Nonaccidental injury and the Orthopaedic Surgeon Peter Worlock
















- Slides: 30

Non-accidental injury and the Orthopaedic Surgeon. Peter Worlock Newcastle General Hospital

Role of doctors: • Be aware of problem. • Recognise unusual injury patterns. • Initiate investigation.

Soft tissue injuries: • Bites. • Burns. • Bruising.

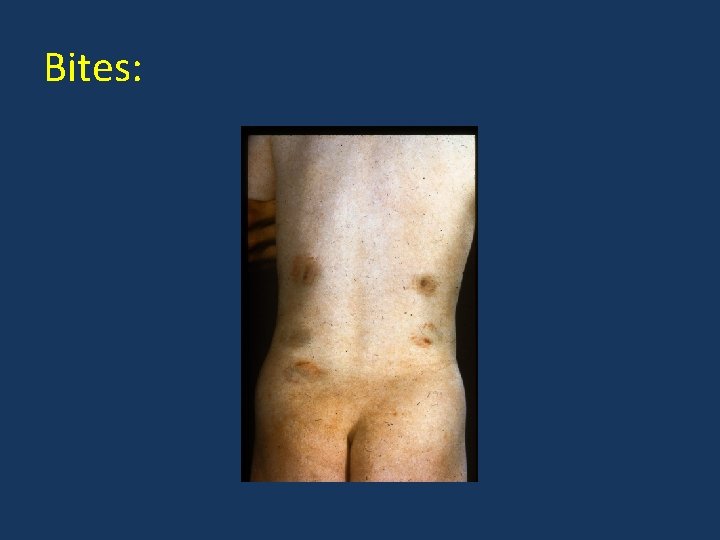
Bites:

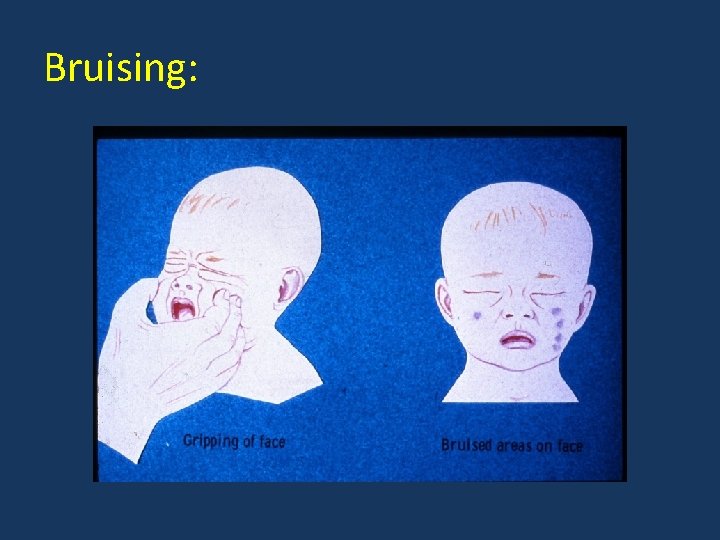
Bruising:

Soft tissue injuries – normal children: • Head/face injuries rare <18 months. • Lumbar injuries unusual before age of 5 years. • Bruising of hands/feet and lower legs is most common injury. Roberton et al, 1982

Soft tissue injuries – NAI: • Head/face injuries present in 60%. • Lumbar injuries common under age of 5 years. Roberton et al, 1982

Fracture pattern: • Accidental Injury (AI) – all children aged <13 years living in Nottingham Jan-June 1981 with a #. • Study group – 826 consecutive children. • Non-accidental injury (NAI) – all children aged <13 years in Nottingham with # from child abuse 1976 -1982. • Study group – 35 children.

