CHAPTER 6 THE SKELETAL SYSTEM THE FRAMEWORK SKELETAL













- Slides: 43

CHAPTER 6 THE SKELETAL SYSTEM: THE FRAMEWORK

SKELETAL SYSTEM OVERVIEW • The skeletal system provides support and allow us to move. • Produces blood cells and stores calcium • Protects vital organs • Acts as a warehouse for mineral storage and fat • There are 305 bones as a newborn and 206 bones in an adult skeleton

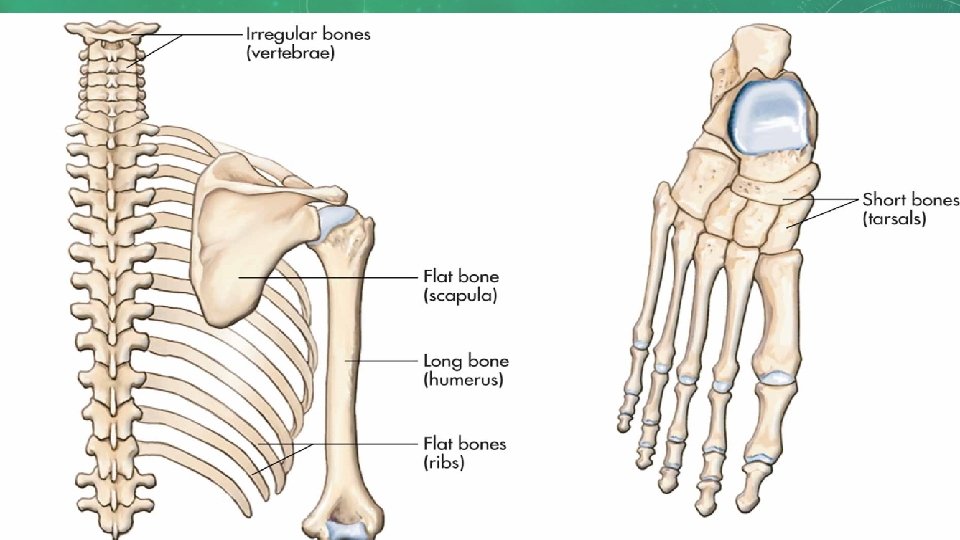
BONE CLASSIFICATION • Long bones: longer than they are wide and can be found in arms and legs • Short bones: Small, cube-shaped bones, found mostly in wrists and ankles • Flat bones: thinner and can be either flat or curved; would include skull, ribs, shoulder blades, and sternum (breast bone) • Irregular bones: like parts of jigsaw puzzle, odd in shape, and include hip bone and vertebrae


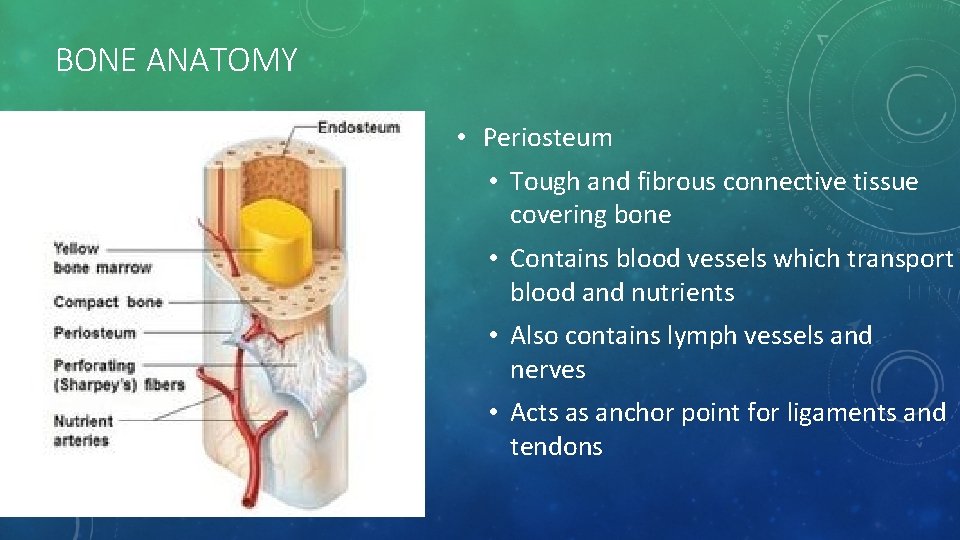
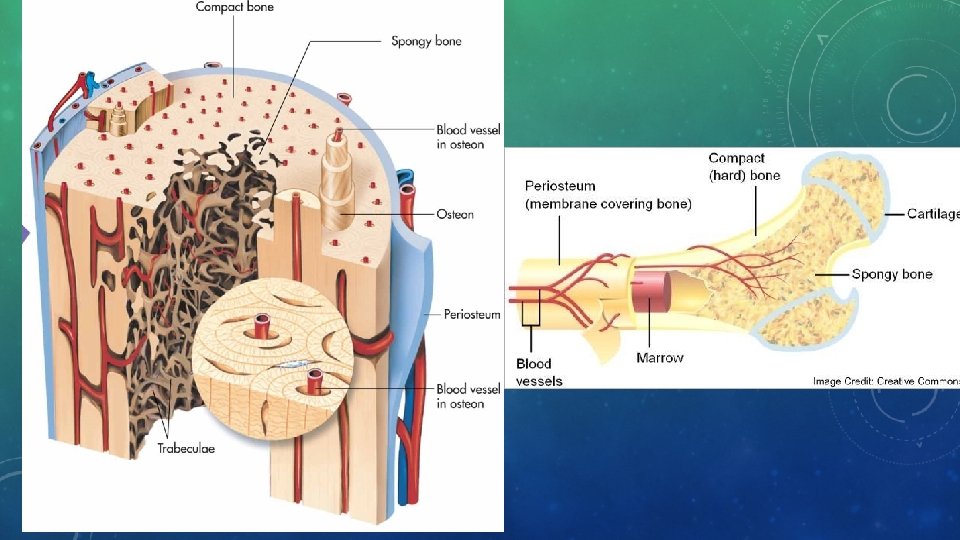
BONE ANATOMY • Periosteum • Tough and fibrous connective tissue covering bone • Contains blood vessels which transport blood and nutrients • Also contains lymph vessels and nerves • Acts as anchor point for ligaments and tendons

