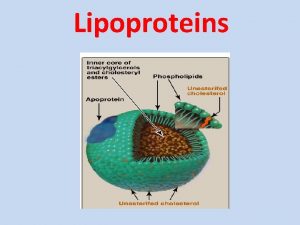
Metabolism of Lipoproteins Plasma lipoproteins The plasma lipoproteins
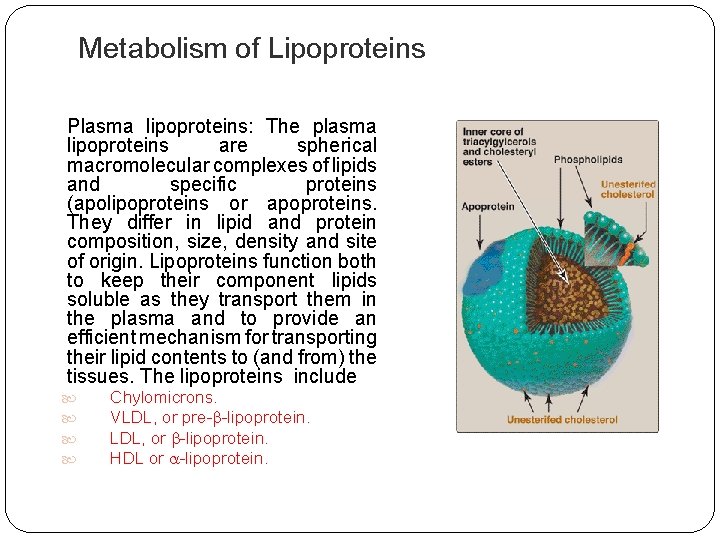
Metabolism of Lipoproteins Plasma lipoproteins: The plasma lipoproteins are spherical macromolecular complexes of lipids and specific proteins (apolipoproteins or apoproteins. They differ in lipid and protein composition, size, density and site of origin. Lipoproteins function both to keep their component lipids soluble as they transport them in the plasma and to provide an efficient mechanism for transporting their lipid contents to (and from) the tissues. The lipoproteins include Chylomicrons. VLDL, or pre- -lipoprotein. LDL, or -lipoprotein. HDL or -lipoprotein.
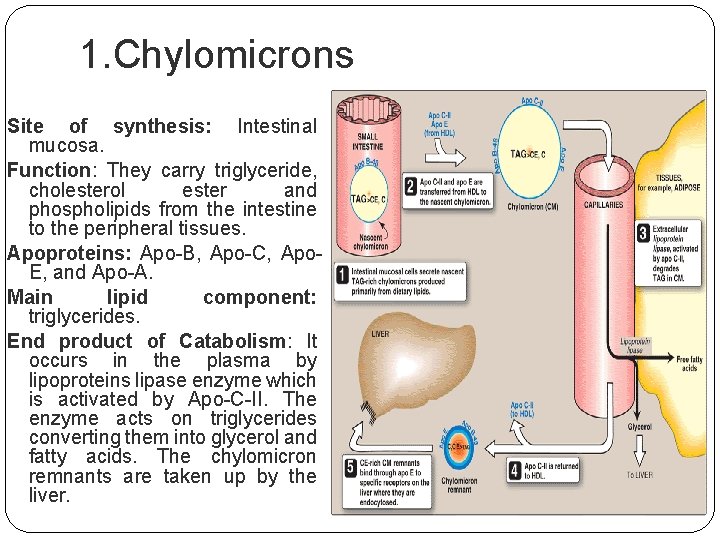
1. Chylomicrons Site of synthesis: Intestinal mucosa. Function: They carry triglyceride, cholesterol ester and phospholipids from the intestine to the peripheral tissues. Apoproteins: Apo-B, Apo-C, Apo. E, and Apo-A. Main lipid component: triglycerides. End product of Catabolism: It occurs in the plasma by lipoproteins lipase enzyme which is activated by Apo-C-II. The enzyme acts on triglycerides converting them into glycerol and fatty acids. The chylomicron remnants are taken up by the liver.
