Infectious Disease I Central Nervous System Infections Courses







































- Slides: 44

Infectious Disease I: Central Nervous System Infections Courses in Therapeutics and Disease State Management Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Learning Objectives (Slide 1 of 3) • Define meningitis and encephalitis • List, in order of relative incidence, the most common age-dependent bacterial causes of meningitis, and identify the fatality rate associated with each • Analyze laboratory values of CSF components and describe the values as normal or as indicative of a specific infective condition • Identify the common signs and symptoms of bacterial meningitis • Select appropriate empirical therapy directed against suspected bacterial meningitis according to age group Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Learning Objectives (Slide 2 of 3) • List the antibiotic of first choice and alternatives to treat meningitis secondary to Streptococcus pneumoniae, Neisseria meningitidis, and Haemophilus influenzae • Identify general principles of chemoprophylaxis after exposure to H. influenzae and N. meningitidis index cases • List the physiochemical properties associated with increased penetration of antibiotics into the CNS • Classify antibiotics according to level of penetration into the CNS • List three reasons why corticosteroid use in bacterial meningitis is controversial Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Learning Objectives (Slide 3 of 3) • Assess the value of dexamethasone as adjunctive therapy in meningitis • Discuss the role vaccination plays in the prevention of meningitis and what impact vaccination is having on the epidemiology of meningitis • Select appropriate antifungal therapy to treat Cryptococcus neoformans • List the viruses most commonly associated with encephalitis and meningoencephalitis and provide recommendations for therapy as appropriate Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Required Reading • Elshaboury RH, Hermsen ED, Holt JS, Mitropoulos IF, Rotschafer JC. Chapter 84. Central Nervous System Infections In: Di. Piro JT, Talbert RL, Yee GC, Matzke GR, Wells BG, Posey L. eds. Pharmacotherapy: A Pathophysiologic Approach, 9 e. New York, NY: Mc. Graw-Hill; 2014. • Tunkel AR, Hartman BJ, Kaplan SL, et. al. . 2004. Practice guidelines for the management of bacterial meningitis. Clin. Infect. Dis. 39: 1267 -1284. • Tunkel AR, Hasbun R, Bhimraj A, et. al. . 2017 Infectious Diseases Society of America’s Clinical Practice Guidelines for Healthcare. Associated Ventriculitis and Meningitis. Clin Infect Dis 2017; 64 (6): e 34 -e 65. Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

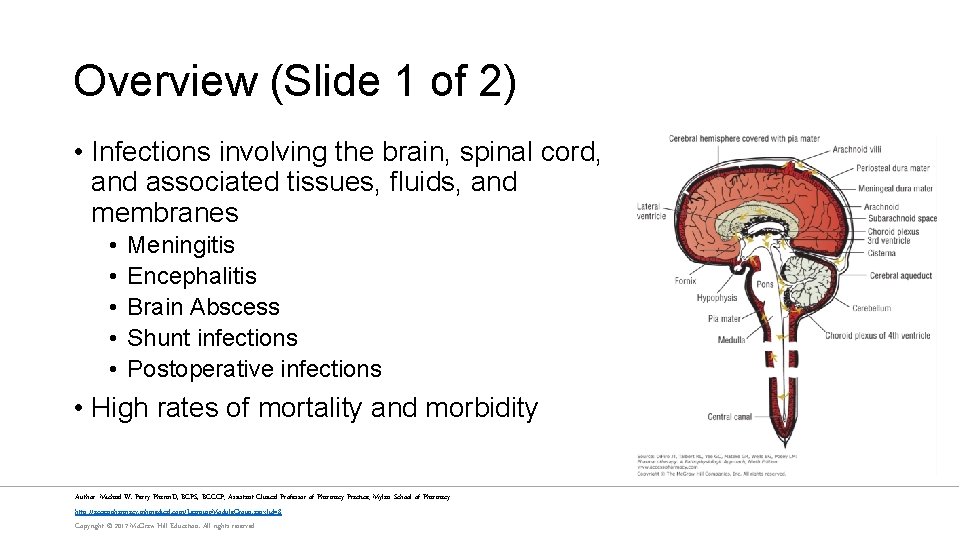
Overview (Slide 1 of 2) • Infections involving the brain, spinal cord, and associated tissues, fluids, and membranes • • • Meningitis Encephalitis Brain Abscess Shunt infections Postoperative infections • High rates of mortality and morbidity Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Overview (Slide 2 of 2) • Community Acquired Meningitis • Healthcare-associated Ventriculitis and Meningitis • • • Cerebrospinal fluid (CSF) shunts CSF drains Intrathecal infusion pumps Deep brain stimulation hardware Neurosurgery or Head Trauma Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Pathophysiology • Blood Brain Barrier • Pathogen gain entry to the CNS • • Contiguous spread Hematogenous seeding Direct inoculation Reactivation of a latent infection • Damage occurs due to immune response to bacterial cellular components Schematic representation of a blood– cerebrospinal fluid barrier capillary, brain tissue capillary, and normal tissue capillary. Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