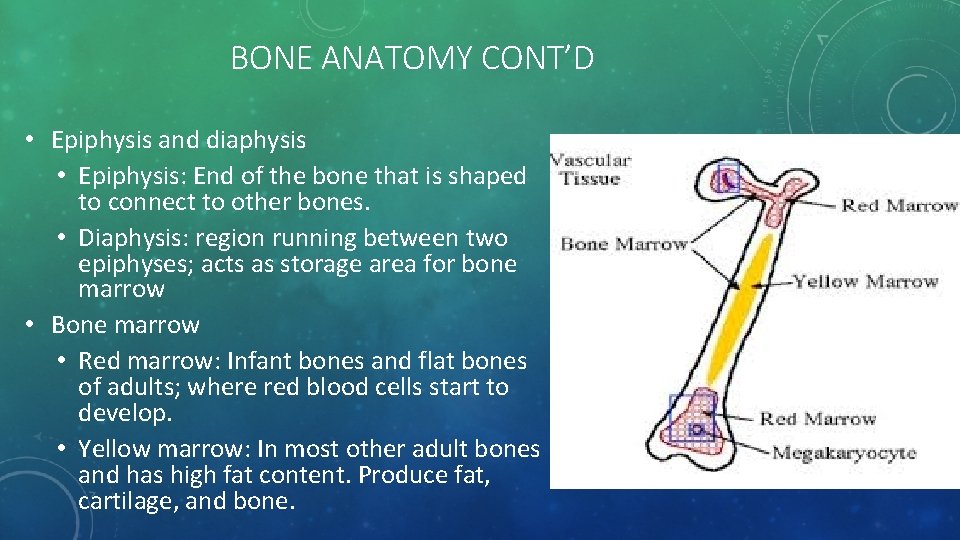
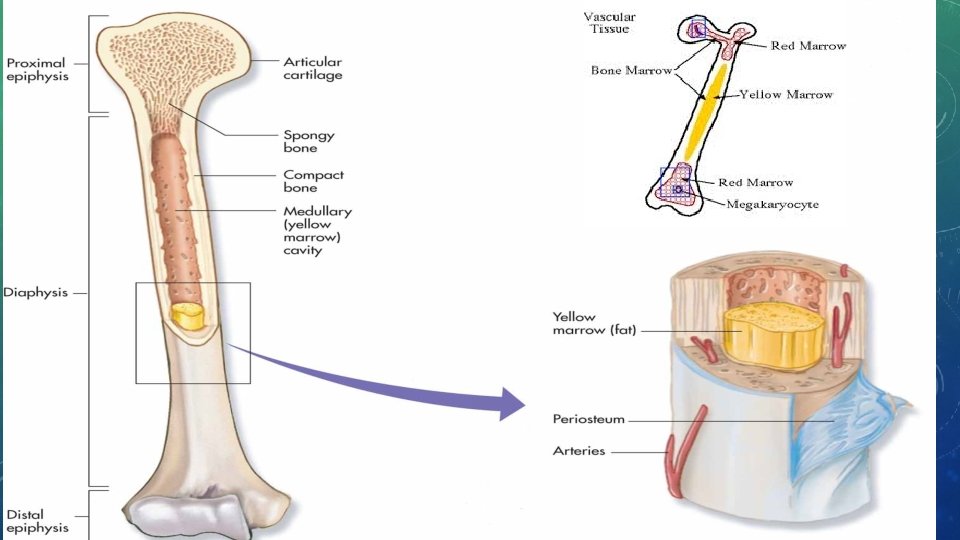
BONE ANATOMY CONT’D • Epiphysis and diaphysis • Epiphysis: End of the bone that is shaped to connect to other bones. • Diaphysis: region running between two epiphyses; acts as storage area for bone marrow • Bone marrow • Red marrow: Infant bones and flat bones of adults; where red blood cells start to develop. • Yellow marrow: In most other adult bones and has high fat content. Produce fat, cartilage, and bone.


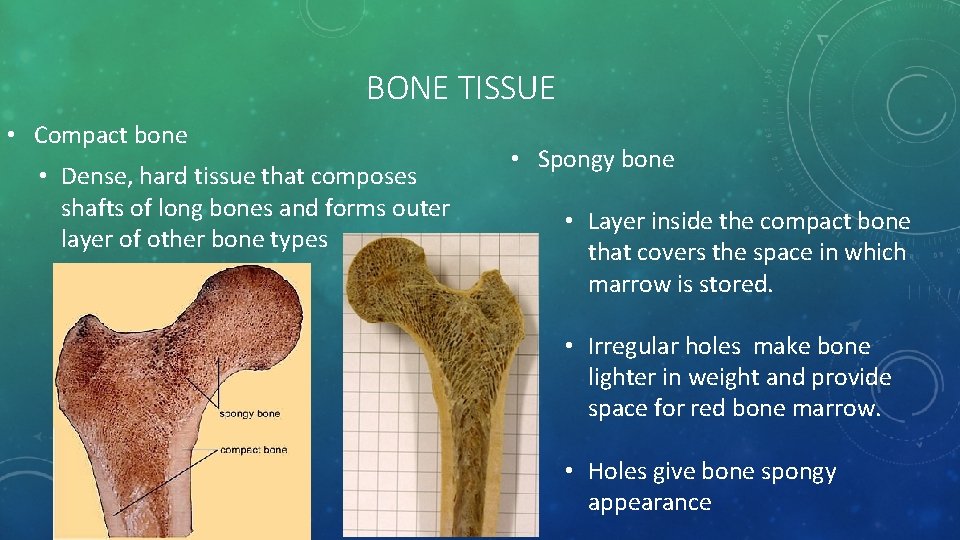
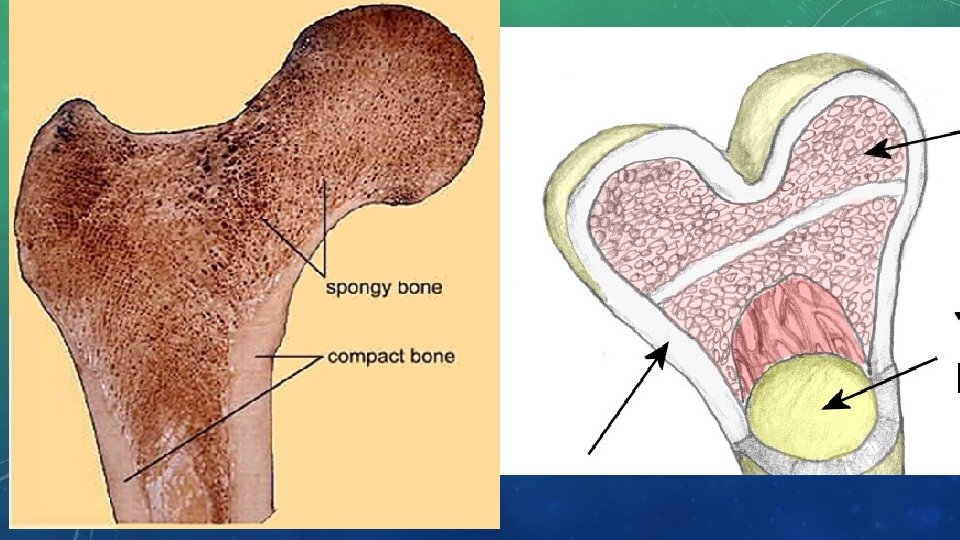
BONE TISSUE • Compact bone • Dense, hard tissue that composes shafts of long bones and forms outer layer of other bone types • Spongy bone • Layer inside the compact bone that covers the space in which marrow is stored. • Irregular holes make bone lighter in weight and provide space for red bone marrow. • Holes give bone spongy appearance

BONE TISSUE


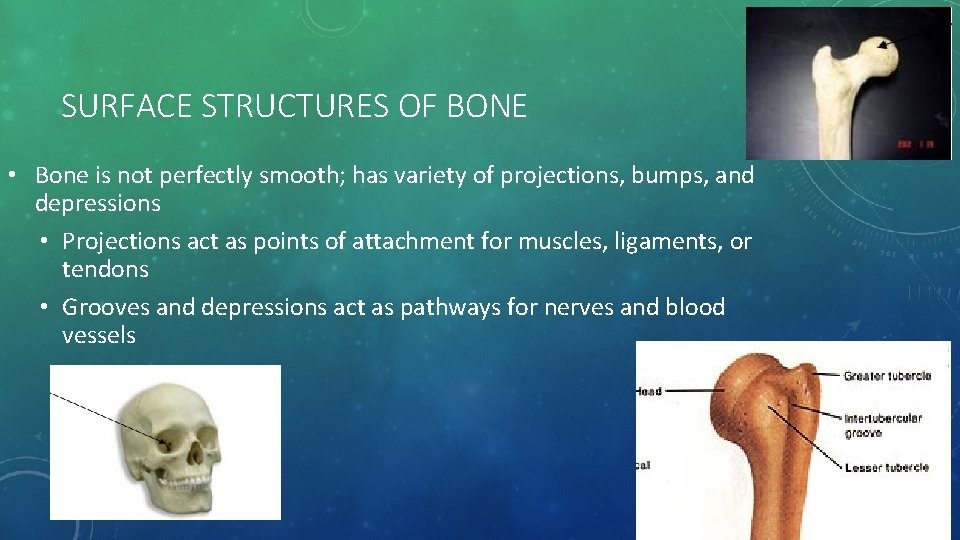
SURFACE STRUCTURES OF BONE • Bone is not perfectly smooth; has variety of projections, bumps, and depressions • Projections act as points of attachment for muscles, ligaments, or tendons • Grooves and depressions act as pathways for nerves and blood vessels

