Update in Clinical Psychopharmacology Peter A De Maria










































- Slides: 52

Update in Clinical Psychopharmacology Peter A. De. Maria, Jr. , M. D. , FASAM Tuttleman Counseling Services Temple University Clinical Associate Professor of Psychiatry Temple University School of Medicine Philadelphia, PA

Disclosures • I have no actual or potential conflict of interest in relation to this educational activity or presentation. • Use of trade versus generic drug names • Off-label use of drugs.

Treatment Planning 1. Medication 2. Psychotherapy 3. Combined medication and psychotherapy

Referral for Psychopharmacologic Evaluation/Treatment 1. When to refer 2. Preparing the patient 3. What to expect 4. The challenge of split treatment – Communication – Dynamics – Ethics – Legal issues 5. What to expect

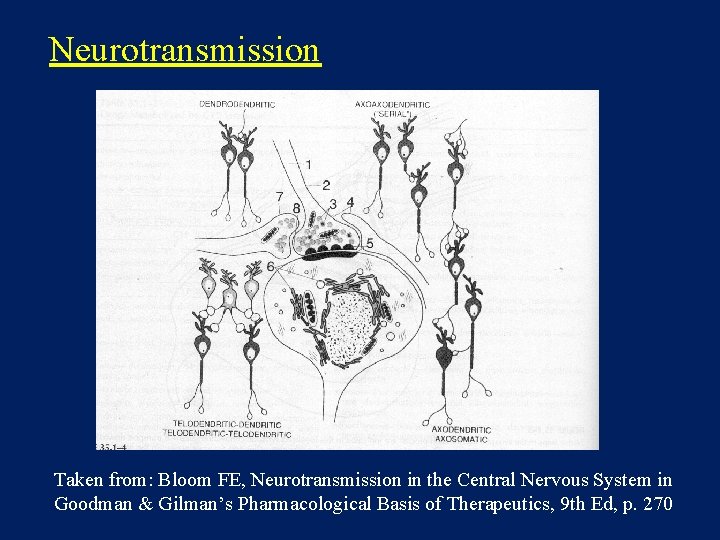
Neurotransmission Taken from: Bloom FE, Neurotransmission in the Central Nervous System in Goodman & Gilman’s Pharmacological Basis of Therapeutics, 9 th Ed, p. 270

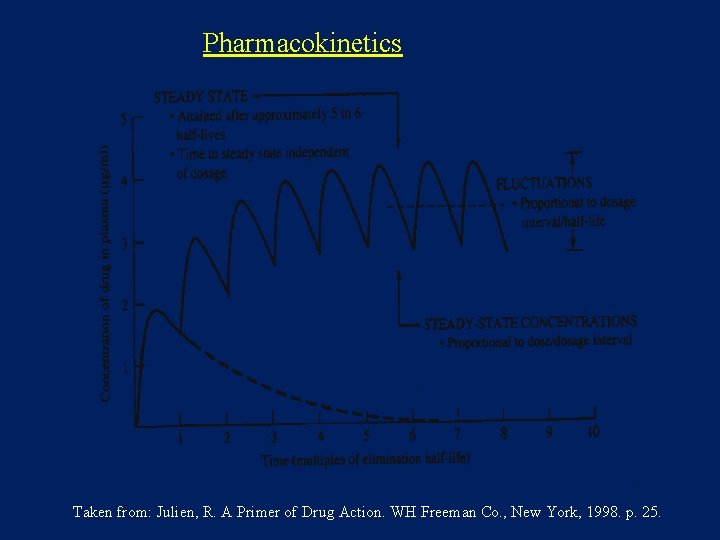
Pharmacokinetics Taken from: Julien, R. A Primer of Drug Action. WH Freeman Co. , New York, 1998. p. 25.

