Dysmenorrhea Preeti Matkins MD CMC Dept of Pediatrics










































- Slides: 54

Dysmenorrhea Preeti Matkins, MD CMC Dept of Pediatrics Teen Health Connection July 2006

Suzie chief complaint of “painful periods” n n n 14 ½ year old female periods about every month soaks through pads about every 3 hours

Menstrual Disorders n n n Amenorrhea Dysfunctional Uterine Bleeding n Longer menses or shortened cycle n Heavy menstrual flow n Longer and heavier flow n Painful menses Menorrhagia Metorrhagia Menometorrhagia Dysmenorrhea

Dysmenorrhea painful menses n Primary Begin in adolescence n Not due to pelvic disease n n Secondary Uncommon in adolescence n Due to pelvic pathology n

Dysmenorrhea n Most common gynecologic condition of adolescence n n Prevalence 20 -90% Most teens do not seek medical care Use OTC n Not sure who will treat n Fear pelvic exam n

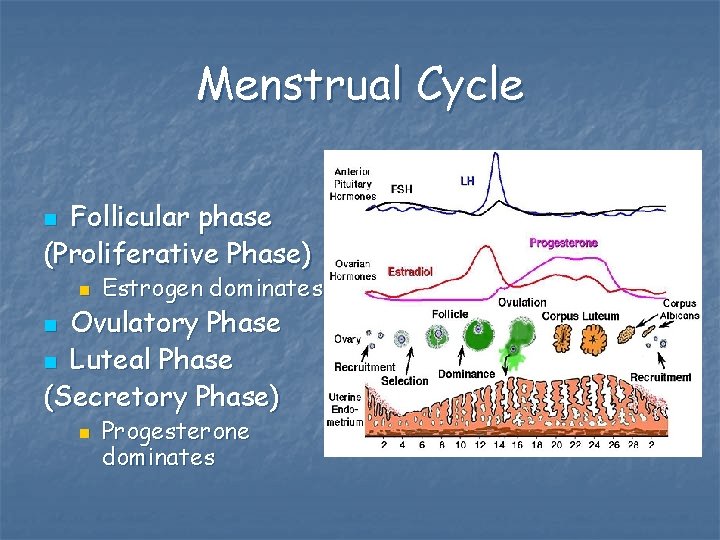
Menstrual Cycle Follicular phase (Proliferative Phase) n n Estrogen dominates Ovulatory Phase n Luteal Phase (Secretory Phase) n n Progesterone dominates

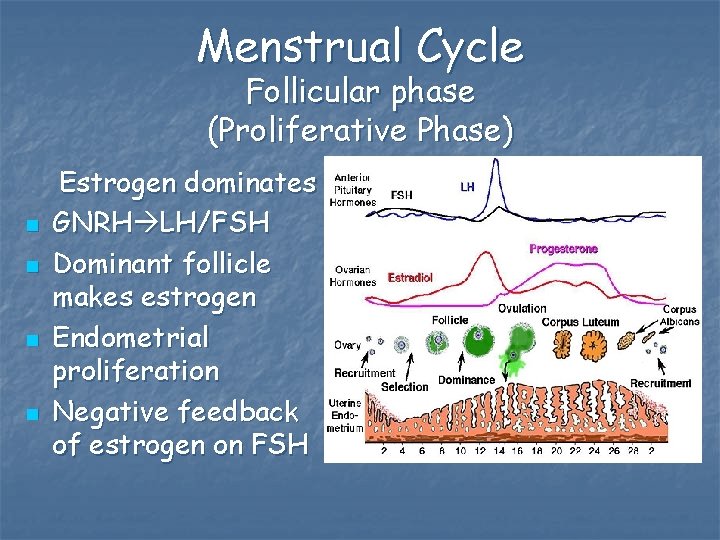
Menstrual Cycle Follicular phase (Proliferative Phase) n n Estrogen dominates GNRH LH/FSH Dominant follicle makes estrogen Endometrial proliferation Negative feedback of estrogen on FSH

