Grampositive bacteria Staphylococci Staphylococcus aureus causes a variety
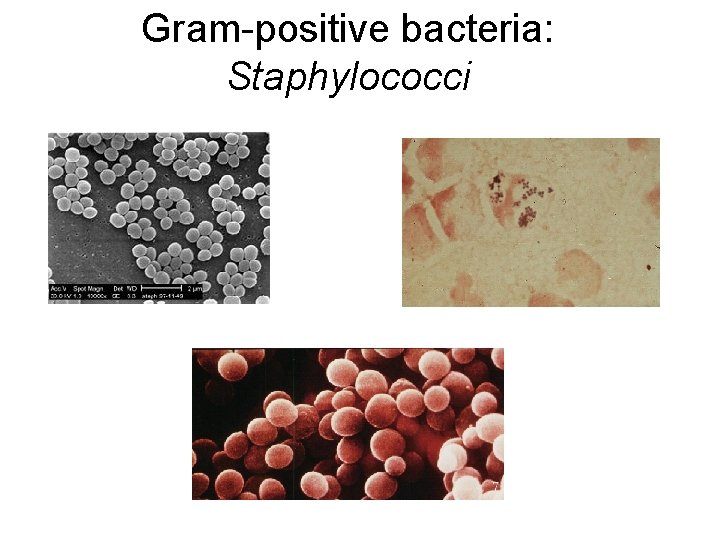
Gram-positive bacteria: Staphylococci
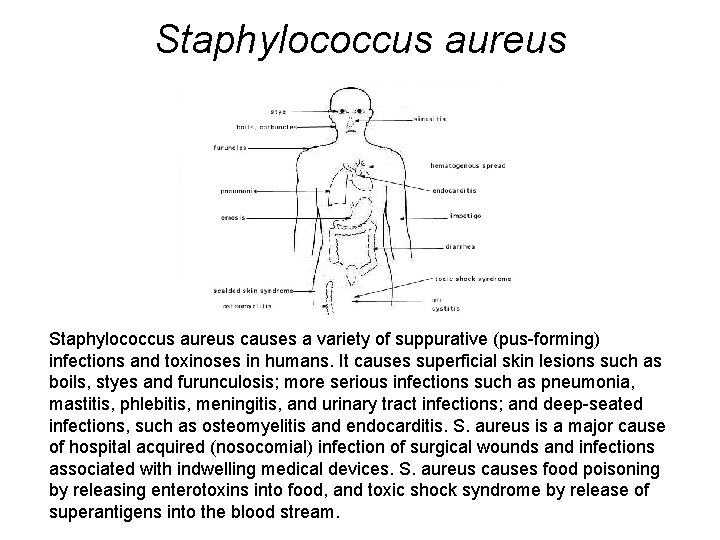
Staphylococcus aureus causes a variety of suppurative (pus-forming) infections and toxinoses in humans. It causes superficial skin lesions such as boils, styes and furunculosis; more serious infections such as pneumonia, mastitis, phlebitis, meningitis, and urinary tract infections; and deep-seated infections, such as osteomyelitis and endocarditis. S. aureus is a major cause of hospital acquired (nosocomial) infection of surgical wounds and infections associated with indwelling medical devices. S. aureus causes food poisoning by releasing enterotoxins into food, and toxic shock syndrome by release of superantigens into the blood stream.

Staphylococcus aureus • http: //www. visualdxhealth. com/pdfs/MRSA %20 Handout. pdf

Superantigens • http: //highered. mcgrawhill. com/sites/0072556781/student_view 0/ chapter 32/animation_quiz_4. html
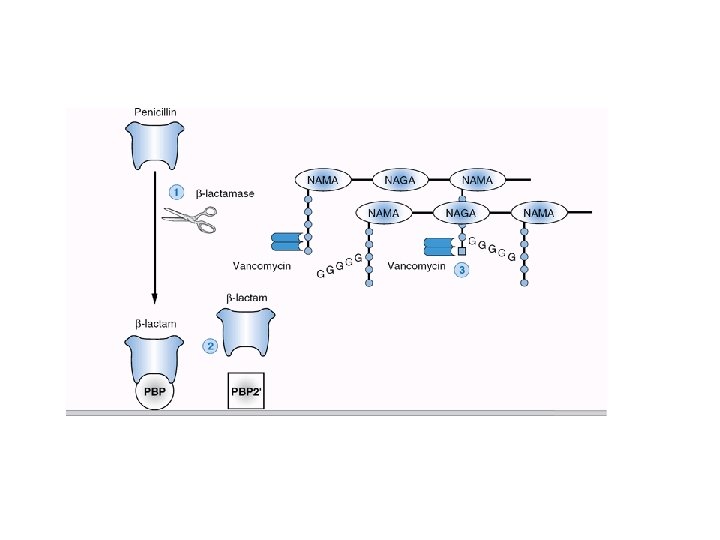

Treatment of Infections Caused by Staphylococcus aureus • Antistaphylococcal penicillins: Nafcillin, oxacillin • First Generation cephalosporins: Cefazolin • Second Generation Cephalosporins: Cefurxime • Third-generation cephalosporins: Ceftriaxone, cefotaxime, ceftizoxime • B-Lactam/b-lactamase inhibitor combinations: Ampicillin-sulbactam, piperacillin-tazobactam, ticarcillin-clavulanate • Carbapenems: Imipenem, meropenem

Treatment of Methicillin-resistant Staphylococcus aureus • • • Vancomycin Linezolid Streptogramins (Quinupristin-dalfopristin) Daptomycin Tigecycline
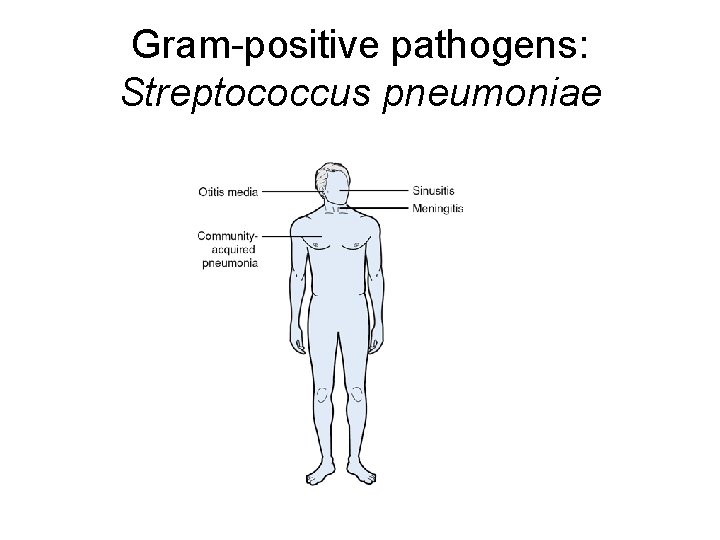
Gram-positive pathogens: Streptococcus pneumoniae
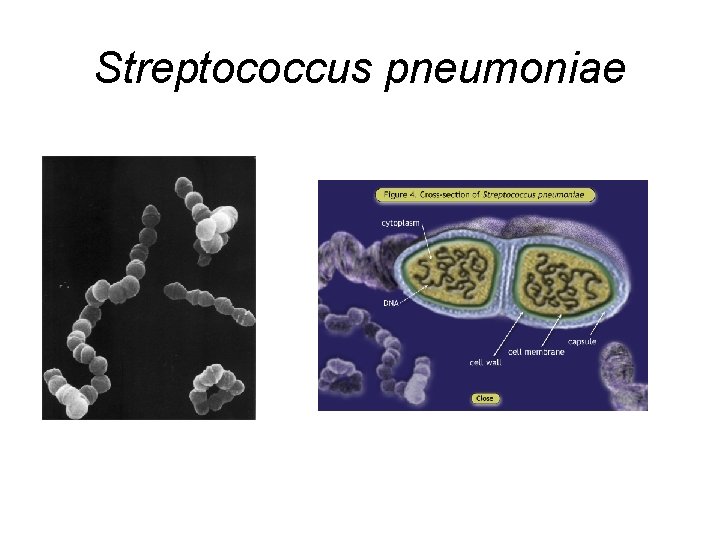
Streptococcus pneumoniae

Treatment of Streptococcus pneumoniae • Penicillin G • Aminopenicillins: Ampicillin

Treatment of Penicillin-resistant Streptococcus pneumoniae • Second Generation Cephalosoporins: Cefuroxime • Third Generation Cephalosporins: Cefotaxime, Ceftriaxone • Quinolones: Moxifloxacin, Levofloxacin • Vancomycin • Macrolides/ketolines: Telithromycin
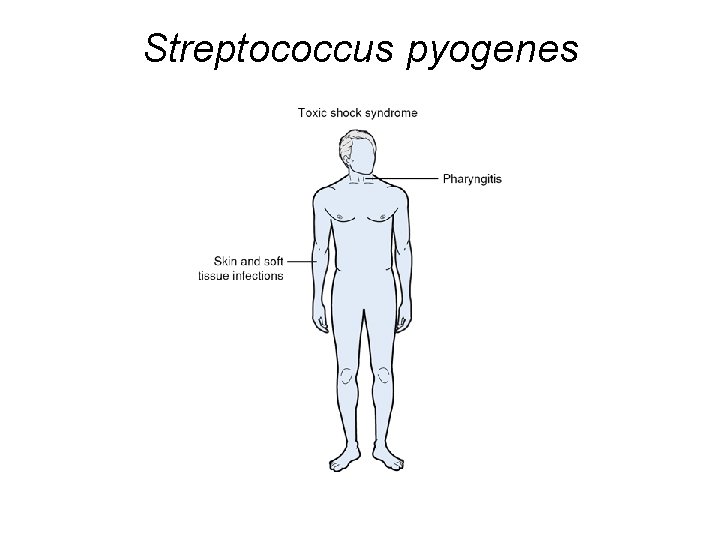
Streptococcus pyogenes
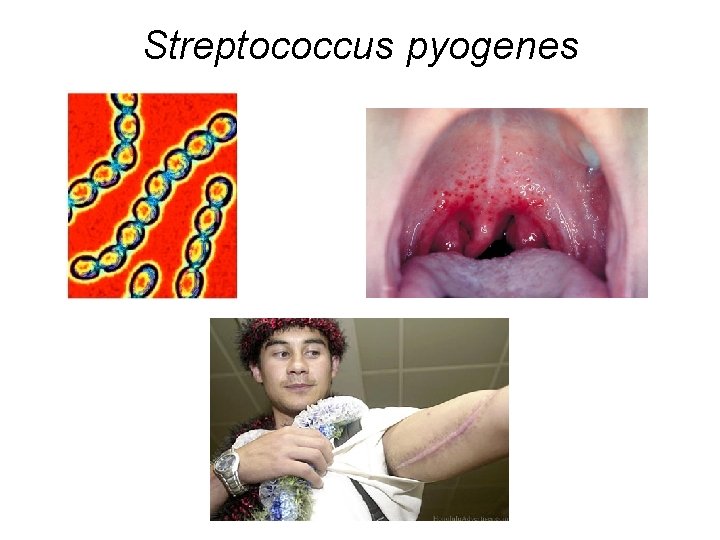
Streptococcus pyogenes

Treatment of Streptococcus pyogenes • Penicillin G • Aminopenicillins: Ampicillin • Aminoglycosides are sometimes added for synergy: Gentamicin • Clindamycin is added for severe invasive Streptococcus pyogenes infections

