Histopathologic Validation of the Intravascular Ultrasound Diagnosis of








- Slides: 22

Histopathologic Validation of the Intravascular Ultrasound Diagnosis of Calcified Coronary Artery Nodules Akiko Maehara, MD Cardiovascular Research Foundation/Columbia University Medical Center, New York

Akiko Maehara, MD § Contracted Research/Grant Support: § Boston Scientific Corporation § Honoraria: § Volcano Therapeutics, Inc.

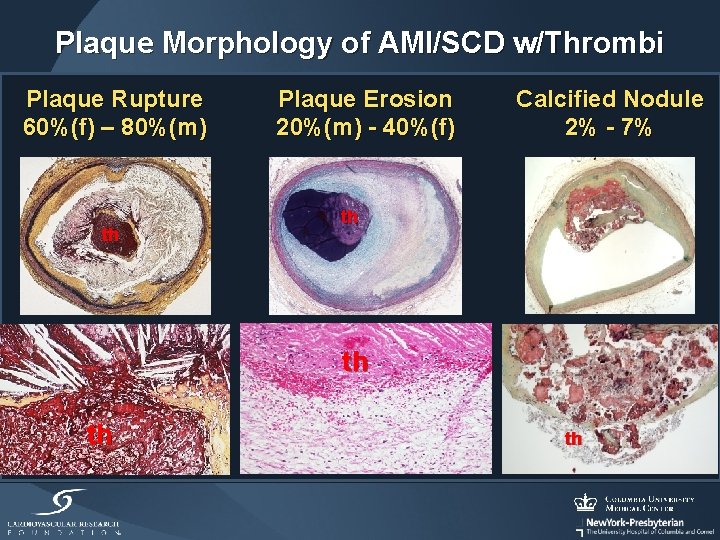
Plaque Morphology of AMI/SCD w/Thrombi Plaque Rupture 60%(f) – 80%(m) th Plaque Erosion 20%(m) - 40%(f) Calcified Nodule 2% - 7% th th

Frequency of Calcified Nodules • 29 coronary arteries (11 LAD, 5 LCX, 13 RCA) in 18 pts • 856 matched pathological slices (every 2 mm) matched IVUS • 268 IVUS frames contained calcification, and 17 frames (6%) appeared calcified nodule, 268 frames (94%) appeared non-nodular calcification. • 2 calcified nodules were solitary, and 15 calcified nodules were adjacent to non-nodular calcium.

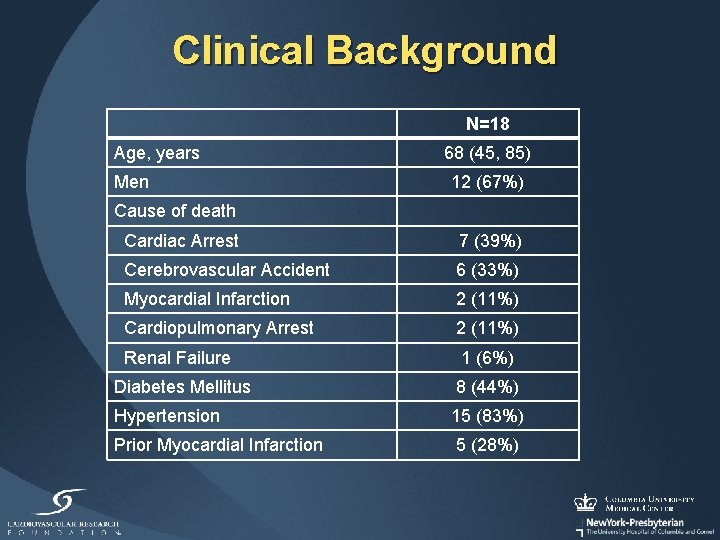
Clinical Background N=18 Age, years Men 68 (45, 85) 12 (67%) Cause of death Cardiac Arrest 7 (39%) Cerebrovascular Accident 6 (33%) Myocardial Infarction 2 (11%) Cardiopulmonary Arrest 2 (11%) Renal Failure 1 (6%) Diabetes Mellitus 8 (44%) Hypertension 15 (83%) Prior Myocardial Infarction 5 (28%)