Drug Interactions · Synergism (e. g. alcohol + sedative) · Induction of enzymes and increased metabolism · Inhibition of enzymes and delayed metabolism · In vitro versus clinical significance FDA approval vs. clinical use (“Off-label use”)

Selecting a Psychotropic Agent • • • Diagnosis/symptom complex Patient’s prior response Family member’s experience FDA approved indication Pharmacologic actions Documented efficacy Side effect profile Insurance coverage/finances Patient preference

DSM-IV Classification of Depressive Disorders • • Adjustment disorder with depressed mood Dysthymia Major depression (MDD) Premenstrual Dysphoric disorder (PMDD)

Pharmacotherapy options • Monoamine oxidase inhibitors (MAOI) • Tricyclic antidepressants (TCA) – Amitriptyline (Elavil) – Nortriptyline (Pamelor) Imipramine (Tofranil) Desipramine (Norpramin) • Selective Serotonin Reuptake Inhibitors (SSRI) • Serotonin and Norepinephrine Reuptake inhibitors (SNRI) • Atypical antidepressants – Bupropion (Wellbutrin) • On the horizon Nefazodone (Serzone)

Selective Serotonin Reuptake Inhibitors (SSRI) 1. Examples Sertraline (Zoloft) Citalopram (Celexa) Paroxetine (Paxil) Fluoxetine(Prozac) Escitalopram (Lexapro) Fluvoxamine (Luvox) 2. Mechanism of Action Blocks re-uptake of serotonin thereby increasing serotonin in the synapse

SSRI - FDA Approved Indications Therapeutic Response • Can take between 2 and 8 weeks • Response is gradual • Others may notice the response before the patient does

SSRI/SNRI Side Effects • • • Gastrointestinal Anxiety/insomnia Flushing/night sweats Vivid dreams Weight change Sexual dysfunction

Antidepressant-Induced Sexual Dysfunction Desire Decreased libido Arousal Difficulties w/ erection/lubrication Orgasm Delayed orgasm/anorgasmia Management – Spontaneous resolution – Decrease dose – Change agent – Adjunctive medication Selective PDE 5 Inhibitor Cyproheptadine (Periactin) Bupropion (Wellbutrin)

“Poop-out” Effect 1. Definition 2. Explanation – Placebo response – Inadequate dose – Potential changes in receptors 3. Management – Drug holiday – Increase dose – Change antidepressant – Add agent with NE or DA properties

Discontinuation Syndrome • Develops after abrupt cessation of SSRI/SNRI • Symptoms = washed-out, flu-like, lightheaded, H/A, emotional liability, diarrhea • Can occur with all SSRIs/SNRIs • May be related to half-life • Worse with paroxetine (Paxil) and venlafaxine (Effexor) • Abates with re-challenge of SSRI/SNRI • Slow taper of SSRI/SNRI or change to longer acting agent.

Serotonin-Norepinephrine Reuptake Inhibitors (SNRI) • Mechanism of Action • Examples and Indications • Side Effects Desvenlafaxine (Pristiq) Duloxetine (Cymbalta) Mirtazapine (Remeron) Venlafaxine (Effexor-XR) MDD GAD X X X PD SAD FM X X X MDD = Major depressive disorder, GAD = Generalized anxiety disorder, PD = Panic disorder, SAD = Social anxiety disorder, FM = Fibromyalgia.

Treatment Resistant Depression 1. Is the patient medication compliant? 2. Is the diagnosis correct? 3. Change agents-Within/between classes 4. Antidepressant combinations -Complementary mechanisms of action 5. Add psychotherapy 6. Augmentation strategies – Lithium – Antipsychotic Thyroid hormone Estrogen 7. ECT/Focal Brain Stimulation

