WORKING WITH URINARY AND FECAL INCONTINENCE AND PELVIC
































- Slides: 37

WORKING WITH URINARY AND FECAL INCONTINENCE AND PELVIC ORGAN PROLAPSE Presented by: Barbara Wiggin, Ph. D, ANP-BC CCA, specializing in UI, FSH, UDS, POP www. cca-center. com Fall 2015

How the Bladder Works � � The bladder is composed of bands of interlaced smooth muscle (detrusor). The innervation of the body of the bladder is different from that of the bladder neck. The body is rich in beta adrenergic receptors. These receptors are stimulated by the sympathetic component of the autonomic nervous system (ANS). Beta stimulation, via fibers of the hypogastric nerve, suppress contraction of the detrusor. Conversely, parasympathetic stimulation, by fibers in the pelvic nerve, cause the detrusor to contract. Sympathetic stimulation is predominant during bladder filling, and theparasympathetic causes emptying. Two sphincters control the bladder outlet. The internal sphincter is composed of smooth muscle like the detrusor and extends into the bladder neck. Like the detrusor, the internal sphincter is controlled by the ANS and is normally closed. The primary receptors in the bladder neck are alpha-adrenergic. Sympathetic stimulation of these alpha receptors, via fibers in the hypogastric nerve, contributes to urinary continence.

How the Bladder Works � � The external sphincter is histologically different from the detrusor and internal sphincter. It is striated muscle. Like skeletal muscle, it's under voluntary control. It receives its innervation from the pudendal nerve, arising from the ventral horns of the sacral cord. During micturition, supraspinal centers block stimulation by the hypogastric and pudendal nerves. This relaxes the internal and external sphincters and removes the sympathetic inhibition of theparasympathetic receptors. The result is unobstructed passage of urine when the detrusor contracts. The ureters pass between the layers of the detrusor and enter the bladder through the trigone. The ureters propel urine into the bladder. The bladder passively expands to accept urine. As the bladder expands and intravesicular pressure increases, the ureters are compressed between the layers of muscle, creating a valve mechanism. This valve mechanism limits the backflow of urine.

How the Bladder Works � � The normal adult bladder can hold about 500 cc of urine. After emptying, the bladder may still retain about 50 cc residual volume. At about 150 cc of volume, stretch receptors in the detrusor begin signaling the CNS via afferent nerves; at 400 cc we are "seeking" an appropriate toilet Summary: Normally, we are able to control where and when we void. This is largely because the cerebrum is able to suppress the sacral micturition reflex. If the sacral reflex is unrestrained, parasympathetic stimulation via the pelvic nerve causes detrusor contraction. Detrusor contraction is suppressed by alpha and beta sympathetic stimulation via the hypogastric nerve. In response to afferent stimulation, the cerebrum becomes aware of the need to void. If it is appropriate, the cerebrum relaxes the external sphincter, blocks sympathetic inhibition, the bladder contracts and urine is expelled Urinary System: Normal Anatomy & Physiology. http: //www. rnceus. com/uro/norm 2. htm

What is Evaluated � � � Health history Continence history Uroflow Bladder Diary Medication evaluation � � Bowel status Urine Analysis Environmental & mobility assessment Urodynamic study

Health HX � � � Neurological disease Back Problems Obstetrical Gynecological Diabetes

Types of UI � � Acute Chronic

Acute Incontinence � � � D delirium I infection (UTI) A atrophic urethritis, vag. P pharmaceuticals P psychological (depression) � � � E excess output: CHF, hyperglycemia R restricted mobility S stool impaction

Chronic Incontinence & Dysfunction � � � SUI & ISD Overactive bladder: with and without incontinence, IC Mixed Overflow & Retention Functional Reflex

