Impact of Intravascular Ultrasound NIRS to Detect Vulnerable

Impact of Intravascular Ultrasound &NIRS to Detect Vulnerable Plaques : Insights from the Lipid-Rich Plaque (LRP) Study Ron Waksman, MD on behalf of the LRP Investigators Med. Star Washington Hospital Center

I, Ron Waksman, MD have the following disclosures: Advisory boards: Abbott Vascular, Amgen, Boston Scientific, Cardioset, Cardiovascular Systems Inc. , Medtronic, Philips Volcano, and Pi-Cardia Ltd. Consultant: Abbott Vascular, Amgen, Biosensors, Biotronik, Boston Scientific, Cardioset, Cardiovascular Systems Inc. , Medtronic, Philips Volcano, Pi. Cardia Ltd. Grant support: Abbott Vascular, Astra. Zeneca, Biosensors, Biotronik, Boston Scientific, Chiesi Speakers bureaus: Astra. Zeneca and Chiesi Investor: Med. Alliance

Background • Plaque burden identified as the most predictive IVUSderived parameter to detect future events in the PROSPECT and the Athero. Remo-IVUS studies. • However, the low positive predictive value and practical implementation of this measure limit the clinical adoption. • The LRP study demonstrated that NIRS using max. LCBI 4 mm can detect future events in non culprit lesions. • The contribution of plaque burden by IVUS to improve the predictive ability of NIRS was a secondary endpoint in the LRP study.
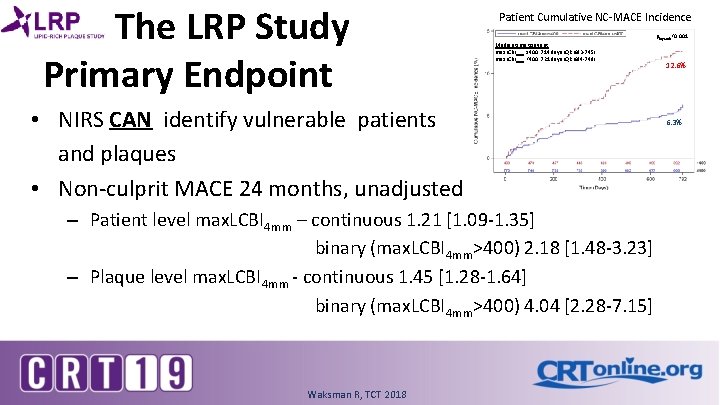
The LRP Study Primary Endpoint Patient Cumulative NC-MACE Incidence plogrank<0. 001 Median time to event max. LCBI 4 mm ≥ 400: 714 days IQR[683 -745] max. LCBI 4 mm <400: 721 days IQR[694 -748] • NIRS CAN identify vulnerable patients and plaques • Non-culprit MACE 24 months, unadjusted – Patient level max. LCBI 4 mm – continuous 1. 21 [1. 09 -1. 35] binary (max. LCBI 4 mm>400) 2. 18 [1. 48 -3. 23] – Plaque level max. LCBI 4 mm - continuous 1. 45 [1. 28 -1. 64] binary (max. LCBI 4 mm>400) 4. 04 [2. 28 -7. 15] Waksman R, TCT 2018 12. 6% 6. 3%

LRP IVUS Sub-analysis Study Aim What is the impact of intravascular ultrasound derived lesion features on non-culprit MACE in the context of the detection of vulnerable plaque by NIRS-IVUS during a 24 -month period?

