Cancer Pain Fremantle Broome Sydney 1 Cancer pain

Cancer Pain Fremantle Broome Sydney 1

Cancer pain o Definition: ‘pain associated with cancer or its treatment’ o Palliation: ‘to relieve or lessen without curing’ (L. palliātus, ‘cloaked’) o 30% of CA patients have pain; 70% at end-of-life o prevalence of CA pain due to… o Aging population-more CA cases o Treatments which cause pain (surgery, chemo-radiotherapy) o Longer survival times (living with CA pain) o Shift in focus from end-of-life pain relief to a chronic pain management approach © Eric J. Visser 2017 UNDA. All rights reserved 2

Types of cancer pain o Acute pain o Breakthrough pain o Incident pain o Nociceptive pain o Neuropathic pain o Visceral pain o Neuroplastic pain (e. g. pathological fracture) (e. g. disease progression) (e. g. procedures, dressings, surgery, pathological fractures) (e. g. fracture, dressings) (e. g. nerve plexus invasion, chemo peripheral neuropathy) (e. g. CA pancreas) (central sensitization) http: //www. subsys. com/assets/subsys/client_files/images/cancer-pain-6. jpg © Eric J. Visser 2017 UNDA. All rights reserved 3

Cancer pain: A brief history o Pre 1980 s: focus on end-of-life palliation o Pain control o Limited access to strong opioids, even for cancer pain o Opioid stigma: fear of addiction, cultural & legal o 1986 -1990: WHO focus on CA pain management o WHO ladder & access to oral morphine resulted in… o Good CA pain control in 90% of cases (weeks, months) (simple analgesics, codeine, opioid injections, nerve blocks) © Eric J. Visser 2017 UNDA. All rights reserved (narcotics treaties) 4

Cancer pain: A brief history o Palliative care movement 1970 s o Advances in oncology, pain management, holistic care o Pain & palliative medicine specialities developed in 1990 s- o Changing CA patient profile (1990 s-) o Longer survival, remissions, pain due to CA treatments o 2000 s: living & functioning with CA pain (Dame Cicely Saunders, hospice care) 5

Cancer pain management approach o Aims: pain & suffering, quality of life & function o Bio-medical-psycho-social (holistic, spiritual) approach o Consider patient’s suffering & losses (stages of grief) -suffering is a sense of inevitable helplessness & hopelessness o Other symptoms -nausea, vomiting, constipation, anorexia, dyspnoea, itch, fatigue, sedation, confusion, anxiety, depression o Team approach -patient, family, GP, palliative care, nursing, allied health, spiritual advisor © Eric J. Visser 2017 UNDA. All rights reserved 6

Opioid analgesia o Opioids are still the mainstay of CA pain treatment o Particularly for severe pain, end-of-life, terminal sedation o Most commonly used opioids… o Morphine, hydromorphone, oxycodone, fentanyl (methadone) o Codeine, tramadol, buprenorphine, tapentadol o Most common routes… o Oral, transdermal, transmucosal, subcutaneous, intrathecal, PR © Eric J. Visser 2017 UNDA. All rights reserved 7

Opioids benefits o Cheap, available, familiar o Allows self-administration o Flexible dosing o Immediate & slow-release forms available o Multiple routes of administration o Antitussive (cough) o Treats dyspnoea & diarrhoea (most countries) (oral, s/L buccal, PR) (titratable) (e. g. for nil by mouth) © Eric J. Visser 2017 UNDA. All rights reserved 8

Opioids disadvantages Classic opioid side effects o Respiratory depression o Sedation o Confusion o Overdose o Nausea & vomiting o Anorexia o Constipation, urinary retention o Itch (accidental, self-harm, euthanasia) © Eric J. Visser 2017 UNDA. All rights reserved 9