Treatment for Penicillin-resistant Streptococcus pyogenes (and other penicillin resistant Streptococcus) • Vancomycin • Second-generation cephalosporins: Cefuroxime • Third-generation cephalosporins: cefotaxime, ceftriaxone
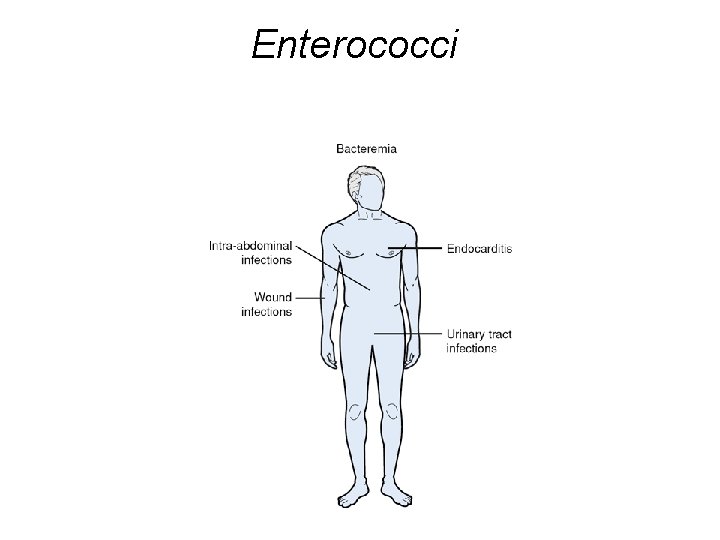
Enterococci
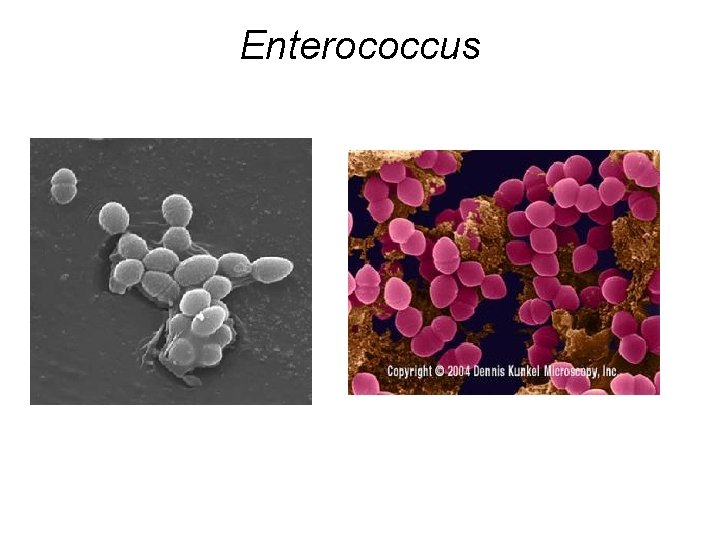
Enterococcus
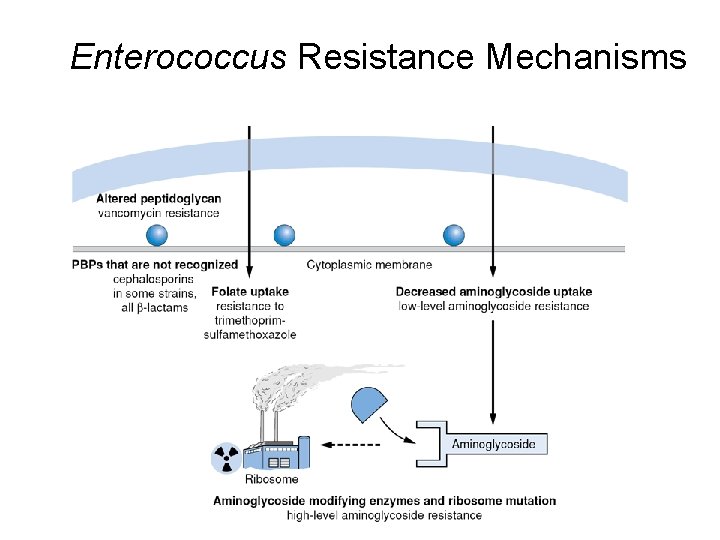
Enterococcus Resistance Mechanisms

Treatment of Infections Caused by Enterococcus • • • Penicillin G Aminopenicillins: Ampicillin Extended-spectrum Penicillins: Piperacillin Carbapenems: Imipenem, meropenem For serious infections, add an aminoglycoside for synergy: Gentamicin

Treatment for Infections Caused by Penicillin-resistant Enterococci • Vancomycin

Treatment for Vancomycin Resistant Enterococci (VRE) • Linezolid • Tetracycline-like: Tigecycline • Sometimes also active: – Daptomycin – Quinupristin/dalfopristin
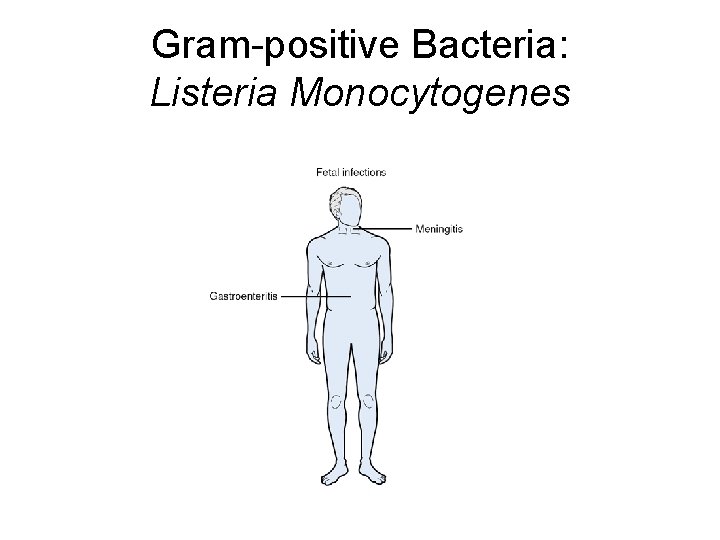
Gram-positive Bacteria: Listeria Monocytogenes
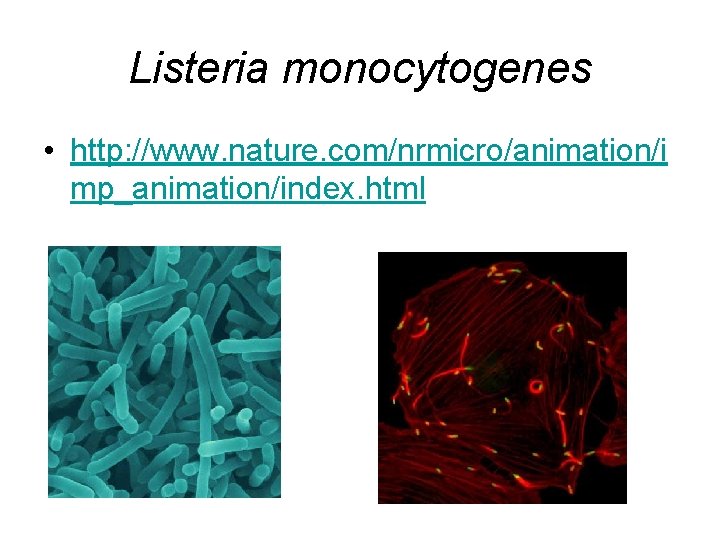
Listeria monocytogenes • http: //www. nature. com/nrmicro/animation/i mp_animation/index. html

Treatment of Infections Caused by Listeria monocytogenes • Ampicillin + Gentamicin • If penicillin allergic: – Trimethoprim-sulfamethoxazole
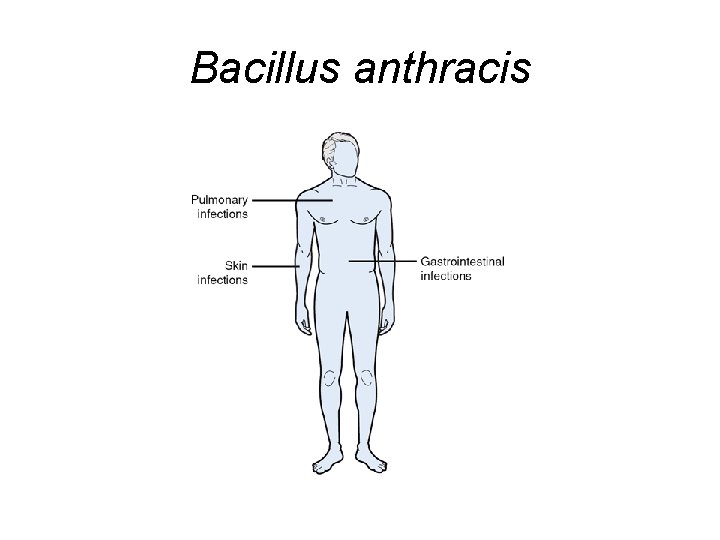
Bacillus anthracis
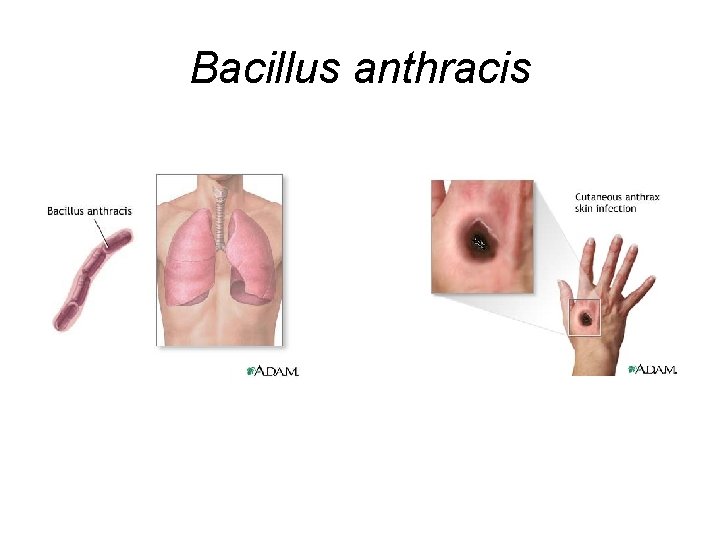
Bacillus anthracis
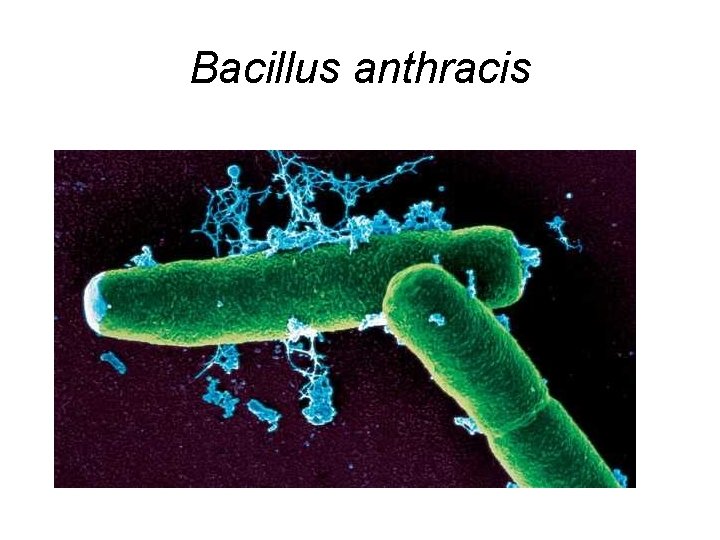
Bacillus anthracis

Treatment of Infections Caused by Bacillus anthracis • Quinolones: Ciprofloxacin • Tetracycline: Doxycycline

