Review of Hospice and Eligibility Requirements for Dementia

Review of Hospice and Eligibility Requirements for Dementia, CHF, COPD and Cancer Patients Laura Mantine M. D. January 18, 2017 ASPIRE Education Day

Hospice Overview �A philosophy of care to assist those in the end stage of life ◦ Designed for those who want no further curative treatment with emphasis on quality of life and symptom relief ◦ Physical, psychological, social and spiritual care is provided ◦ Patient and family form a unique, individualized plan of care

Medicare/Medicaid Regulations �The hospice program must maintain responsibility of the hospice patient’s care at all times and in all settings �Hospice is responsible for coordinating all care �All care must be authorized in advance by the hospice �The hospice program bears the full financial responsibility for the hospice patient’s care

Hospice Benefits �Team approach to care: ◦ Hospice Team: Patient, family, nurse, physician, social worker, home health aide, therapist (PT, OT & ST), chaplain and trained volunteer �Cost for home hospice covered by Medicare 100% �Medications, supplies and equipment related to the terminal disease covered 100% �Acute care in facility setting for symptoms that are unable to be controlled in the home, collapse of support system or imminent death �Respite benefit for caregivers �Ongoing support to the bereaved family

Levels of Care �Routine Home Care: most common; provided in home, ALF, PCH or SNF; regularly scheduled visits from hospice team members �General Inpatient Care: higher level of short-term care; provided in a facility for symptom management (pain, intractable nausea/vomiting, delirium/agitation), wound care, unmanageable respiratory distress, or sudden decline necessitating nursing intervention �Respite Care for Caregiver Stress: 5 consecutive days of inpatient respite per month �Continuous Care: expanded level of skilled care in a patient’s home to manage a crisis; requires a minimum of 8 hours total in a 24 hour period with at least 50% of the total care provided by a nurse

Criteria for Admission to Hospice �Medicare/Medicaid eligibility guidelines (LCD guidelines) available to help with determination of terminal prognosis �Physician certifies terminal diagnosis with 6 month prognosis if disease follows usual course �Primary caregiver is available �Patient and family choose the hospice philosophy goal of comfort care rather than curative treatment; being “hospice ready”

Hospice Eligibility Medicare hospice coverage depends upon a physician’s certification of a life expectancy of 6 months or less if the terminal illness runs its normal course • The physician’s clinical judgment must be supported by “clinical information and other documentation” that provide a basis for a life expectancy of six months or less • Medical necessity must be evaluated and clearly and objectively documented in the clinical record • Recognizing that determination of life expectancy during the course of a terminal illness is difficult, CMS established LCD guidelines (“medical criteria”) for determining prognosis for cancer and non-cancer diagnoses • LCD= “Local Coverage Determination” • ◦ Created to assist in determining eligibility based upon disease severity and burden of illness. ◦ Allows for decline of the beneficiary’s condition be to a factor in determining prognosis. ◦ Many do not reflect current research or medical information on prognosis.

LCD Part I � Decline • • • in clinical status guidelines: Appropriate for all diagnoses Clinical status: weight loss, infections, ↓ albumin or dysphagia Symptoms: dyspnea, cough, poorly controlled nausea, diarrhea, increasing pain Signs: ↓BP, ascites, edema, pleural effusion, weakness, change in LOC Laboratory: ↑p. CO 2, ↓p. O 2, ↓O 2 sat, etc. KPS or PPS < 70% ↑ ER or physician visits, ↑ hospitalizations FAST score 7 A or higher ↑ dependence for ADLs Stage III-IV pressure ulcers

LCD Part II � Non-disease specific baseline guidelines – both A and B should be met A. Physiologic impairment of functional status as demonstrated by: � Karnofsky Performance Status (KPS) or Palliative Performance Score (PPS) < 70% (HIV Disease, Stroke and Coma establish a lower qualifying KPS or PPS). B. Dependence on assistance for 2 or more activities of daily living (ADLs)

LCD Part III �Disease-Specific ◦ ◦ ◦ ◦ Guidelines: Alzheimer’s dementia CHF/heart disease COPD/pulmonary disease Cancer HIV Liver disease Renal disease Stroke or coma

Comorbidities �Although not the primary hospice diagnosis, the presence of diseases such as the following, the severity of which is likely to contribute to a life expectancy of six months or less, should be considered in determining hospice eligibility: • COPD, CHF, Ischemic Heart Disease, DM, Neurologic (CVA, ALS, MS, Parkinsons), Renal, Liver, Cancer, AIDS and Dementia • When supporting prognosis, it isn’t the number of co -morbid conditions but the severity that counts!