Opioids disadvantages o Neuro-excitation (myoclonus, seizures) ( doses) -due to doses of opioid metabolites (e. g. M 3 G, nor-pethidine) o Tolerance (hyperalgesia) o Dependence o Chemical coping o Addiction o Immune suppression o Opioid security (withdrawal when opioid is ceased) (using opioids to cope with stress) (‘constant-craving’ & maladaptive behaviour) (CA recurrence, infection? ) (diversion), legal issues © Eric J. Visser 2017 UNDA. All rights reserved (Schedule 8, Australia) 10

WHO analgesia ladder o Major global public health initiative o Opioids for CA pain o Stepwise in opioid potency for increasing pain o Dosing ‘by mouth & by the clock’ o Simple, low cost, effective, useful in developing nations o May not reflect current practice o WHO analgesic ladder has been modified… (1986 -1990) (e. g. multimodal & ‘background’ analgesia) -adding interventions (nerve blocks) as the ‘final step’ -adding parallel steps: e. g. multimodal analgesics -use in acute & chronic non-cancer pain © Eric J. Visser 2017 UNDA. All rights reserved 11
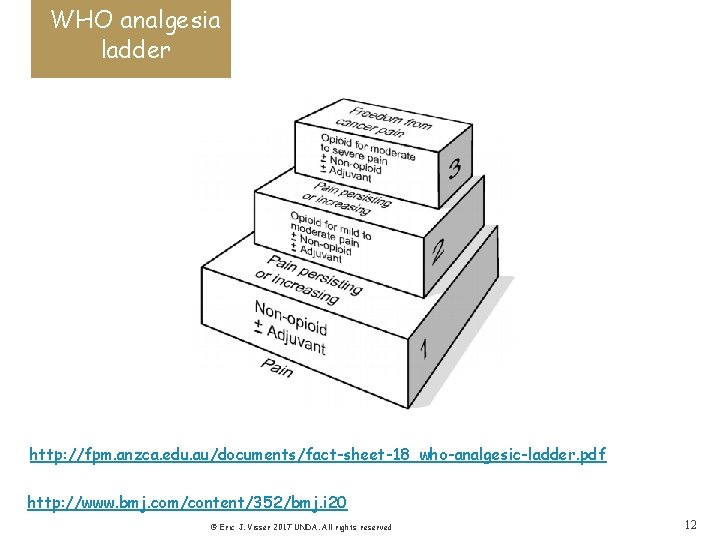
WHO analgesia ladder http: //fpm. anzca. edu. au/documents/fact-sheet-18_who-analgesic-ladder. pdf http: //www. bmj. com/content/352/bmj. i 20 © Eric J. Visser 2017 UNDA. All rights reserved 12

Morphine o ‘Gold standard’ analgesic for cancer pain -not therapeutically ‘better’, but historically most used opioid o Multiple routes: o Renal excretion of active metabolites M 6 G & M 3 G o Accumulation with renal impairment, dehydration o M 6 G: up to 100 x potency of morphine in CNS o M 6 G: longer t 1/2 with renal impairment o M 3 G: neurotoxic in doses o M 3 G: tolerance & hyperalgesia? oral (IR, CR), s/c, iv, intrathecal (myoclonus) © Eric J. Visser 2017 UNDA. All rights reserved 13

Hydromorphone o ‘Cleaner’ morphine? o Multiple routes: o water soluble: able to concentrate in high doses for s/c pumps (less sedation, confusion? ) Oral (IR, CR), s/c, iv, intrathecal (palliative care) o H 6 G: less dependence on renal excretion & less potent than M 6 G o H 3 G: renal excretion, neurotoxic in doses o Tolerance, hyperalgesia © Eric J. Visser 2017 UNDA. All rights reserved (myoclonus) 14

Oxycodone o CNS penetrance, rapid oral absorption & bioavailability makes it very effective for (acute) breakthrough pain o ‘Cleaner’? o Less cognitive side-effects? o efficacy for visceral & neuropathic pain? o Tolerance, hyperalgesia o Oral (IR, CR), PR, IV, s/c, buccal wafer o Combined w/- naloxone CR (minimally-active metabolites, less renal accumulation) (κ antagonist effect) (reduces opioid-induced constipation) © Eric J. Visser 2017 UNDA. All rights reserved 15

