Chapter 16 Adaptive Immunity 235 Adaptive immunity is








































- Slides: 69

Chapter 16 Adaptive Immunity 235 Adaptive immunity is the specific immunity in which the body is able to recognize and defend itself against the invader upon the subsequent infections to the same pathogen. Upon activation by an antigen, the B lymphocyte undergoes cell division to produce antibodies, and the T lymphocyte undergoes cell division to produce specific T cells to provide an adaptive or acquired immunity. This immunity is the third line of defense.

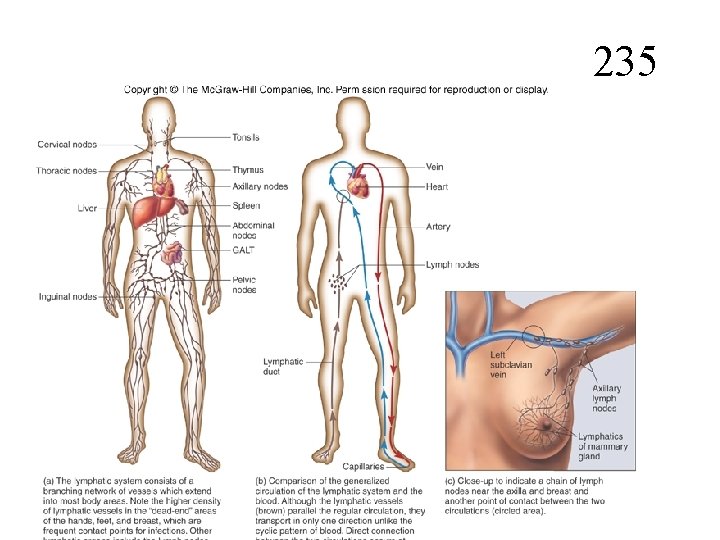
235 Lymphatic System: • Lymphatic vessels (lymphatics) • Lymph (Lymph fluid) • Lymph organs and tissues: thymus, spleen, tonsils, lymph nodes, appendix and clusters of tissues in the mucosa, the mucosa-associated lymphatic tissue (MALT) and gut (small intestine)- associated lymphatic tissue, the Peyer’s patches • Lymphocytes

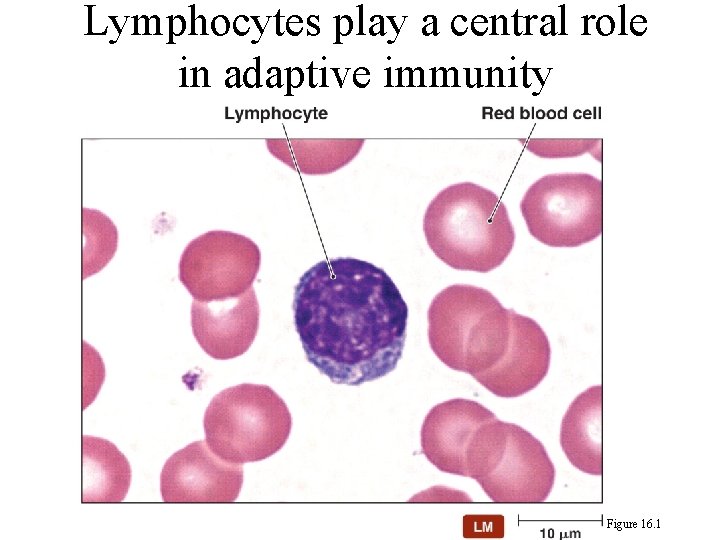
Lymphocytes play a central role in adaptive immunity Figure 16. 1

235

235 Functions of Lymphatic System: 1. It is responsible for returning the excessive fluid and proteins that leak out from the blood vessels and tissues back to the general circulation. 2. Immunity: B cells and T cells 1. Transportation of fats, and metastasis of cancer cells.

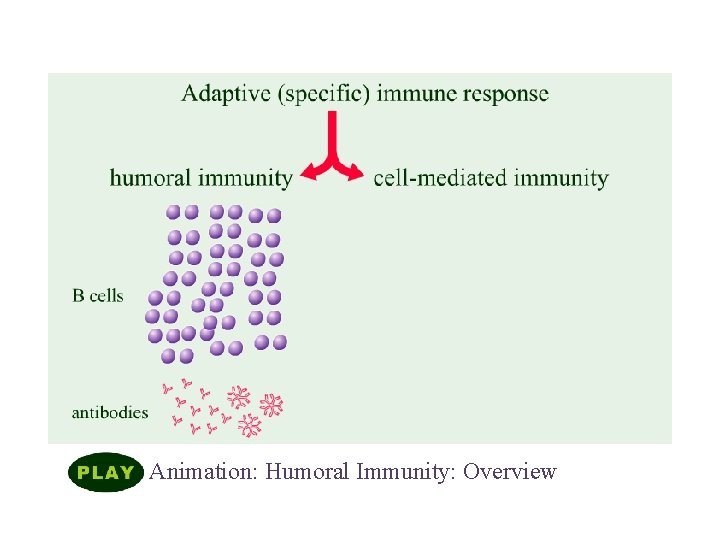
Overview of Adaptive Immunity Animation: Humoral Immunity: Overview

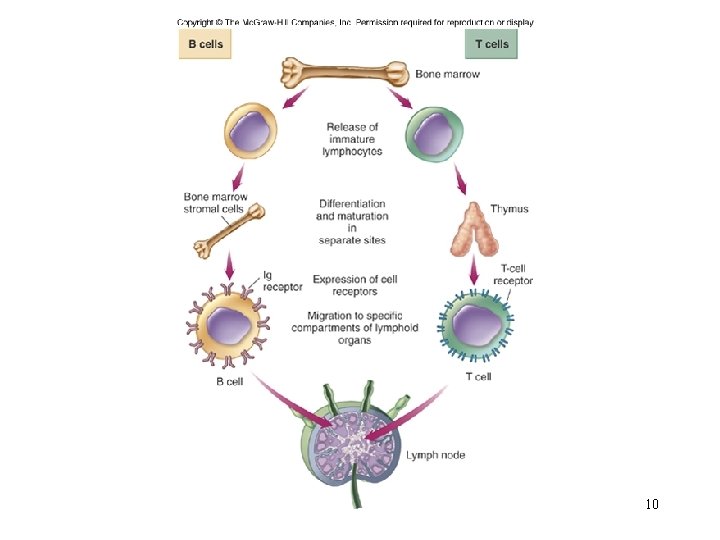
237 Origin and Development of B and T lymphocytes Formation of B cells: 1. Bone marrow produces stem cells (precursor cells). 2. The cells are carried by blood to the Bursa equivalent organs (lymph node, tonsil, appendix, spleen, Peyer’s patches). 3. The cells are influenced by the chemicals in the Bursa equivalent organs. They differentiate into B lymphocytes (B cells).