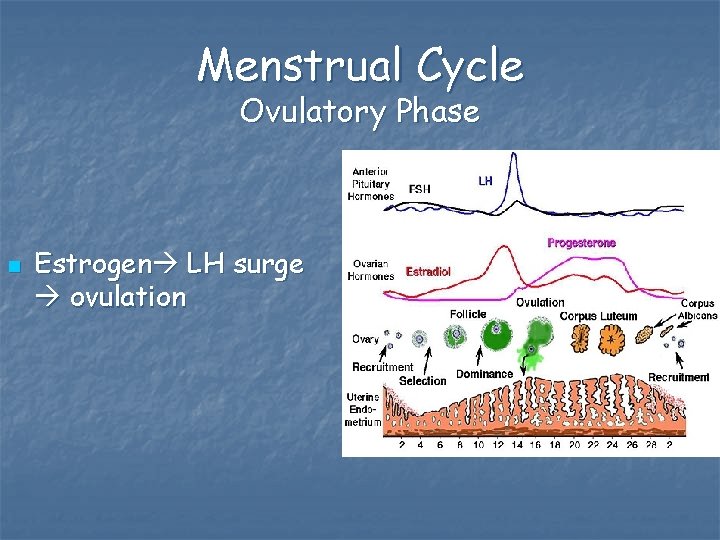
Menstrual Cycle Ovulatory Phase n Estrogen LH surge ovulation

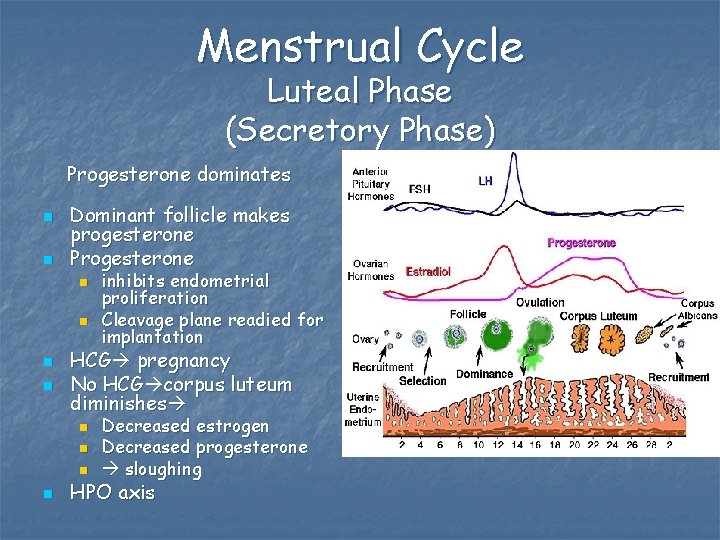
Menstrual Cycle Luteal Phase (Secretory Phase) Progesterone dominates n n Dominant follicle makes progesterone Progesterone n n HCG pregnancy No HCG corpus luteum diminishes n n inhibits endometrial proliferation Cleavage plane readied for implantation Decreased estrogen Decreased progesterone sloughing HPO axis

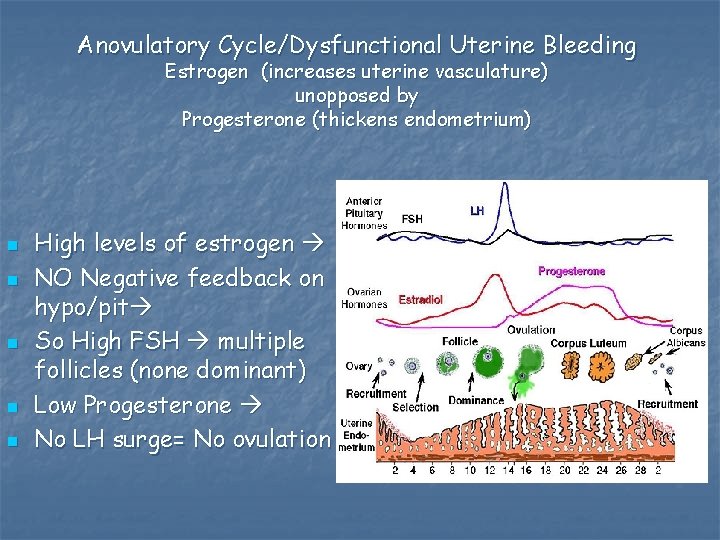
Anovulatory Cycle/Dysfunctional Uterine Bleeding Estrogen (increases uterine vasculature) unopposed by Progesterone (thickens endometrium) n n n High levels of estrogen NO Negative feedback on hypo/pit So High FSH multiple follicles (none dominant) Low Progesterone No LH surge= No ovulation

