Nutritional management of patients with CKD Esther Neill











- Slides: 35

Nutritional management of patients with CKD Esther Neill & Emma Gentles Paediatric Renal Dietitians SPRUN Education Day 9/11/2010

Content • • • Introduction Assessment Requirements Nutritional products Case studies Quiz

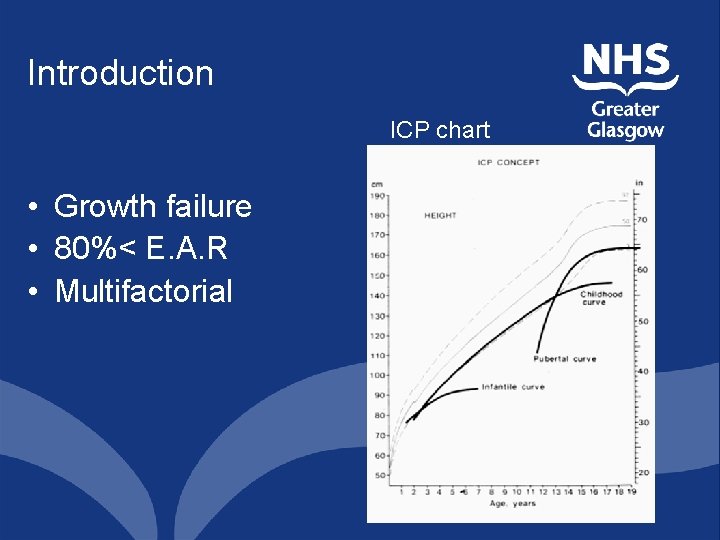
Introduction ICP chart • Growth failure • 80%< E. A. R • Multifactorial

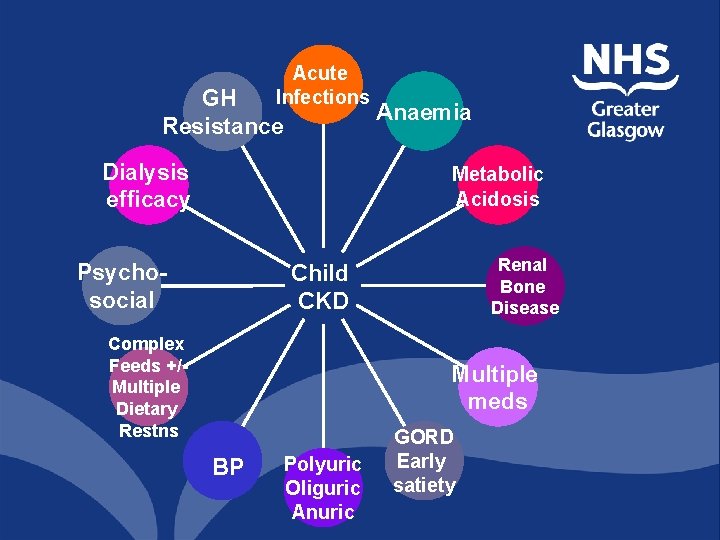
Acute Infections GH Resistance Dialysis efficacy Anaemia Metabolic Acidosis Psychosocial Renal Bone Disease Child CKD Complex Feeds +/Multiple Dietary Restns Multiple meds BP Polyuric Oliguric Anuric GORD Early satiety

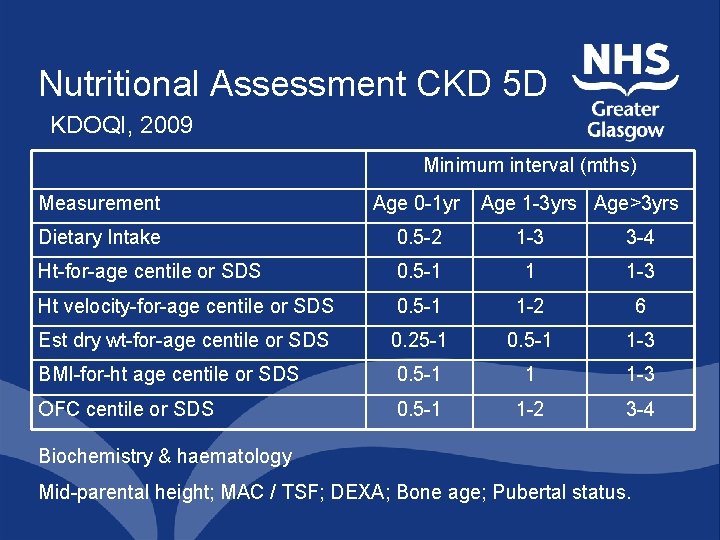
Nutritional Assessment CKD 5 D KDOQI, 2009 Minimum interval (mths) Measurement Age 0 -1 yr Age 1 -3 yrs Age>3 yrs Dietary Intake 0. 5 -2 1 -3 3 -4 Ht-for-age centile or SDS 0. 5 -1 1 1 -3 Ht velocity-for-age centile or SDS 0. 5 -1 1 -2 6 Est dry wt-for-age centile or SDS 0. 25 -1 0. 5 -1 1 -3 BMI-for-ht age centile or SDS 0. 5 -1 1 1 -3 OFC centile or SDS 0. 5 -1 1 -2 3 -4 Biochemistry & haematology Mid-parental height; MAC / TSF; DEXA; Bone age; Pubertal status.

