DYSFUNCTIONAL VOIDING PATTERNS URINARY INCONTINENCE URINARY RETENTION BPH

DYSFUNCTIONAL VOIDING PATTERNS URINARY INCONTINENCE URINARY RETENTION BPH RAHAYU SETYOWATI Degree of Nursing, Padjadjaran University, INDONESIA 1

OBJECTIVE At the end of this session, student should be able to: 1. Understand explain of the definition of urinary incontinence and urinary retention 2. Understand explain of the pathophisiology of urinary incontinence and urinary retention 3. Understand explain of the risk factor of urinary incontinence and urinary retention 4. Understand explain of the clinical manifestation of urinary retention and urinary incontinence 5. Understand explain of the complication of urinary incontinence and urinary retention 6. Understand explain of the diagnostic test of urinary incontinence and urinary retention 7. Understand explain of the medical management of urinary reten tion and urinary incontinence 8. Understand explain of the nursing process of urinary retention 2 and urinary incontinence

URINARY INCONTINENCE 3

DEFINITION Urinary incontinence is the unplanned loss of urine that is suficient to be considered a problem. Smeltzer, SC & Bare, B(2004) PATHOPHYSIOLOGY Continence is maintained via a complex communication system of suprasacral, sacral and local nerve-mediated loops of information. Any break in these loops of communication cause some degree of urinary dysfungtion. 4
Conditions causing adulth voiding dysfungtion Neurologic Disorders • Cerebellar ataxia incontinence • Cerebrovascular accident retention or incontinence • Dementia incontinence • Diabetes incontinence and/or incomplete bledder empty • Multiple sclerosis incontinence or incomplete bledder empty • Parkinson’s Disease incontinence Spinal cord dysfungtion • acut injury urinary retention • degenerative disease incontinence and/or incomplete bledder empty Nonneurologic disorders • bashful bladder inability to initiate voiding in public bathroom • overactive bladder urgency, urge and frequency incontinence • post-prostatectomy incontinence • post general surgery acut urine retention • stress incontinence with cough, position change 5

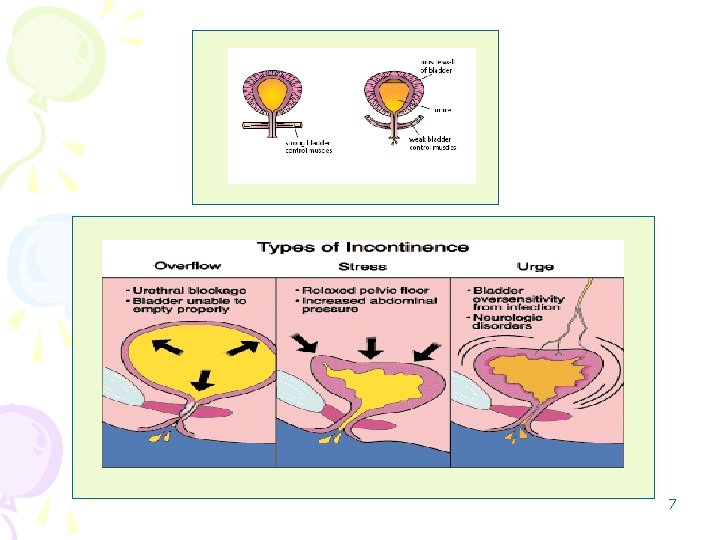
TYPES OF URINARY INCONTINENCE Stress Loss of urine associated with increased intra-abdominal pressure during sneezing, coughing. Quantity of urine lost is usually small. Urge Involuntari loss of urine associated with a strong urge to void Overflow Inability to empty bladder, resulting in overdistention and frequent loss of small amount of urine Incontinence resulting from Fungtional phisical, environmental, or psyco-social causes • Multiple pregnancies • Decreades estrogen level • Prostate surgery • Tumor, asites, obesity • Neurologic disorders • Detrusor muscle overactivity (bladder obstruction, aging, diabetes) • Spinal cord injury below S 2 • Diabetic neuropathy • Prostatic hypertropy • Fecal impaction • Confusion or dementia • Physical disability • Diuretic terapy or sedation 6 • depression
7

