Infectious Diseases in Daycare Settings Olmsted County Public

Infectious Diseases in Daycare Settings Olmsted County Public Health Services Family Child Care, Inc. Workshop April 8 th, 2019
Identify • Identify the roles and responsibilities of State and Local Health Departments and Childcare Providers Define • Define common infectious disease terminology Objectives Understand Identify • Understand the basic epidemiology, preventative measures, and exclusion policies for the most commonly transmitted diseases in childcare settings

Minnesota Department of Health • Surveillance • Prevention and Response • Enforcement—Minnesota Communicable Disease Reporting Rule and Minnesota Statutes

Olmsted County Public Health Services • Disease Investigation • Consultation • Disease specifics • Pertussis • Environmental cleaning • Varicella • Preventative measures • Measles • Guidelines • Mumps • GI Outbreaks

Childcare Provider • Have a basic knowledge of the signs and symptoms of common diseases as well as how to prevent and control them • Report diseases to MDH or OCPHS via phone or fax • 507 -328 -7500 (OCPHS); 651 -201 -5414 (MDH) • Develop and enforce an exclusion policy • Sanitize and disinfect commonly touched surfaces • Encourage good handwashing

Epi 101
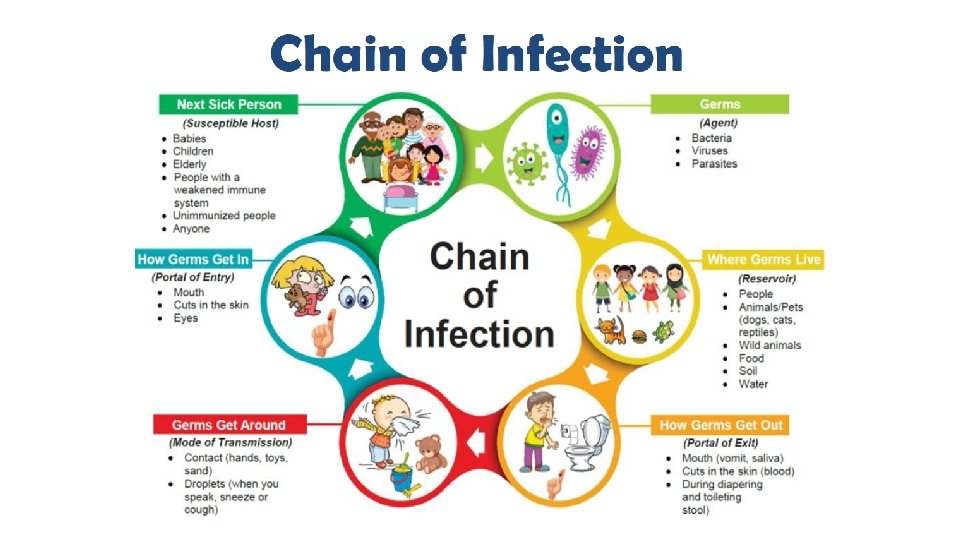

Infectious Disease Terminology • Germ—the thing that causes disease • Bacteria, Viruses, Parasites, Fungi • Transmission (Spread)—how the germs get from one person to another person • Incubation Period—the time from exposure to the germ/sick individual to the start of symptoms • Contagious (Infectious) Period—the timeframe in which a person can spread their illness

Disease is reported to public health Case report initiated Disease Investigation Case (or parent) interviewed Exposure notifications made; interventions put in place [Outbreak investigation initiated]

Case Report—What do we collect? • Who? • Age • Sex/gender • Race/ethnicity • Where? • School, daycare, sports, church groups • When? • Symptom onset • Travel dates • Dates attended activities

Calculating Infectious Period
Exposure Notifications and Interventions • Phone calls and/or letters • Inform of exposure • Education about disease • Action steps Interventions • Environmental cleaning • Exclusion/isolation • Prevention messaging