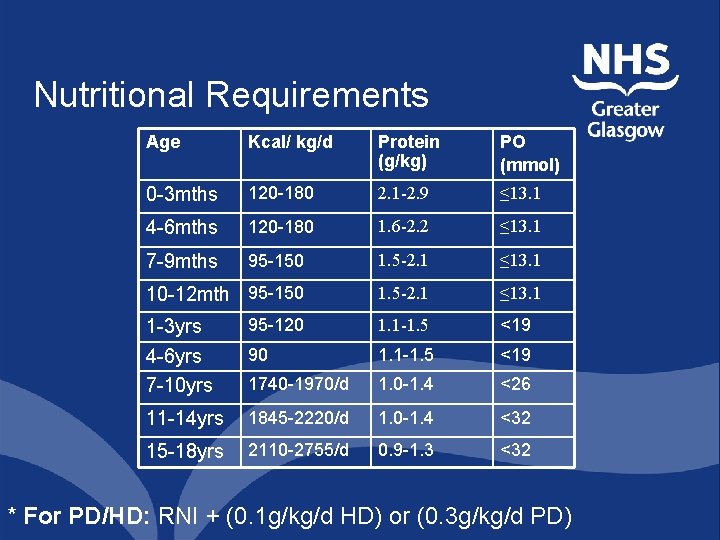
Nutritional Requirements Age Kcal/ kg/d Protein (g/kg) PO (mmol) 0 -3 mths 120 -180 2. 1 -2. 9 ≤ 13. 1 4 -6 mths 120 -180 1. 6 -2. 2 ≤ 13. 1 7 -9 mths 95 -150 1. 5 -2. 1 ≤ 13. 1 10 -12 mth 95 -150 1. 5 -2. 1 ≤ 13. 1 1 -3 yrs 95 -120 1. 1 -1. 5 <19 4 -6 yrs 7 -10 yrs 90 1. 1 -1. 5 <19 1740 -1970/d 1. 0 -1. 4 <26 11 -14 yrs 1845 -2220/d 1. 0 -1. 4 <32 15 -18 yrs 2110 -2755/d 0. 9 -1. 3 <32 * For PD/HD: RNI + (0. 1 g/kg/d HD) or (0. 3 g/kg/d PD)

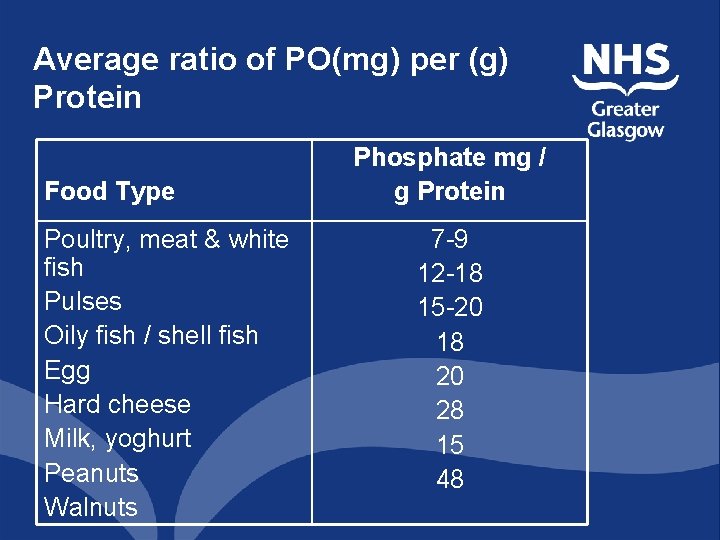
Average ratio of PO(mg) per (g) Protein Food Type Poultry, meat & white fish Pulses Oily fish / shell fish Egg Hard cheese Milk, yoghurt Peanuts Walnuts Phosphate mg / g Protein 7 -9 12 -18 15 -20 18 20 28 15 48


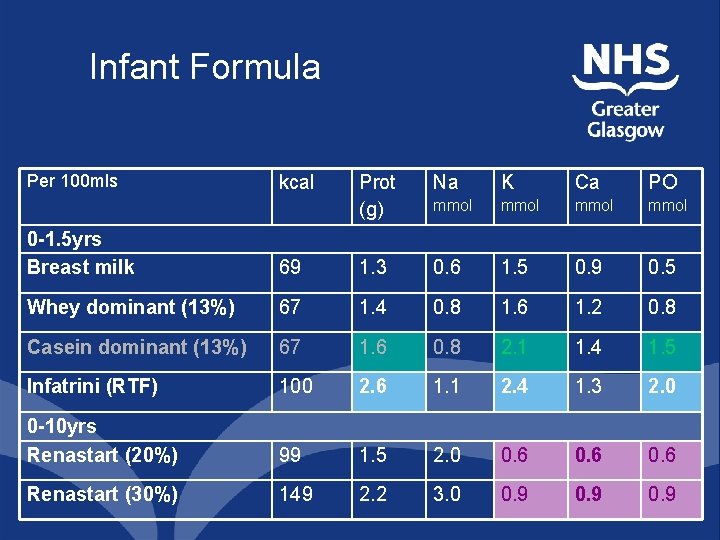
Infant Formula Per 100 mls kcal Prot (g) Na K Ca PO mmol 0 -1. 5 yrs Breast milk 69 1. 3 0. 6 1. 5 0. 9 0. 5 Whey dominant (13%) 67 1. 4 0. 8 1. 6 1. 2 0. 8 Casein dominant (13%) 67 1. 6 0. 8 2. 1 1. 4 1. 5 Infatrini (RTF) 100 2. 6 1. 1 2. 4 1. 3 2. 0 0 -10 yrs Renastart (20%) 99 1. 5 2. 0 0. 6 Renastart (30%) 149 2. 2 3. 0 0. 9

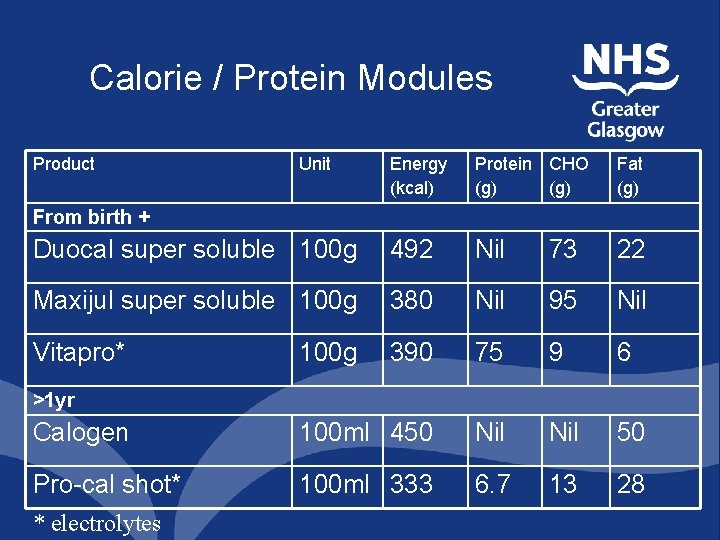
Calorie / Protein Modules Product Unit Energy (kcal) Protein CHO (g) Fat (g) Duocal super soluble 100 g 492 Nil 73 22 Maxijul super soluble 100 g 380 Nil 95 Nil Vitapro* 390 75 9 6 Calogen 100 ml 450 Nil 50 Pro-cal shot* 100 ml 333 6. 7 13 28 From birth + 100 g >1 yr * electrolytes