Secondary Conditions that are directly related to and occur as a result of the primary condition • Examples of conditions that are directly related to the terminal illness: • Dysphagia is a secondary condition of dementia • Dyspnea is a secondary condition of CHF • Examples of a conditions that manifest as a result of the terminal condition: • Decubitus ulcer is a secondary condition of coma • Pneumonia is a secondary condition of ALS •

Disease Specific Guideline: DEMENTIA

Dementia �Irreversible, progressive brain disease that slowly destroys memory, thinking, and motor skills �Caused by various diseases and conditions �Types: • Alzheimer's - most common type (60 -80% of cases), results from deposits of protein plaques and tangles in the brain • Vascular dementia (multi-infarct dementia) - 15 -30% cases • Lewy Body dementia - 10 -15% cases • Frontotemporal dementia - < 1% cases • Parkinson’s Disease w/ Dementia - occurs in 20 -40% of patients with PD, risk rises in patients with PD for > 8 yrs
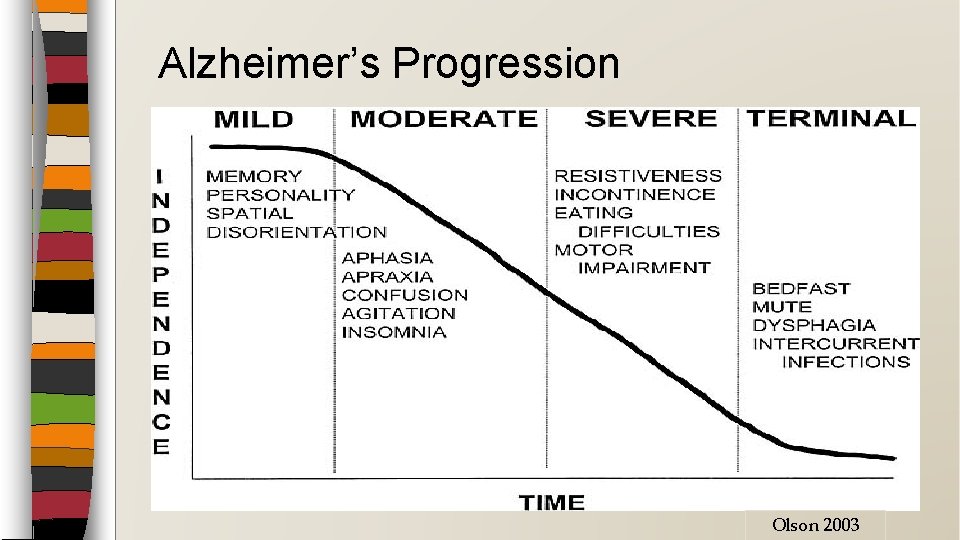
Alzheimer’s Progression Olson 2003

Alzheimer’s & Related Disorders Guidelines KPS or PPS < 70% � Minimally dependent in 2/6 ADLs � FAST score of 7 or beyond ◦ FAST 7: Loss of speech, locomotion, and consciousness � 7 a: Ability to speak limited (1 -5 words/day) � 7 b: All intelligible vocabulary lost � 7 c: Non-ambulatory � 7 d: Unable to sit up independently � 7 e: Unable to smile � 7 f: Unable to hold head up � And one of the following w/in past 12 months: ◦ Aspiration pneumonia ◦ Pyelonephritis ◦ Septicemia ◦ Multiple Stage 3 -4 decubitus ulcers ◦ Recurrent fever despite antibiotics ◦ 10% weight loss during previous six months or serum albumin < 2. 5 gm/dl. �

Case Scenario �Mrs. Smith is a 91 year-old female with Alzheimer’s dementia, CAD and NIDDM, living at home with daughter. She requires assistance with bathing, dressing and medication management and is wheelchair bound with the assist of one to transfer. She was hospitalized in October with UTI and sepsis. �Physical Examination: AVSS; height 5’ 9” 89 pounds; alert but confused with exam remarkable for cachexia only. �What is her FAST, PPS and is she hospice eligible?