DIAGNOSTIC TESTS Urinalysis and urine culture v Post voiding residual volume (PVR) v Cystometrography v Uroflowmetry v Intravenous Pyelography v Ultrasounography v 8

MEDICAL MANAGEMENT Surgery Medications Stress and urge incontinence may improve with drug. Postmenopausal incontinence, estrogen therapy may effective. Urge incontinence may be treated with preparations that increase bladder capacity. Surgery may be used to treat stress incontinence associated with cystocele or urethrocele and oferflow incontinence associated with an enlarged prostate gland. Other surgical procedures of potential benefit in the treatment of incontionence include implanation of the artificial sphincter, formation of the uretral sling, augmentation of the bladder with bowel. 9

NURSING PROCESS q Assessment Health history : - voiding diary - frequency of incontinent episodes - amount of urine loss - activities associated with incontonence - use of Kegel exercise or medication - chronic disease releated surgeries Physical examination : - physical limitation or impaired cognition - bladder distention (inspect, palpate, percuss) - inspect perineal tisue for redness, irritation, tissue breakdown 10

Cont…nursing process q Nursing Diagnoses 1. Urinary Incontinence : Stress and/or Urge 2. Self-care deficit : toileting 3. Social Isolation 11

1. Urinary incontinence : stress and or urge Intervention : - instruct to keep voiding diary (voiding diaries provide valuable information for identifying the type of incontinence) - teach pelvic floor muscle exercise - suggest dietary and fluid intake modifications to reduce incontinence. Limiting caffeine, alcohol, citrus juice, limited fluid intake to n less than 1, 5 – 2, 0 L per day, limited evening fluid. 12

Pelvic Floor (Kegel) Exercise • Identify the pelvic muscles with these : - stop the flow of urine during voiding and hold for a few second - tighten the muscles at the vaginal entrance around a gloved finger or tampon - tighten the muscle around the anus as through resisting defecation • Perform exercise by tightening pelvic muscles, holding for 10 second, and relaxing for 10 – 15 second. Continue the sequence (tighten, hold, relax) for 10 repetitions • Keep abdominal muscles and brething relaxed while performing exercises • Initially, exercise should be performing twice per day, working up to four times per day 13

2. Self care deficit : toileting intervention : - ass physical and mental abilities and limitations - provide assistive devices as a needed - plan to toileting schedule - position for ease of voiding - adjust fluid intake - assist with clothing that is easily removed 14

URINARY RETENTION 15

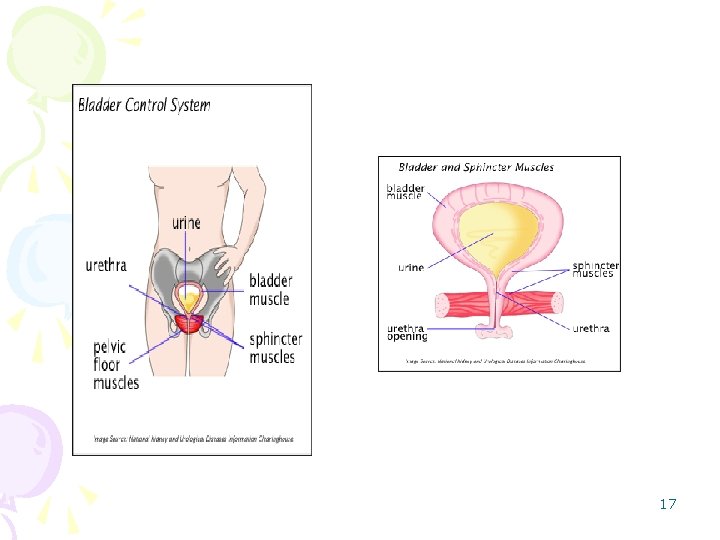
DEFINITION Incomplete emptying of the bladder, can lead to overdistention of the bladder, poor detrusor muscle contractility, and unability to urinate. Lemone, P & Burke, K(2004) PHYSIOLOGY REVIEW Bladder emptying is controlled by the interaction of muscle tone and the autonomic nervous system. The sympatetic nervous syetem relaxes the detrusor musle(closed the internal sphincter) the bladder fill with urine. Pressure in the bladder (150 -300 ml) spinal cord & cerebral cortex parasympathetic stimulation the destrusor musce to contract (opening the internal sphincter) micturition 16
17