Treatment of Infections Caused by Bacillus anthracis • For Inhalation Anthrax, a Second Agent Should be Added from the Following List: – – – – Rifampin Vancomycin Penicillin G Ampicillin Chloramphenicol Carbapenem: Imipenem Clindamycin Macrolide: Clarithromycin
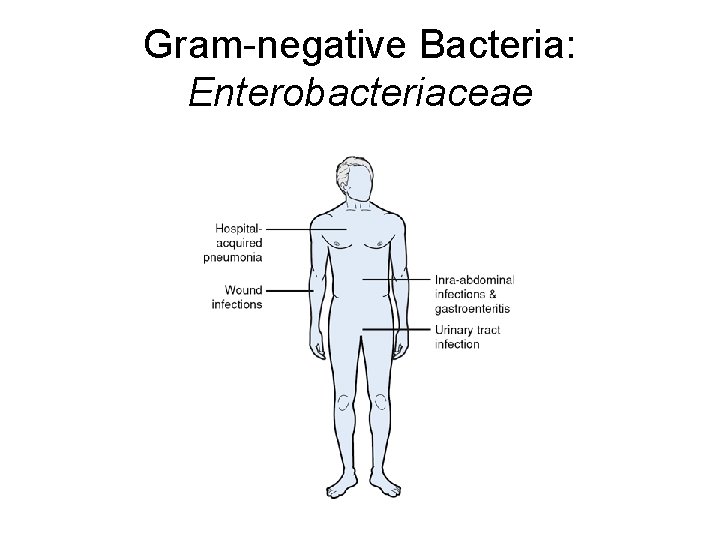
Gram-negative Bacteria: Enterobacteriaceae
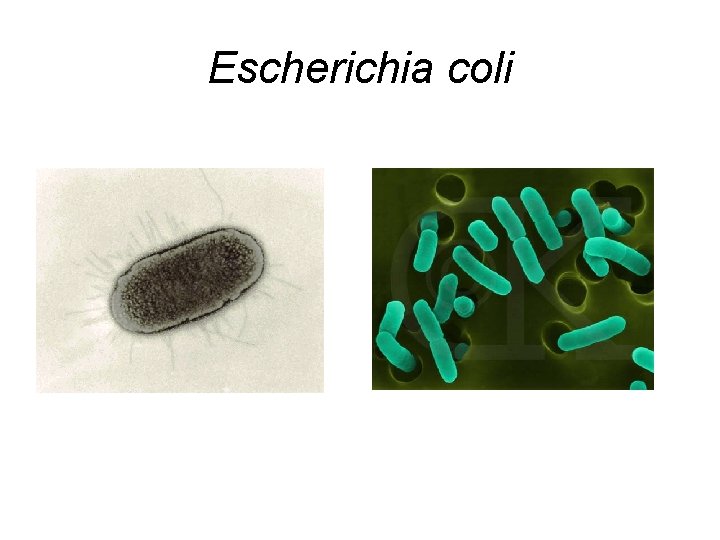
Escherichia coli
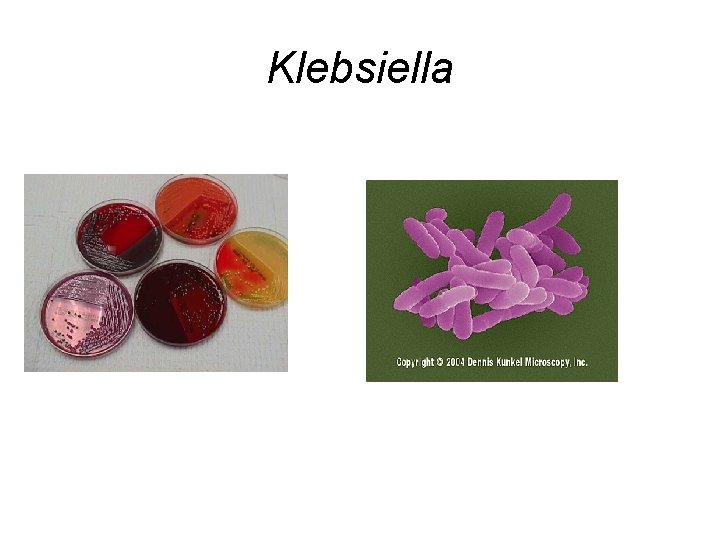
Klebsiella
Proteus

Escherichia coli. • http: //www. hhmi. org/biointeractive/media/e coli-lg. mov • http: //www. drkoop. com/animation/93/43. ht ml

Treatment of Infections Caused by: E. coli. , K. pneumoniae, Proteus • Aminopenicillins: Ampicillin • First Generation Cephalosporins: Cefazolin • Sulfa drugs: Trimethoprimsulfamethoxazole • Quinolones: Ciprofloxacin, levofloxacin, moxifloxacin

Treatment of Resistant Infections Caused by: E. coli. , K. pneumoniae, Proteus • Third Generation Cephalosporins: Cefoxaxime, ceftriaxone, ceftizoxime • Monobactam: Aztreonam • Extended Spectrum penicillins + blactamase inhibitor: Piperacillintazobactam, ticarcillin-clavulanate • Carbapenems: Imipenem, meropenem, ertapenem • Carbapenem + aminoglycoside in serious infections: Add Gentamicin, Tobramycin, amikacin

Treatment of Infections Caused by: Enterobacter, Serratia, Citrobacter, Providencia, and Morganella Spp. • Carbapenems: Imipenem, meropenem, ertapenem • Sulfa Drugs: Trimethoprimsulfamethoxazole • Quinolones: Ciprofloxacin, levofloxacin • Fourth Generation Cephalosporins: Cefepime • + aminoglycoside: Gentamicin, tobramycin, amikacin

Treatment of Infections Caused by: Salmonella enterica, Shigella spp. • Quinolones: Ciprofloxacin • Third-generation cephalosporins: Cefotaxime, ceftriaxone, ceftizoxime • Macrolides: Azithromycin

Treatment of Infections Caused by: Yersinia spp. • Aminoglycosides: Gentamicin, streptomycin • Tetracyclines: Doxycycline • Quinolones: Ciprofloxacin • Sulfa drugs
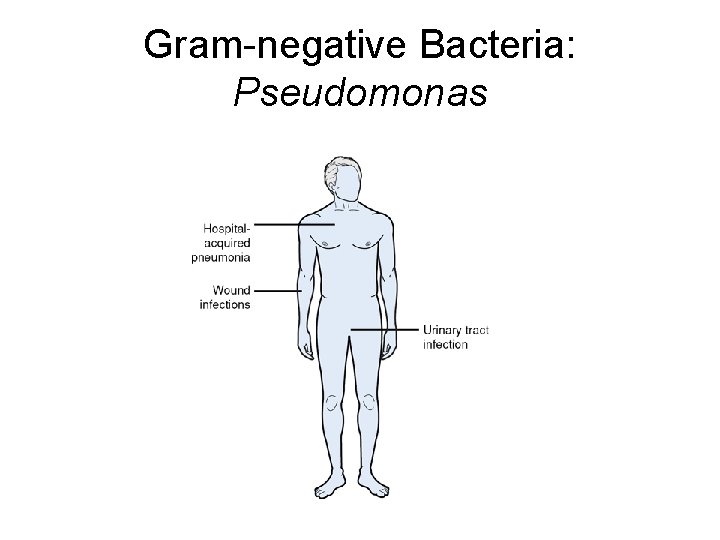
Gram-negative Bacteria: Pseudomonas
Pseudomonas
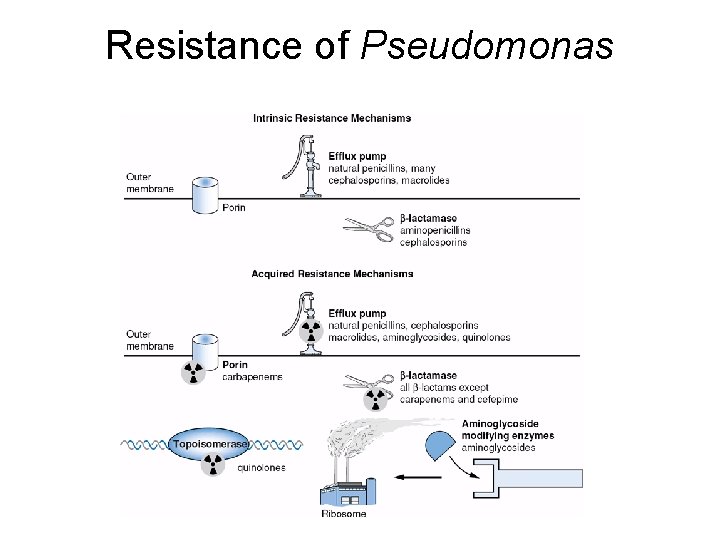
Resistance of Pseudomonas

Treatment of Infections caused by Pseudomonas aeruginosa • Extended spectrum penicillins: Piperacillin, Ticarcillin • Third Generation Cephalosporins: Ceftazidime • Fourth-generation Cephalosporins: Cefepime • Carbapenems: Imipenem, meropenem • Monobactams: Aztreonam • Quinolones: Ciprofloxacin, Levofloxacin • Aminoglycosides: Gentamicin, tobramycin, amikacin

Treatment of Serious Infections Caused by Pseudomonas aeruginosa • Antipseudomonal b-lactam + aminoclycoside: Ceftazidime + Tobramycin • Extended-spectrum penicillin + antipseudomonal quinolone: Piperacillin + Ciprofloxacin
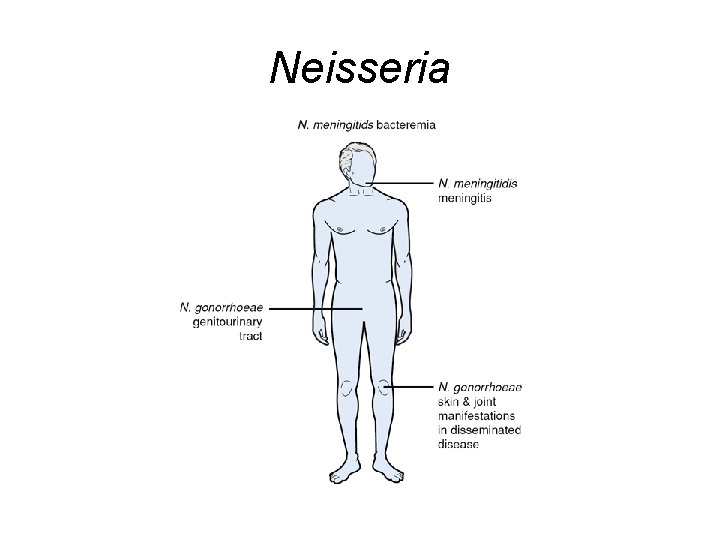
Neisseria
Neisseria meningitidis
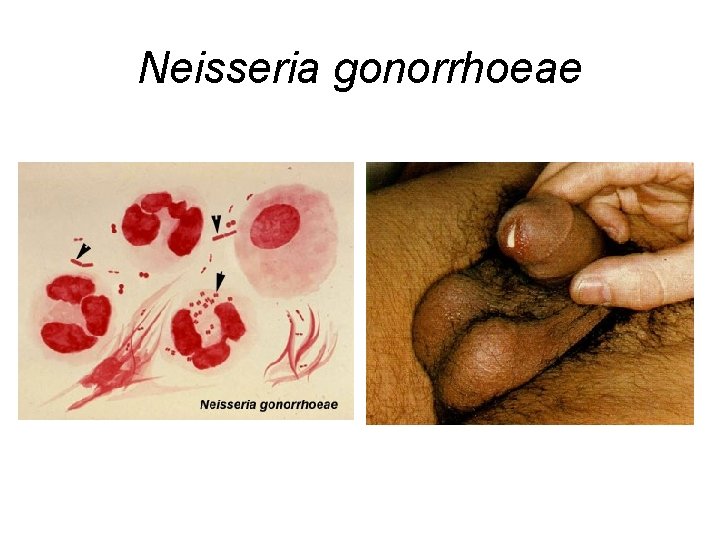
Neisseria gonorrhoeae

Treatment of Infections Caused by Neisseria meningitidis • Penicillin G • Third generation cephalosporins: Ceftriaxone, cefotaxime

Treatment of Infections Caused by Neisseria Gonorrhoeae • Third Generation Cephalosporins: Ceftriaxone, cefixime

Curved Gram Negative Bacilli • Includes: – Campylobacter jejuni, – Helicobacter pylori, – Vibrio cholerae
Campylobacter jejuni
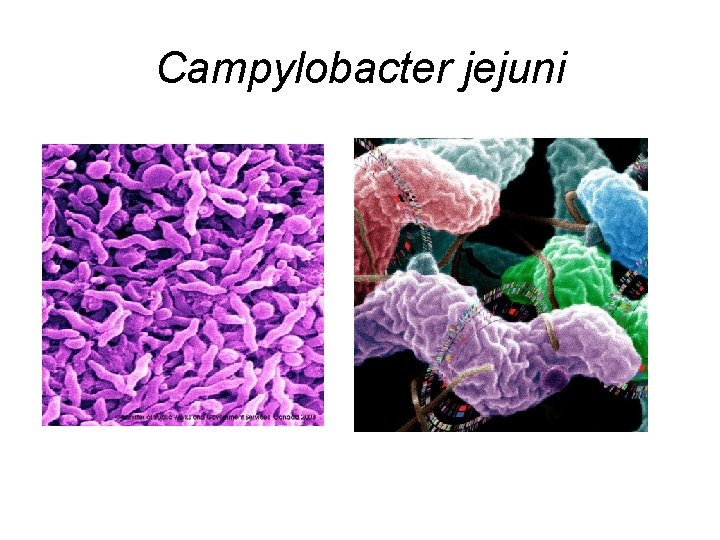
Campylobacter jejuni