Disease Specific Guidelines: CHF/Heart Disease & COPD/Pulmonary Disease

Trajectory of Illness: “Saw-Toothed” and other organ system failures/conditions (HIV, liver, renal, etc. ) �A slow incremental decline punctuated by multiple episodes of acute exacerbations Decline: never get back to previous baseline Health Status �Cardio-pulmonary Time Death Resource: Field MJ, Cassel CK (eds), Institute of Medicine. Approaching Death: Improving Care at the End-of-life. Washington, DC: National Academy Press. 1997

Congestive Heart Failure �Heart failure: Progressive disorder resulting from an underlying disease causing structural or functional damage to the heart ◦ Weakening the heart’s pumping function �Heart Disease Guidelines: ◦ Patient has been optimally treated for heart disease, or is not a candidate or declines surgical procedures. (Optimally treated means that patients who are not on vasodilators have a medical reason for refusing these drugs, e. g. , hypotension or renal disease. ) ◦ Exhibit NYHA Class IV disease. ◦ Ejection fraction of < 20% (not required)

New York Heart Association (NYHA) Classification Class I - Patients have no limitation in physical activity • Class II - Patients have slight limitation of physical activity • Class III - Patients have marked limitation of physical activity • Class IV - Patients have symptoms even at rest and are unable to carry on any physical activity without discomfort •

Congestive Heart Failure � The following are not required, but help to establish hospice eligibility: ◦ Treatment-resistant symptomatic SVT; ◦ History of cardiac arrest or resuscitation; ◦ History of unexplained syncope; ◦ Brain embolism of cardiac origin; and ◦ Concomitant HIV disease � The patient with terminal heart failure has refractory heart failure and serious heart failure symptoms remain, despite using all recommended therapies. � The terminal disease trajectory resembles a “saw tooth” with periods of compensation, subsequent crisis, followed by compensation until death.

CHF: Comorbid and Secondary Conditions Comorbid conditions: • How does the comorbid condition impact the terminal disease trajectory? Secondary conditions: • Dyspnea • Depression • Pneumonia • Renal failure • Venous stasis ulcers

Case Scenario � 75 year-old male with HX CAD; post-hospitalization following M. I. reports feeling tired all the time and “winded; able to ambulate 10 feet with 5 minute recovery time; optimally treated with Lisinopril, Lasix, and Digoxin; loss of 10 pounds in past month (normal weight 175 pounds) �Physical exam: Vital signs: 100/52 - 88 – 22 and 92% on 2 liters via nasal cannula; weight 165 pounds, height 5’ 10” (BMI 23. 7); Pertinent positives of ¾ HSM, fine bibasilar crackles and 2 -3+ BLE edema �Ejection fraction: 20% during last hospitalization �What is the patient NYHA Class? Is he hospice eligible?

COPD � The patient with terminal lung disease presents with serious respiratory failure symptoms despite intervention with all the recommended therapies. � The dying trajectory resembles a “saw tooth, ” with periods of compensation, subsequent crisis, followed by compensation until death.

COPD � 1 and 2 should be present: 1. Severe chronic lung disease with – – Disabling dyspnea at rest (e. g. , bed to chair existence, fatigue, cough) Progression of disease with increased ER visits and/or hospitalizations for pulmonary infections/respiratory failure, or increased physician visits 2. Hypoxemia at rest with PO 2 55 mm. Hg or oxygen saturation < 88% � • • • The following lend support to the terminal prognosis: Cor pulmonale - right-sided heart failure secondary to pulmonary disease) Unintentional progressive weight loss of greater than 10% body weight over the preceding six months Resting tachycardia > 100/min


COPD: Secondary and Comorbid Conditions �Secondary conditions: • Delirium • Pneumonia • Weight loss • Decubitus ulcers • Peptic ulcers �Comorbid conditions: • How do the comorbid conditions impact the terminal disease trajectory?