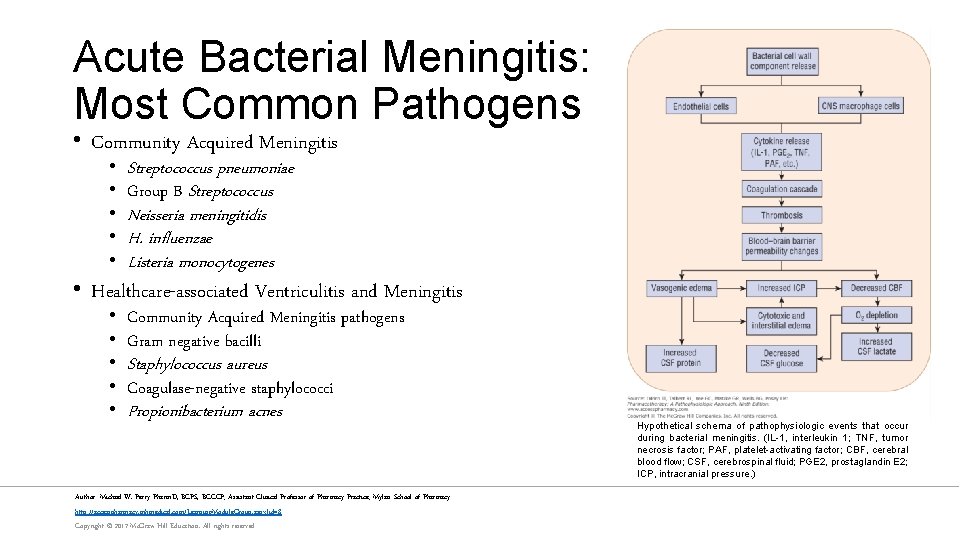
Acute Bacterial Meningitis: Most Common Pathogens • Community Acquired Meningitis • • • Streptococcus pneumoniae Group B Streptococcus Neisseria meningitidis H. influenzae Listeria monocytogenes • Healthcare-associated Ventriculitis and Meningitis • • • Community Acquired Meningitis pathogens Gram negative bacilli Staphylococcus aureus Coagulase-negative staphylococci Propionibacterium acnes Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved Hypothetical schema of pathophysiologic events that occur during bacterial meningitis. (IL-1, interleukin 1; TNF, tumor necrosis factor; PAF, platelet-activating factor; CBF, cerebral blood flow; CSF, cerebrospinal fluid; PGE 2, prostaglandin E 2; ICP, intracranial pressure. )

Clinical Presentation, Signs and Symptoms (Slide 1 of 2) • • • Headache Fever Nuchal rigidity Altered mental Status Nausea • Focal neurological deficits • Brudzinski’s sign • Kernig’s sign • Seizures • Photophobia • Skin lesions • Petechial rash • Neonates • • Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved Altered feeding/ sleeping Bulging fontanel Seizures Irritability/ lethargy

