Assessment and Management of Urinary Incontinence in the
































- Slides: 44


Assessment and Management of Urinary Incontinence in the Clinic Kathryn L. Burgio, Ph. D Associate Director for GRECC Research & Patricia S. Goode, MD Associate Director for GRECC Clinical Programs Birmingham/Atlanta Geriatric Research Education and Clinical Center – July 27, 2006

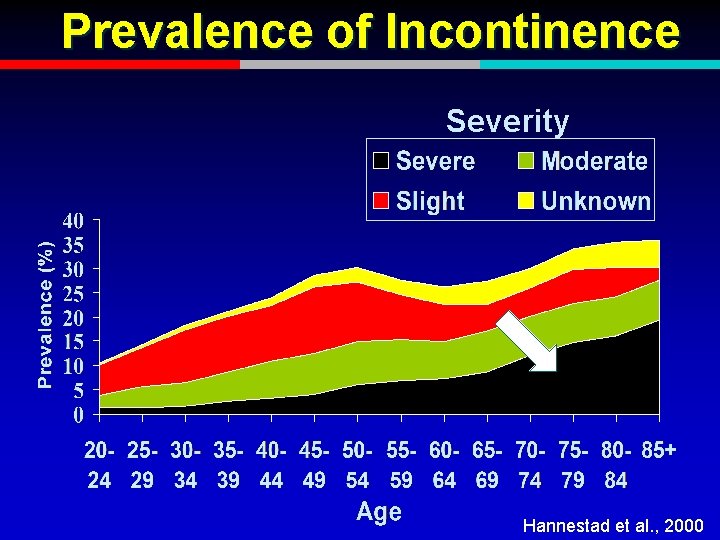
Prevalence of Incontinence Severity Hannestad et al. , 2000

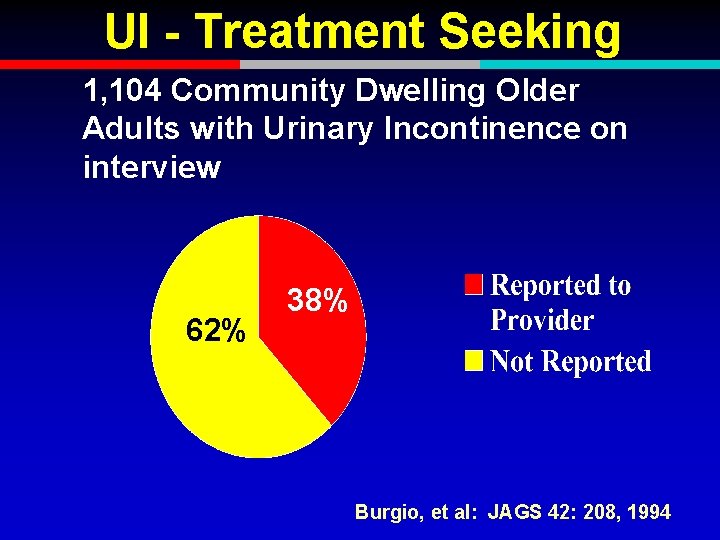
UI - Treatment Seeking 1, 104 Community Dwelling Older Adults with Urinary Incontinence on interview 62% 38% Burgio, et al: JAGS 42: 208, 1994

Reasons for Not Reporting Incontinence to Provider u. Not aware that can be treated u. Normal part of aging u. Personal problem (not medical) u. Embarrassed u. Fear of nursing home placement u. Afraid treatment requires surgery

Include Incontinence in the Review of Systems for all geriatric patients.

Patient Case u 75 year old man u Goes to the bathroom every 1 -2 hours daytime and 3 times at night. u About once a week, on the way to the bathroom, he can’t make it and wets his clothes. Evaluation? Diagnosis? Appropriate treatment?

