Heelkundige en Medicamenteuze Fertiliteitssparende Behandeling in de Gynaecologische

Heelkundige en Medicamenteuze Fertiliteitssparende Behandeling in de Gynaecologische oncologie Ignace Vergote, MD Ph. D FACS Voorzitter Leuvens Kanker Instituut (LKI) Diensthoofd Gynaecologie-Verloskunde Universitaire Ziekenhuizen Leuven

FER sparend in gyn oncologie • Cervix - Conisatie Trachelectomie Portioamputatie Neoadjuvante chemotherapie + Conisatie • Ovarium - Borderline - Invasieve epitheliale tumoren - Niet-epitheliale tumoren • Endometriumcarcinoom
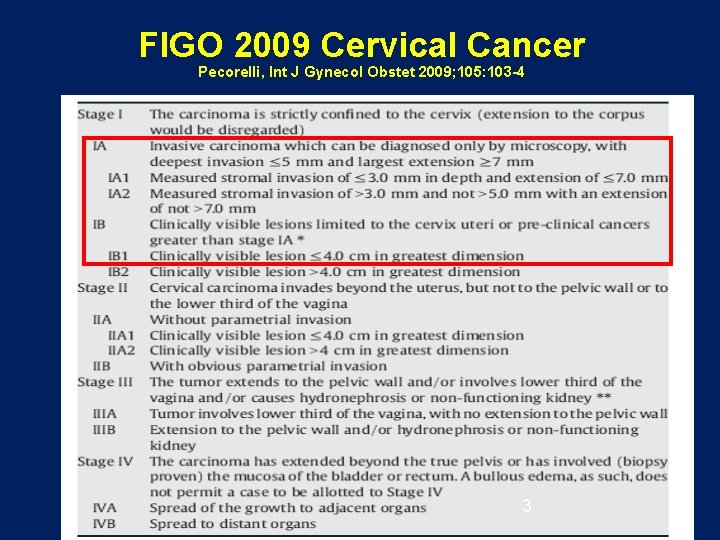
FIGO 2009 Cervical Cancer Pecorelli, Int J Gynecol Obstet 2009; 105: 103 -4 3
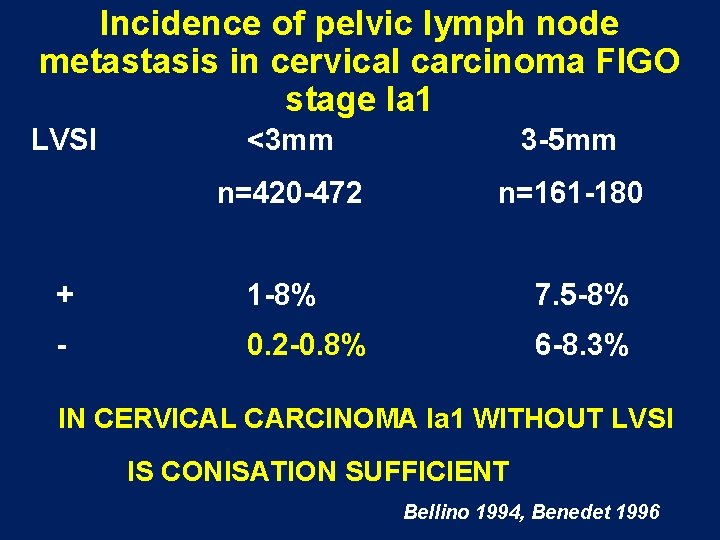
Incidence of pelvic lymph node metastasis in cervical carcinoma FIGO stage Ia 1 LVSI <3 mm 3 -5 mm n=420 -472 n=161 -180 + 1 -8% - 0. 2 -0. 8% 7. 5 -8% 6 -8. 3% IN CERVICAL CARCINOMA Ia 1 WITHOUT LVSI IS CONISATION SUFFICIENT Bellino 1994, Benedet 1996

