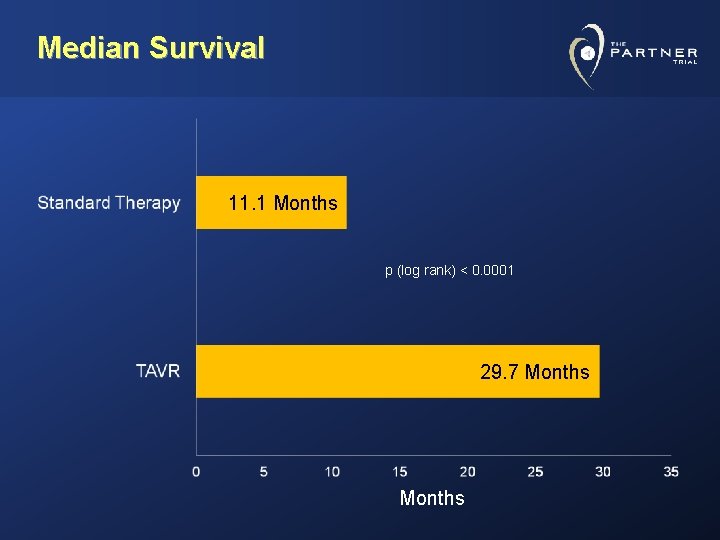
Median Survival 11. 1 Months p (log rank) < 0. 0001 29. 7 Months

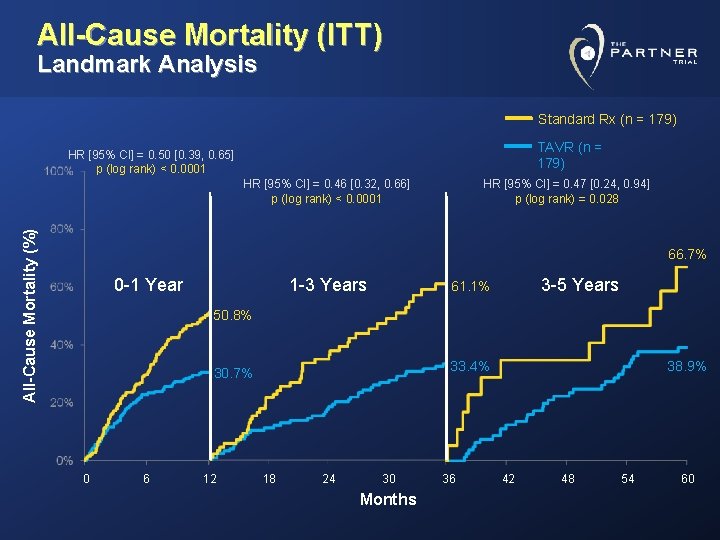
All-Cause Mortality (ITT) Landmark Analysis Standard Rx (n = 179) TAVR (n = 179) HR [95% CI] = 0. 50 [0. 39, 0. 65] p (log rank) < 0. 0001 All-Cause Mortality (%) HR [95% CI] = 0. 46 [0. 32, 0. 66] p (log rank) < 0. 0001 HR [95% CI] = 0. 47 [0. 24, 0. 94] p (log rank) = 0. 028 66. 7% 0 -1 Year 1 -3 Years 3 -5 Years 61. 1% 50. 8% 0 6 12 38. 9% 33. 4% 30. 7% 18 24 30 Months 36 42 48 54 60

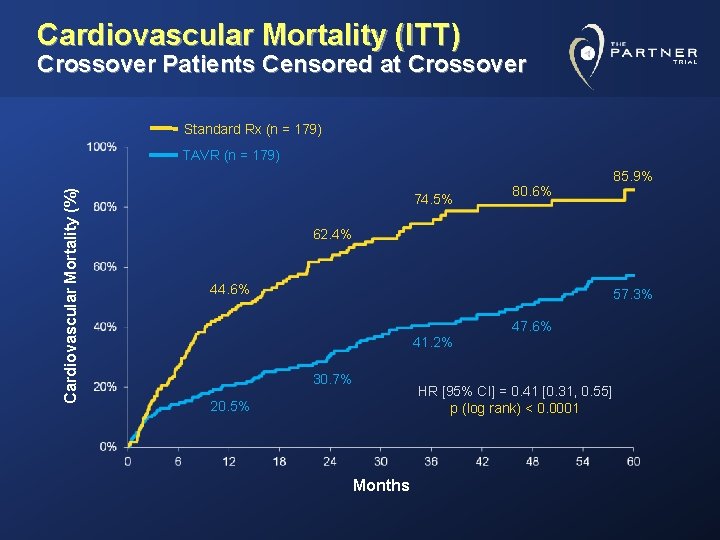
Cardiovascular Mortality (ITT) Crossover Patients Censored at Crossover Standard Rx (n = 179) Cardiovascular Mortality (%) TAVR (n = 179) 74. 5% 80. 6% 85. 9% 62. 4% 44. 6% 57. 3% 47. 6% 41. 2% 30. 7% HR [95% CI] = 0. 41 [0. 31, 0. 55] p (log rank) < 0. 0001 20. 5% Months

