Blood and Blood Forming Organs Diseases and Disorders

Blood and Blood Forming Organs Diseases and { Disorders Shelby Engel and Sarah Heins

Blood transports necessary nutrients and hormones Color, volume, viscosity, and p. H RBCs/erythrocytes – transport oxygen WBCs/leukocytes – infection prevention 4, 500 -11, 000 count >11, 00 indicates infection Platelets/thrombocytes cause blood coagulation 4. 2 -6. 3 million live 120 days Hemoglobin typically 13. 5 -18 g/100 ml for males, 12 -16 for females Clump at site of injury Calcium builds at site Fibrin clot is formed Clot is removed, scar tissue A, B, AB, O +/- blood classified by antigens in blood Blood forming organs Lymph nodes – protection from pathogens Bone marrow – major blood cell-producing organ Spleen – produces lymphocytes, plasma cells, and antibodies; filters microorganisms in blood, removes old blood from body Liver – blood-forming organ; aids in blood coagulation Anatomy & Physiology

Common Signs & Symptoms Increases or decreases in production of cells – RBC, WBC, Platelets HIGH VOLUME RBC WBC LOW VOLUME Erythrocytosis - reddened skin tones, bloodshot eyes, increased blood volume and pressure, increase in heart workload Erythrocyopenia leads to anemia – headache, fatigue, pallor, shortness of breath Leukocytosis – response to acute infection Leukocytopenia – weakened immune system Thrombocytosis – no serious side PLATELETS effects Thrombocytopenia – clotting problems, bruising, nosebleeds, blood lesions

Complete blood count – identifies RBCs, WBCs, and platelets; see page 128 in book Differential – more detailed count, identifies the number of each type of leukocyte Hematocrit – reflects the amount of red cell mass as a proportion of whole blood Hemoglobin – reflects oxygen-carrying potential available Mean corpuscular volume – average size of RBC Mean corpuscular hemoglobin – average hemoglobin content Mean corpuscular hemoglobin concentration – average hemoglobin concentration Blood smears Biopsy of blood-forming organs Bleeding time test – prick earlobe and measure time until clot Diagnostic Tests

Anemia Disorders of Red Blood Cells Iron Deficiency Anemia Folic Acid Deficiency Anemia Vitamin B 12 Deficiency Anemia Pernicous Anemia Hemolytic Anemia Sickle Cell Anemia Hemorrhagic Anemia Aplastic Anemia Polycythemias Polycythemia (Primary or Vera) Secondary Polycythemia (Erythrocytosis)

Anemia = Most common A decrease in RBC mass that can be caused by a number of different processes Can be serious enough if not determined or corrected Symptoms: Shortness of breath and headache Rapid heart beat Dizziness Pale skin Weakness and fatigue Treatment –Depends on the type of anemia Prevention – Eating a healthy diet with foods high in iron and b complex vitamins Vitamin B 12 Deficiency Anemia Results from dietary deficiency in B 12 or inability of the digestive tract to absorb it

Folic Acid Deficiency Anemia Can be related to poor diet, overcooking vegetables, and alcoholism Infancy and pregnancy Symptoms: Fatigue Weight loss Abdominal pain Black or bloody stools Chest pain Treatment – Increase intake of green leafy vegetables, mushrooms, lima beans, and kidney beans Prevention – Diet high in folic acids

Pernicous Anemia Usually affects older individuals and has an unusual cause Symptoms: People affected usually have an autoimmune disorder Pallor (paleness) Weakness Confusion Depression Numbness in the hands and feet Diagnosis – History, physical examinations, and blood testing for vitamin B 12 Treatment – Depends on the cause of the deficiency Absorption and diet – can be treated with oral vitamin tablets or injectable vitamin B 12 Monthly injection for life Not preventable