LRP Study: IVUS Endpoints Pre-specified secondary hypotheses for the vulnerable-plaque level analysis: • Plaque burden >70% by grayscale IVUS plus a max. LCBI 4 mm>400 in a coronary artery segment will be a stronger predictor of risk that max. LCBI 4 mm>400 alone *Non-culprit MACE (independently adjudicated by CEC blinded to NIRS) • Cardiac death • Cardiac arrest • Non-fatal myocardial infarction • Acute coronary syndrome • Revascularization by CABG or PCI • Rehospitalization for progressive angina with >20% stenosis progression
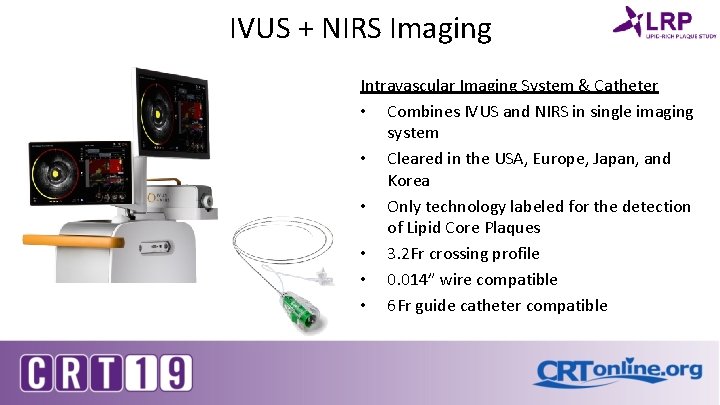
IVUS + NIRS Imaging *Device used in trial was previous model TVC MC 8, Model TVC-MC 10 shown. Intravascular Imaging System & Catheter • Combines IVUS and NIRS in single imaging system • Cleared in the USA, Europe, Japan, and Korea • Only technology labeled for the detection of Lipid Core Plaques • 3. 2 Fr crossing profile • 0. 014” wire compatible • 6 Fr guide catheter compatible
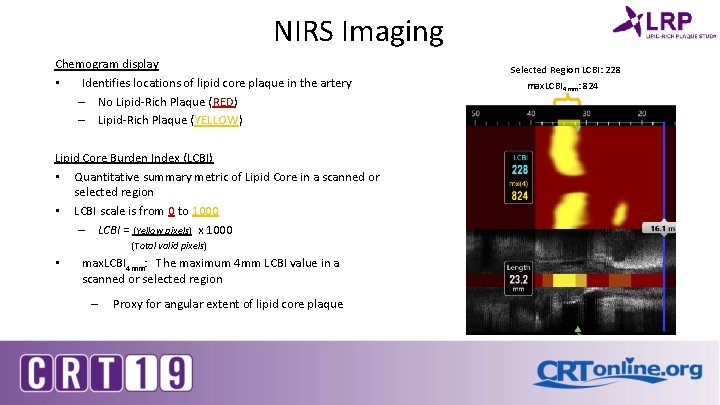
NIRS Imaging Chemogram display • Identifies locations of lipid core plaque in the artery – No Lipid-Rich Plaque (RED) – Lipid-Rich Plaque (YELLOW) Lipid Core Burden Index (LCBI) • Quantitative summary metric of Lipid Core in a scanned or selected region • LCBI scale is from 0 to 1000 – LCBI = (Yellow pixels) x 1000 (Total valid pixels) • max. LCBI 4 mm: The maximum 4 mm LCBI value in a scanned or selected region – Proxy for angular extent of lipid core plaque Selected Region LCBI: 228 max. LCBI 4 mm: 824

Statistical Methodology • Co-primary endpoints assessed max. LCBI 4 mm as a continuous variable using timeto-event Cox proportional hazard models • Key secondary endpoints assessed with the max. LCBI 4 mm dichotomized at 400 • Vulnerable Plaque-Level – Evaluation was conditional on the Patient-Level being met – Max. LCBI 4 mm was computed in each eligible Ware segments – NC-MACE evaluated only in corresponding segments where imaging occurred
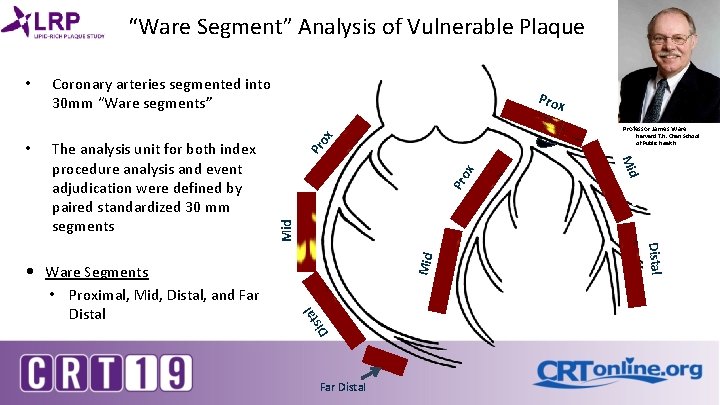
“Ware Segment” Analysis of Vulnerable Plaque • Coronary arteries segmented into 30 mm “Ware segments” Pro x Professor James Ware ox Pro x Pr st Di Distal al • Ware Segments • Proximal, Mid, Distal, and Far Distal Mid The analysis unit for both index procedure analysis and event adjudication were defined by paired standardized 30 mm segments Mid • Harvard T. H. Chan School of Public Health