BONE GROWTH AND REPAIR • Ossification: describes formation of bone in body. 2 types (Intramembranous and endochondral) • Bones grow longitudinally to develop height and horizontally (wider and thicker) so they can more efficiently support body weight and any other weight we support

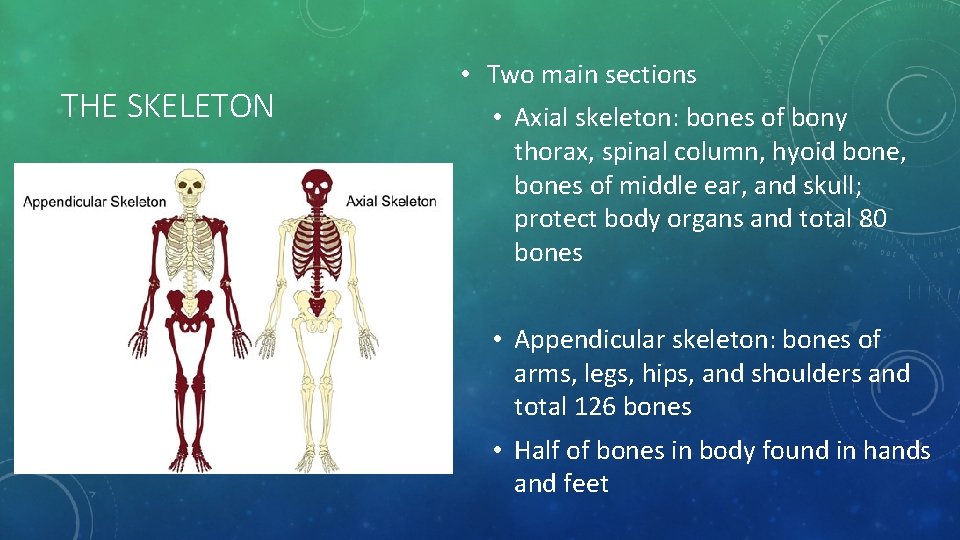
THE SKELETON • Two main sections • Axial skeleton: bones of bony thorax, spinal column, hyoid bone, bones of middle ear, and skull; protect body organs and total 80 bones • Appendicular skeleton: bones of arms, legs, hips, and shoulders and total 126 bones • Half of bones in body found in hands and feet

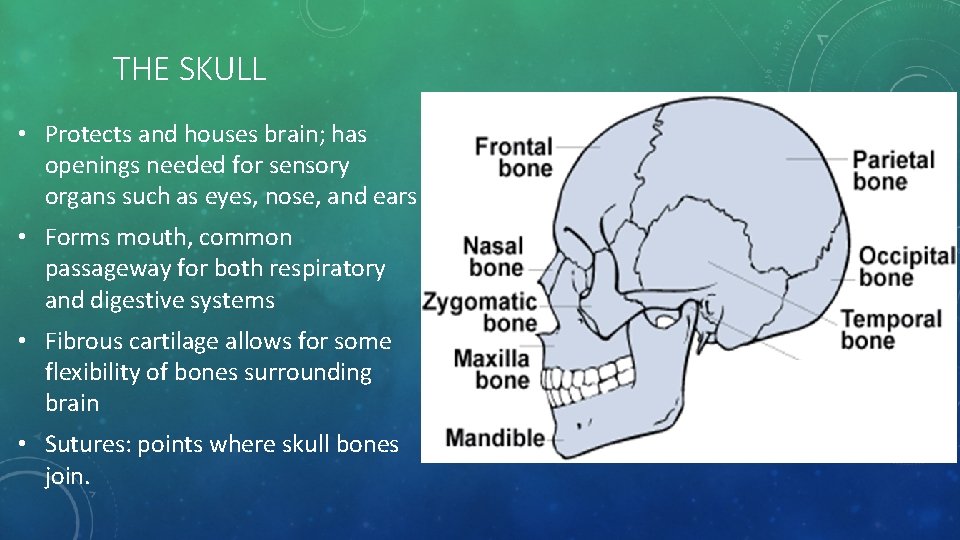
THE SKULL • Protects and houses brain; has openings needed for sensory organs such as eyes, nose, and ears • Forms mouth, common passageway for both respiratory and digestive systems • Fibrous cartilage allows for some flexibility of bones surrounding brain • Sutures: points where skull bones join.

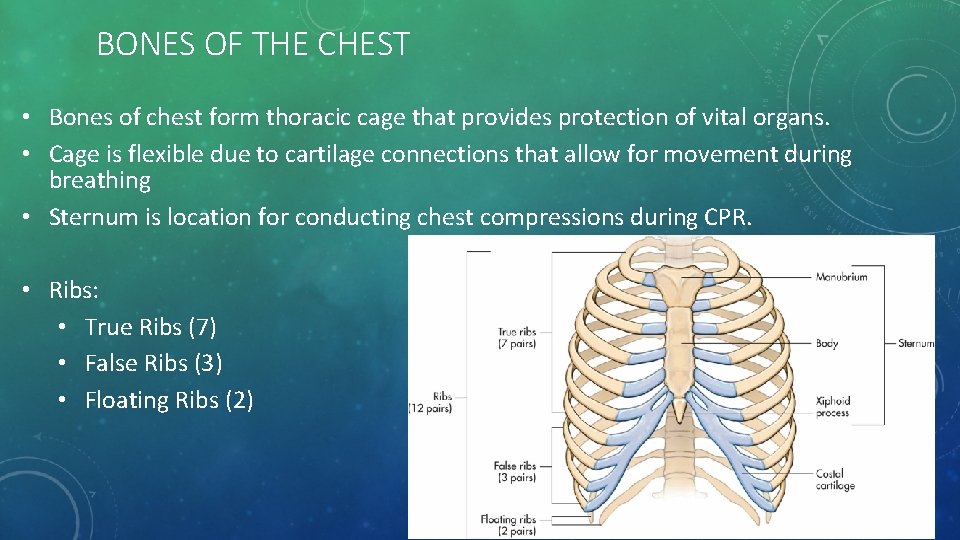
BONES OF THE CHEST • Bones of chest form thoracic cage that provides protection of vital organs. • Cage is flexible due to cartilage connections that allow for movement during breathing • Sternum is location for conducting chest compressions during CPR. • Ribs: • True Ribs (7) • False Ribs (3) • Floating Ribs (2)