Fentanyl o Transdermal, transmucosal o Potent, rapid onset o No renal accumulation of metabolites o Advantage in… o Renal impairment o Nil-by-mouth o Effective for breakthrough or incident pain o Tolerance, hyperalgesia (lollipops, tablets), iv, s/c (not oral) (e. g. transmucosal lollipop) (more rapid onset? ) © Eric J. Visser 2017 UNDA. All rights reserved 16

Opioid rotation Effective ‘trouble shooting’ o Changing the opioid drug or route of administration to improve analgesia and/or reduce side-effects o Improves analgesia & side effects in 80% of cases o opioid tolerance & hyperalgesia o When changing the opioid… -it’s not critical which opioid you choose, as long as it’s different o Changing route of administration o OR is an example of a ‘personalised medicine’ approach o So, if you have a problem with an opioid, just change it (e. g. oral to s/c or intrathecal) © Eric J. Visser 2017 UNDA. All rights reserved 17

Opioid rotation Why does it work? Significant inter-individual & population variability in o Opioid receptors -genetics, distribution, pharmacodynamics -incomplete cross-tolerance between opioids at receptor o Opioid metabolism (pharmacogenomics) -cytochrome P 450 (2 D 6) polymorphism o Clinical states -renal & liver function (metabolism, clearance) -oral absorption -drug interactions -age, illness © Eric J. Visser 2017 UNDA. All rights reserved 18

Breakthrough pain o Increase in background pain requiring prn opioid doses o Usually ≥ 4 prn doses per day o Why is the pain getting worse? o Try opioid rotation (first) or… o Increase the prn opioid dose or… o Introduce or increase background opioid analgesia o Use multimodal analgesia (disease progression, tolerance) (e. g. NSAID, paracetamol, pregabalin) https: //www. lazanda. com/breakthrough_cancer_pain © Eric J. Visser 2017 UNDA. All rights reserved 19

Incident pain o Pain due to procedures, physical activity or intercurrent disease o Physio, dressings, surgery, biopsies, mucositis, PHN o Timing of prn analgesia is critical o Multimodal approach o Rapid/short acting opioids: fentanyl or oxycodone o IV, PCA, buccal, intranasal o Topical agents o Nitrous oxide/O 2 (Entonox) o Ketamine lozenges (give pre-procedure) (may need sedation, anxiolysis) (e. g. lidocaine) © Eric J. Visser 2017 UNDA. All rights reserved 20
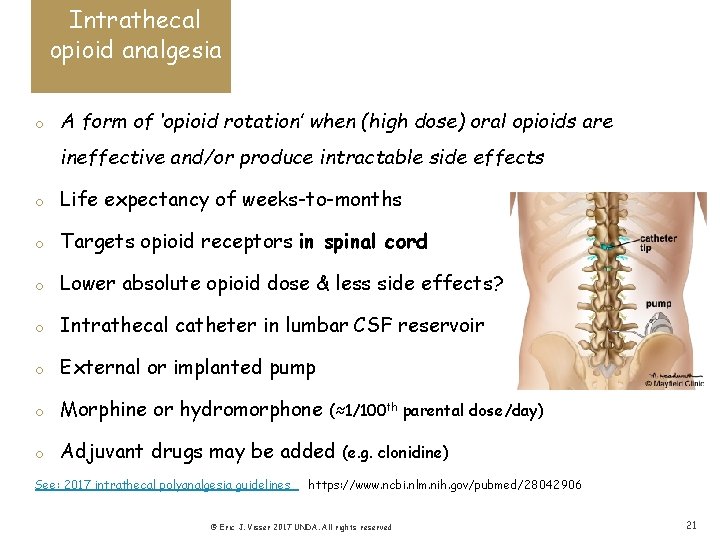
Intrathecal opioid analgesia o A form of ‘opioid rotation’ when (high dose) oral opioids are ineffective and/or produce intractable side effects o Life expectancy of weeks-to-months o Targets opioid receptors in spinal cord o Lower absolute opioid dose & less side effects? o Intrathecal catheter in lumbar CSF reservoir o External or implanted pump o Morphine or hydromorphone o Adjuvant drugs may be added See: 2017 intrathecal polyanalgesia guidelines (≈1/100 th parental dose/day) (e. g. clonidine) https: //www. ncbi. nlm. nih. gov/pubmed/28042906 © Eric J. Visser 2017 UNDA. All rights reserved 21