Selection Criteria for Fertility Preserving Therapy in cervical cancer Ia 2 - IB 1 PATIENTS’ CRITERIA 1. Strong desire to preserve fertility 2. Age limit ? (less than 35, 40, 45? ) TUMOR CRITERIA 1. Tumor size (expert colposcopy / volume – NMR) 2. Preoperative biopsy (exclude neuroendocrine ca), LVSI, VSI LVSI, lymphovascular space involvement
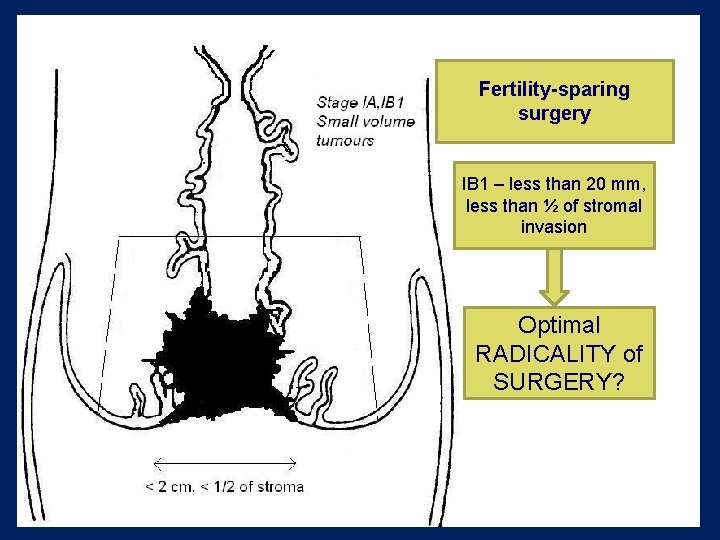
Fertility-sparing surgery IB 1 – less than 20 mm, less than ½ of stromal invasion Optimal RADICALITY of SURGERY?
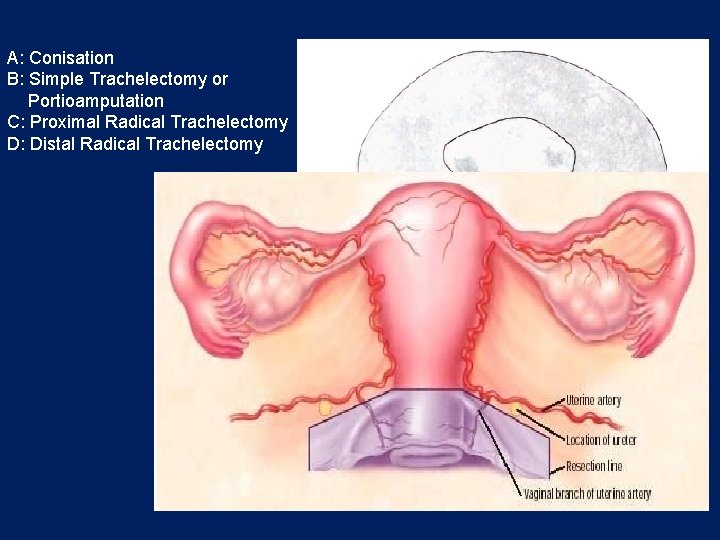
A: Conisation B: Simple Trachelectomy or Portioamputation C: Proximal Radical Trachelectomy D: Distal Radical Trachelectomy
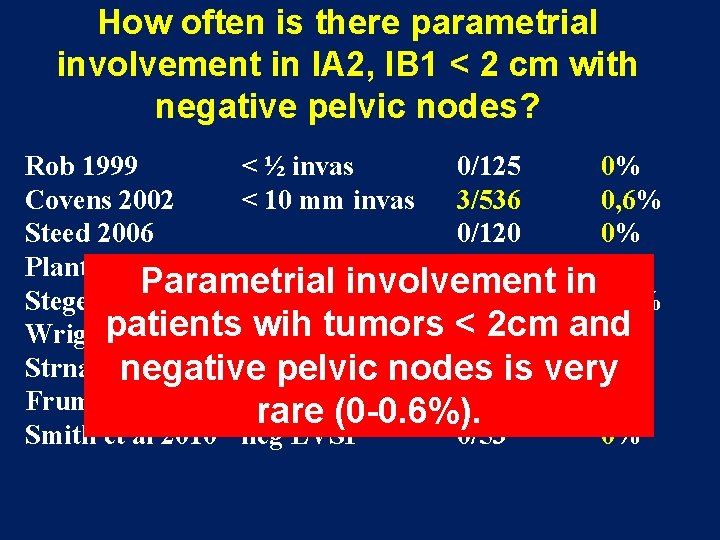
How often is there parametrial involvement in IA 2, IB 1 < 2 cm with negative pelvic nodes? Rob 1999 < ½ invas 0/125 0% Covens 2002 < 10 mm invas 3/536 0, 6% Steed 2006 0/120 0% Plante 2006 0/76 0% Parametrial involvement in Stegeman 2007 < 10 mm invas 5/799 0. 6% Wrightpatients wih tumors < 2 cm and 2007 neg LVSI Strnad 2008 0/133 0% negative pelvic nodes is very Frumovitz 2009 neg LVSI 0/125 0% rare (0 -0. 6%). Smith et al 2010 neg LVSI 0/53 0%
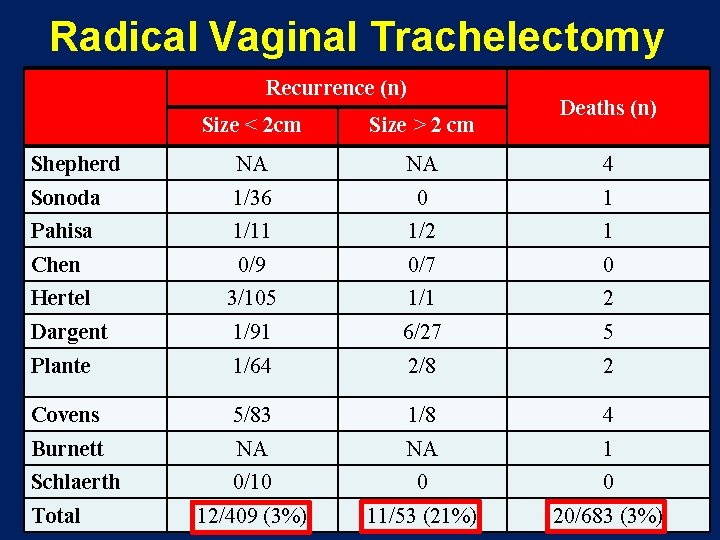
Radical Vaginal Trachelectomy Recurrence (n) Deaths (n) Size < 2 cm Size > 2 cm Shepherd NA NA 4 Sonoda 1/36 0 1 Pahisa 1/11 1/2 1 Chen 0/9 0/7 0 Hertel 3/105 1/1 2 Dargent 1/91 6/27 5 Plante 1/64 2/8 2 Covens 5/83 1/8 4 Burnett NA NA 1 Schlaerth 0/10 0 0 12/409 (3%) 11/53 (21%) 20/683 (3%) Total
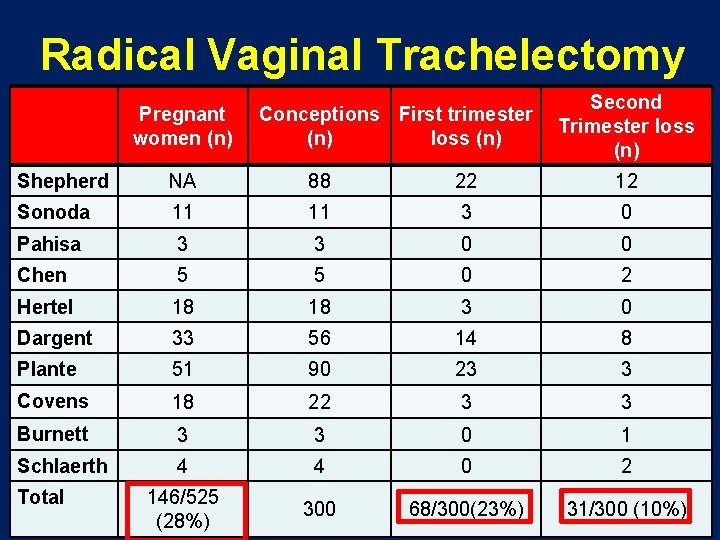
Radical Vaginal Trachelectomy Pregnant women (n) Second Conceptions First trimester Trimester loss (n) (n) Shepherd NA 88 22 12 Sonoda 11 11 3 0 Pahisa 3 3 0 0 Chen 5 5 0 2 Hertel 18 18 3 0 Dargent 33 56 14 8 Plante 51 90 23 3 Covens 18 22 3 3 Burnett 3 3 0 1 Schlaerth 4 4 0 2 146/525 (28%) 300 68/300(23%) 31/300 (10%) Total