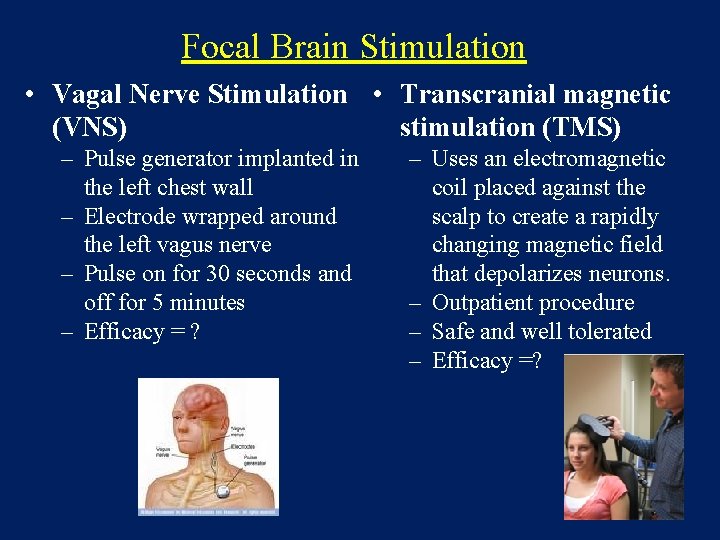
Focal Brain Stimulation • Vagal Nerve Stimulation • Transcranial magnetic (VNS) stimulation (TMS) – Pulse generator implanted in the left chest wall – Electrode wrapped around the left vagus nerve – Pulse on for 30 seconds and off for 5 minutes – Efficacy = ? – Uses an electromagnetic coil placed against the scalp to create a rapidly changing magnetic field that depolarizes neurons. – Outpatient procedure – Safe and well tolerated – Efficacy =?

How long to Treat? • 6 -12 months • Longer if, – Return of symptoms on discontinuation of AD – Recurrent episodes of depression – Severe depression (suicide attempt, psychosis) Number of Prior Episodes of Depression Recurrence Rate 1 < 50% 2 50 -90% 3 or more >90% Taken from: Stahl S. Essential Psychopharmacology: Neuroscientific Basis and Practical Applications. 2 nd Ed. , Cambridge University Press. 2000, p. 150. )

FDA Suicide Warning • Black Box Warning • All antidepressants • Increased risk of suicidal thinking and behaviors • Affects 18 -24 y/o

On the Horizon • Corticotropin releasing factor-1 (CRF 1) antagonists • Glucocorticoid receptor antagonists • Substance P receptor antagonists • NMDA receptor antagonists • Melanocyte inhibiting factor (nemifitide) • Omega -3 fatty acids • Melatonin receptor antagonists • Focal and deep brain stimulation therapies

STAR*D • Largest (n=4041, age 18 -75 y/o) study of treatment of non-psychotic MDD • Multiple real-world psychiatric and primary care settings • Conducted between July 2001 and April 2004 • Funded by National Institute of Mental Health (NIMH) • Goal was remission (< 5 on the QIDS-C 16) • Treatment involved 6 levels with patient ability to choose options • Available at www. star-d. org

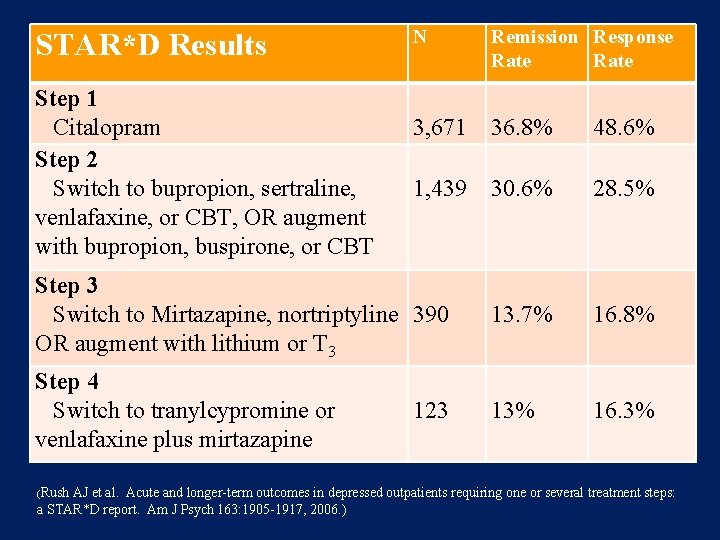
N Remission Response Rate 3, 671 36. 8% 48. 6% 1, 439 30. 6% 28. 5% Step 3 Switch to Mirtazapine, nortriptyline 390 OR augment with lithium or T 3 13. 7% 16. 8% Step 4 Switch to tranylcypromine or venlafaxine plus mirtazapine 13% 16. 3% STAR*D Results Step 1 Citalopram Step 2 Switch to bupropion, sertraline, venlafaxine, or CBT, OR augment with bupropion, buspirone, or CBT (Rush 123 AJ et al. Acute and longer-term outcomes in depressed outpatients requiring one or several treatment steps: a STAR*D report. Am J Psych 163: 1905 -1917, 2006. )