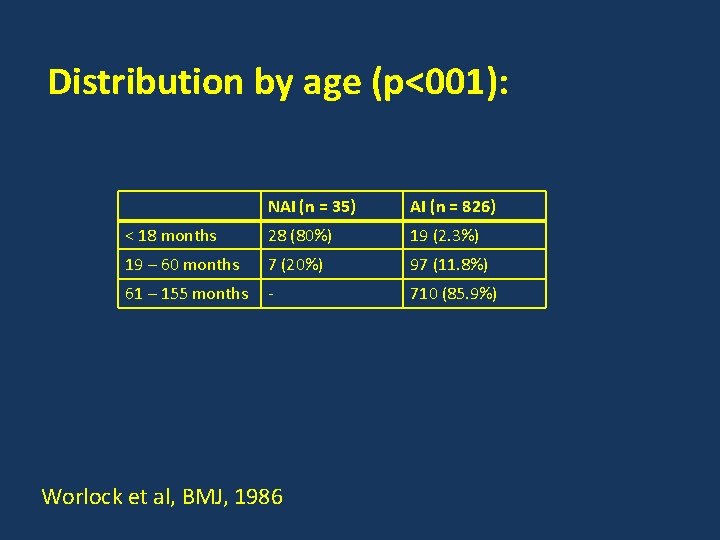
Distribution by age (p<001): NAI (n = 35) AI (n = 826) < 18 months 28 (80%) 19 (2. 3%) 19 – 60 months 7 (20%) 97 (11. 8%) 61 – 155 months - 710 (85. 9%) Worlock et al, BMJ, 1986

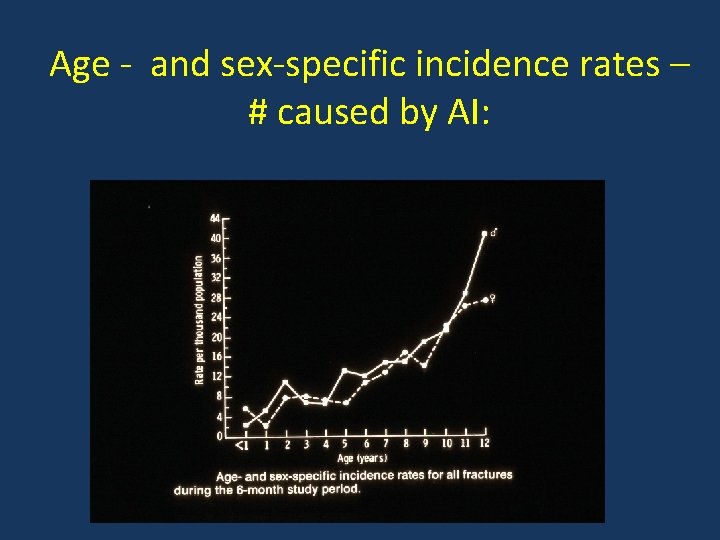
Age - and sex-specific incidence rates – # caused by AI:

AI group # incidence during six month study period (p<0. 001): Pop. at risk Incidence < 18 months 10, 989 1. 7/1000 19 – 60 months 23, 564 4. 8/1000 61 -155 months 68, 288 10. 4/1000 Worlock et al, BMJ, 1986

Annual # incidence (NAI : AI): < 18 months NAI AI 4/10, 000 34/10, 000 19 – 60 months 0. 4/10, 000 Worlock et al, BMJ, 1986 96/10, 000

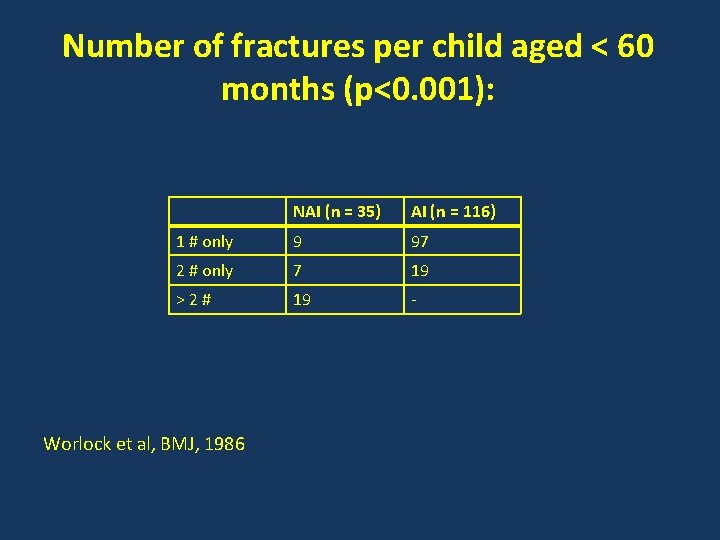
Number of fractures per child aged < 60 months (p<0. 001): NAI (n = 35) AI (n = 116) 1 # only 9 97 2 # only 7 19 >2# 19 - Worlock et al, BMJ, 1986

