Inherited Coagulation Disorders Dr Galila Zaher Consultant Hematologist





























- Slides: 41

Inherited Coagulation Disorders Dr Galila Zaher Consultant Hematologist KAUH

BLOOD CLOTTING Blood clotting interactions Plasma protein clotting factors Platelets Vascular endothelium

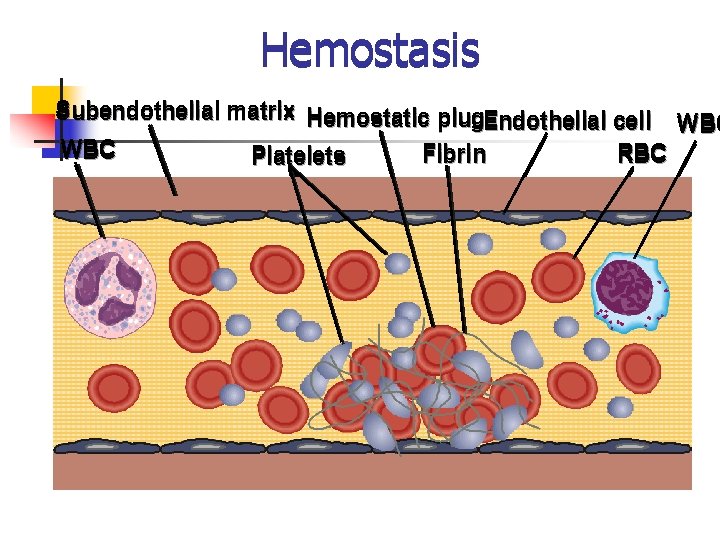
Hemostasis Subendothelial matrix Hemostatic plug. Endothelial cell WBC Fibrin RBC Platelets

COAGULOPATHIES Bleeding Clotting factors platelets Thrombosis Natural anticoagulant

Clot formation Platelet activation No &count Fibrin generation plasma clotting factors Primary hemostasis (immediate) Secondary hemostasis (delayed)

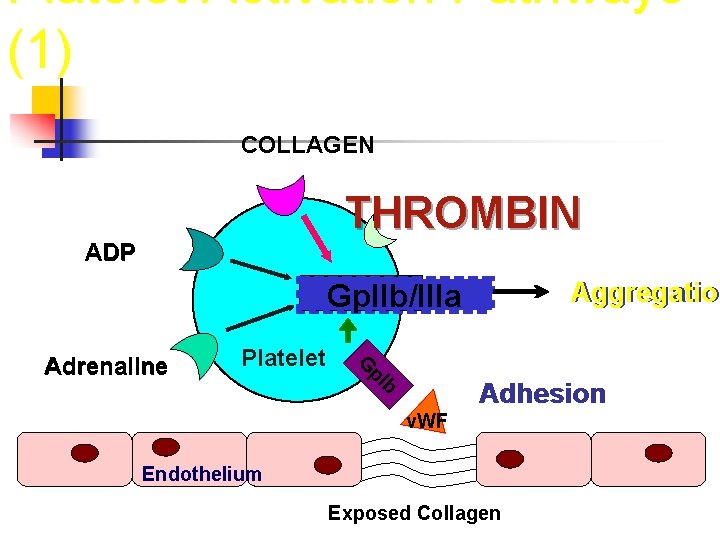
Platelet Activation Pathways (1) COLLAGEN THROMBIN ADP Aggregation Aggregatio Gp. IIb/IIIa Platelet G p. I Adrenaline b Adhesion v. WF Endothelium Exposed Collagen

Clotting factor production Liver: source of plasma clotting factors except VWF Factor VIII: produced by liver & endothelium VWF: endothelial cells & megakaryocytes Vitamin K dependent clotting factors are: II, VII, IX, X

COAGULATION PATHWAYS Intrinsic & extrinsic pathways “conclude” in the common pathway Intrinsic pathway clotting factors Extrinsic pathway clotting factors Common pathway clotting factors

NORMAL COAGULATION PATHWAYS Intrinsic pathway clotting factors Factor XII Factor VIII Extrinsic pathway clotting factors Tissue factor (TF)* Factor VII Common pathway clotting factors Factor X Factor V Factor II Prothrombin Factor I Fibrinogen Factor IX Factor XI

