Think Delirium Karen Goudie National Clinical Lead Assuring






















- Slides: 26

Think Delirium Karen Goudie National Clinical Lead

Assuring Delirium Care

Policy and Standards Appropriateness Availability Continuity Respect and Caring Efficacy

Standard 8

Think delirium Our Challenge. . helping staff understand see the process of gold standard Delirium care. Testing innovative approach to delirium care throughout Scottish Acute Hospitals


Listen to experience


OPAH Inspection Proportionate Multidisciplinary Driven by data Report reflects overall reliability Support time for QI Appreciation of data over time

Risk Factors for Delirium Multi-factorial • Advanced Age • Dementia/Frailty • Illness • Multiple Medications • • • Functional deficits Dehydration Pain and Depression Immobility Sensory Impairment (de. Lange E, et al. Int. Jrnl. Geri. Psychiatry 2013; 28; 127134)

Around a third of delirium is Preventable Care planning can have significant impact CGA Fundamentals of Care

Vulnerability Use process to find Delirium Seek carer, family Early recognition Risk to those with Hypoactive delirium Think about Hospital acquired delirium

Education Triggers Systematic approach to process Risk reduction Stress and Distress

ALERTNESS AMT 4 ATTENTION ACUTE CHANGE

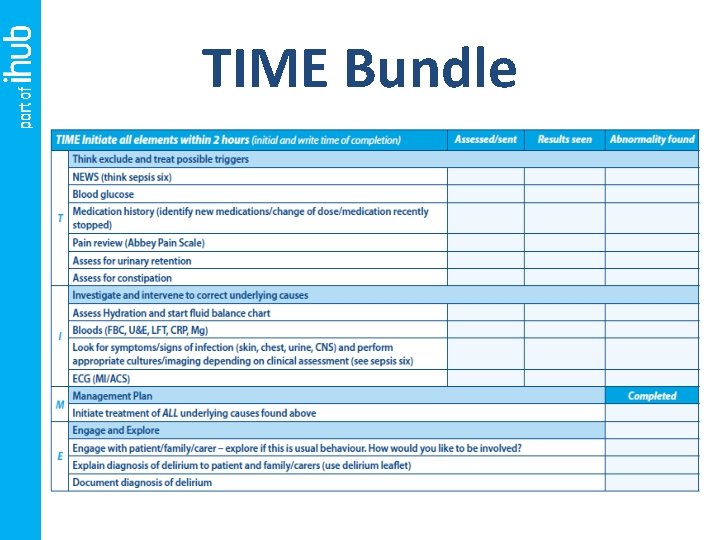
TIME Bundle



Speak to families and carers

What Next for Think Delirium ? Up to 70% in patients admitted to Long Term Care. 34% Hypoactive 24% Hyperactive 42% Mixed type Substantially worsens outcomes in a population who are already burdened by functional decline • Delirium in older adults is poorly recognized and poorly noted on discharge • Over 80% were on central nervous system active drugs • Length of stay was significantly higher in patients with delirium • • • (Inouye SK. Delirium in older persons. N Engl. J Med 2006; 354: 1157 -1165. de. Lange. E, et al. Int. Jrnl. Geri. Psychiatry 2013; 28; 127 -134 Fick D. J Hosp. Med. 2013 Sep; 8(9): 500 -5. )

• Do we routinely assess risk of delirium when we admit residents to our care home? • Do staff involved in admitting residents know the risk factors for delirium? • Where do we record in resident’s notes that we have assessed their risk of developing delirium? • For those people at risk of delirium, do care staff know that they should monitor them for recent changes in behaviour , including cognition, perception, physical function and social behaviour? • If there are concerns that a resident has developed delirium, do care staff know how to request a clinical assessment?

Think about vulnerability

Reducing risk of falling Falls are the most common adverse incident in hospitals and care homes, nearly always affecting frail elderly people, many of whom have dementia or delirium Risk management must be balanced against the need to promote functional independence and to respect autonomy

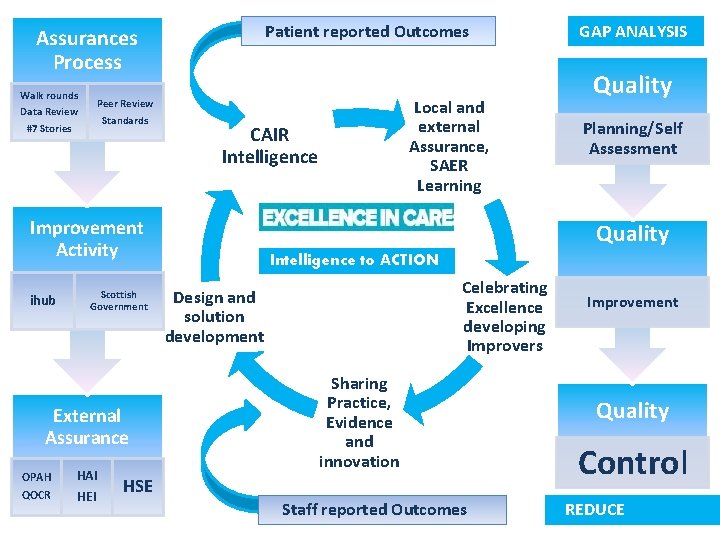
Patient reported Outcomes Assurances Process Walk rounds Data Review Standards #7 Stories CAIR Intelligence Improvement Activity ihub Scottish Government External Assurance OPAH QOCR Local and external Assurance, SAER Learning Peer Review HAI HEI GAP ANALYSIS Quality Planning/Self Assessment Quality Intelligence to ACTION Celebrating Excellence developing Improvers Design and solution development Sharing Practice, Evidence and innovation HSE Staff reported Outcomes Improvement Quality Control REDUCE VARIATION

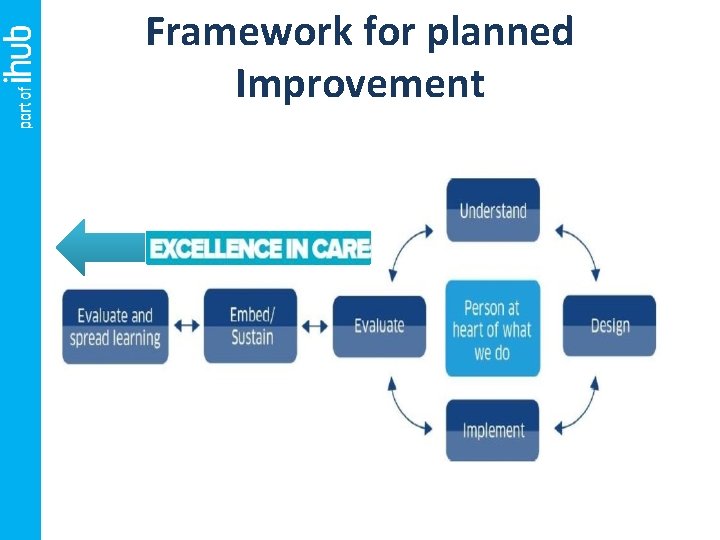
Framework for planned Improvement


Thank you