Haz Mat for WV Hospitals Decontamination Disposal Documentation





































- Slides: 45

Haz. Mat for WV Hospitals: Decontamination, Disposal, Documentation Module IV

This course was developed by En. Magine, who we wish to gratefully acknowledge. The material has been modified by WV DHHR in cooperation with the West Virginia Hospital Association’s Disaster Preparedness Task Force in the teaching of Hospital Decontamination.

Objectives • Explain decontamination procedures for victims, personnel, and equipment. • Discuss application of relevant Standard Operating Procedures. • Describe proper disposal and documentation procedures during a Decon response.

Decontamination • Removing or neutralizing contaminants – Personnel – Equipment

Types of Decon • Primary/Technical – Done at the scene, usually by Emergency Services • Secondary – Done at hospital for patients who received decon at the scene (detailed decon) • Emergency – Done at hospital for patients who have bypassed on-scene decon

Who, What, When & Why • Who/What: People & equipment – Patients – Responders – Equipment

Who, What, When & Why • Who should do Decon : – properly trained & equipped personnel • What/How to Decon: – Decon individuals who have not received primary decon and those who need secondary decon – No absolute method of decon – Only general guides for decon

Who, What, When & Why • When: Anytime you suspect contamination – Material is visible – Patient complains of pain, odor, etc. – Patient was in the release

Who, What, When & Why: Degree of Contamination • • • Amount of material on the patient Length of time it’s on the patient Concentration of material Physical state of material Ambient temperatures

Who, What, When & Why • Why: Prevent escalation of problem – Exposure: patient is exposed to release or product – Contamination: it is on patient – Exposure of others; contamination of facility, etc.

Who, What, When & Why Consequences of No Decon • Acute/Chronic health effects • Problem gets bigger • Death!

Performing Decon • Physical removal • Chemical removal • Emergency Decon

Performing Decon • Procedures follow logical order • Go from “dirty” to “clean” • Check your plan

Decon Procedures • Anytime you suspect contamination • Use common sense – Life risk – Level of exposure

Decon Procedures • Remove all clothing from victim – Including undergarments • Use copious amounts of water – Copious=more than you have used • Large amounts: high volume

Decon Procedures • Precautions – Avoid contact w/clothing (use PPE) – Ensure privacy of victim(s) • Barriers/garments • Segregate by gender

Decon Procedures • Hospital Considerations – Did individuals receive decon prior to transport? – Protect staff/facility/equipment – Secure contaminated clothing

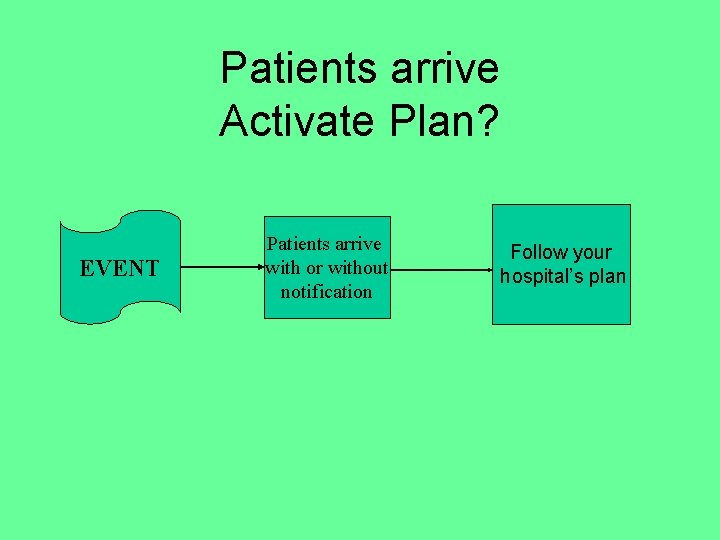
Patients arrive Activate Plan? EVENT Patients arrive with or without notification Follow your hospital’s plan

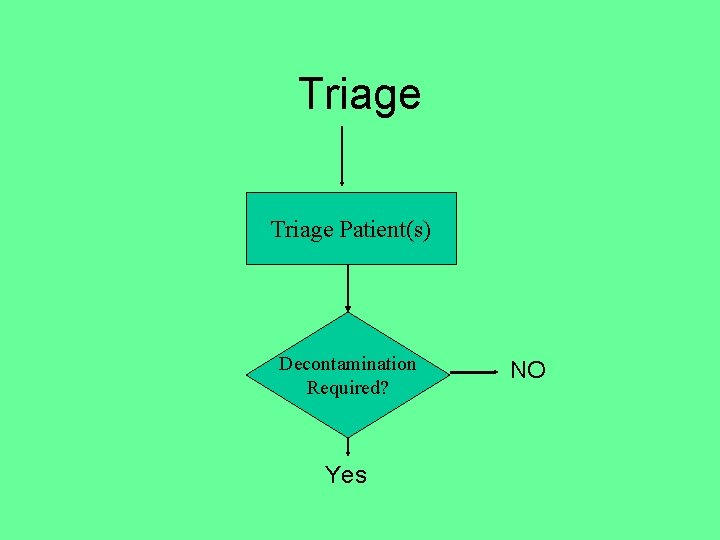
Triage Patient(s) Decontamination Required? Yes NO

No decon required NO Patient(s) to Treatment Area Assess and Treat Disposition

Decon required Yes Activate hospital Decon protocols Collect personal belongings/ evidence** Secondary Triage Emergency Treatment required?