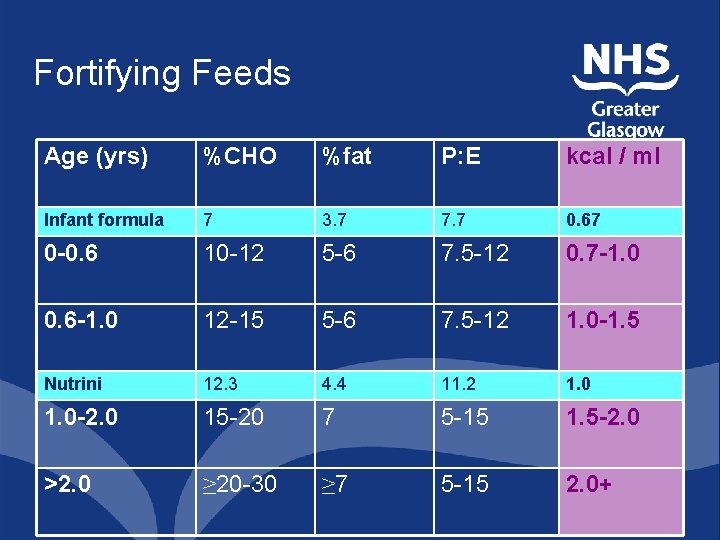
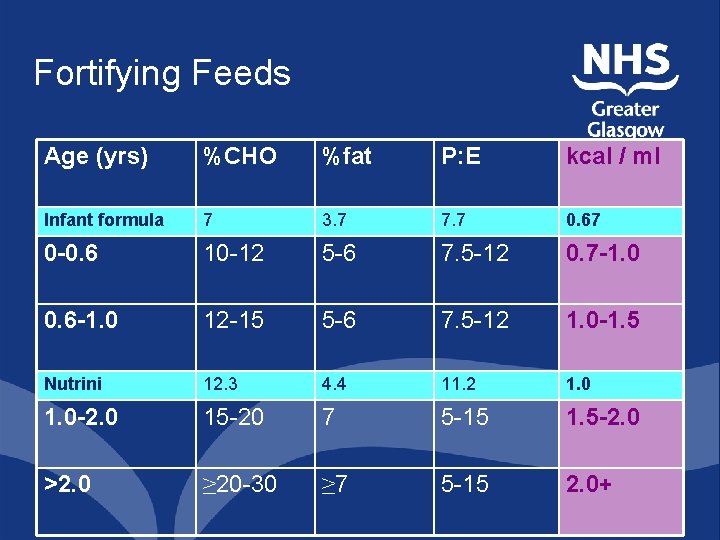
Fortifying Feeds Age (yrs) %CHO %fat P: E kcal / ml Infant formula 7 3. 7 7. 7 0. 67 0 -0. 6 10 -12 5 -6 7. 5 -12 0. 7 -1. 0 0. 6 -1. 0 12 -15 5 -6 7. 5 -12 1. 0 -1. 5 Nutrini 12. 3 4. 4 11. 2 1. 0 -2. 0 15 -20 7 5 -15 1. 5 -2. 0 >2. 0 ≥ 20 -30 ≥ 7 5 -15 2. 0+

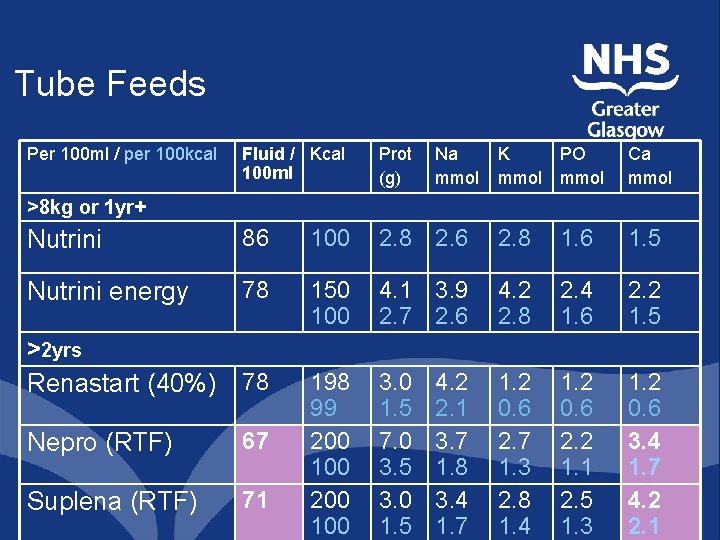
Tube Feeds Per 100 ml / per 100 kcal Fluid / Kcal 100 ml Prot (g) Nutrini 86 100 Nutrini energy 78 Renastart (40%) 78 Nepro (RTF) 67 Suplena (RTF) 71 Na mmol K mmol PO mmol Ca mmol 2. 8 2. 6 2. 8 1. 6 1. 5 150 100 4. 1 3. 9 2. 7 2. 6 4. 2 2. 8 2. 4 1. 6 2. 2 1. 5 198 99 200 100 3. 0 1. 5 7. 0 3. 5 3. 0 1. 5 1. 2 0. 6 2. 7 1. 3 2. 8 1. 4 1. 2 0. 6 2. 2 1. 1 2. 5 1. 3 1. 2 0. 6 3. 4 1. 7 4. 2 2. 1 >8 kg or 1 yr+ >2 yrs 4. 2 2. 1 3. 7 1. 8 3. 4 1. 7