Clinical Presentation, Signs and Symptoms (Slide 2 of 2) Link: Schematic of Brudzinski’s signs Link: Schematic of Kernig’s sign Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Laboratory Tests • Lumbar Puncture • • Opening Pressure CSF composition CSF gram stain CSF culture • Blood Cultures • Scraping of skin lesions • WBC Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved • Cranial Imaging • Magnetic resonance imaging (MRI) • Computed tomography (CT) scan

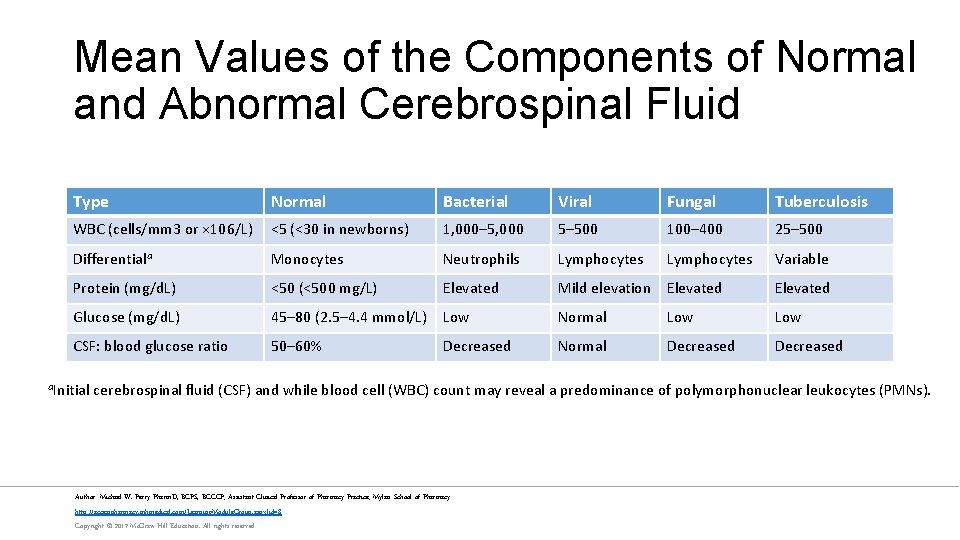
Mean Values of the Components of Normal and Abnormal Cerebrospinal Fluid Type Normal Bacterial Viral Fungal Tuberculosis WBC (cells/mm 3 or × 106/L) <5 (<30 in newborns) 1, 000– 5, 000 5– 500 100– 400 25– 500 Differentiala Monocytes Neutrophils Lymphocytes Variable Protein (mg/d. L) <50 (<500 mg/L) Elevated Mild elevation Elevated Glucose (mg/d. L) 45– 80 (2. 5– 4. 4 mmol/L) Low Normal Low CSF: blood glucose ratio 50– 60% Decreased Normal Decreased a. Initial cerebrospinal fluid (CSF) and while blood cell (WBC) count may reveal a predominance of polymorphonuclear leukocytes (PMNs). Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Goals of Therapy • Prevent Death • Prevent residual neurological deficits • Eradicate or control invading organism by starting appropriate antimicrobial therapy • Ameliorate clinical signs and symptoms • Provide supportive care • Prevent future infections through timely introduction of vaccination and chemoprophylaxis Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Nonpharmacological Treatment • Respiratory and Circulatory Support as needed Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Pharmacological Treatment • Early administration of appropriate antimicrobial therapy • Antimicrobial agents must have sufficient CNS penetration • Initial empiric antimicrobial therapy based on patient specific factors • Focused and targeted antimicrobial therapy once pathogen identified • Supportive Care • • Fluids Electrolytes Antipyretics Analgesics Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