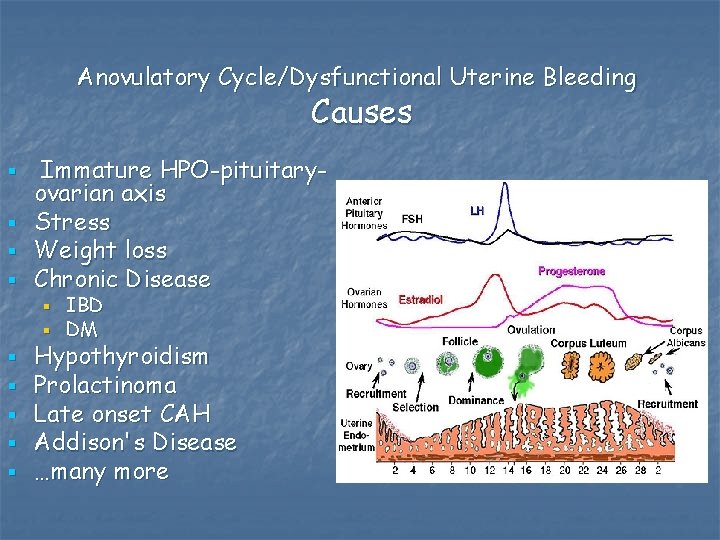
Anovulatory Cycle/Dysfunctional Uterine Bleeding Causes § § Immature HPO-pituitaryovarian axis Stress Weight loss Chronic Disease § § § § IBD DM Hypothyroidism Prolactinoma Late onset CAH Addison's Disease …many more

Anovulotory cycles How long is normal? n n 55 -80% anovulatory 2 yrs post menarche 10 -20% anovulatory up to 5 yrs post menarche “Menstrual Disorders” Braverman, Peds in Review, Vol 18, No 1 Jan 1997. Age of menarche 50% ovulatory cycles <12 12 -13 yo >13 yo 1 year 3 years 4. 5 yrs Apter; Clin End and Metab 1980

Dysmenorrhea Pathophysiology n Ovulation PG increase in cell membrane phospholipids n Release AA and Omega 7 fatty Acids n PG and LK start inflammatory cascade * uterus is more sensitive to PG in second half of cycle n n Prostaglandin n n Cyclooxygenase metabolite Myometrial hypertrophy Uterine Vasoconstriction Leukotrienes n n n Increases sensitivity of uterine pain fibers Vasoconstriction of uterus Inflammatory mediator

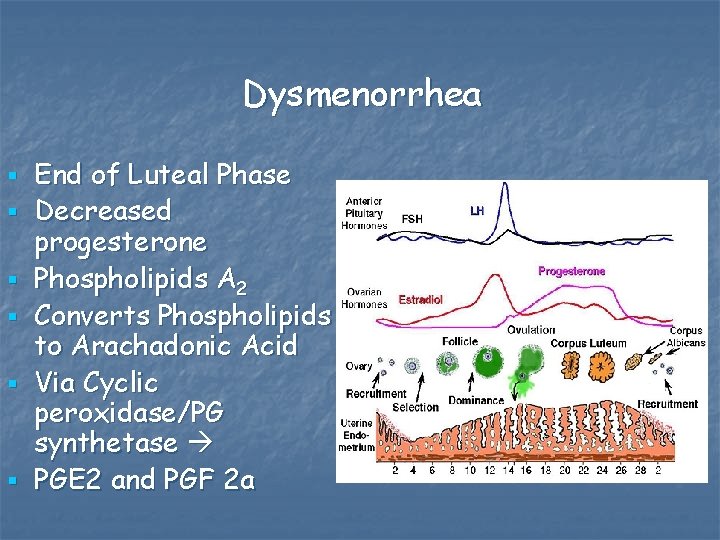
Dysmenorrhea § § § End of Luteal Phase Decreased progesterone Phospholipids A 2 Converts Phospholipids to Arachadonic Acid Via Cyclic peroxidase/PG synthetase PGE 2 and PGF 2 a

Primary Dysmenorrhea n n HPO axis takes time to mature 1/3 of females are not having ovulatory cycles until 5 yrs post menarche Must be ovulating to have dysmenorrhea May not have symptoms of dysmenorrhea until few years after menarche

2 o dysmenorrhea n n n Fibroid Endometriosis Adenomyosis

Risk factors n n n Early menarche Heavy flow Nulliparity n n Age <20 yo Family history Depression/anxiety +/- tobacco

Dysmenorrhea n Not risk factors n n n Ht Wt BMI History of abortion, uterine instrumentation, or surgery Protective? n Tobacco may decrease estrogen levels and result in anovulatory cycles (inconsistent)

