MANAGEMENT OF ACUTE AND CHRONIC PANCREATITIS R A
























- Slides: 35

MANAGEMENT OF ACUTE AND CHRONIC PANCREATITIS R. A. Singh MD FRCPC AGAF Clinical Assistant Professor of Medicine Division of Gastroenterology, UBC

Disclosures • Speaker honorarium from: Takeda Abbvie Janssen Pentax • Clinical Research Funds Celgene Gilead Takeda Janssen No financial disclosures for this specific talk

Learning Objectives • Distinguish the pathophysiology, complications and management between acute and chronic pancreatitis • Distinguish between the in- patient management between acute and chronic pancreatitis

Introduction • Acute Pancreatitis (AP) and Chronic Pancreatitis(CP) are two distinct disease states • Most common cause of AP is gallstones and alcohol • Less common cause include hyperlipidemia, hypercalcemia, celiac disease, autoimmune, drugs • Chronic Pancreatitis is rarely dealt with in hospital • CP is usually caused by alcohol • Smoking is an independent risk factor for CP progression

Pathophysiology • Acute pancreatitis is caused by acute inflammation of the pancreatic parenchyma • Acute inflammation can lead to systemic inflammatory response syndrome ( SIRS) • SIRS can lead to respiratory depression, renal failure and hypovolemic shock • Sepsis is typically caused by transmural lumenal bacterial migration

Pathophysiology • Chronic pancreatitis is caused by chronic inflammation and fibrosis • This damage can lead to exocrine dysfunction ( diarrhea) or endocrine dysfunction ( diabetes) and cancer • Pain is common • Acute on chronic pancreatitis is caused by acute parenchymal inflammation on the background of CP • This leads to self limited abdominal pain and short stays in hospital • Serious acute complications are rare

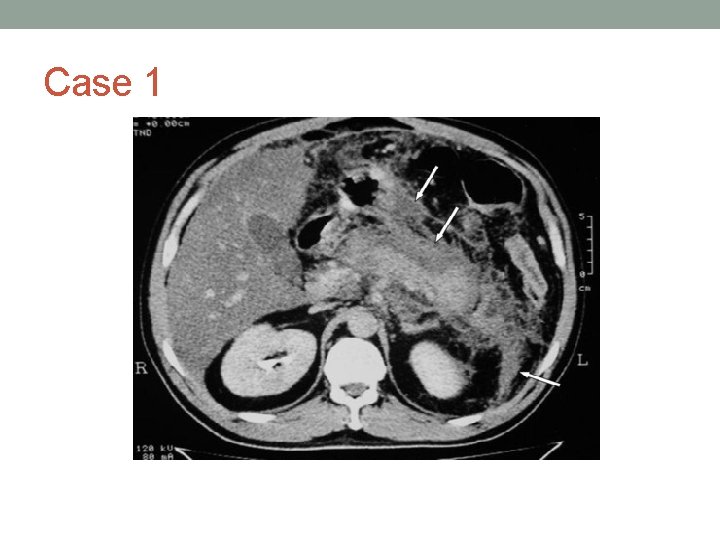
Case 1 • 35 year old woman presents with 24 h of epigastric pain, emesis • History of alcohol abuse ( 1 bottle vodka/d) • No meds • T 36. 8, P 92, BP 147/92, RR 15 Sa. O 2 95% on Rm air • Tender in Epigastrium • JVP difficult to see • Chest clear • WBC, 19. 4, HGB 175, urea 4. 9, Cr 80, GLU 8, Ca 2. 20, LFTs N, Lipase 620 • Diagnosis : Acute Alcoholic Pancreatitis