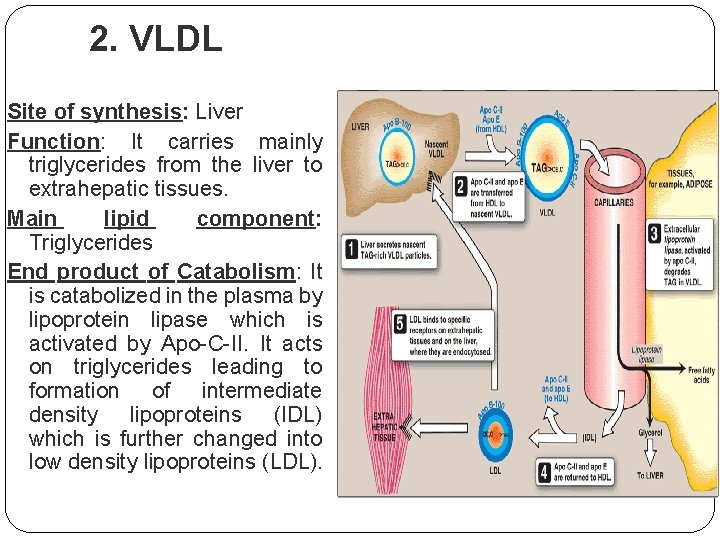
2. VLDL Site of synthesis: Liver Function: It carries mainly triglycerides from the liver to extrahepatic tissues. Main lipid component: Triglycerides End product of Catabolism: It is catabolized in the plasma by lipoprotein lipase which is activated by Apo-C-II. It acts on triglycerides leading to formation of intermediate density lipoproteins (IDL) which is further changed into low density lipoproteins (LDL).
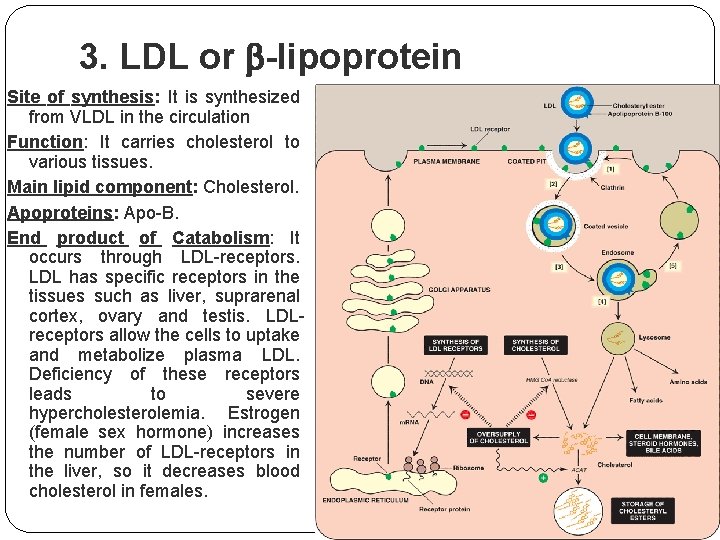
3. LDL or -lipoprotein Site of synthesis: It is synthesized from VLDL in the circulation Function: It carries cholesterol to various tissues. Main lipid component: Cholesterol. Apoproteins: Apo-B. End product of Catabolism: It occurs through LDL-receptors. LDL has specific receptors in the tissues such as liver, suprarenal cortex, ovary and testis. LDLreceptors allow the cells to uptake and metabolize plasma LDL. Deficiency of these receptors leads to severe hypercholesterolemia. Estrogen (female sex hormone) increases the number of LDL-receptors in the liver, so it decreases blood cholesterol in females.