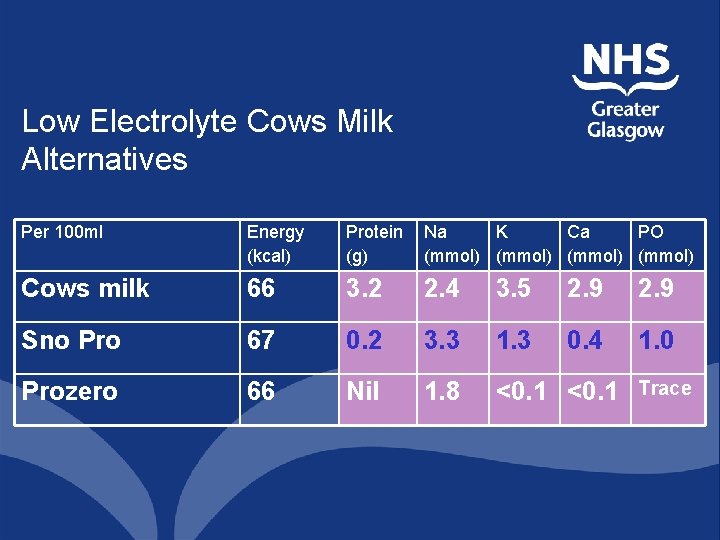
Low Electrolyte Cows Milk Alternatives Per 100 ml Energy (kcal) Protein (g) Na K Ca PO (mmol) Cows milk 66 3. 2 2. 4 3. 5 2. 9 Sno Pro 67 0. 2 3. 3 1. 3 0. 4 1. 0 Prozero 66 Nil 1. 8 <0. 1 Trace

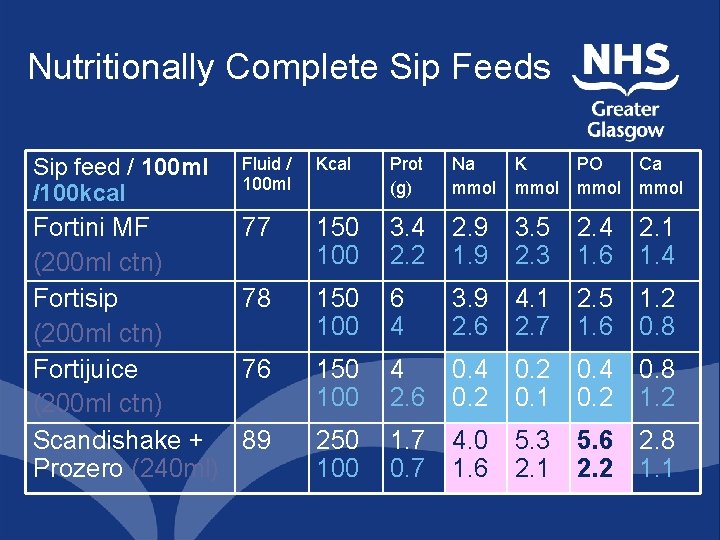
Nutritionally Complete Sip Feeds Sip feed / 100 ml /100 kcal Fluid / 100 ml Kcal Prot (g) Na mmol K mmol PO mmol Ca mmol Fortini MF (200 ml ctn) Fortisip (200 ml ctn) Fortijuice (200 ml ctn) Scandishake + Prozero (240 ml) 77 150 100 3. 4 2. 2 2. 9 1. 9 3. 5 2. 3 2. 4 1. 6 2. 1 1. 4 78 150 100 6 4 3. 9 2. 6 4. 1 2. 7 2. 5 1. 6 1. 2 0. 8 76 150 100 4 2. 6 0. 4 0. 2 0. 1 0. 4 0. 2 0. 8 1. 2 89 250 100 1. 7 0. 7 4. 0 1. 6 5. 3 2. 1 5. 6 2. 2 2. 8 1. 1

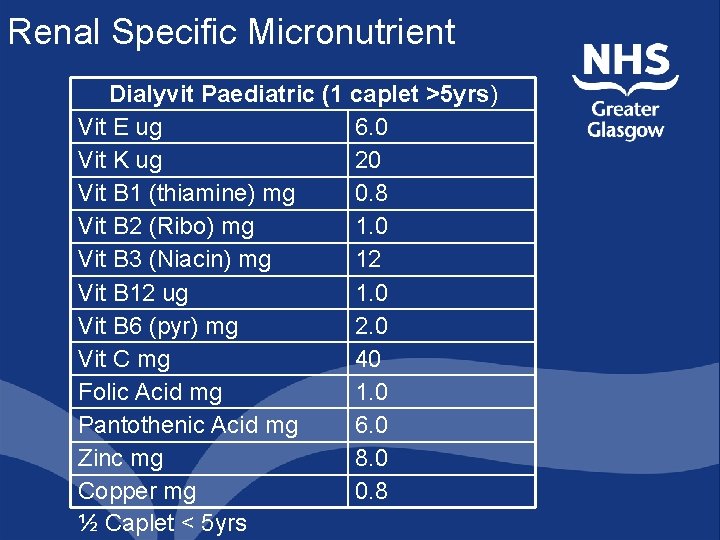
Renal Specific Micronutrient Dialyvit Paediatric (1 caplet >5 yrs) Vit E ug 6. 0 Vit K ug 20 Vit B 1 (thiamine) mg 0. 8 Vit B 2 (Ribo) mg 1. 0 Vit B 3 (Niacin) mg 12 Vit B 12 ug 1. 0 Vit B 6 (pyr) mg 2. 0 Vit C mg 40 Folic Acid mg 1. 0 Pantothenic Acid mg 6. 0 Zinc mg 8. 0 Copper mg 0. 8 ½ Caplet < 5 yrs

