Chronic Headaches Fremantle Broome Sydney Introduction Chronic daily

Chronic Headaches Fremantle Broome Sydney

Introduction Chronic daily headaches o ≥ 15 headache days per month for ≥ 3 months (IHS 2013) o 5% of population (F>M 4: 1) o 5 Fs (Fat, Female, Forties, Frightened) o Caucasian, lower SES o Stress & anxiety o Quality of life & economic burden o Top-ten worldwide health disabilities (WHO)

Alice in Wonderland http: //migraine. blogs. nytimes. com/2008/02/10/down-the-rabbit-hole/? _r=0
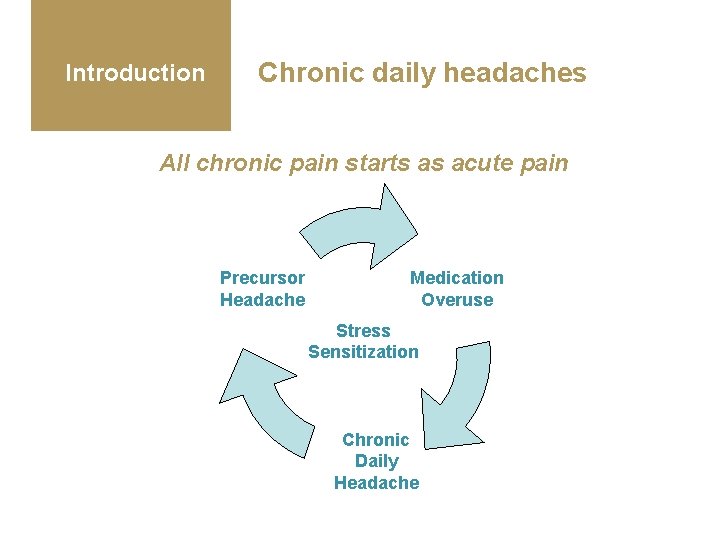
Introduction Chronic daily headaches All chronic pain starts as acute pain Precursor Headache Medication Overuse Stress Sensitization Chronic Daily Headache

Precursor headaches o Primary headaches -migraine -tension-type -cluster o Secondary headaches -medication overuse -cervicogenic (‘whiplash’) -others -sinus, orofacial -neuralgias (occipital, trigeminal) -red flags
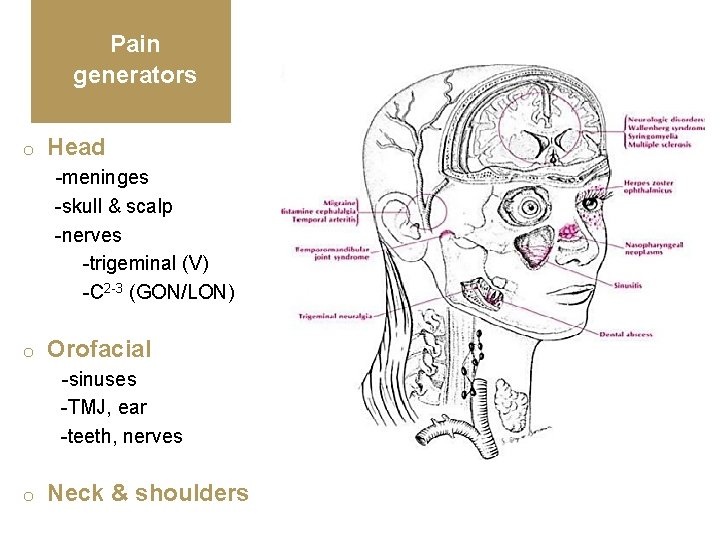
Pain generators o Head -meninges -skull & scalp -nerves -trigeminal (V) -C 2 -3 (GON/LON) o Orofacial -sinuses -TMJ, ear -teeth, nerves o Neck & shoulders
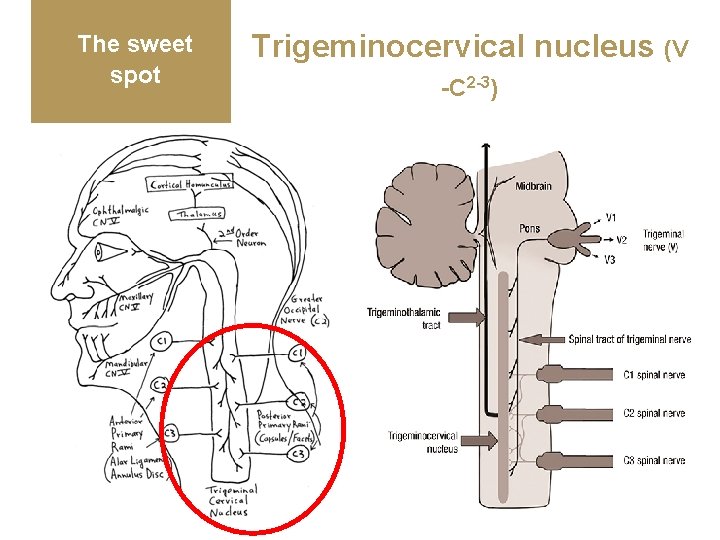
The sweet spot Trigeminocervical nucleus (V -C 2 -3)