Multimodal analgesia o The rational use of two-or-more analgesics to improve pain and/or reduce side effects o Usually by adding other analgesics to opioids o An opioid-sparing technique o Not well studied in RCTs for CA pain o Based on evidence extrapolated from acute pain management © Eric J. Visser 2017 UNDA. All rights reserved 22

Multimodal analgesia o Paracetamol, NSAIDs, COX-2 inhibitors (nociceptive pain) -e. g. metastatic bone pain o Anticonvulsants (pregabalin, gabapentin) (neuropathic pain) -e. g. radiculopathy, post-mastectomy, acute zoster pain o Antidepressants (amitriptyline, duloxetine) (neuropathic pain) -e. g. polyneuropathy, post-herpetic neuralgia o Ketamine (opioid sparing, neuropathic pain) -modest analgesia & opioid sparing in CA pain (level III) o Antispasmodics -diazepam, baclofen for skeletal mm spasm -buscopan for smooth mm spasm © Eric J. Visser 2017 UNDA. All rights reserved 23
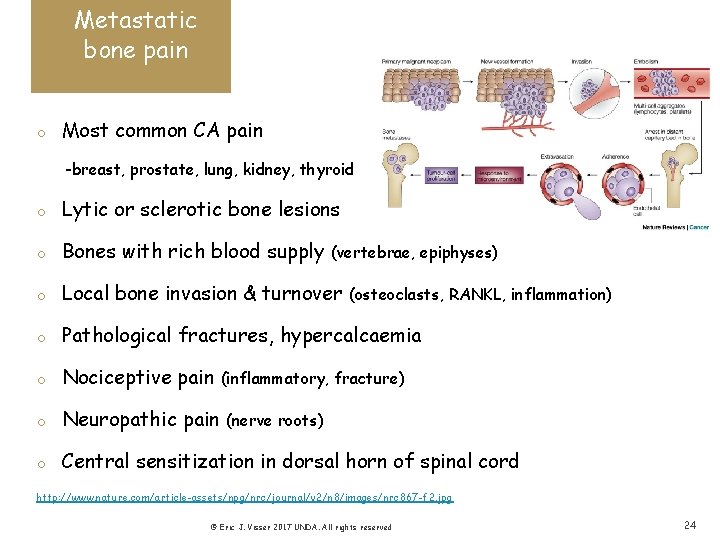
Metastatic bone pain o Most common CA pain -breast, prostate, lung, kidney, thyroid o Lytic or sclerotic bone lesions o Bones with rich blood supply o Local bone invasion & turnover o Pathological fractures, hypercalcaemia o Nociceptive pain o Neuropathic pain o Central sensitization in dorsal horn of spinal cord (vertebrae, epiphyses) (osteoclasts, RANKL, inflammation) (inflammatory, fracture) (nerve roots) http: //www. nature. com/article-assets/npg/nrc/journal/v 2/n 8/images/nrc 867 -f 2. jpg © Eric J. Visser 2017 UNDA. All rights reserved 24
Metastatic bone pain management o Multimodal analgesia approach o Treat the cancer (chemo-radiotherapy, immunotherapy, hormones, surgery) -remember hypercalcaemia o Nociceptive pain o Opioids & multimodal analgesia o NSAIDs & COX-2 inhibitors (inflammatory, bone turnover, fractures) -Musculoskeletal & visceral pain (renal colic) -part of multimodal analgesia -adverse effects: renal, gut, bleeding (NSAIDs) http: //www. wheelessonline. com/images/i 1/brst 1. jpg Metastatic breast cancer humerus © Eric J. Visser 2017 UNDA. All rights reserved 25