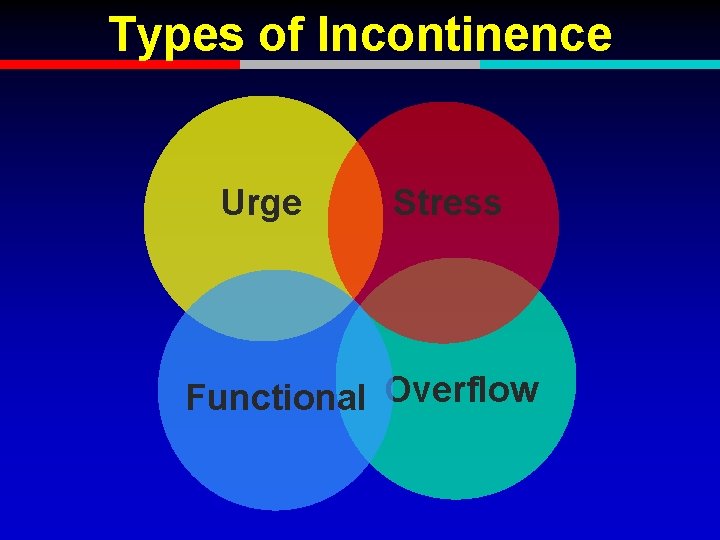
Types of Incontinence Urge Stress Functional Overflow

Work-up of Incontinence u. History u. Physical u. Urinalysis u. Post-void Volume Residual

Incontinence History Type u Do you leak urine during physical activity such as coughing, sneezing, lifting, or exercising? u Do you get the urge to go and can’t make it without leaking? Onset Severity u Frequency of leakage u Need for absorbent products

Incontinence History u. Lower urinary tract symptoms u. Urgency, frequency, nocturia, dysuria, weak stream, straining to void, etc. u. Fluid intake – volume and type u. Previous treatments and effects on incontinence

Medical History u Medical, neurological, history u Surgical history u Prostatectomy u Review u Habits medications including OTC (caffeine, tobacco, alcohol use)

Physical Exam u. Brief Neurologic Exam u. Gait u. Lower extremity strength u. Cogwheel rigidity u. Sphincter tone and voluntary contraction u. Rectal (and Pelvic for women)

Urinalysis u Bacteriuria u Pyuria u Glycosuria u Hematuria

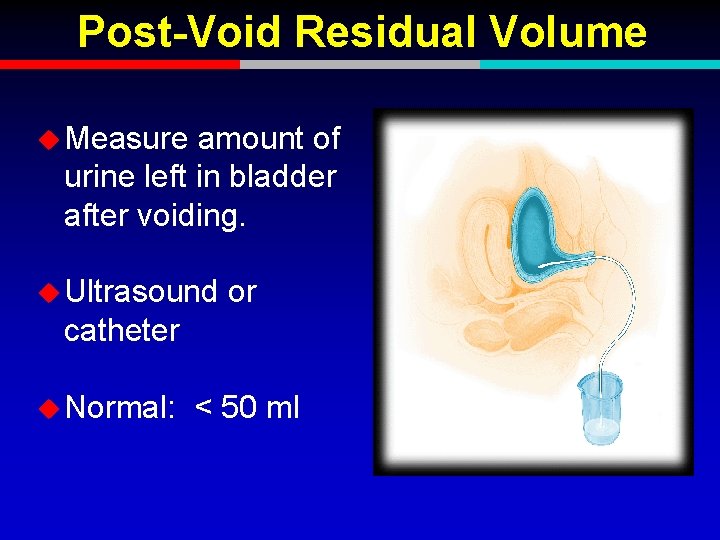
Post-Void Residual Volume u Measure amount of urine left in bladder after voiding. u Ultrasound or catheter u Normal: < 50 ml

Patient Case u 75 year old man u Frequent voiding and weekly urge incontinence u Work up u Hx: Diabetes for 10 years, tries to adhere to diet – drinks about 4 -5 diet sodas/day. Insomnia – takes Tylenol PM. Constipation. u Physical: hard stool in vault u UA: 2+ glucose (and Hgb A 1 C = 9. 8 one month ago) u PVR: 200 m. L u Diagnosis? u Treatment Options?