Hemolytic Anemia Increased destruction on RBCs Can be severe and lead to death Can be brought on by exposure to chemicals such as benzene; medications, including aspirin and penicillin; and bacterial toxins Symptoms Pallor (paleness) Weakness Fatigue Tachycardia (rapid heart rate) Diagnosis – thorough history, physical examinations, and blood testing Prevention – Genetic = not preventable; Acquired = preventable with proper screening
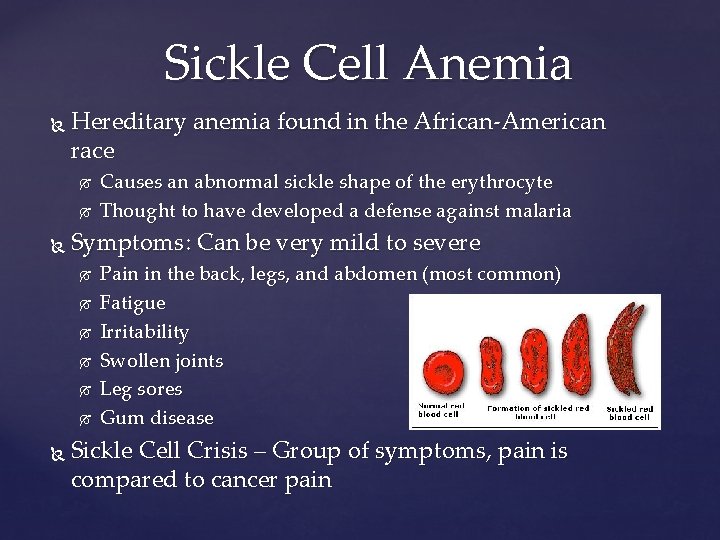
Sickle Cell Anemia Hereditary anemia found in the African-American race Symptoms: Can be very mild to severe Causes an abnormal sickle shape of the erythrocyte Thought to have developed a defense against malaria Pain in the back, legs, and abdomen (most common) Fatigue Irritability Swollen joints Leg sores Gum disease Sickle Cell Crisis – Group of symptoms, pain is compared to cancer pain

Sickle Cell Anemia cont. Diagnosis – History and blood testing Two blood tests Treatment – No cure and treatment is symptomatic 1 st = Measures the amount of normal and abnormal hemoglobin in the blood 2 nd = Measures the percent of red sickle cells after mixing a small drop of blood with a deoxygenating agent Increased fluid intake can help by increasing blood volume and improve sickle cell movement Prevention – Genetic counseling and decision to avoid childbearing

Hemorrhagic Anemia Loss of whole blood and can be called blood loss anemia Symptoms Pallor (paleness) Cool clammy skin Tachypnea Tachycardia If large amounts of blood is lost symptoms can include: Common complication = hypovolemic shock Dizziness Fainting Extreme thirst (result from dehydration) Diagnosis – History and physical examinations Treatment – Acute blood loss = apply oxygen, intravenous fluids and liquids taken by mouth; Severe blood loss = blood transfusion Prevention – Accident prevention and controlling chronic bleeding

Aplastic Anemia Failure of bone marrow to produce blood components Symptoms: This decrease in blood cells leads to anemia, infection, and hemorrhage Diagnosis – History and physical examination with blood testing Treatment – Severe cases have a poor prognosis with 50% fatality Due to injury or destruction of blood-forming area of the bone marrow Causes : Chemotherapy, radiation, viruses, and chemical toxins Discontinuing or avoiding the causative agent Bone marrow transplantation or blood transfusion Prevention – Avoiding causative agent, but often the agent is unknown which makes prevention impossible

Polycythemia (Primary or vera) Condition of too many blood cells Symptoms: Caused by hyperplasia of the cell-forming tissues of the bone marrow Raised blood pressure Enlarged spleen Bloodshot eyes Redness of skin Shortness of breath Dizziness Diagnosis – Can be accidently discovered through routine blood testing Treatment – Reduce the red cell count, blood removal at regular intervals will reduce the volume (common treatment) Prevention – Cannot be prevented

Secondary Polycythemia (Erythrocytosis) Red cell numbers increase Symptoms: Headaches Weakness Fatigue Lightheadedness Shortness of breath Diagnosis – History, physical exam, and blood testing Treatment – Treated by addressing the cause of the disorder Prevention – Stopping the causative factor or by doing the things that deprive the body of needed oxygen, avoiding smoking, and avoid living in high altitudes

