DKA DKA Precipitating Factors Failure to take insulin





















- Slides: 25

DKA

DKA Precipitating Factors • Failure to take insulin • Failure to increase insulin – Illness/Infection • Pneumonia • MI • Stroke – Acute stress • Trauma • Emotional • Medical Stress – Counterregulatory hormones • Oppose insulin • Stimulate glucagon release • Hypovolmemia – Increases glucagon and catecholamines • Decreased renal blood flow • Decreases glucagon degradation by the kidney

Diabetic Ketoacidosis Due to: Severe insulin deficiency Excess counterregulatory hormones Glucagon Epinephrine Cortisol Growth hormone

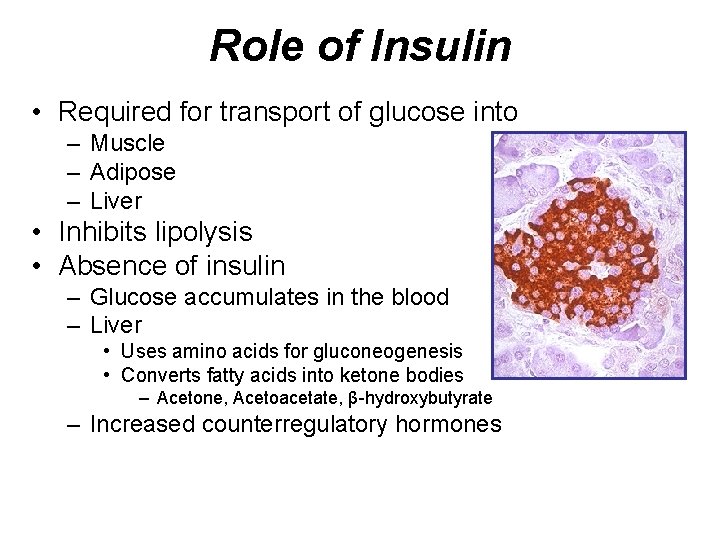
Role of Insulin • Required for transport of glucose into – Muscle – Adipose – Liver • Inhibits lipolysis • Absence of insulin – Glucose accumulates in the blood – Liver • Uses amino acids for gluconeogenesis • Converts fatty acids into ketone bodies – Acetone, Acetoacetate, β-hydroxybutyrate – Increased counterregulatory hormones

Counterregulatory Hormones - DKA Epinephrine Increases insulin resistance Activates glycogenolysis and gluconeogenesis Activates lipolysis Inhibits insulin secretion X X X Glucagon X Cortisol X Growth Hormone X X

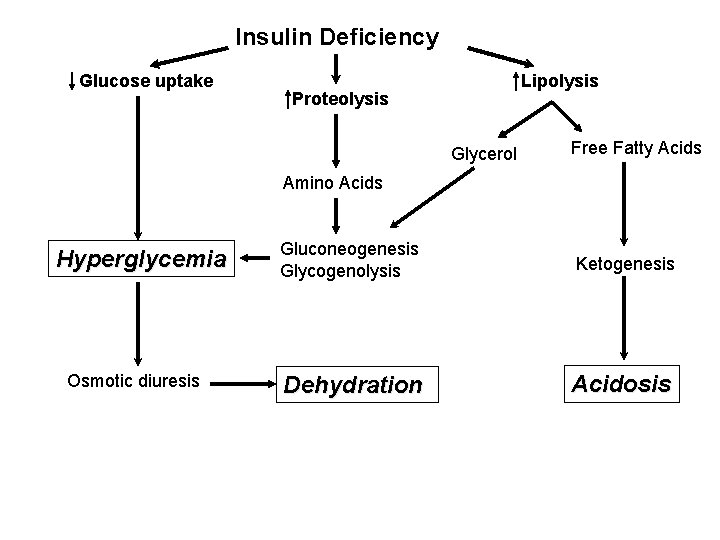
Insulin Deficiency Glucose uptake Lipolysis Proteolysis Glycerol Free Fatty Acids Amino Acids Hyperglycemia Osmotic diuresis Gluconeogenesis Glycogenolysis Ketogenesis Dehydration Acidosis