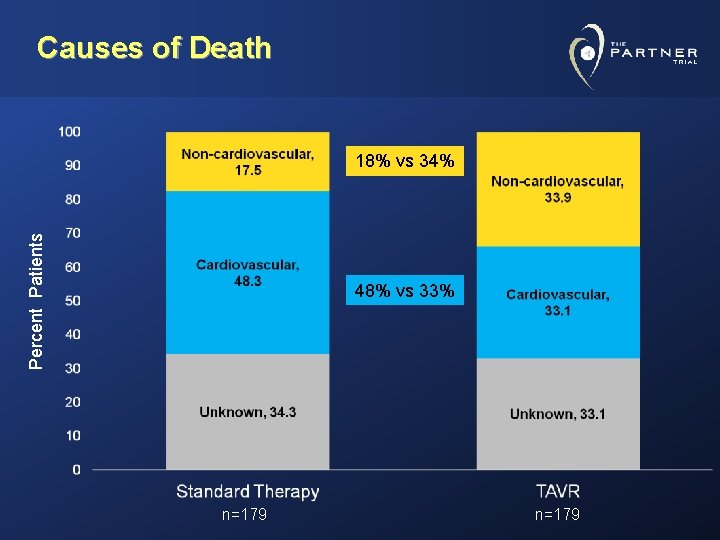
Causes of Death Percent Patients 18% vs 34% 48% vs 33% n=179

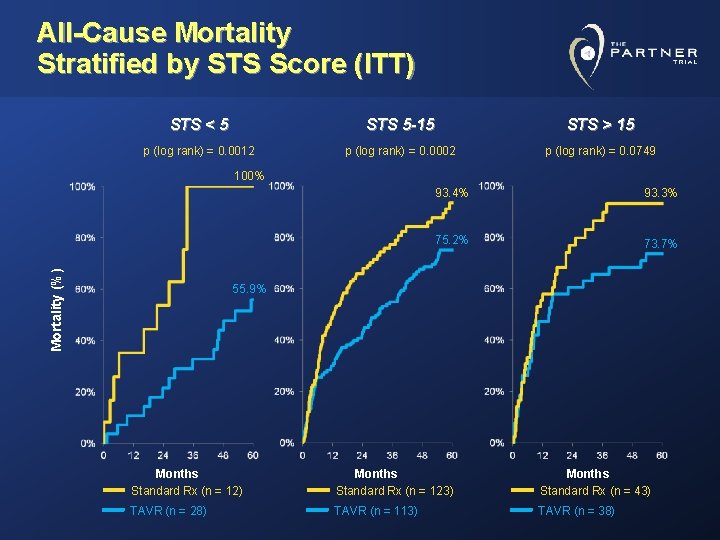
All-Cause Mortality Stratified by STS Score (ITT) STS < 5 STS 5 -15 STS > 15 p (log rank) = 0. 0012 p (log rank) = 0. 0002 p (log rank) = 0. 0749 Mortality (%) 100% 93. 4% 93. 3% 75. 2% 73. 7% 55. 9% Months Standard Rx (n = 12) Months Standard Rx (n = 123) Months Standard Rx (n = 43) TAVR (n = 28) TAVR (n = 113) TAVR (n = 38)

