Oral neplasia surgery The most common malignant oral









- Slides: 16

Oral neplasia surgery

The most common malignant oral tumors of dogs are malignant melanoma, squamous cell carcinoma, fibrosarcoma osteosarcoma. Squamous cell carcinoma represents approximately 70% of feline oral tumors, with fibrosarcoma and osteosarcoma occurring less commonly.

While benign, well-circumscribed lesions such as cysts and odontomas may be treated conservatively with enucleation or curettage techniques, malignant oral tumors and benign but locally invasive tumors (such as canine acanthomatous ameloblastoma) require more aggressive surgical treatment, typically involving removal of a portion of the maxilla or mandible

There are four potential goals of oral oncologic surgery: (1)surgery to cure, (2)(2) surgery for debulking, (3) surgery for local control (4) surgery for palliation Surgical excision is considered curative for benign, locally aggressive tumors such as acanthomatous ameloblastoma. It is also possible to achieve cure of malignant tumors (such as squamous cell carcinomas in dogs) if metastasis has not already occurred at the time of the procedure.

Debulking, which leaves macroscopic tumor behind, may be performed prior to radiation therapy for large tumors which cannot be completely excised. Surgery for local control is typically the goal for patients with malignant oral tumors such as melanoma, where the potential for early metastasis is high and where adjunctive therapy may be performed following surgical excision of the primary tumor.

However, some oral cancers cannot be eliminated by any treatment modality. In these cases, surgery for palliation may be undertaken to temporarily relieve pain, improve function and increase quality of life

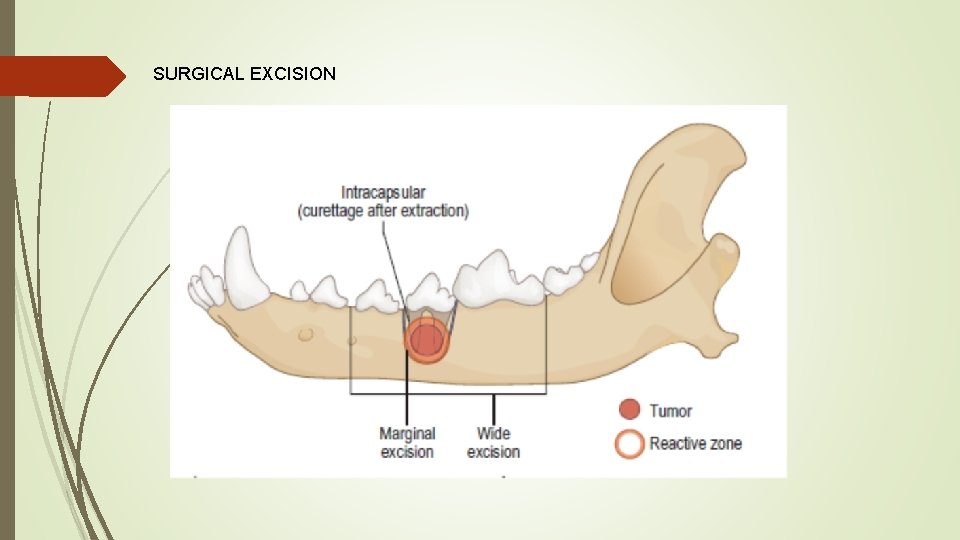
SURGICAL EXCISION

Four types of excision have been described: -Intracapsular excision: ‘debulking’ procedure that leaves behind macroscopically visible tumor. Local recurrence will happen unless surgery is followed by radiation therapy. This type of excision is acceptable for well-differentiated, benign tumors such as odontomas. -Marginal excision: Excision immediately outside the pseudocapsule of the tumor, within the reactive zone (which consists mostly of inflammatory cells). Some neoplastic cells may remain visible microscopically. This type of excision may be appropriate for a well-differentiated benign tumor such as peripheral odontogenic fibroma