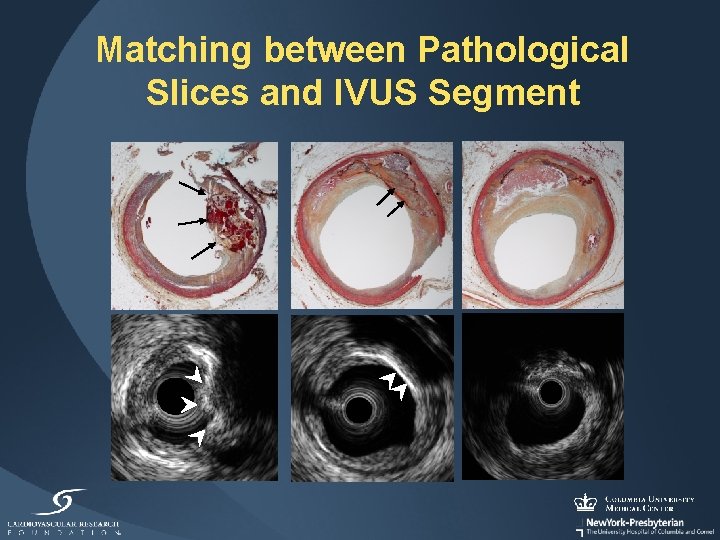
Matching between Pathological Slices and IVUS Segment

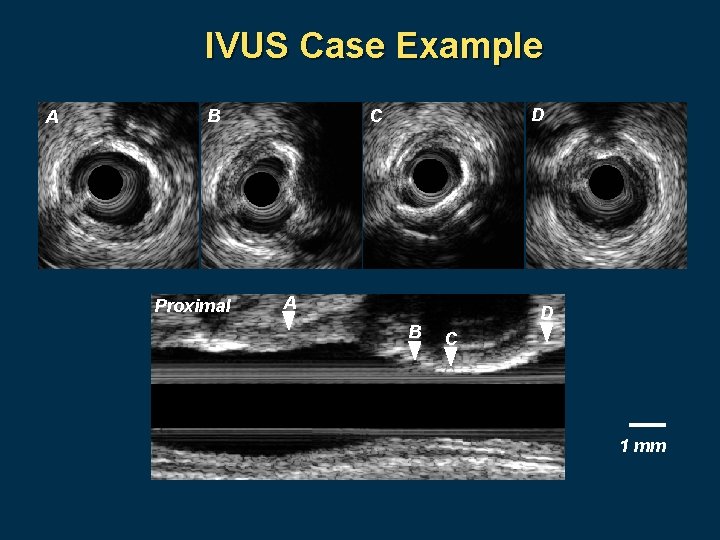
IVUS Case Example A B Proximal D C A B D C 1 mm