Disorders of White Blood Cells Common problems of the hematologic system Mononucleoisis Leukemia Lymphoma Hodgkin’s Disease Non-Hodgkin’s Lymphoma Multiple Myeloma

Primarily affects children and young adults Contagious by direct contact with saliva Last several weeks Epstein-Barr Virus (EBV) Fatigue, sore throat, fever, swollen lymph glands, spleen enlargement Diagnosed by WBC count high Rest, analgesics, throat gargles, avoiding sports activities Prevent through good oral hygiene Mononucleoisis, the “kissing disease”
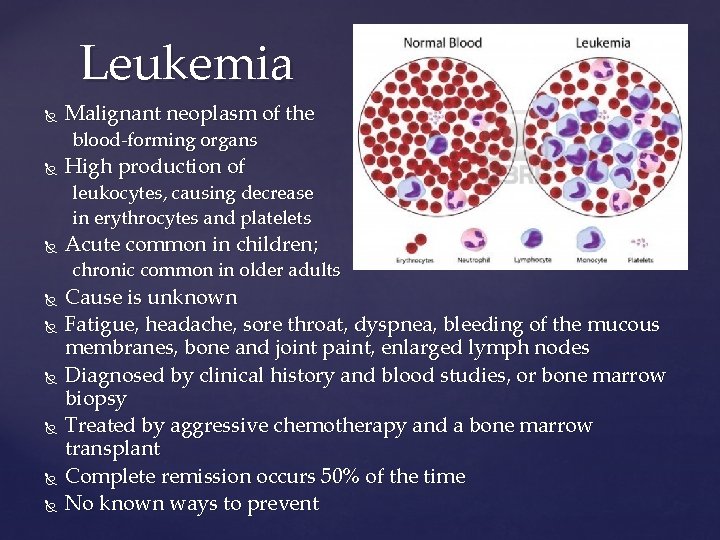
Leukemia Malignant neoplasm of the blood-forming organs High production of leukocytes, causing decrease in erythrocytes and platelets Acute common in children; chronic common in older adults Cause is unknown Fatigue, headache, sore throat, dyspnea, bleeding of the mucous membranes, bone and joint paint, enlarged lymph nodes Diagnosed by clinical history and blood studies, or bone marrow biopsy Treated by aggressive chemotherapy and a bone marrow transplant Complete remission occurs 50% of the time No known ways to prevent

Lymphomas Neoplasms that affect lymphoid tissue Lead to impaired immunity Most common type of blood cancer Hodgkin’s Disease Non-Hodgkin’s Lymphoma Multiple myeloma

Most common lymphoma Orderly spread of disease from one lymph node group to another Cause is thought to be viral Painless enlargement of the lymph nodes in the neck, weight loss, fever Primarily affects young adults, average of 35 Men at higher risk than women Reed-Sternberg Diagnosed with lymph node and bone marrow biopsy Treated with radiation and chemotherapy Complete cure after 5 years of remission 93% cure rate – one of the most curable forms of cancer 20% mortality rate No known preventive measures Hodgkin’s Disease