Treatment of Infection Caused by Campylobacter jejuni • Macrolides: Erythromycin, azithromycin, clarithromycin • Quinolones: Ciprofloxacin
Helicobacteri pylori

Helicobacter pylori
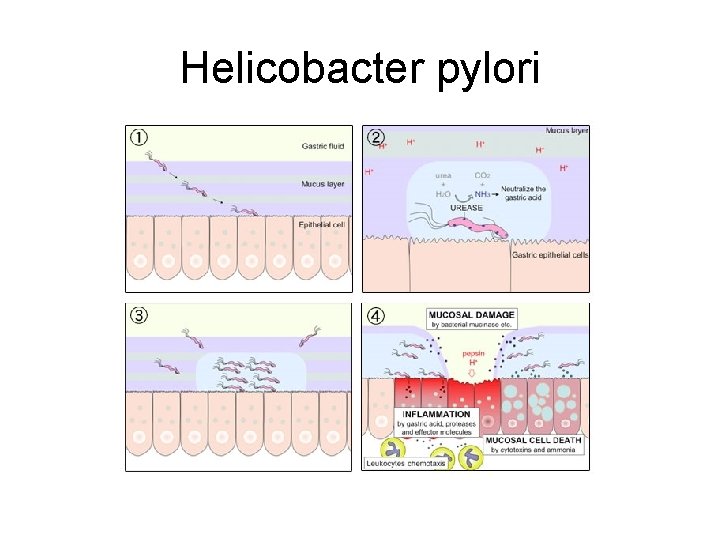
Helicobacter pylori
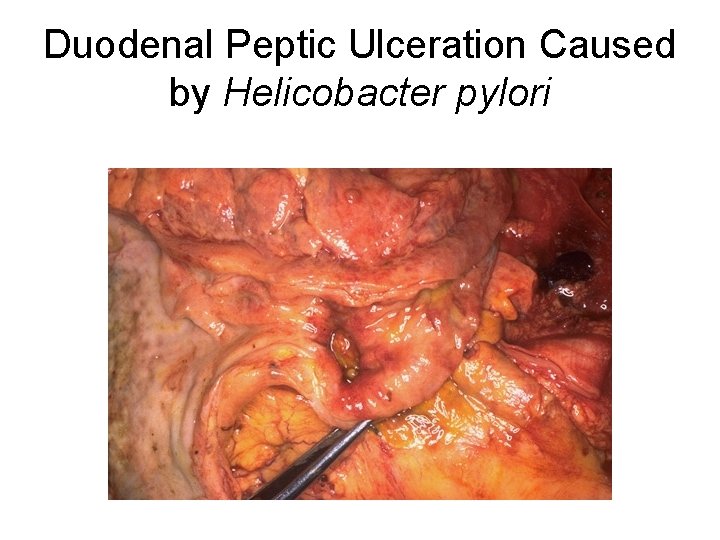
Duodenal Peptic Ulceration Caused by Helicobacter pylori

Treatment of Infection Caused by Helicobacter pylori • Amoxicillin + clarithromycin + proton pump inhibitor • Metronidazole + clarithromycin + proton pump inhibitor • Bismuth subsalicylate + metronidazole + tetracycline + proton pump inhibitor
Vibrio cholerae
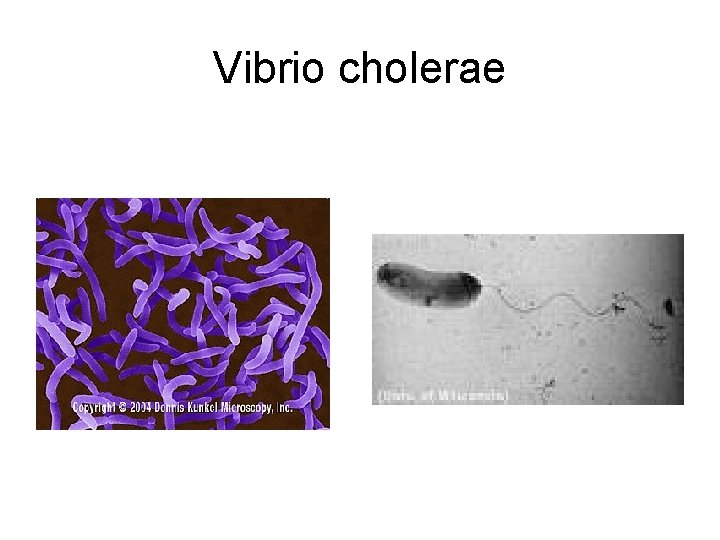
Vibrio cholerae

Treatment of Infection Caused by Vibrio cholerae • Tetracyclines: tetracycline, doxycycline • Sulfa drugs: Trimethoprimsulfamethoxazole • Quinolones: Ciprofloxacin • Macrolides: Erythromycin, Azithromycin
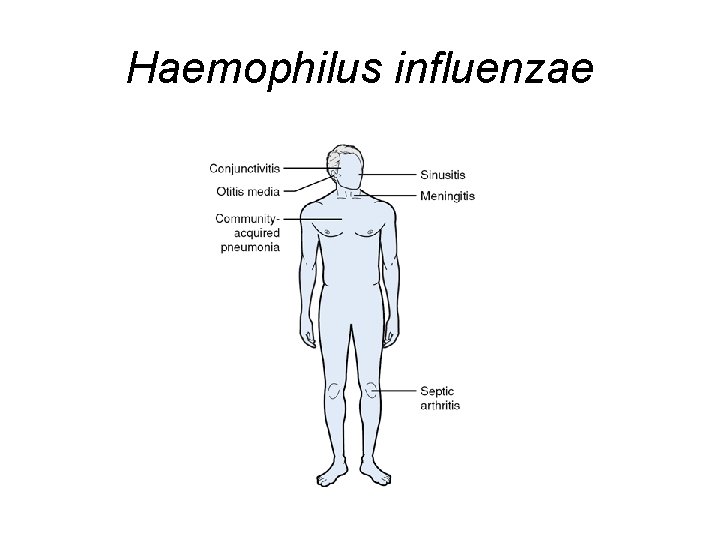
Haemophilus influenzae
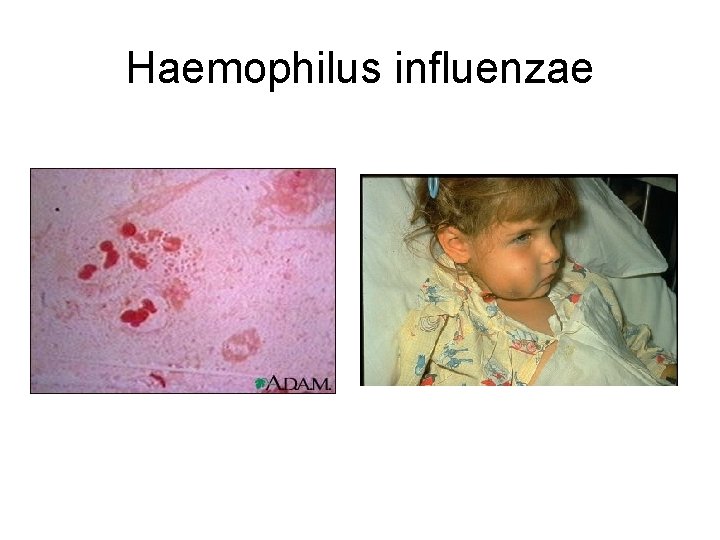
Haemophilus influenzae
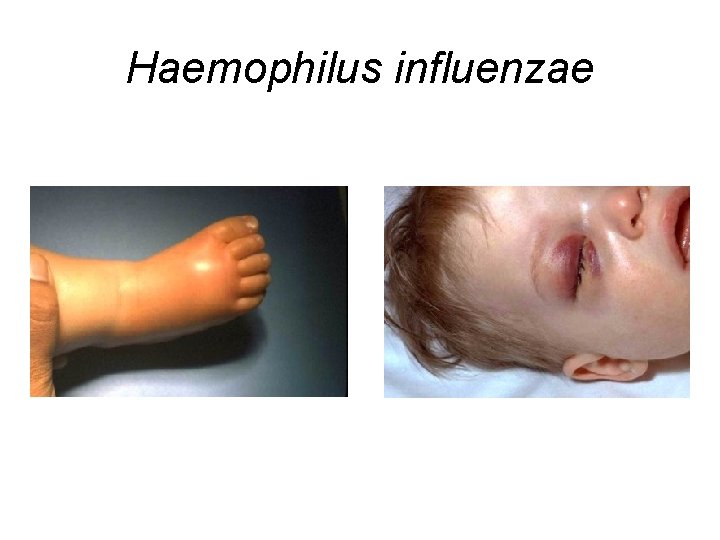
Haemophilus influenzae

Treatment of Infections Caused by Haemophilus influenzae • Aminopenicillins + b-lactamase inhibitor: – Amoxicillin/clavulanate – Ampicillin/sulbactam • Second-generation cephalosporin – Cefuroxime • Third-generation cephalosporin – Ceftriaxone – Cefotaxime
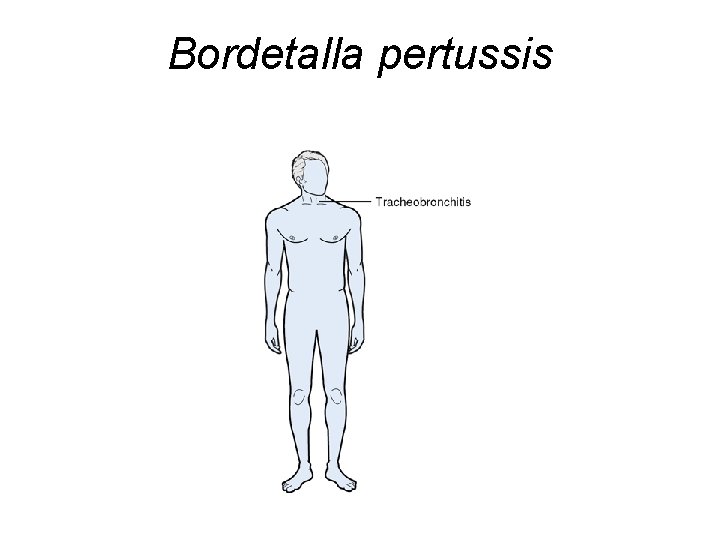
Bordetalla pertussis
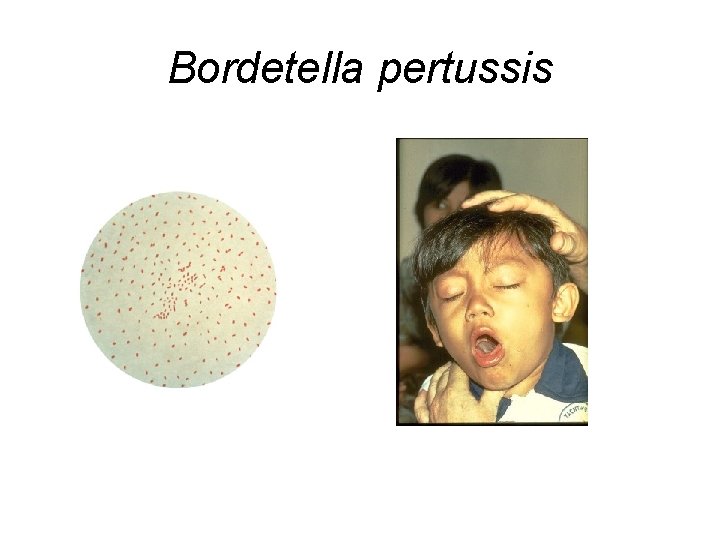
Bordetella pertussis

Treatment of Infection Caused by Bordetella pertussis • Macrolides: Azithromycin, Clarithromycin, Erythromycin

Moraxella catarrhalis • Causes otitis media, pneumonia, and sinusitis • Usually produces b-lactamase