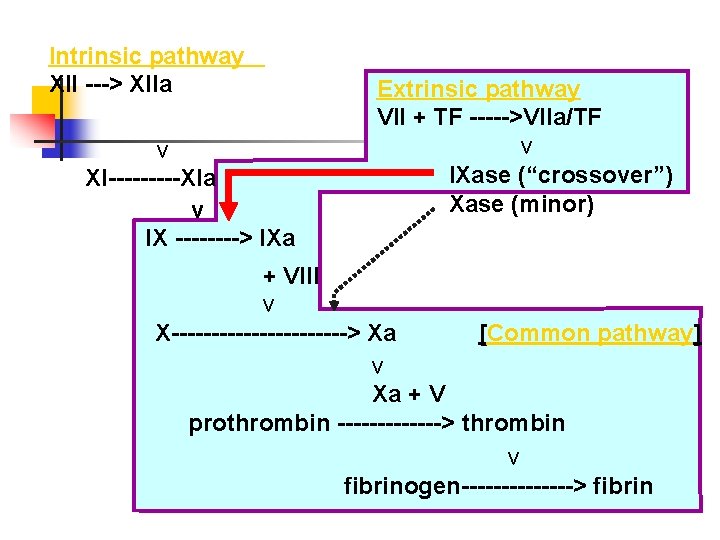
Intrinsic pathway XII ---> XIIa v XI-----XIa v IX ----> IXa Extrinsic pathway VII + TF ----->VIIa/TF v IXase (“crossover”) Xase (minor) + VIII v X-----------> Xa [Common pathway] v Xa + V prothrombin -------> thrombin v fibrinogen-------> fibrin

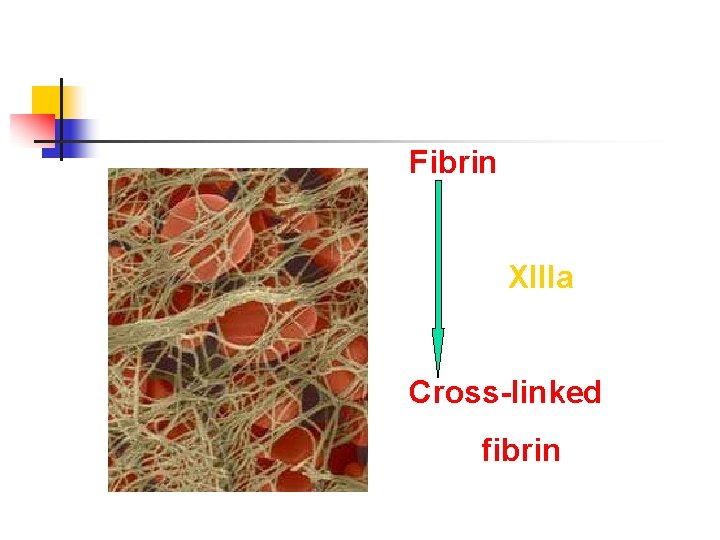
Fibrin XIIIa Cross-linked fibrin

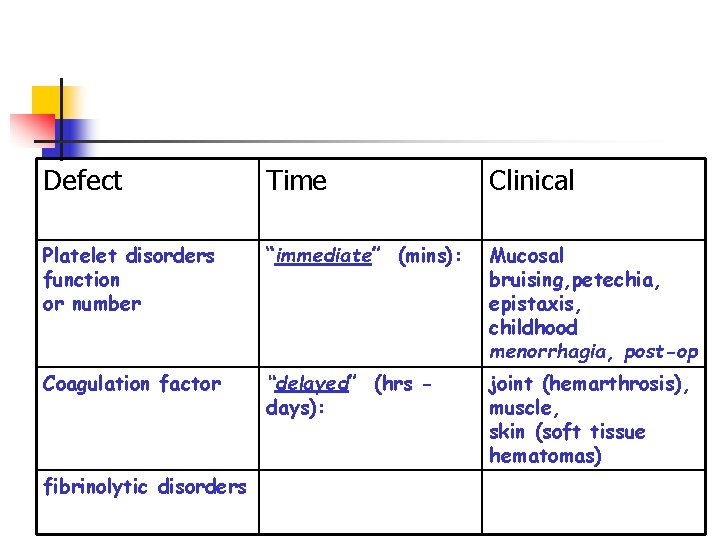
Defect Time Clinical Platelet disorders function or number “immediate” (mins): Mucosal bruising, petechia, epistaxis, childhood menorrhagia, post-op Coagulation factor “delayed” (hrs days): joint (hemarthrosis), muscle, skin (soft tissue hematomas) fibrinolytic disorders

Deficiencies of: Ø Factor XII Ø High molecular weight kininogen Ø Prekallikrein Ø - Do NOT produce bleeding diatheses

COAGULATION TESTS Ø Platelet tests <150, 000 thrombocytopenia >400, 000 thrombocytosis Ø Tests of clotting factors