Case study 1 • 9 mth old boy – DW 8 kg (9 th) & 70 cm (9 -25 th) • Δ renal dysplasia • PD catheter inserted • PEG & fundo in situ • Fluid allowance 800 ml = 100 ml/kg • Very poor diet Hx Meds: Na. Cl; Na. HCO; 1 -alpha; Ca carb; domperidone; ranitidine U&E: Na 138; K 4. 5; HCO 20; Ur 16; Cr 518; Ca 2. 6; PO 1. 9

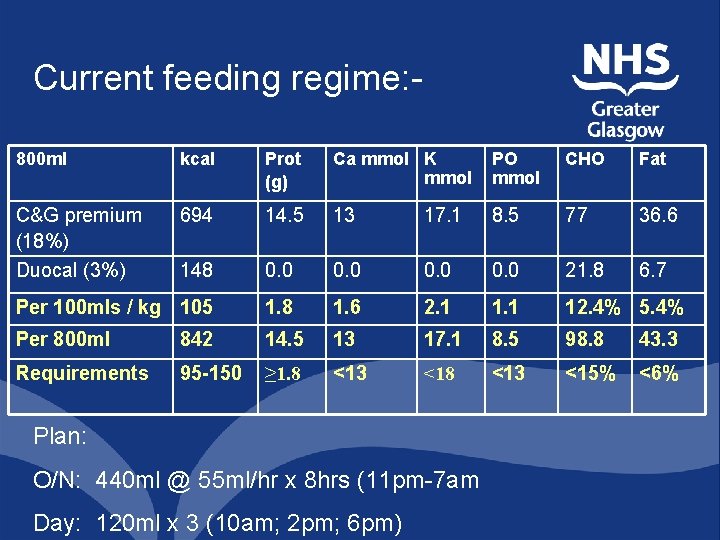
Current feeding regime: 800 ml kcal Prot (g) Ca mmol K mmol PO mmol CHO Fat C&G premium (18%) Duocal (3%) 694 14. 5 13 17. 1 8. 5 77 36. 6 148 0. 0 21. 8 6. 7 Per 100 mls / kg 105 1. 8 1. 6 2. 1 12. 4% 5. 4% Per 800 ml 842 14. 5 13 17. 1 8. 5 98. 8 43. 3 Requirements 95 -150 ≥ 1. 8 <13 <15% <6% Plan: O/N: 440 ml @ 55 ml/hr x 8 hrs (11 pm-7 am Day: 120 ml x 3 (10 am; 2 pm; 6 pm)

Continued… PC. PD drainage issues • Fluid restricted to 650 ml • Vomiting – reluctant to e&d • K 6. 6 • PO 2. 5

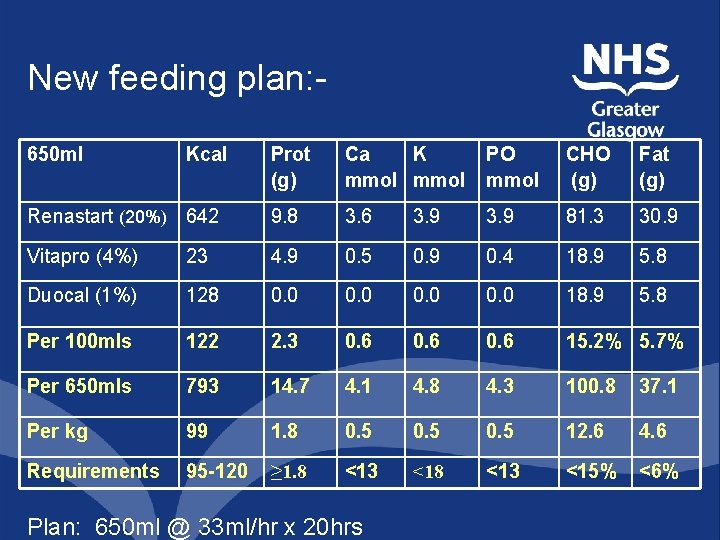
New feeding plan: 650 ml Kcal Prot (g) Ca K mmol PO mmol CHO (g) Fat (g) Renastart (20%) 642 9. 8 3. 6 3. 9 81. 3 30. 9 Vitapro (4%) 23 4. 9 0. 5 0. 9 0. 4 18. 9 5. 8 Duocal (1%) 128 0. 0 18. 9 5. 8 Per 100 mls 122 2. 3 0. 6 15. 2% 5. 7% Per 650 mls 793 14. 7 4. 1 4. 8 4. 3 100. 8 37. 1 Per kg 99 1. 8 0. 5 12. 6 4. 6 Requirements 95 -120 ≥ 1. 8 <13 <15% <6% Plan: 650 ml @ 33 ml/hr x 20 hrs

Case study 2 • • 6 yr 11 mth girl ESRF Lap fundo + PEG + PD DW 21 kg (25 th) & ht 114. 7 (9 -25 th) Fluid restriction 1. 4 L/d Poor DHx Meds: EPO; Lactulose; Losartan; KCl; Sytron; Na. HCO; Domperidone; Ranitidine; GH; Sevelemar • U&E: Na 139; K 4. 6; HCO 21; Ur 14; Cr 410; Ca 2. 5; PO 2. 5; Alb 33; PTH 17