PATHOPHYSIOLOGY Either mechanical obstruction of the bladder outlet or Fungtional problem can cause urinary retention. • Benign Prostatic Hypertropy (BPH) is a common cause. • Urethral pathology (infection, tumor, calculus) • Bladder calculi • trauma (pelvic injuries) • pregnancy • neurology disorder (CVA, spinal cord injury, parkinson’s disease, multiple sclerosis) 18
COMPLICATION Ø Ø Ø Chronic infection hyhroureter hydronephrosis DIAGNOSTIC TEST -Urinalysis (hematuria) - Ultrasound 19

NURSING PROCESS q q q Assessment - Health history - Physical Examination Nursing diagnoses Impaired Urinary Elimination Intervention : - catheterization Implementation Evaluation 20

BENIGN PROSTATIC HYPERPLASIA (BPH) 21

DEFINITION BPH : nonmalignant enlargement of the prostate gland, is a common disorder of the aging male. The prostate, very small at birth, grows at puberty. Benign hyperplasia (increased number of cells) begins at 40 to 45 years of age. 22
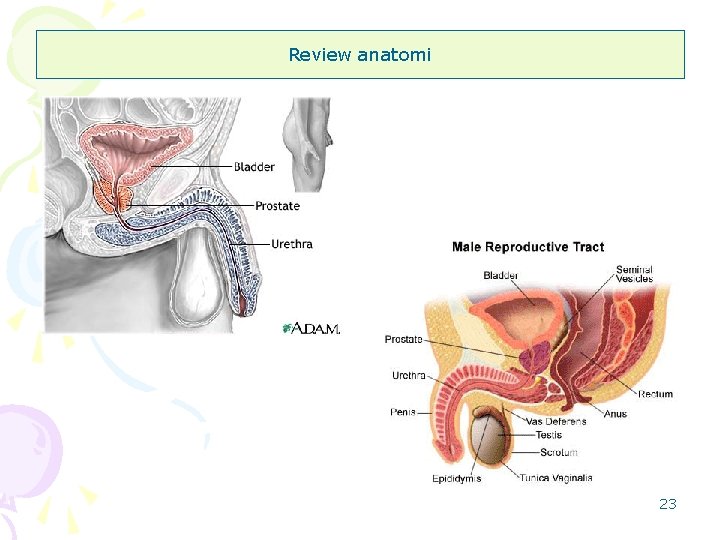
Review anatomi 23
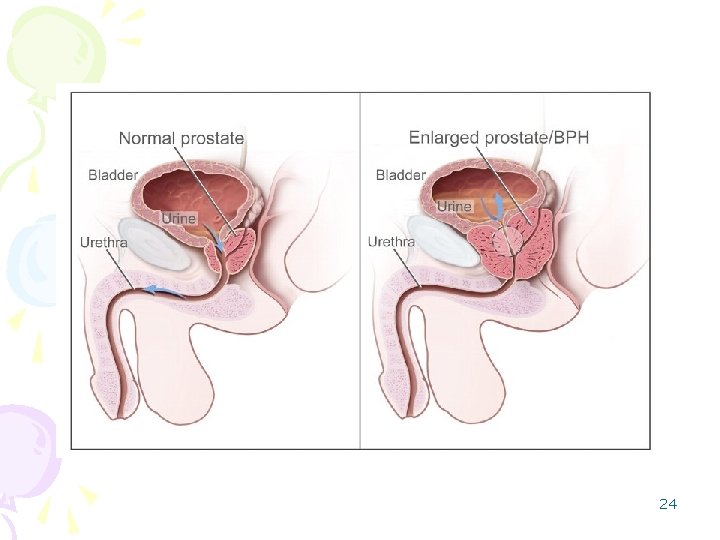
24
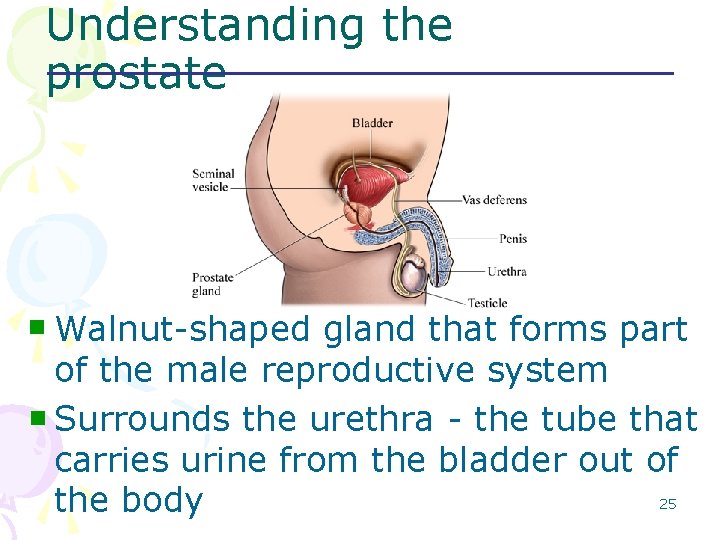
Understanding the prostate Walnut-shaped gland that forms part of the male reproductive system n Surrounds the urethra - the tube that carries urine from the bladder out of 25 the body n
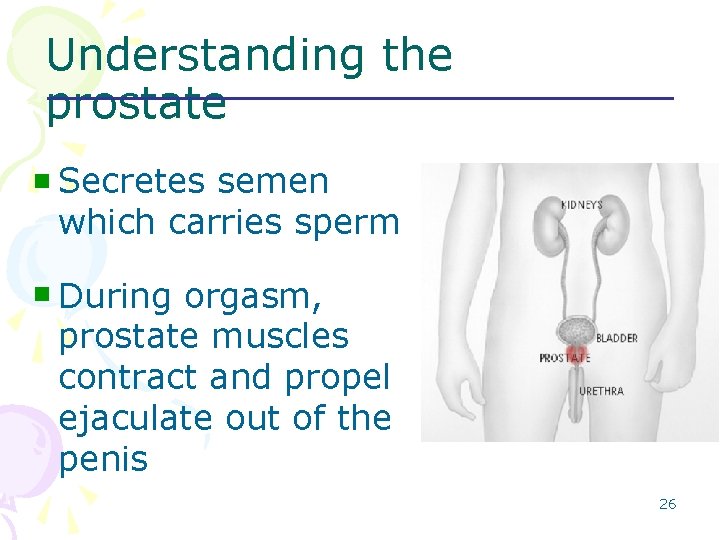
Understanding the prostate n Secretes semen which carries sperm n During orgasm, prostate muscles contract and propel ejaculate out of the penis 26