Common Infectious Diseases in Child Care Settings

Conjunctivitis (Pink Eye) • Germ: • Viruses, bacteria, or allergens • Transmission: • Touching secretions from eyes, nose, or mouth • Incubation: • 1 -3 days usually (1 -12 days) • Symptoms: • Pink/red color in white of the eye(s); swelling of eyelid; watery eye; itching, irritation, and/or burning; discharge; crusting of eyelid or lashes • Duration: • Viral (7 -14 days); Bacterial (2 -5 days); Allergen (once allergen removed) • Contagious Period: • While symptoms are present

Viral • Watery discharge • Starts in one eye and can spread within days to other eye Conjunctivitis: What’s the Difference? Bacterial • Thicker, pus-like discharge • Eyelids stuck together • May occur with ear infection Allergen • Both eyes • Intense itching, tearing, and swelling of eyes • May occur with itchy nose, sneezing, scratchy throat, or asthma

Conjunctivitis (Pink Eye) • Exclusions: • Until seen by doctor if bacterial with thick white or yellow discharge and eye pain • NO exclusion if clear, watery discharge without eye pain or fever • Prevention: • Cover nose and mouth when sneezing or coughing • Do not rub eyes • Do not share towels, eye drops, or other objects that come in contact with the eye • Handwashing • Clean and sanitize/disinfect objects such as toys, tables, door knobs

Head Lice • Germ: • Louse • Transmission: • Head-to-head contact CANNOT jump or fly • Sharing personal products such as combs, brushes, hats, hair ties • Incubation: • 7 -10 days from eggs laid to hatch • Symptoms: • Itching of the head/neck, crawling lice, scratch marks on the head/back of neck • Duration: • 2 weeks • Contagious Period: • Until treated with lice killing products

Head Lice • Exclusions: • None, but recommended to wait until first complete treatment • DO NOT recommend a “No Nit” policy—all lice do not need to be gone • Prevention: • • • Do NOT share hair products, accessories, or towels Vacuum carpets, furniture, mattresses, and car seats thoroughly Wash clothes, pillow cases, towels in hot water and on a hot dryer cycle Un-washables can be sealed in a plastic bag Don’t be surprised if you need to do a second treatment 7 -10 days later

Common Childhood Rashes: Name that Rash
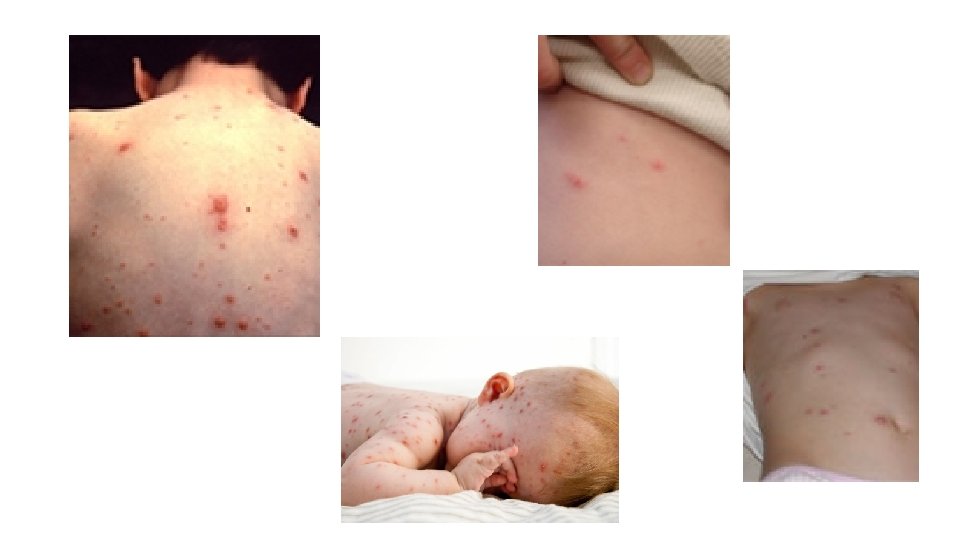

Varicella (Chickenpox)* • Germ: • Duration: • Transmission: • Contagious Period: • Virus • Contact with blister fluid or secretions from the nose or mouth; coughing or sneezing • Incubation: • 10 -21 days after exposure • Symptoms: • Red spots that turn into fluid-filled blisters; itchy; fever; tiredness; loss of appetite; headache • 4 -7 days • 1 -2 days before rash onset until spots are dry and scabbed