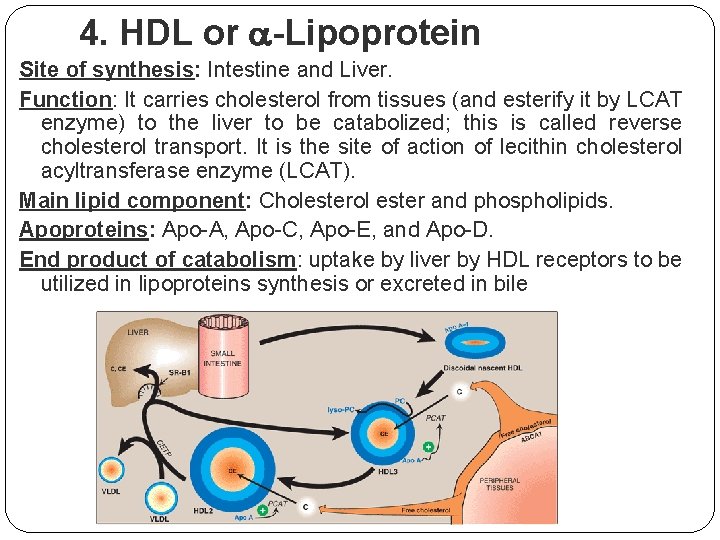
4. HDL or -Lipoprotein Site of synthesis: Intestine and Liver. Function: It carries cholesterol from tissues (and esterify it by LCAT enzyme) to the liver to be catabolized; this is called reverse cholesterol transport. It is the site of action of lecithin cholesterol acyltransferase enzyme (LCAT). Main lipid component: Cholesterol ester and phospholipids. Apoproteins: Apo-A, Apo-C, Apo-E, and Apo-D. End product of catabolism: uptake by liver by HDL receptors to be utilized in lipoproteins synthesis or excreted in bile

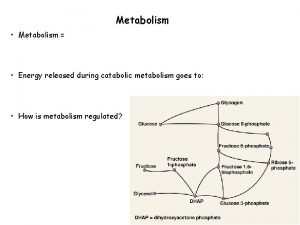
Cholesterol Metabolism Biosynthesis of cholesterol: Site and carbon source: - The cytosol of liver is the major site of cholesterol biosynthesis, and other tissues (e. g. , the intestine, adrenals, gonads, skin, neural tissue, brain (of new-born) and aorta. - All carbon atoms of cholesterol are derived from acetyl-Co. A, with the initial steps similar to ketogenesis. Steps: 1. Formation of Mevalonate 2. Formation of of squalene 3. Cyclization of squalene to form lanosterol 4. Conversion of lanosterol to cholesterol:
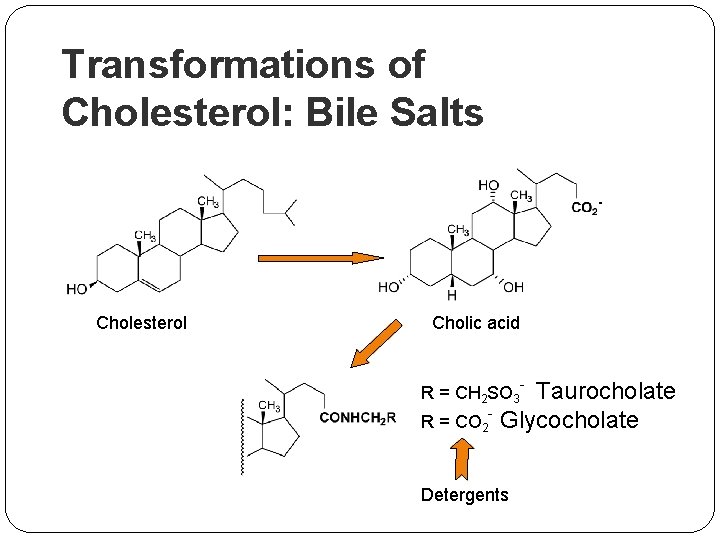
Transformations of Cholesterol: Bile Salts Cholesterol Cholic acid - Taurocholate R = CO 2 Glycocholate R = CH 2 SO 3 Detergents

: Functions of bile acids 1. Emulsification of dietary fats, , form micelles with lipids that help their absorption, 2. Activation of pancreatic lipase 3. Help absorption of fat-soluble vitamins. 4. Stimulate intestinal motility, 5. Choleretic (stimulates its own secretion), 6. Solubilize cholesterol in the bile juice, 7. Buffer stomach acid, and have antiseptic effect in the intestine (prevent putrefaction).
