Overview and Introduction Alzheimers Disease The Challenge of


























- Slides: 27

Overview and Introduction Alzheimer’s Disease The Challenge of Early Diagnosis

Benefits of Early Diagnosis and Treatment of Alzheimer’s Disease ► Alzheimer’s disease can be diagnosed approximately 90% of the time with a general medical and psychiatric evaluation 1, 2 ► Early diagnosis has many advantages 3, 4 l l l Allows time for planning Empowers the patients to make treatment decisions early on Facilitates caregiver participation ► May slow the progression of symptoms 2 ► Offers the patient potential for greater functioning and independence 2, 3 ► Can help ease the stress for caregivers 2, 3 Sources: 1. Small GW, et al. JAMA. 1997; 278: 1363 -1372. 2. National Institute on Aging. National Institutes of Health; 2000. NIH publication 00 -4859: l-62. 3. Doraiswamy PM, et al. J Clin Psychiatry. 1998; 59(suppl 13): 6 -18. 4. Knopman DS. In: Early Diagnosis of Alzheimer’s Disease. Totowa, NJ: Humana Press, Inc; 2000: 298.

Discussion Points Dementia is underrecognized (even with behavioral symptoms) and undertreated ► 67. 7% of residents* have dementia l Of those with dementia 73% were adequately evaluated 52% were adequately treated 70% had clinically significant behavioral symptoms Used 262 min/d of staff time vs no dementia 126 min/d (P<. 005) *The results are based on a randomized cohort of assisted living (AL) residents of 22 randomly selected AL facilities in Baltimore and 7 Maryland counties. Source: Rosenblatt A, et al. J Am Geriatr Soc. 2004; 52: 1618 -1625.

Barriers to Early Diagnosis Stigma ► First-degree relatives of AD patients reluctant to approve cognitive status examination ► Those of patients with more behavioral problems show greater reluctance Misconceptions ► Perception of uselessness of examination ► Perception of limited treatment options Early Stages ► Patients maintain social skills in mild stages Source: Werner P, Heinik J. Int J Geriatr Psychiatry. 2004; 19: 479 -486.

Barriers to Early Diagnosis (cont) Failure to Recognize the Importance of Cognitive/Functional Changes Racial Barriers ► Racial bias in screening tools ► Duality of respect for the patient— “normalization” ► Cultural ignorance or insensitivity Source: Cloutterbuck J, et al. Dementia. 2003; 2: 221 -243.

Discussion Points Dementia Screening Tools: Effect of Ethnicity ► Brief screening tests often incorrectly classify African Americans with dementia (42%) compared to Caucasians (6%) ► The specificity of standardized cognitive assessments for dementia is particularly bad for African Americans ► Comparison of the utility of the Clock Drawing Test (CDT), Cognitive Abilities Screening Instrument, and MMSE l l All tests were affected by education level CDT was most sensitive to poorly educated non-English speakers Sources: Stephenson J. JAMA. 2001; 286: 779 -780. Lampley-Dallas VT. J Natl Med Assoc. 2001; 93: 323 -328. Fillenbaum G, et al. J Clin Epidemiol. 1990; 43: 651 -660. Borson S, et al. J Gerontol A Biol Sci Med Sci. 1999; 54: M 534 -M 540.

Discussion Points Ethnic Differences in Knowledge and Perception of AD ► Elderly have misperceptions about the prevalence, etiology, diagnosis, and financial coverage for AD treatments ► Older Hispanic and Asian adults frequently consider AD a contagious but curable disease ► Hispanic, Asian, and African Americans more often consider AD a form of insanity ► Education levels partially explain differences in AD knowledge between Caucasians and Hispanics ► For Asians, the number of years speaking English is correlated with better knowledge of AD Source: Ayalon L, et al. Int J Geriatr Psychiatry. 2004; 19: 51 -57.

Barriers to Early Diagnosis (cont) ► Barriers associated with PCPs ► Differential diagnosis l ► Differentiating dementia, delirium, and depression Time l l ► Lewy Comorbid conditions l ► Vascular dementia, frontotemporal dementia, body dementia 1 hour required for diagnosis, but only 15 minutes reimbursed Knowledge of appropriate reimbursement codes Overabundance of tests

Discussion Points Vascular Dementia (Va. D) - Key Elements ► ► Cognitive impairment caused by cerebrovascular disease or cerebrovascular accident Mixed dementia = Va. D + AD ► “Stairstep” progression of illness ► May have motor impairment early in the course of illness ► Care Notes l Treat hypertension, diabetes, ↑ lipids l May be associated with severe or refractory depression l Accommodate hemiplegia in interactions with staff/environment Source: Black SE. Postgrad Med. 2005; 117(1): 15 -16, 19 -25.