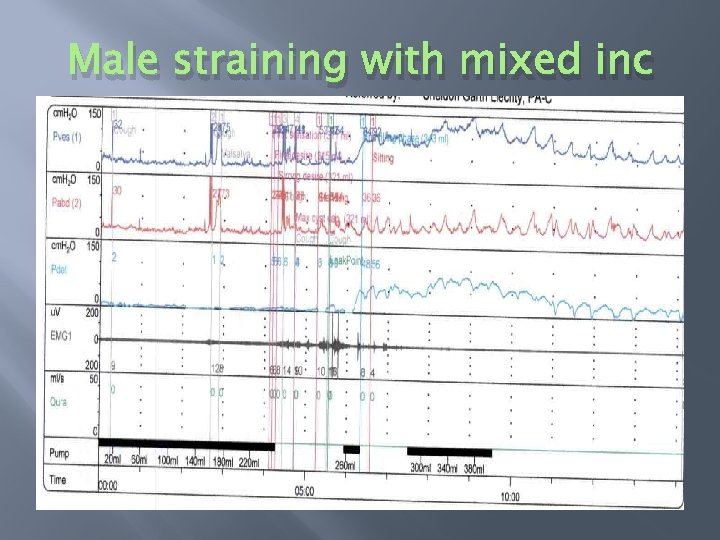
Urodynamic Studies

Male straining with mixed inc

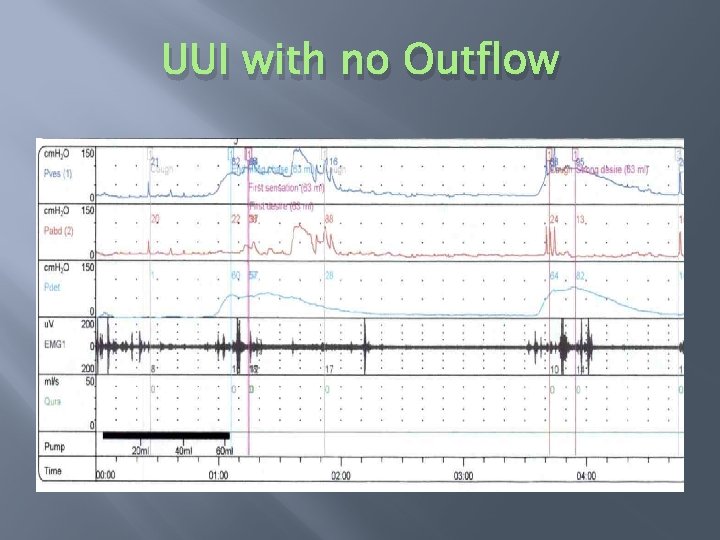
UUI with no Outflow

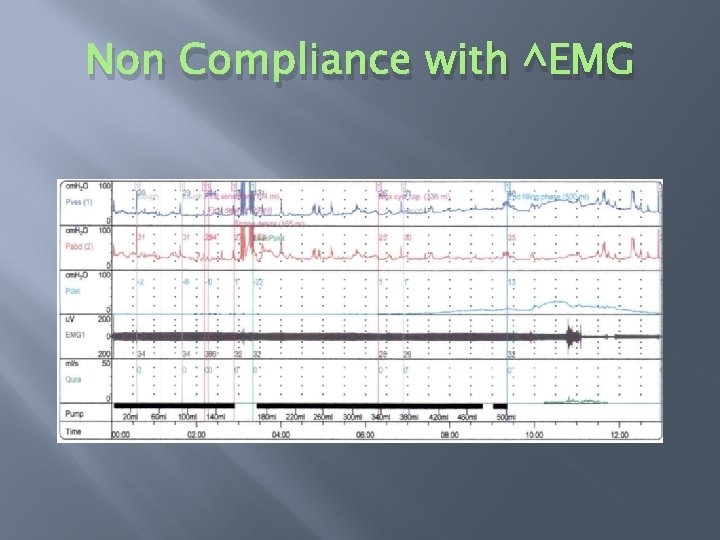
Non Compliance with ^EMG

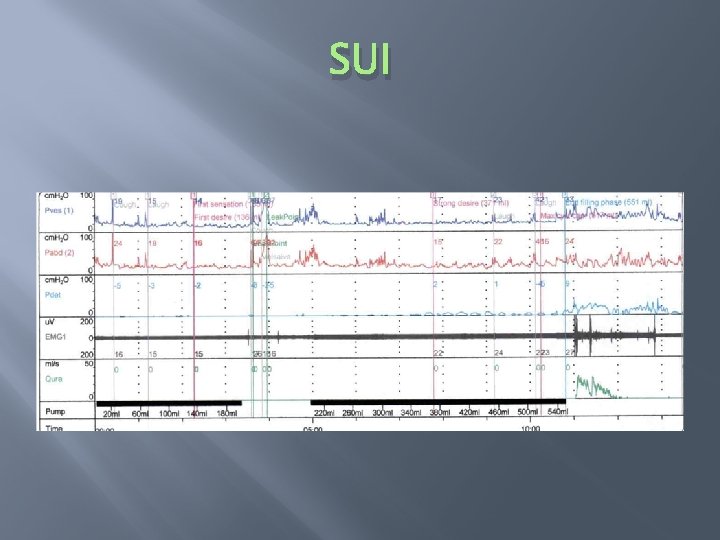
SUI

Medication to Treat OAB Anticholinergics � � � Oxybutynin: IR, ER, patch Tolterodine: IR, ER: less constipation than oxybutynin, dry mouth Trospium: lower constipation Solifenacin: lowest constipation (more selective for M 3 receptors) Darifenacin: less mental confusion, fewer cardiac side effects (more selective for M 3 receptors) Mirabegron(b 3 adrenergic agonist) SE: palpitation, urinary retention, dry mouth, HTN, cold symptoms

Contraindications for Anticholinergics � � � Glaucoma (usually just narrow angle) Hx of Constipation GI hypo motility Hx of Urinary retention Diminished mentation Hx of tachycardia

Treatment for UUI � � onabotulinum toxin. A : blocks action of acetylcholine and paralyses bladder muscle, lasts for several months Urgent PC: percutaneous tibial nerve stimulation (PTNS), mild impulses from the stimulator travel through the needle electrode, along your leg and to the nerves in your pelvis that control bladder function