STAR*D • MDD is a chronic and recurrent illness. • Using objective measurements of symptoms and side effects a can help with treatment decisions. • Remission can take time (at least 8, but up to 14 weeks). • Many steps may be needed to reach remission. – Remission rate of 50% was reached after 2 steps. – Remission rate of 70% was reached after 4 steps • Remission results in better log-term outcomes. • Participant attrition is high. (Warden D et al. The STAR*D project results: a comprehensive review of findings. Current Psychiatry Reports 9: 449 -459, 2007. )


DSM-IV Anxiety Disorders 1. Adjustment disorder 2. Generalized anxiety disorder (GAD) 3. Panic disorder 4. Obsessive-compulsive disorder (OCD) 5. Social anxiety disorder (social phobia) 6. Acute stress disorder 7. Post traumatic stress disorder (PTSD) 8. Specific phobia

Benzodiazepines Taken from: Kaplan SI, Sadock BJ. Kaplan & Sadock’s Synopsis of Psychiatry, 8 th ed. , Lippincott, Williams & Wilkins, Philadelphia, 1998, p. 996. Advantages -Rapid onset of action -Highly effective Disadvantages -Physiologic dependence -Addicting -Impaired cognition Anterograde amnesia

J of Clin. Psychiatry, 60(5), 252, May 1999

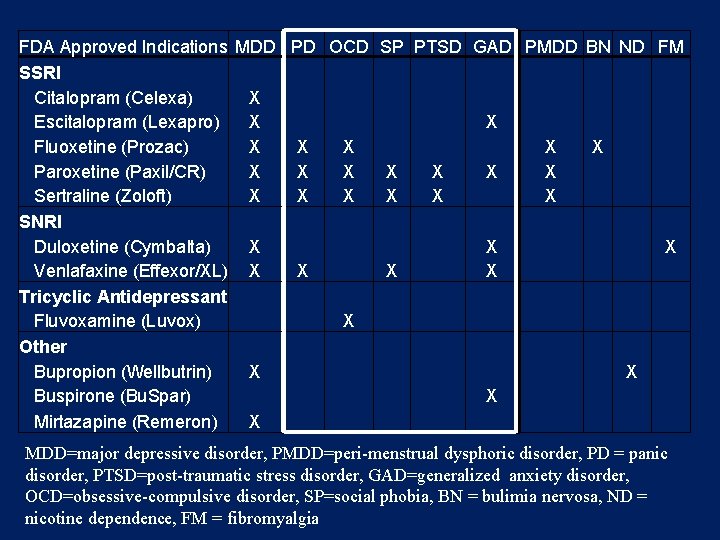
FDA Approved Indications MDD PD OCD SP PTSD GAD PMDD BN ND FM SSRI Citalopram (Celexa) X Escitalopram (Lexapro) X Fluoxetine (Prozac) X X X Paroxetine (Paxil/CR) X X X X Sertraline (Zoloft) X X X X SNRI Duloxetine (Cymbalta) X X Venlafaxine (Effexor/XL) X X X X Tricyclic Antidepressant Fluvoxamine (Luvox) X Other Bupropion (Wellbutrin) X X Buspirone (Bu. Spar) X Mirtazapine (Remeron) X MDD=major depressive disorder, PMDD=peri-menstrual dysphoric disorder, PD = panic disorder, PTSD=post-traumatic stress disorder, GAD=generalized anxiety disorder, OCD=obsessive-compulsive disorder, SP=social phobia, BN = bulimia nervosa, ND = nicotine dependence, FM = fibromyalgia