Varicella (Chicken Pox)* • Exclusion: • All blisters need to be dry and scabbed over (around 5 days after rash onset) • Prevention: • • Cover nose and mouth when sneezing and coughing Handwashing Clean and disinfect objects and surfaces Vaccination • Dose 1: 12 -15 months • Dose 2: 4 -6 years
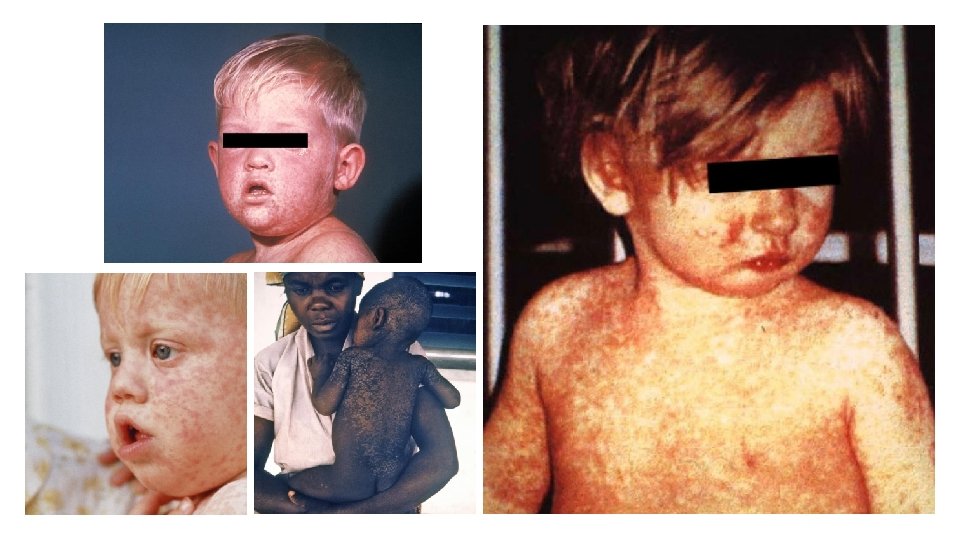

Measles* • Germ: • Virus • Transmission: • Airborne (can stay in air for 2 hours); touching secretions • Incubation: • 10 -21 days (rash usually starts around day 14) • Symptoms: • High fever, cough, runny nose, watery eyes, red/brown rash on 3 rd-7 th day • Duration: • 4 -7 days for rash • Contagious Period: • 4 days prior to rash to 4 days after rash

Measles* • Exclusion: • Until 4 days after onset of rash • If exposed and unvaccinated, exclude for 21 days from LAST exposure. • Unless they received a vaccine within 72 hours or were given immune globulin within 6 days of exposure • Prevention: • Vaccine • Dose 1: 12 months • Dose 2: 4 -6 years • Cover nose and mouth when coughing or sneezing • Handwashing • Clean and sanitize/disinfect surfaces and toys
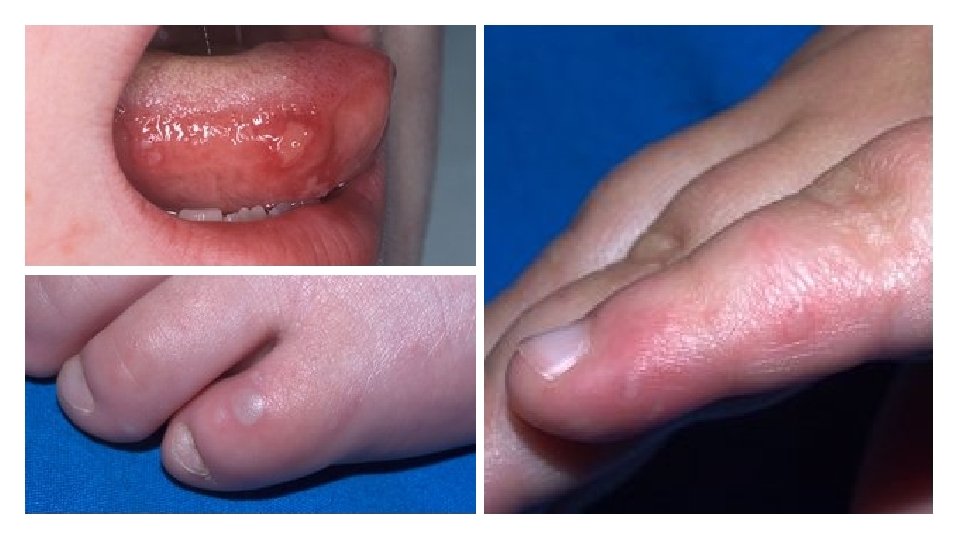

