Pre Admission Education Session National Orthopaedic Hospital Cappagh











































- Slides: 54

Pre Admission Education Session National Orthopaedic Hospital Cappagh

Welcome

Welcome You have chosen to have a joint replacement to relieve your pain and to improve your mobility. The aim of today is to explain the importance of planning ahead and preparing yourself and your family for your operation. Topics for discussion: § Preparing for Surgery § Discharge Planning § Your Hospital Stay § Potential Complications

Preparing yourself for Surgery

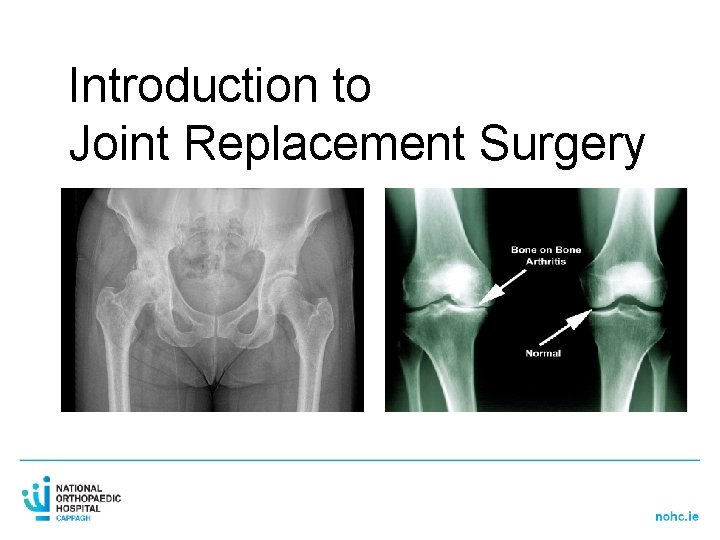
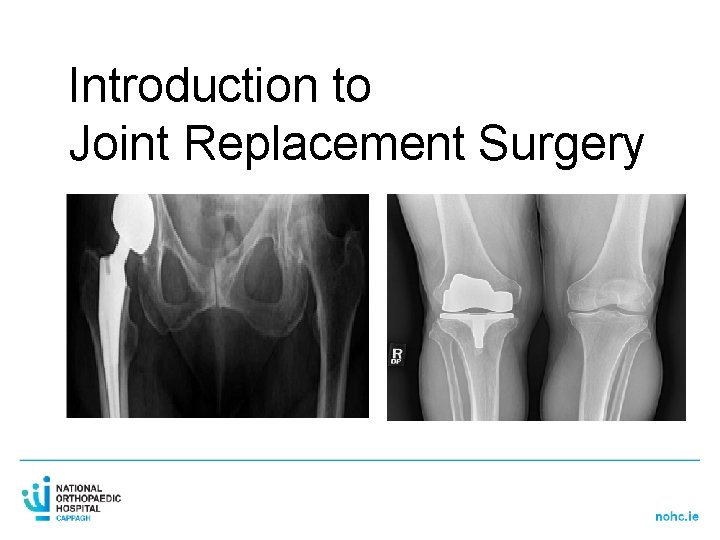
Introduction to Joint Replacement Surgery

Introduction to Joint Replacement Surgery

Irish National Orthopaedic Register (INOR) § Helps assist surgeons to decide which joint replacements are performing well § Aims to improve the quality of services, safety and care § INOR will collect and record your personal information and details of your surgery and implants § You must complete a questionnaire today § Followed up 6 months after your surgery and at 2 and 5 year intervals in a nurse led clinic

Bone Bank § The National Bone Bank was established in 1996 to retrieve bone from suitable consenting donors undergoing total hip replacement surgery § During total hip replacement surgery the damaged femoral head is removed to allow the new hip to be fitted, this bone is often suitable to be used as bone graft § Bone graft is used to strengthen or replace lost bone for another patient during their surgery § The Bone Bank co-ordinators, Eimear and Ken will meet with suitable, potential bone donors and invite them to participate in the bone donor programme

What you need to do

What you need to do § Organise your lift to and from Hospital § Remember you may be discharged from day 1 onwards § Arrange help for home, if you need it (e. g. washing feet, putting on shoes/socks etc. ) § You may want to ask a friend or relative to stay for a few nights after discharge