SSRI/SNRIs in Anxiety Disorders Advantages • High efficacy • Non-addicting • Effective for a number of conditions Disadvantages • Can take 2 -8 weeks or longer to be effective • Side effects • Drug interactions • Discontinuation syndrome

Other Options for Anxiety Disorders • Buspirone (Bu. Spar) • Beta blockers • Combinations – SSRI/SNRI + Benzodiazepine • Antipsychotics – Trifluoperazine (Stelazine) – Quetiapine (? ) • Pregabalin (? )

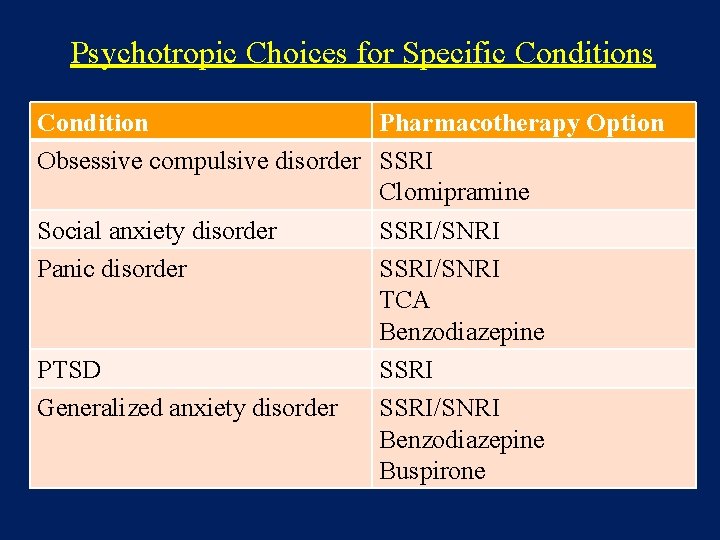
Psychotropic Choices for Specific Conditions Condition Pharmacotherapy Option Obsessive compulsive disorder SSRI Clomipramine Social anxiety disorder SSRI/SNRI Panic disorder SSRI/SNRI TCA Benzodiazepine PTSD SSRI Generalized anxiety disorder SSRI/SNRI Benzodiazepine Buspirone

DSM-IV Psychotic Disorders 1. Schizophreniform disorder 2. Schizophrenia 3. Schizoaffective disorder 4. Brief psychotic disorder

The Disease Process Positive Symptoms • Hallucinations • Delusions • Disorganization • Agitation Negative symptoms • Blunted affect • Emotional withdrawal • Social withdrawal • Anhedonia

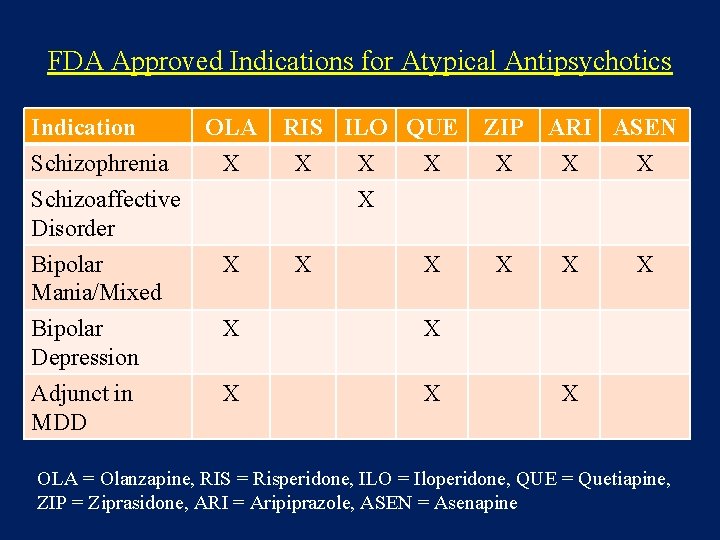
FDA Approved Indications for Atypical Antipsychotics Indication Schizophrenia Schizoaffective Disorder OLA X RIS ILO QUE X X Bipolar Mania/Mixed X X X Bipolar Depression X X Adjunct in MDD X X ZIP X X ARI ASEN X X X OLA = Olanzapine, RIS = Risperidone, ILO = Iloperidone, QUE = Quetiapine, ZIP = Ziprasidone, ARI = Aripiprazole, ASEN = Asenapine