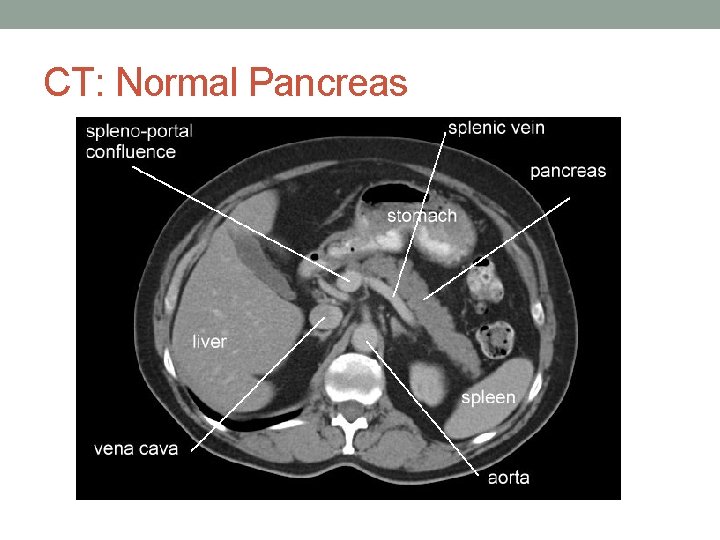
CT: Normal Pancreas

Case 1

Case 1 Initial resuscitation should be aggressive 250 -300 cc/h Monitor urine output CIWA protocol Avoid excessive analgesics/sedation DVT Prophylaxis Practical Nursing Issues: Wide range narcotics dangerous Monitor urine output (poorly done) Monitor Resp/ O 2 saturations Check for DVT prophylaxis

Case 1 ( 12 h post admission) • Patient has been on the ward for 2 h • Urine output 50 cc/hr • Pain under control. BP/P stable. RR 22/min Sa. O 2 92% • No evidence of withdrawal • Concerns? • RR is increased , Sa. O 2 decreased • Next steps • Notify MRP, ABG, CXR, increase O 2 • CXR shows bilateral pleural effusions and evidence of pulmonary edema • ABG( Room Air) p. H 7. 32 PO 2 60, PCO 2 55 BE 6

Case 1 • ICU asked to assess • Patient brought to ICU for observation • Patient continues to deteriorate in ICU and is intubated within 2 hr of admission to ICU ( 16 h post admission) • Practical Nursing Issues: AP patients can deteriorate quickly, changes in respiratory status can be subtle

Case 1 • Severity of Pancreatitis difficult to assess on admission • Number of Scoring Models to assess Severity • Ranson’s Criteria is the most commonly used : • Admission Age >55 WBC >16, 000 GLU > 11 LDH >350 AST >250 48 h Fall in HCT >10% Increase BUN>1. 98 Ca < 2 mmol p. O 2 <60 mm. Hg BE>4 Fluid Seq>6 L Severe Pancreatitis greater or equal to 3

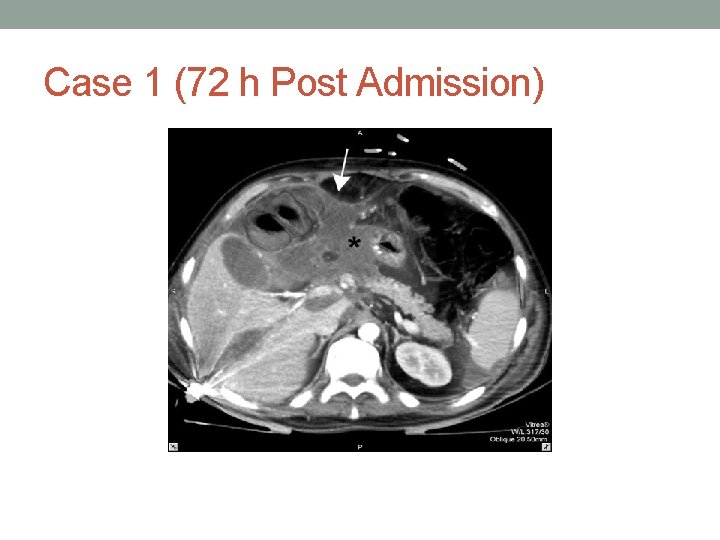
Case 1 • Radiographic Evidence of Necrosis, Significant Peripancreatitic edema/fluid indicate severe pancreatitis • Admission CT may not show necrosis or significant peripancreatic edema

Case 1 (72 h Post Admission)

Case 1 • Severe Pancreatitis based on Ranson’s Criteria and CT • Enteral feeds should be considered for all patients with severe pancreatitis • Feeding should start by 72 h • NG feeds likely acceptable • Semi elemental feeds