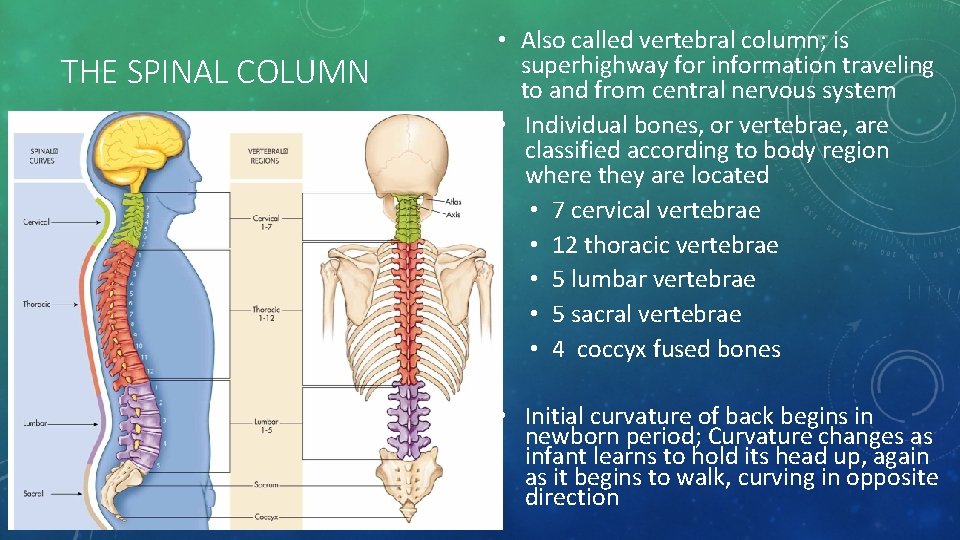
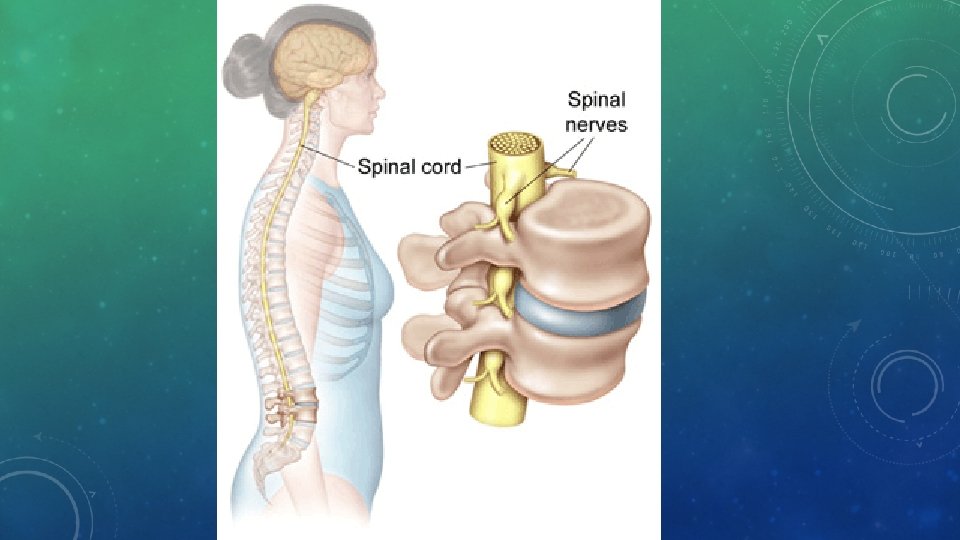
THE SPINAL COLUMN • Also called vertebral column; is superhighway for information traveling to and from central nervous system • Individual bones, or vertebrae, are classified according to body region where they are located • 7 cervical vertebrae • 12 thoracic vertebrae • 5 lumbar vertebrae • 5 sacral vertebrae • 4 coccyx fused bones • Initial curvature of back begins in newborn period; Curvature changes as infant learns to hold its head up, again as it begins to walk, curving in opposite direction


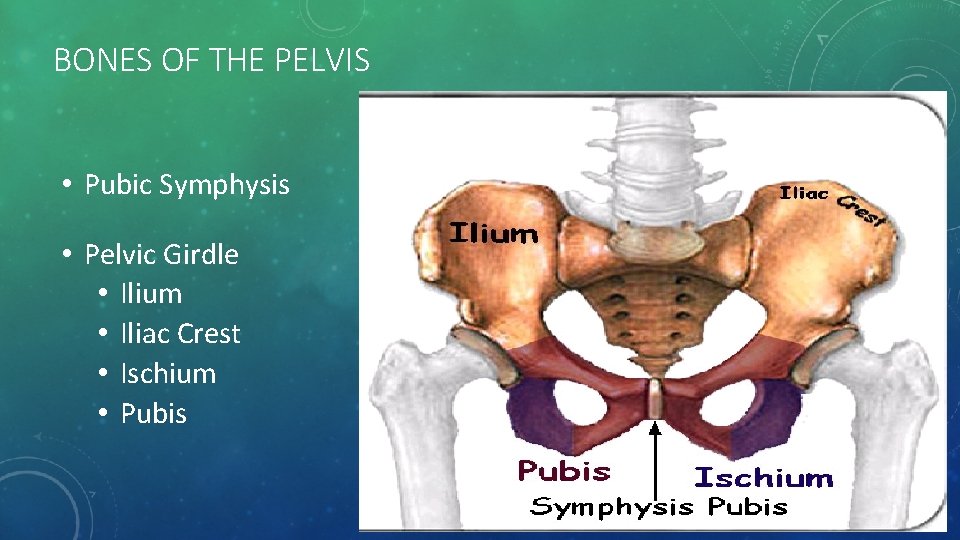
BONES OF THE PELVIS • Pubic Symphysis • Pelvic Girdle • Ilium • Iliac Crest • Ischium • Pubis

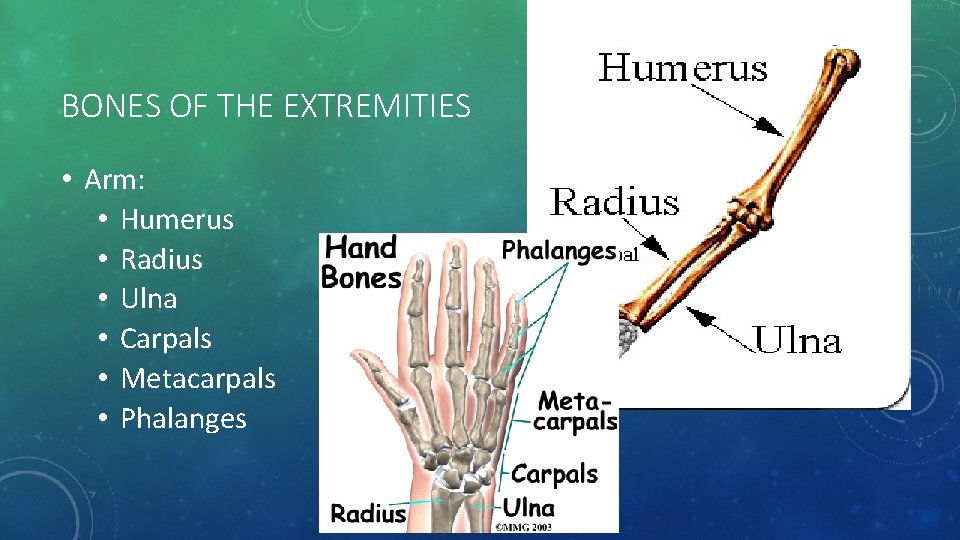
BONES OF THE EXTREMITIES • Arm: • Humerus • Radius • Ulna • Carpals • Metacarpals • Phalanges