Treatment of Infections Caused by Moraxella catarrhalis • Extended spectrum penicillins: piperacillin, ticarcillin • B-lactam/b-lactamase inhibitor combinations: piperacillin/tazobactam, ticarcillin/clavulanate • Second and third-generation cephalosporins

Acinetobacter • Recent outbreak among soldiers in Iraq • Second leading cause of infection among troops during the Vietnam conflict
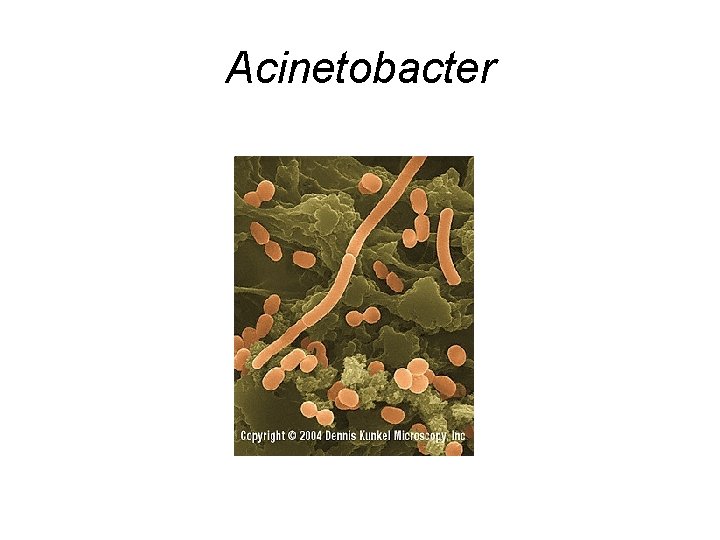
Acinetobacter

Treatment of Infection Caused by Acinetobacter • Sulbactam • Carbapenems • Quinolones
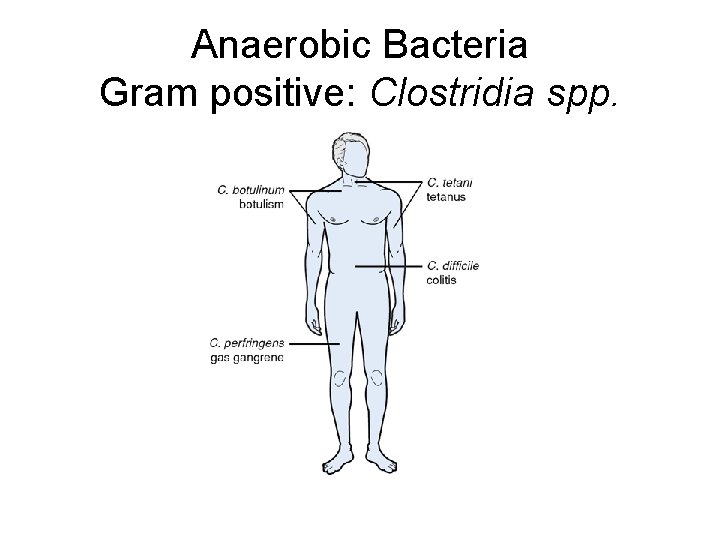
Anaerobic Bacteria Gram positive: Clostridia spp.
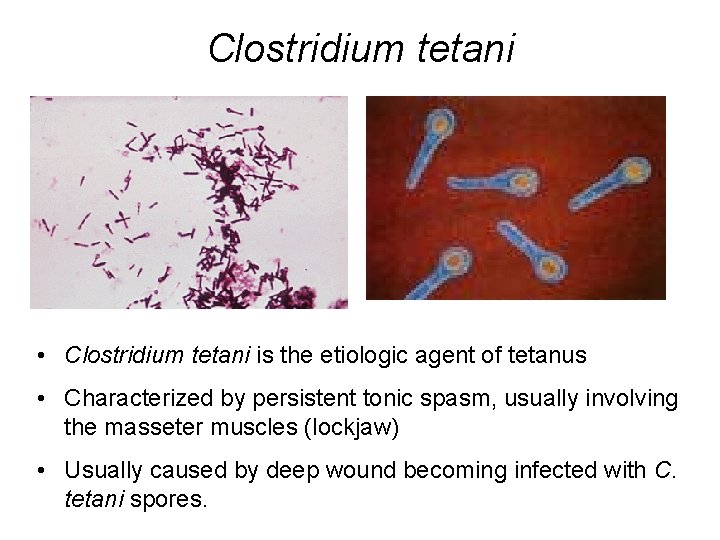
Clostridium tetani • Clostridium tetani is the etiologic agent of tetanus • Characterized by persistent tonic spasm, usually involving the masseter muscles (lockjaw) • Usually caused by deep wound becoming infected with C. tetani spores.
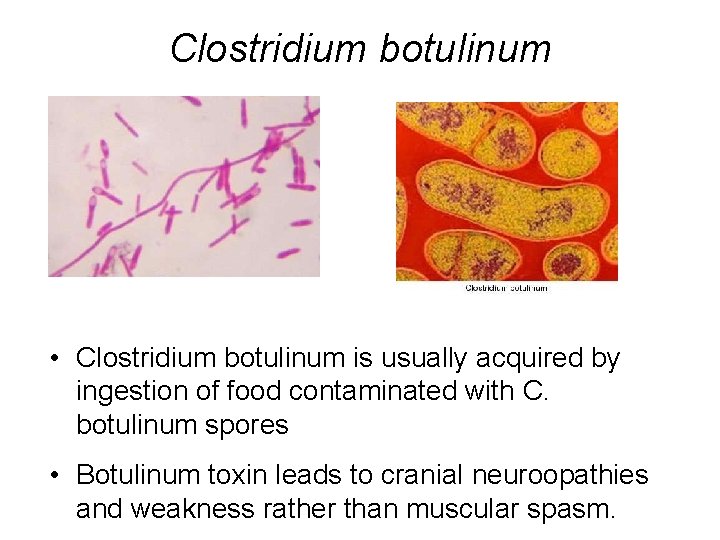
Clostridium botulinum • Clostridium botulinum is usually acquired by ingestion of food contaminated with C. botulinum spores • Botulinum toxin leads to cranial neuroopathies and weakness rather than muscular spasm.
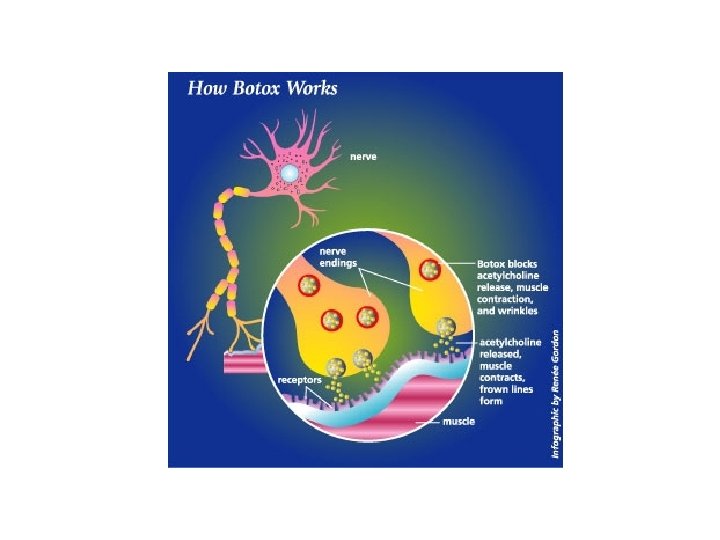

Treatment of Infections Caused by Clostridium spp. • Penicillin G • Metronidazole (may be associated with better outcomes
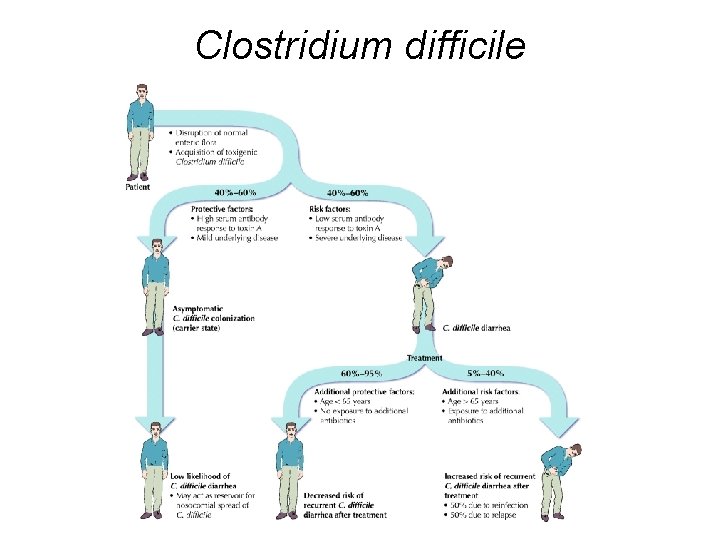
Clostridium difficile
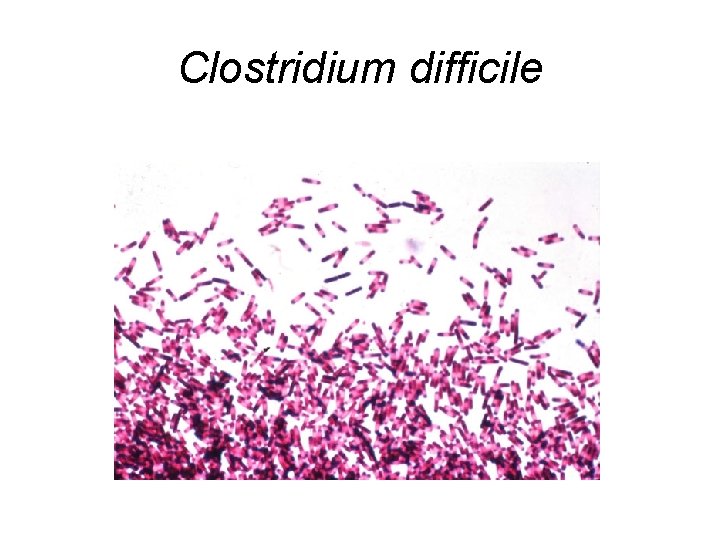
Clostridium difficile

Treatment of Infections Caused by Clostridium difficile • Oral metronidazole • Oral vancomycin
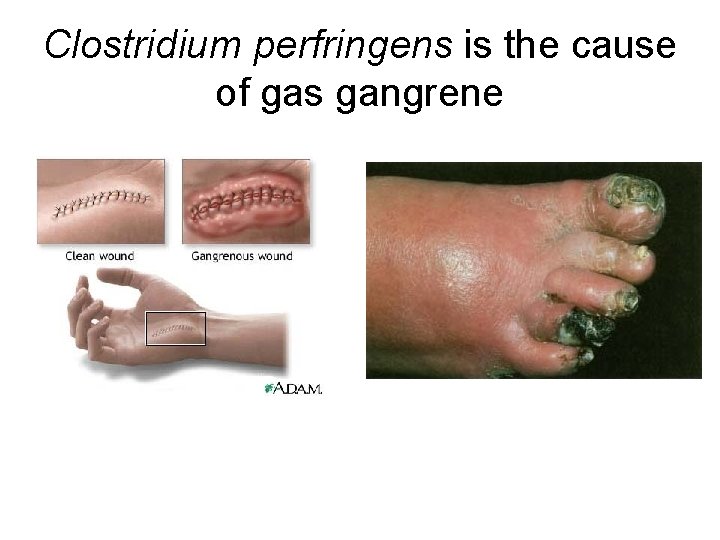
Clostridium perfringens is the cause of gas gangrene

Treatment of Infections Caused by Clostridium perfringens • Penicillin + one of the following: – Clindamycin – Tetracycline – Metronidazole
Anaerobic Gram-negative Bacteria

Common Anaerobic Gram-negative Pathogens • Bacteroides fragilis – Usually produces b-lactamase • Prevotella • Porphyromonas

Treatment of Anaerobic Gramnegative Infections • b-lactam/b-lactamase inhibitor combinations – Ampicillin-sulbactam – Piperacillin-tazobactam – Ticarcillin-clavulanate • Carbapenems: Imipenem, Meropenem, Ertapenem • Metronidazole
Atypical Bacteria: Chlamydia
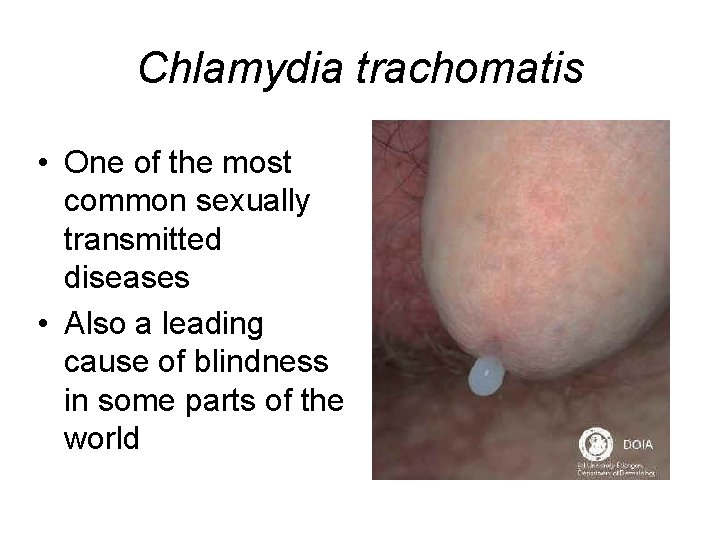
Chlamydia trachomatis • One of the most common sexually transmitted diseases • Also a leading cause of blindness in some parts of the world

Chlamydia trachomatis Chlamydia is a bacterial infection of the genital tract spread through sexual contact. If untreated, it can result in various medical complications, including damage to the reproductive organs. The disease affects both women and men, although reported cases for women greatly exceed those for men. Chlamydia affects people in all age groups, but it is particularly prevalent among teenagers and young adults. According to the U. S. Centers for Disease Control and Prevention (CDC), the infection is most prevalent among women aged 20 to 25.