Platelet tests Test Platelet count Comment Part of routine CBC, normal count: 150, 000 - 400, 000/u. L Mean platelet volume MPV Some analyzers provide MPV measurement; in healthy individuals, MPV varies inversely with platelet count Platelet aggregation and secretion tests Not routine tests, used only in special circumstances

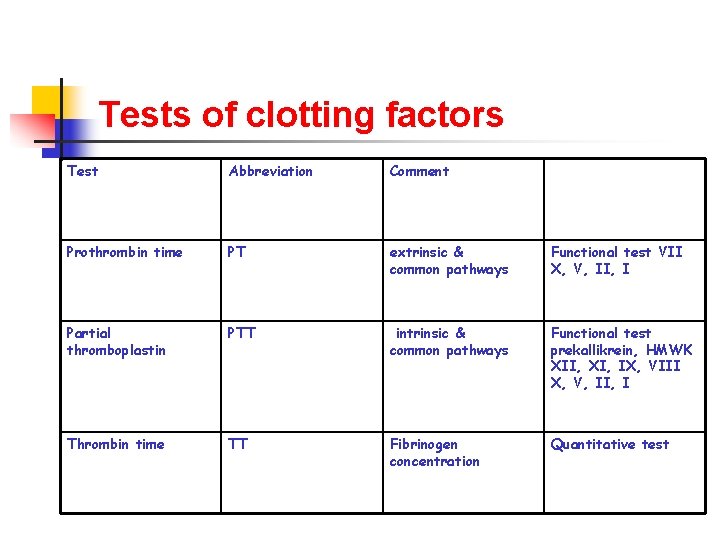
Tests of clotting factors Test Abbreviation Comment Prothrombin time PT extrinsic & common pathways Functional test VII X, V, II, I Partial thromboplastin PTT intrinsic & common pathways Functional test prekallikrein, HMWK XII, XI, IX, VIII X, V, II, I Thrombin time TT Fibrinogen concentration Quantitative test

Hemophilia A = Factor VIII deficiency Ø B = Factor IX deficiency Ø Affects one in 6000 males Ø A is 5 X > B Ø Mild > 5 % normal amount of factor Ø Moderate 2 - 5 %, severe < 2 % Ø Levels remain stable throughout life

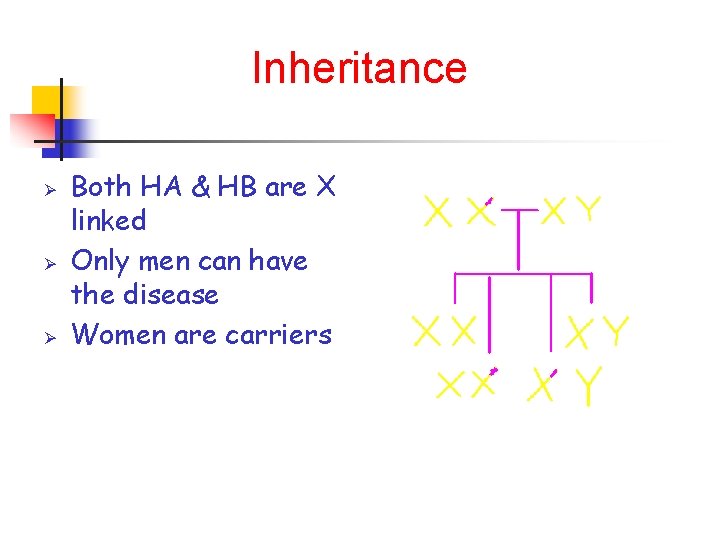
Inheritance Ø Ø Ø Both HA & HB are X linked Only men can have the disease Women are carriers

Clinical presentation Ø < 2 years: joint bleeds Rare Only bruising or mouth bleeds are seen Head injuries are a major concern Ø > 2 years joint and muscle bleeds become more common

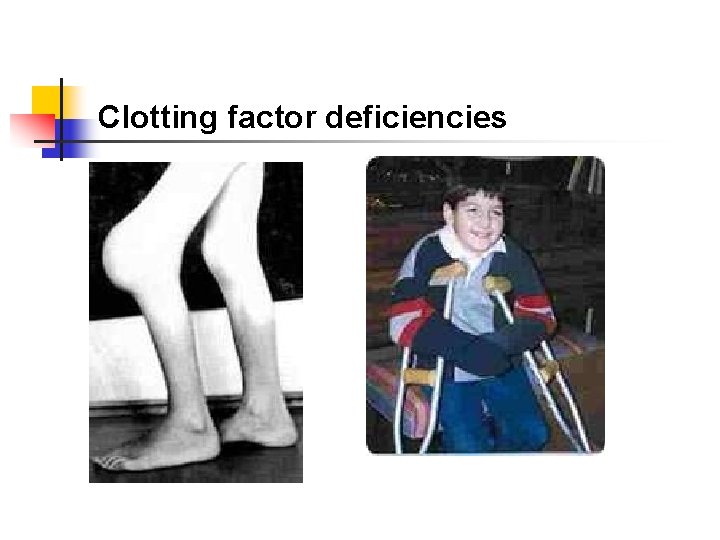
Clotting factor deficiencies

Laboratory Diagnosis n n Isolated prolongation of APTT Microcytic hypochromic anemia Normal platelets count Mixing studies : corrected.