Radical Vaginal Trachelectomy Delivery (n) Ongoing pregnancy Term Pregnancy loss or Shepherd 10 35 NA 7 delivery before 32 Sonoda 0 0 4 4 Pahisa 0 0 1 2 weeks in 44% of the Chen 0 1 1 1 Hertel 12 NA NA 3 patients! Dargent 5 NA 29 NA Before week 32 Weeks 3236 Plante 4 9 51 NA Covens 3 3 12 NA Burnett 0 0 2 NA Schlaerth 0 1 1 NA 34/300 (11%) 49 101 17 Total
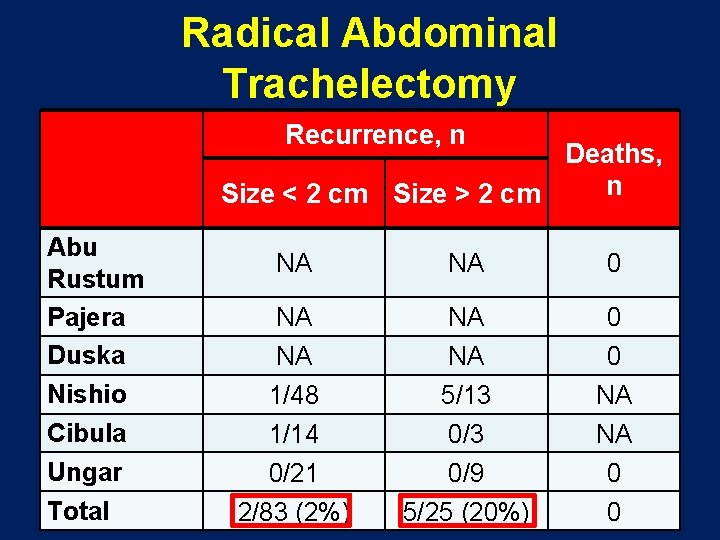
Radical Abdominal Trachelectomy Recurrence, n Deaths, n Size < 2 cm Size > 2 cm Abu Rustum Pajera Duska Nishio Cibula Ungar Total NA NA 0 NA NA 1/48 1/14 0/21 2/83 (2%) NA NA 5/13 0/9 5/25 (20%) 0 0 NA NA 0 0
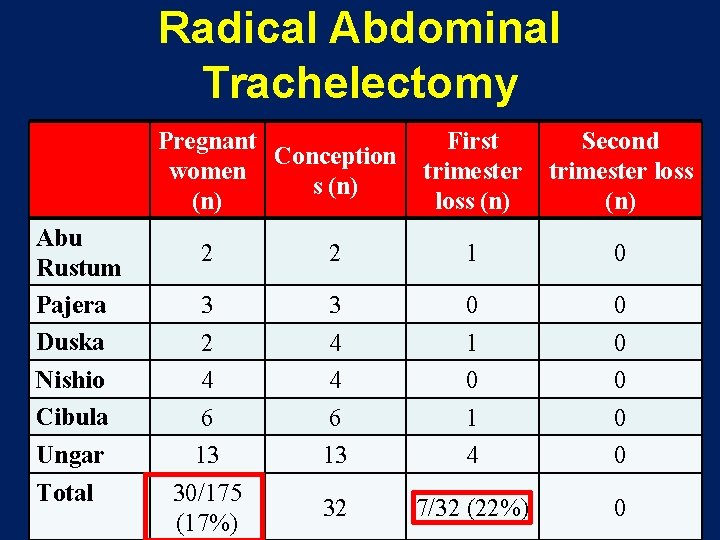
Radical Abdominal Trachelectomy Pregnant Conception women s (n) Abu Rustum Pajera Duska First trimester loss (n) Second trimester loss (n) 2 2 1 0 3 2 3 4 0 1 0 0 Nishio 4 4 0 0 Cibula 6 6 1 0 Ungar 13 30/175 (17%) 13 4 0 32 7/32 (22%) 0 Total