Non-Hodgkin’s Lymphoma Not containing the Reed-Sternberg cell characteristics; more widespread than Hodgkin’s Affects more older adults, average of 50 years Men are affected 1. 5 X more often than women Cause is unknown Patients who receive/have received immuno-suppressive medication 100 X more likely chance of developing NHL Painless enlargement of lymph nodes in neck, axilla, and inguinal areas; fever, night sweats, weight loss Diagnosed by absence of Reed-Sternberg, and lymph node and bone marrow biopsy Combination of radiation and chemotherapy Those at increased risk – exposure to pesticides, solvents and fertilizers Cure rate of 63% Mortality rate of 33%
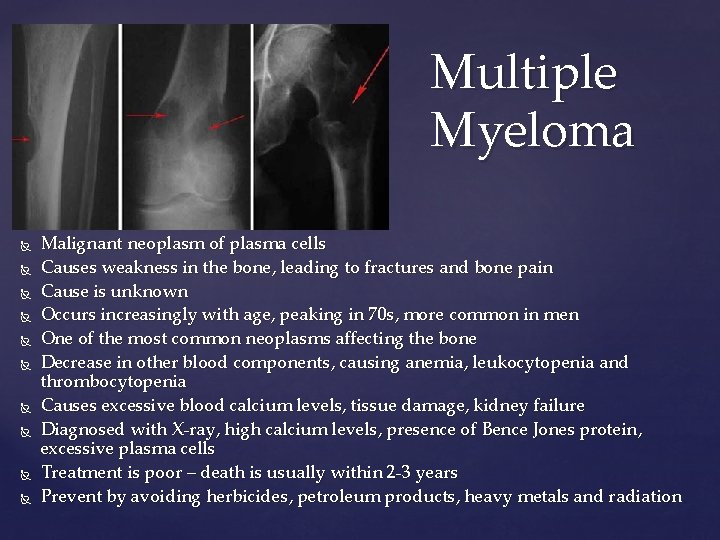
Multiple Myeloma Malignant neoplasm of plasma cells Causes weakness in the bone, leading to fractures and bone pain Cause is unknown Occurs increasingly with age, peaking in 70 s, more common in men One of the most common neoplasms affecting the bone Decrease in other blood components, causing anemia, leukocytopenia and thrombocytopenia Causes excessive blood calcium levels, tissue damage, kidney failure Diagnosed with X-ray, high calcium levels, presence of Bence Jones protein, excessive plasma cells Treatment is poor – death is usually within 2 -3 years Prevent by avoiding herbicides, petroleum products, heavy metals and radiation

Disorders of Platelets and Clotting Platelet disorders vary in terms of cause, severity, and treatment All share common symptom of bleeding Many of these disorders are inherited Hemophilia Thrombocytopenia Disseminated Intravascular Coagulation (DIC)

Hemophilia Group of bleeding disorders characterized by abnormally slow clotting and long bleeding times Hemophiliacs lack a blood protein that plays a role in clot formation Symptoms: X-linked hereditary bleeding disorder Commonly occurs in male children Frequent nosebleeds Bruising Prolonged bleeding in a male child (can indicate hemophilia) Can be mild to severe Severe cases are called hemarthrosis or bleeding into joints, which is painful, and recurrent episodes can lead to joint deformity
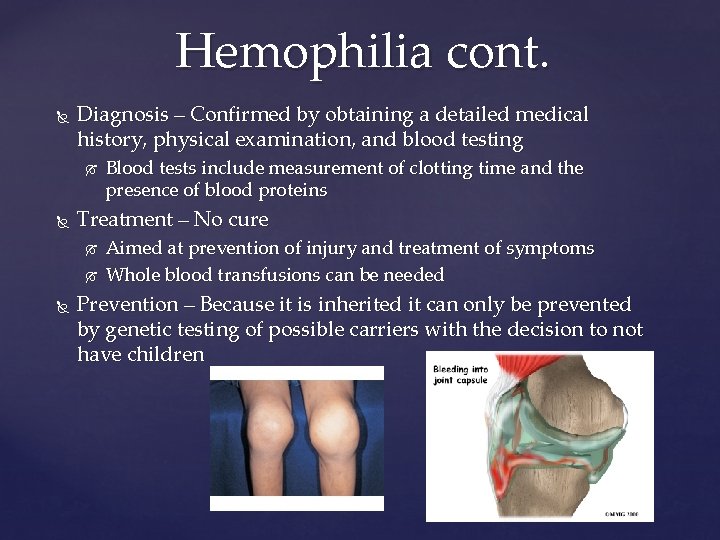
Hemophilia cont. Diagnosis – Confirmed by obtaining a detailed medical history, physical examination, and blood testing Treatment – No cure Blood tests include measurement of clotting time and the presence of blood proteins Aimed at prevention of injury and treatment of symptoms Whole blood transfusions can be needed Prevention – Because it is inherited it can only be prevented by genetic testing of possible carriers with the decision to not have children