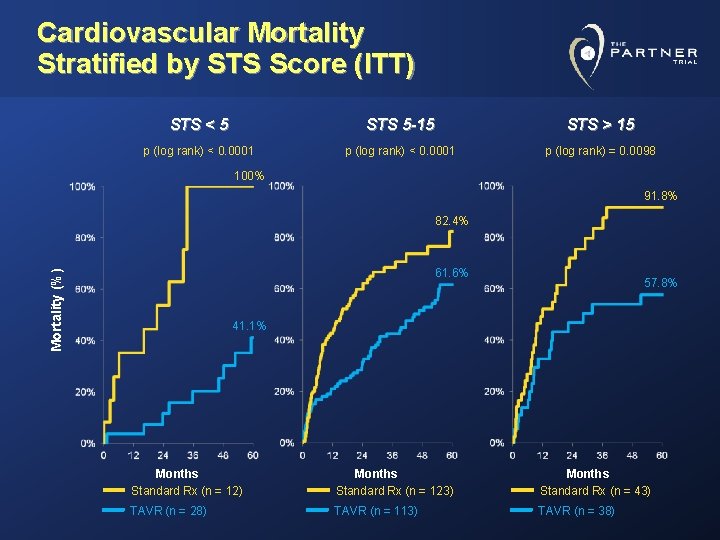
Cardiovascular Mortality Stratified by STS Score (ITT) STS < 5 STS 5 -15 STS > 15 p (log rank) < 0. 0001 p (log rank) = 0. 0098 100% 91. 8% 82. 4% Mortality (%) 61. 6% 57. 8% 41. 1% Months Standard Rx (n = 12) Months Standard Rx (n = 123) Months Standard Rx (n = 43) TAVR (n = 28) TAVR (n = 113) TAVR (n = 38)

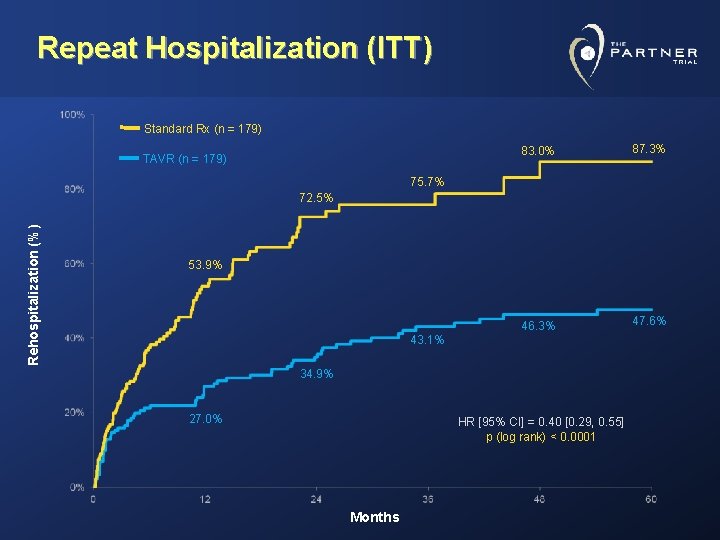
Repeat Hospitalization (ITT) Standard Rx (n = 179) TAVR (n = 179) 83. 0% 87. 3% 46. 3% 47. 6% 75. 7% Rehospitalization (%) 72. 5% 53. 9% 43. 1% 34. 9% 27. 0% HR [95% CI] = 0. 40 [0. 29, 0. 55] p (log rank) < 0. 0001 Months

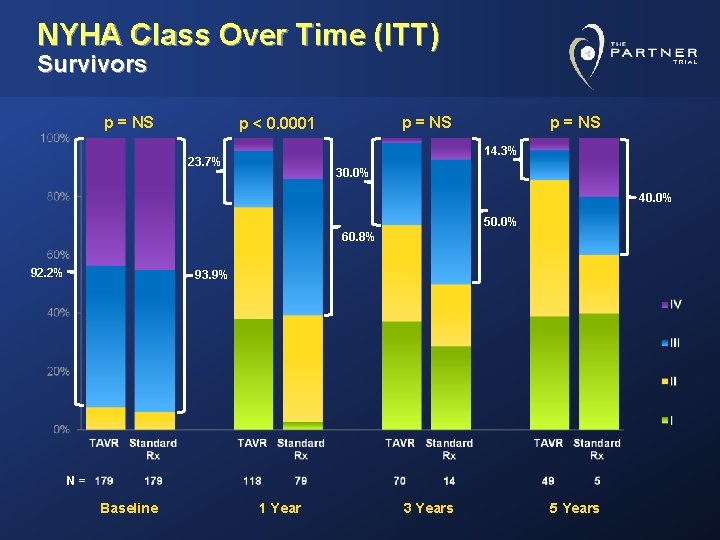
NYHA Class Over Time (ITT) Survivors p = NS p < 0. 0001 p = NS 14. 3% 23. 7% 30. 0% 40. 0% 50. 0% 60. 8% 92. 2% 93. 9% N= Baseline 1 Year 3 Years 5 Years