Radical Abdominal Trachelectomy Delivery, n Abu Rustum Pajera Duska Nishio Cibula Ungar Total Ongoing pregnancy Before week 32 Weeks 32 -36 Term 0 1 5 3 5/32 (16%) 2/32 13/32 5/32 Pregnancy loss or 0 0 0 1 delivery before 32 1 0 2 0 0 1 1 1 weeks in 38% of the 2 0 patients! 2 0 3 0
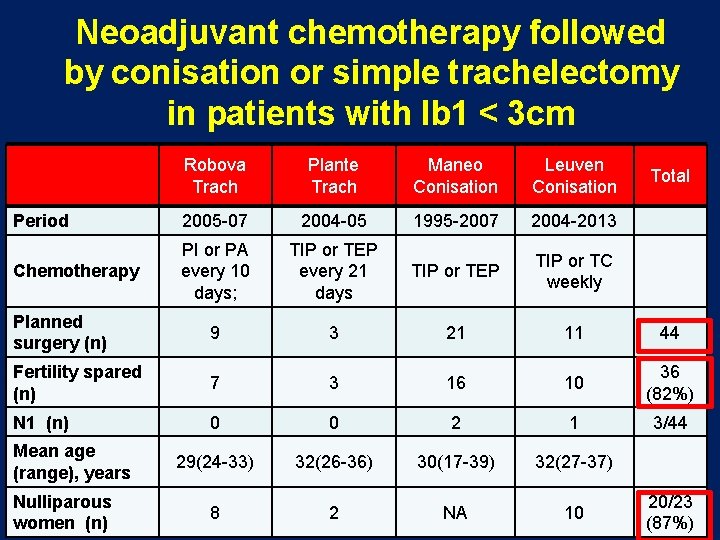
Neoadjuvant chemotherapy followed by conisation or simple trachelectomy in patients with Ib 1 < 3 cm Robova Trach Plante Trach Maneo Conisation Leuven Conisation Period 2005 -07 2004 -05 1995 -2007 2004 -2013 Chemotherapy PI or PA every 10 days; TIP or TEP every 21 days TIP or TEP TIP or TC weekly Planned surgery (n) 9 3 21 11 44 Fertility spared (n) 7 3 16 10 36 (82%) N 1 (n) 0 0 2 1 3/44 29(24 -33) 32(26 -36) 30(17 -39) 32(27 -37) 8 2 NA 10 Mean age (range), years Nulliparous women (n) Total 20/23 (87%)
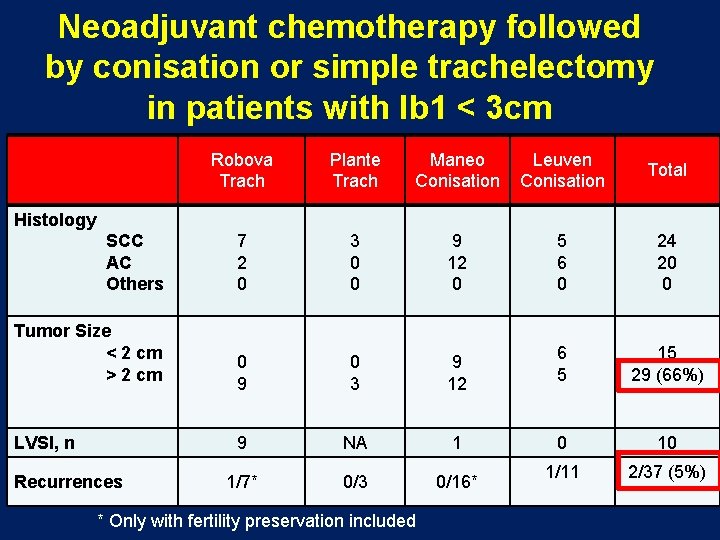
Neoadjuvant chemotherapy followed by conisation or simple trachelectomy in patients with Ib 1 < 3 cm Robova Trach Plante Trach Maneo Conisation Leuven Conisation Total 7 2 0 3 0 0 9 12 0 5 6 0 24 20 0 0 9 0 3 9 12 6 5 15 29 (66%) 9 NA 1 0 10 1/7* 0/3 0/16* 1/11 2/37 (5%) Histology SCC AC Others Tumor Size < 2 cm > 2 cm LVSI, n Recurrences * Only with fertility preservation included