Hand, Foot, and Mouth Disease • Germ: • Duration: • Transmission: • Contagious Period: • Virus • Fecal-oral—contact with stool from an infected person on hands, food, or objects; coughing/sneezing; contact with blisters (RARE) • Incubation: • 3 -6 days • Symptoms: • Fever; reduced appetite; sore throat; small red ulcers in mouth, small red fluid-filled bumps on palms of hands, and soles of feet (knees, elbows, buttocks, genital area) • 7 -10 days • First week of illness most infectious, but can spread for several weeks after symptoms go away

Hand, Foot, and Mouth Disease • Exclusion: • Until 24 hours after fever is gone and can resume routine activity • NOTE: sores and rash may still be present • Prevention: • Cover nose/mouth when sneezing and coughing • Handwashing • Clean and sanitize/disinfect objects and surfaces (toys, diaper changing area, and potty chairs)
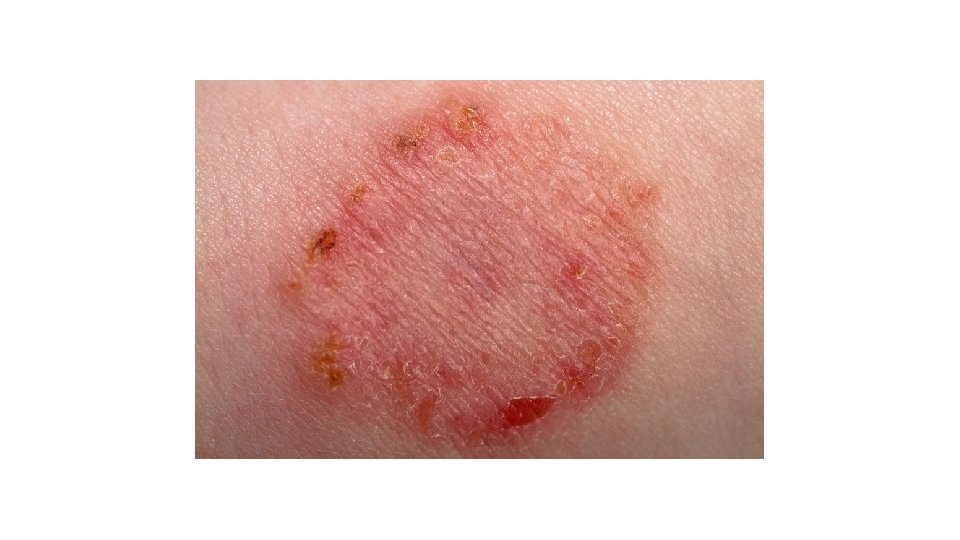

Ringworm • Cause: • Duration: • Transmission: • Contagious Period: • Fungi • Touching rash; sharing objects (hats, combs, towels, pillows, bedding) • Incubation: • 7 -21 days • Symptoms: • Flat, ring-shaped rash; as it spreads, the center becomes clear; itchy; “athletes foot”, patchy scaling or cracking skin on the foot • 2 -4 weeks • 24 -48 hours after treatment