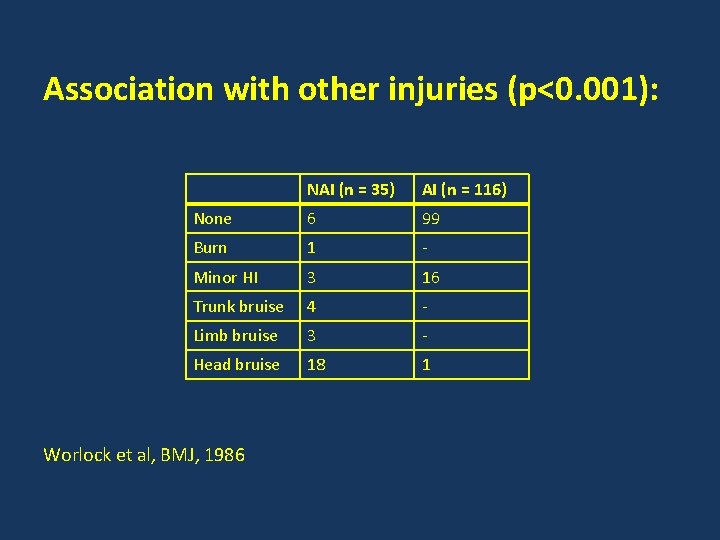
Association with other injuries (p<0. 001): NAI (n = 35) AI (n = 116) None 6 99 Burn 1 - Minor HI 3 16 Trunk bruise 4 - Limb bruise 3 - Head bruise 18 1 Worlock et al, BMJ, 1986

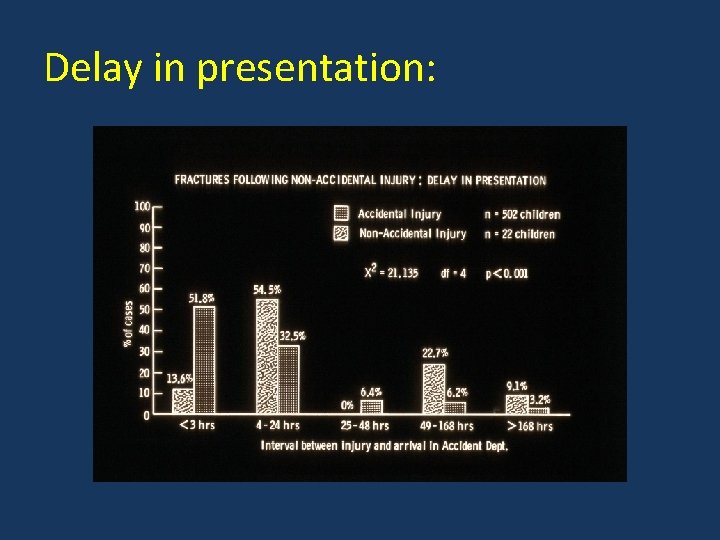
Delay in presentation:

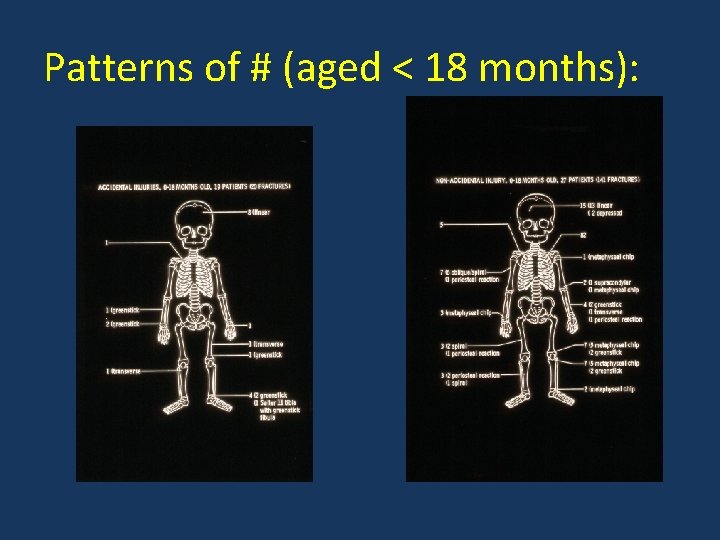
Patterns of # (aged < 18 months):

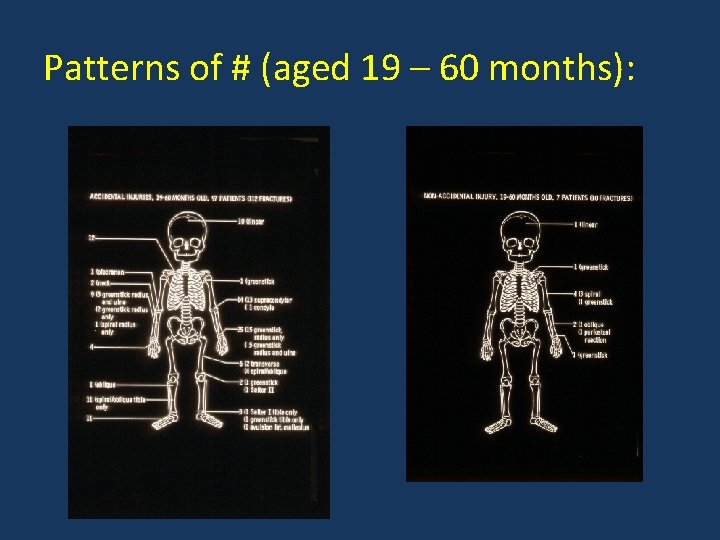
Patterns of # (aged 19 – 60 months):

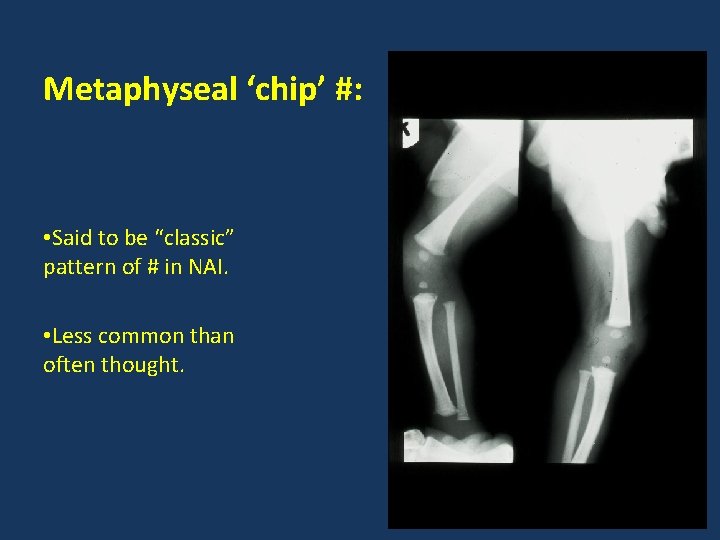
Metaphyseal ‘chip’ #: • Said to be “classic” pattern of # in NAI. • Less common than often thought.