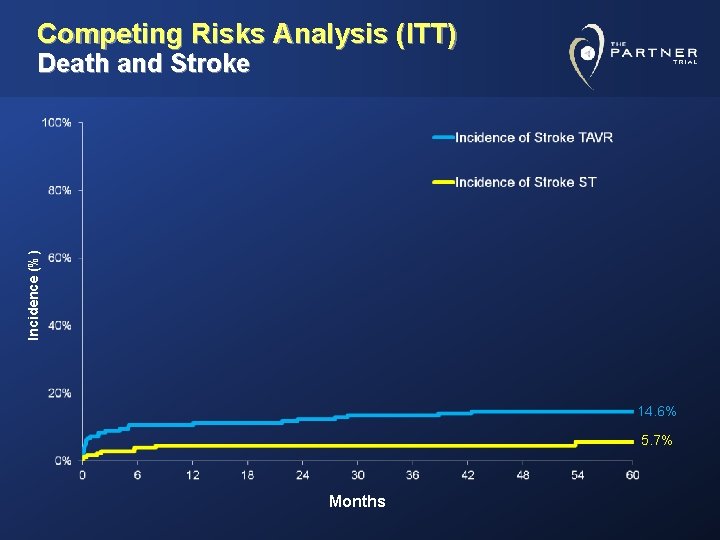
Competing Risks Analysis (ITT) Incidence (%) Death and Stroke 14. 6% 5. 7% Months

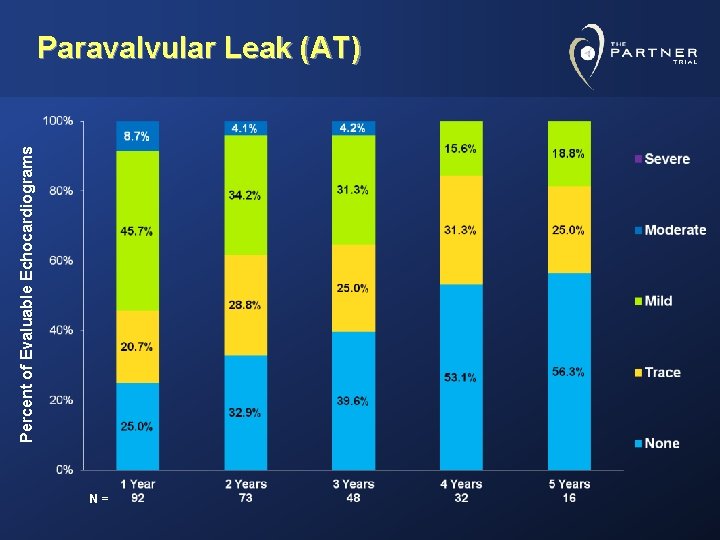
Percent of Evaluable Echocardiograms Paravalvular Leak (AT) N=

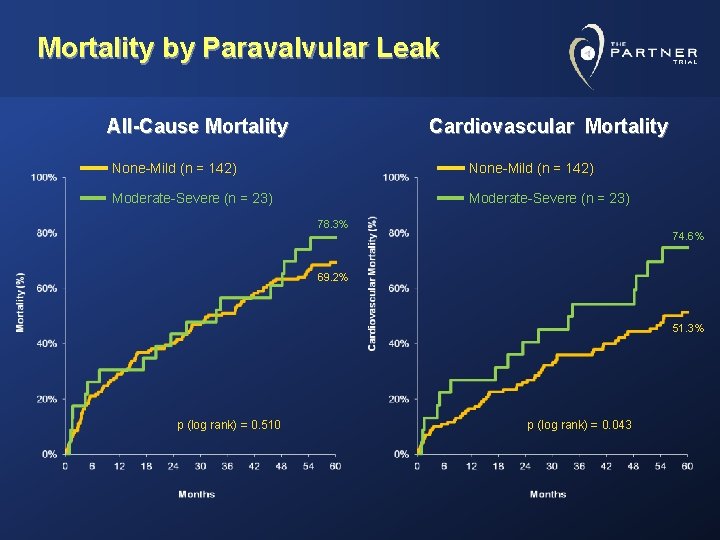
Mortality by Paravalvular Leak All-Cause Mortality Cardiovascular Mortality None-Mild (n = 142) Moderate-Severe (n = 23) 78. 3% 74. 6% 69. 2% 51. 3% p (log rank) = 0. 510 p (log rank) = 0. 043