Ringworm • Exclusion: • Until treatment started • No swimming, gym, or other close contact until lesions can be covered or 72 hours after treatment started • Prevention: • Do not share brushes, combs, towels, bedding, hats, etc. . • Handwashing • Have separate bedding and pillows for each child and wash in hot soapy water daily when an individual is infected
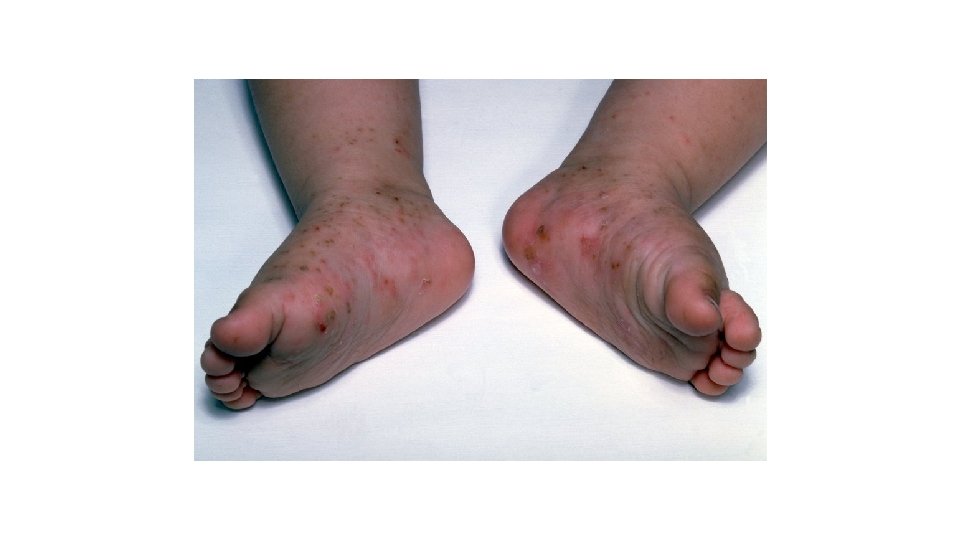

Scabies • Germ: • Mites • Transmission: • Skin-to-skin contact; sharing bedding and towels • Incubation: • 2 -6 weeks • Symptoms: • Tiny red bumps or blisters (usually between fingers, around wrist, elbows, and armpits); intense itching • Duration: • 2 -3 weeks • Contagious Period: • Rash onset until 24 hours after treatment

Scabies • Exclusion: • 24 hours after treatment • Prevention: • Wash bedding and towels in hot water and dry on high heat cycle • Vacuum furniture and carpeting
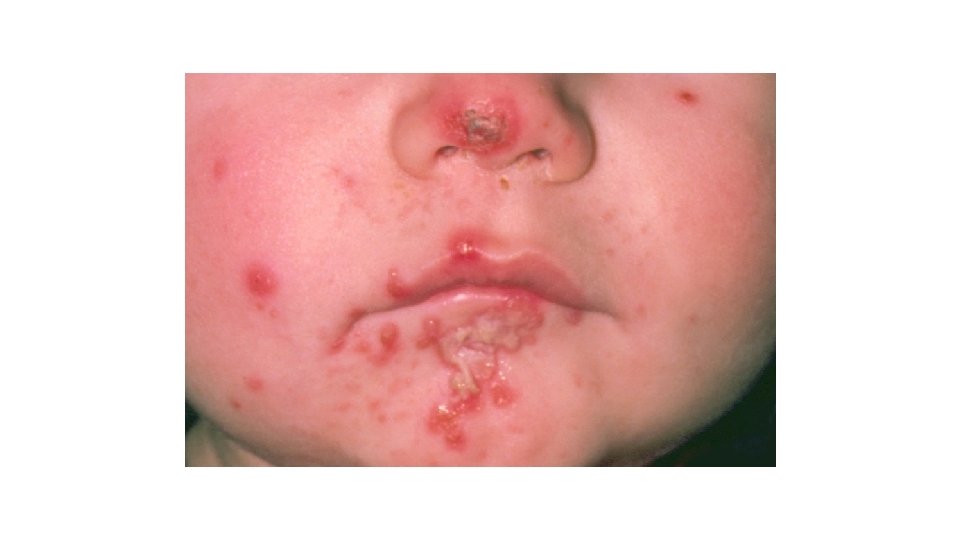