Treatment for UUI � � � Electrical Stimulation Extracorporeal Magnetic Innervation (Neotonus Chair) Inter. Stim. Medtronic Bladder Control Therapy (Sacral Neuromodulation, delivered by the Inter. Stim® System) has been FDA-approved since 1997 for urge incontinence and since 1999 for urinary retention and significant symptoms of urgency-frequency. Medtronic Bladder Control Therapy is not intended for patients with a urinary blockage.

Treatment for SUI � � � Behavioral Pelvic Muscle Rehab (written, verbal, biofeedback) Supportive � pessaries � Intraurethral Device � Fem. Soft � � Electrical Stimulation Neotonus Chair Surgery Estrogen

Behavioral Management for UI � � � Fluid Management Prevention of Constipation Elevation of LE DC fluids 2 -3 hours before HS Take a deep breath and lean forward when voiding � � Timed toileting Suppression techniques: “Quick Flicks” Monitor bladder irritants Use of Absorbent pads for Urinary Incontinence

PFME � � 10 second sustained contraction of pelvic floor muscle followed by 10 second relaxation of the pfm done 10 times twice a day. Use of biofeedback effective if unable to do pfme

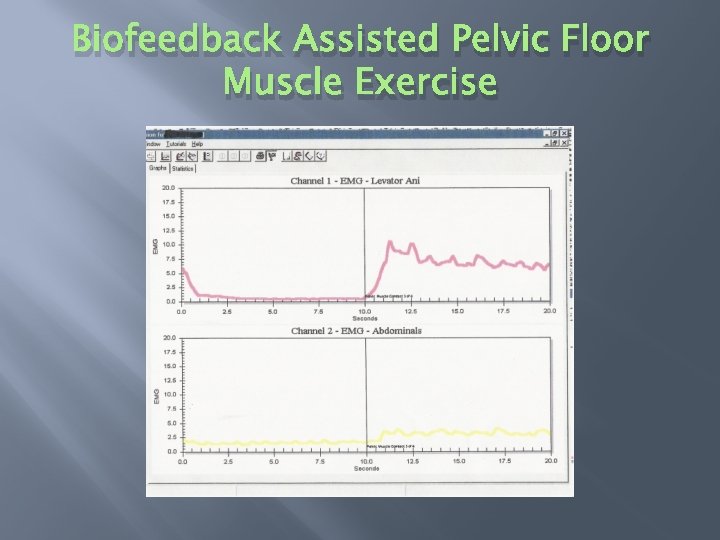
Biofeedback Assisted Pelvic Floor Muscle Exercise