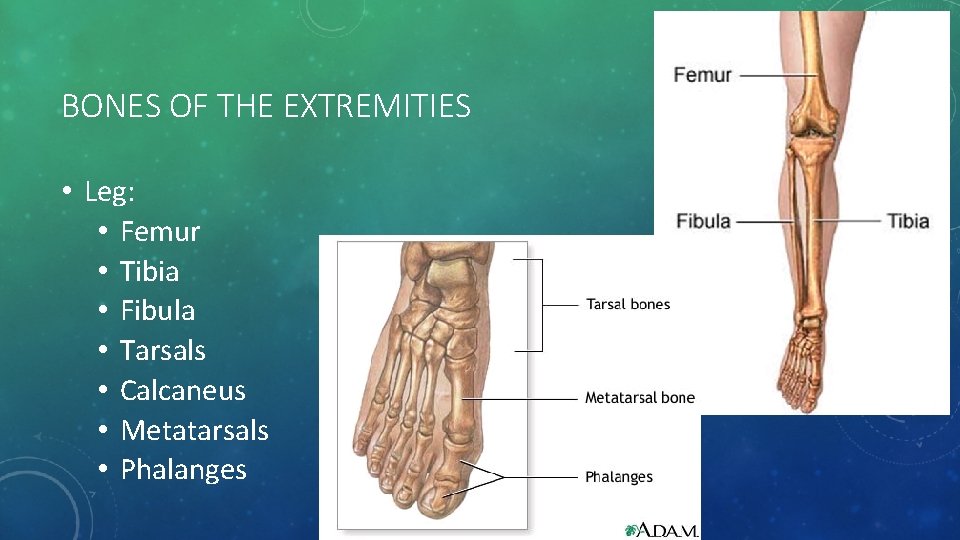
BONES OF THE EXTREMITIES • Leg: • Femur • Tibia • Fibula • Tarsals • Calcaneus • Metatarsals • Phalanges

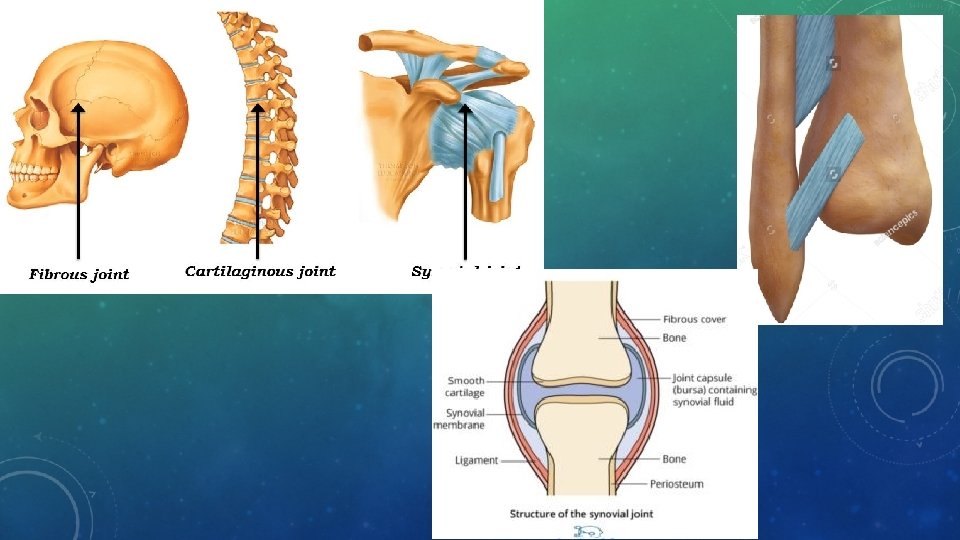
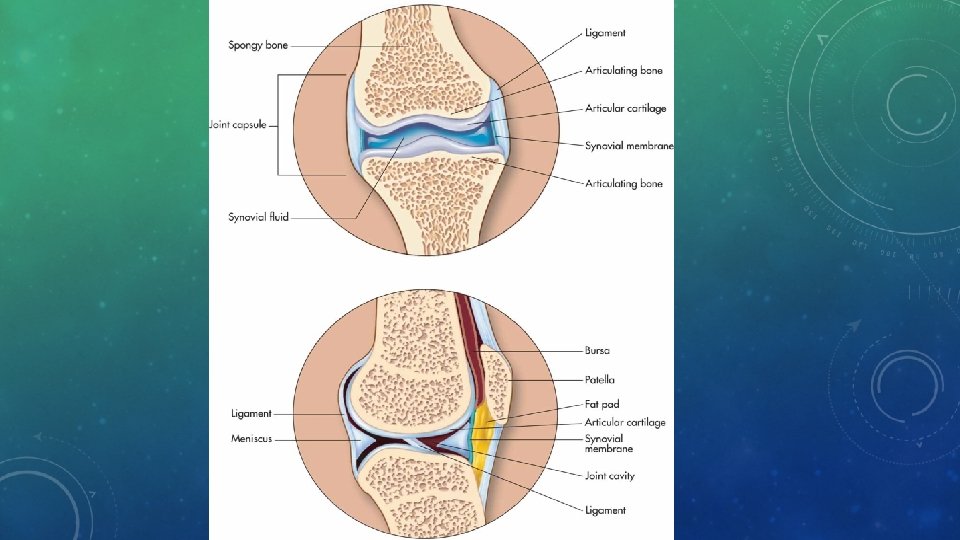
JOINTS, LIGAMENTS, TENDONS • Joints are points where bones connect. • Ligaments: tough bands that connect from bone to bone and can withstand heavy stress • Tendons: cord-like structures that attach muscle to bone • Movement of the joint depends on the bodies need. • Fibrous joints are held together by short connective tissue strands. They are either immobile or slightly movable. (Ex. skull bones & between the tibia and fibula) • Cartilaginous joints are held together by cartilage disks. They are either immobile or slightly movable. (Ex. Vertebrae & between the pubic bones) • Synovial joints features a fluid-filled space between smooth cartilage pads at the end of articulating bones. (ex. Elbow and knee joint)