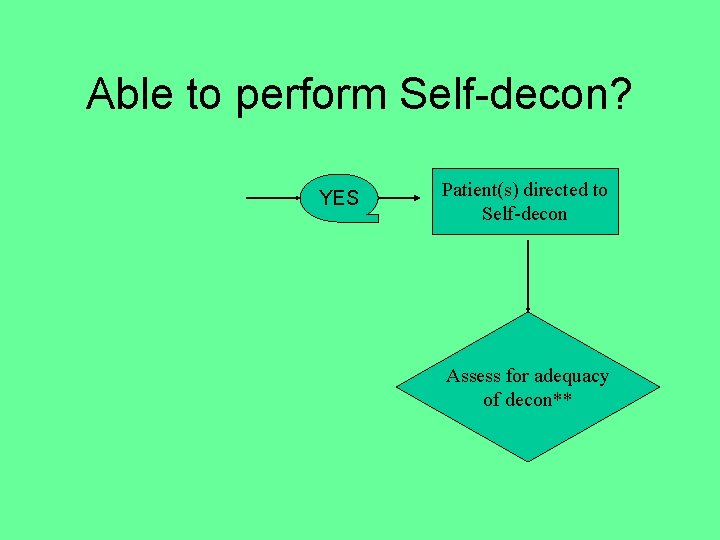
Able to perform Self-decon? YES Patient(s) directed to Self-decon Assess for adequacy of decon**

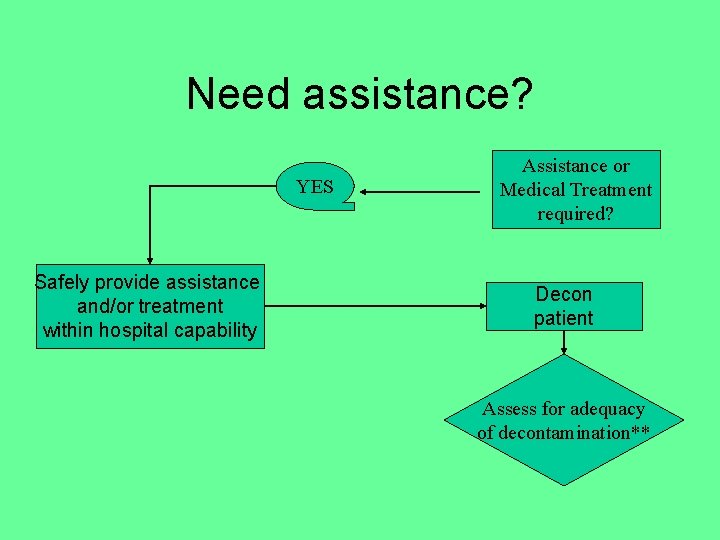
Need assistance? YES Safely provide assistance and/or treatment within hospital capability Assistance or Medical Treatment required? Decon patient Assess for adequacy of decontamination**

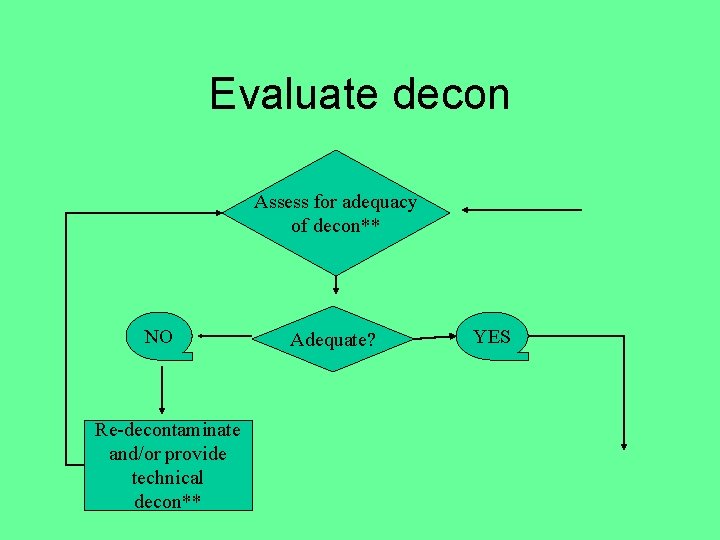
Evaluate decon Assess for adequacy of decon** NO Re-decontaminate and/or provide technical decon** Adequate? YES