Atypical (2 nd Generation) Antipsychotics HL=haloperidol (Haldol), CPZ=chlorpromazine (Thorazine), CLZ=clozapine (Clozaril), RIS=risperidone (Risperdal), OLZ=olanzapine (Zyprexa), QTP=quetiapine (Seroquel), ZIP=ziprasidone (Geodon) (Taken from: Jam, MW. Advances in the treatment of psychosis: a multidisciplinary continuing education program. Power-Pak CE, New York, NY 2001, p. 8. )

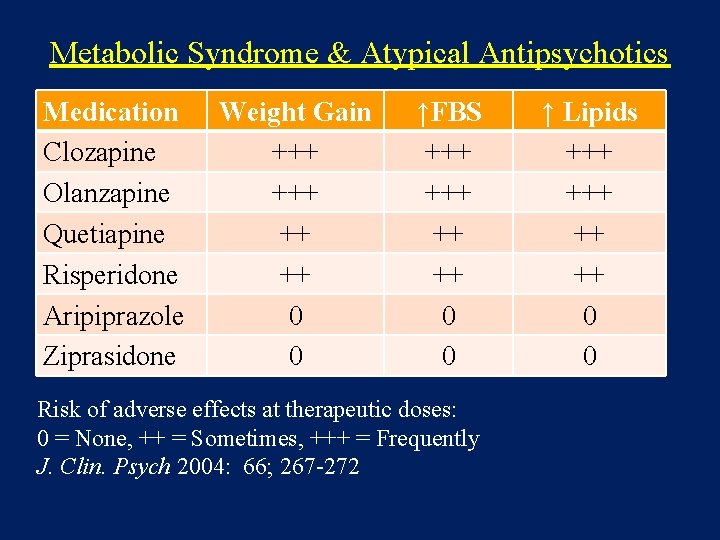
Metabolic Syndrome & Atypical Antipsychotics Medication Clozapine Olanzapine Quetiapine Risperidone Aripiprazole Ziprasidone Weight Gain +++ ++ ++ 0 0 ↑FBS +++ ++ ++ 0 0 Risk of adverse effects at therapeutic doses: 0 = None, ++ = Sometimes, +++ = Frequently J. Clin. Psych 2004: 66; 267 -272 ↑ Lipids +++ ++ ++ 0 0

CATIE • 1460 “real-world” schizophrenics (no first-break schizophrenics) • NIMH funded • Comparison of second generation antipsychotics to a representative first generation antipsychotic (perphenazine). Agent Time to Discontinuation All Cause (months) Discontinuation Rate Olanzapine Perphenazine Quetiapine Risperidone Ziprasidone 9. 2 5. 6 4. 8 3. 5 64% 75% 82% 74% 79%

CATIE • Overall findings: – Discontinuation rates for all agents were high. – Olanzapine was the most efficacious medication, however, it was associated with the greatest weight gain, and the worst metabolic profiles. – For those patients changing drugs due to tolerability, olanzapine and risperidone were more efficacious second choice drugs. – Ziprasidone had a better metabolic profile.