Contributors to UI to Treat First Drugs and Diet Infection Atrophic Urethritis Psychological - Depression, Delirium Endocrine - Diabetes, Hypercalcemia Restricted Mobility Stool Impaction

Contributors to UI to Treat First Drugs Sedatives including alcohol ACE inhibitors (cough) Antipsychotics (pseudoparkinsonism) Diuretics (bad timing) Alpha Blockers – worsen stress UI Anticholinergics – incomplete emptying

Contributors to UI to Treat First Drugs and Diet – Caffeine & Fluids Infection Atrophic Urethritis Psychological - Depression, Delirium Endocrine - Diabetes, Hypercalcemia Restricted Mobility Stool Impaction

Patient Case u 75 year old man u Frequent voiding and weekly urge incontinence u Work up u Hx: Diabetes for 10 years, tries to adhere to diet – drinks about 4 -5 diet sodas/day. Insomnia – takes Tylenol PM. Constipation. u Physical: hard stool in vault u UA: 2+ glucose (and Hgb A 1 C = 9. 8 one month ago) u PVR: 200 m. L

Patient Case u 75 year old man u Frequent voiding and weekly urge incontinence u Work up u. Hx: Otherwise negative u. Physical: unremarkable u. UA: normal u. PVR: 45 m. L u Diagnosis? u Treatment options?

First Line Treatments u Medications u Anticholinergics u. Oxybutynin – generic, Ditropan XL, Oxytrol patch u. Tolterodine - Detrol u. Solifenacin - VESIcare u. Trospium - Sanctura u. Darifenacin - Enablex u Alpha blocker for BPH u Other treatments u Behavioral training – try BEFORE or with drug

Least Invasive – Use First !! Diet & Fluid Management Behavioral Strategies PFM Training and Exercise Behavioral Approaches Bladder Training Biofeedback Weight Loss Bladder Diaries

Behavioral Treatment: Multi-component Program u. Pelvic floor muscle training u. Home practice of exercises u. Increase duration of contraction/relaxation over time u. Bladder Control Techniques u. Self-Monitoring w/ bladder diaries

When the Urge Strikes – Freeze and Squeeze u. Stop and stay still u. Squeeze u. Relax pelvic floor muscles rest of body u. Concentrate on suppressing urge u. Wait until the urge subsides u. Walk to bathroom at normal pace Burgio et al. Staying Dry: A Practical Guide to Bladder Control. 1989.

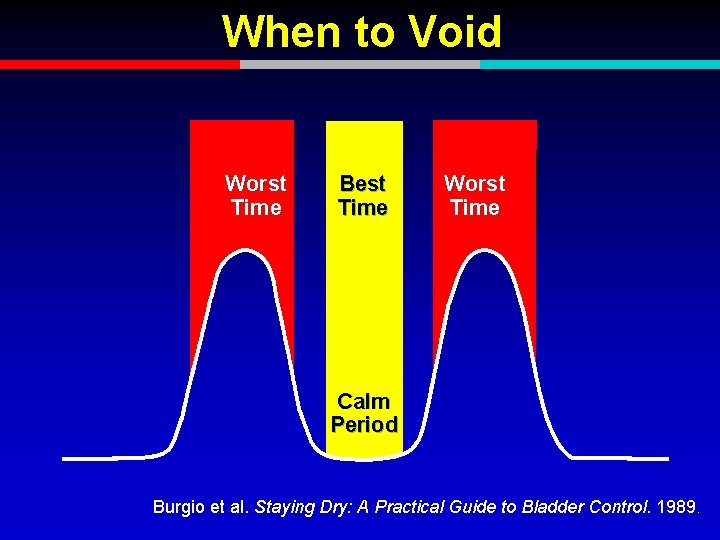
When to Void Worst Time Best Time Worst Time Calm Period Burgio et al. Staying Dry: A Practical Guide to Bladder Control. 1989.

Other Behavioral Strategies u Stress Strategy Squeeze before you sneeze (or cough or lift) u u Post Void Dribbling Strategy u Squeeze after voiding

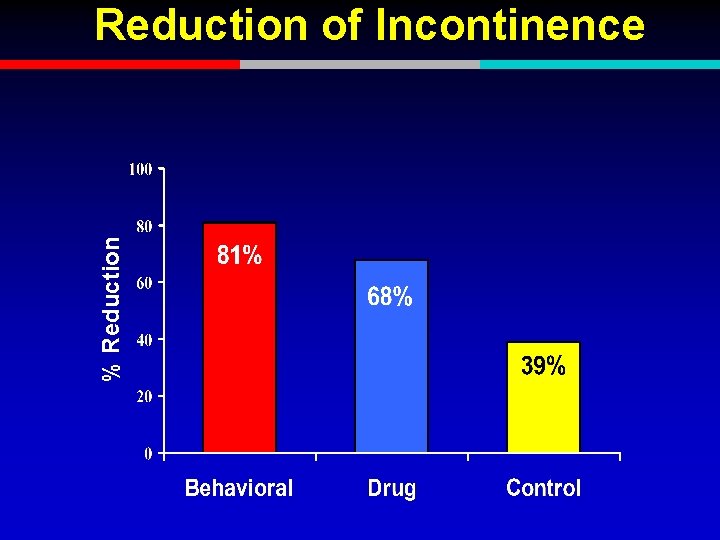
RCT Comparing Behavior and Drug Therapy 197 older women with urge incontinence u Randomized to 8 weeks of: u Behavioral training (biofeedback) u Drug therapy (oxybutynin) u Placebo control u Burgio et al, JAMA, 1998