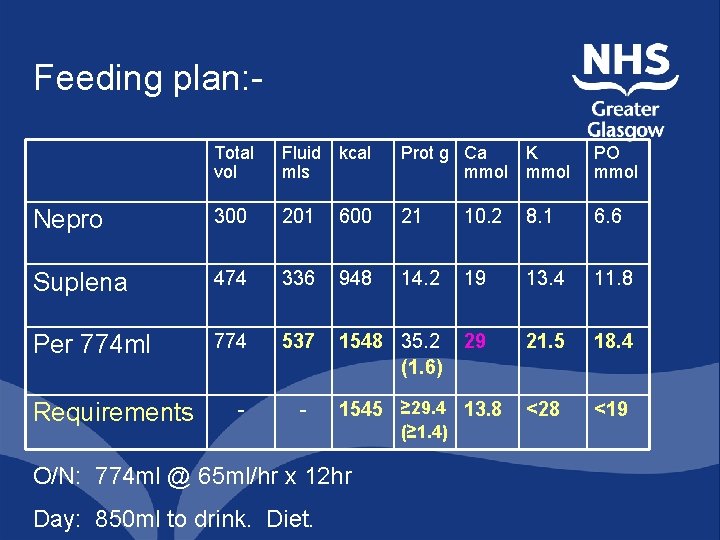
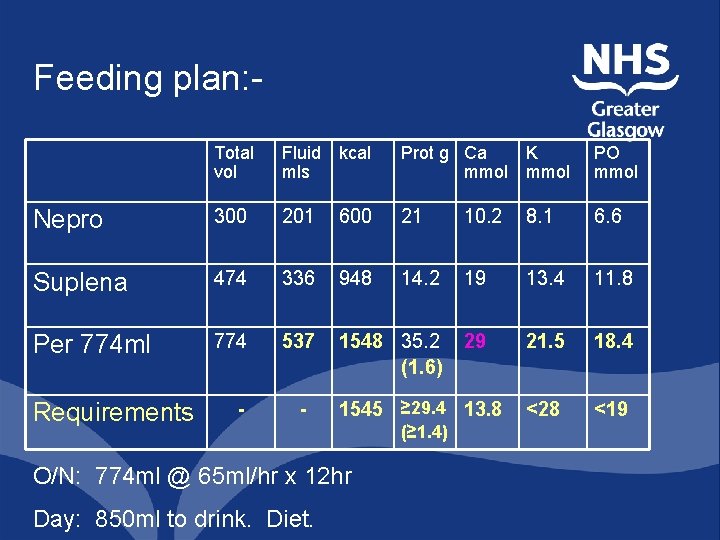
Feeding plan: Total vol Fluid kcal mls Prot g Ca mmol K mmol PO mmol Nepro 300 201 600 21 10. 2 8. 1 6. 6 Suplena 474 336 948 14. 2 19 13. 4 11. 8 Per 774 ml 774 537 1548 35. 2 (1. 6) 29 21. 5 18. 4 <28 <19 Requirements - - 1545 ≥ 29. 4 13. 8 O/N: 774 ml @ 65 ml/hr x 12 hr Day: 850 ml to drink. Diet. (≥ 1. 4)

Fortifying Feeds Age (yrs) %CHO %fat P: E kcal / ml Infant formula 7 3. 7 7. 7 0. 67 0 -0. 6 10 -12 5 -6 7. 5 -12 0. 7 -1. 0 0. 6 -1. 0 12 -15 5 -6 7. 5 -12 1. 0 -1. 5 Nutrini 12. 3 4. 4 11. 2 1. 0 -2. 0 15 -20 7 5 -15 1. 5 -2. 0 >2. 0 ≥ 20 -30 ≥ 7 5 -15 2. 0+

Feeding plan: Total vol Fluid kcal mls Prot g Ca mmol K mmol PO mmol Nepro 300 201 600 21 10. 2 8. 1 6. 6 Suplena 474 336 948 14. 2 19 13. 4 11. 8 Per 774 ml 774 537 1548 35. 2 (1. 6) 29 21. 5 18. 4 <28 <19 Requirements - - 1545 ≥ 29. 4 13. 8 O/N: 774 ml @ 65 ml/hr x 12 hr Day: 850 ml to drink. Diet. (≥ 1. 4)

Case study 3 • • • 14 yr old boy ESRF HD (3 x/wk) Fluid restriction 1000 ml DW 40 kg (9 th) IDWt gain: 3. 2 kg Ht: 160 (25 -50 th) U&E: Na 140; K 6; HCO 20; Ur 24; Cr 1166; Ca 2. 4; PO 1. 9; PTH 33; • meds: Ca carb; enalapril; Dialyvit; folic A; Ergo; Darbo; venofer. PC: hyperkalaemia; hyperphosphataemia fluid overloaded; hypertensive

Diet History Breakfast • Fruitibix (50 g) + ssmilk 200 ml • ssm 50 ml with meds Mid-morn • Walkers s’n’v + Diet Coke (330 ml) Lunch • Pizza (c’n’t) (180 g) • Diet Coke (330 ml) Mid-afternoon • Kit. Kat (2) Dinner • Jacket Spud (180 g) + Beans (130 g) + Cheese (30 g) • Icecream (2 sc). Diluting juice (90 ml) 1528 kcal; 54 g prot; 70 mmol K ; 40 mmol PO; 98 mmol Na

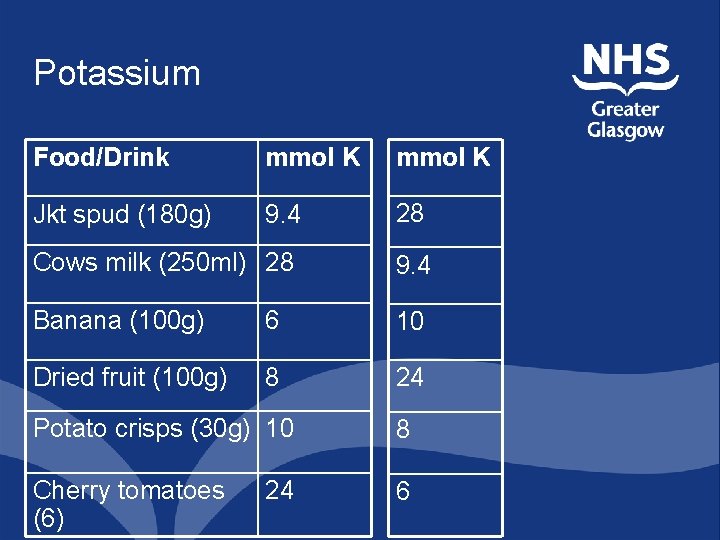
Potassium Food/Drink mmol K Jkt spud (180 g) 9. 4 28 Cows milk (250 ml) 28 9. 4 Banana (100 g) 6 10 Dried fruit (100 g) 8 24 Potato crisps (30 g) 10 8 Cherry tomatoes (6) 6 24