DSM-IV Mood Disorders Bipolar disorder (manic-depressive disorder) · Bipolar I (recurrent major depression and mania) · Bipolar II (recurrent major depression with hypomania) · Specifiers q Rapid cycling (more than 4 episodes in a 12 month period) q Seasonal pattern Cyclothymia

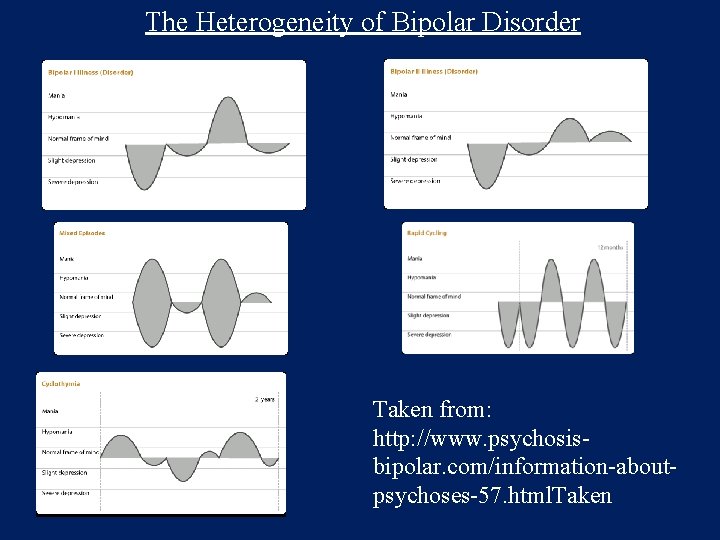
The Heterogeneity of Bipolar Disorder Taken from: http: //www. psychosisbipolar. com/information-aboutpsychoses-57. html. Taken

Pharmacotherapy for Mood Disorders 1. Mood stabilizers Lithium 2. Anticonvulsant Mood Stabilizers Valproic acid (Depakote) Carbamazepine (Tegretol) Oxcarbazepine (Trileptal) Lamotrigine (Lamictal) Topiramate (Topamax)-? 3. Atypical Antipsychotics Olanzapine (Zyprexa) Risperidone (Risperdal) Quetiapine (Seroquel) Aripiprazole (Abilify) Ziprasidone (Geodon) 4. Combination Olanzapine/fluoxetine (Symbyax)

Treating Bipolar Disorder • Use mood charting. • Combination pharmacotherapy is the rule rather than the exception. • Mood stabilizers are the cornerstone of therapy. • Optimize therapeutic effect and tolerability while minimizing side effects. • Antidepressants mat worsen the disease course. • Anticonvulsants & FDA suicide warning

Pharmacotherapy for Bipolar Disorder Phase Mania Treatment Options Lithium (Li) Valproate (VP) Atypical antipsychotic Carbamazepine/oxcarbamazepine Li/VP + atypical antipsychotic Electroconvulsive therapy (ECT) Depression Optimize mood stabilizer Lamotrigine Quetiapine Olanzapine/fluoxetine Mood stabilizer + antidepressant Maintenance In general, continue regimen that is working, however, simplify as clinically indicated.

Insomnia • • • A symptom, not a diagnosis Evaluate for underlying cause Promote good sleep hygiene Use a sleep log Pharmacotherapy – 10 days or less – Options • • • Non-benzodiazepine hypnotics Benzodiazepine hypnotics Sedating antihistamines Sedating antidepressants Sedating antipsychotics

Attention Deficit Hyperactivity Disorder 1. Stimulants – – Amphetamine salts (Adderall) Methylphenidate (Ritalin, Concerta, Focalin) Dextroamphetamine (Dexedrine) Pemoline (Cylert) 2. Non-stimulants – Atomoxetine (Strattera) – Guanfacine extended release (Intuniv) – Others • Bupropion(Wellbutrin) • Tricyclic antidepressants • Venlafaxine (Effexor) 3. New Delivery Systems – Methylphenidate patch (Daytrana) – Pro-drug: lisdexamfetamine (Vyvanse)

Pharmacotherapy for Eating Disorders 1. Classification Anorexia nervosa Bulimia nervosa Eating disorder NOS 2. Pharmacotherapy options SSRIs for bingeing/purging Topiramate for binging/purging - ? Treatment for co-morbid disorders