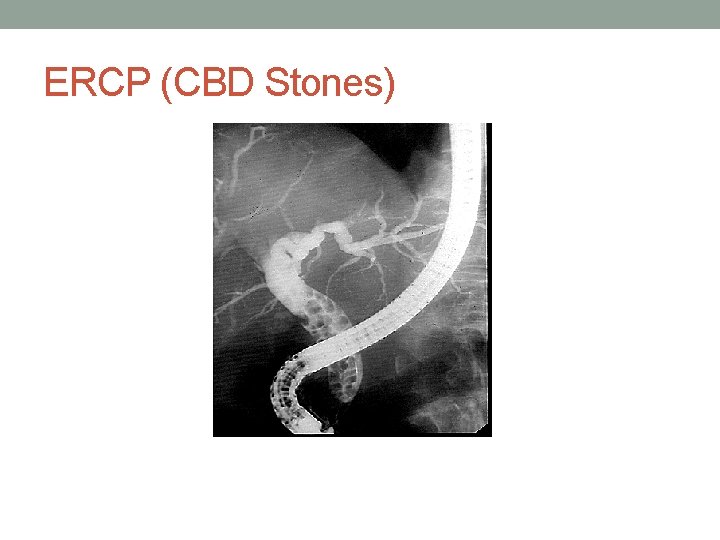
Case 1: Role for ERCP? • ERCP indicated for biliary pancreatitis with jaundice, dilated biliary tree, ascending cholangitis • If risk for stone is low or moderate, less invasive imaging with MRCP or EUS indicated first

ERCP (CBD Stones)

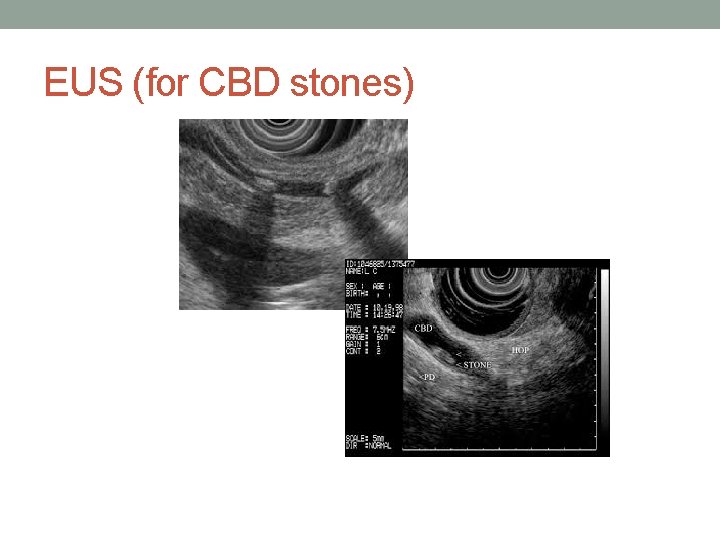
EUS (for CBD stones)