IVUS Defined Variables • • • Cross-sectional images spaced precisely 1 mm apart were selected for measurement within the max. LCBI 4 mm segment The lumen and external elastic membrane (EEM) were traced by manual planimetry Minimum lumen area (MLA) – Defined as the MLA within the max. LCBI 4 mm segment • Plaque area – The area occupied between the lumen and external elastic membrane (EEM) • Plaque Burden – EEM area−Lumen area × 100 EEM area
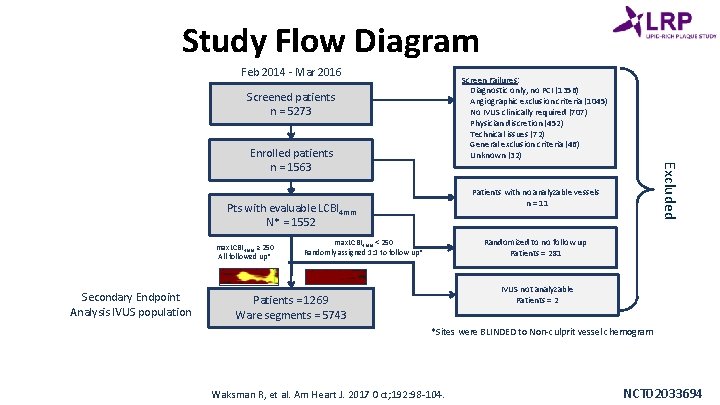
Study Flow Diagram Feb 2014 - Mar 2016 Screen Failures: Diagnostic only, no PCI (1356) Angiographic exclusion criteria (1045) No IVUS clinically required (707) Physician discretion (452) Technical issues (72) General exclusion criteria (46) Unknown (32) Screened patients n = 5273 Patients with no analyzable vessels n = 11 Pts with evaluable LCBI 4 mm N* = 1552 max. LCBI 4 mm ≥ 250 All followed up* Secondary Endpoint Analysis IVUS population Excluded Enrolled patients n = 1563 Randomized to no follow up Patients = 281 max. LCBI 4 mm < 250 Randomly assigned 1: 1 to follow up* IVUS not analyzable Patients = 2 Patients = 1269 Ware segments = 5743 *Sites were BLINDED to Non-culprit vessel chemogram Waksman R, et al. Am Heart J. 2017 Oct; 192: 98 -104. NCT 02033694
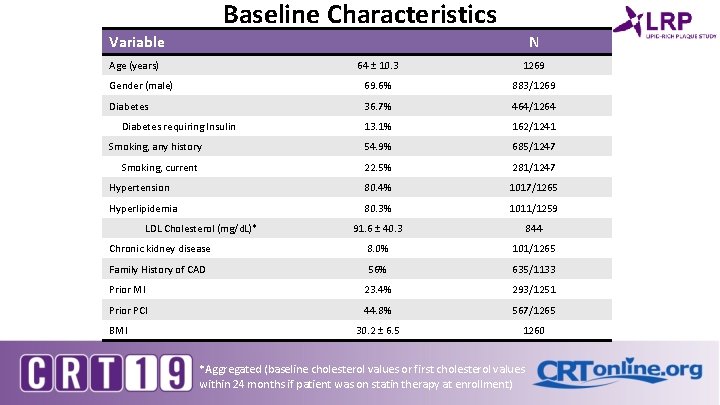
Baseline Characteristics Variable N Age (years) 64 ± 10. 3 1269 Gender (male) 69. 6% 883/1269 Diabetes 36. 7% 464/1264 13. 1% 162/1241 54. 9% 685/1247 22. 5% 281/1247 Hypertension 80. 4% 1017/1265 Hyperlipidemia 80. 3% 1011/1259 91. 6 ± 40. 3 844 Chronic kidney disease 8. 0% 101/1265 Family History of CAD 56% 635/1133 Prior MI 23. 4% 293/1251 Prior PCI 44. 8% 567/1265 30. 2 ± 6. 5 1260 Diabetes requiring Insulin Smoking, any history Smoking, current LDL Cholesterol (mg/d. L)* BMI *Aggregated (baseline cholesterol values or first cholesterol values within 24 months if patient was on statin therapy at enrollment)
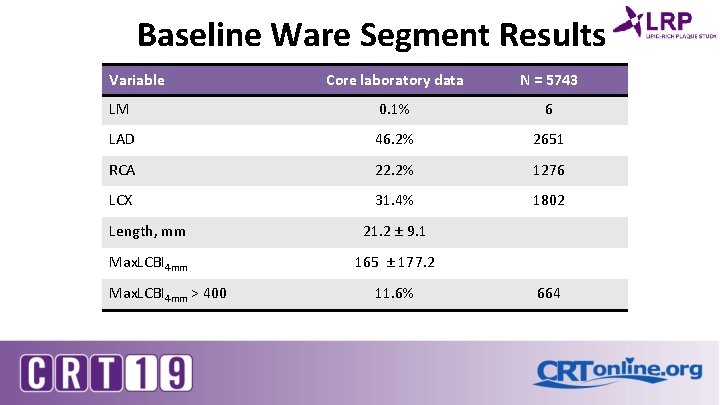
Baseline Ware Segment Results Variable Core laboratory data N = 5743 LM 0. 1% 6 LAD 46. 2% 2651 RCA 22. 2% 1276 LCX 31. 4% 1802 Length, mm 21. 2 ± 9. 1 Max. LCBI 4 mm 165 ± 177. 2 Max. LCBI 4 mm > 400 11. 6% 664
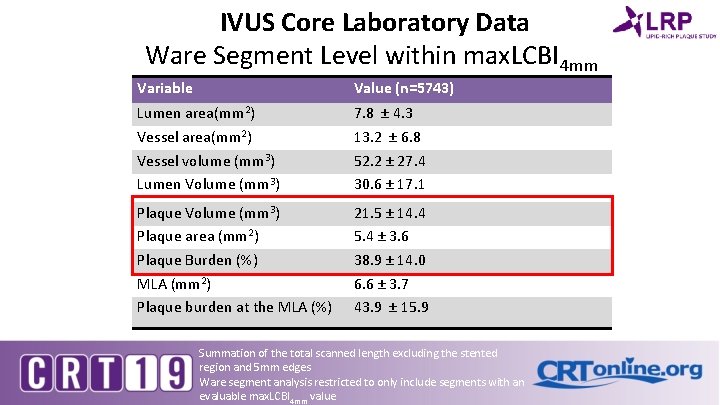
IVUS Core Laboratory Data Ware Segment Level within max. LCBI 4 mm Variable Value (n=5743) Lumen area(mm 2) Vessel volume (mm 3) Lumen Volume (mm 3) 7. 8 ± 4. 3 13. 2 ± 6. 8 52. 2 ± 27. 4 30. 6 ± 17. 1 Plaque Volume (mm 3) Plaque area (mm 2) Plaque Burden (%) MLA (mm 2) Plaque burden at the MLA (%) 21. 5 ± 14. 4 5. 4 ± 3. 6 38. 9 ± 14. 0 6. 6 ± 3. 7 43. 9 ± 15. 9 Summation of the total scanned length excluding the stented region and 5 mm edges Ware segment analysis restricted to only include segments with an evaluable max. LCBI 4 mm value