Non Uterine effects of Dysmenorrhea n n Low back Pain n Referred pain from spinal nerves n PG effect on smooth muscle n Related to decreased estrogen in premenstrual stage of cycle Bloating Migraine Headaches Loose Bowel Movements n n PG mediated “PMS” n n Hormonal fluctuations in estrogen/progesterone Neurotransmitter changes

PMDD premenstrual dysmorphic disorder n DSM-IV Depressive Disorder NOS 311. 0 Symptoms last week of luteal phase n Significantly impair life/work n Absence of symptoms at least 1 wk post menses n n Incidence 3 -5% menstruating women Serafem (flouxetine) Eli Lilly 10 -20 mg/d days 14 -28

Suzie chief complaint of “painful periods” n n n Menarche age 11 ½ Loose bm and HA when her “period is coming” No family history of n n n Endometriosis Menorrhagia Bleeding disorders Infertility Breast or ovarian cancer

Differential Diagnosis n n n PID Pelvic adhesions Ovarian cysts IBD IBS Interstitial cystitis

Symptoms of 1 o dysmenorrhea n Crampy abdominal pain n n n Begin 1 -2 days prior to menses; worst first days of flow; resolve by end of menses Bloating Headaches Referred pain Nausea/emesis Breast tenderness

Symptoms of 2 o dysmenorrhea n Begin several days to 2 w before flow n Persist throughout flow

Exam n n Mild mid abdominal pain No rebound No CMT or AT Mass n Consider uterine outlet obstruction n n severe pain early after menarche Other tumors

Pelvic exam n Not always necessary n Sexual history n STD, PID, AT, CMT Vaginal discharge n Non menstrual uterine pain n n Do need external genital exam n Imperforate hymen

Suzie chief complaint of “painful periods” n n A/B honor roll Misses 1 -2 days of school /mo Sits out cross country practice Confidential Interview Has boyfriend of 2 months n No sexual contact n

Other conditions to consider (Common is Common) n n n n n Irritable Bowel Syndrome IBD GER Gastritis Didelphic uterus Vaginal septum Cervical agenesis Cervical stenosis Uterine septum

Evaluation n Get a history first! n n Symptom Calendar Hemoglobin n Menorrhagia n n Bleeding disorder- von Willebrands Disease IBD Consider Hemoccult Consider bimanual exam or ultrasound if initial tx does not alleviate symptoms

Suzie chief complaint of “painful periods” n n Hemoglobin 11. 5 Medications Tylenol n Midol n n n periods about every month soaks through pads about every 3 hours

Treatment n n NSAIDS Other OTC n n OCP n n Used by 30 -70% of adolescents Extended cycling Other hormonal therapies Non medical treatments CAM

Treatment NSAIDS (cyclooxygenase inhibitors) n n Inhibit prostaglandin synthesis Decrease volume of menses n n May also decrease diarrhea, nausea Most effective If started before pain and menstrual flow n Do not need to continue through flow n

Treatment NSAIDS (cyclooxygenase inhibitors) n n n All NSAIDS and aspirin more effective than acetomenophen n Ibuprofen n Naproxen n FYI: COX-2 similar to NSAIDS; no better Appropriate Dose n 400 -800 mg every 8 hours 1 -2 before flow to 1 -2 d into flow n *Consider GI (and other) side effects Cochrane Review: NSAIDS are effective treatment

OTC Analgesics Marketed for Dysmenorrhea Multicomponent Formulations Midol (Bayer Healthcare LLC) n n n “Menstrual Complete” n 500 mg acetaminophen, 60 mg caffeine, 15 mg pyrilamine (antihistamine) “Premenstrual Syndrome” n 500 mg acetaminophen, 25 mg pamabrom(diuretic), 15 mg pyrilamine “Teen Formula” n 500 mg acetaminophen, 25 mg pamabrom Hilliard, P. , ”Dysmenorrhea”, Peds in Review, Vol 27, No 2 Feb 2006

OTC Analgesics Marketed for Dysmenorrhea Multicomponent Formulations Midol (Bayer Healthcare LLC) n n “Cramps and body aches” n ibuprofen 200 mg “Maximum strength extended relief” n naproxen sodium 200 mg (approved by FDA) Hilliard, P. , ”Dysmenorrhea”, Peds in Review, Vol 27, No 2 Feb 2006

OTC Analgesics Marketed for Dysmenorrhea Multicomponent Formulations Pamprin (Chattem, Inc) n “Multi-symptom” n n “All Day” n n 500 mg acetaminophen, 25 mg pamabrom, 25 mg pyrilamine similar to Midol Premenstrual except 15 mg pyrilamine pamabrom is a diuretic 220 mg naproxen sodium “Cramp” 250 mg acetaminophen, 250 mg magnesium salicylate, 25 mg pamabrom n Hilliard, P. , ”Dysmenorrhea”, Peds in Review, Vol 27, No 2 Feb 2006