-Wide excision: Removal of the tumor, its pseudocapsule, and the reactive zone, with complete margins of normal tissue on all aspects. In general, 10 mm of normal tissue is recommended for most malignant tumors. However, some aggressively infiltrative tumor types, such as fibrosarcoma, may require much wider margins to achieve surgical cure. Partial mandibulectomy or partial maxillectomy are examples of wide excision. Local recurrence is unexpected -Radical excision: Removal of the entire anatomical structure orcompartment containing the tumor. This approach is indicated for malignant oral tumors with extensive infiltration, such as fibrosarcoma, or involving a major part of the jaw. Local recurrence is unexpected

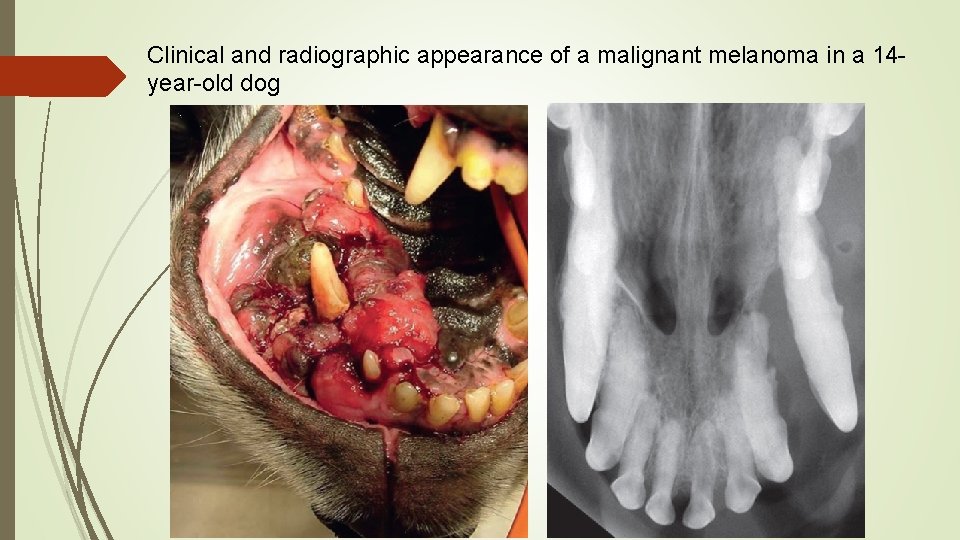
Clinical and radiographic appearance of a malignant melanoma in a 14 year-old dog

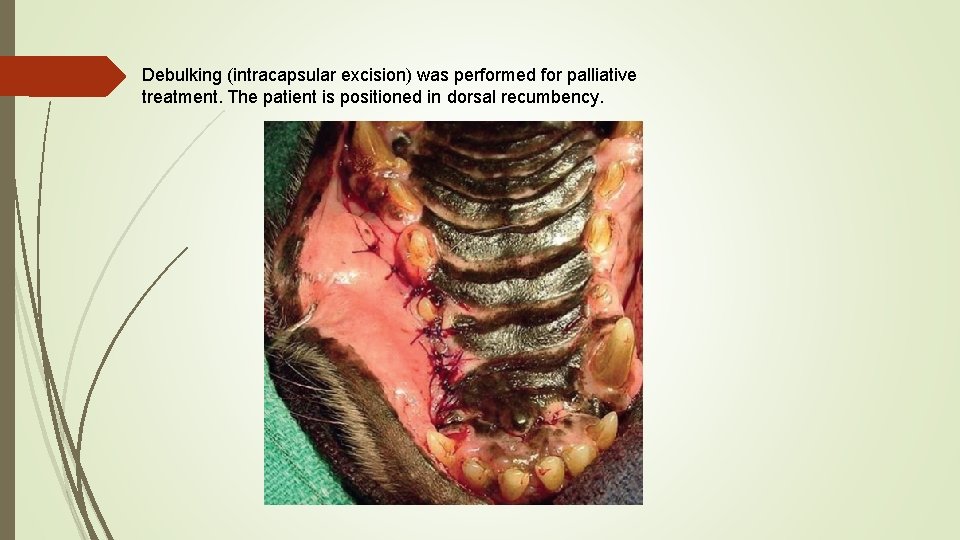
Debulking (intracapsular excision) was performed for palliative treatment. The patient is positioned in dorsal recumbency.