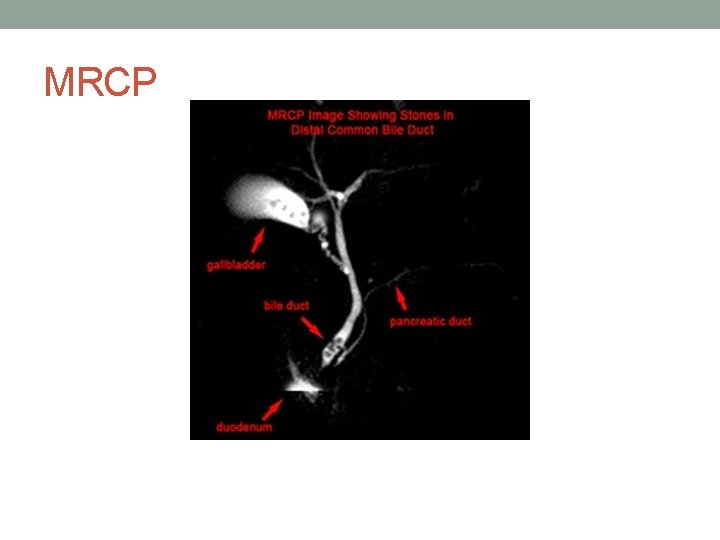
MRCP

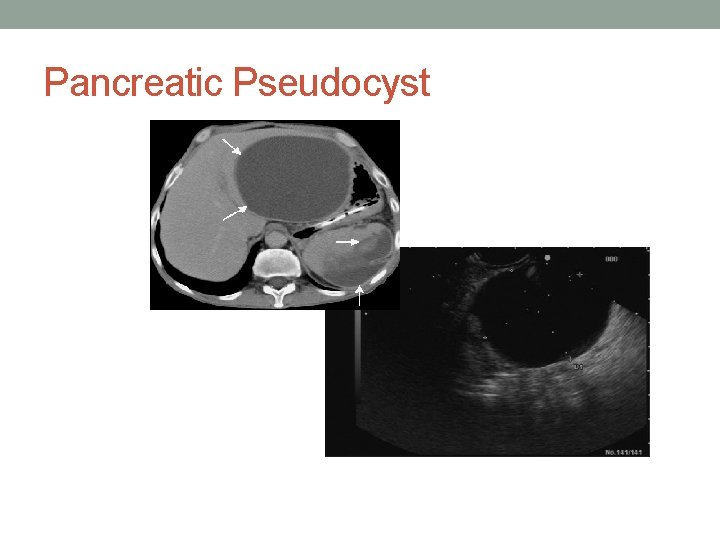
Case 1 • Patient recovers and is discharged • She represents to hospital 2 months later with LUQ pain, early satiety and intermittent emesis. VSS; afebrile • Lab work shows a mild increase in lipase, normal WBC • CT shows a large 9 x 6 cm loculated cyst in the lesser sac compressing the stomach • Diagnosis : Pseudocyst

Pancreatic Pseudocyst

Pancreatic Pseudocyst Drainage • Percutaneous Drainage • Endoscopic Drainage ( ERCP v EUS approach) • Surgical

Percutaneous Drainage • Largely historical interest • Used primarily for acutely infected fluid collections • Drainage results poor • Fistula formation

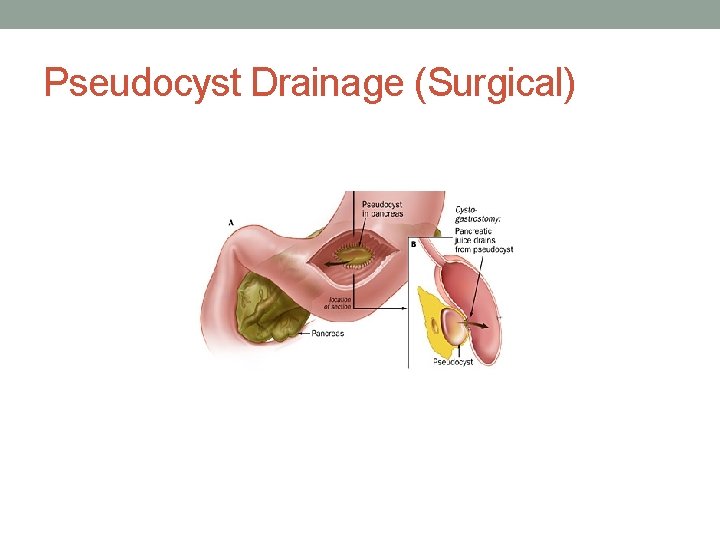
Surgical Drainage • More morbid than endoscopic drainage • Indicated for Complex loculated pseudocysts • Indicated for Cysts not causing bulge in the stomach • Indicated for failed drainage procedures

Pseudocyst Drainage (Surgical)