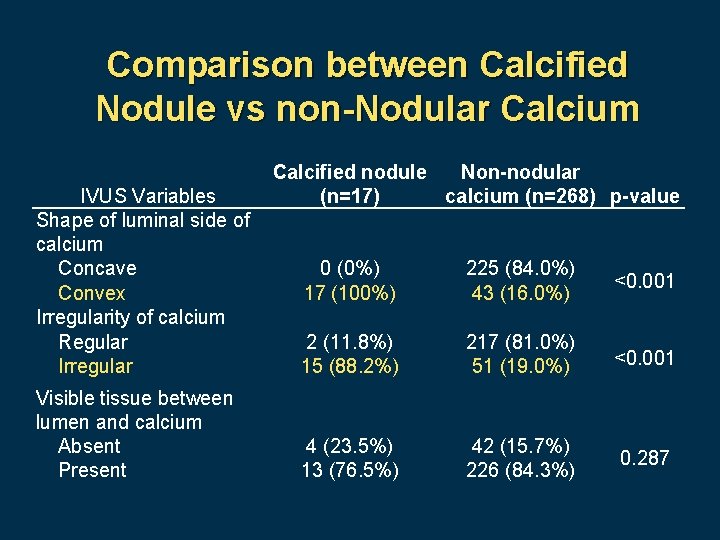
Comparison between Calcified Nodule vs non-Nodular Calcium IVUS Variables Shape of luminal side of calcium Concave Convex Irregularity of calcium Regular Irregular Visible tissue between lumen and calcium Absent Present Calcified nodule Non-nodular (n=17) calcium (n=268) p-value 0 (0%) 17 (100%) 225 (84. 0%) 43 (16. 0%) <0. 001 2 (11. 8%) 15 (88. 2%) 217 (81. 0%) 51 (19. 0%) <0. 001 4 (23. 5%) 13 (76. 5%) 42 (15. 7%) 226 (84. 3%) 0. 287

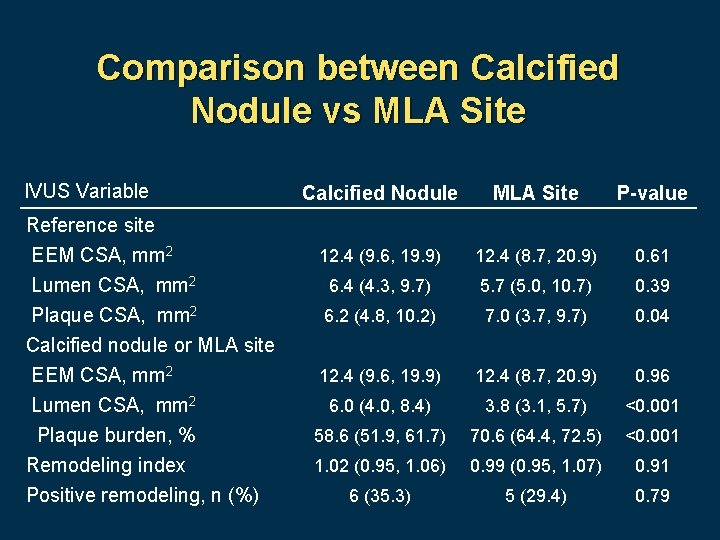
Comparison between Calcified Nodule vs MLA Site IVUS Variable Reference site EEM CSA, mm 2 Lumen CSA, mm 2 Plaque CSA, mm 2 Calcified nodule or MLA site EEM CSA, mm 2 Lumen CSA, mm 2 Plaque burden, % Remodeling index Positive remodeling, n (%) Calcified Nodule MLA Site P-value 12. 4 (9. 6, 19. 9) 12. 4 (8. 7, 20. 9) 0. 61 6. 4 (4. 3, 9. 7) 5. 7 (5. 0, 10. 7) 0. 39 6. 2 (4. 8, 10. 2) 7. 0 (3. 7, 9. 7) 0. 04 12. 4 (9. 6, 19. 9) 12. 4 (8. 7, 20. 9) 0. 96 6. 0 (4. 0, 8. 4) 3. 8 (3. 1, 5. 7) <0. 001 58. 6 (51. 9, 61. 7) 70. 6 (64. 4, 72. 5) <0. 001 1. 02 (0. 95, 1. 06) 0. 99 (0. 95, 1. 07) 0. 91 6 (35. 3) 5 (29. 4) 0. 79