Effective Management of UI � PFMT with Biofeedback is most effective non surgical modality for treatment of SUI

Surgical Treatment � � � Sling (use of cadaveric tissues, synthetic mesh, animal or donor tissue) Colpopexy mesh Urethral Bulking (Collagen) � Injection of bulking materials around the urethra to increase outlet resistance � Inter. Stim Therapy � Stimulation of sacral nerve for treatment of overactive bladder or retention. Neurostimulator supplying constant mild electrical pulses Electrode system placed at L/R 3 rd sacral foramen �Sacral nerves most common distal autonomic and somatic nerve supply to the pelvic floor and lower urinary and gastrointestinal tract

Fecal Incontinence � Evaluate Bowel Status � Treatment � Formed or not � Biofeedback � Timing � Fiber � Physical exam of � Scheduled evacuation rectum � Current problem � Fluid � Exercise

Pessary Use and Management � Indications: prolapse, desire not to have surgery, diagnostic tool for surgical relief, prediction of surgical outcome, Correcting stress incontinence, uterine retrodisplacement, preterm cervical dilation

Pessary Use and Management � Pessary Wear and Care � Intercourse � Removal/Cleaning � When to get a new one � Refitting � Tips � Menses � Gelhorn: Use a short stem if long stem bothers the patient

Pessary Use and Management � New Visit Health history/sexual activity � Focused physical � Pessary fitting � Teach patient how to care for pessary � Follow up in 2 weeks and then in 1 -2 months � If patient managing care of pessary q 6 months � If patient not managing pessary � � F/U Check U/A, uroflow, PVR � Go over patient is managing pessary � Evaluate if pessary is supporting prolapse � Stand to evaluate Evaluate skin integrity � Manage problems � Schedule at appropriate interval �

Pessary Use and Management � Contraindication � Pelvic infections Properly Fitted Pessary � Lacerations or ulcers � Patient is unaware of � Non-compliance � Wide introitus, short vaginal vault � the pessary � No pain or discomfort � Symptoms are relieved

Skin Care � � � Move and toilet pt at least every 2 -3 hours Clean soiled area with water and/or cleanser Use a skin barrier (A&D ointment) Notify appropriate staff if skin is breaking down Change pads when soiled � � � Good hydration Good nutrition Adequate fluid intake (6 -8 8 oz glasses of non-caffeinated fluids) Monitor urine color and odor Monitor pt for confusion, elevated temp, not feeling well

Prevention of UTIs � � � Adequate hydration Dabbing when wiping Pt. checked to ensure he/she is emptying completely Void q 2 -3 hours Take a deep breath/lean forward to empty Taking enough time to void � � � Using water to cleanse vulva Unavoidable if has indwelling catheter, CIC decreases UTIs Consider UTI if pt has increased confusion, odorous urine, changed bladder pattern

Case Study LL Sex: F Age: 92 c/o: frequency, nocturia, ui Health Hx: arthritis, glaucoma, hypertension (not a problem now), osteoporosis Current medications: None

Case Study LL � � � Previous treatment: anticholinergics Focused physical exam: pale vag. tissue, little recruitment of pfm, U/A neg UDS: normal capacity, poor compliance, SUI at low pressure (56 cm H 20), empties well, increased pfm tone with voiding Plan of Care: fluid management, elevation of legs, stress technique, biofeedback assisted pfme Results of Treatment: often does not wear pads, continues to do pfme, discussed collagen implants.

