Polycystic Ovarian Syndrome Dr Pierre Smith FRANZCOG FRACGP












- Slides: 14

Polycystic Ovarian Syndrome Dr Pierre Smith FRANZCOG FRACGP


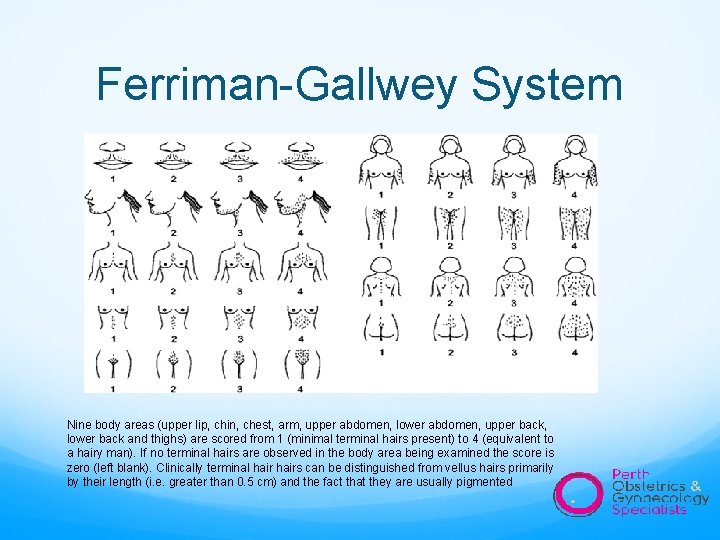
Ferriman-Gallwey System Nine body areas (upper lip, chin, chest, arm, upper abdomen, lower abdomen, upper back, lower back and thighs) are scored from 1 (minimal terminal hairs present) to 4 (equivalent to a hairy man). If no terminal hairs are observed in the body area being examined the score is zero (left blank). Clinically terminal hairs can be distinguished from vellus hairs primarily by their length (i. e. greater than 0. 5 cm) and the fact that they are usually pigmented

Learning Objectives: Outline diagnostic criteria for PCOS Rotterdam Criteria (2003) International Evidence Based Guidelines (2018) Outline management options for PCOS

Overview Pathophysiology Diagnosis Adolescents Clinical implications Investigations Management Insulin Resistance

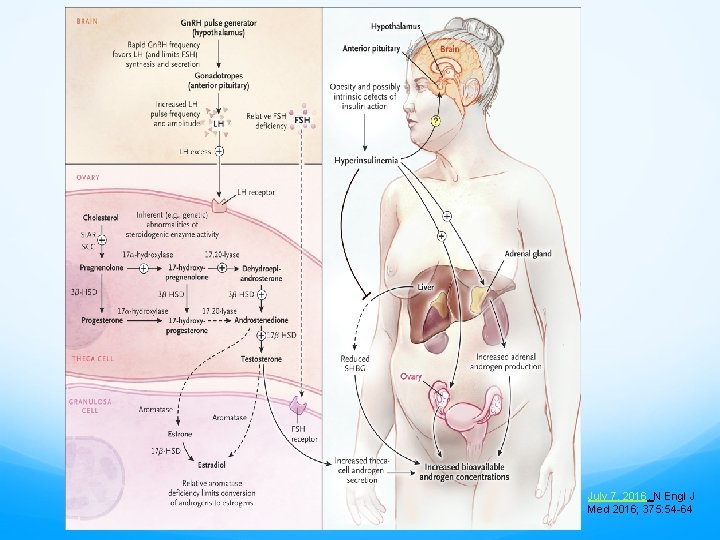
July 7, 2016, N Engl J Med 2016; 375: 54 -64

Diagnosis Rotterdam Criteria (2003) =12 -21% of productive age women Any 2 out of the following 3 (+ rule out other causes) 1. Oligo or anovulation Anovulation: no period for 90 days Oligomenorrhoea: less than 9 cycles a yr 2. Polycystic ovaries on transvaginal ultrasound Ovarian volume of 10 ml or more and /or 12 or more follicles of 2 -9 mm size 2018 Consensus International guidelines states more than 20 3. Clinical/Chemical hyperandrogenism Hirsutism, acne, male pattern baldness Elevated free androgen index/free testosterone index

Adolescents Irregular cycles are normal in 1 st year post menarche 1 -3 yrs post menarche a normal cycle = 21 -45 days > 3 yr post menarche a normal cycle= 21 -35 days Ultrasound unreliable for diagnosis in first 8 years after menarche Short cycles or heavy periods often signal anovulation Secondary Amenorrhoea = no period for 90 days

Clinical Implications of PCOS Menstrual irregularities Cosmetic effects Subfertility Endometrial carcinoma “Metabolic syndrome” Diabetes Obesity Hypertension Hypercholesterolaemia Effects on pregnancy

Investigations Ultrasound is not essential for diagnosis Blood tests are not essential for diagnosis Oral GTT when other risk factors and pre conception AMH testing not recommended (yet) Assess for depression (as at increased risk) Assess for cardiac risk factors Consider Endometrial Assessment Consider Obstructive Sleep Apnoea Assessment

Management of PCOS Education Chronic condition that can be effectively managed Lifestyle: Exercise, Diet, Weight loss Combined oral contraceptive pill- lowest dose Wait 6/12 before adding anti- androgens Yaz/Yasmin no better Avoid Dianne et al due to increased risk of Thrombosis Endometrial protection COCP/Microlut/Mirena/Depo-Provera

Management of PCOS Manage “Metabolic Syndrome” Anovulation: Weight loss Letrozole rather than Clomid +/- Metformin Laparoscopic ovarian drilling Cosmetic Add Spironolactone Cosmetic treatments for hirsutism Acne treatment eg Doxycyclin/Isotretinoin

Insulin Resistance Metformin 500 mg -2000 mg slow release nocte As adjuct to COCP and Letrozole Improves ovulation Reduces insulin resistance Assists with weight loss Possibly slows progression to Diabetes

Summary PCOS is common PCOS is a multi system disease It is a chronic disease Diagnosed by Rotterdam Criteria Difficult to diagnose in Adolescece Management is straight forward in most cases International Evidence Based Guideline 2018: https: //www. monash. edu/__data/assets/pdf_file/0004/14126 44/PCOS_Evidence-Based-Guidelines_20181009. pdf