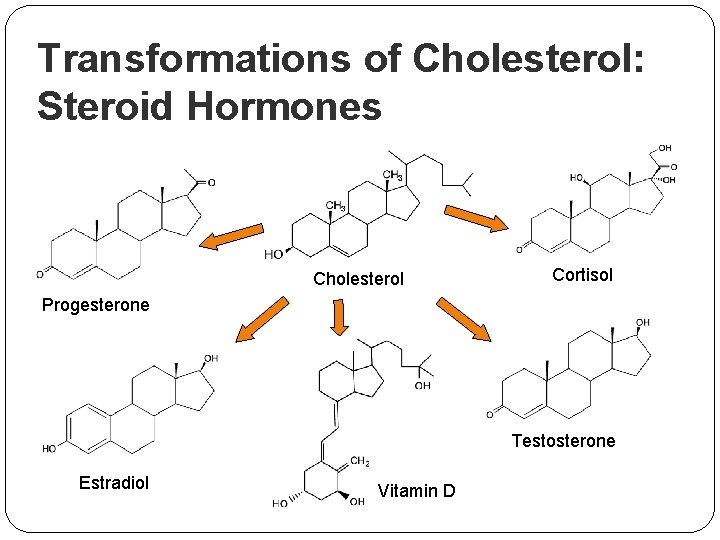
Transformations of Cholesterol: Steroid Hormones Cholesterol Cortisol Progesterone Testosterone Estradiol Vitamin D
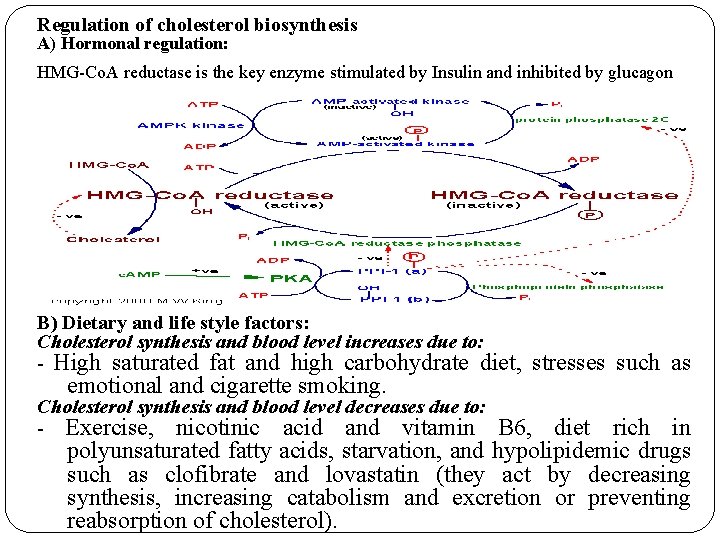
Regulation of cholesterol biosynthesis A) Hormonal regulation: HMG-Co. A reductase is the key enzyme stimulated by Insulin and inhibited by glucagon B) Dietary and life style factors: Cholesterol synthesis and blood level increases due to: - High saturated fat and high carbohydrate diet, emotional and cigarette smoking. Cholesterol synthesis and blood level decreases due to: - Exercise, nicotinic acid and vitamin stresses such as B 6, diet rich in polyunsaturated fatty acids, starvation, and hypolipidemic drugs such as clofibrate and lovastatin (they act by decreasing synthesis, increasing catabolism and excretion or preventing reabsorption of cholesterol).