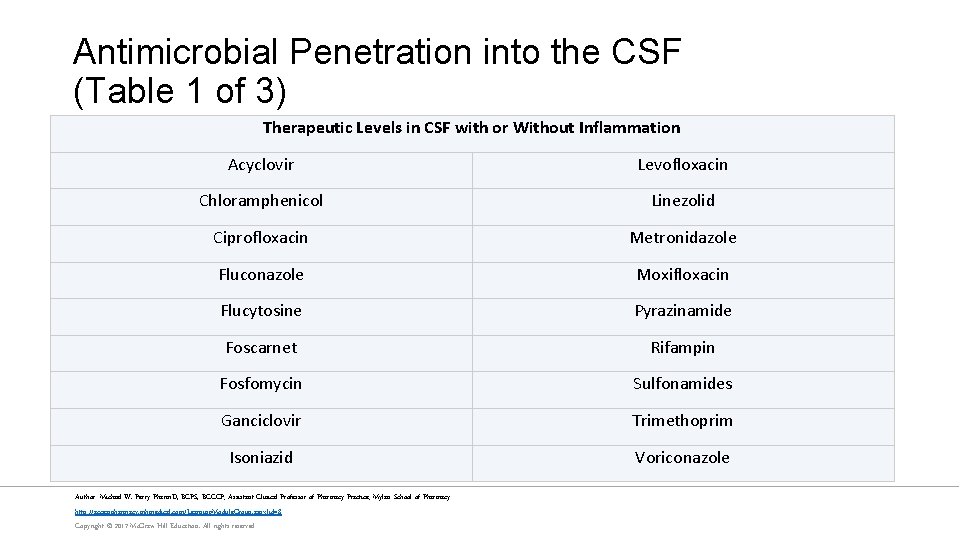
Antimicrobial Penetration into the CSF (Table 1 of 3) Therapeutic Levels in CSF with or Without Inflammation Acyclovir Levofloxacin Chloramphenicol Linezolid Ciprofloxacin Metronidazole Fluconazole Moxifloxacin Flucytosine Pyrazinamide Foscarnet Rifampin Fosfomycin Sulfonamides Ganciclovir Trimethoprim Isoniazid Voriconazole Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