What you need to do § It is important that you plan for discharge before you come into hospital § Your discharge date will be decided by the team of Health Care professionals caring for you in discussion with you and your family. This normally occurs when you have reached your goals such as distance you can walk or that your wound is healing well § Patients generally return to their own homes after discharge from hospital as they typically do better in their own familiar environment § In exceptional circumstances there may be times when there are challenges for a patient to return home after surgery. If you think you may be unsuitable for discharge home please inform us today as this will give the team time to assist you in planning for your discharge home

What you need to do § You should stop smoking at least four weeks prior to your surgery § Speak to your GP for smoking cessation advice § Reduce Alcohol intake

Stop smoking § There is strong evidence of high risks and worse surgical outcomes when a patient continues to smoke § Higher risk of chest infection and heart complications § Higher risk of post-operative infection § Have impaired would healing § Require longer hospital stay and high drug doses

Maintain a healthy weight This is one of the most effective things you can do to reduce the symptoms of arthritis If you are overweight losing just 10% of your body weight can reduce your pain levels by up to 50%

Maintain a healthy weight Walking transmits x 3 – 5 times body weight across the hip and knee joint. It has been estimated that over-eating just 60 calories a day will lead to obesity in 10 years!

What you need to do § Any exercise you do is beneficial. It is proven that increasing exercise before an operation improves your fitness and recovery. It also makes you feel happier and healthier. § Examples of exercise – Swimming, walking, cycling, dancing § Aim for 20 mins each day

Dress for success Loose comfortable clothes and trainers for the day Long night dress or loose pyjamas are best for night time Light dressing gown Comfortable shoes – without a heel!

Eating and Drinking § Please eat & drink as normal § Have a good meal the night before surgery § No food after 12 midnight water up until 0600 hours (unless you are instructed otherwise) § If you eat and drink after these cut off times your surgery will be cancelled § Please ensure you are not constipated prior to your admission

Your stay at hospital

Admission day § Admitted to St Catherine’s Ward (Admissions Ward) § Shower at home § Clean clothes § Please let us know as soon as possible if you feel unwell § No valuable items or large sums of money

Theatre and recovery § § § Spinal Anaesthetic Approximately 2 hours in theatre Recovery room after surgery for close monitoring Pain relief if required Porter and nurse will transfer you to ward

Back to the ward post surgery § Drip/oxygen § Dressing to hip bulky dressing to knee § Fluids and antibiotics § Regular pain relief and anti nausea § Pain score § Sips of water § Get up walking in afternoon § Visiting hours 2 -4 and 6. 30 to 8 pm

Day 1 and 2 Post Op § § § § Get dressed in your comfortable clothes Physio X-ray Aim to sit out for your meals Shower when the nurse advises its safe to do Bloods Surgical Team will review Drip will be removed and oxygen discontinued

Potential Complications

Risk of surgery § § § Joint Infection Chest infection Deep vein thrombosis (DVT) – Leg Clot Pulmonary embolism (PE) – Lung Clot Constipation Difficulty passing urine Your anaesthetist and Surgeon will discuss other serious potential complications

Reducing Infection § § § Shower before admission Keep visitors to a minimum Patient and relatives to use hand gel on ward Eat and drink well Stop smoking

Avoiding chest infection § Stop smoking § Deep breathing exercises hourly § Sit out or up in bed as soon as possible after surgery