Neuromodulation Trigeminocervical nucleus (V -C 2 -3)

Chronic daily headaches o Transformed precursor headache o Becomes more like TTH o Mild sensory sensitivity, nausea o Headache spectrum o Sensitization (V-C 2 -3) o Time patterns (morning or late day) o Cognitive & functional impacts

Chronic daily headaches Most common o Chronic migraine (transformed) o Chronic tension-type o Cervicogenic -whiplash-associated o Medication overuse headache o New daily persistent headache (remembers exact day of onset) o Others (e. g. intracranial pressure syndromes)
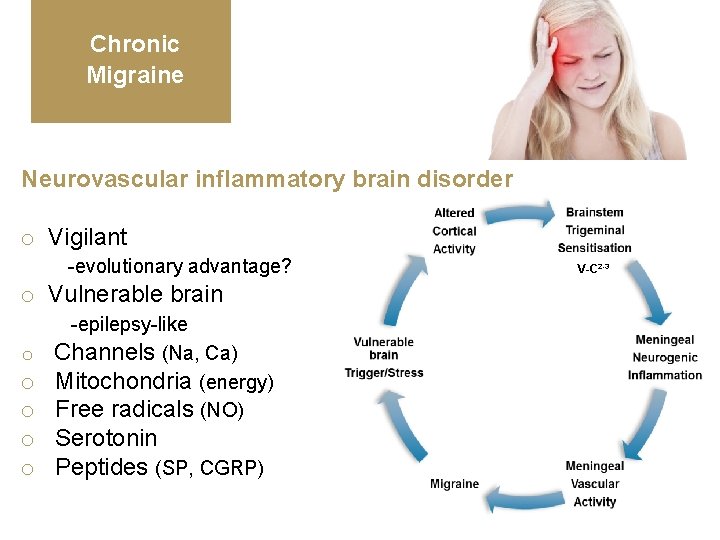
Chronic Migraine Neurovascular inflammatory brain disorder o Vigilant -evolutionary advantage? o Vulnerable brain o -epilepsy-like Channels (Na, Ca) Mitochondria (energy) Free radicals (NO) o o o Serotonin o Peptides (SP, CGRP) V-C 2 -3
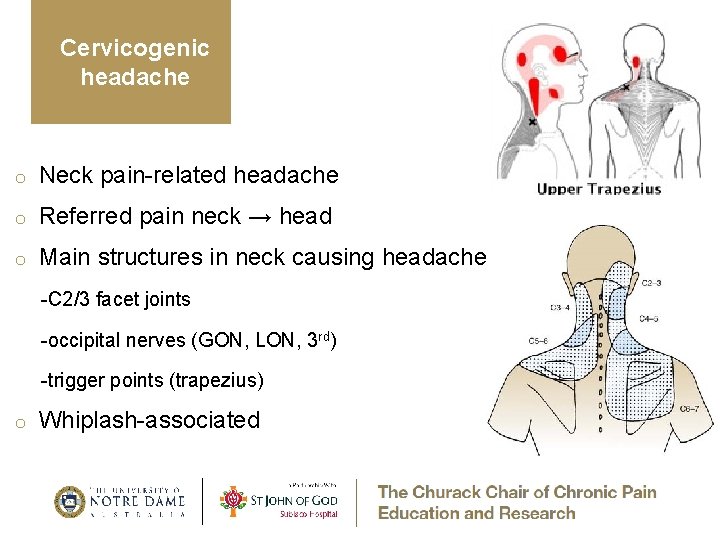
Cervicogenic headache o Neck pain-related headache o Referred pain neck → head o Main structures in neck causing headache -C 2/3 facet joints -occipital nerves (GON, LON, 3 rd) -trigger points (trapezius) o Whiplash-associated
Whiplashassociated headache o Pain generators o Regional pain sensitization -inflammation (cytokines, Toll) -autonomic dysfunction (α receptors) -vascular trash theory o Dural tear → CSF leak (low pressure headache)