BPH n The size of prostate enlarged microscopically since the age of 40. Half of all men over the age of 60 will develop an enlarged prostate n By the time men reach their 70’s and 80’s, 80% will experience urinary symptoms But only 25% of men aged 80 will be receiving BPH treatment 27
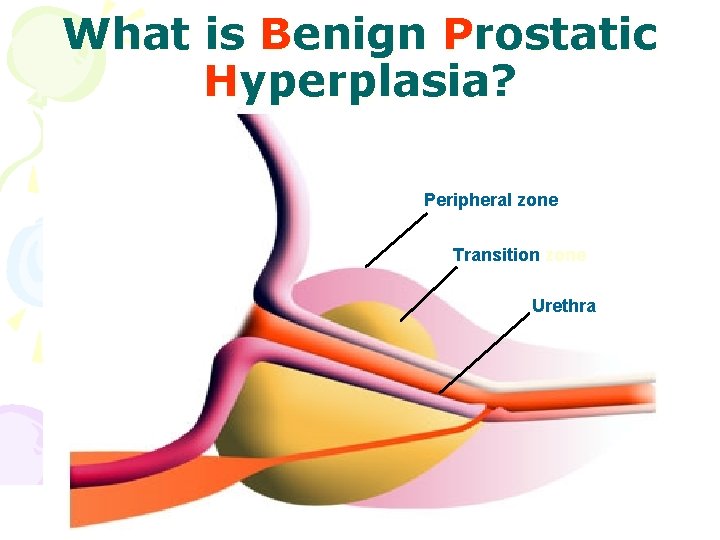
What is Benign Prostatic Hyperplasia? Peripheral zone Transition zone Urethra 28
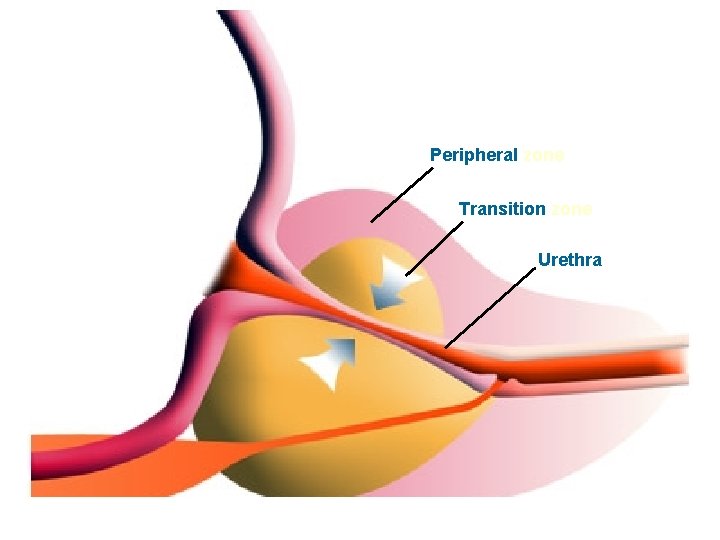
Peripheral zone Transition zone Urethra 29

ETIOLOGI The cause of BPH is unknown. Risk fact include : • age (increases with age) • famili history (higher rates) • race (highest in African American) • ethnicity (lowest in japanese) • hormonal factors 30

What’s LUTS? Voiding (obstructive) symptoms • Hesitancy • Weak stream • Straining to pass urine • Prolonged micturition • Feeling of incomplete bladder emptying • Urinary retention Storage (irritative or filling) symptoms • Urgency • Frequency • Nocturia • Urge incontinence LUTS is not specific to BPH – not everyone with LUTS has BPH and not everyone with BPH has LUTS Blaivas JG. Urol Clin North Am 1985; 12: 215– 24 31

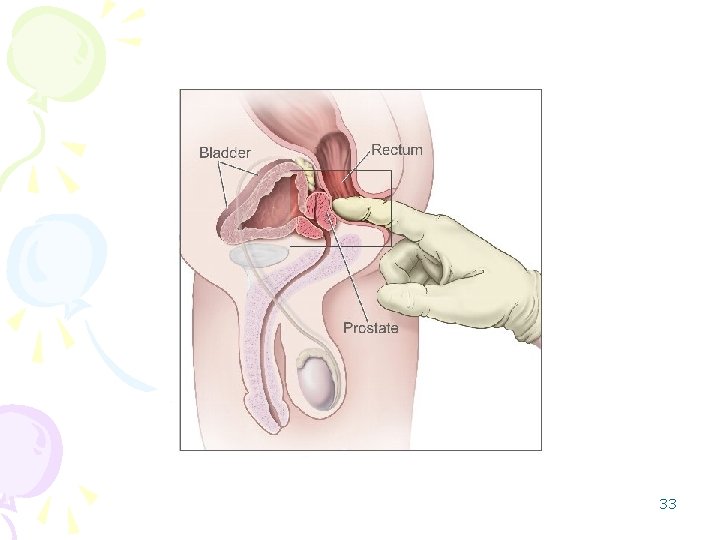
DIAGNOSTIC TESTS Urinalysis : detects bacteria, WBC, or microscopic RBC Ø Serum creatinine levels Ø PSA ( Prostate Specific Antigen) levels. PSA is a glicoprotein produced only in the cytoplasm of benign prostate cell. Ø DRE examines : external surface of the prostate gland. Ø Residual urine : amount of urine remaining in the bladder after voiding. Ø 32
33