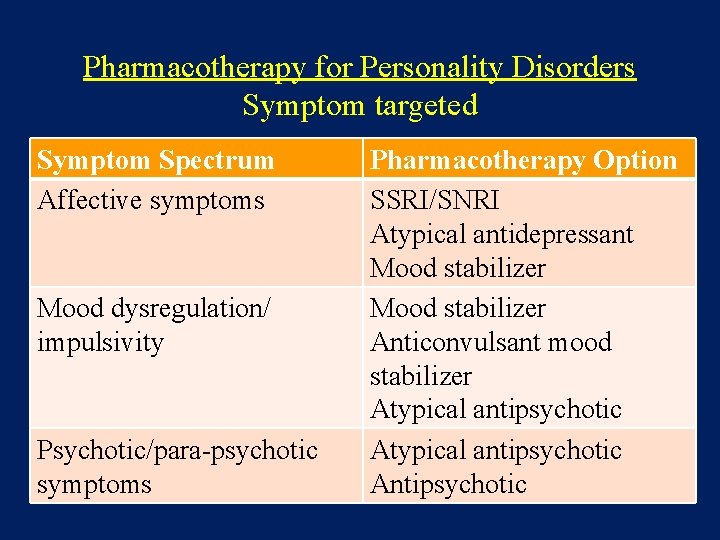
Pharmacotherapy for Personality Disorders Symptom targeted Symptom Spectrum Affective symptoms Mood dysregulation/ impulsivity Psychotic/para-psychotic symptoms Pharmacotherapy Option SSRI/SNRI Atypical antidepressant Mood stabilizer Anticonvulsant mood stabilizer Atypical antipsychotic Antipsychotic

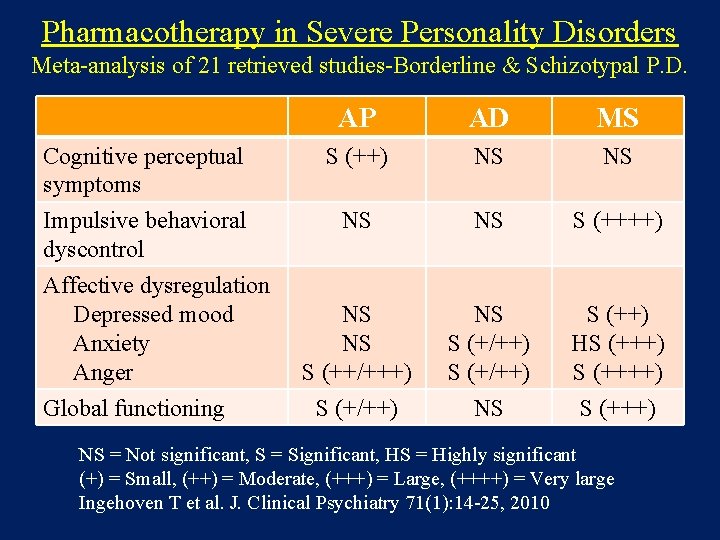
Pharmacotherapy in Severe Personality Disorders Meta-analysis of 21 retrieved studies-Borderline & Schizotypal P. D. AP AD MS Cognitive perceptual symptoms S (++) NS NS Impulsive behavioral dyscontrol NS NS S (++++) NS NS S (++/+++) S (+/++) NS S (++) HS (+++) Affective dysregulation Depressed mood Anxiety Anger Global functioning NS = Not significant, S = Significant, HS = Highly significant (+) = Small, (++) = Moderate, (+++) = Large, (++++) = Very large Ingehoven T et al. J. Clinical Psychiatry 71(1): 14 -25, 2010

Pharmacotherapy for Substance Use Disorders • Drugs for intoxication/withdrawal • Aversive agents – Disulfiram (Antabuse) • Maintenance agents – Methadone – Buprenorphine (Suboxone/Subutex) • Anticraving agents – Nicotine replacement therapy (NRT) – Naltrexone (Re. Via. Vivitrol) – Acamprosate (Campral) – Varenicline (Chantix) – Topiramate (Topamax) - ?