Discussion Points Dementia With Lewy Bodies - Key Elements ► ► Wide fluctuations in cognition, responsiveness, and function Vivid visual hallucinations and paranoid delusions Parkinsonism occurs early Care notes l Some antipsychotics will cause severe parkinsonism at low doses l Quetiapine, aripiprazole, or clozapine may be tolerated best l Cholinesterase inhibitors are helpful l Levodopa and Parkinson’s disease medications have limited effectiveness for movement disorders Sources: Mc. Keith IG, et al. Neurology. 1996; 47: 1113 -1124. Mc. Keith IG, et al. Neurology. 1999; 53: 902 -905.

Discussion Points Frontotemporal Dementia - Key Elements Frontal lobe dementia, Pick’s disease ► Earlier age of onset than AD ► Gradual decline ► Early problems with memory and language expression ► Prominent personality changes—socially inappropriate, disinhibited, and compulsive (sexualized, eating) behaviors often observed ► Care notes l Cholinesterase inhibitors not very effective l Safe environment for harmful compulsive behaviors ► Source: Mc. Khann GM, et al. Arch Neurol. 2001; 58: 1803 -1809.

Alzheimer’s Disease ► Multiple cognitive deficits, with both memory impairment and 1 or more of the following deficits: ● Aphasia (language) ● Apraxia (learned motor skills) ● Agnosia (visuospatial/sensory) ● Executive functioning (planning, insight anticipation) ► Impairment in social or occupational functioning, representing a significant decline from a previous level of functioning ► Gradual onset and progressive cognitive decline Adapted from: American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders. 4 th ed. Washington, DC: American Psychiatric Association; 1994: 142 -143.

Overcoming Barriers to AD Diagnosis ► Time Schedule high-risk patients at end of day l AD does not have to be diagnosed in a single visit ► Reimbursement l Know appropriate codes for AD diagnosis and for extra time ► Coexisting illnesses l AD treatments may permit sustained self-management of other illnesses ► Depression l Evaluate patients using Geriatric Depression Scale (15 questions) ► Screening tools l Start slowly in gathering information, eg, MMSE (10 -15 minutes) and CDT (1 -5 minutes) l FAQ 10 questions completed by family l

Targeted Screening ► Patients at least 65 years of age, when clinical presentation suggests the possibility of dementia (eg, forgetfulness, poor hygiene, poor compliance) ► All patients at least 80 years of age, with regular frequency Screening assesses quantitative and objective measures rather than qualitative responses. Sources: Kaiser Permanente Care Management Institute. Guidelines for the diagnosis and management of dementia in primary care. Available at: http: //members. kaiserpermanente. org/kpweb/pdf/feature/247 clinicalpracguide/CMI_ Dementia. Guideline_public_web_020604. pdf. Accessed August 17, 2005. Knopman DS, et al. Neurology. 2001; 56: 1143 -1153.

Discussion Points ► Is there a relationship between mild cognitive impairment (MCI) and AD? (16% of MCI patients convert to AD per year) ► How do we differentiate MCI from AD? ► Government recommendation not to screen (Agency for Healthcare Research and Quality)

The Case for Universal Cognitive Screening ► Memory complaints are common and can be associated with subsequent dementia ► Early dementia symptoms can be difficult to recognize ► Cognitive impairment affects how medical care is provided l l l Management (and costs) of other diseases Follow through with medical recommendations Prevention of complications

Discussion Points ► Which screening tools do you recommend? l A dialogue on the utility of screening tools ► Educational preceptorship—warning signs and public awareness l Community l Doctors l Consumers l Alzheimer’s Association

Dementia Diagnostic Process ► General l screen Signs of acute/chronic disease: how well controlled? Common conditions Weight loss, dehydration, subnutrition Include obstructive sleep apnea, insomnia, depression ► Neurologic l l l Vascular or Parkinson’s dementia, frontal signs Gait, balance, and falls Neuropathy ► Laboratory l l screen Vitamin B 12 deficiency, hypothyroidism Associated problems, secondary complications, and additional causes ► Brain l l screen structural screen Noncontrast CT or MRI Surgical and vascular lesions

Evaluation of the AD Patient ►In approximately 90% of patients who have AD, the diagnosis can be made on the basis of: l Detailed medical history obtained from the patient and a reliable informant l Medical examination l Mental status examination ►A 15 -minute office visit is insufficient for fully evaluating the AD patient. For patients seen regularly, a 3 -stage assessment may be more appropriate Source: Cefalu C, Grossberg GT. Diagnosis and Management of Dementia. American Family Physician Monograph, No. 2. Leawood, Kan: American Academy of Family Physicians; 2001.

The Office History ► Memory impairment: repetitive; trouble remembering recent conversations, events, appointments; frequently misplaces objects ► Executive impairment: deterioration of complex task performance; decreased ability to solve problems; impaired driving ► Drugs: alcohol, prescriptions, over-thecounter (OTC) medications ► Focal motor or sensory neurologic symptoms

Evaluation of the AD Patient (cont) First Visit ► Take comprehensive history l Medical history, medications (including OTC drug use) ► Interview immediate family member/caregiver ► If time permits and patient is cooperative, perform MMSE ► Assess family needs and caregiver stress Source: Cefalu C, Grossberg GT. Diagnosis and Management of Dementia. American Family Physician Monograph, No. 2. Leawood, Kan: American Academy of Family Physicians; 2001.