Impetigo • Germ: • Duration: • Transmission: • Contagious Period: • Bacteria • Direct contact with the sores; contact with contaminated objects (RARE) • Incubation: • 1 -10 • Symptoms: • Red sores or blister with crusty brown discharge; itchy • 2 -4 weeks • Until sores are healed or 24 hours after antibiotics started

Impetigo • Exclusion: • 24 hours after antibiotics started and sores drying/improving • Prevention: • • • Handwashing Cover sores Wear gloves when applying medication to the sores Do not share towels, washcloths, or clothing Clean and sanitize/disinfect toys and surfaces
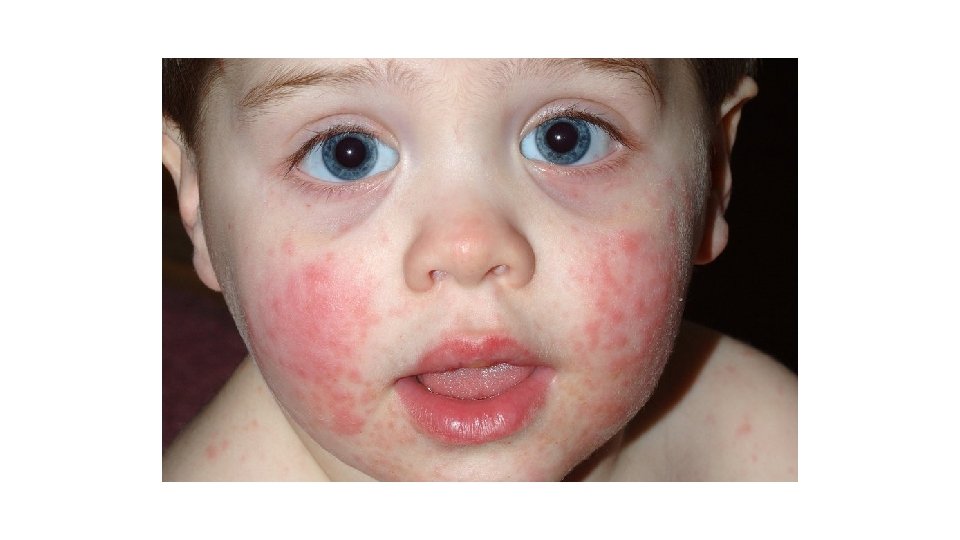

5 th Disease (Slapped Cheek Syndrome) • Cause: • Virus • Transmission: • Coughing or sneezing; touching secretions • Incubation: • 4 -21 days • Symptoms: • Bright red rash on cheeks; fever; sore throat • Duration: • 3 -7 days; may reoccur over several weeks • Contagious Period: • Just before rash onset until rash onset

5 th Disease • Exclusion: • None—no longer infectious once rash begins • Prevention: • Handwashing • Cover nose and mouth when coughing or sneezing • Clean and sanitize/disinfect toys and surfaces