Signs and Symptoms of DKA • Polyuria, polydipsia – Enuresis • Dehydration – Tachycardia – Orthostasis • Abdominal pain – Nausea – Vomiting • Fruity breath – Acetone • Kussmaul breathing • Mental status changes – Combative – Drunk – Coma

Lab Findings • Hyperglycemia • Anion gap acidosis – (Na + K) – (Cl + Bicarb) >12 – Bicarbonate <15 m. Eq/L – p. H <7. 3 • Urine ketones and serum ketones • Hyperosmolarity

Differential Diagnosis Anion Gap Acidosis • • • Alcoholic ketoacidosis Lactic acidosis Renal failure Ethylene glycol or methyl alcohol poisoning Starvation in late pregnancy or lactation (rare)

Atypical Presentations • DKA can be present with BS <300 – Impaired gluconeogenesis • • Liver disease Acute alcohol ingestion Prolonged fasting Insulin-independent glucose is high (pregnancy) – Chronic poor control but taking insulin • Bedside urine ketones false negatives – Measure acetoacetate not β-hydroxybutyrate – Send blood to lab

Treatment of DKA Fluids and Electrolytes • Fluid replacement – Restores perfusion of the tissues • Lowers counterregulatory hormones – Average fluid deficit 3 -5 liters • Initial resuscitation – 1 -2 liters of normal saline over the first 2 hours – Slower rates of 500 cc/hr x 4 hrs or 250 cc/hr x 4 hours • When fluid overload is a concern • If hypernatremia develops ½ NS can be used

Treatment of DKA Fluids and Electrolytes • Hyperkalemia initially present – Resolves quickly with insulin drip – Once urine output is present and K<5. 0, add 20 -40 meq KCL per liter. • Phosphate deficit – May want to use Kphos • Bicarbonate not given unless p. H <7 or bicarbonate <5 mmol/L

Treatment of DKA Insulin Therapy • IV bolus of 0. 1 -0. 2 units/kg (~ 10 units) regular insulin • Follow with hourly regular insulin infusion • Glucose levels – Decrease 75 -100 mg/dl hour – Minimize rapid fluid shifts • Continue IV insulin until urine is free of ketones

Treatment of DKA Glucose Administration • Supplemental glucose – Hypoglycemia occurs • Insulin has restored glucose uptake • Suppressed glucagon – Prevents rapid decline in plasma osmolality • Rapid decrease in insulin could lead to cerebral edema • Glucose decreases before ketone levels decrease • Start glucose when plasma glucose <300 mg/dl

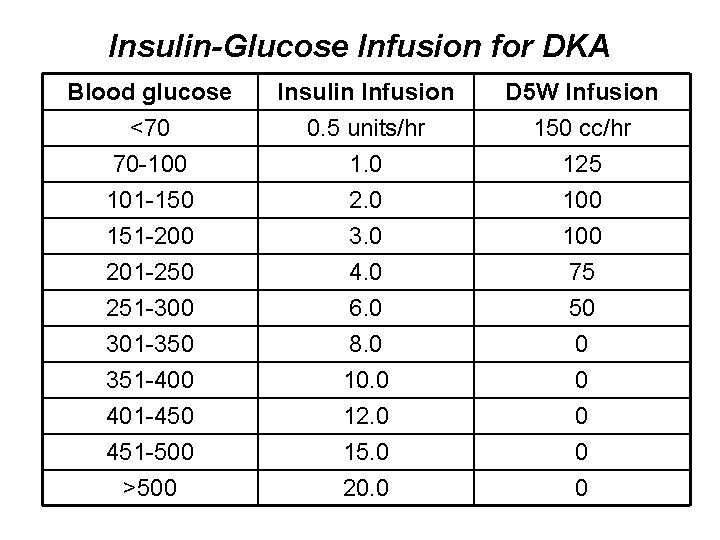
Insulin-Glucose Infusion for DKA Blood glucose <70 70 -100 101 -150 Insulin Infusion 0. 5 units/hr 1. 0 2. 0 D 5 W Infusion 150 cc/hr 125 100 151 -200 201 -250 251 -300 301 -350 351 -400 401 -450 451 -500 >500 3. 0 4. 0 6. 0 8. 0 10. 0 12. 0 15. 0 20. 0 100 75 50 0 0