Evaluation of the AD Patient (cont) Second Visit ► ► ► CBC, electrolytes, LFTs, TSH, B 12, folate, UA, EKG, HIV, VDRL, ESR, homocysteine Neuroimaging Perform MMSE if not performed on first visit Reassess family needs and caregiver stress Consider neuropsychological testing CBC = complete blood count; LFTs = liver function tests; TSH = thyroid-stimulating hormone; UA = unstable angina; EKG = electrocardiogram; HIV = human immunodeficiency virus; VDRL = Venereal Disease Research Laboratory test; ESR = erythrocyte sedimentation rate. Source: Cefalu C, Grossberg GT. Diagnosis and Management of Dementia. American Family Physician Monograph, No. 2. Leawood, Kan: American Academy of Family Physicians; 2001.

Evaluation of the AD Patient (cont) Third Visit ► Review laboratory findings and results of testing ► Discuss treatment options, follow-up plans for patient ► Readdress family and caregiver needs Source: Cefalu C, Grossberg GT. Diagnosis and Management of Dementia. American Family Physician Monograph, No. 2. Leawood, Kan: American Academy of Family Physicians; 2001.

Discussion Points What Is the Place for Imaging? ► Noncontrast CT or MRI scan in the initial evaluation is appropriate (American Academy of Neurology Guideline) ► The use of positron emission tomography ► Value of imaging is to rule out other forms of intracranial pathology that may be contributing to cognitive change or for unusual presentations: l Rapid onset (duration <3 months), subdural hematoma, cerebral neoplasms, head trauma, history of cerebrovascular accident(s), seizures, new-onset urinary or fecal incontinence, abnormal gait, postural instability, focal signs, visual field deficit, headaches, suspect malignant tumor Sources: American Academy of Neurology. 2001; 56: 1133 -1142. American Academy of Neurology. 2001; 56: 1143 -1153.

Practical Consequences of Improved Diagnostic Accuracy ►Accurate diagnostic information and education reduce family/caregiver burden ►Decreased likelihood of repeated diagnostic assessments and testing ►“AD label” improves caregiver attitudes ►Information about the disease improves quality of life for family/patient and delays nursing home placement Sources: Mittelman M, et al. JAMA. 1996; 276: 1725 -1731. Wadley V, et al. J Gerontol B Psychol Sci Soc Sci. 2001; 56: P 244 -P 252.

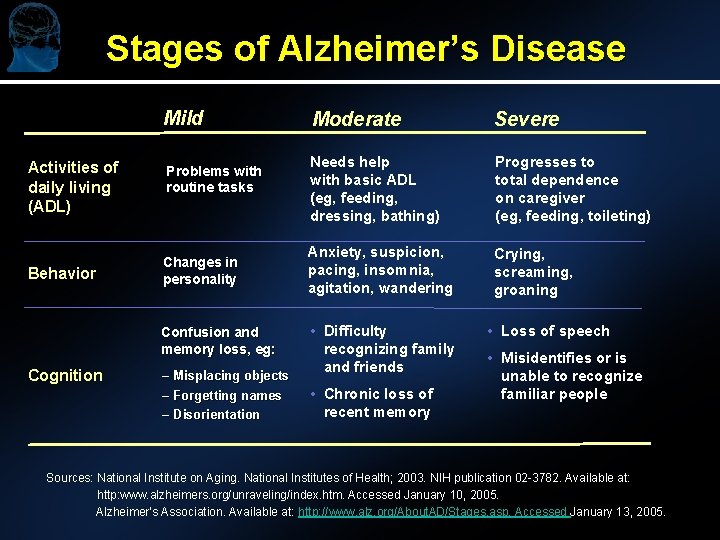
Stages of Alzheimer’s Disease Mild Activities of daily living (ADL) Behavior Problems with routine tasks Changes in personality Confusion and memory loss, eg: Cognition – Misplacing objects – Forgetting names – Disorientation Moderate Severe Needs help with basic ADL (eg, feeding, dressing, bathing) Progresses to total dependence on caregiver (eg, feeding, toileting) Anxiety, suspicion, pacing, insomnia, agitation, wandering Crying, screaming, groaning • Difficulty recognizing family and friends • Chronic loss of recent memory • Loss of speech • Misidentifies or is unable to recognize familiar people Sources: National Institute on Aging. National Institutes of Health; 2003. NIH publication 02 -3782. Available at: http: www. alzheimers. org/unraveling/index. htm. Accessed January 10, 2005. Alzheimer’s Association. Available at: http: //www. alz. org/About. AD/Stages. asp. Accessed January 13, 2005.

Summary ► Marked changes in memory are not a normal part of aging and may signal a developing dementia ► Universal screening for AD is important ► Effective diagnosis and management take time l ► Three separate visits may be required It is important to recognize and overcome the barriers to early diagnosis of AD