Dural tear headache
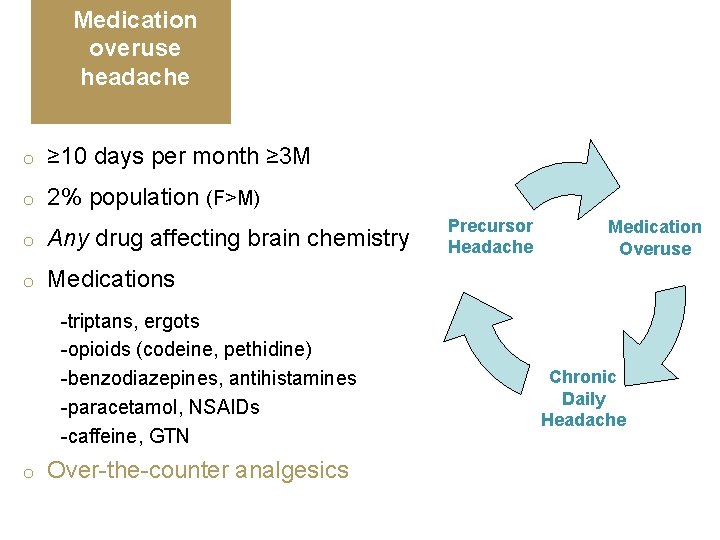
Medication overuse headache o ≥ 10 days per month ≥ 3 M o 2% population (F>M) o Any drug affecting brain chemistry o Medications -triptans, ergots -opioids (codeine, pethidine) -benzodiazepines, antihistamines -paracetamol, NSAIDs -caffeine, GTN o Over-the-counter analgesics Precursor Headache Medication Overuse Chronic Daily Headache
Medication overuse headache o Rebound theory o Habitual behaviours -dose control -doctor shopping, dependency -eye opener doses -injections o High risk medications -triptans -OTC -pethidine Precursor Headache Medication Overuse Chronic Daily Headache

CDH management Bio-medical-psycho-social-environmental approach Multimodal, multidisciplinary o Diagnosis (medication use, red flags) o Education, information & lifestyle o Pharmacotherapies o Physical therapies o Behavioural therapies o Interventions

CDH management o Establish a headache diagnosis -chronic daily headache -precursor headache -medication overuse o Exclude ‘red flags’ T. I. N. T (<1%) o MRI head (neck) in previous 2 years o Review by a neurologist
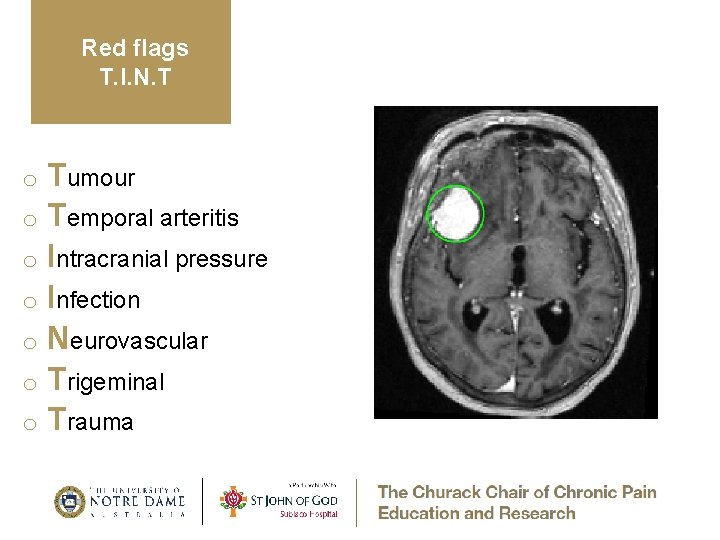
Red flags T. I. N. T Tumour o Temporal arteritis o Intracranial pressure o Infection o Neurovascular o Trigeminal o Trauma o