Reducing the risk of leg/lung clot

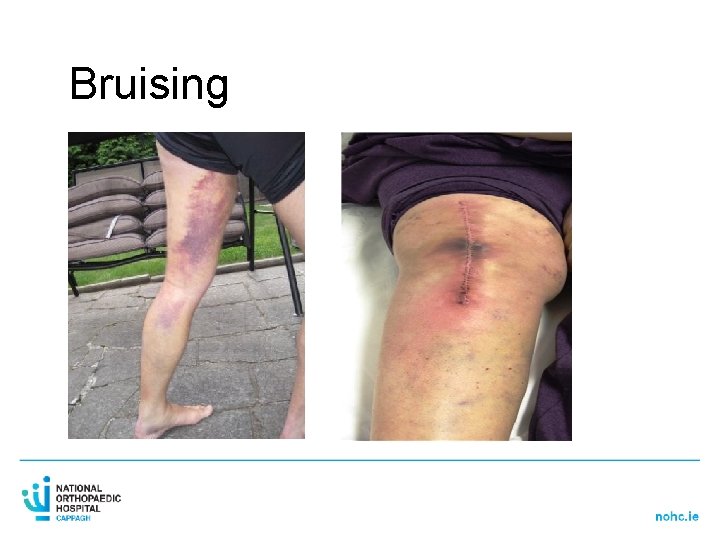
Bruising

Discharge Planning

Discharge advice § § § § Eat and drink well Take medication as advised Some form of exercise every 2 hours Exercises (10 of each, 3 times a day) Apply ice - 15 minutes max, every two hours Arrange appointment with the nurse at GP practice Review 6 weeks & INOR 6 months post op

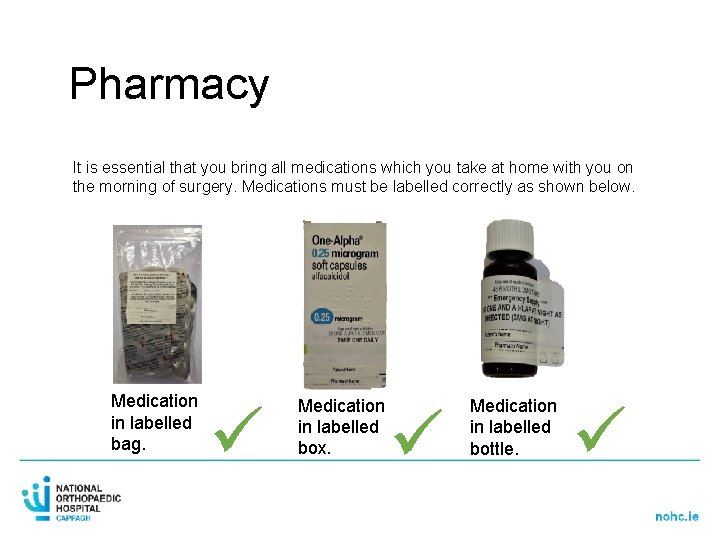
Pharmacy It is essential that you bring all medications which you take at home with you on the morning of surgery. Medications must be labelled correctly as shown below. Medication in labelled bag. Medication in labelled box. Medication in labelled bottle.

Pharmacy Medication presented like those shown in the photographs below causes confusion and may result in your surgery being cancelled Blister packs X Pill box x Loose or unlabelled cards X

Pharmacy § If you are taking any over the counter medications these may not be labelled, but please present these medications in their original packs to the pharmacist on the morning of surgery. § Some medications will need to be stopped a number of days prior to surgery. If this is relevant to you, you will be advised of this in the preassessment clinic.

Pharmacy § Do not take any medication before coming to hospital on the morning of surgery. A pharmacist will assess which medications should be taken before surgery when you arrive on St Catherine’s ward. § To ensure your medications are presented in the correct format please present the yellow sheet in your folder entitled ‘Bring your medicines into hospital on admission’ to your usual community pharmacy.

Physiotherapy helps restore movement and function when someone is affected by injury, illness or disability.

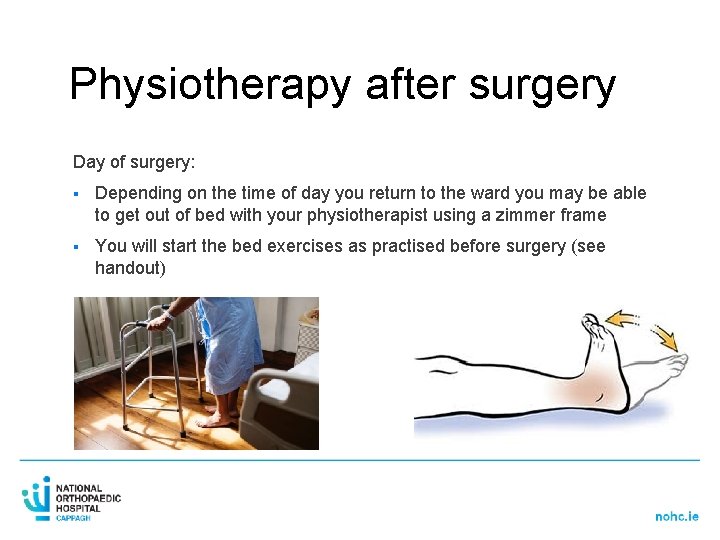
Physiotherapy after surgery Day of surgery: § Depending on the time of day you return to the ward you may be able to get out of bed with your physiotherapist using a zimmer frame § You will start the bed exercises as practised before surgery (see handout) – Depending on the time of day you return to the ward you may be able to get out of bed with your physiotherapist using a zimmer frame – You will start the bed exercises as practised before surgery (see handout)