Case Study DS Sex: F Age: 77 c/o: overactive bladder Health Hx: depression/anxiety, arthritis, hysterectomy, HTN Current medications: lansoprazole, estrogen, valsartan, nabumetone, escitalopram, tolterodine

Case Study DS � � � Previous treatment: tolterodine Focused physical exam: pale vag. tissue, reddened vulva, sl recruitment of pfm, atrophic introitus, U/A neg UDS: delayed 1 st sensation, normal capacity, SUI at low pressure (75 cm H 20), empties well, emg activity during void, after contraction Plan of Care: Dc’d tolterodine, discussed collagen implant, or sling, stress technique, urge technique, biofeedback assisted pfme Results of Treatment: pt. feel she is much improved, continues to do pfme, does not want referral to urologist.

Bibliography Doughty, D. B. Urinary and fecal incontinence (3 rd ed. ) (pp. 21 -54). St. Louis, MO: Mosby/Elsevier. Dr. Rose’s peripheral brain. (2012, October 24). Neurogenic bladder: Bladder dysfunction and urinary incontinence. http: //faculty. washington. edu/momus/PB/tableofc. htm Effective Health Care Program (2012, April) Non-surgical treatments for urinary incontinence, A review of the research for women. Agency for Healthcare, Research and Quality. Pub No. 11(12)EHCO 74 -A Gray, M. L. (2006). Physiology of voiding. In Doughty, D. B. Urinary and fecal incontinence (3 rd ed. ) (pp. 21 -54). St. Louis, MO: Mosby/Elsevier. Kershen, R. T. , Appell, R. A. (2003). Voiding dysfunction after anti-incontinence surgery in women. Issues in Incontinence, Spring/Summer, 1, 9 -11. Krissovich, M. (2006). Pathology and management of the overactive bladder. In Doughty, D. B. Urinary and fecal incontinence (3 rd ed. ) (pp. 109 -165). St. Louis, MO: Mosby/Elsevier. Mayo Clinic. (1998 -2007). Overactive bladder. http: //www. mayoclinic. com/print/overactivebladder/DS 00827/DSECTION=all&METHO. . . Medtronic. What Is Medtronic Bladder Control Therapy? http: //www. medtronic. com/patients/overactive-bladder/about-therapy/what-is-it/index. htm National guidelines and clinical evidence only modestly influence prescribing of antihypertensive agents. (2007, January). Research Activities, 317, 15. Newman, D. K. (2007, March). Dawning of a dry day: Fresh perspectives in managing overactive bladder. Paper presented at the Annual Symposium of the Society of Urologic Nurses and Associates, Colorado Springs, CO.

Bibliography Newman, D. K. (2006, October). Pharmacologic Management of OAB-You make the call. Paper presented the Annual Meeting of the Society of Urologic Nurses and Associates, Kansas City, MO. Sand, P. K. , Dmochowski, R. (2002). Analysis of the standards of terminology of lower urinary tract dysfunction: Report from the standardisation sub-committee of the International Continence Society. Neurology and Urodynamics, 21, 167 -78. NIH. (2007). Urologic disease cost Americans $11 billion a year. http: //www. nih. gov/news/pr/may 2007/niddk-01. htm. Serels, S. R. , Appell, R. A. (2002, 2001). Bladder control problems. Newton, PA: Handbooks in Health Care Co. Staskin, D. (2004). Lower urinary tract dysfunction in the female. In A. P. Bourcier, E. J. Mc. Guire, & P. Abrams (Eds. ), Pelvic floor disorders (pp. 43 -56). Philadelphia, PA: Elsevier Saunders. Urinary Incontinence in Adults Guideline Update Panel. (1996). Urinary incontinence in adults: Acute and chronic management. Clinical Practice Guideline, No. 2, 1996 Update. Rockville, MD: U. S. Department of Health and Human Services. Public Health Service, Agency for Health Care Policy and Research (AHCPR Publication No. 96 -0682). Urinary System: Normal Anatomy & Physiology. http: //www. rnceus. com/uro/norm 2. htm Uroplasty. Urgent ® PC Neuromodulation System. https: //www. uroplasty. com/healthcare