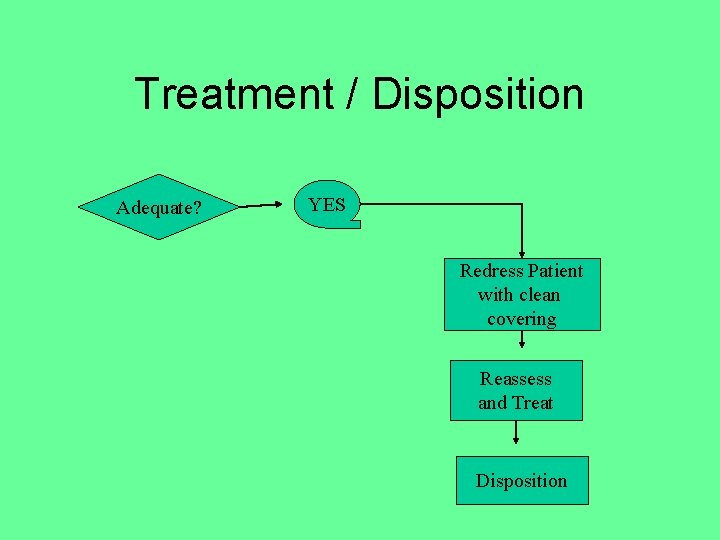
Treatment / Disposition Adequate? YES Redress Patient with clean covering Reassess and Treat Disposition

Medical Management of Contaminated Patients • Is patient in severe distress? – Airway compromise? – Severe wheezing or respiratory distress? – Persistent nausea/vomiting? – Having a seizure? • May need emergency medical treatment – Chemical antidotes (atropine, 2 PAM, etc. ) – Intubation

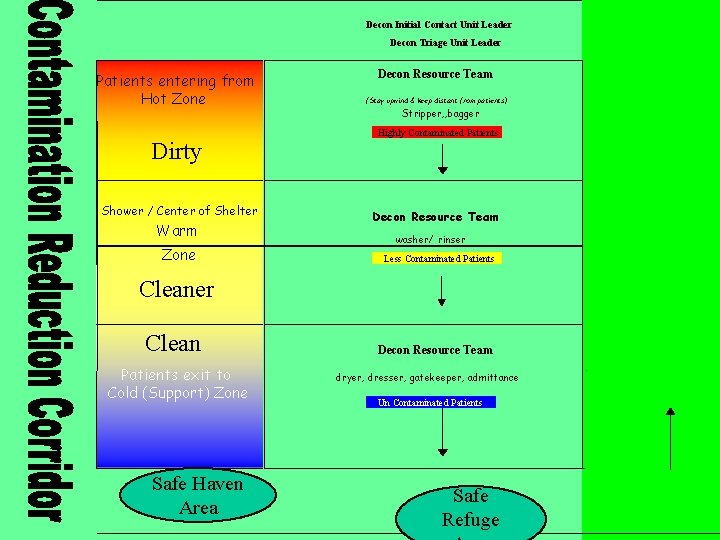
Decon Initial Contact Unit Leader Decon Triage Unit Leader Patients entering from Hot Zone Dirty Shower / Center of Shelter Warm Zone Decon Resource Team (Stay upwind & keep distant from patients) Stripper, , bagger Highly Contaminated Patients Decon Resource Team washer/ rinser Less Contaminated Patients Cleaner Clean Patients exit to Cold (Support) Zone Safe Haven Area Decon Resource Team dryer, dresser, gatekeeper, admittance Un Contaminated Patients Safe Refuge

Decon Organization • Decon Group Positions – – – Decon Group Supervisor Technical Reference Site Access Control Decon Leader Entry Leader Assistant Safety Officer* • *Reports to Safety Officer

Decon Resource Team

Decontamination Procedures

Mass Decon Hospital Based

Photos courtesy of Andrew Fulton, CREM



What do you do/ if one of the Decon Resource Team goes down?

Reasons for Documentation of Decon Activities • Cost recovery • Exposure records

Disposal of Contaminated Items All contaminated items are to be bagged and in a secure location until they can properly removed and de-contaminated /disposed of by a licensed firm or government agency.

Components of Documentation • Date, time and location • Names of all response personnel – What jobs were they assigned? • Incident conditions, observations and statements • Material name/s, weather conditions

Components of Documentation • Actions taken, resources used, costs incurred • Statements & Observations of witnesses • Diagrams, photos, and video

Decon Exposure Records Mike Zolotoff Salazar, Robert • Keep exposure records! – Employer must keep for 30 years • All responders: keep own copies

Decon Exposure Records • Date, time and location of incident • Chemical name • Decon or medical aid given

Post Event Monitoring • Personnel (Work w/Employee Health Services) – Respiratory Monitoring – Chronic and Acute exposure and affects – Chemical Exposure Records for files

Role of the FRO • Safely and competently respond • Within appropriate – – Level – Resources and – Capabilities

Summary of Module IV - Decon • Decon of victims – Who, What, When, Why – How to decon – Directed, self decon vs. Mass decon – Documentation – Disposal • Some may need medical management

Questions?