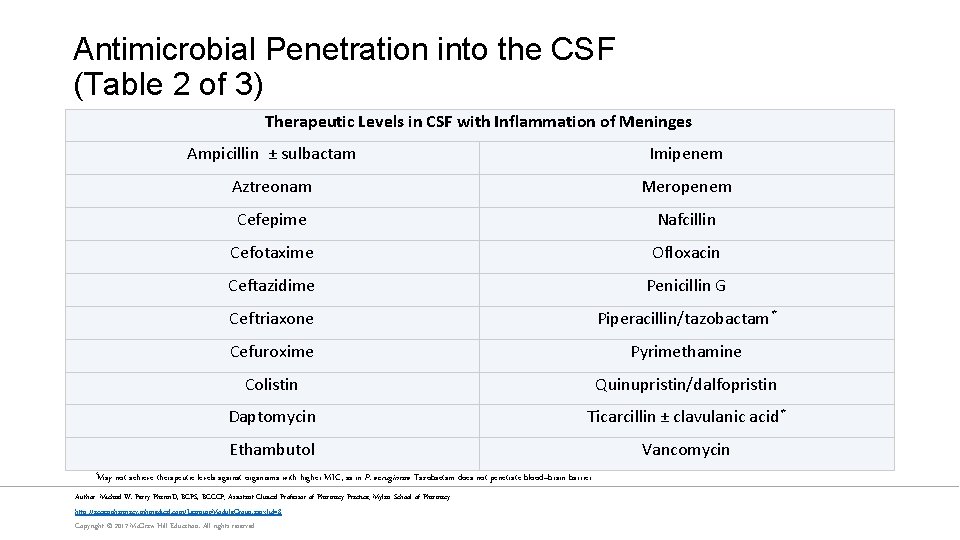
Antimicrobial Penetration into the CSF (Table 2 of 3) Therapeutic Levels in CSF with Inflammation of Meninges *May Ampicillin ± sulbactam Imipenem Aztreonam Meropenem Cefepime Nafcillin Cefotaxime Ofloxacin Ceftazidime Penicillin G Ceftriaxone Piperacillin/tazobactam* Cefuroxime Pyrimethamine Colistin Quinupristin/dalfopristin Daptomycin Ticarcillin ± clavulanic acid* Ethambutol Vancomycin not achieve therapeutic levels against organisms with higher MIC, as in P. aeruginosa. Tazobactam does not penetrate blood–brain barrier. Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Antimicrobial Penetration into the CSF (Table 3 of 3) Nontherapeutic Levels in CSF with or Without Inflammation Aminoglycosides Cephalosporins (second generation)ⱡ Amphotericin B Doxycycline◊ β-Lactamase inhibitors□ Itraconazole∆ Cephalosporins (first generation) ⱡCefuroxime is an exception. effectiveness for Borrelia burgdorferi. □Includes clavulanic acid, sulbactam, and tazobactam. ∆ Achieves therapeutic concentrations for Cryptococcus neoformans therapy. ◊Documented Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Empiric Therapy: Most Common Pathogens by Age (Slide 1 of 4) • Less than 1 months old • Pathogens • • • S. agalactiae E. coli Klebsiella pneumoniae Enterobacter spp. Listeria monocytogenes • Empiric Antibiotics • Ampicillin IV plus cefotaxime IV or ampicillin IV plus aminoglycoside IV Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Empiric Therapy: Most Common Pathogens by Age (Slide 2 of 4) • 1 -23 months old • Pathogens • • Streptococcus pneumoniae Neisseria meningitidis H. influenzae S. agalactiae • Empiric Antibiotics • Vancomycin IV plus third-generation cephalosporin IV (cefotaxime or ceftriaxone) Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Empiric Therapy: Most Common Pathogens by Age (Slide 3 of 4) • 2 -50 years • Pathogens • Neisseria meningitidis • Streptococcus pneumoniae • Empiric Antibiotics • Vancomycin IV plus third-generation cephalosporin IV (cefotaxime or ceftriaxone) Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Empiric Therapy: Most Common Pathogens by Age (Slide 4 of 4) • > 50 years • Pathogens • • • Neisseria meningitidis Streptococcus pneumoniae Listeria monocytogenes E. coli Klebsiella pneumoniae Enterobacter spp. • Empiric Antibiotics • Ampicillin IV plus third-generation cephalosporin IV (cefotaxime or ceftriaxone) plus vancomycin IV Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Empiric Therapy: Most Common