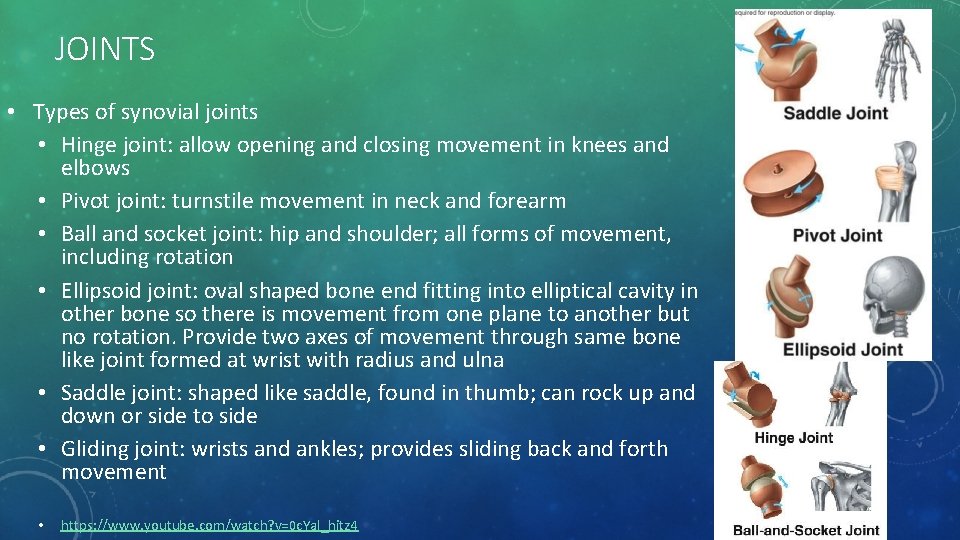
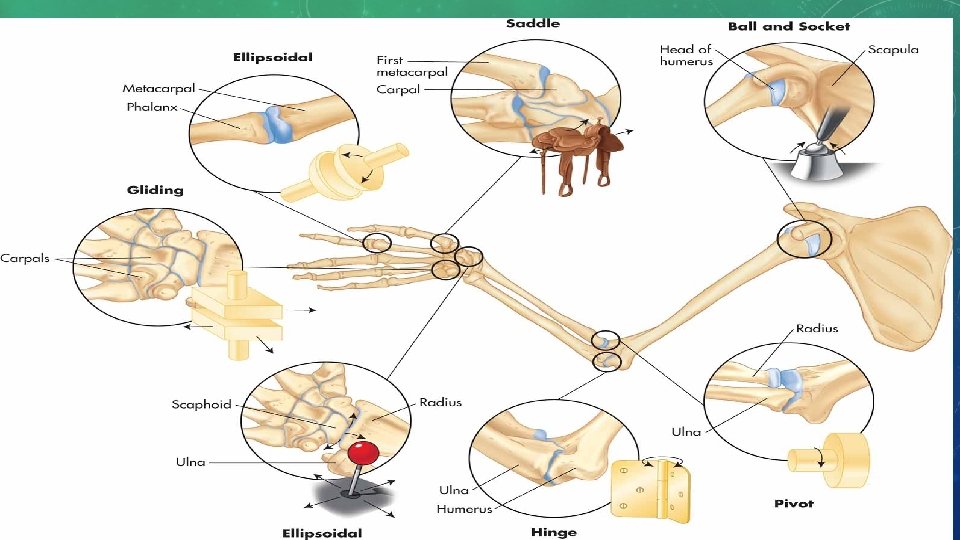
JOINTS • Types of synovial joints • Hinge joint: allow opening and closing movement in knees and elbows • Pivot joint: turnstile movement in neck and forearm • Ball and socket joint: hip and shoulder; all forms of movement, including rotation • Ellipsoid joint: oval shaped bone end fitting into elliptical cavity in other bone so there is movement from one plane to another but no rotation. Provide two axes of movement through same bone like joint formed at wrist with radius and ulna • Saddle joint: shaped like saddle, found in thumb; can rock up and down or side to side • Gliding joint: wrists and ankles; provides sliding back and forth movement • https: //www. youtube. com/watch? v=0 c. Yal_hitz 4


JOINTS JOINT POSSIBLE MOVEMENT • Wrist Flexion, Extension, Abduction, Adduction and Circumduction • Radio-Ulnar Rotation, Pronation and Supination • Elbow Flexion and Extension • Shoulder Flexion, Extension, Horizontal Flexion, Horizontal Extension, Abduction, Adduction, Rotation and Circumduction • Spine/Vertebrae Flexion, Extension, Lateral Flexion and Rotation • Hip Flexion, Extension, Abduction, Adduction, Rotation and Circumduction • Knee Flexion and Extension • Ankle Dorsiflexion, Plantar Flexion, Inversion, & Eversion

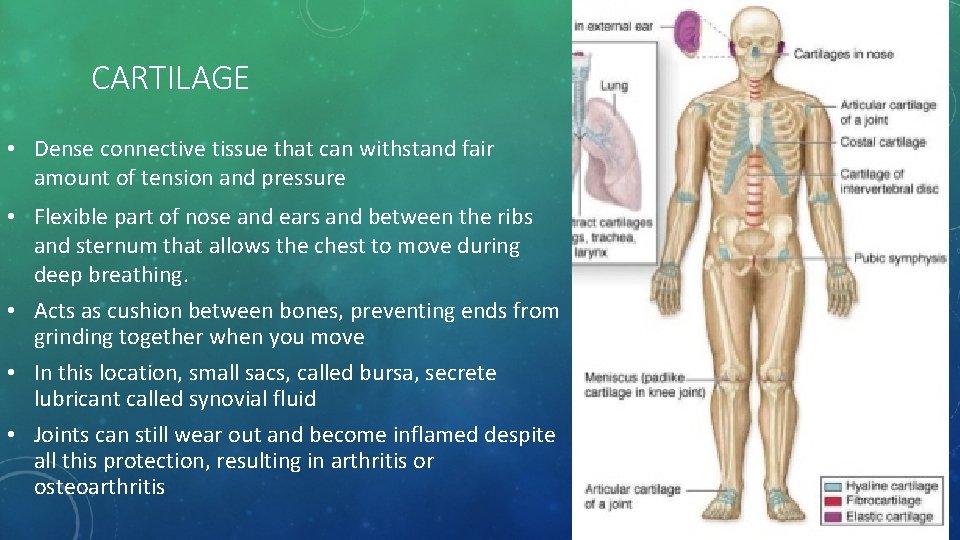
CARTILAGE • Dense connective tissue that can withstand fair amount of tension and pressure • Flexible part of nose and ears and between the ribs and sternum that allows the chest to move during deep breathing. • Acts as cushion between bones, preventing ends from grinding together when you move • In this location, small sacs, called bursa, secrete lubricant called synovial fluid • Joints can still wear out and become inflamed despite all this protection, resulting in arthritis or osteoarthritis


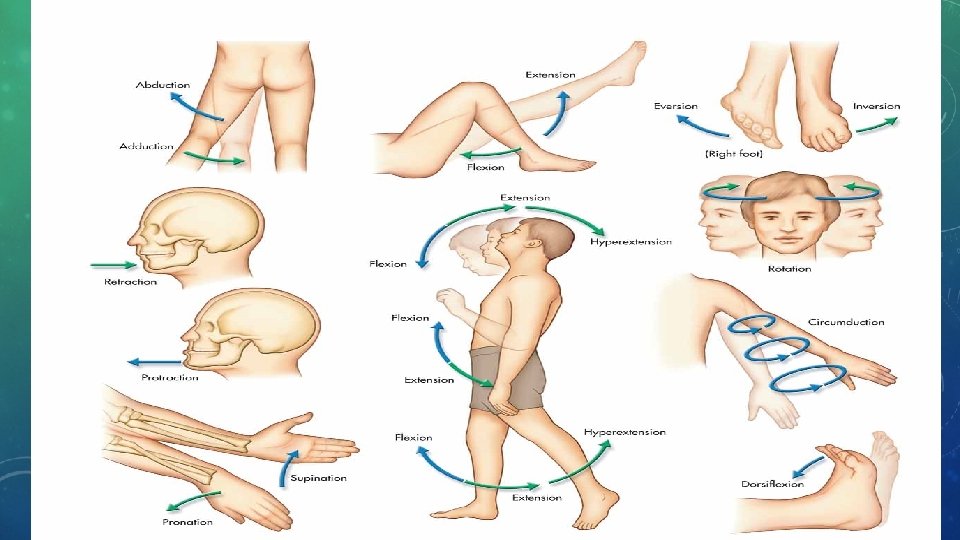
MOVEMENT CLASSIFICATION • Flexion: bending a joint and decreasing angle between involved bones • Extension: straightening a joint • Plantar flexion: pointing toes down • Dorsiflexion: bending foot up toward body • Abduction: moving away from body’s midline • Adduction: moving toward midline of body

MOVEMENT CLASSIFICATION CONT’D • Inversion: turning foot inward toward other foot • Eversion: turning foot outward away from opposing foot • Supination: turning hand palm up • Pronation: turning hand palm down • Circumduction: circular arm movement of a pitcher


• The 6 Types of Joints Video • https: //www. youtube. com/watch? v=q. QOky. Gmi. B 4 A

