Dyspnoea II PE and Pneumonia EMC 2015 SDMH




















- Slides: 30

Dyspnoea II – PE and Pneumonia EMC 2015 SDMH

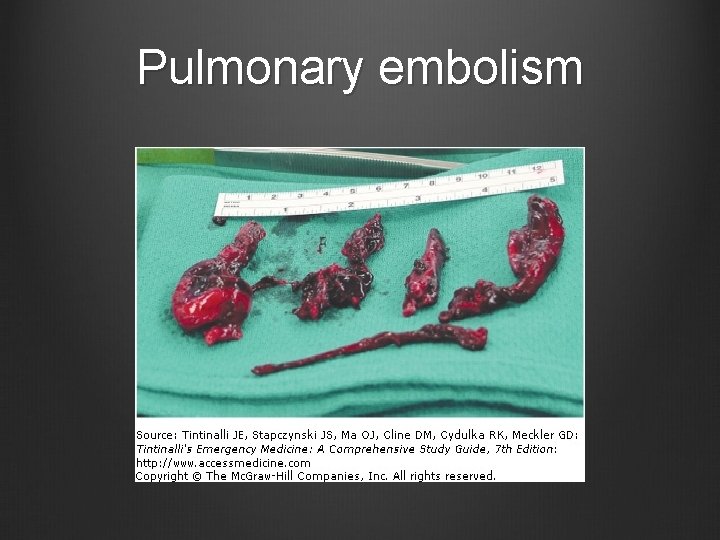
Pulmonary embolism

Objectives Know when to suspect PE – presenting syndromes Use of a risk stratified approach to assessment for PE Investigations of utility in PE assessment PE management

Presenting symptoms Unexplained dyspnoea cardinal symptom (74% pt’s) Only 50% describe this as ‘sudden onset’ Chest pain less frequent (44 -63%) – may be varying character Cough, wheeze, haemoptysis only variably present (2030% cases) Central PE – Dyspnoea, syncope, hypotension, tachycardia, ‘cardiac’ chest pain Peripheral PE – Pleuritis, gradual dyspnoea(multiple)

Clinical features Frequently normal exam Sinus tachycardia only consistent finding in large PE Hypoxia often absent ECG often reflects STach, frequently normal Classical features, RBBB, STach and S 1 Q 3 T 3

Risk assessment Difficult to dx on clinical grounds Requires diagnostic testing – testing expensive and irradiating Require strategies to reduce risk to <2% or >80% Can justify not treating/treating on these grounds How high is high risk? How low is low risk?

Scoring systems ‘Gestalt’ Wells score – now dichotimised to high risk/low risk with cut off score of 4 Geneva score Use insight or logistically derived variables to increase or decrease pre-test probability Pre-test probability determines subsequent test performance

Test probability If pre test probability = ‘low risk’, baseline risk ~ 4 -8% If pre test probability = ‘high risk’ baseline risk ~ 50 -75% Therefore, low risk patients need test to lower risk < 2 -3% (‘rule out’); and high risk patients need test to increase risk >80% (‘rule in’) ‘Rule out’ tests generally high sensitivity, but low specificity Higher specificity (‘Rule in’) testing in PE more resource intensive and involve radiation exposure

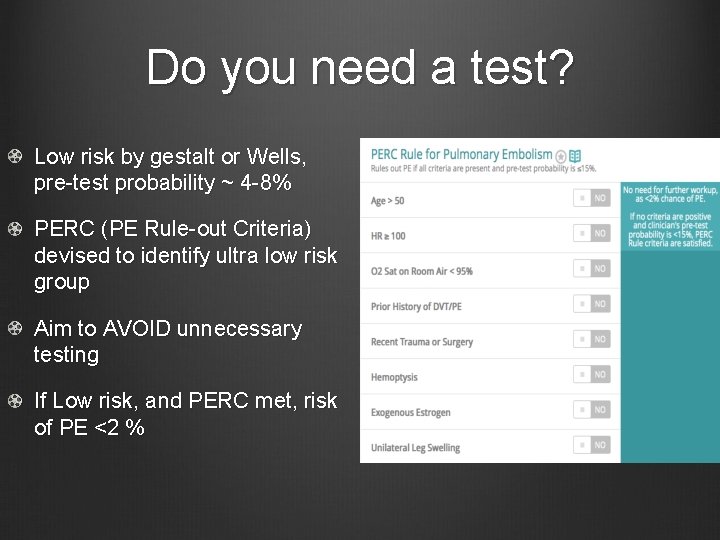
Do you need a test? Low risk by gestalt or Wells, pre-test probability ~ 4 -8% PERC (PE Rule-out Criteria) devised to identify ultra low risk group Aim to AVOID unnecessary testing If Low risk, and PERC met, risk of PE <2 %