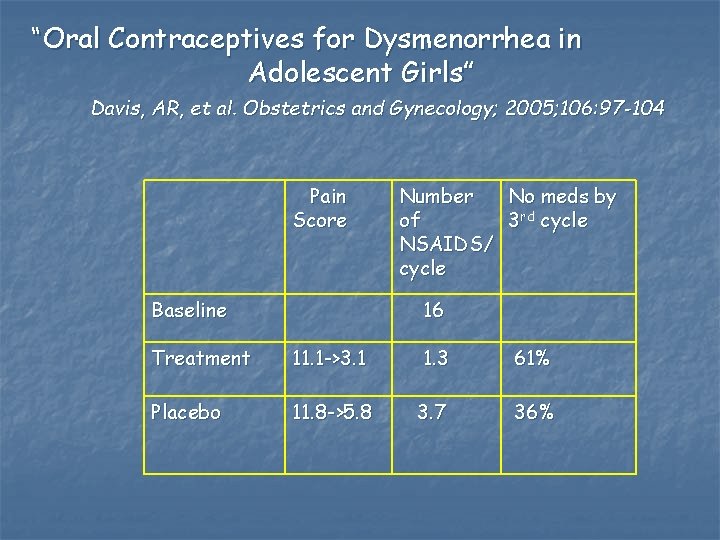
“Oral Contraceptives for Dysmenorrhea in Adolescent Girls” Davis, AR, et al. Obstetrics and Gynecology; 2005; 106: 97 -104 n n n n= 76; <19 yo Screen for depression, stress Randomized to low dose (20 mcg estrogen) OCP or placebo Could take other OTC meds Moos Menstrual Distress Scale Phone f/u monthly x 2; then exit interview month 3 Baseline : severe pain 58%; 55% nausea, 39% missed activites

Moos Menstrual Distress Scale n n n Designed 1968 6 point Likert Scale Cycle n n menstrual, premenstrual, intermenstrual Symptoms n n n Pain Concentration Behavior changes Autonomic reactions Water retention Control

“Oral Contraceptives for Dysmenorrhea in Adolescent Girls” Davis, AR, et al. Obstetrics and Gynecology; 2005; 106: 97 -104 Pain Score Baseline Number No meds by of 3 rd cycle NSAIDS/ cycle 16 Treatment 11. 1 ->3. 1 1. 3 61% Placebo 11. 8 ->5. 8 3. 7 36%

Treatment Oral Contraceptive Pills n Inhibit ovulation Decreased progesterone less PG n Less menstrual flow n n Cochrane rates as effective n n No evidence low dose vs 30 or 35 mcg estrogen pills Pelvic exam not always required

Treatment Oral Contraceptive Pills n n Use Monophasic estrogen containing pills Lower estrogens n n spotting less efficacious as contraception if n n n >155 pounds Miss pills 30 mcg 35 mcg Some studies used 50+ mcg estrogen/pill n Nausea!

Treatment n n n Depo-Provera Extended cycling OCP Mirena

Treatment n Extended Cycling Oral Contraceptives n n n Reduced flow Less frequent flow Seasonale Can use any monophasic OCP Other benefits

Treatment Other Hormonal n Contraceptive Patch: Ortho Evra n n Less effective than oral OCP for dysmenorrhea Intravaginal OCP

Treatment Leukotriene Recepetor Antagonists Will Singulair decrease PG and relieve symptoms? * n n= 22 adolescents completed n n n mean age 16 4 + 1 year post menarche RDB crossover n n n 13 got 10 mg Singulair days 21 to end of cycle x 2 cycles; then 2 month placebo other group had reverse order 3 drop-outs: noncompliance, other disease dx “The Use of the Leukotriene Antagonist Montelukast (Singulair)in the Management of Dysmenorrhea in Adolescents” Harel, et al. J of Pediatric and Adolescent Gynecology, 2004; 17: 183 -186. * Funded by Merck

Treatment Leukotriene Receptor Antagonists Will Singulair decrease PG and relieve symptoms? * Cox Menstrual Scale n No difference in pain scores with use of Singulair for dysmenorrhea n “The Use of the Leukotriene Antagonist Montelukast (Singulair)in the Management of Dysmenorrhea in Adolescents” Harel, et al. J of Pediatric and Adolescent Gynecology, 2004; 17: 183 -186. * Funded by Merck