Neoadjuvant chemotherapy followed by conisation or simple trachelectomy in patients with Ib 1 < 3 cm Robova Trach Pregnant women, n Plante Trach Maneo Cone Leuven Cone 5/9* 18/35 (51%) 6 24 1 2 (8%) 0 0 0 1 4 3 (12%) 2 16 0 1 Pregnancy loss or delivery before 32 weeks in 20% of the patients! Conceptions, n 1 st trimester loss, n 2 nd trimester loss, n Delivery Before week 32 Weeks 32 -36 Term Ongoing pregnancy, n 5/7* 2/3* 6/16* 5 3 10 0 0 1 0 3 0 1 2 2 0 7 1 NA NA * Only with fertility preservation included Total

Prague series: Simple Trachelectomy Cx ca Ia 2 and Ib 1 (< 2 cm) Less than 2 cm/less than ½ stromal invasion Ia 1 with LVSI (n= 3) , Ia 2 (n = 10), Ib 1 (n = 21) • All with negative pelvic lymph nodes • N = 34 , 32 fertility spared • One central recurrence • 23 pregancies (17 patients pregnant) • 5 first trimester and 3 second trimester losse Rob L Gynecol Oncol 2008

Simple conization and lymphadenectomy for Stage IB 1 Cx. Ca Maneo et al, Gynecol Oncol 2011 • N=36 • Median age is 31 (range, 24 -40) • Median tumor diameter is 11. 7 mm (median, 1825 mm) • LVSI 5% • Median FU is 66 months (range, 6 -168 months) • 1 nodal relapse • 21 pregnancies in 17 patients and 14 live babies Simple cone is according to these authors a feasible option in tumors < 20 mm with negative pelvic nodes.

Conclusions (1) Fertility sparing in cervical cancer Ia 2 -Ib 1 1. Patients should be very well selected: – Strong fertility wish – Ia 2 or Ib 1 (< 2 cm) or < 3 cm ( only with neoadjuvant chemotherapy). – Negative pelvic lymph nodes 2. Abdominal, vaginal and laparoscopic (robotic) trachelectomies are options, however in patients with Ia 2 with negative nodes these operations are an overtreatment. 3. In some series of radical trachelectomy up to 40% of the patients did not have residual tumor (after conisation).

Conclusions (2) Fertility sparing in cervical cancer Ia 1 -Ib 1 4. Radical trachelectomy resulted in a about 40% pregnancy loss or delivery before week 32. 5. In some patients a simple trachelectomy or wide conisation might suffice when tumor < 1 (? ) cm and negative nodes and: – no LVSI ? – < 10 mm invasion?

Conclusions (2) Fertility sparing in early cervical cancer. 6. Neoadjuvant chemotherapy followed by conisation seems to be a valuable alternative, especially in patients with larger tumors and/or LVSI. I personally prefer this option in all Ib 1 tumors because: 7. NACT and conisation resulted in a pregnancy loss or delivery before week 32 of only 20% 8. and more patients (51%) seem to conceive than after radical trachelectomy (25%). 9. Paclitaxel-Carboplatin weekly seems to be a very effective and well tolerated regimen.