Chlamydia trachomatis Some signs and symptoms that may be present in people infected with chlamydia are: • • • Abnormal discharge from the penis or vagina Burning sensation during urination Lower abdominal or back pain Nausea Fever Pain during intercourse Burning or itching around the head of the penis Swollen or tender testicles Bleeding between menstrual cycles Proctitis (inflammation of the rectum)

Treatment of Infections Caused by Chlamydia trachomatis • Tetracyclines – Tetracycline – Doxycycline • Macrolides – Azithromycin – Erythromycin – Telithromycin • Quinolones – Ofloxacin – Moxifloxacin – Gemifloxacin
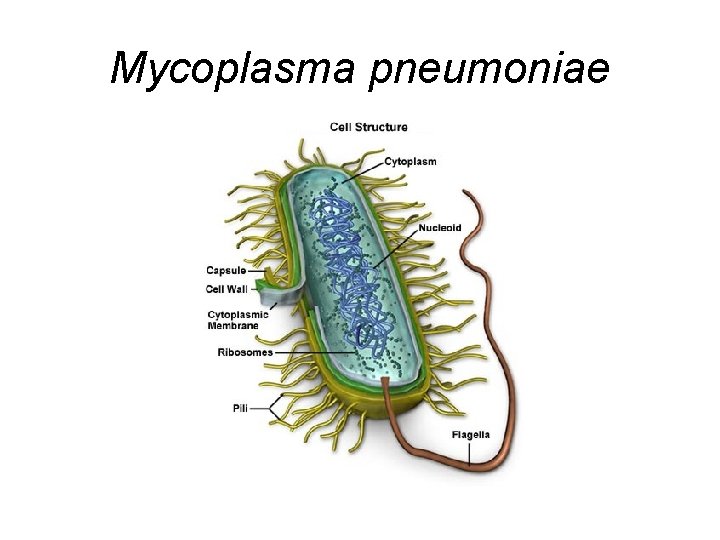
Mycoplasma pneumoniae
Mycoplasma pneumoniae

Treatment of Infections Caused by Mycoplasma pneumoniae • Macrolides: Azithromycin, clarithromycin, erythromycin telithromycin • Tetracyclines: Tetracycline, doxycycline • Quinolones: Levofloxacin, moxifloxacin, gemifloxacin
Atypical Bacteria: Legionella • Legionella pneumophila is the most common species, and is the causative agent of Legionaires’ disease • Once in the lung, Legionella organisms are taken up by macrophages and multiply within them.
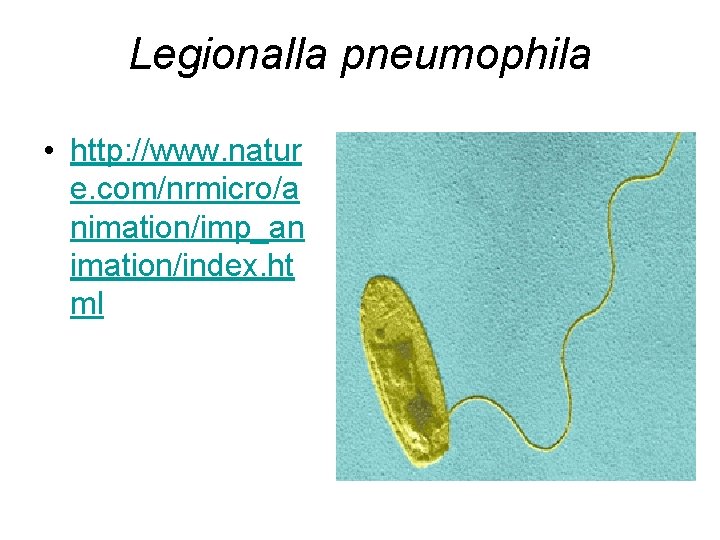
Legionalla pneumophila • http: //www. natur e. com/nrmicro/a nimation/imp_an imation/index. ht ml

Treatment of Infections Caused by Legionella pneumophila • Macrolides: Azithromycin • Quinolones: Levofloxacin, moxifloxacin

Brucella • Brucellosis is a disease of animals, that is occasionally transmitted to humans • Contact with animals and/or ingestion of unpasteurized milk or cheese are risk factors
Brucella
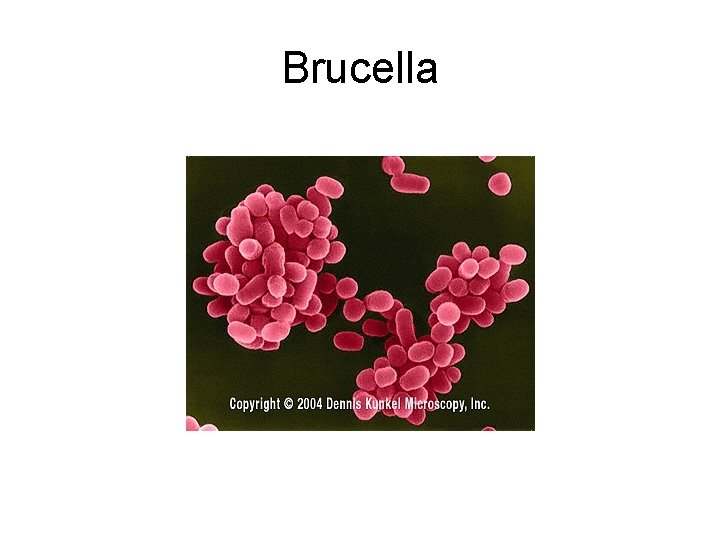
Brucella

Treatment of Infections Caused by Brucella spp. • Doxycycline + rifampin • Dixycycline + gentamicin • Doxycycline + streptomycin
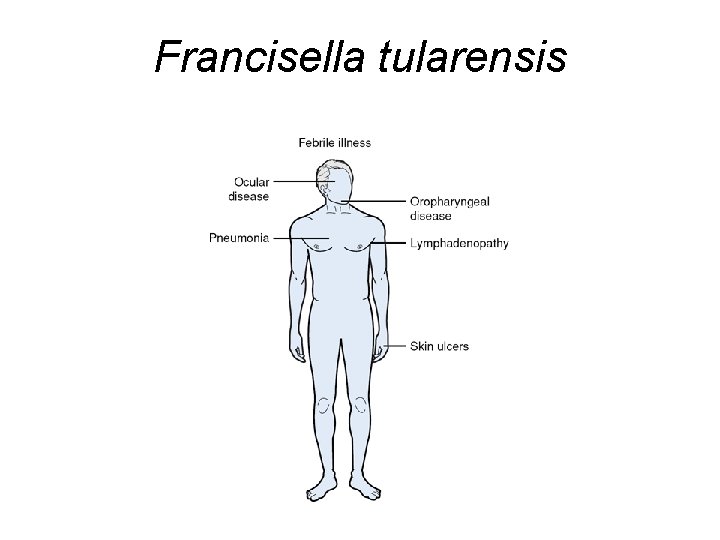
Francisella tularensis
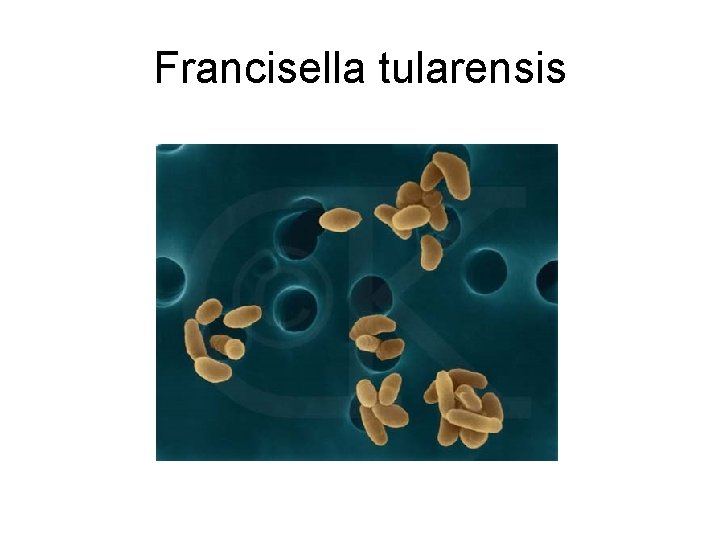
Francisella tularensis

Treatment of Infections Caused by Francisella tularensis • Aminoglycosides: Streptomycin, Gentamicin • Tetracyclines: Tetracycline, doxycycline
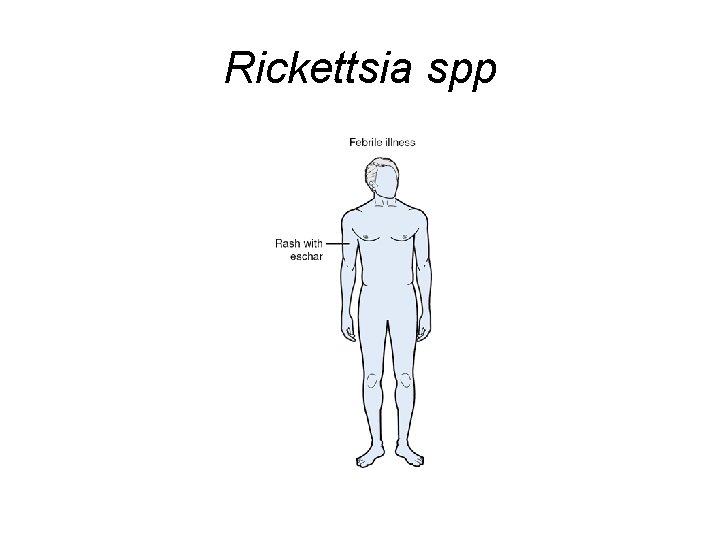
Rickettsia spp

Rickettsia rickettsii Rocky Mountain spotted fever is the most severe and most frequently reported rickettsial illness in the United States. The disease is caused by Rickettsia rickettsii, a species of bacteria that is spread to humans by ixodid (hard) ticks.