237 4. These B cells circulate in the blood looking for any invaders (the foreign antigens). 5. When the cells encounter the foreign antigens, the cells are activated. 6. They enter the thymus-independent region of the lymph node to proliferate. 7. After several (5 to 8) cell divisions by mitosis, the cells transform into plasma cells.

237 8. The plasma cells secrete antibodies. 9. Each plasma cell secretes about 2, 000 antibody molecules per second. 10. After about 5 to 7 days, the plasma cells die. 11. The antibodies attack the invaders. We are protected. This type of immunity is known as the humoral immunity.

10

237 Formation of T cells: 1. Bone marrow produces stem cells (precursor cells). 2. The cells are carried by blood to the thymus organ. 3. The cells are influenced by the chemicals and hormones in the thymus organ. They differentiate into T lymphocytes (T cells).

237 4. These T cells circulate in the blood looking for any invaders (the foreign antigens). 5. When the T cells encounter the antigens, the cells are activated. 6. They enter the thymus-dependent region of the lymph node to proliferate to form clones of T cells. 7. The cells attack the invaders. We are protected. This type of immunity is known as the cell-mediated immunity.

238 An antigen is a substance that can stimulate our immune system to respond to produce a specific lymphocyte and/or antibody to attack the antigen (invader). Antigenicity is the ability of an antigen to stimulate our immune system to initiate an immune response.

238 Properties of Antigen: 1. It must be recognized by our immune system as foreign (non-self) cells or molecules. 2. The antigen molecule must be large, can be either one of the following chemical categories: Proteins Polysaccharides Glycoproteins Lipoproteins Nucleoproteins

238 • • • Epitope (antigenic determinant): Idiotype: Hapten: Autoantigen: normal cell antigen Alloantigen: Heterophile antigen:

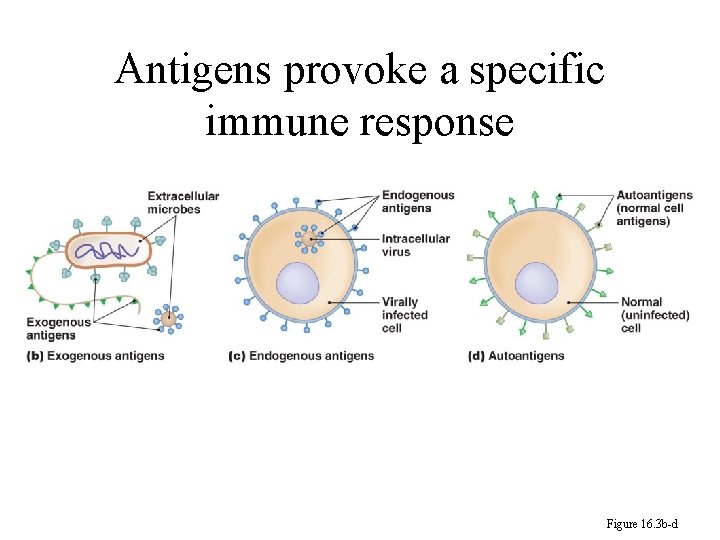
Antigens provoke a specific immune response Figure 16. 3 b-d

239 • Endogenous antigen is an antigen produced by microorganism that multiplies inside a host cell. • Exogenous antigen is an antigen produced by microorganism that multiplies outside a host cell.

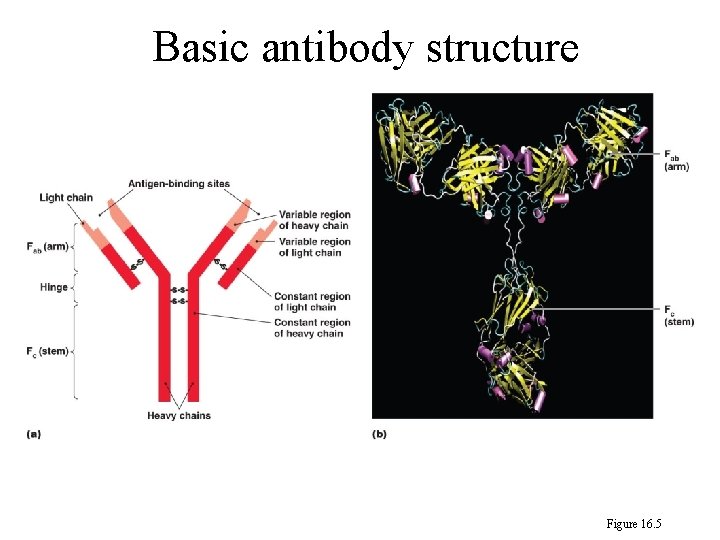
239 The Structure of Immunoglobulins (Antibodies): 1. The antibody consists of four polypeptides (2 light chains and 2 heavy chains). 2. Each light chain contains about 214 amino acids. 3. Each heavy chain has about 450 to 700 amino acids.

Basic antibody structure Figure 16. 5

239 4. The light and heavy chains are joined by disulfide bonds to form a Y shape molecule. 5. The two limbs of the Y configuration, which have amino (NH 2) ends are known as the Fab fragments (F: fragment; ab: antigen-binding). 6. The Fc fragment (F: fragment; c: crystallizable) has carboxyl (COOH) end. 7. The Fc fragment determines the physical properties of an antibody molecule.

239 8. Half of the light chain and half of the heavy chain of the two Fab fragments that contain the amino ends are called the variable regions. The remaining portions of the polypeptides, which contain the carboxyl ends are known as the constant regions.