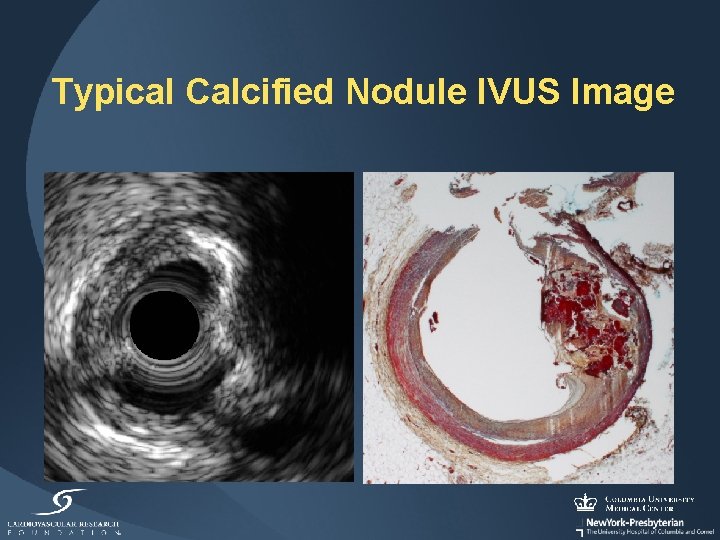
Typical Calcified Nodule IVUS Image

The PROSPECT Trial 700 pts with ACS UA (with ECGΔ) or NSTEMI or STEMI >24º undergoing PCI of 1 or 2 major coronary arteries at up to 40 sites in the U. S. and Europe Metabolic S. • Waist circum • Fast lipids • Fast glu • Hgb. A 1 C • Fast insulin • Creatinine PCI of culprit lesion(s) Successful and uncomplicated Formally enrolled PI: Gregg W. Stone Sponsor: Abbott Vascular; Partner: Volcano Biomarkers • Hs CRP • IL-6 • s. CD 40 L • MPO • TNFα • MMP 9 • Lp-PLA 2 • others

Virtual histology lesion classification Lesions are classified into 5 main types 1. Fibrotic 2. Fibrocalcific 3. Pathological intimal thickening (PIT) 4. Thick cap fibroatheroma (Th. CFA) 5. VH-thin cap fibroatheroma (VH-TCFA)

Frequency of calcified nodules • Among 623 patients with 1573 vessels imaged and qualified for analysis, a total of 314 calcified nodules were detected in 250 arteries in 185 patients. • Thus, the prevalence of at least one calcified nodule was 16% per artery (250 of 1573) and 30% per patient (185 of 623). • Two or more calcified nodules were detected in 48 coronary arteries (3%) in 76 patients (12%).

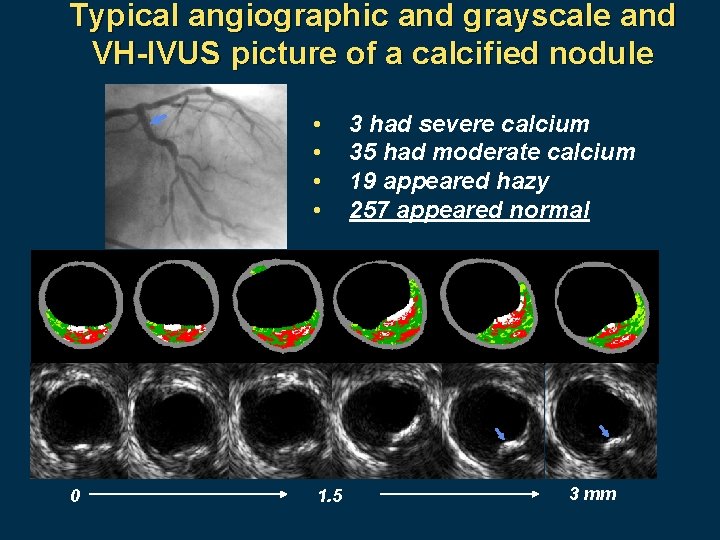
Qualitative grayscale IVUS findings of calcified nodules • The arc of nodular calcium measured 33. 6± 11. 7 degrees. • 91% were superficial and 9% were mixed, but none was only deep. • In 33% of calcified nodules (105/314) there was a branch near the calcified nodule site. The distance between the calcified nodule site and the branch measured 3. 0 ± 0. 8 mm.