Fertility sparing in « early » ovarian cancer
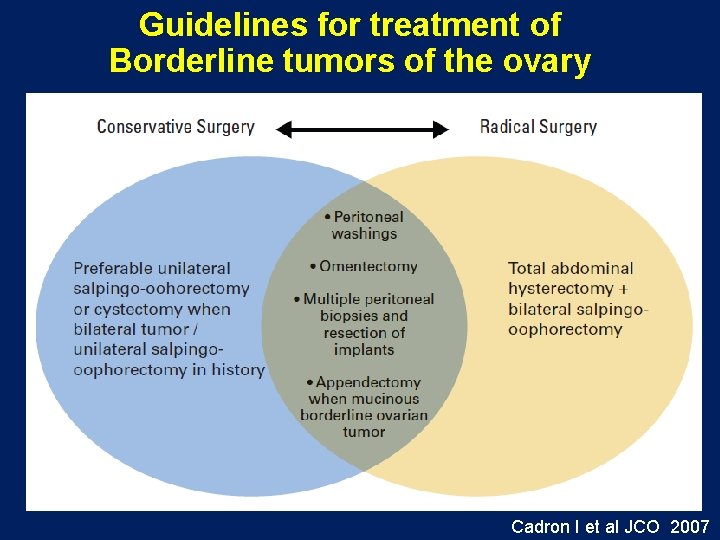
Guidelines for treatment of Borderline tumors of the ovary Cadron I et al JCO 2007
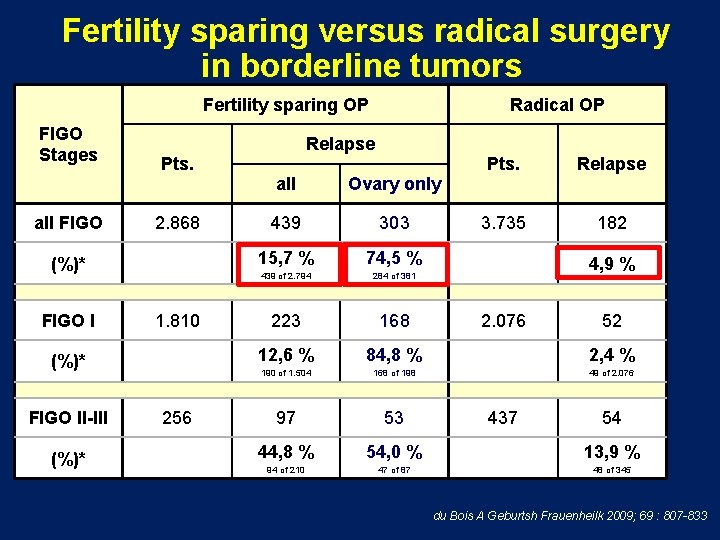
Fertility sparing versus radical surgery in borderline tumors Fertility sparing OP FIGO Stages all FIGO Pts. 2. 868 (%)* FIGO I 1. 810 (%)* FIGO II-III (%)* 256 Radical OP Relapse Pts. Relapse 3. 735 182 all Ovary only 439 303 15, 7 % 74, 5 % 439 of 2. 794 284 of 381 223 168 12, 6 % 84, 8 % 2, 4 % 190 of 1. 504 168 of 198 49 of 2. 076 97 53 44, 8 % 54, 0 % 13, 9 % 94 of 210 47 of 87 48 of 345 4, 9 % 2. 076 437 52 54 du Bois A Geburtsh Frauenheilk 2009; 69 : 807 -833
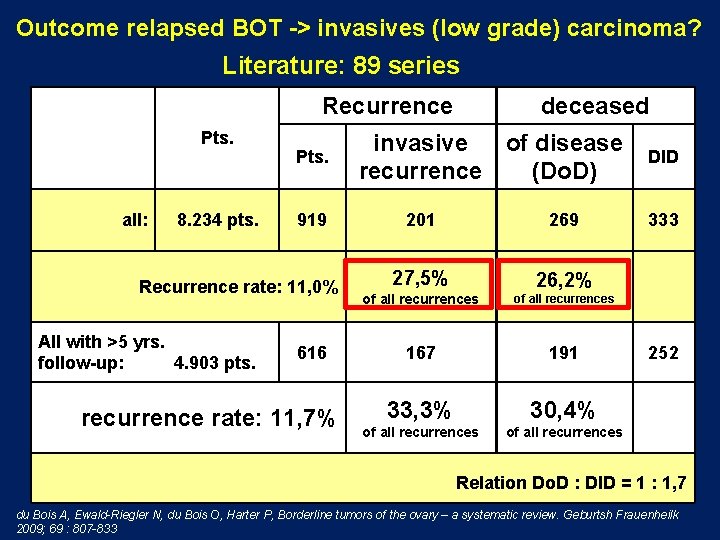
Outcome relapsed BOT -> invasives (low grade) carcinoma? Literature: 89 series Recurrence Pts. all: 8. 234 pts. Pts. 919 Recurrence rate: 11, 0% All with >5 yrs. follow-up: 4. 903 pts. 616 recurrence rate: 11, 7% deceased invasive of disease recurrence (Do. D) 201 269 27, 5% 26, 2% of all recurrences 167 191 33, 3% 30, 4% of all recurrences DID 333 252 Relation Do. D : DID = 1 : 1, 7 du Bois A, Ewald-Riegler N, du Bois O, Harter P, Borderline tumors of the ovary – a systematic review. Geburtsh Frauenheilk 2009; 69 : 807 -833
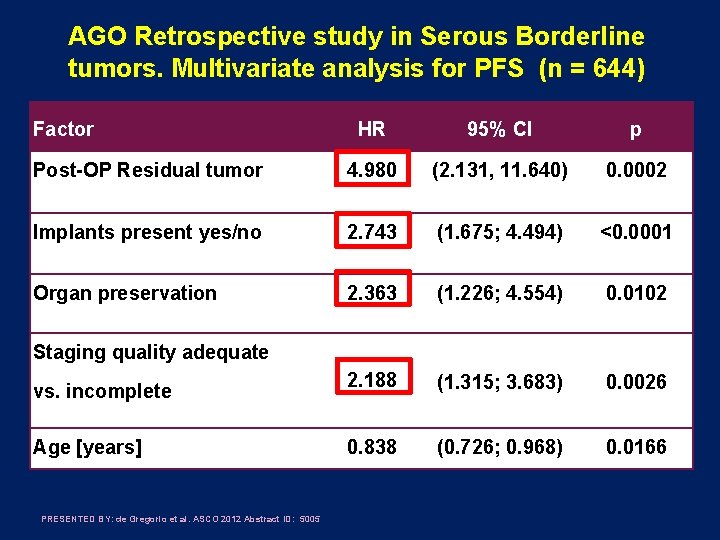
AGO Retrospective study in Serous Borderline tumors. Multivariate analysis for PFS (n = 644) Factor HR 95% CI p Post-OP Residual tumor 4. 980 (2. 131, 11. 640) 0. 0002 Implants present yes/no 2. 743 (1. 675; 4. 494) <0. 0001 Organ preservation 2. 363 (1. 226; 4. 554) 0. 0102 2. 188 (1. 315; 3. 683) 0. 0026 0. 838 (0. 726; 0. 968) 0. 0166 Staging quality adequate vs. incomplete Age [years] PRESENTED BY: de Gregorio et al. ASCO 2012 Abstract ID: 5005
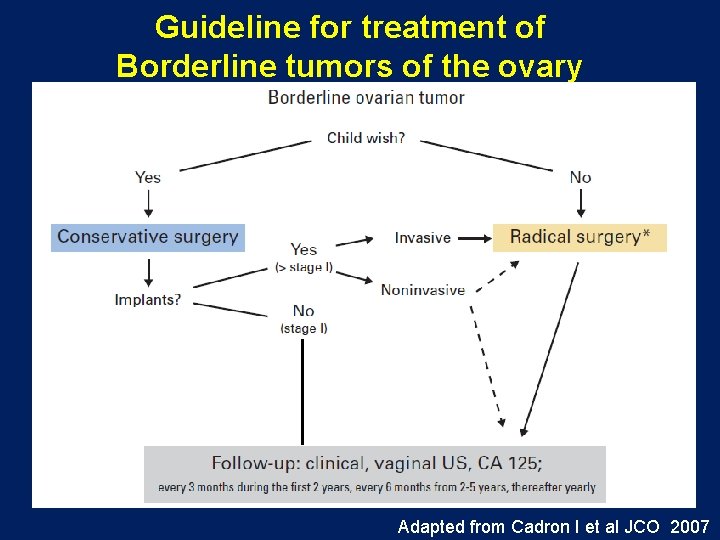
Guideline for treatment of Borderline tumors of the ovary Adapted from Cadron I et al JCO 2007
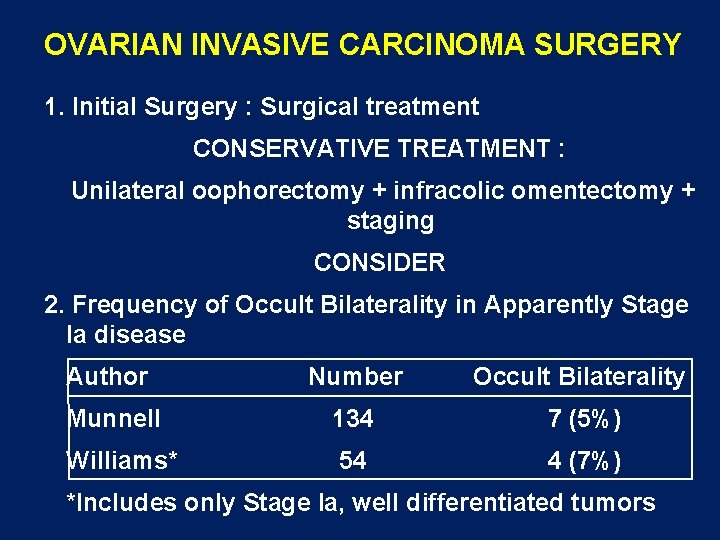

