HEPARIN INDUCED THROMBOCYTOPENIA GALILA ZAHER MBB ch dip

HEPARIN INDUCED THROMBOCYTOPENIA GALILA ZAHER MBB ch, dip C Path, MRC Path

Heparin induced thrombocytopenia(HIT) HIT: is an immune mediated side effect which can be life threatening. Incidence : 1 -3%of patient receiving heparin.
Heparin induced thrombocytopenia Higher risk for HIT *Therapeutic > prophylactic doses. *Bovine lung extract > porcine heparin *Unfractunated heparin > LMWH. HIT *IV , SC, hepsal flush , extra corporal blood circuit & heparin coated materials.

Pathogenesis Heparin treatment release platelet factor 4. Heparin can bind to PF 4 on platelet surface & vascular endothelium. Antibodies are directed against heparin -PF 4 (H-PF 4). Antibodies involved in HIT are usually Ig. G , but Ig. A & Ig. M have been reported.

Type 1 HIT The most common form of HIT. Early onset (3 -5 d). Mild thrombocytopenia(80 -100 x 109/l). Direct effect of heparin. Reversible Asymptomatic.

Type II HIT Less frequent than type I HIT Delayed onset (5 -14 d). Plt count is <60 x 109/L Can be life threatening 29% mortality rate (HITT). Immunological reaction. Requires clinical intervention & immediate discontinuation of heparin.
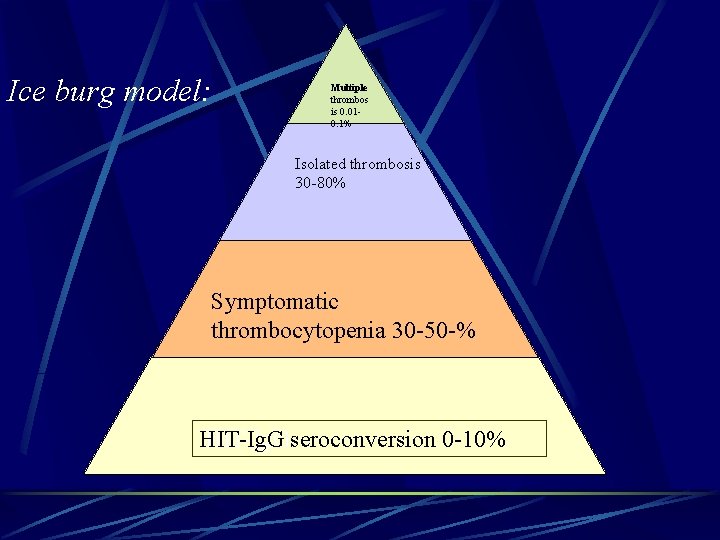
Ice burg model: Multiple thrombos is 0. 010. 1% Isolated thrombosis 30 -80% Symptomatic thrombocytopenia 30 -50 -% HIT-Ig. Gseroconversion 0 -10%

Clinical presentation of type II HIT Males and females are equally affected. All ages. Venous thrombosis more common than arterial. Patient who develop skin lesions at heparin injection sites are at increased risk of thrombosis. CVD arterial. Post operative venous thrombosis.

Clinical presentation *Venous thrombosis : DVT&PE. Warfarin induced venous limb gangrene. Cerebral sinus thrombosis. Adrenal hemorrhagic infarction. *Arterial thrombosis: lower limb (distal aortic or iliofemoral). Stroke & Myocardial infarction. *Acute plt activation syndrome : *Skin lesions

Laboratory diagnosis of HIT Existing lab methods do not distinguish between HIT & HITTS. * 14 C Seratonin release assay. * H-PF 4 ELISA. * The platelets aggregation assay. * Flow-cytometric assay. Until improved laboratory diagnosis of HIT clinical impression are best used to direct therapy in patient with suspected HIT

Flow cytometry in diagnosis of HIT Provides rapid diagnosis. 100% specificity and sensitivity. Reproducible. flow cytometric assay of CD 62 P can distinguish HIT from HITTS.

Heparin therapy Regular platelets count. Type I HIT syndrome - observation. Type II HIT syndrome : *D/C heparin *no platelet concentrate *no warfarin during the acute phase *no LMWH *Heparinoid

Thrombin inhibitors HIRUIDIN: *Natural hiruidin : The leech salivary extract (hirudo medicinalis). *synthetic hirudin (argatroban). *recombinant (r- hiruidin). Danaparoid. Hirulogs.

PLASMAPHERESIS Removal of plasma &replacement with normal plasma or colloids. It has been done on 3 consecutive days. Early treatment (4 days) reduces the incidence of mortality It dose not affect the number of the thrombotic events.

Extremity Arterial Thrombosis & Stroke. Digits only : *Argatroban. Entire extremity : *Thrombolytic therapy, *Continue argatroban, *Plasmapharesis. Stroke with no evidence of hemorrhage: *Argatroban Stroke with evidence of hemorrhage : *Plasmapheresis.

Laboratory diagnosis. ctd Combined results of the three assays enhances the positive response to 83%of the total population with HIT. The combination of the three testing with multiple samples offers the best chance of confirming a positive diagnosis of HIT. Clinical event & a positive reliable laboratory test confirms the diagnosis of HIT.

14 C serotonin release assay The gold standard for diagnosis. It is a biologic assay. It requires the use of radioactive materials. It has a sensitivity of 55%. The complexity & the slow turn around time of the assay compromise its practical usefulness for immediate treatment decisions.

THANK YOU
- Slides: 18