IVUS Endpoint Vulnerable Plaque Level Cox Proportional Hazards Models 00 Variable max. LCBI 4 mm continuous Hazard Ratio [95% CI] max. LCBI 4 mm > 400 Unadjusted LCBI alone max. LCBI 4 mm 1. 45 [1. 28 -1. 64] 4. 04 [2. 28 -7. 15] Multivariable-Adjusted Model max. LCBI 4 mm >400 3. 46 [1. 89 -6. 35] Plaque burden within max. LCBI 4 mm ≥ 70% 3. 99 [1. 37 -11. 61] MLA within max. LCBI 4 mm ≤ 4 mm² 1. 84 [1. 04 -3. 26]
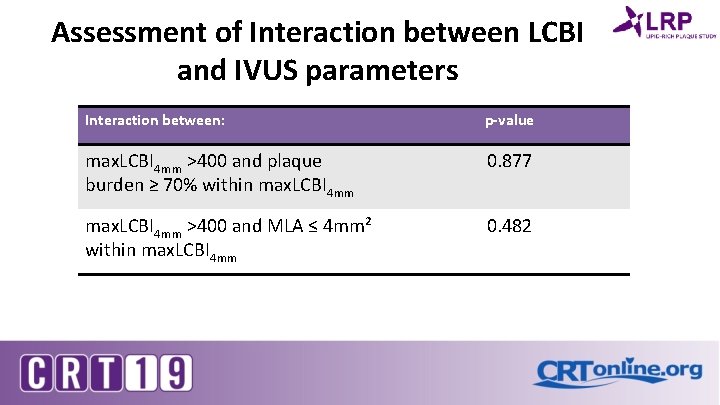