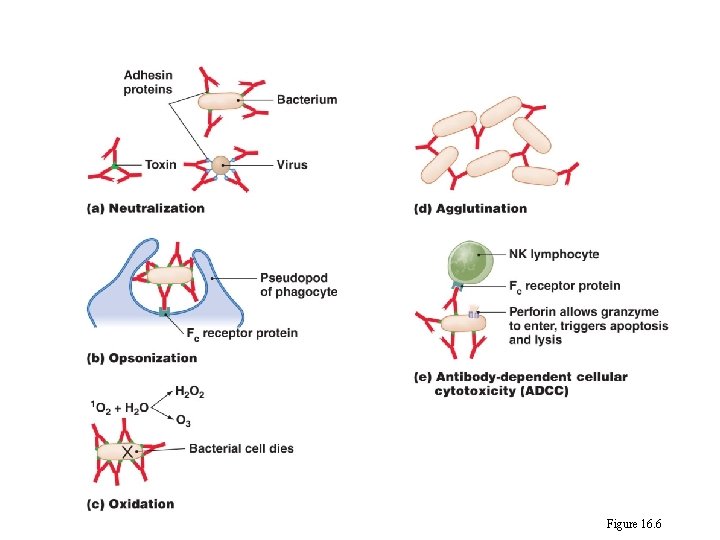
Elements of Adaptive Immunity • B Lymphocytes (B Cells) and Antibodies • Antibody function – Antigen-binding sites are complementary to epitopes – Antibodies function in several ways • • • Activation of complement and inflammation Neutralization Opsonization Killing by oxidation Agglutination Antibody-dependent cellular cytotoxicity (ADCC)

Four functions of antibodies Figure 16. 6

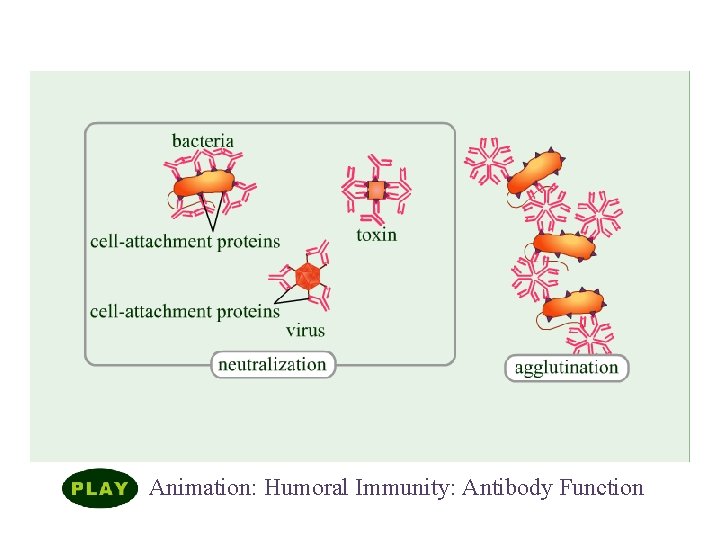
Elements of Adaptive Immunity Animation: Humoral Immunity: Antibody Function

25

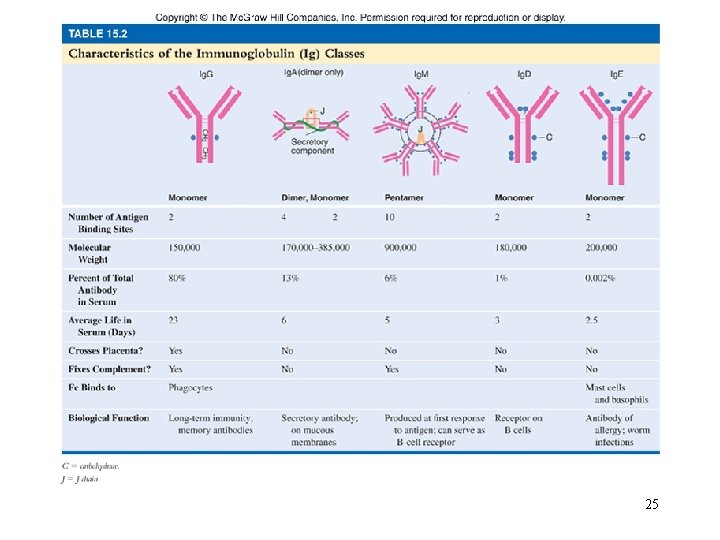
242 Classes and Functions of Immunoglobulins: Refer to page 242

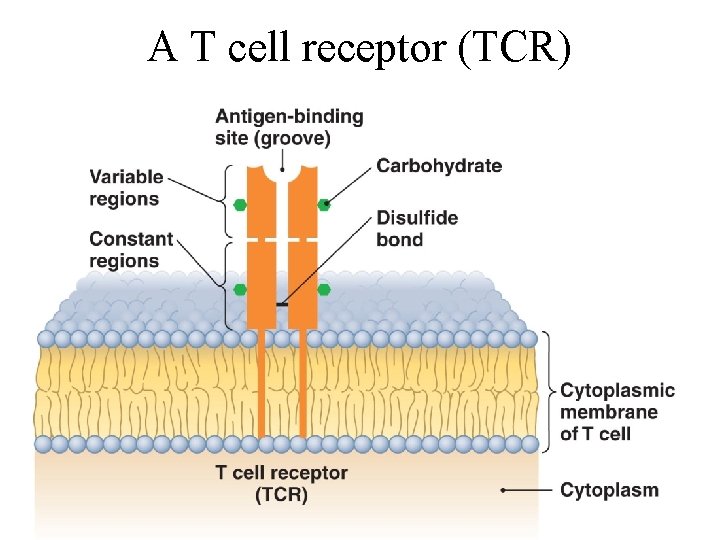
243 • T Lymphocytes (T Cells): consist of 70 -85% of all lymphocytes, each has half a million copies of T cell receptor (TCR): -each has two polypeptides -the groove between the variable regions is the antigen-binding site -binds only to epitope associated with MHC There at least 109 different TCRs.

A T cell receptor (TCR) Figure 16. 7

243 Types of Lymphocytes 1. Cytotoxic T lymphocyte (Tk, Tc, or CD 8 cells): directly kills other cells perforins and granzymes apoptosis 2. Helper T lymphocyte (TH, T 4, or CD 4 cells): regulates the activities of B cells and cytotoxic T cells interleukin-2: activates B and T cells interleukin-4, -5, -6 to stimulate B cells

243 • T helper cells are stimulated by binding to antigen-MHC II complex. Depending on cytokines released by the antigen-presenting cell. They differentiate into: a. T helper 1 (TH 1) cells if the cytokine is IL-2 or interferon gamma. It can activate more T cells and is also involved in hypersentivity. b. T helper 2 (TH 2) cells if the cytokine is IL-4. TH 2 activates B cell and suppresses TH 1 cell.