% Reduction of Incontinence

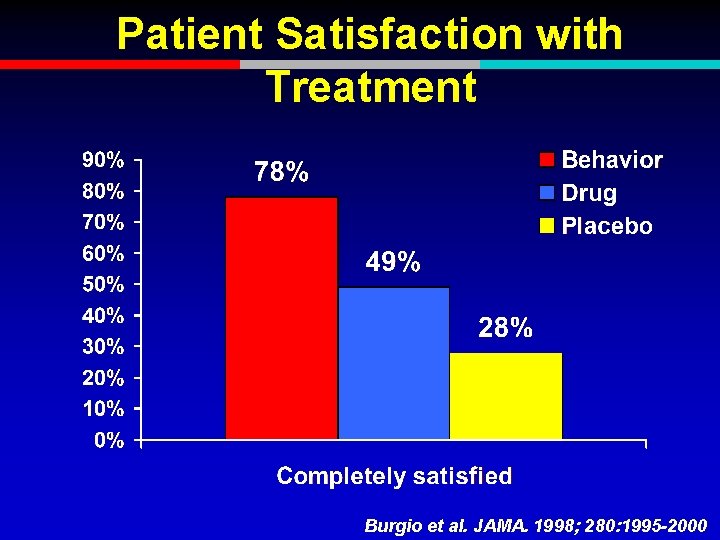
Patient Satisfaction with Treatment Burgio et al. JAMA. 1998; 280: 1995 -2000

Patient Case u 85 year old woman u Frequently leaks on the way to the bathroom u Work up u Hx: Aricept for dementia u Physical: Frail, walks slowly, uses a walker u UA: normal u PVR: 85 m. L u Diagnosis? u Treatment Options?

The Patient with Functional Limitations u. Avoid anticholinergic drugs in pts with dementia u. Facilitate functional status u. Mobility devices u. Physical therapy u. Bedside commode u. Urinal for men u. Prompted voiding – VERY effective

Post-Prostatectomy Incontinence u 65 yo had radical prostatectomy 1 year ago u Leaks when he coughs, sneezes or lifts something heavy u Wears a pad in the daytime, dry at night u No problem making it to the bathroom u Diagnosis? u Treatment Options?

Behavioral Treatment of Post. Prostatectomy Incontinence u 20 men; 55 -87 years old u. Average 2 ½ years since surgery u 8 weeks of biofeedback-assisted behavioral training u 78. 3% decrease in accidents (range of -12 – 100%) Burgio, et. al. , J Urology, 1989

Behavioral Training for Post. Prostatectomy Incontinence u u u Case Series of 27 men with persistent post-prostatectomy UI Taught pelvic floor muscle exercises without using biofeedback 56. 6% reduction in leakage Meaglia et al. J Urol. 1990; 144: 674

Post-Prostatectomy Incontinence u u 65 yo considering radical prostatectomy Continent Read that 72% of patients reported incontinence persisting 1 year after surgery and 40% wearing pads What can he do to help prevent incontinence? Stanford, et. al. JAMA, 2000