Assessment of Interaction between LCBI and IVUS parameters Interaction between: p-value max. LCBI 4 mm >400 and plaque burden ≥ 70% within max. LCBI 4 mm 0. 877 max. LCBI 4 mm >400 and MLA ≤ 4 mm² within max. LCBI 4 mm 0. 482

IVUS Summary • When adjusted for plaque burden ≥ 70% and MLA ≤ 4 mm² by IVUS at the site of max. LCBI 4 mm the adjusted hazard ratio for max. LCBI 4 mm greater than 400 was 3. 46 (95% CI [1. 89– 6. 35], p < 0. 001) and remained statistically significant. • There was no interaction between the max. LCBI 4 mm and plaque burden or MLA within max. LCBI 4 mm by IVUS.
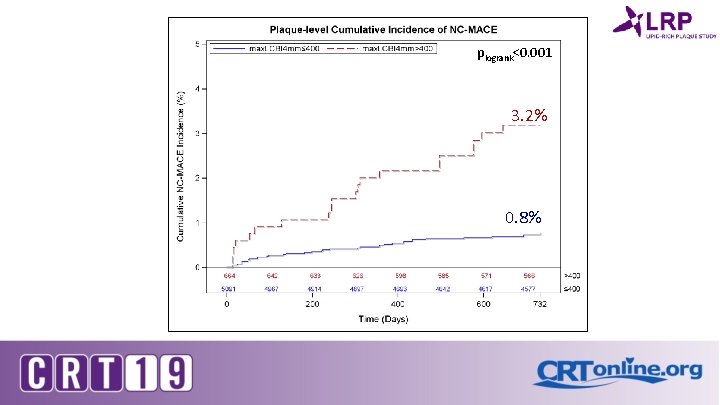
plogrank<0. 001 3. 2% 0. 8%

Discussion • The ability of NIRS to detect the plaques with lipid-rich cores is more powerful than plaque burden since some of the lesions with plaque burden have a low LCBI. • In the LRP study, the number of patients with plaque burden ≥ 70% was smaller than PROSPECT, which had an entry criterion of at least ≥ 40% plaque burden at baseline for each lesion with the mandatory 3 vessel imaging. • In the LRP study, all arteries were scanned irrespective to the presence of plaque burden. This may explain the lack of interaction between the NIRS and plaque burden in the LRP study.
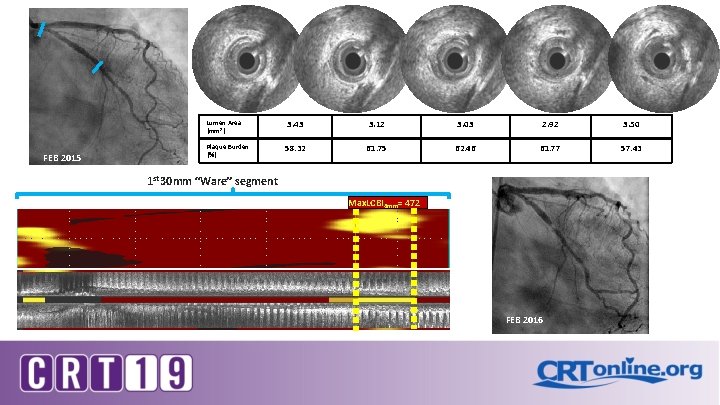
Lumen Area (mm 2) FEB 2015 Plaque Burden (%) 3. 43 3. 12 3. 03 2. 92 3. 50 58. 32 61. 75 62. 46 61. 77 57. 43 1 st 30 mm “Ware” segment Max. LCBI 4 mm= 472 FEB 2016
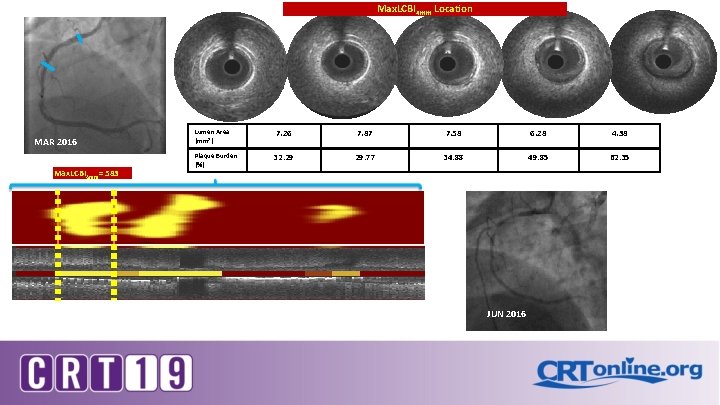
Max. LCBI 4 mm Location MAR 2016 Max. LCBI 4 mm= 583 Lumen Area (mm 2) Plaque Burden (%) 7. 26 7. 87 7. 58 6. 28 4. 38 32. 29 29. 77 34. 88 49. 85 62. 35 JUN 2016