Physiotherapy after surgery Day 1 onwards: You will be seen by the physiotherapist for : § Progression to crutches/ sticks as able § Completion of exercises § Stair practice as required § You will be encouraged to practice your mobility and exercise programme independently or with a nurse as advised by your physiotherapist

Benefits of early mobilisation and discharge § § § § Less time in hospital Less risk of hospital acquired infections Fewer complications and readmissions Planned earlier rehabilitation Faster recovery Eat better at home Sleep better at home

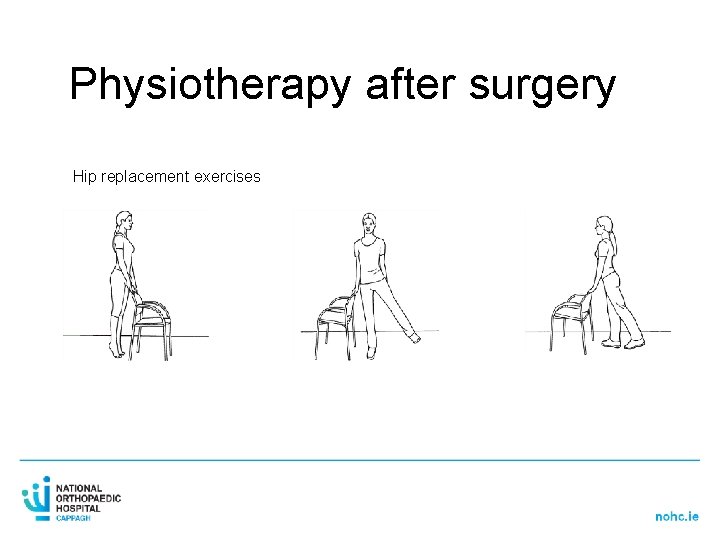
Physiotherapy after surgery Hip replacement exercises

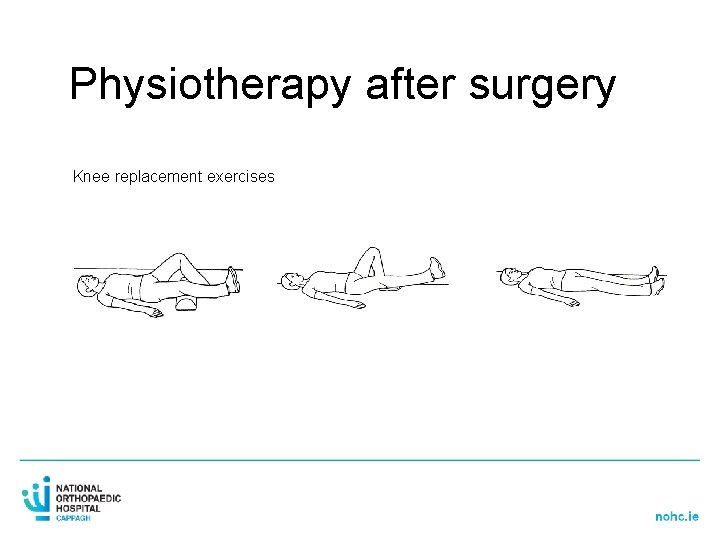
Physiotherapy after surgery Knee replacement exercises