When should BPH be treated? BPH needs to be treated ONLY IF: Symptoms are severe enough to bother the patient and affect his quality of life n n Complications related to BPH 34

Choosing the right treatment n Consider risks, benefits and effectiveness of each treatment n Consider the outcome and lifestyle needs 35

Treatment options n “Watchful waiting” n Medication n Surgical approaches Minimal invasive n. TURP n. Invasive “open” procedures n 36

“watchful waiting” n For mild symptoms. follow up 1 to 2 times yearly n Offer suggestions that help reduce symptoms Avoid caffeine and alcohol n Avoid decongestants and antihistamines n 37

Medication n n First line of defense against bothersome urinary symptoms Two major types: n α blockers - relax the smooth muscle of prostate and provide a larger urethral opening n 5 (Hytrin, Doxaben, Harnalidge) α reductase inhibitor Shrink the prostate gland (Proscar, Avodart) 38

Possible side effects of medication n • Impotence n Dizziness • n • Headaches n • Fatigue n • Loss of sexual drive 39
Surgical treatment 40

Indication of surgical intervention • Acute urinary retention • Gross hematuria • Frequent UTI • Vesical stone • BPH related hydronephrosis or renal function deterioration • Obstruction IPSS≧ 8, prostate size, image study, UFR cystoscopic findings, residual urine 41

Conventional Surgical Therapy • Transurethral resection of the prostate (TURP) • Open simple prostatectomy 42
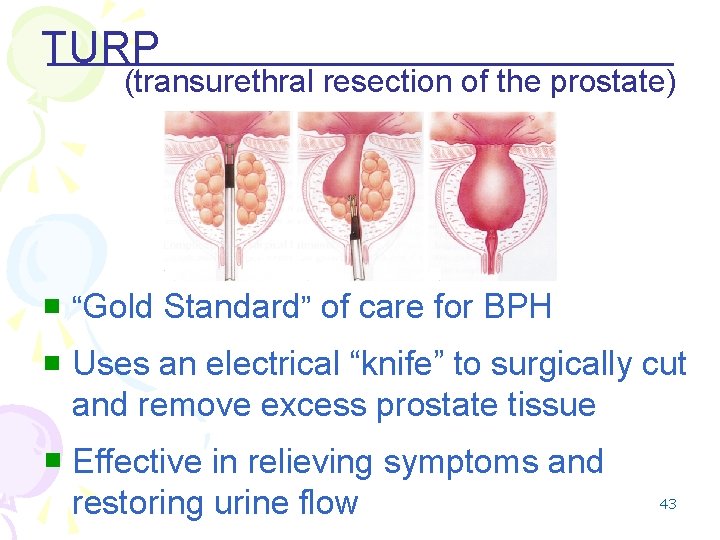
TURP (transurethral resection of the prostate) n “Gold Standard” of care for BPH n Uses an electrical “knife” to surgically cut and remove excess prostate tissue n Effective in relieving symptoms and restoring urine flow 43

TURP • “Gold standard” of surgical treatment for BPH • 80~90% obstructive symptom improved • 30% irritative symptom improved • Low mortality rate 0. 2% 44

The “gold standard”- TURP Disadvantages Benefits n Widely available n Effective n Long lasting n n Greater risk of side effects and complications 1 -4 days hospital stay 1 -3 days catheter 4 -6 week recovery 45

Complication of TURP • Immediate complication bleeding capsular perforation with fluid extravasation TUR syndrome • Late complication urethral stricture bladder neck contracture (BNC) retrograde ejaculation impotence (5 -10%) incontinence (0. 1%) 46

Open Simple Prostatectomy • “too large prostate” -- >100 gm • Combined with bladder diverticulum or vesical stone surgery • Suprapubic or retropubic method 47

NURSING CARE NURSING PROBLEM v Urinary Retention v Risk for infection v Deficit knowledge 48

49
- Slides: 49