OVARIAN INVASIVE CARCINOMA SURGERY 1. Initial Surgery : Surgical treatment CONSERVATIVE TREATMENT : Unilateral oophorectomy + infracolic omentectomy + staging CONSIDER 2. Frequency of Occult Bilaterality in Apparently Stage Ia disease Author Number Occult Bilaterality Munnell 134 7 (5%) Williams* 54 4 (7%) *Includes only Stage Ia, well differentiated tumors
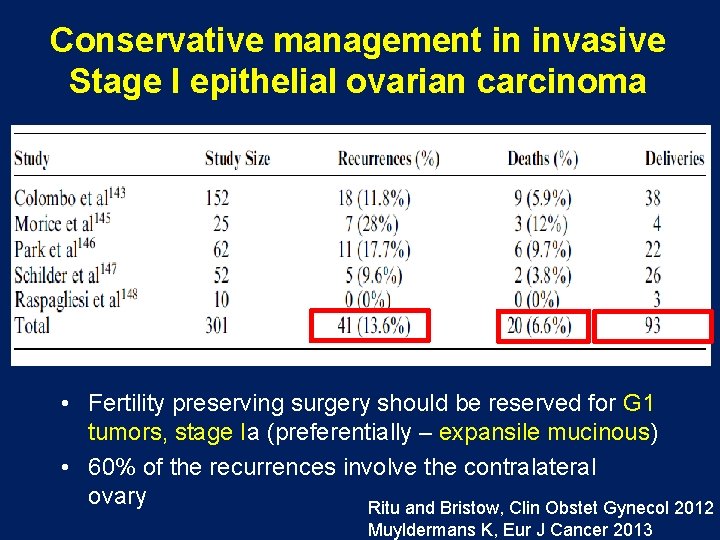
Conservative management in invasive Stage I epithelial ovarian carcinoma • Fertility preserving surgery should be reserved for G 1 tumors, stage Ia (preferentially – expansile mucinous) • 60% of the recurrences involve the contralateral ovary Ritu and Bristow, Clin Obstet Gynecol 2012 Muyldermans K, Eur J Cancer 2013