Atherosclerosis: Definition: It is a disease condition in which cholesterol esters and other lipids remaining in the oxidized-LDL are deposited in subendothelial layers of the wall of the arteries. Causes: It associates hyperlipidemic conditions such as diabetes mellitus, hypothyroidism and inherited hyperlipidemias. Prevention: Polyunsaturated fatty acids from vegetable oils prevent this disease by mobilizing cholesterol as esters to the liver, stimulating conversion into bile acids, increasing expression of hepatic receptors for LDL and prevent LDL uptake by blood vessels. Vegetable oils contain natural antioxidants that prevent the oxidative modification of LDL that are not being removable by the liver.
Fatty Liver Definition: It is the accumulation of abnormal amount of fat in liver leading to impairment of its functions Factors regulating fat content of the liver: 1. Dietary lipid content. 2. Rate of denovo synthesis of fatty acids in the liver. 3. Rate of mobilizing fatty acids from adipose tissue to the liver. 4. Rate of mobilization of fat from liver to blood then to adipose tissue. 5. Rate of oxidation of fatty acids in the liver.

Causes: 1. Over-feeding of fats (dietary type): This leads to increased circulating chylomicrons that is taken up by liver (pinocytosis) or acted upon by lipoprotein lipase that release their fatty acids which can be taken up by the liver for reesterification, synthesis of triacylglycerols and secretion of more VLDL. 2. Over-feeding of carbohydrates (dietary type): : Surplus carbohydrate supply is converted into fatty acids and triacylglycerols and secreted as VLDL from the liver to go to adipose tissue. This leads to high blood level of VLDL, LDL and triacylglycerols. 3. Over-mobilization of fat from adipose tissue to liver (physiological type): In conditions with carbohydrate deficiency, e. g. , carbohydrate-free diet, starvation or conditions with impaired carbohydrate utilization, e. g. , in diabetes mellitus. Over-lipolysis in adipose tissue depletes its lipid content and prevents it from reesterifying free fatty acids due to absence of glycerol kinase. The liver has to control blood free fatty acid concentration by reesterifying them into triacylglycerols. This leads to hyperlipidemia and ketosis and/or ketoacidosis.

4. Under-mobilization of fat from the liver to the plasma (pathological type): It is due to absence or deficiency of factors required by the liver to synthesize VLDL and/or secretes it. These include deficient apolipoproteins and lipotropic factors such as phosphoglycerolipids, polyunsaturated fatty acids and vitamins (B complex) required for their synthesis. 5. Liver poisons (toxic type): It is caused by damage to liver cells by toxins such as carbon tetrachloride that inhibits apolipoprotein synthesis among other effects 6. Alcoholism: Ethyl alcohol causes increased triacylglycerols and cholesterol synthesis, inhibit fatty acid oxidation and lipid secretion from the liver 7. Deficiency of Lipotropic factors

Lipotropic factors Definition: They are nutritional factors that facilitate mobilization of fat from the liver and prevent fatty liver (particularly the pathological type). They include: 1. Essential polyunsaturated fatty acids. They are required for synthesis of phospholipids and cholesterol esters. 2. Vitamin B complex. B 12 and folate are very essential in transmethylation, e. g. , ethanolamine into choline. Lack of pantothenic acid (Vit. B 5) leads to deficiency of Co. ASH required for fatty acid activation. Deficiency of B 6 interferes with polyunsaturated fatty acids and Co. ASH metabolism. 3. Choline, inositol and methionine. They are required for synthesis of phospholipids. Other essential amino acids are required for synthesis of apolipoproteins. Casein is lipotropic due to its high biological value and high content of methionine. 4. Proteins of high biological value: including all essential amino acids required for apoproteins, choline and carnitine synthesis.

THANK YOU
- Slides: 16