Respiratory: Name that Cough
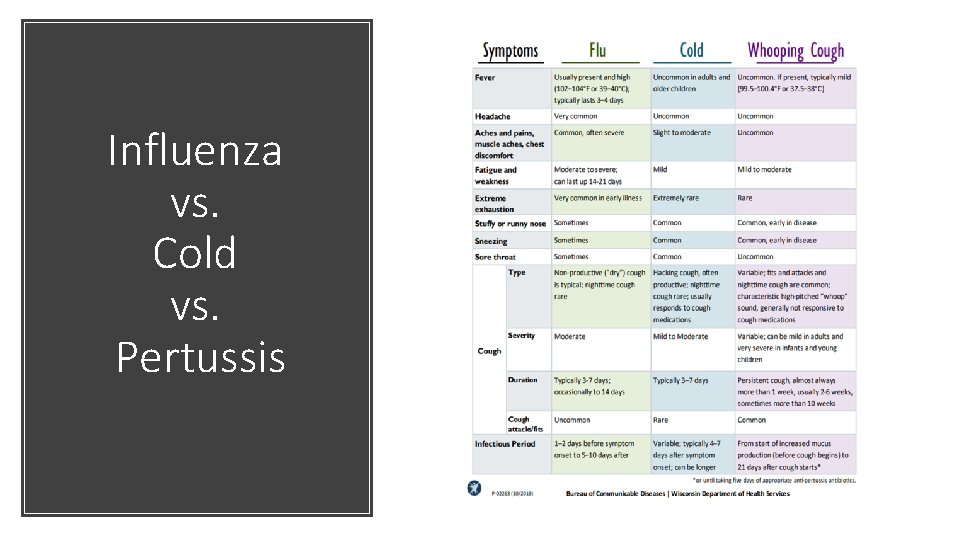
Influenza vs. Cold vs. Pertussis

Influenza • Germ: • Duration: • Transmission: • Contagious Period: • Virus • Coughing or sneezing; touching secretions • Incubation: • 1 -4 days (usually 2) • Symptoms: • Rapid onset of fever, chills, body aches, cough, runny nose, sore throat • 3 -7 days • 1 day before symptoms until symptoms resolve

Influenza • Exclusion: • 24 hours after fever resolves • Child is well enough to perform normal activities • Prevention: • • • Yearly influenza vaccine Cover nose and mouth when coughing or sneezing Handwashing Clean and sanitize/disinfect toys and surfaces Stay home when sick

Pertussis (Whooping Cough)* • Germ: • Bacteria • Transmission: • Coughing, sneezing, talking, and singing; touching secretions • Incubation Period: • 4 -21 days after exposure (usually 7 -10 days) • Symptoms: • Week 1 -2: sneezing, runny nose, lowgrade fever, cough • Symptoms Continued: • Week 2 -6 (up to 10): Coughing in sudden, uncontrollable bursts, highpitched whoop sound following coughing episode, gagging or vomiting after coughing episode, coughing often worse at night • Duration: • weeks to months nicknamed the 100 day cough • Contagious Period: • Cough onset until either 3 weeks after cough onset or until 5 days of antibiotics taken

Pertussis (Whooping Cough)* • Exclusion Policy: • If treated, 5 days antibiotics completed. • If not treated, 3 weeks of coughing has passed. • If exposed AND symptomatic, negative swab or 3 weeks of coughing has passed. • Prevention: • • Vaccine @ 2, 4, and 6 months, 15 -18 months, and 4 -6 years Cover nose and mouth when sneezing and coughing Handwashing Clean and sanitize/disinfect toys and surfaces

Stomach Bugs

Norovirus • Germ: • Virus • Transmission: • Fecal-oral • Incubation: • 12 -48 hours • Symptoms: • Watery diarrhea, vomiting, fever, headache, fatigue, stomach cramps • Duration: • 1 -3 days • Contagious Period: • Symptom onset to 72 hours after symptoms resolve

Norovirus • Exclusion: • 24 hours after last bout of diarrhea or vomiting • Prevention: • Handwashing • Clean and sanitize/disinfect toys and surfaces

E. coli* • Germ: • Bacteria • Transmission: • Fecal-oral • Incubation: • 1 -8 days (usually 3 -4 days) • Symptoms: • Watery diarrhea, stomach cramps, low grade fever; bloody diarrhea (O 157) • Duration: • 5 -10 days • Contagious Period: • Symptom onset until several weeks or months after symptom resolution

E. coli* • Exclusion: • Shiga-toxin producing E. coli (STEC) O 157 or other STEC that produce shiga toxin: Need 2 consecutive negative stool results at least 24 hours apart • Any other E. coli— 24 hours after last bout of diarrhea • Prevention: • Handwashing • Clean and sanitize/disinfect toys and surfaces