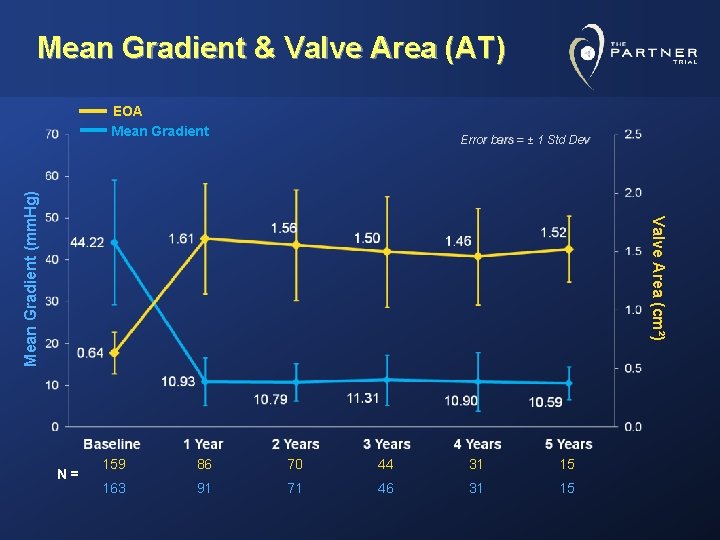
Mean Gradient & Valve Area (AT) EOA Mean Gradient Valve Area (cm²) Mean Gradient (mm. Hg) Error bars = ± 1 Std Dev N= 159 86 70 44 31 15 163 91 71 46 31 15

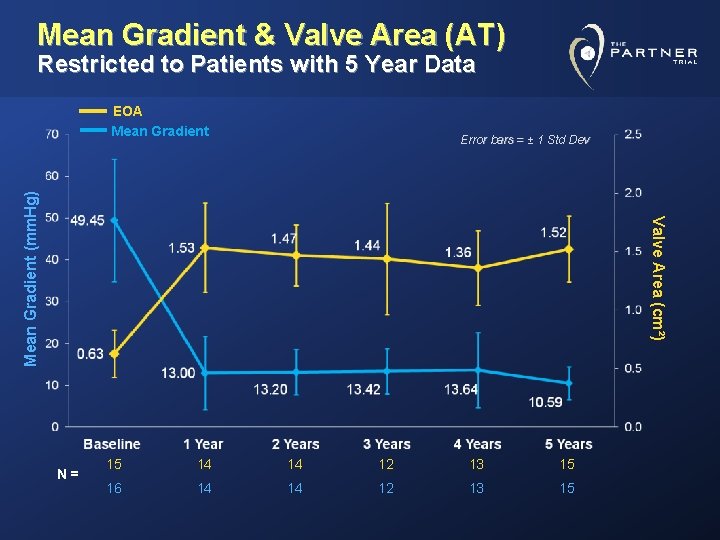
Mean Gradient & Valve Area (AT) Restricted to Patients with 5 Year Data EOA Mean Gradient Valve Area (cm²) Mean Gradient (mm. Hg) Error bars = ± 1 Std Dev N= 15 14 14 12 13 15 16 14 14 12 13 15