Treatment of Infections Caused by Rickettsia spp. • Tetracyclines – Doxycycline – Tetracycline
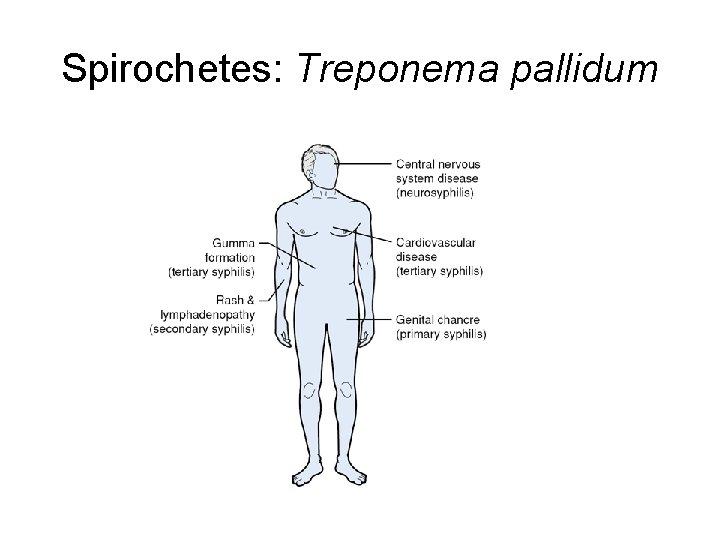
Spirochetes: Treponema pallidum
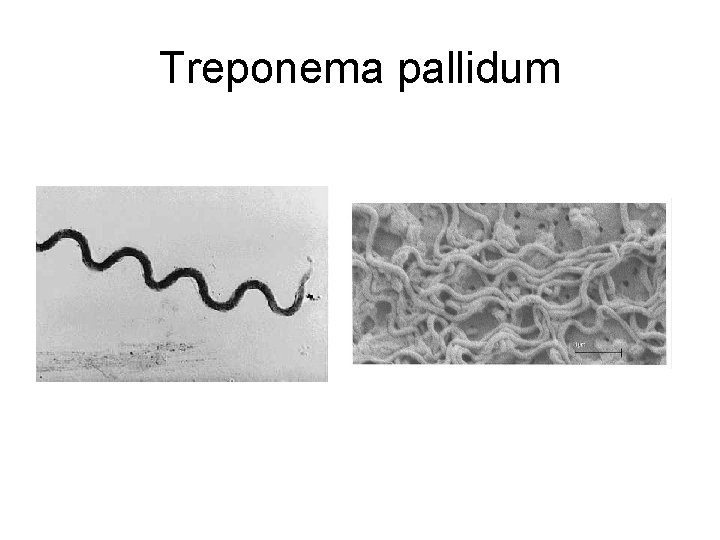
Treponema pallidum
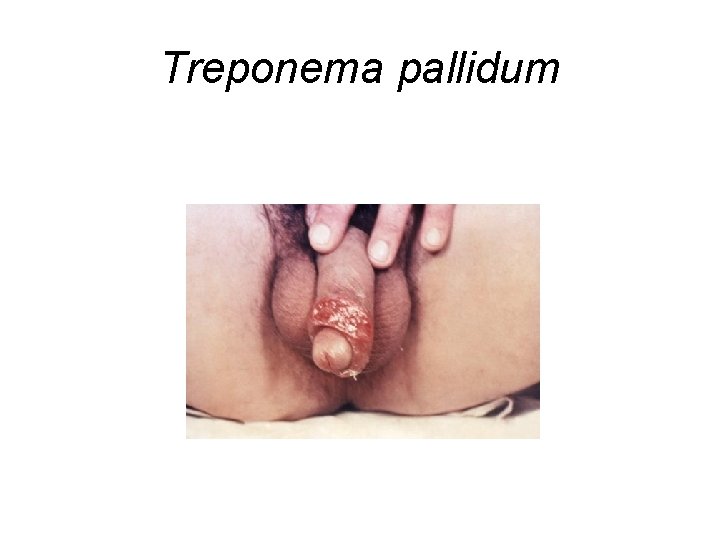
Treponema pallidum
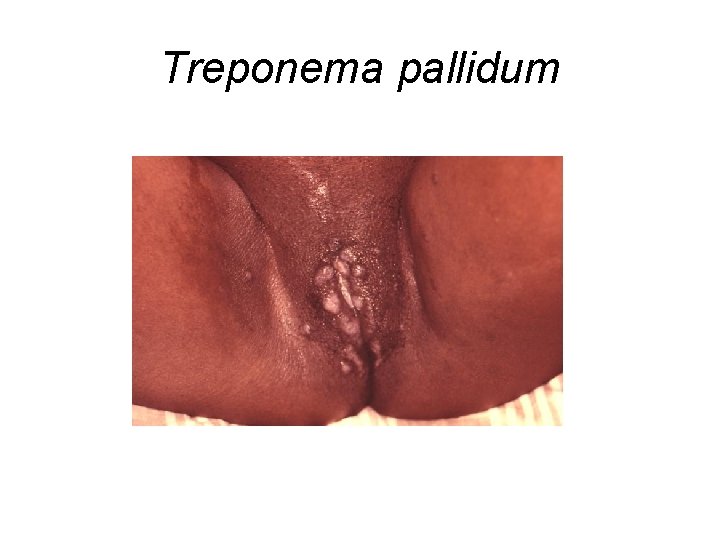
Treponema pallidum

Treatment of Infections Caused by Treponema pallidum • Penicillin G (including benzathine penicillin) • Tetracyclines • Third Generation Cephalosporins
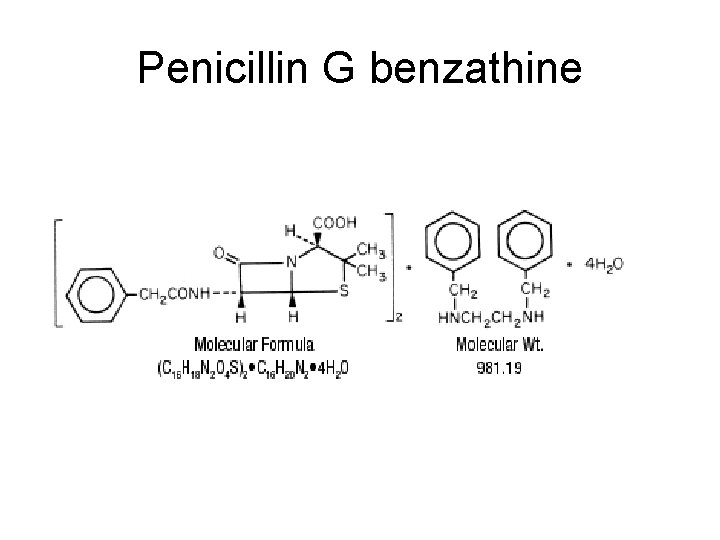
Penicillin G benzathine
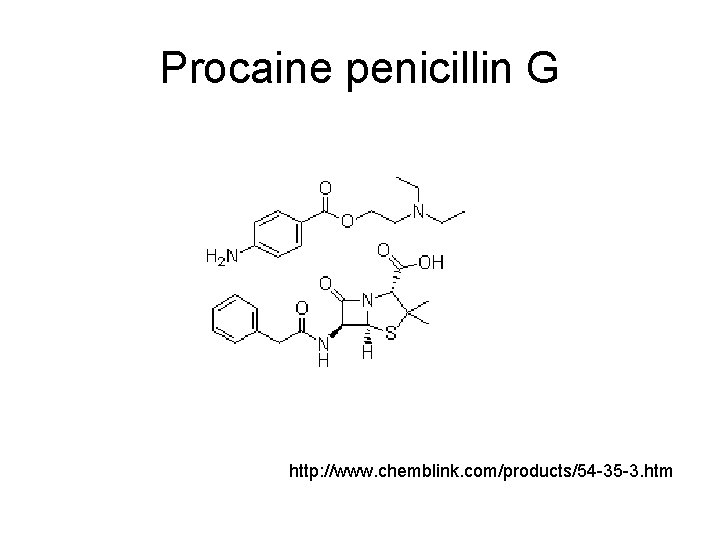
Procaine penicillin G http: //www. chemblink. com/products/54 -35 -3. htm
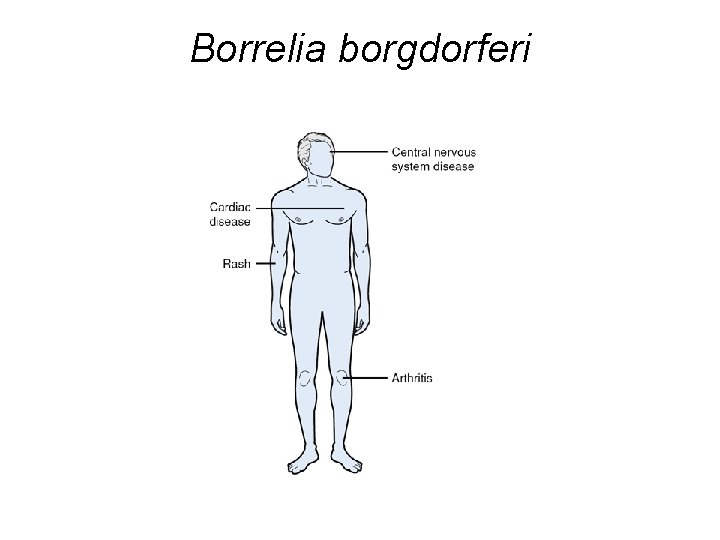
Borrelia borgdorferi
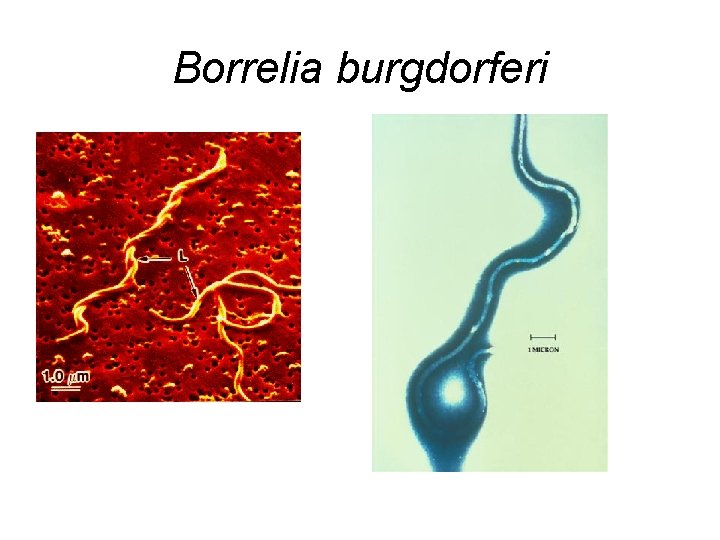
Borrelia burgdorferi

Borrelia burgdorferi is the causative agent of Lyme Disease

Treatment of Infections Caused by Borrelia burgdorferi • Tetracyclines: Doxycycline • Aminopenicillins: Amoxicillin
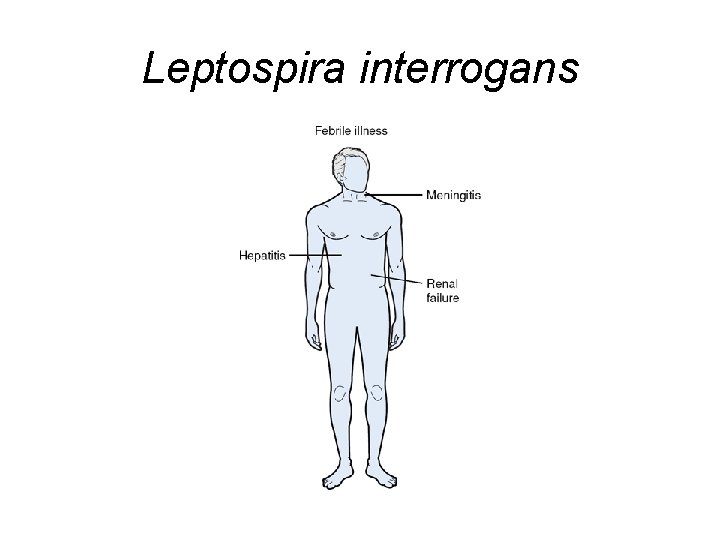
Leptospira interrogans
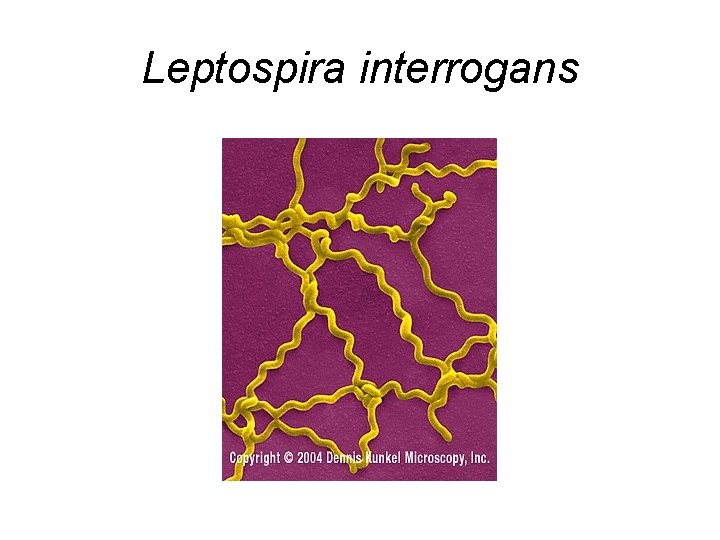
Leptospira interrogans