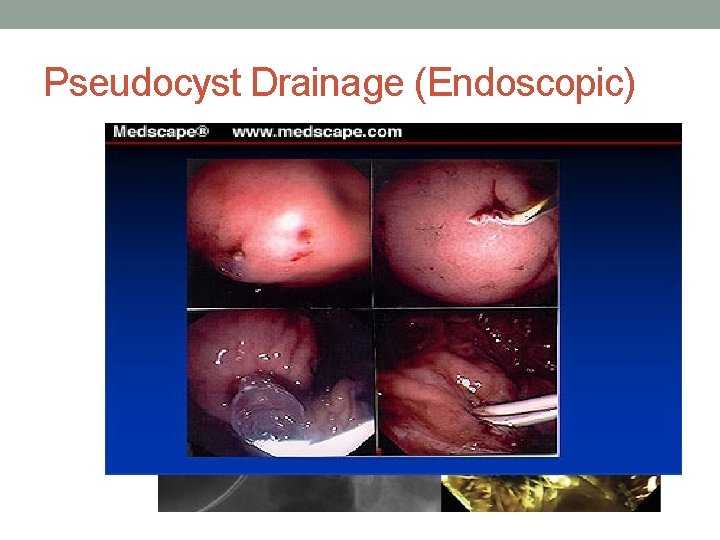
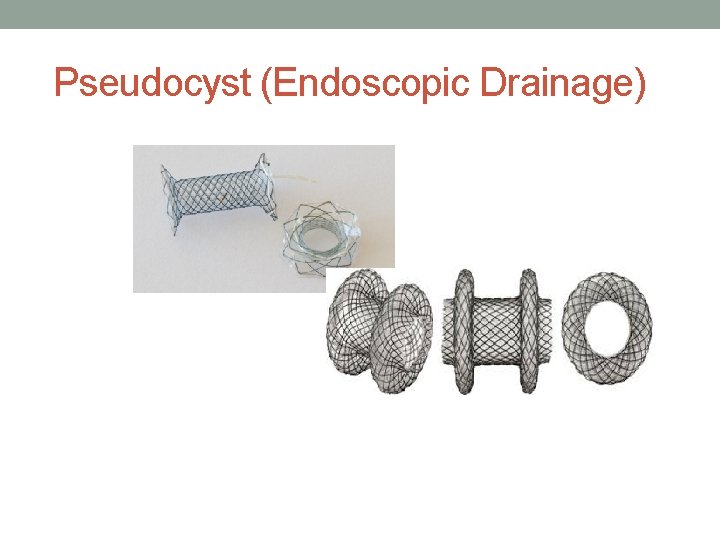
Pseudocyst Drainage ( Endoscopic) • ERCP approach. Needle knife cut followed by placement of double pigtail stents • EUS guided and placement of fully covered metal stent • Echoendoscope is not the ideal scope for pseudocyst draineage

Pseudocyst Drainage (Endoscopic)

Pseudocyst (Endoscopic Drainage)

Acute Pancreatitis Key Points • First 48 h crucial • Aggressive fluid resuscitation required • Urine output should be monitored • Remember DVT prophylaxis • Beware of respiratory compromise and sepsis • Enteral feeding should be started early in SAP • Pseudocyst drainage can often be managed endoscopically

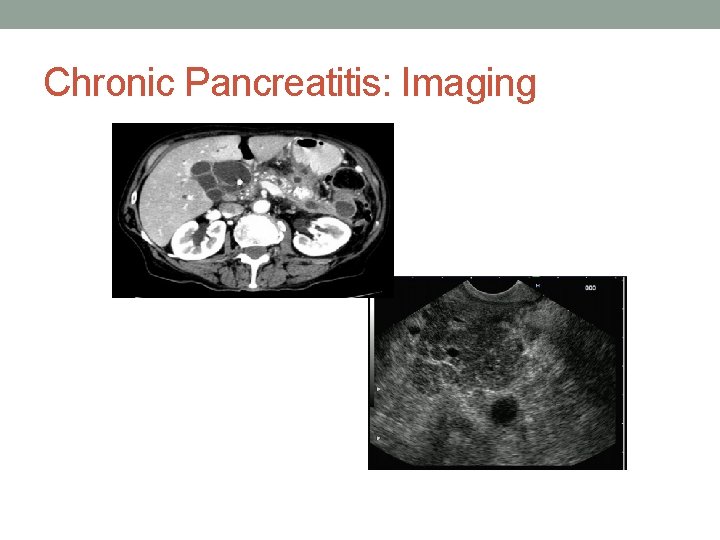
Case 2 • 43 yo man presents with epigastric pain for weeks. Some nausea. No vomiting. • Vitals stable; afebrile • CBC, lytes, BUN/Cr normal. GLU 10. 5 • Lipase 250 • CT Atrophic Pancreas, Numerous Calcifications in Pancreatic parenchyma. No peripancreatic edema or fluid • Dx Acute exacerbation of CP

Chronic Pancreatitis: Imaging

Chronic Pancreatitis: Management • IV fluids and analgesics • Little risk of infection, SIRS or respiratory failure • Symptoms usually settle in a few days • Push for Alcohol and smoking cessation • Complications are typically long term such as pancreatic insufficiency, biliary obstruction and cancer • May be a role for pancreatic enzymes for pain control • Minimal role for EUS guided celiac plexus blockade

Chronic Pancreatitis: Risk of Cancer • Well documented increased risk • No surveillance guidelines • Tumour is often difficult to distinguish from focal chronic pancreatitis

Chronic Pancreatitis: Key Points • Hospitalized patients follow a benign course • Management is largely supportive • Priority is to eliminate triggers ( e. g. alcohol and smoking) • Pancreatic enzymes can be used to treat pain or steatorrhea