Pathogen Healthcare-associated Ventriculitis and Meningitis • Pathogens • • • Community Acquired Meningitis pathogens Gram negative bacilli Staphylococcus aureus Coagulase-negative staphylococci Propionibacterium acnes Empiric Antibiotics • Vancomycin IV or Linezolid IV plus ceftazidime IV or cefepime IV, or meropenem IV Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Streptococcus pneumoniae Targeted Therapy (Slide 1 of 3) • Penicillin MIC < 0. 1 mg/L • Standard Therapy • Penicillin G 4 million units IV Q 4 H • Ampicillin 2 gm IV Q 4 H • Alternate Therapies • Ceftriaxone 2 gm IV Q 12 H • Cefotaxime 2 gm IV Q 4 H • True β-lactam Allergy • Chloramphenical 50 -100 mg/kg/day in divided doses every 6 hours; max daily dose: 4 g/day • Duration of treatment • 10 -14 days Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Streptococcus pneumoniae Targeted Therapy (Slide 2 of 3) • Penicillin MIC 0. 1 -1 mg/L • Standard Therapy • Ceftriaxone 2 gm IV Q 12 H • Cefotaxime 2 gm IV Q 4 H • Alternate Therapies • Meropenem 2 gm IV Q 8 H • Cefepime 2 gm IV Q 8 H • True β-lactam Allergy • Chloramphenical 50 -100 mg/kg/day in divided doses every 6 hours; max daily dose: 4 g/day • Duration of treatment • 10 -14 days Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Streptococcus pneumoniae Targeted Therapy (Slide 3 of 3) • Penicillin MIC > 2 mg/L or Ceftriaxone MIC ≥ 1 • Standard Therapy • Ceftriaxone 2 gm IV Q 12 H PLUS Vancomycin • Cefotaxime 2 gm IV Q 4 H PLUS Vancomycin • Alternate Therapies • Moxifloxacin 400 mg IV q 24 H • Duration of treatment • 10 -14 days Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Neisseria meningitidis Targeted Therapy (Slide 1 of 2) • Penicillin MIC < 0. 1 mg/L • Standard Therapy • Penicillin G 4 million units IV Q 4 H • Ampicillin 2 gm IV Q 4 H • Alternate Therapies • Ceftriaxone 2 gm IV Q 12 H • Cefotaxime 2 gm IV Q 4 H • Chloramphenical 50 -100 mg/kg/day in divided doses every 6 hours; max daily dose: 4 g/day • Duration of treatment • 7 -10 days Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Neisseria meningitidis Targeted Therapy (Slide 2 of 2) • Penicillin MIC 0. 1 -1 mg/L • Standard Therapy • Ceftriaxone 2 gm IV Q 12 H • Cefotaxime 2 gm IV Q 4 H • Alternate Therapies • Meropenem 2 gm IV Q 8 H • Cefepime 2 gm IV Q 8 H • True β-lactam Allergy • Moxifloxacin 400 IV Q 24 H • Chloramphenical 50 -100 mg/kg/day in divided doses every 6 hours; max daily dose: 4 g/day • Duration of treatment • 7 -10 days Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