The Low Risk patient Stratified low risk by Wells/Gestalt/Geneva Unable to rule out with PERC D-Dimer testing – LR 0. 15 if -ve, 2. 0 if +ve Causes positive D-Dimer Age Arterial thrombosis Pregnancy GI hemorrhage Infection Smoking . 15 x 8% 1% risk if –ve Trauma(surgery) However, 2. 0 x 8% = 16% risk if +ve, ACS i. e little use Inflammatory conditions D-Dimer degrades in 72 hrs Multiple false positives CVA Malignancy

The High Risk patient V/Q scan CT pulmonary angiogram TTE Doppler USS Troponin? BNP? ABG?

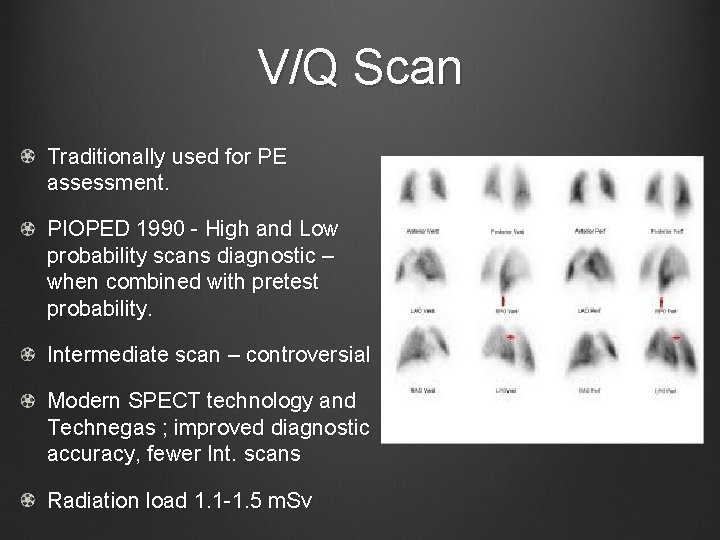
V/Q Scan Traditionally used for PE assessment. PIOPED 1990 - High and Low probability scans diagnostic – when combined with pretest probability. Intermediate scan – controversial Modern SPECT technology and Technegas ; improved diagnostic accuracy, fewer Int. scans Radiation load 1. 1 -1. 5 m. Sv

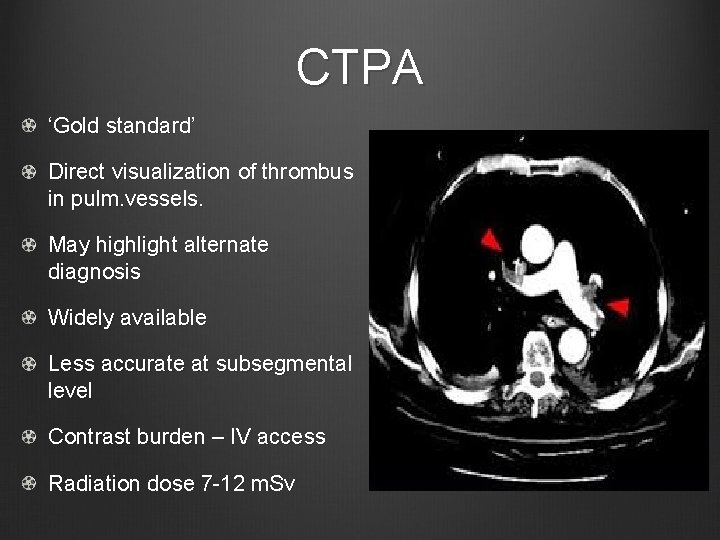
CTPA ‘Gold standard’ Direct visualization of thrombus in pulm. vessels. May highlight alternate diagnosis Widely available Less accurate at subsegmental level Contrast burden – IV access Radiation dose 7 -12 m. Sv