Treatment of Infection Caused by Leptospira interrogans • Tetracyclines: Doxycycline • Aminopenicillins: Amoxicillin • Severe Disease can be treated with Penicillin G, Ampicillin, or Ceftriaxone

Mycobacteria • Mycobacterium tuberculosis • Mycobacterium avium complex • Mycobacterium leprae
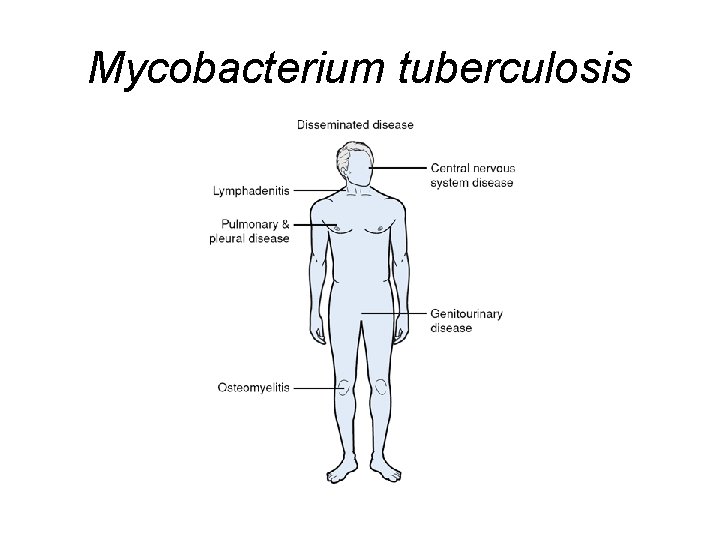
Mycobacterium tuberculosis
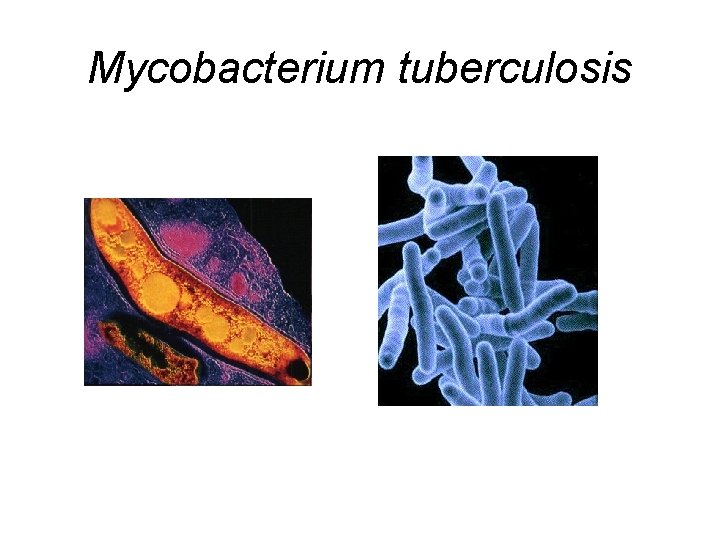
Mycobacterium tuberculosis
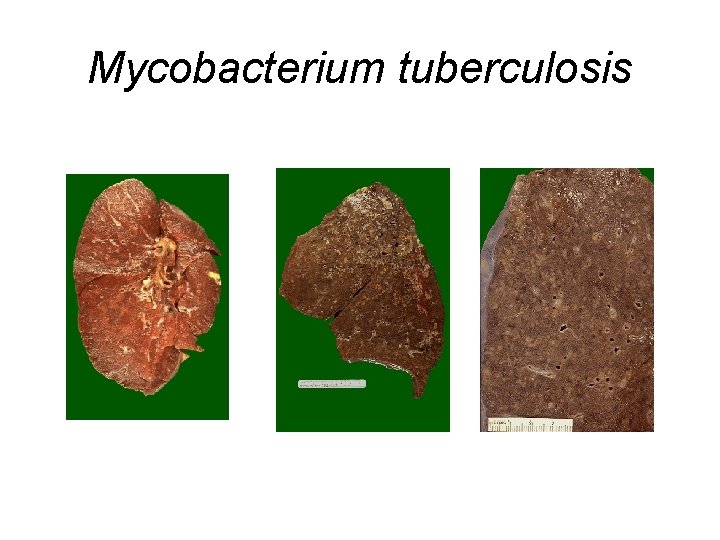
Mycobacterium tuberculosis

Treatment of Infections Caused by Mycobacterium tuberculosis • Active Disease – Isoniazid + Rifampin + Pyrazinamide + Ethambutol for two months – Followed by: Isoniazid + Rifampin for Four months • Latent Disease – Isoniazid for 9 months
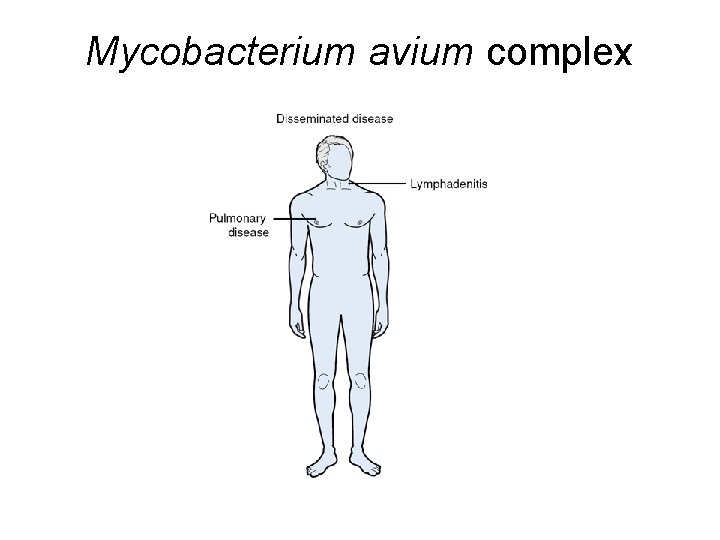
Mycobacterium avium complex
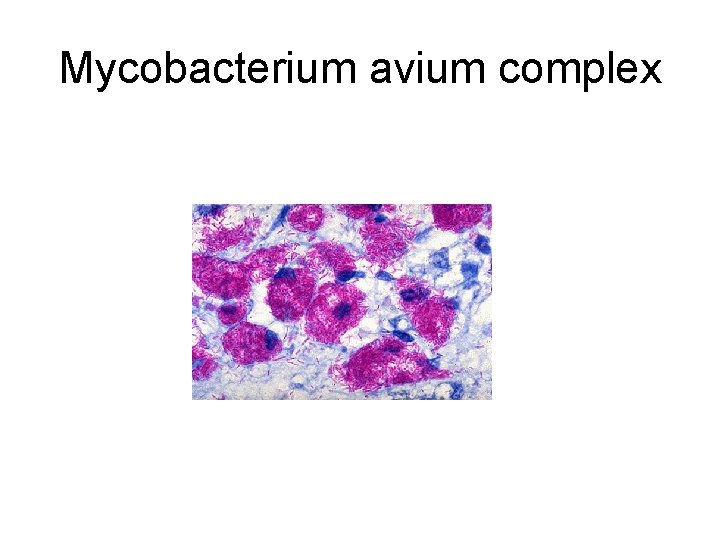
Mycobacterium avium complex

Treatment of Infections Caused by Mycobacterium avium complex (MAC) • Clarithromycin + ethambutol + rifabutin
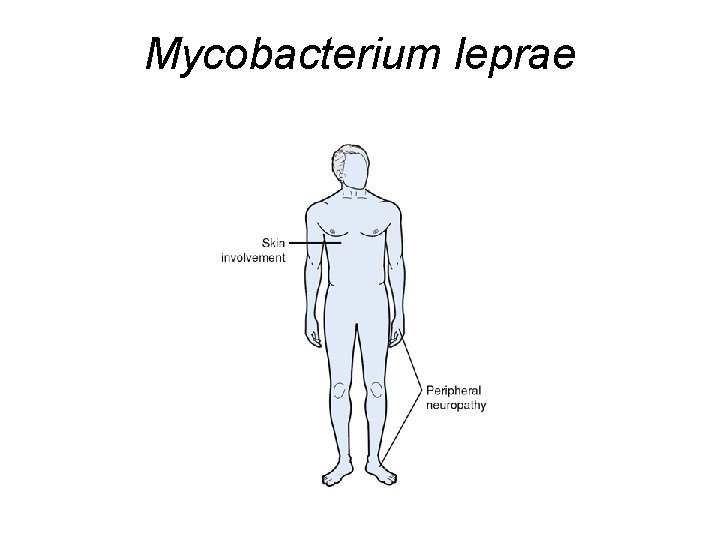
Mycobacterium leprae
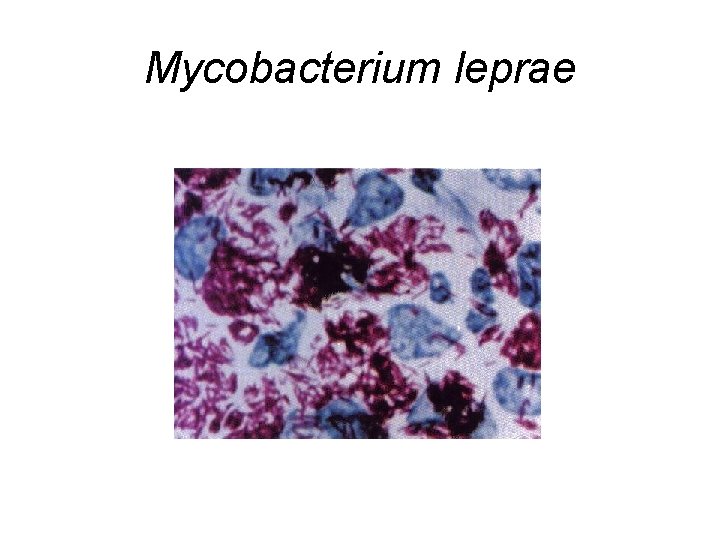
Mycobacterium leprae
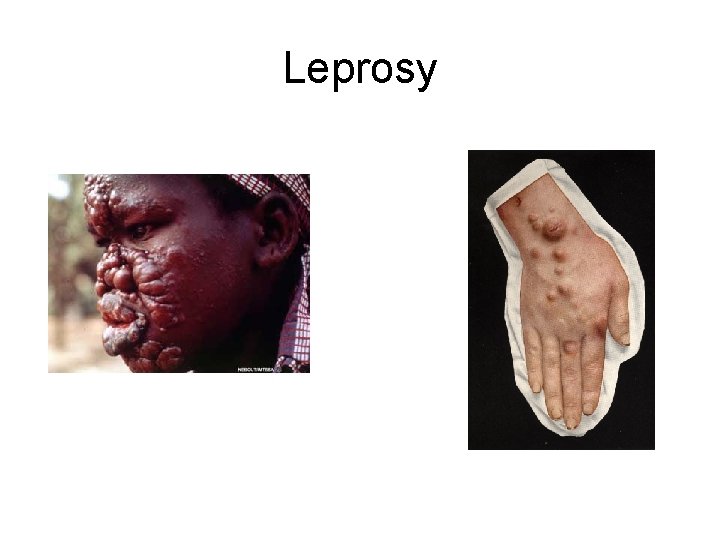
Leprosy

Treatment of Infections Caused by Mycobacterium leprae • Dapsone + rifampin + clofazimine
- Slides: 133