H. influenza Targeted Therapy (Slide 1 of 2) • β-lactamase negative • Standard Therapy • Ampicillin 2 gm IV Q 4 H • Alternate Therapies • • Ceftriaxone 2 gm IV Q 12 H Cefotaxime 2 gm IV Q 4 H Cefepime 2 gm IV Q 8 H True β-lactam Allergy • Moxifloxacin 400 IV Q 24 H • Chloramphenical 50 -100 mg/kg/day in divided doses every 6 hours; max daily dose: 4 g/day • Duration of Treatment • 7 -10 days Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

H. influenza Targeted Therapy (Slide 2 of 2) • β-lactamase positive • Standard Therapy • Ceftriaxone 2 gm IV Q 12 H • Cefotaxime 2 gm IV Q 4 H • Alternate Therapies • Cefepime 2 gm IV Q 8 H • True β-lactam Allergy • Moxifloxacin 400 IV Q 24 H • Chloramphenical 50 -100 mg/kg/day in divided doses every 6 hours; max daily dose: 4 g/day • Duration of Treatment • 7 -10 days Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Listeria monocytogenes Targeted Therapy • Standard Therapy • Ampicillin 2 gm IV Q 4 H • Alternate Therapies • Meropenem 2 gm IV Q 8 H • True β-lactam Allergy • Trimethoprim/ Sulfamethoxazole IV • 10 -20 mg TMP/kg/day in divided doses every 6 -12 hours • Duration of Treatment • 21 days Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Methicillin Susceptible Staphylococcus Aureus Targeted Therapy • Standard therapy • Nafcillin or Oxacillin 1. 5 -3 gm IV Q 4 H • Alternate Therapy • Meropenem 2 gm IV Q 8 H • True β-lactam Allergy • Vancomycin • Duration of Treatment • 2 -3 weeks • 4 -6 weeks if shunt involved Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Methicillin Resistant Staphylococcus Aureus Targeted Therapy • Standard Therapy • Vancomycin • Alternate Therapy • Trimethoprim/ Sulfamethoxazole • 10 -20 mg TMP/kg/day in divided doses every 6 -12 hours • Linezolid 600 mg IV Q 12 H • Duration of Treatment • 3 -4 weeks • 4 -6 weeks if shunt involved Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Cryptococcus neoformans Targeted Therapy • Standard Therapy • Amphotericin B combined with flucytosine for 2 weeks • Alternate Therapy • Amphotericin B plus High dose Fluconazole • Amphotericin B plus Voriconazole or Itraconazole • Duration of Treatment • 2 to 6 weeks of induction therapy • 8 weeks of consolidation therapy Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Viral Encephalitis and Meningoencephalitis Targeted Therapy • Common Viruses • Herpes simplex virus • West Nile virus • Enteroviruses • Standard Therapy • Acyclovir 10 mg/kg IV Q 8 H • Alternate Therapy • Foscarnet 120 -200 mg/kg IV per day in divided doses every 8 -12 hours • Duration of Treatment • 14 -21 days Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Dexamethasone • Corticosteroids inhibit the production of pro-inflammatory cytokines • Clinical trial data surrounding the benefits of corticosteroids in meningitis is conflicting • A series trials and systematic review showed steroids may improve neurological and mortality outcomes in adult patients • A larger trial showed conflicting data • Various antimicrobial agents were used • Dexamethasone was administered at different times in relation to the first antimicrobial dose • Patients had varying levels of illness severity • Overall use of corticosteroids in the setting of meningitis is controversial Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Dexamethasone Recommendations • Infants and children • H. influenza: Dexamethasone 0. 15 mg/kg Q 6 H for 2 -4 days • Administer before or concurrently with the first dose of antibiotics • Pneumococcal: not routinely recommended must weigh risk versus benefit • Adults • Pneumococcal: Dexamethasone 10 mg IV Q 6 H for 2 -4 days • Administer before or concurrently with the first dose of antibiotics • Other bacterial causes of meningitis: not routinely recommended Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Evaluation of Outcomes • Monitor the following every 4 hours for 3 days • • • Fever Headache Meningismus Vital signs Acute changes in Mental Status/ Glasgow Coma Scale • Adjust antimicrobial therapy based on microbiologic findings Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Prophylactic Antibiotics (Slide 1 of 2) • Prophylaxis of close contacts should be started only after consultation with the local health department • Close Contacts • • Members of same household Individuals who share the same sleeping quarters Day care contacts Individuals exposed to oral secretions of infected patient Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Prophylactic Antibiotics (Slide 2 of 2) • Neisseria meningitidis • Close contacts • • Rifampin 600 mg PO BID x 2 days Ciprofloxacin 500 mg PO x 1 dose Ceftriaxone 250 mg IM x 1 dose Azithromycin 500 mg PO x 1 dose • H. influenza • Close Contacts • Rifampin 600 mg PO BID x 4 days • Fully vaccinated children do not require prophylactic antibiotics Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Vaccination • Neisseria meningitidis • Meningococcal Polysaccharide Vaccine (Groups A / C / Y and W-135) • Meningococcal (Groups A / C / Y and W-135) Diphtheria Conjugate Vaccine • Meningococcal Group B vaccine • Streptococcus pneumoniae • Pneumococcal Conjugate Vaccines • 7 -valent • 13 -valent • Pneumococcal Polysaccharide Vaccine • 23 -valent • H. influenza • Hib Conjugate vaccine Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

Summary • Meningitis is an infection of the central nervous system with high rates of morbidity and mortality • Early identification of meningitis and early initiations of antibiotics is key to improve outcomes • High doses of antimicrobials that penetrate the CNS are required • Adjust therapy as soon as cultures finalized • Prevention with vaccination and prophylactic antibiotics Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved

References • Elshaboury RH, Hermsen ED, Holt JS, Mitropoulos IF, Rotschafer JC. Chapter 84. Central Nervous System Infections In: Di. Piro JT, Talbert RL, Yee GC, Matzke GR, Wells BG, Posey L. eds. Pharmacotherapy: A Pathophysiologic Approach, 9 e. New York, NY: Mc. Graw-Hill; 2014. • Tunkel AR, Hartman BJ, Kaplan SL, et. al. . 2004. Practice guidelines for the management of bacterial meningitis. Clin. Infect. Dis. 39: 1267 -1284. • Tunkel AR, Hasbun R, Bhimraj A, et. al. . 2017 Infectious Diseases Society of America’s Clinical Practice Guidelines for Healthcare. Associated Ventriculitis and Meningitis. Clin Infect Dis 2017; 64 (6): e 34 -e 65. Author: Michael W. Perry Pharm. D, BCPS, BCCCP; Assistant Clinical Professor of Pharmacy Practice; Mylan School of Pharmacy http: //accesspharmacy. mhmedical. com/Learning. Module. Group. aspx? id=8 Copyright © 2017 Mc. Graw-Hill Education. All rights reserved