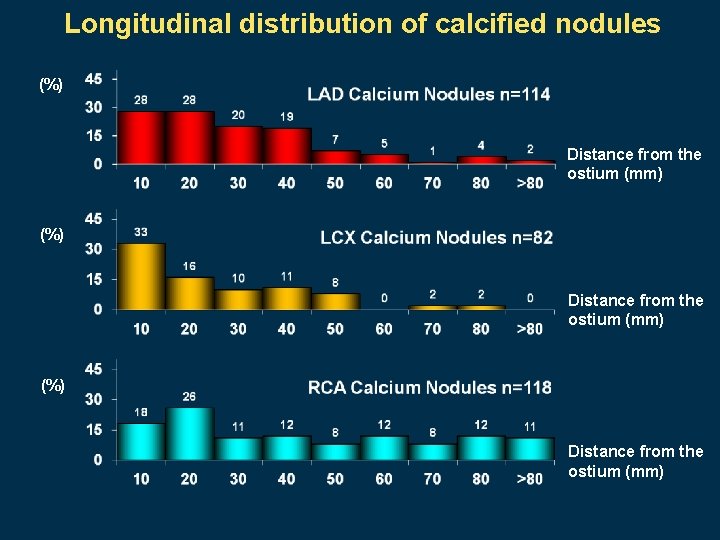
Longitudinal distribution of calcified nodules (%) Distance from the ostium (mm)

Typical angiographic and grayscale and VH-IVUS picture of a calcified nodule • • 0 1. 5 3 had severe calcium 35 had moderate calcium 19 appeared hazy 257 appeared normal 3 mm

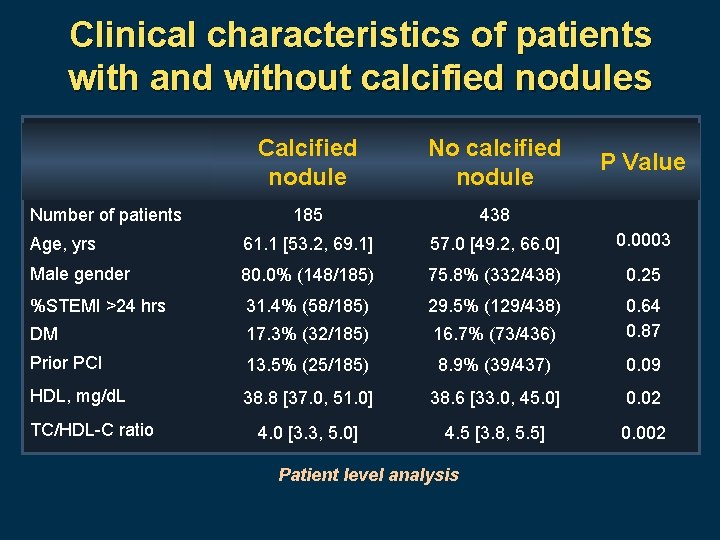
Clinical characteristics of patients with and without calcified nodules Calcified nodule No calcified nodule 185 438 Age, yrs 61. 1 [53. 2, 69. 1] 57. 0 [49. 2, 66. 0] 0. 0003 Male gender 80. 0% (148/185) 75. 8% (332/438) 0. 25 %STEMI >24 hrs 31. 4% (58/185) 29. 5% (129/438) DM 17. 3% (32/185) 16. 7% (73/436) 0. 64 0. 87 Prior PCI 13. 5% (25/185) 8. 9% (39/437) 0. 09 HDL, mg/d. L 38. 8 [37. 0, 51. 0] 38. 6 [33. 0, 45. 0] 0. 02 4. 0 [3. 3, 5. 0] 4. 5 [3. 8, 5. 5] 0. 002 Number of patients TC/HDL-C ratio Patient level analysis P Value