When to treat Ø Ø All joint bleeds: Pain, swelling , warmth or loss of movement. Muscle bleeds that cause severe pain or are in a dangerous location Bruises usually don’t need treatment When in doubt.

Treatment Ø Ø Ø Keep weight off of joint Ice pack Factor replacement - the sooner the better Amicar or tranexamic acid : mouth bleed CVL s : Frequent bleeds or factor given on a regular basis Port-a-catheters

Dose & Duration Ø Ø Ø 1 IU/kg of factor VIII increases the level by 2% 1 IU/kg of factor IX increases the level by 1% Every 12 hours the level decreases by half

Prophylaxis Ø Ø Ø To prevent bleeds Started after developing a target joint Usually it is administered 3/week Stepwise approach: Initially 1/week, increasing to 2 -3/week if needed Goal is to prevent long-term joint damage

Team Approach Ø We all work together Child and parents Doctor and nurses Physiotherapy Social work Ø Ø Everyone has an essential role The aim is to get life to be as normal as possible

Factor VIII Replacement Ø Ø Mechanism of action : activate FX Mode of administration : IV Monitoring : no predict the effectiveness of treatment Indications : HA & HB Ø Ø Severe surgical bleeding Factor VII deficiency

Factor VIII Ø Ø Ø Derived from pooled human plasma Derived from pig (porcine) plasma Recombinate products

Porcine factor VIII Ø Ø Ø Hyate: C Apparently no pig viruses present Can replace human Factor VIII in clotting cascade Minimal cross reactivity with AHF antibodies Minimal von Willebrand factor present

von Willebrand Factor (V W F) Ø VWF bridges platelets to collagen exposure from blood vessel injury Ø VWF contributes to primary hemostasis Ø Factor VIII circulates bound to VWF. Ø VWD: clinically similar to platelet disorders Ø Most common inherited bleeding disorder

VWD Ø Ø Ø Ø Inherited as a dominant or recessive. Most common congenital bleeding disorder Affecting 1 -3% of the population. Personal and family bleeding history. Highly heterogeneous Ranging from asymptomatic to a life threatening bleeding. The most common bleeding symptoms ever were epistaxis, bruising Menorrhagia is one of the most important and frequent complications in women

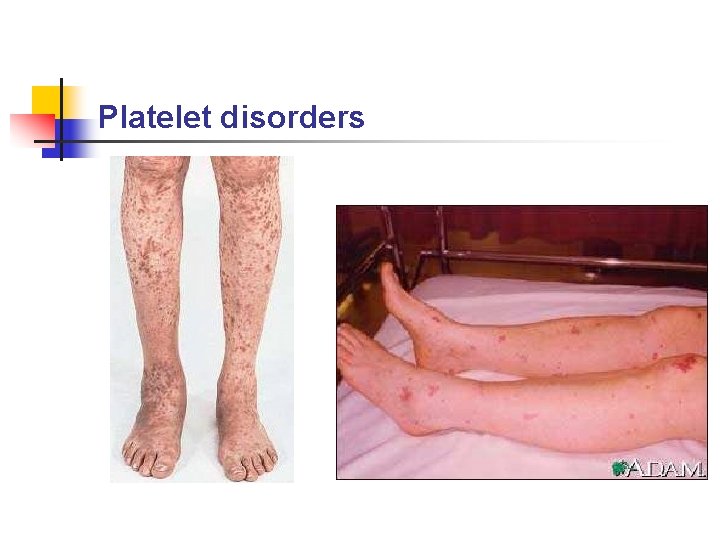
Platelet disorders

DIAGNOSIS Ø Ø The condition is caused by a quantitative or qualitative deficiency of v. WF. Prolonged bleeding time (BT) & activated partial thromboplastin time (APTT) iron deficiency anemia. type 1 v. WD

Managment Ø Ø The aim of treatment is to correct the dual defect of hemostasis ( low VIII: C & prolonged bleeding time). DDAVP is the treatment of choice for the mild forms of type 1 and 2 VWD Unresponsive to DDAVP, plasma virally inactivated concentrates of factor VIII Tranexamic acid