243 3. Regulatory T lymphocyte (Tr): previously known as suppressor T cells They regulate the production of antibody by plasma cell, inhibit the actions of TH cells, and prevent autoimmune diseases.

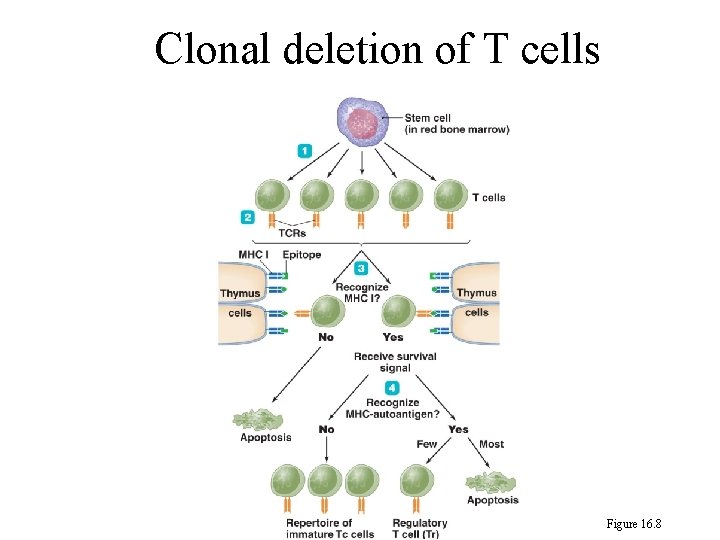
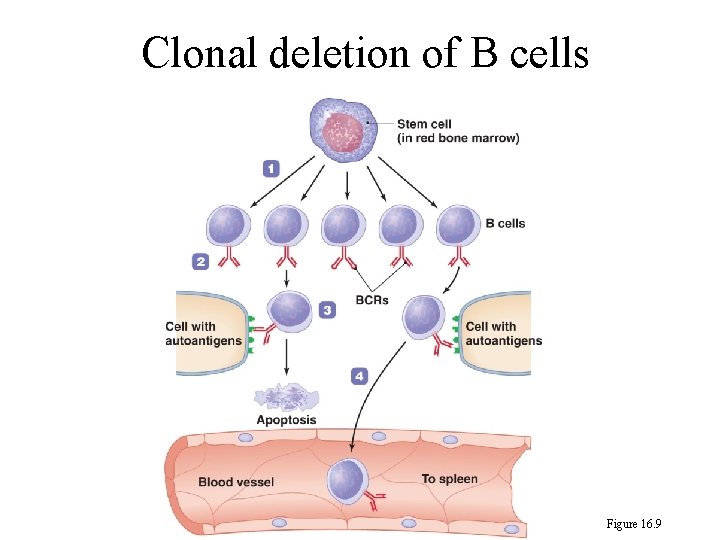
244 Clonal Deletion of T cells 1. T Cells: stay in thymus about 1 week. The T cells that recognize the body’s own MHC protein in conjunction with foreign epitope will survive. If not, they undergo apoptosis. 2. B cells: each has its own B cell receptor (BCR). If BCR is complementary to autoantigen, the B cell is eliminated by apoptosis. If not, the cell is released from the bone marrow.

Clonal deletion of T cells Figure 16. 8

Clonal deletion of B cells Figure 16. 9

244 Clonal Selection Theory: 1. Our immune system has millions of different types of lymphocytes, each with a specific receptor. 2. When an antigen enters the body, it selects one specific lymphocyte (the one with a specific receptor that fits the epitope of the antigen), and stimulates the lymphocyte to undergo proliferation to form a clone of cells.

244 3. The cells will react only with the specific antigen that activates it. In the case of B cell, the cell undergoes cell divisions to give rise to plasma cells. The plasma cells secrete a specific antibody that reacts only with the antigen that activates it.

244 Cytokines: regulatory proteins secreted by skin, kidney and immune system Interleukin (IL): Interferon (IFN): Growth factors: Tumor necrosis factor (TNF): Chemokines:

245 Major Histocompatibility Complex: It is a gene complex located on chromosome number 6. It codes for protein receptors on the surface of all cells except the red blood cells. These proteins are joined with carbohydrate side chains to form glycoproteins, which serve as surface markers called MHC antigens. These receptors were first found on the surface of human leukocytes, they are also known as human leukocyte antigens (HLA).

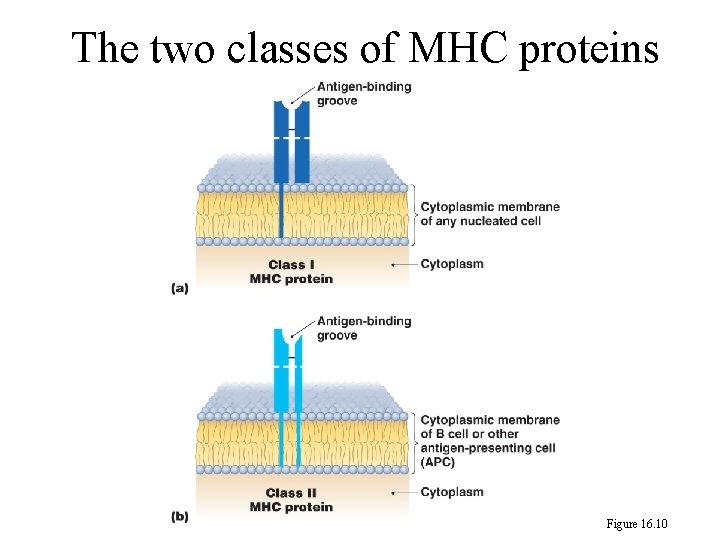
245 Classes of MHC Class I MHC genes: code for markers called transplantation antigens found on the surface of all cells. Class II MHC genes: code for receptors on the surface of macrophages, B cells and T helper cells. Class III MHC genes: code for complement components (C 2 and C 4 and factor B).