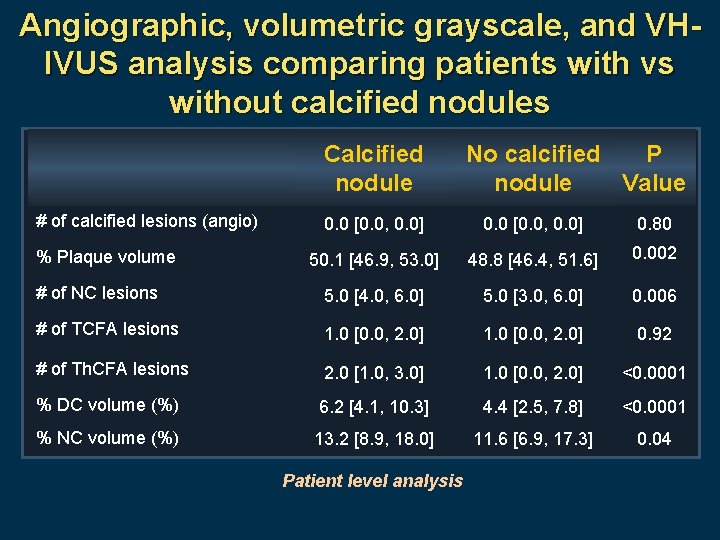
Angiographic, volumetric grayscale, and VHIVUS analysis comparing patients with vs without calcified nodules Calcified nodule # of calcified lesions (angio) No calcified P nodule Value 0. 0 [0. 0, 0. 0] 0. 80 50. 1 [46. 9, 53. 0] 48. 8 [46. 4, 51. 6] 0. 002 # of NC lesions 5. 0 [4. 0, 6. 0] 5. 0 [3. 0, 6. 0] 0. 006 # of TCFA lesions 1. 0 [0. 0, 2. 0] 0. 92 # of Th. CFA lesions 2. 0 [1. 0, 3. 0] 1. 0 [0. 0, 2. 0] <0. 0001 % DC volume (%) 6. 2 [4. 1, 10. 3] 4. 4 [2. 5, 7. 8] <0. 0001 % NC volume (%) 13. 2 [8. 9, 18. 0] 11. 6 [6. 9, 17. 3] 0. 04 % Plaque volume Patient level analysis

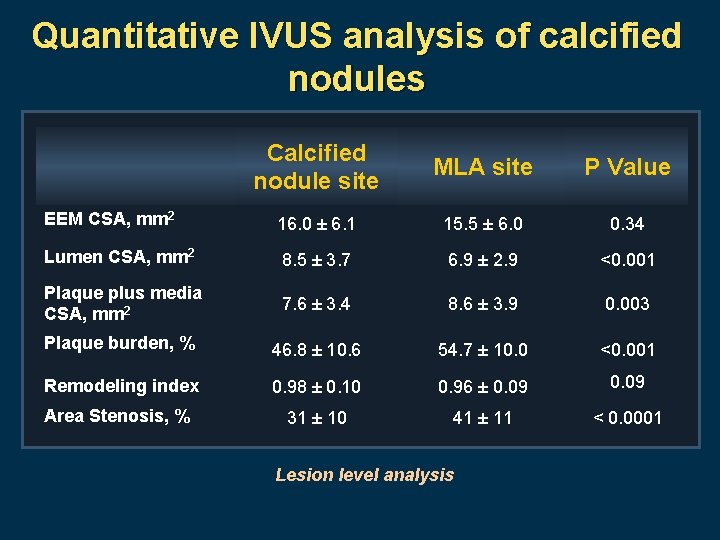
Quantitative IVUS analysis of calcified nodules Calcified nodule site MLA site P Value EEM CSA, mm 2 16. 0 ± 6. 1 15. 5 ± 6. 0 0. 34 Lumen CSA, mm 2 8. 5 ± 3. 7 6. 9 ± 2. 9 <0. 001 Plaque plus media CSA, mm 2 7. 6 ± 3. 4 8. 6 ± 3. 9 0. 003 Plaque burden, % 46. 8 ± 10. 6 54. 7 ± 10. 0 <0. 001 Remodeling index 0. 98 ± 0. 10 0. 96 ± 0. 09 Area Stenosis, % 31 ± 10 41 ± 11 < 0. 0001 Lesion level analysis