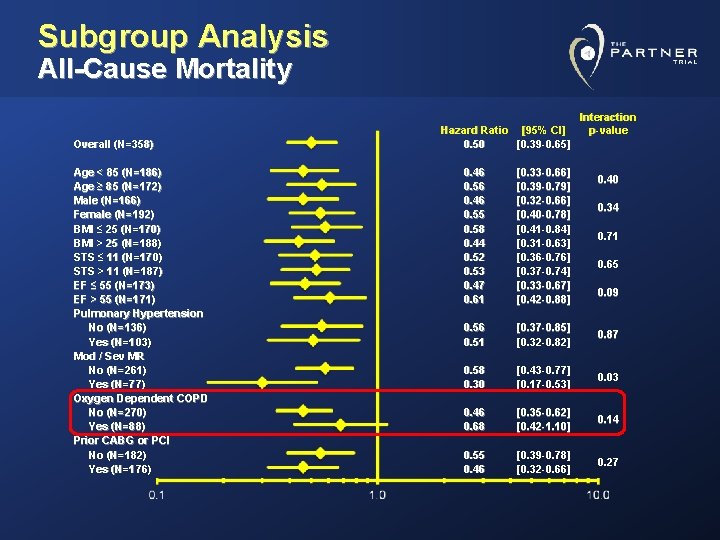
Subgroup Analysis All-Cause Mortality Overall (N=358) Age < 85 (N=186) Age ≥ 85 (N=172) Male (N=166) Female (N=192) BMI ≤ 25 (N=170) BMI > 25 (N=188) STS ≤ 11 (N=170) STS > 11 (N=187) EF ≤ 55 (N=173) EF > 55 (N=171) Pulmonary Hypertension No (N=136) Yes (N=103) Mod / Sev MR No (N=261) Yes (N=77) Oxygen Dependent COPD No (N=270) Yes (N=88) Prior CABG or PCI No (N=182) Yes (N=176) Hazard Ratio [95% CI] 0. 50 [0. 39 -0. 65] Interaction p-value 0. 46 0. 56 0. 46 0. 55 0. 58 0. 44 0. 52 0. 53 0. 47 0. 61 [0. 33 -0. 66] [0. 39 -0. 79] [0. 32 -0. 66] [0. 40 -0. 78] [0. 41 -0. 84] [0. 31 -0. 63] [0. 36 -0. 76] [0. 37 -0. 74] [0. 33 -0. 67] [0. 42 -0. 88] 0. 56 0. 51 [0. 37 -0. 85] [0. 32 -0. 82] 0. 87 0. 58 0. 30 [0. 43 -0. 77] [0. 17 -0. 53] 0. 03 0. 46 0. 68 [0. 35 -0. 62] [0. 42 -1. 10] 0. 14 0. 55 0. 46 [0. 39 -0. 78] [0. 32 -0. 66] 0. 27 0. 40 0. 34 0. 71 0. 65 0. 09

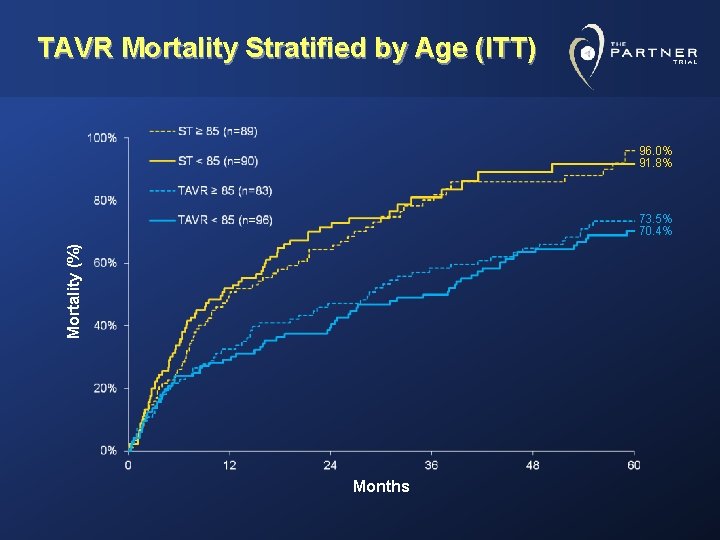
TAVR Mortality Stratified by Age (ITT) 96. 0% 91. 8% Mortality (%) 73. 5% 70. 4% Months

Clinical Observations • Mortality benefit was similar in elderly (>85 yr) patients compared to those ≤ 85 years. • Cardiovascular mortality and all-cause mortality benefit was seen even in patients with high STS score. • Patients with O 2 dependent COPD may have less mortality benefit. • Beyond early procedural risk of stroke there was no persistent risk over 5 -year follow up. • Moderate and severe paravalvular leak is associated with higher cardiovascular mortality particularly in patients with less comorbidities.

Main Conclusions • At 5 years follow-up benefits of TAVR were sustained as measured by: – All-Cause Mortality – Cardiovascular Mortality – Repeat Hospitalization – Functional Status • Valve durability was demonstrated with no increase in transvalvular gradient or attrition of valve area.

Thank You to the Dedicated Study Teams at All PARTNER Investigational Sites