The two classes of MHC proteins Figure 16. 10

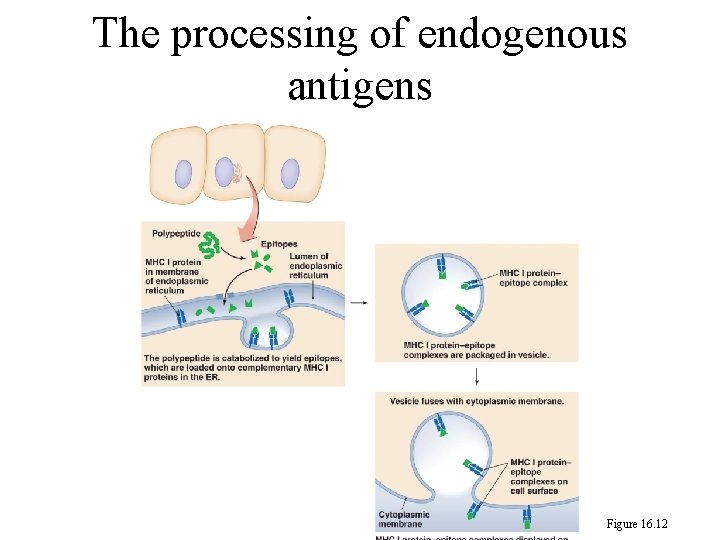
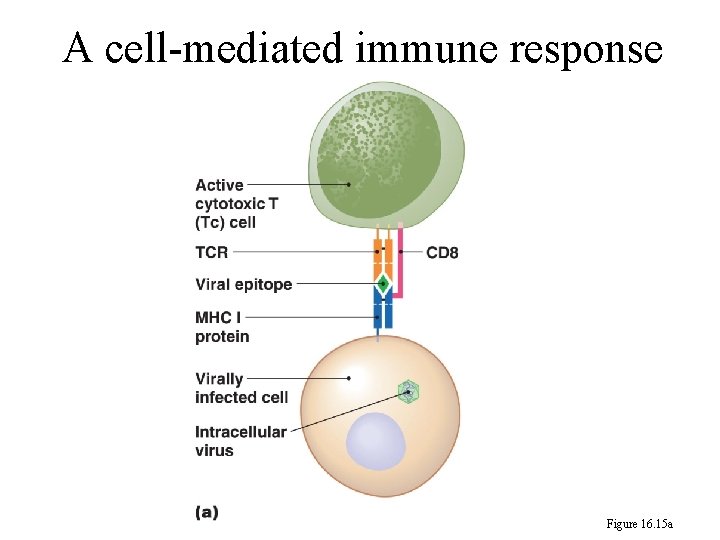
246 Cell-Mediated Immune Responses 1. Cytotoxic Cell Is Activated By Endogenous Antigen: a. The endogenous antigen such as viruses replicate inside the cell. The epitope of virus is loaded onto MHC 1 protein which is exported to the cytoplasmic membrane. b. A cytotoxic cell (Tc) with TCR (T cell receptor) attaches to the epitope to form an immunological synapse.

The processing of endogenous antigens Figure 16. 12

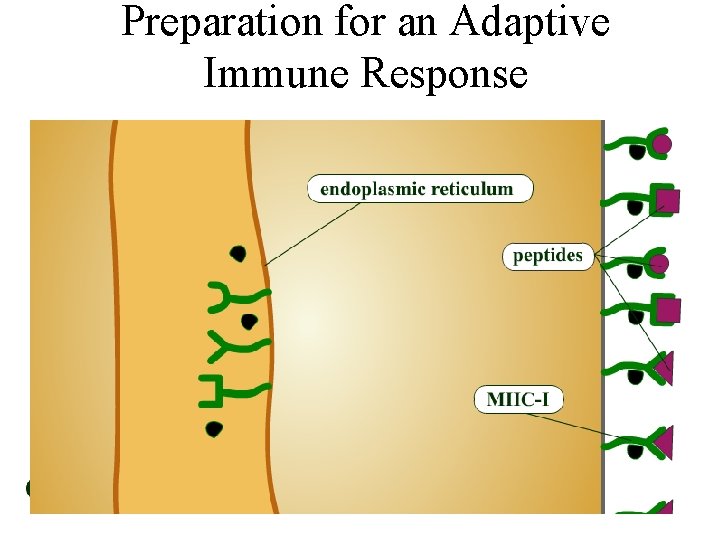
Preparation for an Adaptive Immune Response Animation: Antigen Processing and Presentation: Steps

A cell-mediated immune response Figure 16. 15 a

246 c. Once connected, the cytotoxic cell secretes interleukin II (IL 2) to trigger cell division and differentiation to form (1) activated Tc cells, and (2) memory T cells.

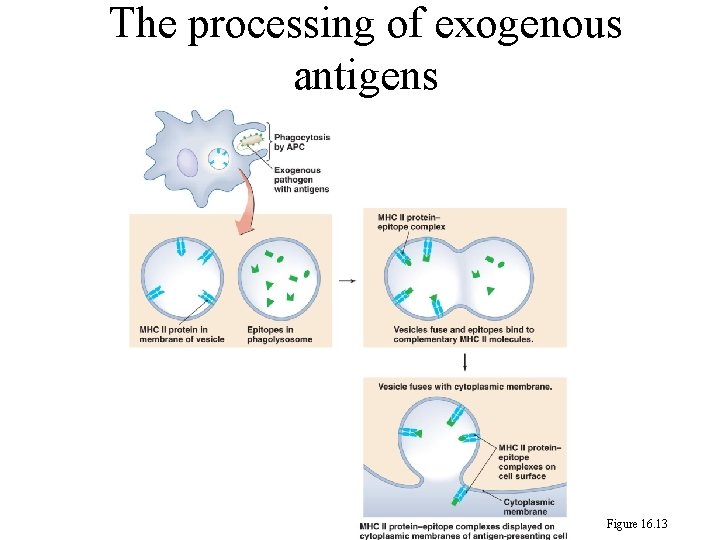
246 2. Cytotoxic Cell Is Activated By Exogenous Antigen: a. A dendritic cell phagocytizes and processes antigen and loads the epitope on both of its MHC I and MHC II proteins. b. A cytotoxic cell (Tc) binds to the epitope. MHC I, and a T helper cell (Th) binds to the epitope-MHC II of the dendritic cell.