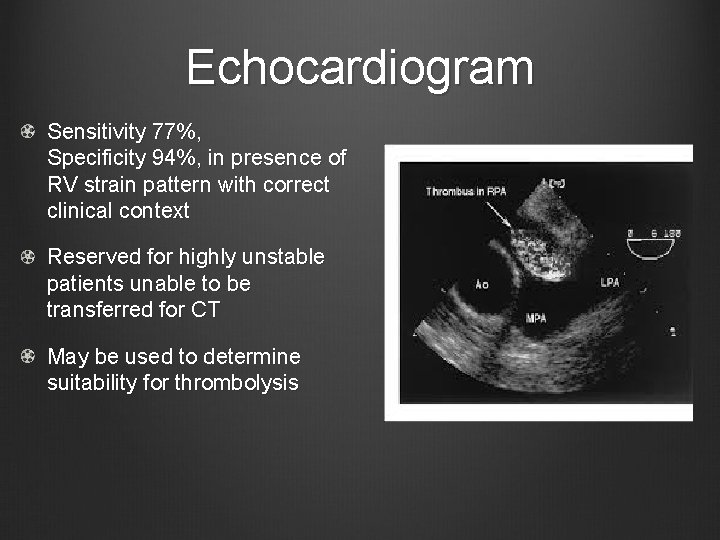
Echocardiogram Sensitivity 77%, Specificity 94%, in presence of RV strain pattern with correct clinical context Reserved for highly unstable patients unable to be transferred for CT May be used to determine suitability for thrombolysis

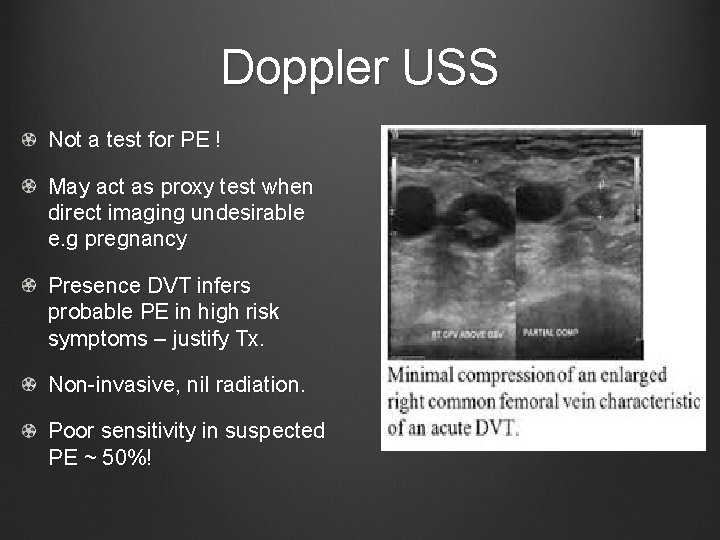
Doppler USS Not a test for PE ! May act as proxy test when direct imaging undesirable e. g pregnancy Presence DVT infers probable PE in high risk symptoms – justify Tx. Non-invasive, nil radiation. Poor sensitivity in suspected PE ~ 50%!

Ancillary testing v Troponin v ABG – ‘the A-a gradient’ Often ordered for chest pain workup Historically used to detect hypoxia Shown to reflect worse outcome for ? pre-dates the pulse oximeter? PE. No diagnostic value; May be used for risk stratification May be useful in shocked PE pt. v BNP Similar to troponin. Suggestive of RV strain Doesn’t alter management acutely May be used for risk stratification

Treatment – Stable patient Heparinisation mainstay of therapy UFH and enoxparin equally efficacious – initial treatment recommendation. Warfarin and Novel Anticoagulants equally efficacious Enoxaparin and No. ACs unable to be used in significant renal impairment Provoked PE – 3 mths therapy Unprovoked – at least 3 mths, ? longer. Recurrent events = lifelong Low risk pts potentially able to be risk stratified and discharged from ED (not at SDMH)

Treatment – Shocked pt IN hypotensive/shocked/arrested patient with PE – Thrombolysis Alteplase 10 mg stat then 90 mg infusion over 2 hrs OR Tenecteplase as per STEMI guideline with concurrent heparinisation Presence of RV strain, elevated biomarkers now NOT considered grounds for thrombolysis; Benefits in short term offset with bleeding risk in intermediate term

Adult Pneumonia

Objectives Assessment of pneumonia Severity scoring and associated management The severe pneumonia pt

Assessment Classic symptoms – cough, fever, sputum, SOB, +/- chest pain Atypical – Headache, nausea, diarrhoea Elderly – confusion, falls Exam - Unilateral crepitations +/- fever, increased Wo. B Chest infiltrate on CXR

Higher risk Group Pathogen Neutropaenia/Chemotherapy Ps aeruginosa/Staph/fungi CLL, Myeloma, Nephrotic syndrome Strep. pneumoniae and Haemophilus AIDS/Immunosuppressed (prednisone!) PCP, Legionella, Strep, Viral and fungal pneumonias