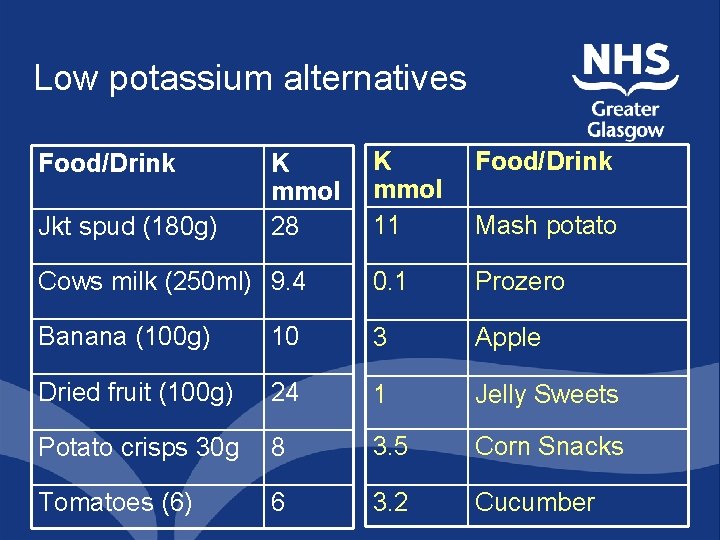
Low potassium alternatives K mmol 11 Food/Drink Cows milk (250 ml) 9. 4 0. 1 Prozero Banana (100 g) 10 3 Apple Dried fruit (100 g) 24 1 Jelly Sweets Potato crisps 30 g 8 3. 5 Corn Snacks Tomatoes (6) 6 3. 2 Cucumber Food/Drink Jkt spud (180 g) K mmol 28 Mash potato

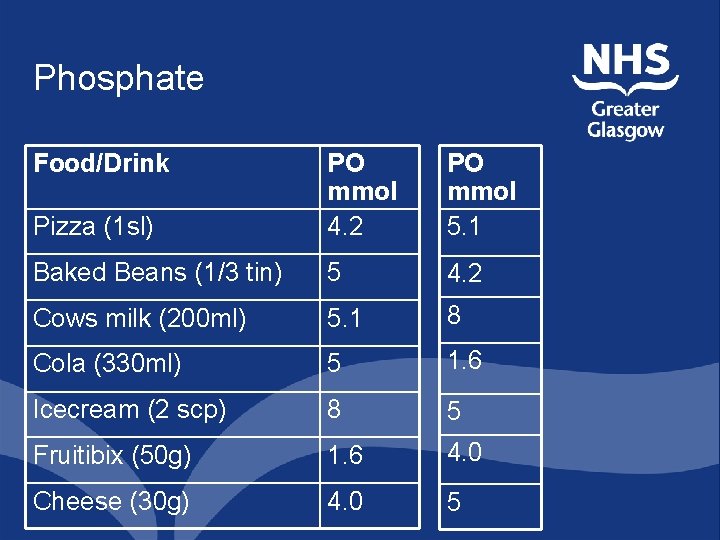
Phosphate Food/Drink Pizza (1 sl) PO mmol 4. 2 PO mmol 5. 1 Baked Beans (1/3 tin) 5 4. 2 Cows milk (200 ml) 5. 1 8 Cola (330 ml) 5 1. 6 Icecream (2 scp) 8 5 Fruitibix (50 g) 1. 6 4. 0 Cheese (30 g) 4. 0 5

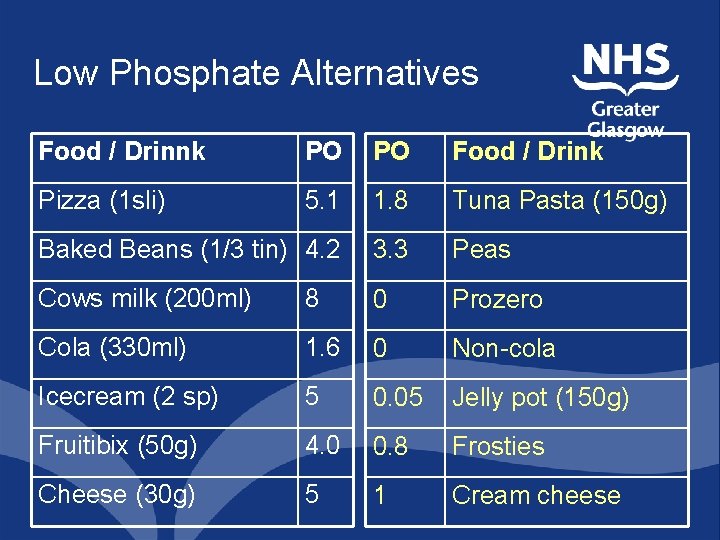
Low Phosphate Alternatives Food / Drinnk PO PO Food / Drink Pizza (1 sli) 5. 1 1. 8 Tuna Pasta (150 g) Baked Beans (1/3 tin) 4. 2 3. 3 Peas Cows milk (200 ml) 8 0 Prozero Cola (330 ml) 1. 6 0 Non-cola Icecream (2 sp) 5 0. 05 Jelly pot (150 g) Fruitibix (50 g) 4. 0 0. 8 Frosties Cheese (30 g) 5 1 Cream cheese