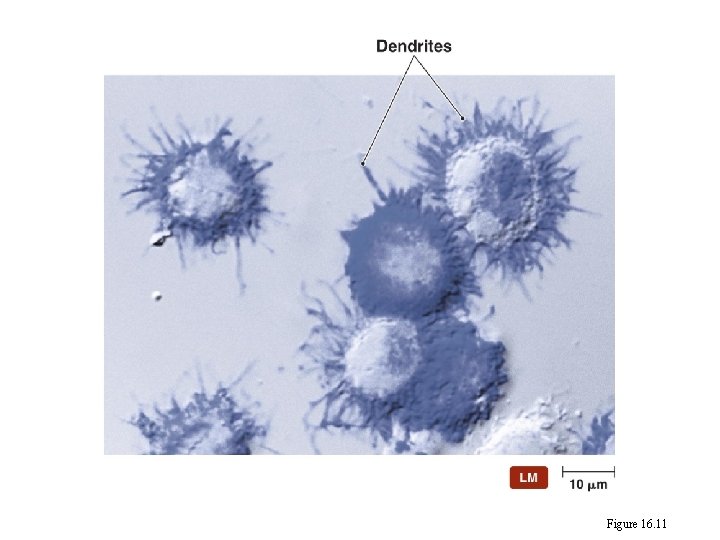
Dendritic cells Figure 16. 11

The processing of exogenous antigens Figure 16. 13

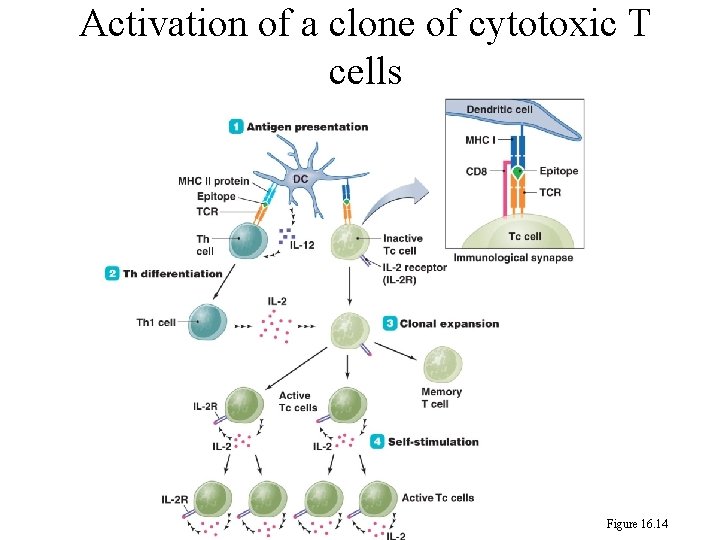
Activation of a clone of cytotoxic T cells Figure 16. 14

246 c. The dendritic cell secretes interleukin 12 (IL-12) to stimulate T helper cell (Th) which differentiates to become a clone of type I T helper cells (Th 1). d. The Th 1 cell secretes interleukin 2 (IL-2) to stimulate cytotoxic T cell to form activated T cells (Tc) and memory T cells. The activated cytotoxic cell also secretes interleukin 2 (IL-2) to trigger cell division (self stimulation).

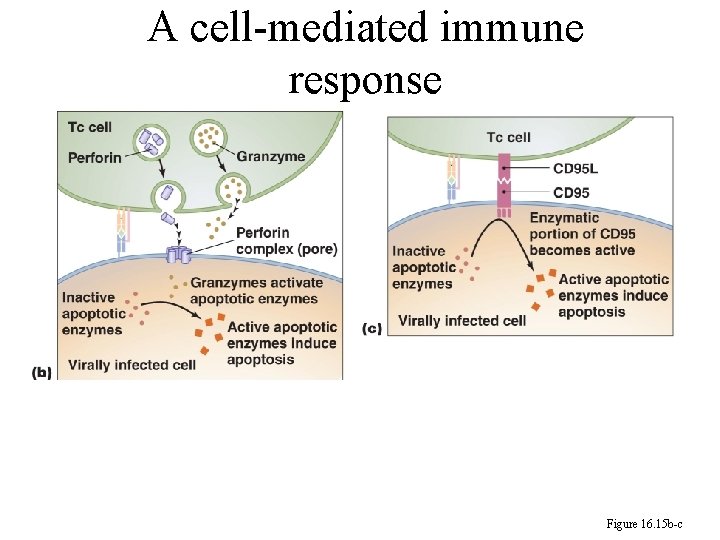
246 The activated T cells (Tc) kill their targets through one of two pathways: 1. Perforin-granzyme pathway: The perforin causes lysis and allows granzyme to enter the cell. The granzyme activates the enzymes of apoptosis to kill the target cell.

246 2. The CD 95 Cytotoxic Pathway: The CD 95 L of Tc binds to CD 95 on the target, and the TCR of Tc binds to the epitope-MHC I complex. The simultaneous bindings activate the enzyme portion of CD 95. The activated CD 95 activates the inactive apoptotic enzymes, which then cause the cell to undergo apoptosis.

A cell-mediated immune response Figure 16. 15 b-c

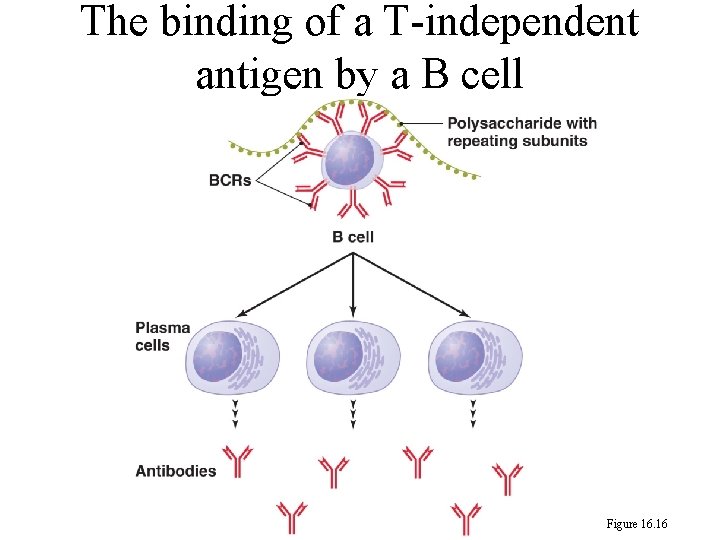
247 Humoral Immune Responses 1. T-independent humoral immunity: a. An antigen with repeating subunits of polysaccharide or lipopolysaccharide of capsule, cell walls, and flagella or capsids of some viruses connects to the receptors on B cell. b. A B cell is activated to undergo cell division to form plasma cells, and with little or no memory B cells. The plasma cells secrete antibodies.