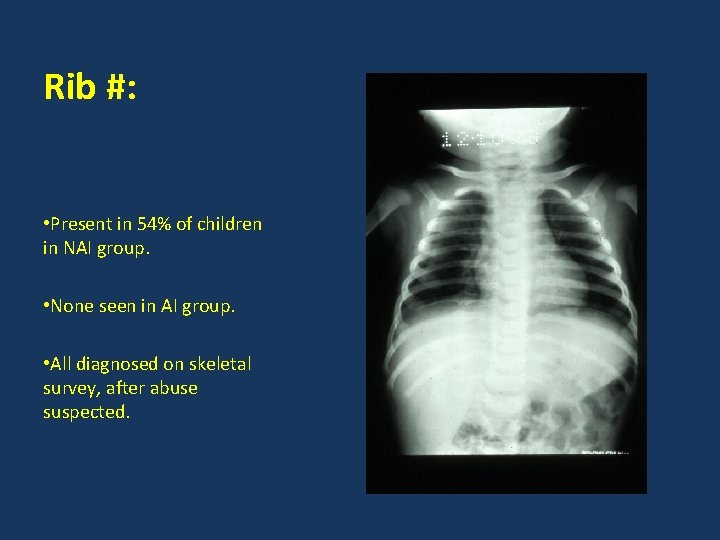
Rib #: • Present in 54% of children in NAI group. • None seen in AI group. • All diagnosed on skeletal survey, after abuse suspected.

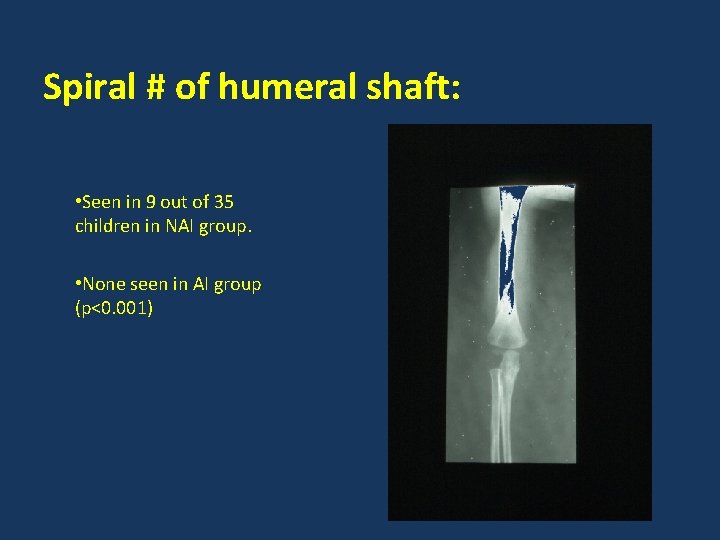
Spiral # of humeral shaft: • Seen in 9 out of 35 children in NAI group. • None seen in AI group (p<0. 001)

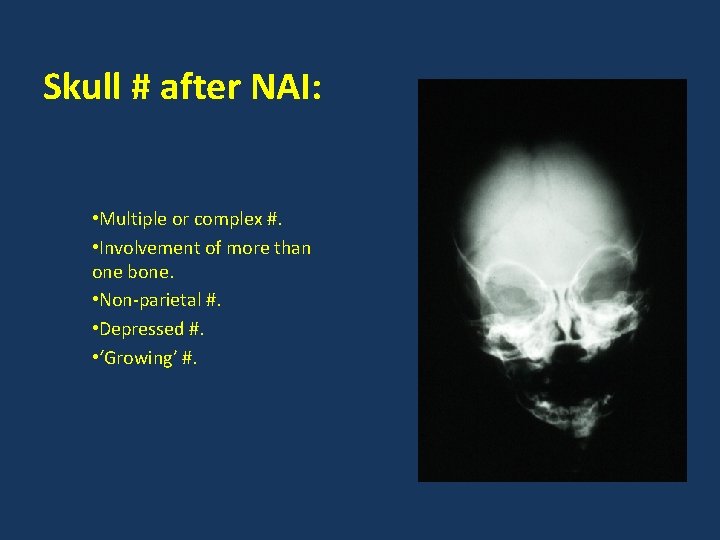
Skull # after NAI: • Multiple or complex #. • Involvement of more than one bone. • Non-parietal #. • Depressed #. • ‘Growing’ #.