Complications of DKA • Infection – Precipitates DKA – Fever – Leukocytosis can be secondary to acidosis • Shock – If not improving with fluids r/o MI • Vascular thrombosis – Severe dehydration – Cerebral vessels – Occurs hours to days after DKA • Pulmonary Edema – Result of aggressive fluid resuscitation • Cerebral Edema – – First 24 hours Mental status changes Tx: Mannitol May require intubation with hyperventilation

Once DKA Resolved Treatment • Most patients require 0. 5 -0. 6 units/kg/day • Pubertal or highly insulin resistant patients – 0. 8 -1. 0 units/kg/day • Long acting insulin – 1/2 -2/3 daily requirement – NPH, Lente, Ultralente or Lantus • Short acting insulin – 1/3 -1/2 given at meals – Regular, Humalog, Novolog • Give insulin at least 2 hours prior to weaning insulin infusion.

Prevention of DKA Sick Day Rules • Never omit insulin – Cut long acting in half • • • Prevent dehydration and hyperglycemia Monitor blood sugars frequently Monitor for ketosis Provide supplemental fast acting insulin Treat underlying triggers Maintain contact with medical team

Hyperosmolar Non-ketotic Syndrome • Extreme hyperglycemia and dehydration – Unable to excrete glucose as quickly as it enters the extracellular space – Maximum hepatic glucose output results in a plateau of plasma glucose no higher than 300500 mg/dl – When sum of glucose excretion plus metabolism is less than the rate which glucose enters extracellular space.

Hyperosmolar Non-ketotic Syndrome • Extreme hyperglycemia and hyperosmolarity • High mortality (12 -46%) • At risk – Older patients with intercurrent illness – Impaired ability to ingest fluids • Urine volume falls – Decreased glucose excretion • Elevated glucose causes CNS dysfunction and fluid intake impaired • No ketones – Some insulin may be present – Extreme hyperglycemia inhibits lipolysis

Hyperosmolar Nonketotic Syndrome Presentation • • Extreme dehydration Supine or orthostatic hypotension Confusion coma Neurological findings – Seizures – Transient hemiparesis – Hyperreflexia – Generalized areflexia

Hyperosmolar Nonketotic Syndrome Presentation • Glucose >600 mg/dl • Sodium – Normal, elevated or low • Potassium – Normal or elevated • Bicarbonate >15 m. Eq/L • Osmolality >320 m. Osm/L • Creatinine may increased

Hyperosmolar Nonketotic Syndrome Treatment • Fluid repletion – NS 2 -3 liters rapidly – Total deficit = 10 liters • Replete ½ in first 6 hours • Insulin – Make sure perfusion is adequate – Insulin drip 0. 1 U/kg/hr • Treat underlying precipitating illness

Clinical Errors • Fluid shift and shock – Giving insulin without sufficient fluids – Using hypertonic glucose solutions • Hyperkalemia – Premature potassium administration before insulin has begun to act • Hypokalemia – Failure to administer potassium once levels falling • Recurrent ketoacidosis – Premature discontinuation of insulin and fluids when ketones still present • Hypoglycemia – Insufficient glucose administration

Conclusion • Successful management requires – Judicious use of fluids • Establish good perfusion – Insulin drip • Steady decline • Complete resolution of ketosis – Electrolyte replacement – Frequent neurological evaluations – High suspicion for complications • Determine etiology to avoid recurrent episodes