Ovarian Germ cell tumors • Very rarely bilateral (1%) except in dysgerminoma (Stage Ib: 10 -15%) • However, pure dysgerminoma is extremely chemosensitive and can almost always be cured at relapse with chemotherapy IN YOUNG PATIENTS WITH GERM CELL TUMORS: TREAT (ALWAYS) CONSERVATIVE. WHEN DOUBT ABOUT PATHOLOGY: WAIT FOR FINAL HISTOLOGY.

Fertility-Sparing Surgery in granulosacell tumors • 134 young patients (≤ 50 years) with stage I • 5 and 10 year survival of 97% and 94% • 71 (54%) had a fertility-sparing surgery • There was no difference in the outcome of women who had a standard vs conservative surgery (97% vs 98%) Zhang M, et al. Gynecol Oncol. 2007; 104(2): 396 -400.

Fertility sparing in endometrial cancer

Progestagen treatment of endometrial cancer in patients wishing to preserve fertility Literature review (n = 197): Tangjitgamol Gynecol Obstet Invest 2009 104 with CR without recurrence 40 with progression or persistent disease 53 with recurrence after first CR

Progestagen treatment of endometrial cancer in patients wishing to preserve fertility Korean series ( n= 148) • • • G 1 endometrioid ca No myometrial invasion < 40 y 115 CR (78%) of which 35 recurred 33 progression or persistence (hence 54% of 148 remained in CR –med F-up 58 months) • All recurrences or persistence remained limited to the uterus and none died. • 44 (38%) patients had at least one viable pregnancy Park Eur J Cancer 2013
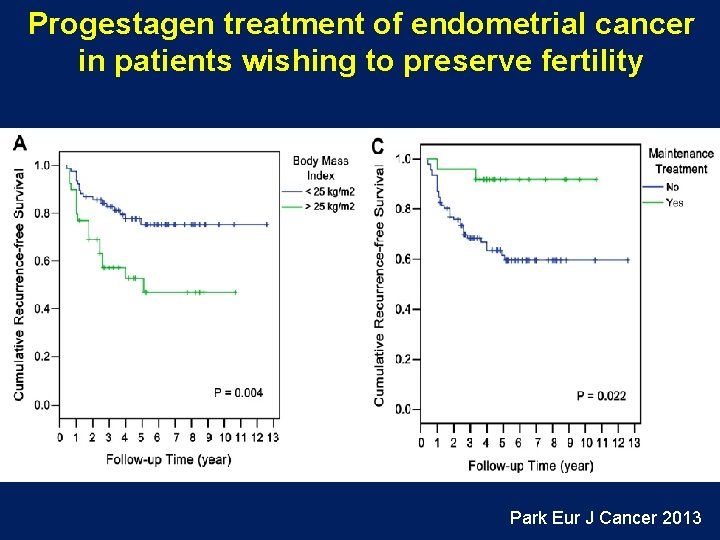
Progestagen treatment of endometrial cancer in patients wishing to preserve fertility Park Eur J Cancer 2013

Progestagen treatment of endometrial cancer in patients wishing to preserve fertility . Tangjitgamol Gynecol Obstet Invest 2009
- Slides: 37