Thrombocytopenia Decrease in platelets that leads to an inability to clot blood normally Symptoms: Abnormal bleeding in the skin, mucous membranes, and internal organs Small hemorrhagic spots on skin; larger purplish hemorrhagic spots Frequent nosebleeds Blood in urine Can be due to inadequate or abnormal platelet production or destruction Cause is unknown Diagnosis – Individual clinical history along with platelet count and bleeding time

Thrombocytopenia cont. Treatment : Avoid tissue trauma to reduce potential bleeding Administration of vitamin K to improve clotting Transfusion on platelets Prevention- Most cases are not preventable, but there are two steps that can be taken to prevent complications Avoid taking medications that decrease platelet aggregation or stickiness, thus making them less likely to clot. (Ex: Aspirin or Ibuprophen) Avoid heavy drinking because alcohol slows platelet production
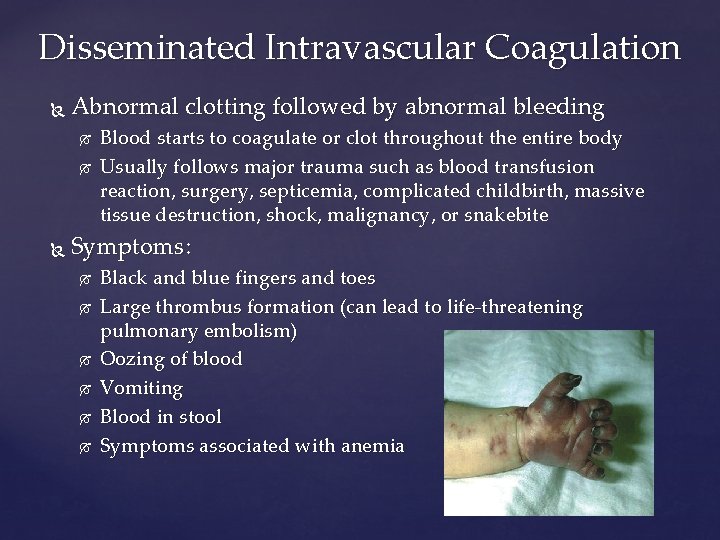
Disseminated Intravascular Coagulation Abnormal clotting followed by abnormal bleeding Blood starts to coagulate or clot throughout the entire body Usually follows major trauma such as blood transfusion reaction, surgery, septicemia, complicated childbirth, massive tissue destruction, shock, malignancy, or snakebite Symptoms: Black and blue fingers and toes Large thrombus formation (can lead to life-threatening pulmonary embolism) Oozing of blood Vomiting Blood in stool Symptoms associated with anemia

DIC cont. Diagnosis – History of trauma and blood studies Treatment – Identifying and treating underlying cause can stop DIC Medications Heparin – an anticoagulant medication to halt the formation of thrombi Platelet administration to increase clotting ability Difficult to manage This condition is usually life-threatening and can lead to death Often times it is referred to as “Death Is Coming” (DIC) Prevention – Getting prompt medical treatment for any condition that might bring on this disorder

Rare Diseases Thalassemia Von Willebrand’s Disease Hereditary hemolytic anemia Mediterranean descent Dysfunctional RBCs leading to anemia symptoms Hereditary, congenital bleeding disorder Deficiency in clotting and platelet function Lymphosarcoma Similar to Hodgkin’s Disease With remission, prognosis is good

Childhood Diseases: Acquired Immunodeficiency Syndrome & Leukemia Acquired Immunodeficiency Syndrome (AIDS ) affects thousands of children in the US 1980 s – HIV infection mainly acquired through blood transfusions Today – Most all HIV infections in children are a result of maternalfetal transfer through blood (also called perinatal transmission) Symptoms: Many children to not experience symptoms and live a normal life for years Diagnosis – When T-cell count drops below 200 cells per microliter Treatment – Good nutrition, antiviral drugs, and other support therapies Prevention- prevent mother-to-child transmission, provide pediatric treatment, and prevent infection among adolescents

References Cancer. gov CDC. gov Human Diseases, 3 rd Ed. , M. Neighbors & R. Tannehill-Jones
- Slides: 32