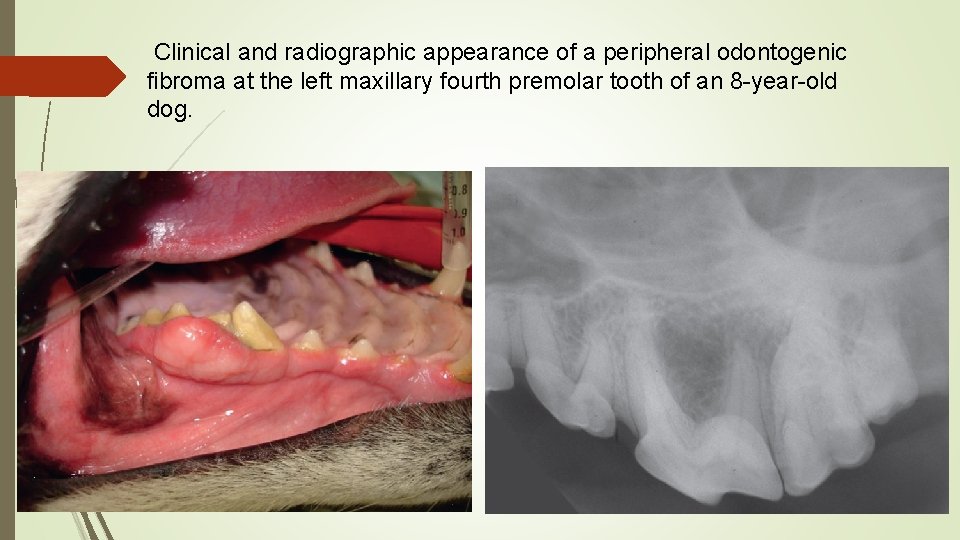
Clinical and radiographic appearance of a peripheral odontogenic fibroma at the left maxillary fourth premolar tooth of an 8 -year-old dog.

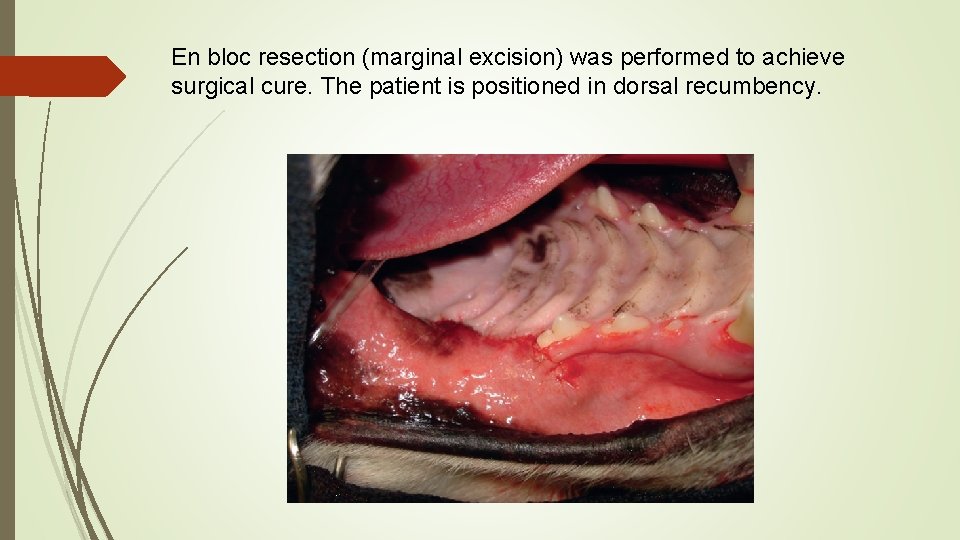
En bloc resection (marginal excision) was performed to achieve surgical cure. The patient is positioned in dorsal recumbency.