Case Scenario � 76 year-old male with COPD and HTN with 56 year smoking history that reports “I can’t do anything anymore and I am totally exhausted all of the time. I can’t catch my breath even when I am sitting doing nothing. ” Ambulates 10 feet and requires 5 -10 minute recovery period and is primarily wheelchair bound. �Physical exam: 110 bpm at rest, 88% RA, 94% on 3 liters nasal cannula continuously; 5’ 9” height, 120 pounds (BMI 17. 7%) noted pursed-lipped breathing; Pertinent positives: temporal wasting, decreased breath sounds throughout �Is he hospice eligible?

Disease Specific Guideline: CANCER
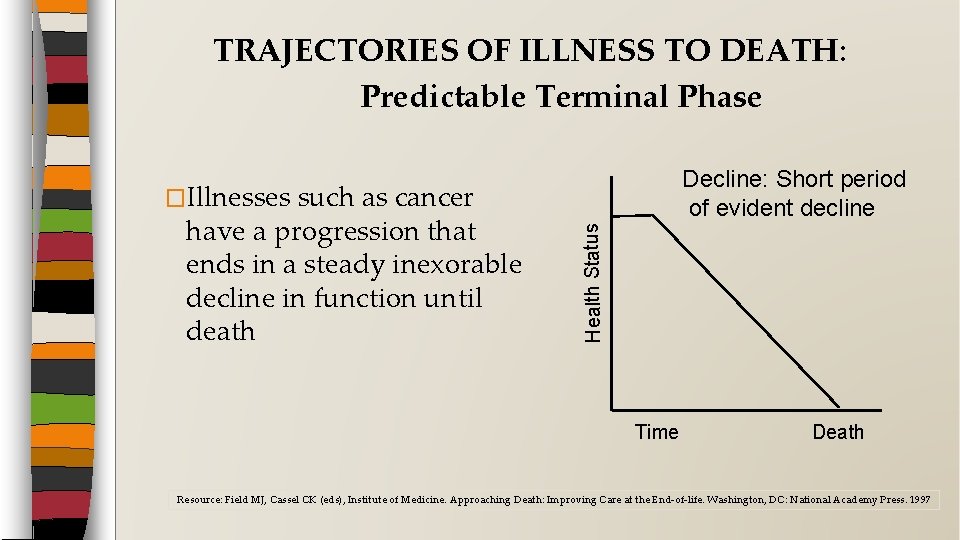
TRAJECTORIES OF ILLNESS TO DEATH: Predictable Terminal Phase �Illnesses Health Status such as cancer have a progression that ends in a steady inexorable decline in function until death Decline: Short period of evident decline Time Death Resource: Field MJ, Cassel CK (eds), Institute of Medicine. Approaching Death: Improving Care at the End-of-life. Washington, DC: National Academy Press. 1997

Cancer �Documentation must demonstrate that the patient meets: • Part II: Non-disease specific baseline guidelines AND • Cancer guidelines in Part III PLUS • Comorbid conditions in Part II/III, if applicable

Cancer �KPS or PPS < 70% �Dependent in 2/6 ADLs �Metastases at presentation OR �Progression from an earlier stage metastatic disease with either: of disease to ◦ A continued decline in spite of therapy or ◦ Patient declines further directed therapy Note: Certain cancers with poor prognoses (e. g. , small cell lung, brain and pancreatic cancer) may be hospice eligible without fulfilling the other criteria.

Case Scenario � 46 year-old male with glioblastoma and unremarkable past medical history. Reports constant headache, dizziness and nausea. Patient reports that radiation treatments are “no longer working. ” �Physical exam: AVSS, patient noted to be in a darkened room, holding head in both hands and grimacing at slightest noise, remaining exam unremarkable �Is the patient hospice eligible? What is his trajectory of illness?

- Slides: 35