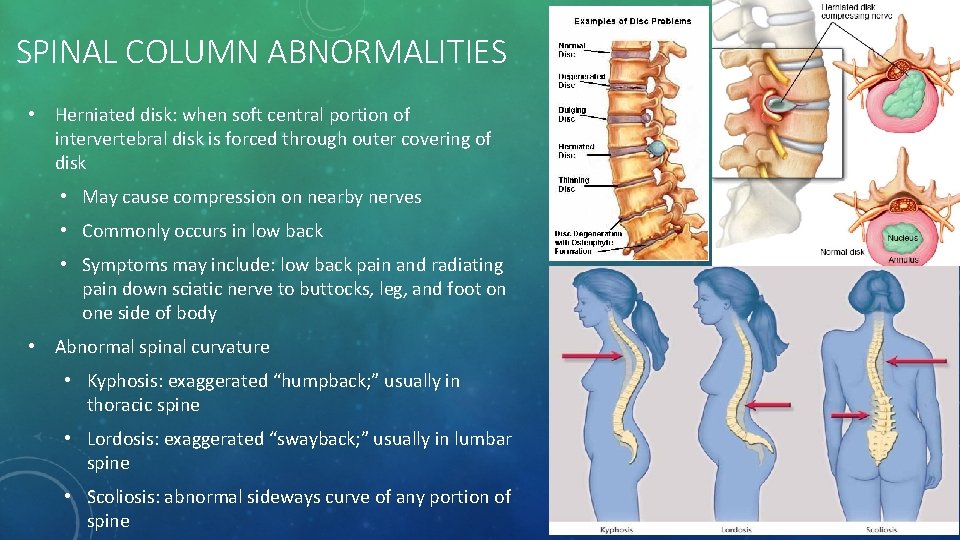
SPINAL COLUMN ABNORMALITIES • Herniated disk: when soft central portion of intervertebral disk is forced through outer covering of disk • May cause compression on nearby nerves • Commonly occurs in low back • Symptoms may include: low back pain and radiating pain down sciatic nerve to buttocks, leg, and foot on one side of body • Abnormal spinal curvature • Kyphosis: exaggerated “humpback; ” usually in thoracic spine • Lordosis: exaggerated “swayback; ” usually in lumbar spine • Scoliosis: abnormal sideways curve of any portion of spine

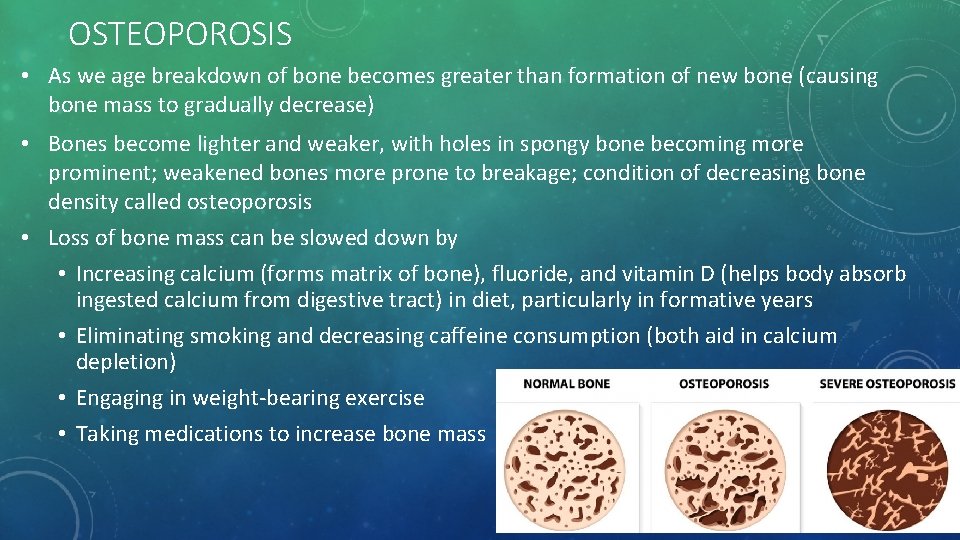
OSTEOPOROSIS • As we age breakdown of bone becomes greater than formation of new bone (causing bone mass to gradually decrease) • Bones become lighter and weaker, with holes in spongy bone becoming more prominent; weakened bones more prone to breakage; condition of decreasing bone density called osteoporosis • Loss of bone mass can be slowed down by • Increasing calcium (forms matrix of bone), fluoride, and vitamin D (helps body absorb ingested calcium from digestive tract) in diet, particularly in formative years • Eliminating smoking and decreasing caffeine consumption (both aid in calcium depletion) • Engaging in weight-bearing exercise • Taking medications to increase bone mass

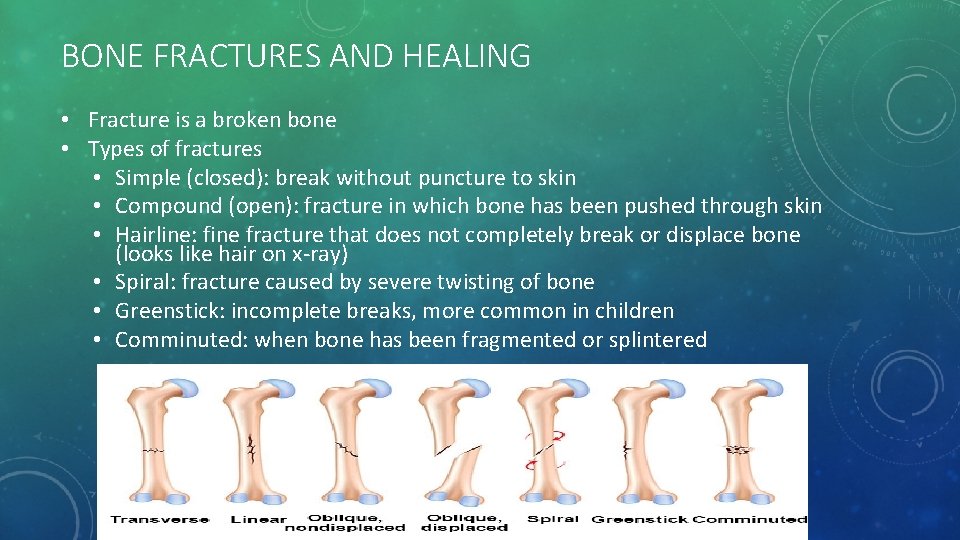
BONE FRACTURES AND HEALING • Fracture is a broken bone • Types of fractures • Simple (closed): break without puncture to skin • Compound (open): fracture in which bone has been pushed through skin • Hairline: fine fracture that does not completely break or displace bone (looks like hair on x-ray) • Spiral: fracture caused by severe twisting of bone • Greenstick: incomplete breaks, more common in children • Comminuted: when bone has been fragmented or splintered