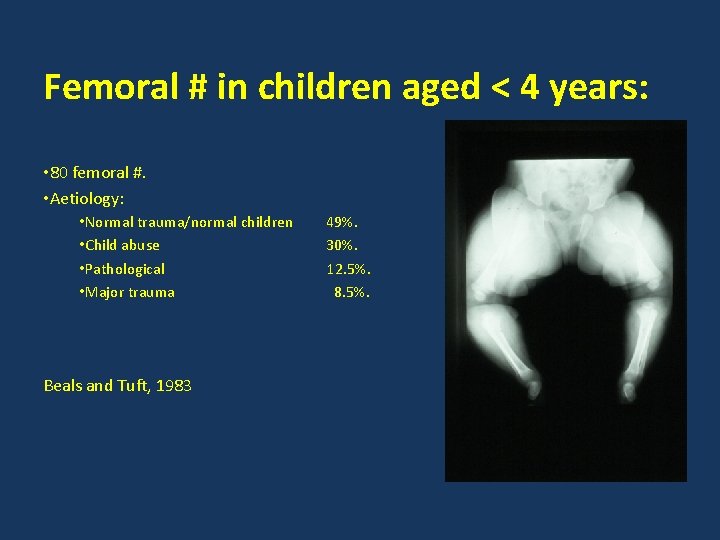
Femoral # in children aged < 4 years: • 80 femoral #. • Aetiology: • Normal trauma/normal children • Child abuse • Pathological • Major trauma Beals and Tuft, 1983 49%. 30%. 12. 5%. 8. 5%.

Risk of injury on falling out of bed: • 76 children fallen from bed, cot or chair. • Height of falls from 1 – 3 ft. • Injuries: – Minor bruise/no injury – Head/face bruise or laceration – Linear skull # – Limb # (in pt with OI) Nimityongskul & Anderson, 1987 63. 5%. 30. 0%. 1. 3%.

NAI and osteogenesis imperfecta: • Type I: autosomal dominant with blue sclera. Most common type. • Type II: autosomal recessive with blue sclera. Lethal in foetal or perinatal period. • Type III: autosomal recessive with normal sclera. Moderate/severe bone fragility with rapidly progressive deformity.

NAI and osteogenesis imperfecta: • Type IV: autosomal dominant, but occasional spontaneous mutation. Normal sclera. Mild/moderate bone fragility with variable deformity. • Rare! Incidence: 1 in 120, 000 live births.

NAI and osteogenesis imperfecta: • Occurrence in absence of blue sclera, no family history and lack of progressive deformity is about 1 in 3, 000 live births. • A city of 500, 000 people with 6000 live births per year would produce one case of Type IV OI by spontaneous mutation every 100 – 300 years. Taitz, BMJ, 1987

Other conditions causing spontaneous # in infancy : • Prematurity. Usually <1500 g at birth, with evidence of rickets and/or osteoporosis on XR. Raised Alk. Phosphatase. • Copper deficiency. Can occur in pre-term babies given Cu-deficient feed, after TPN lacking Cu or in severe malabsorption with Cu-deficient diet. Children with # all have severe haematological abnormalities and osteoporosis on XR.

NAI and the Orthopaedic Surgeon: • # uncommon in normal children < 18 months, but # due to NAI most common in this age group. • 1 child in 8 aged < 18 months with a # may be victim of abuse. • Rib # on skeletal survey, in absence of major chest trauma, is virtually diagnostic of NAI.

NAI and the Orthopaedic Surgeon: • Metaphyseal ‘chip’ # relatively uncommon. • Diaphyseal injuries in NAI are due to gripping/twisting – spiral # or periosteal new bone formation. • You need to be able to recognise unusual injury patterns.

NAI and the Orthopaedic Surgeon: • Be prepared to initiate investigation. • Know your own hospital’s procedure for investigating suspected NAI. • Do not accuse parents – leave interviewing family to the experts. • Children’s Act 1992 – safety and well-being of the child is paramount.