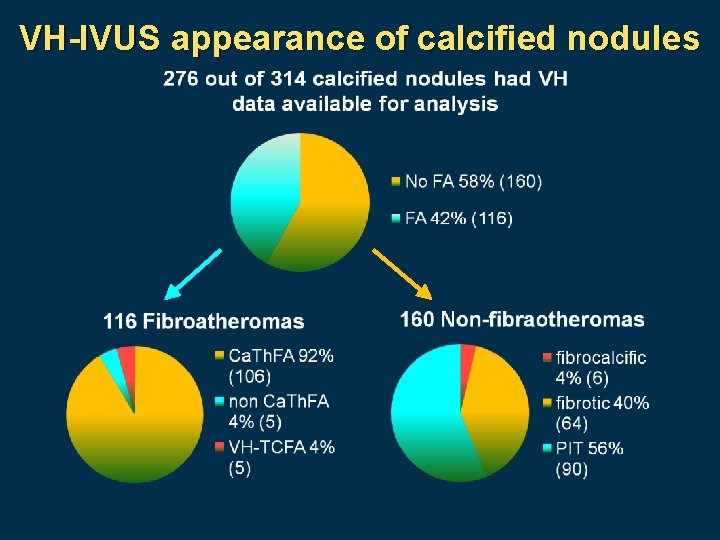
VH-IVUS appearance of calcified nodules

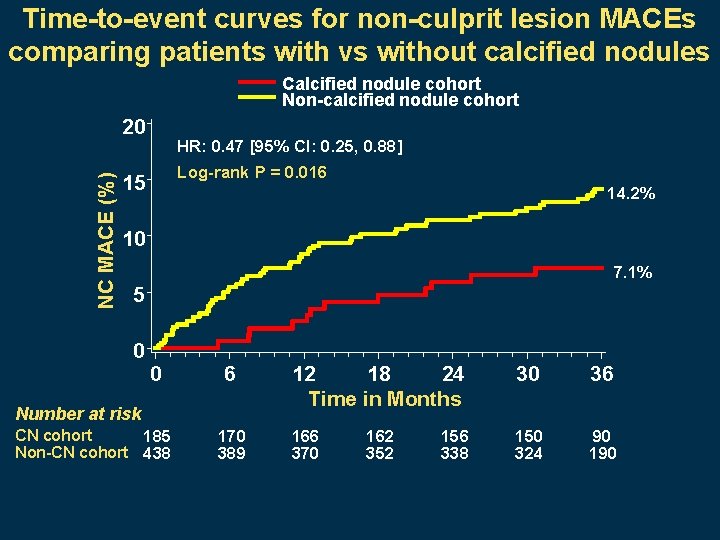
Time-to-event curves for non-culprit lesion MACEs comparing patients with vs without calcified nodules Calcified nodule cohort Non-calcified nodule cohort NC MACE (%) 20 HR: 0. 47 [95% CI: 0. 25, 0. 88] Log-rank P = 0. 016 15 14. 2% 10 7. 1% 5 0 0 6 Number at risk CN cohort 185 Non-CN cohort 438 170 389 12 18 24 Time in Months 30 36 166 370 150 324 90 162 352 156 338

Take Home Message • Calcified nodule appears a typical pattern by grayscale IVUS (convex shape, irregular surface) and can be identified accurately. • Calcified nodule is common (30% of patient). • Calcified nodule related to the older age and more advanced atherosclerosis. • The patients with calcified nodule has better clinical outcome. This indicates that calcium nodule detected by IVUS would be the result of sub-clinical (thrombotic? ) phenomenon, not a predictor of future event