The binding of a T-independent antigen by a B cell Figure 16. 16

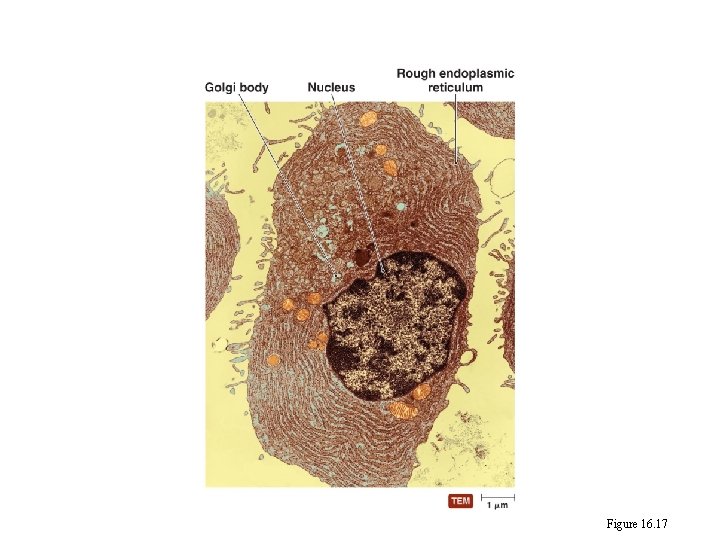
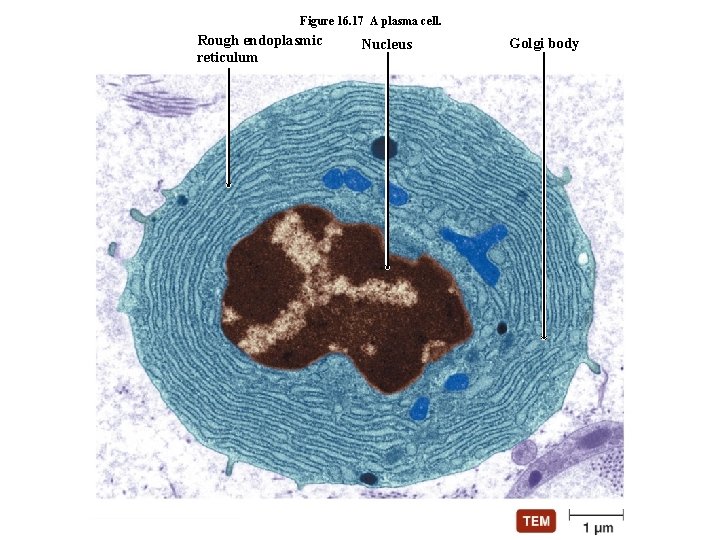
A plasma cell Figure 16. 17

Figure 16. 17 A plasma cell. Rough endoplasmic reticulum Nucleus Golgi body

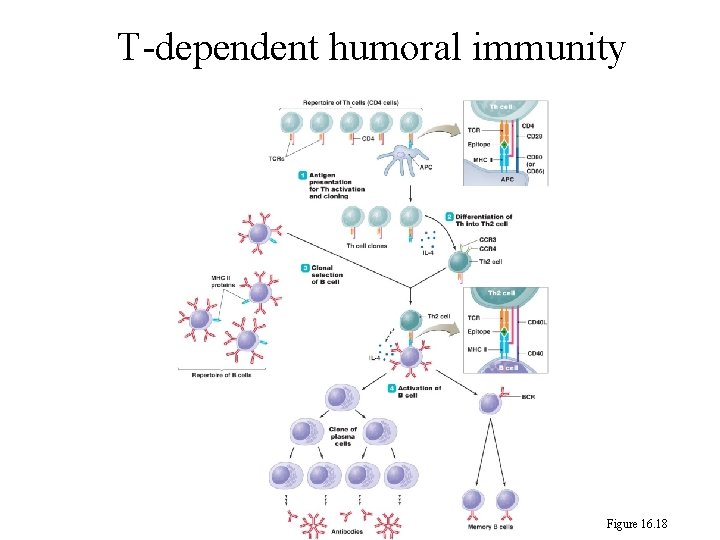
247 2. T-dependent humoral immunity: a. A dendritic cell (antigen-presenting cell, APC) processes the antigen, and presents the epitope on its MHC II protein. b. A T helper cell (Th) with its T cell receptor (TCR) connects to the epitope. MHC II complex on the APC to form an immunological synapse.

247 c. The APC secretes interleukin 4 (IL-4) to activate the T helper cell (Th), which differentiate into type 2 T helper cell (Th 2). d. The type 2 T helper cell (Th 2) connects to the MHC II protein on the B cell. The Th 2 cell also secretes interleukin 4 to activate B cell. e. The Th 2 produces a protein called CD 40 L and inserts it into its cytoplasmic membrane.

247 The CD 40 L binds to CD 40 on the surface of B cell. f. B cell is activated and undergoes cell division to form a clone of plasma cells and memory B cell. The plasma cells secrete antibodies---Humoral immunity.

T-dependent humoral immunity Figure 16. 18

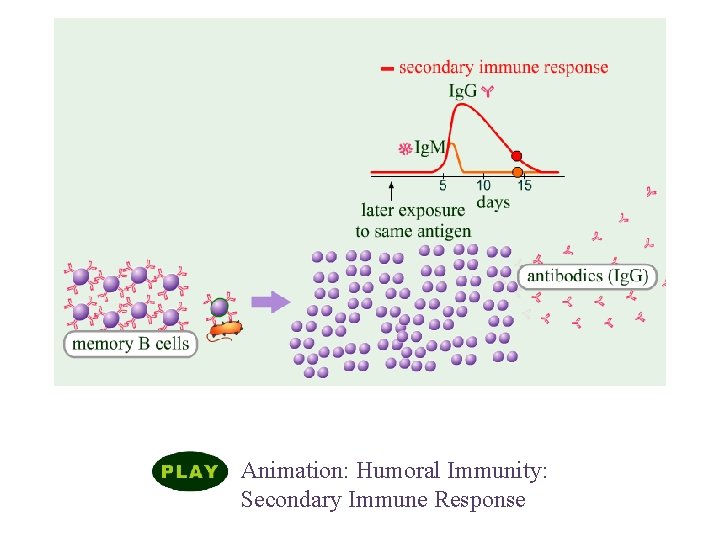
248 Memory T Cells: When they encounter the same MHC-epitope complex, they response immediately to produce a clone of cytotoxic T cells to destroy the pathogen. They do not require the interaction with antigen-presenting cells (APC). This immune response is called anamnestic, secondary or memory immune response.