Severity assessment Clinical assessment CXR UEC/Albumin/FBC Sputum and blood cultures if hospitalised Consider viral respiratory screen ABG only for severe disease Urine assays pneumococcal/legionella Ag may be useful

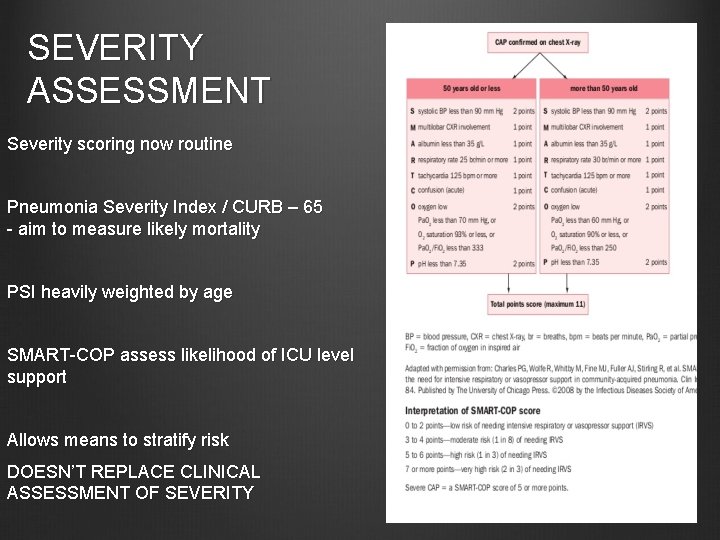
SEVERITY ASSESSMENT Severity scoring now routine Pneumonia Severity Index / CURB – 65 - aim to measure likely mortality PSI heavily weighted by age SMART-COP assess likelihood of ICU level support Allows means to stratify risk DOESN’T REPLACE CLINICAL ASSESSMENT OF SEVERITY

MANAGEMENT Penicillin based regimes highly effective at treating pneumonia Severity scoring can risk stratify patients suitable for oral outpatient therapy Ceftriaxone replaces penicillin where allergy a concern for IV treatment Outpatient IV therapy not required (except HLCNH pt’s)

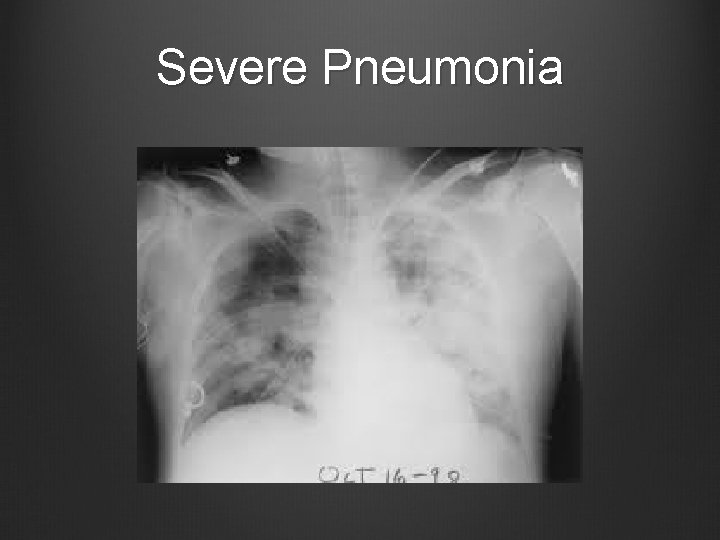
Severe Pneumonia

Severe pneumonia Often able to be predicted in ED. RR most sensitive indicator Hypotension/Severe sepsis criteria Falling O 2 sats, or Pa. O 2/Fi. O 2 ratio <250 predicts need for ICU ventilatory assistance Hyponatraemia, leucopaenia, renal failure, thrombocytopaenia suggestive of severe pneumonia Multilobe involvement, cavitation, pleural effusion also suggest worse course

In ED Recognise deteriorating clinical state Antibiotics within 1 st hour – ceftriaxone + azithromycin Consider Staph, anaerobes, Ps. aeruginosa depending upon clinical picture – amend a/b cover O 2 support and ICU consultation early if difficulty maintaining Sats. Hypoxia and hypotension CVC and inotropes early, avoid excessive fluid loading NIPPV usually NOT able to be mainstay of treatment – intubation often required, and should be anticipated and attended early

Questions?

Summary Consider relative risk of PE – do you need a test? PERC and D-dimer can exclude large proportion of patients Thrombolysis now only for shocked patients Pneumonia may be suitable for outpatient therapy Establish severity of pneumonia when diagnosing Severe pneumonia often needs intubation – get ICU help early