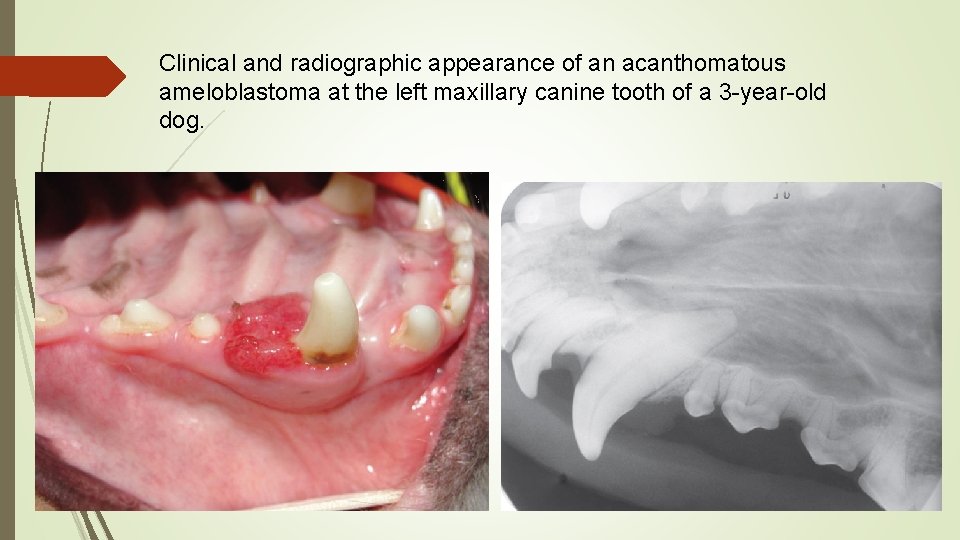
Clinical and radiographic appearance of an acanthomatous ameloblastoma at the left maxillary canine tooth of a 3 -year-old dog.

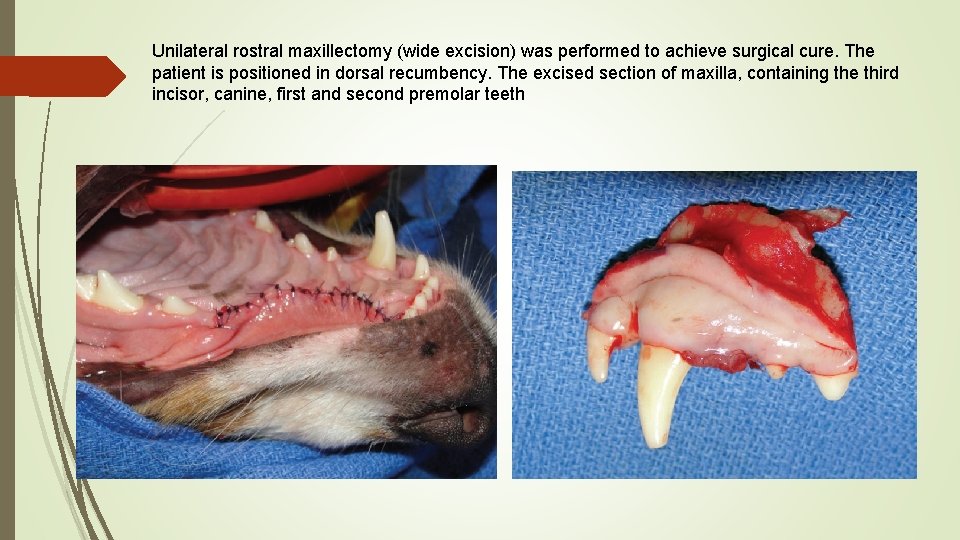
Unilateral rostral maxillectomy (wide excision) was performed to achieve surgical cure. The patient is positioned in dorsal recumbency. The excised section of maxilla, containing the third incisor, canine, first and second premolar teeth

Small Animal Dentistry A manual of techniques Cedric Tutt www. vet-dentist. com Oral and maxilla gacial surgery in dogs and cats Frank J M Verstraete, Milinda J Lommer Saunders elsevier 2012