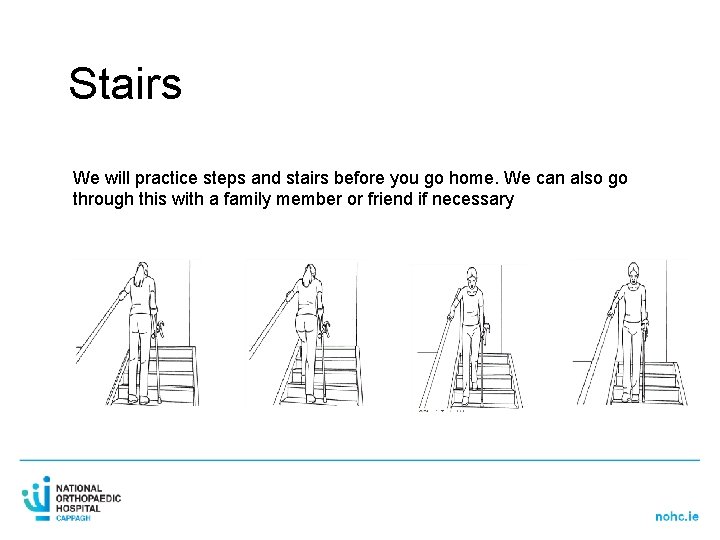
Stairs We will practice steps and stairs before you go home. We can also go through this with a family member or friend if necessary

Goals to be achieved Prior to discharge the following goals will need to be achieved: § Independent and safe on sticks/crutches § Independent and safe on stairs § Independent with exercises § Practise transfers – in/out bed, on/off chairs – – Independent and safe on sticks/crutches Independent and safe on stairs Independent with exercises Practise transfers – in/out bed, on/off chairs

Will I need therapy after I go home? § § § You will continue with your exercises and walking after you go home Physiotherapy is only routinely arranged for patients who have undergone a total knee replacement Follow up physiotherapy will be arranged on discharge

Occupational therapy Occupational Therapists can assess how you will manage their everyday activities of daily living within your home environment such as: § washing and dressing, § getting around indoors and outdoors, § bathing, § preparing and eating meals, § participating in work, Following your surgery, you will be encouraged by all staff to be as independent as possible with tasks. If you are having difficulties, an OT can problem solve with you how to overcome these.

Occupational Therapy Following a total hip replacement you will be seen on the ward by the OT Assistant for the following: § Education on managing daily activities (washing, dressing, toileting etc). § For those undergoing a Primary Total Hip Replacement, there are no longer hip precautions in place. § The OT assistant will review you to determine what equipment, if any, you need to complete dressing and toileting independently. Shoe horn Sock aid Easy Reacher Raised toilet seat

Washing and dressing Recommendations: § Initially strip wash – you may need a chair to perch on when washing § If you have a level access shower and you feel able to stand for long enough you can use this § You can use a shower with step access BUT Do you feel you can manage the step? (It will be slippery after your shower) § Are you able to stand for duration? § Can someone assist legs and feet/long handed equipment? Shower Chair Long-handled sponge

Activities Driving: § No driving for 6 weeks following surgery Flying: § Check with your consultant at 6 week appointment Journeys: § Regular rest breaks to keep the joint moving. § Sit in the front passenger seat of the car and push the seat back. Active hobbies § Can be discussed with your therapist

Medical Social Work § Medical Social Workers can assist with any social or emotional issues that may arise as a result of hospital admission. § Discharge planning is a multi disciplinary assessment. § Supports/Services in the community are needs based an assessment is required. § Information is available on private home care agencies if required. § Please tell a member of staff today if you have any concerns and want to speak to a social worker.

Planning for your recovery at home Meals: § Stock the freezer, enquire about local meals on wheels, Wiltshire Farm Foods Shopping: § Consider getting shopping delivered or asking for help from family/ friends/ neighbours TEDs for hips: § You will need help to change these 2 -3 times a week for up to 6 weeks

Enjoy your life with your new joint Billy Joel Elizabeth Taylor Arnold Schwarzenegger Andy Murray

Medical Social Work § Medical Social Workers can assist with any social or emotional issues that may arise as a result of hospital admission. § Discharge planning is a multi disciplinary assessment. § Supports/Services in the community are needs based an assessment is required. § Information is available on private home care agencies if required. § Please tell a member of staff today if you have any concerns and want to speak to a social worker.

Thank you Looking forward to seeing you soon. Any Questions?