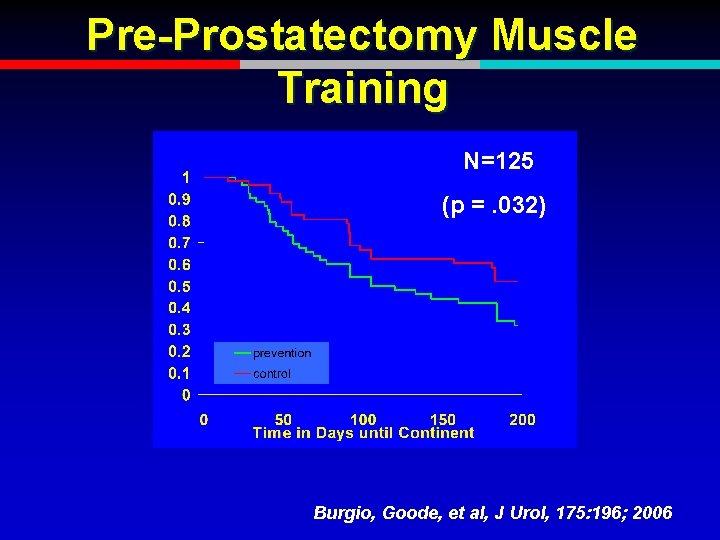
Pre-Prostatectomy Muscle Training N=125 (p =. 032) Burgio, Goode, et al, J Urol, 175: 196; 2006

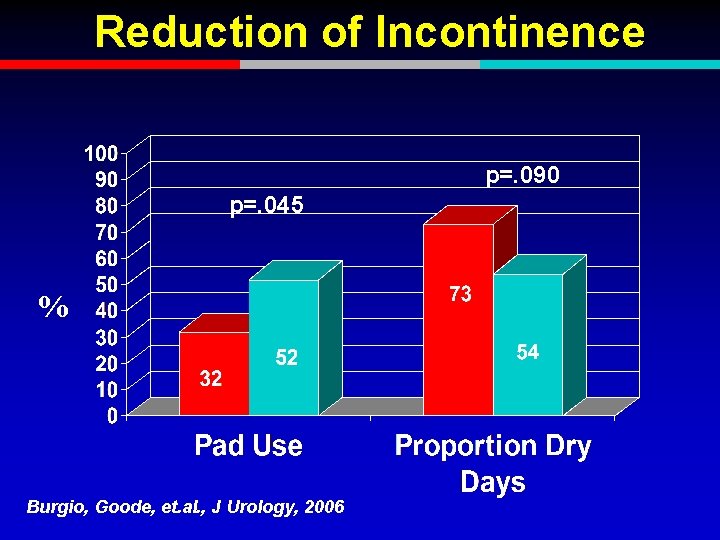
Reduction of Incontinence p=. 090 p=. 045 % Burgio, Goode, et. al. , J Urology, 2006

Pre-Prostatectomy Muscle Training u Median Time to Continence: u. Intervention Group - 3. 5 months u. Control Group - > 6 month u Number Needed to Treat to get 1 additional man out of pads at 6 months = 5 Burgio, Goode, et al, J Urol, 175: 196; 2006

Summary - Work-up of Incontinence u. History u. Physical u. Urinalysis u. Post-void Volume Residual

Summary: Contributors to Incontinence to Treat First Drugs and Diet Infection Atrophic Urethritis Psychological - Depression, Delirium Endocrine - Diabetes, Hypercalcemia Restricted Mobility Stool Impaction

Urinary Incontinence Treatments u Behavioral Treatments u Pelvic Floor Muscle Exercises (Kegel) u Bladder training u Timed/Prompted voiding u Bladder Control Techniques u Biofeedback u Medications u Pessary u Pelvic Floor Electrical Stimulation u Magnetic u Urethral u Surgery Chair Bulking Agents

Current Studies at Bham/ATL GRECC u MOTIVE - Combined medication and behavioral therapy for overactive bladder in men (VA Rehab R&D) u Pros. Tech – Behavioral therapy with and without biofeedback and electrical stimulation for persistent incontinence in men after radical prostatectomy (NIH) u COMBO - Combined medication and behavioral therapy for urge incontinence in women (VA Rehab R&D) u ATLAS – Behavioral therapy or pessary or combined for stress incontinence in women (NIH) u RUBI - Botox injections for refractory urge incontinence in women (NIH)

Contact Information u u Patricia Goode, MD pgoode@aging. uab. edu 205 -934 -3249 Kathryn Burgio, Ph. D kburgio@aging. uab. edu 205 -558 -7067 Ken Shay, DDS, MS kenneth. shay@va. gov 734 -222 -4325 http: //vaww. sites. lrn. va. gov/vacatalog/cu_detail. asp? id=2 2318