Conclusion • NIRS-IVUS imaging in non-obstructive coronary arteries can identify non-culprit segments in the coronary arteries at high-risk for future events. • The addition of plaque burden ≥ 70% did not alter the hazard ratio or have an interaction with max. LCBI 4 mm > 400. • NIRS’s ability to predict plaques vulnerable to events appears to be independent of IVUS plaque burden or MLA within the site of max. LCBI 4 mm.

§ § § § § § LRP Study Sites Northwell Health - Dr. Varinder Singh Columbia University Medical Center - Dr. Ziad Ali Baptist Health Lexington - Dr. William Skinner Methodist Hospitals - Dr. Andre Artis Radboud University Medical Center - Dr. Tim ten Cate Medical University of South Carolina Hospital - Dr. Eric Powers Davis Hospital and Medical Center - Dr. Christopher Kim Erasmus Medical Center - Dr. Evelyn Regar New York Presbyterian Hospital - Cornell - Dr. Shing Chiu-Wong Charleston Area Medical Center - Dr. Stephen Lewis Academic Medical Center - Dr. Joanna Wykrzykowska Medstar Washington Hospital Center - Dr. Ron Waksman Community Heart and Vascular Hospital - Dr. Sandeep Dube The Shelton Heart Center at Crittenton Hospital - Dr. Samer Kazziha Maasstad Hospital - Dr. Martin van der Ent St. John's Hospital - Dr. Nilesh Goswami University of Edinburgh - Dr. David Newby Palmetto General Hospital - Dr. Miguel Diaz St. Luke's Medical Center - Dr. George Younis Royal Brompton Hospital - Dr. Carlo Di Mario Emory University Hospital Midtown - Dr. Henry Liberman § § § § § (In order of enrollments) Emory University Hospital - Dr. Habib Samady Metro Health Hospital - Dr. John Hodgson JFK Medical Center - Dr. Lawrence Lovitz Hillcrest Oklahoma Heart Institute - Dr. Wayne Leimbach University of Minnesota Medical Center - Dr. Ganesh Raveendran SUSCCH, a. s. - Dr. Martin Hudec Heart Hospital Baylor Plano - Dr. Srinivasa Potluri Palm Beach Gardens Medical Center - Dr. Augusto Villa Florida Hospital Orlando - Dr. Jose Arias Delray Medical Center - Dr. Robert Carida San Giovanni Addolorata Hospital - Dr. Francesco Prati Latvian Centre of Cardiology - Dr. Andrejs Ērglis Mc. Laren Bay Region - Dr. Daniel Lee St. John Detroit - Dr. Thomas La. Londe Alexian Brothers Heart and Vascular Institute - Dr. Andrei Pop University of Texas Galveston - Dr. Umamahesh Rangasetty University of California Los Angeles Medical Center - Dr. J. Tobis Memorial Hospital West - Dr. Luis Tami Mc. Laren Macomb - Dr. Mark Zainea Golden Jubilee National Hospital - Dr. Margaret Mc. Entegart
- Slides: 24