C. diff • Germ: • Bacteria • Transmission: • Fecal-oral • Incubation: • 5 -10 days • Symptoms: • Watery diarrhea, fever, loss of appetite, nausea, stomach cramps • Duration: • Varies • Contagious Period: • Unknown—less contagious after symptoms diminish and treatment taken

C. diff • Exclusion: • 24 hours after last bout of diarrhea • Prevention: • Handwashing • Clean and sanitize/disinfect toys and surfaces • Wear gloves when changing diapers and disinfect changing area after each change

Prevention and Control

Cleaning, Sanitizing, and Disinfecting • Cleaning—using soap and water to remove dirt, debris, and many germs • Sanitizing—using a chemical to remove disease-causing germs from food contact surfaces or mouthed toys or objects (Bleach Solution 2) • Disinfecting—using a chemical of stronger concentrations to remove disease-causing germs from non-food contact surfaces (Bleach Solution 1)

Food Safety • • • Healthy food handlers Cold foods cold (<41); Hot foods hot (>140) When in doubt use 165 (cooking, reheating) Consider a metal, tip sensing digital thermometer Cool foods rapidly (or discard left-overs) Keep raw and ready-to-eat foods separated

Handwashing is the single most effective way to prevent the spread of infection!

Gloves

Cover your Cough

Exclusion Policies • Providers should have written exclusion policies • Exclusions vary by disease—refer to technical fact sheets from Hennepin Co • Basic exclusions include: • Fever, Diarrhea, and Vomiting AND 24 hours after • When the child cannot perform normal activities • When a serious contagious illness has been diagnosed • Just because a parent or provider says the child can be in childcare, does not necessarily mean they should be there!

Immunization Policies • Immunization records must be kept in accordance with Minnesota Statutes, section 121 A. 15 • Children should be up to date on Measles, Rubella, Diptheria, Tetanus, Pertussis, Polio, Mumps Haemophilus influenzae type b, and Hepatitis B • OR have a medical or conscientious exemption • You have the responsibility and the right to enforce this State Statute. You can turn children away if not immunized.

Emergency Preparedness Scenario

Emergency Preparedness Scenario • Day 1: • 2 year old child comes in with a cough, sore throat, and runny nose • Parents say it started yesterday and think it is just a cold as she has not had a fever • Around noon, the child develops a fever and is sent home • Day 2: • Parents call you to let you know the child still has a fever and will not be in today

Emergency Preparedness Scenario • Day 3: • Parents call to let you know the child is still and they will be taking her into the doctor today • Day 4: • Olmsted County Public Health calls to notify you that the child was tested and positive for measles

What’s next? • What information do you as the childcare provider need to give to parents? • What do information do you need to give to public health? • What precautions are being implemented? • Are unvaccinated children being allowed to attend? • When would you shut down?

Give a list of children who were exposed with vaccination records OCPHS & Childcare Facility Work Together Immune children okay to return No evidence of immunity: • Excluded for 21 days (incubation period) • If still within 72 hours of INITIAL exposure, can receive a MMR vaccine and return to school. Still need to monitor for symptoms. • If still within 6 days of INITIAL exposure, can receive immunoglobulin (IG)

Resources • Hennepin County Infectious Diseases in Childcare Settings and Schools Manual • https: //www. hennepin. us/residents/health-medical/infectiousdiseases • MDH • http: //www. health. state. mn. us/divs/idepc/index. html • CDC • https: //www. cdc. gov/diseasesconditions/index. html • OCPHS • 507 -328 -7500; General Line • 507 -328 -7581; Disease Control Specialist

Libby Schmidt, Disease Control Specialist Leah Espinda-Brandt, Disease Prevention & Control Nurse Manager Stacy Sundve, Director of Health Assessment & Planning Mike Melius, Environmental Health Manager Olmsted County Public Health Services

Questions
- Slides: 70