Treatment Depo-Provera n n n Most patients amenorrheic by 9 months May have irregular bleeding 3 -6 months Bone effects n May recover

Treatment Suppression of Menses n n n Danazol (Danocrine) Leuprolide acetate (Lupron) Expensive Significant Side effect Generally not for Primary dysmenorrhea

Treatment Other Modalities n Supplements RCT showed pain reduction compared to placebo Thiamine 100 mg daily n Fish Oil n Vitamin E n n Herbal remedies Insufficient data

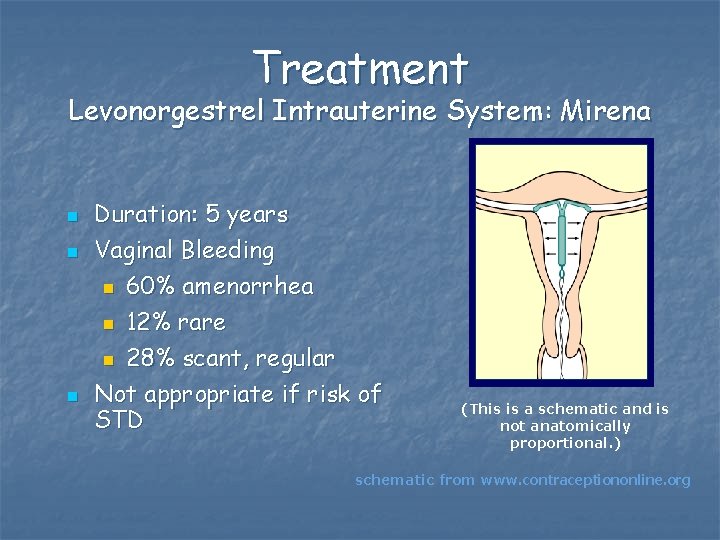
Treatment Levonorgestrel Intrauterine System: Mirena n n n Duration: 5 years Vaginal Bleeding n 60% amenorrhea n 12% rare n 28% scant, regular Not appropriate if risk of STD (This is a schematic and is not anatomically proportional. ) schematic from www. contraceptiononline. org

Treatment Other Modalities n n Exercise Heat Relaxation/Yoga Acupuncture and Acupressure n n TENS (Transcutaneous electric nerve stimulation) n n Some randomized controlled studies show reduction in pain Insufficient evidence Spinal manipulation n No evidence to support

Suzie Primary Dysmenorrhea n NSAIDS n n Menstrual Symptom Diary n n 400 -600 mg ibuprofen 1 d prior to menses If continues symptoms, consider OCP Multivitamin with iron

Dysmenorrhea When to Refer to Gynecologist n Persists on appropriate dose medications n n n NSAIDS OCP STD ? (remember Urine PCR) n Severe symptoms with 1 o relative with endometriosis n Exam concerning for endometriosis n n n Posterior uterus pain Cul de sac pain Significant disability

Selected Bibliography n n n Braverman, PK, “Menstrual Disorders” Pediatrics in Review, Vol 18, No 1, Jan 1997, 17 -26. Rimsza, M. “Dysfunctional Uterine Bleeding” Pediatrics in Review, Vol 23, No 7, July 2002, 227 -233. French, L. “Dysmenorrhea” American Family Physician 2005; V 71: No 2 285 -291 Hilliard, P. , ”Dysmenorrhea”, Pediatrics in Review, Vol 27, No 2 Feb 2006 Davis, AR “Primary Dysmenorrhea in Adolescent Girls and treatment with Oral Contraceptives” J Pediatrics and Adolescent Gynecology, 2001 Vol 14 3 -8. n n n Apter “Anovulatroy Cycles” Clinical Endo and Metabolism 1980 “Oral Contraceptives for Dysmenorrhea in Adolescent Girls” Davis, AR, et al. Obstetrics and Gynecology; 2005; 106: 97 -104 “The Use of the Leukotriene Antagonist Montelukast (Singulair) in the Management of Dysmenorrhea in Adolescents” Harel, et al. J of Pediatric and Adolescent Gynecology, 2004; 17: 183 -186. Moos, R. The Development of a Menstrual Distress Questionnaire Psychosomatic Medicine 30: 853 -867 (1968) DSM IV –R American Psychiatric Association Pediatric and Adolescent Gynecology, Emans, Laufer, Goldstein, ed. Lippincot-Raven, 2004