Metastatic bone pain management o Bisphonates (calcitonin is not effective) -first line treatment, very effective (level I evidence) - bone pain in days to weeks - bone osteoclast activity ( fracture risk & Ca++) -adverse effects: renal, jaw osteonecrosis o Denosumab? -human monoclonal antibody against RANKL ( osteoclast development) - fractures (breast CA metastases; needs further study re bone pain) o Radiotherapy -whole body, focal beam, radiopharmaceuticals (Sr 89, Sa o Surgical fixation, vertebroplasty o Physical measures 153) (cement injected into fracture) (splints, braces) © Eric J. Visser 2017 UNDA. All rights reserved 26
Metastatic bone pain management o Neuropathic pain (nerve roots, plexus, spinal cord) -pregabalin, ketamine -IV lidocaine o Central sensitization (spinal dorsal horn) -pregabalin, ketamine o Preventive treatments (pathological fractures) -bisphonates, surgical fixation -radiotherapy? o Corticosteroids -acute spinal cord compression Metastatic sclerotic lesions CA prostate compressionhttps: //images. radiopaedia. org/images/5814286/30 d 663 fdf 739 e 2288277 ec 5 b 436379_jumbo. JPG 27
Mucositis pain o Painful inflammation & ulceration of (high cell-turnover) mucous membranes due to chemo or radiotherapy o Haematological cancers, bone marrow transplant, often in kids o Oropharynx, oesophagus, rectum o Acute nociceptive & neuropathic pain lasting days to weeks o Extremely painful, can’t swallow or speak o Significant psychological distress o Parenteral opioids o Multimodal analgesia o Topical agents o Low level laser red light buccal therapy (e. g. PCA) (e. g. IV ketamine) (mouth wash: salt & soda, lidocaine, sucralfate, doxepin, ketamine) http: //diseasespictures. com/mucositis/ © Eric J. Visser 2017 UNDA. All rights reserved 28
Gut obstruction, liver distension o Visceral pain, peritoneal (capsule-stretch) pain o Parental (IV) opioid analgesia & drug therapies o (nil by mouth) Antispasmodics (hyoscine, glycopyrrolate) -severe colic, reduces gut secretions o Anti-secretion (octreotide) o Anti-inflammatory (dexamethasone) (upper gut obstruction) -bowel obstruction, liver distension, IVC obstruction o NGT, stenting, venting gastrostomy, enterostomy o Peritoneal tap (gut obstruction) (ascites) © Eric J. Visser 2017 UNDA. All rights reserved 29
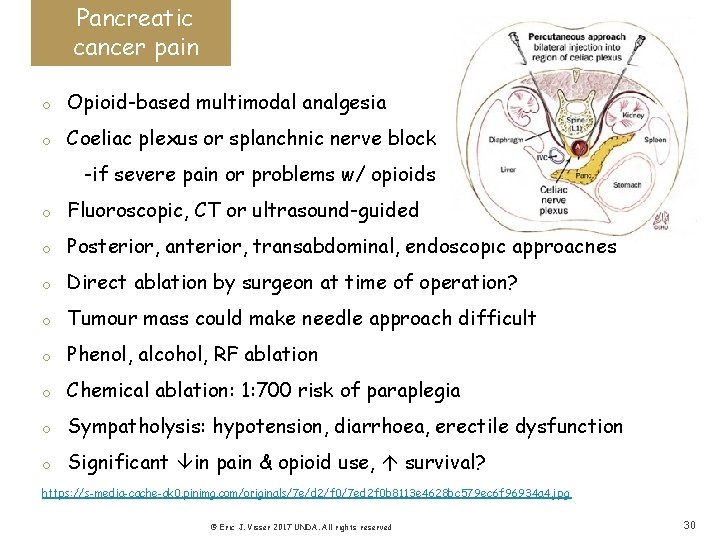
Pancreatic cancer pain o Opioid-based multimodal analgesia o Coeliac plexus or splanchnic nerve block -if severe pain or problems w/ opioids o Fluoroscopic, CT or ultrasound-guided o Posterior, anterior, transabdominal, endoscopic approaches o Direct ablation by surgeon at time of operation? o Tumour mass could make needle approach difficult o Phenol, alcohol, RF ablation o Chemical ablation: 1: 700 risk of paraplegia o Sympatholysis: hypotension, diarrhoea, erectile dysfunction o Significant in pain & opioid use, survival? https: //s-media-cache-ak 0. pinimg. com/originals/7 e/d 2/f 0/7 ed 2 f 0 b 8113 e 4628 bc 579 ec 6 f 96934 a 4. jpg © Eric J. Visser 2017 UNDA. All rights reserved 30
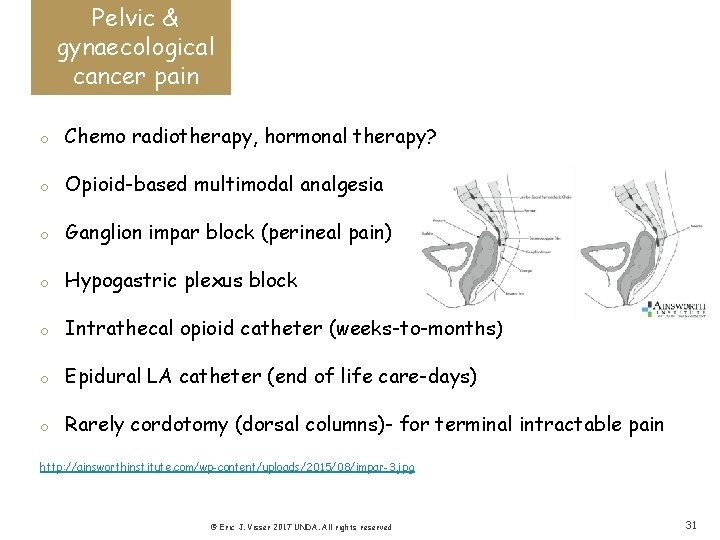
Pelvic & gynaecological cancer pain o Chemo radiotherapy, hormonal therapy? o Opioid-based multimodal analgesia o Ganglion impar block (perineal pain) o Hypogastric plexus block o Intrathecal opioid catheter (weeks-to-months) o Epidural LA catheter (end of life care-days) o Rarely cordotomy (dorsal columns)- for terminal intractable pain http: //ainsworthinstitute. com/wp-content/uploads/2015/08/impar-3. jpg © Eric J. Visser 2017 UNDA. All rights reserved 31