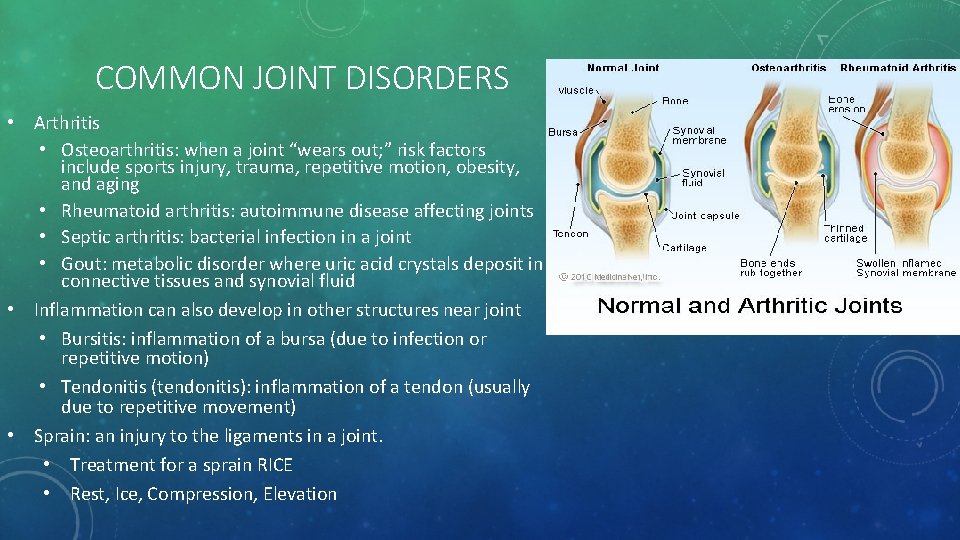
COMMON JOINT DISORDERS • Arthritis • Osteoarthritis: when a joint “wears out; ” risk factors include sports injury, trauma, repetitive motion, obesity, and aging • Rheumatoid arthritis: autoimmune disease affecting joints • Septic arthritis: bacterial infection in a joint • Gout: metabolic disorder where uric acid crystals deposit in connective tissues and synovial fluid • Inflammation can also develop in other structures near joint • Bursitis: inflammation of a bursa (due to infection or repetitive motion) • Tendonitis (tendonitis): inflammation of a tendon (usually due to repetitive movement) • Sprain: an injury to the ligaments in a joint. • Treatment for a sprain RICE • Rest, Ice, Compression, Elevation

BONE HEALING • Bones take several weeks to heal; can only heal normally if ends of bones are touching; if bones are not touching (are poorly aligned), bone must be set (reduced) • In first few hours after injury hematoma, or blood clot, forms around broken bone and inflammation sets in • For next 3 -4 weeks soft callus forms, replacing hematoma and bridging gap between broken ends of bone; soft callus starts as hyaline cartilage which eventually has some bone cells within it; capillaries invade site, ready to vascularize healing bone • From week 4 to week 12 after injury, bony callus forms, replacing soft callus via endochondral ossification; usually bony callus will contain excess bone • Remodeling necessary after bony callus formation to make repaired bone match rest of bone

BONE FORMATION • Cell types involved in bone formation and growth • Osteoprogenitor cells • Osteoblasts • Osteocytes • Osteoclasts

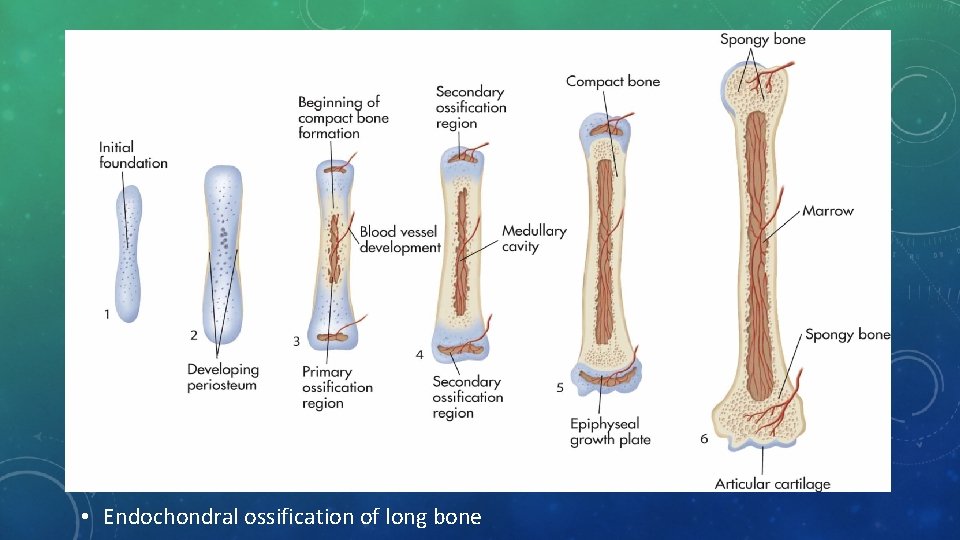
ENDOCHONDRAL OSSIFICATION • Majority of bones form through endochondral ossification • Shaped cartilage replaced by bone • Periosteum surrounds diaphysis of cartilage bone as cartilage itself begins to break down • Osteoblasts come into region and create spongy bone in area that is then referred to as primary ossification center • Other osteoblasts begin to form compact bone under periosteum; osteoclasts break down spongy bone of diaphysis to create medullary cavity

• Endochondral ossification of long bone

• Epiphyseal plate (growth plate) • After we are born, epiphysis on long bones continues to grow • Plate is thin band of cartilage formed between primary and secondary ossification centers • Plate exists as long as bones need to lengthen and widen; controlled by hormones, plate will eventually ossify and stop growth process

• Osteoprogenitor cells: non-specialized cells found in periosteum, endosteum, and central canal of compact bones; can turn into other types of cells as needed • Osteoblasts: cells that actually form bones; arise from non-specialized osteoprogenitor cells and are cells that secrete a matrix of calcium with other minerals that give bone its typical characteristics • Osteocytes: considered mature bone cells that started as osteoblasts; osteoblasts surround themselves with matrix to then become mature osteocytes • Osteoclasts: believed to originate from type of white blood cell called monocyte found in red bone marrow; job is to tear down bone material and help move calcium and phosphate into blood

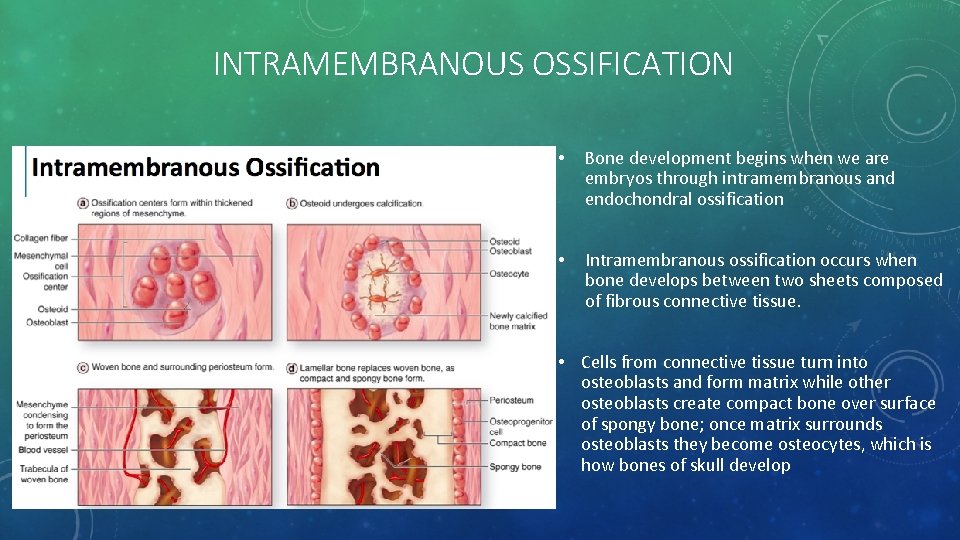
INTRAMEMBRANOUS OSSIFICATION • Bone development begins when we are embryos through intramembranous and endochondral ossification • Intramembranous ossification occurs when bone develops between two sheets composed of fibrous connective tissue. • Cells from connective tissue turn into osteoblasts and form matrix while other osteoblasts create compact bone over surface of spongy bone; once matrix surrounds osteoblasts they become osteocytes, which is how bones of skull develop

• https: //www. youtube. com/watch? v=r. DGqk. MHPDq. E