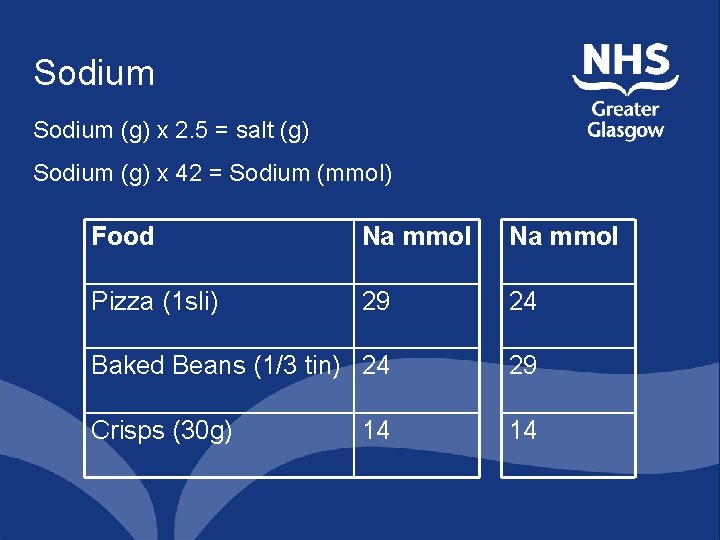
Sodium (g) x 2. 5 = salt (g) Sodium (g) x 42 = Sodium (mmol) Food Na mmol Pizza (1 sli) 29 24 Baked Beans (1/3 tin) 24 29 Crisps (30 g) 14 14

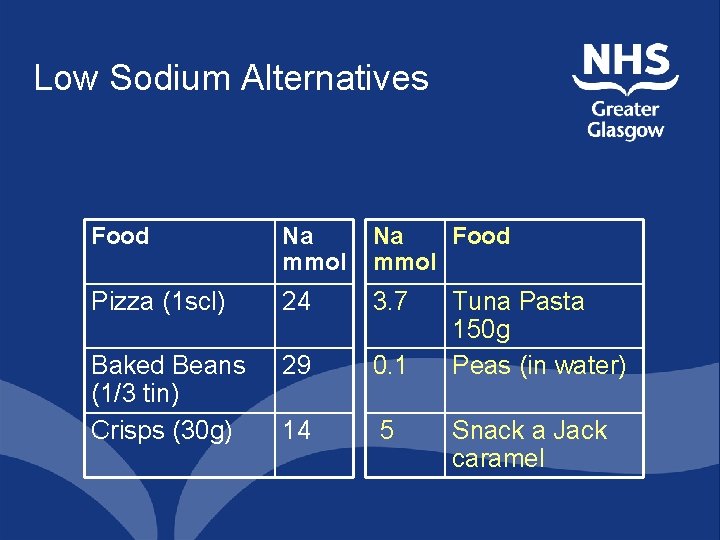
Low Sodium Alternatives Food Na mmol Na Food mmol Pizza (1 scl) 24 3. 7 Baked Beans (1/3 tin) Crisps (30 g) 29 0. 1 14 5 Tuna Pasta 150 g Peas (in water) Snack a Jack caramel

Diet History Breakfast • Fruitibix (50 g) + ssmilk 200 ml • ssm 50 ml (with meds) Mid-morn • Walkers s’n’v + Diet Coke (330 ml) Lunch • Pizza (c’n’t) (180 g) • Diet Coke (330 ml) Mid-afternoon • Kit. Kat (2) Dinner • Jacket Spud (180 g) + Beans (130 g) + Cheese (30 g) • Icecream (2 sc). Diluting juice (90 ml) 1528 kcal; 54 g prot; 70 mmol K ; 40 mmol PO; 98 mmol Na

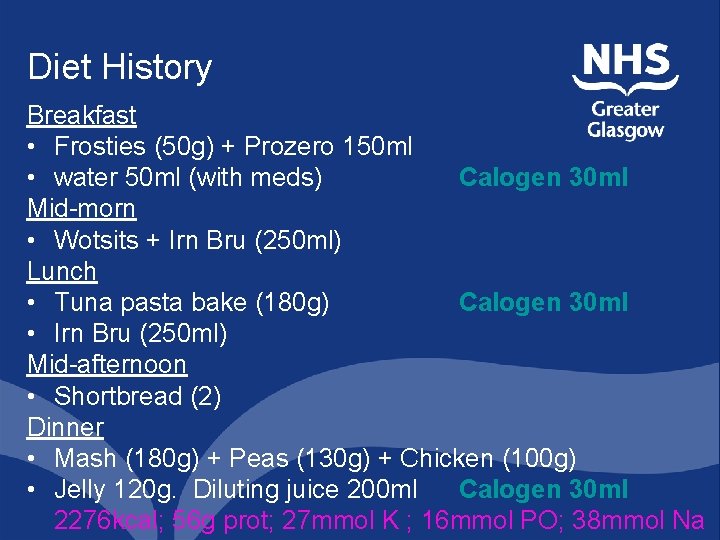
Diet History Breakfast • Frosties (50 g) + Prozero 150 ml • water 50 ml (with meds) Calogen 30 ml Mid-morn • Wotsits + Irn Bru (250 ml) Lunch • Tuna pasta bake (180 g) Calogen 30 ml • Irn Bru (250 ml) Mid-afternoon • Shortbread (2) Dinner • Mash (180 g) + Peas (130 g) + Chicken (100 g) • Jelly 120 g. Diluting juice 200 ml Calogen 30 ml 2276 kcal; 56 g prot; 27 mmol K ; 16 mmol PO; 38 mmol Na

References KDOKI Clinical Practice Guideline for Nutrition in Children with CKD. American Journal of Kidney Diseases, 2009, 53 s 1 -124. Royle, J The Kidney. In Clnical Paediatric Dietetics, 3 rd edition. 2007 pp 203238 Ruley EJ et al, Feeding disorders and gastrooesophagael reflux in infants with chronic renal failure. Ped Neph 1989: 3: 424 -429. Ledermann SE et al, Long-term outcomes of PD in infants. J Ped 136: 2429, 2000 Warady BA et al, Nutritional and behavioural aspects of NG tube feeding in infants receiving chronic PD. Adv Per Dial, 1990: 6: 265 -268. Ratsh IM et al, Energy and nutritient intake of patients with mild-moderate chronic renal failure. Eur J Ped, 1992: 151: 701 -705. Coleman JE. Micronutrient supplements for children. Br J Ren Med, 1998, 3 21 -23 Ledermann SE et al, Long-term enteral nutrition in infants and young children with chronic renal failure. Ped Neph, 1999, 13 870 -5. Coleman et al Provision of dietetic care in children on chronic PD. J Ren Nutr, 1999, 9 145 -8

Thank you very much