BREAST-CANCER-Surgery. Pain-Churack. Masterclass-June 2015. ppt © Eric J. Visser 2017 UNDA. All rights reserved 32

Physical & comfort measures o Positioning, turns, pressure care, mattress o Splints, massage o Ventilation, windows, O 2 (dyspnoea) o Aromatherapy o Acupuncture o TENS machine o Hot, cold packs o Urinary catheter o NGT (bowel obstruction) © Eric J. Visser 2017 UNDA. All rights reserved 33

Palliative care o o o o Multidisciplinary team approach (home vs hospice/hospital) Total management of the person & family Distress, pain & other symptom Mx Anxiety (‘angst’) Dyspnoea Nausea & vomiting, itch Cognitive & conscious changes Bladder & bowel (tenesmus, constipation, diarrhoea) Renal, gut (nutrition, hydration) Effusions, AF CCF Hypercalcaemia Infection (UTI, pneumonia) s/c & intrathecal infusions Terminal sedation © Eric J. Visser 2017 UNDA. All rights reserved 34

Psychological options o Existential angst o Manage depression, anxiety (panic), sleep o Antidepressants, anxiolytics o Psychological therapies (stages of grief) o Spiritual care o Information, education o Music & distraction o Mindfulness based stress reduction o Hypnosis o Home or garden visits, animal therapy o Family & carers © Eric J. Visser 2017 UNDA. All rights reserved 35
- Slides: 35