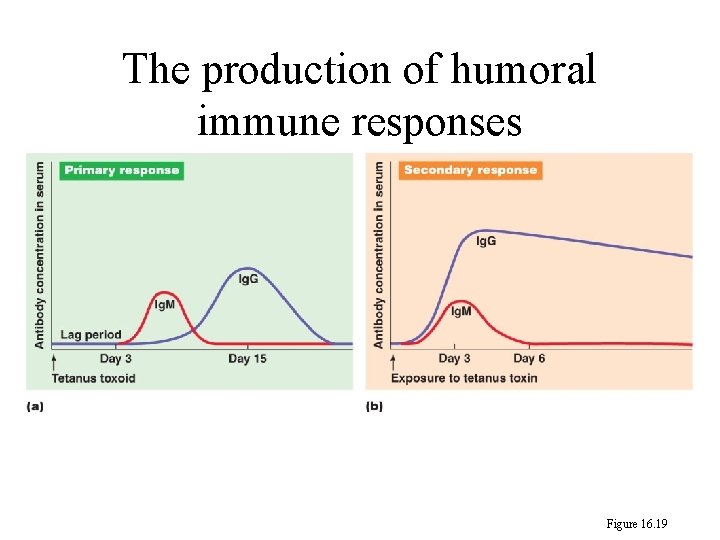
248 • Primary immune response: • Secondary immune response: (anamnestic response)

The production of humoral immune responses Figure 16. 19

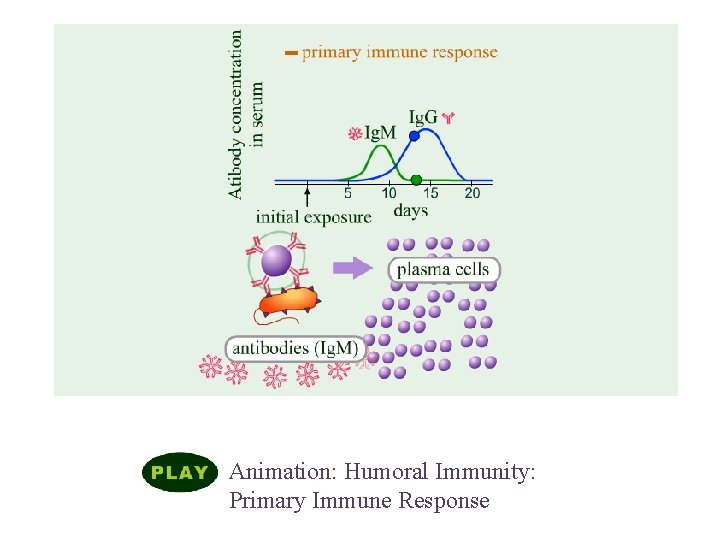
Humoral Immune Responses Animation: Humoral Immunity: Primary Immune Response

Humoral Immune Responses Animation: Humoral Immunity: Secondary Immune Response

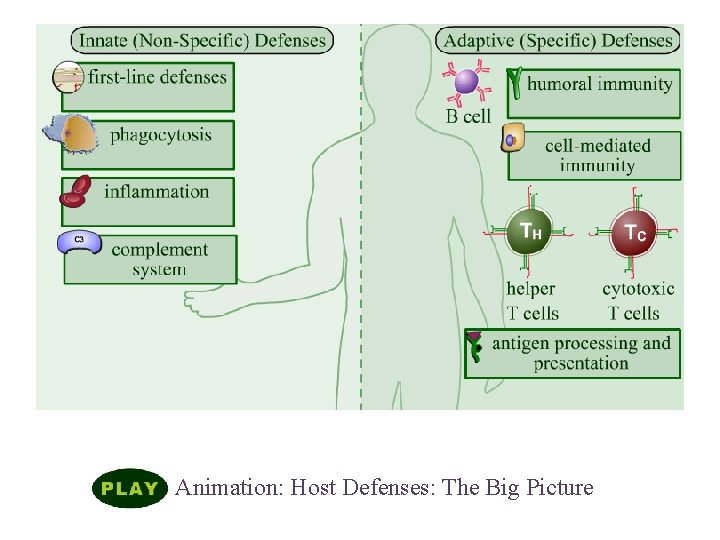
Humoral Immune Responses Animation: Host Defenses: The Big Picture

248 A General Scheme for Classifying Immunities: I. Natural immunity: 1. Species immunity: 2. Racial immunity: 3. Individual immunity:

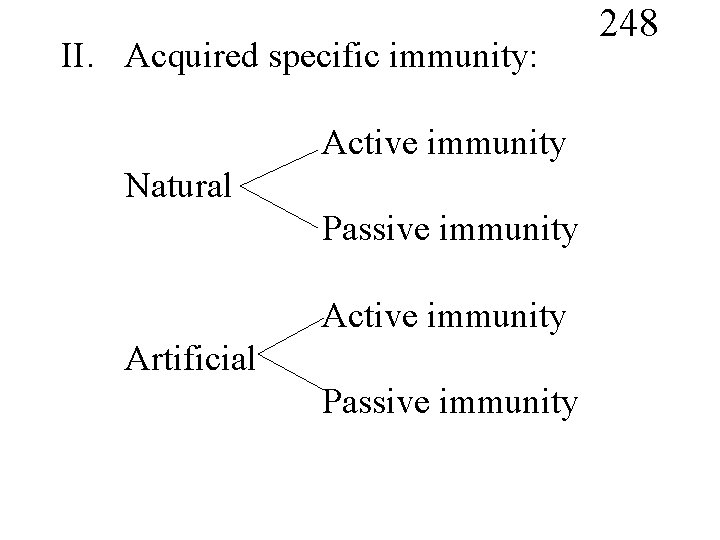
II. Acquired specific immunity: Active immunity Natural Passive immunity Active immunity Artificial Passive immunity 248