MANAGEMENT OF MALNUTRITION Severe Acute Malnutrition Weight for























- Slides: 24

MANAGEMENT OF MALNUTRITION

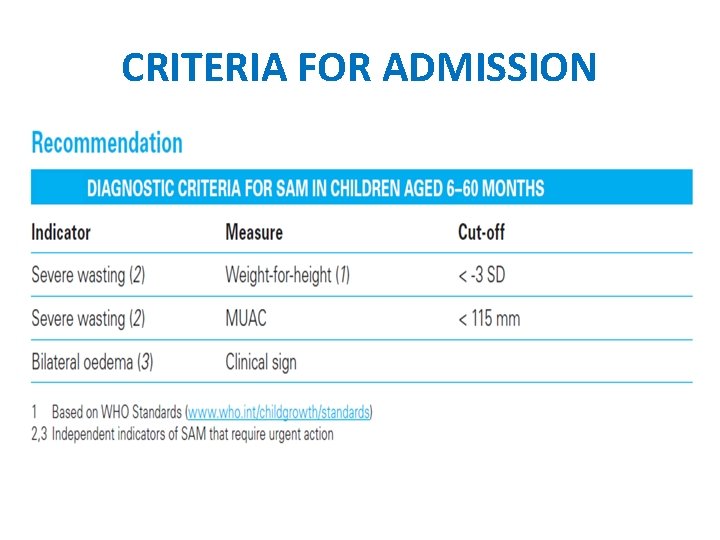
Severe Acute Malnutrition • • Weight for height/length <70% or<3 SD Bipedal edema MUAC < 11. 5 cm Visible wasting

CRITERIA FOR ADMISSION


INITIAL ASSESSMENT • History • Examination

STEPS OF MANAGEMENT 1. Treat/prevent hypoglycemia 2. Treat/prevent hypothermia 3. Treat/prevent dehydration 4. Correct electrolyte imbalance 5. Treat/prevent infection

STEPS OF MANAGEMENT 6. Correct micronutrient deficiencies 7. Start cautious feeding 8. Achieve catch-up growth 9. Provide sensory stimulation and emotional support 10. Followup after recovery

HYPOGLYCEMIA • Blood glucose <54 mg% or 3 mmol/l • Symptomatic or asymptomatic • Hypoglycemia, hypothermia, infection occur as a triad • Treatment: – 10% dextrose orally/NG Tube/IV – Start feeds

HYPOTHERMIA • Rectal temp <35. 5 deg. C • Axillary temp <35 deg. C • Treatment: – Feeding – Covering – Rewarming – Antibiotics

DEHYDRATION • Assessment of severity difficult • Treatment: reduced osmolarity ORS • IVF for severe dehydration

DYSELECTROLYTEMIA • Excess of body sodium • Low serum potassium and magnesium • Treatment: – supplement potassium : 3 -4 meq/kg/day – Magsulf : 0. 3 ml/kg IM

INFECTIONS • Clinical signs may be subtle • Investigations to be done • Treatment: – broad spectrum antibiotics

MICRONUTRIENT DEFICIENCY • Upto twice the RDA • Do not give Iron till 1 week

INITIATE REFEEDING • Initiate feeding as soon as possible with feeds: – osmolality <350 mosm/l – Lactose not more than 2 -3 g/kg/d – Appropriate renal solute load

INITIATE REFEEDING • Initiate feeding as soon as possible with feeds – Adequate bioavailability of micronutrient – Initial percentage of calories from proteins of 5% – Adequate bioavailability of micronutrients – Low viscosity, easy to prepare and socially acceptable – Adequate storage, cooking and refrigeration

INITIATE REFEEDING • Start feeding early • Recommended energy intake : – 100 kcal/kg/d – Protein : 1 -1. 5 g/kg/d • Total fluid recommended: 130 ml/kg/d • Continue breast feeding ad libitum

TYPES OF DIETS • F 75 • F 100 • RUTF (Ready to Use Therapeutic Food ) • Home based food

CATCH UP GROWTH • Calorie intake increased to 150 -200 kcal/kg/d • Proteins: 4 -6 g/kg/d

SENSORY STIMULATION AND EMOTIONAL SUPPORT • Cheerful stimulating environment • Age appropriate structured play • Age appropriate physical activity • Tender loving care

PREPARE FOR FOLLOWUP • Primary failure: – Failure to regain appetite by d 4 – Failure to start losing edema by d 4 – Presence of edema on d 10 – Failure to gain at least 5 g/kg/d by d 10

PREPARE FOR FOLLOWUP • Secondary failure: – Failure to gain at-least 4 g/kg/d for 3 consecutive days during the rehabilitative phase

CRITERIA FOR DISCHARGE • Absence of infection • Child is eating at least 120 – 130 Kcal/Kg/day and is receiving adequate micronutrients • There is consistent weight gain (of at least 5 gm/Kg/day for 3 consecutive days) on exclusive oral feeding

CRITERIA FOR DISCHARGE • WFH >3 SD • Absence of edema • Completed immunization appropriate for age • Caretakers are sensitized to home care

Thanks!