Increased PT Deficient, function or inhibition : Liver disease production/ vit K malabsorption vit. K antagonists warfarin (blocks carboxylation) Heparin the PTT is a more sensitive test FDPs inhibits coagulation lupus anticoagulant PTT is a better test (LA)

Increased PTT Heparin unfractionated heparin inhibits Xa and IIa vit K antagonists PT is a more sensitive fibrin/fibrinogen inhibits coagulation degradation products lupus anticoagulant PTT is a better than PT

TT increased Ø Congenital disorders afibrinogenemia homozygous def. hypofibrinogenemia heterozygous def. dysfibrinogenemia dysfunctional fibrinogen Ø Acquired disorders hypofibrinogenemia dysfibrinogenemia Fibrin degradation products Heparin liver disease, (disseminated intravascular coagulation), thrombolytic therapy liver disease, hepatic malignancy inhibits coagulation inactivates IIa

Fibrinogen level hypofibrinogenemia) Liver disease decreased production Consumption disseminated intravascular coagulation (DIC) Thrombolytic therapy Congenital def. afibrinogenemia: homo. def. hypofibrinogenemia: hetero.

Fibrinogen assay quantitative immunoassay: Functional “immunologic” or “antigenic” fibrinogen Increased: Estrogen Pregnancy Acute phase response decreased hypofibrinogenemia) also - dysfunctional fibrinogen (dysfibrinogenemia

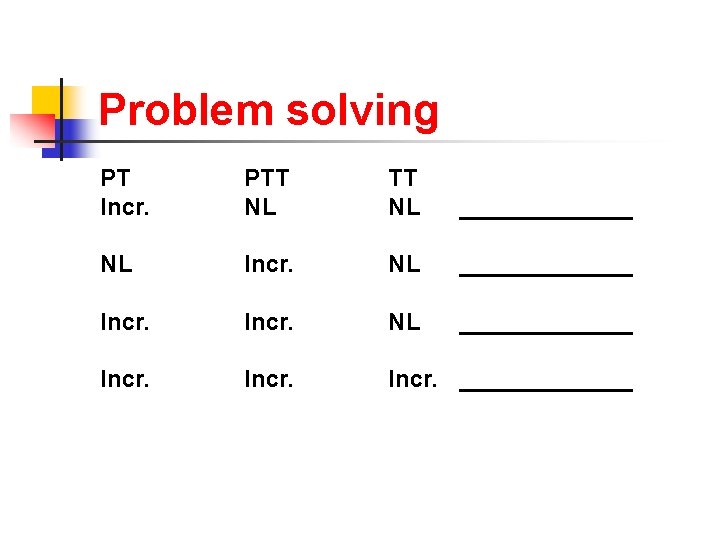
Problem solving PT Incr. PTT NL _______ NL Incr. NL _____________ Incr. _______

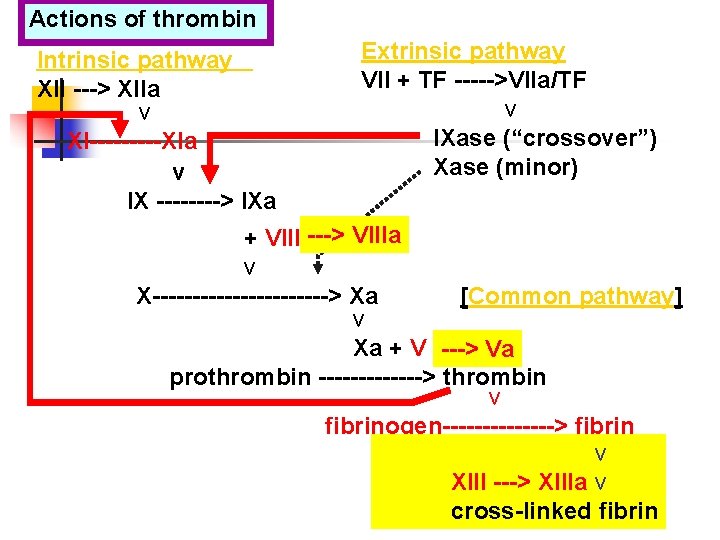
Actions of thrombin Intrinsic pathway XII ---> XIIa v XI-----XIa v IX ----> IXa Extrinsic pathway VII + TF ----->VIIa/TF v IXase (“crossover”) Xase (minor) + VIII ---> VIIIa v X-----------> Xa [Common pathway] v Xa + V ---> Va prothrombin -------> thrombin v fibrinogen-------> fibrin v XIII ---> XIIIa v cross-linked fibrin