Examination o Nerves -cranial nerves examination -trigeminal -scalp nerves (sensation) -GON, LON -temporal, periorbital o Arteries -temporal (ESR, CRP) -carotid
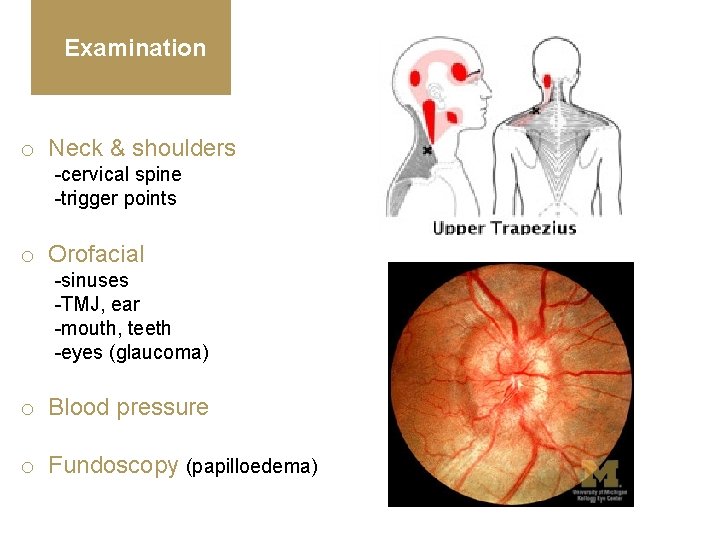
Examination o Neck & shoulders -cervical spine -trigger points o Orofacial -sinuses -TMJ, ear -mouth, teeth -eyes (glaucoma) o Blood pressure o Fundoscopy (papilloedema)

Education o Information o Medication overuse o Headache diary (triggers, medications) o Stress o Sleep o Lifestyle (work) o BMI, exercise, diet, caffeine, alcohol, smoking o Websites

Pharmacology Vitamin therapy (level II evidence)
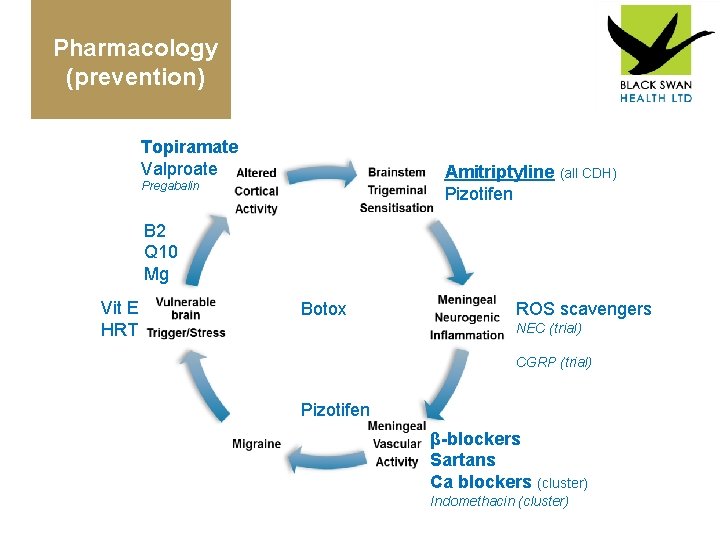
Pharmacology (prevention) Topiramate Valproate Amitriptyline (all CDH) Pizotifen Pregabalin B 2 Q 10 Mg Vit E HRT Botox ROS scavengers NEC (trial) CGRP (trial) Pizotifen β-blockers Sartans Ca blockers (cluster) Indomethacin (cluster)
Migraine trial Antioxidants
Physical therapies o o o o o Exercise Posture Range of movement Manipulation (flare-up pain) Watson technique Trigger points Dry needling Low level laser (Cochrane) TENS

Behavioural Clinical psychology o Mood, anxiety o Stress reduction o Mindfulness o Yoga o Sleep o Biofeedback o Habitual behaviours (medication overuse) o Drug & alcohol
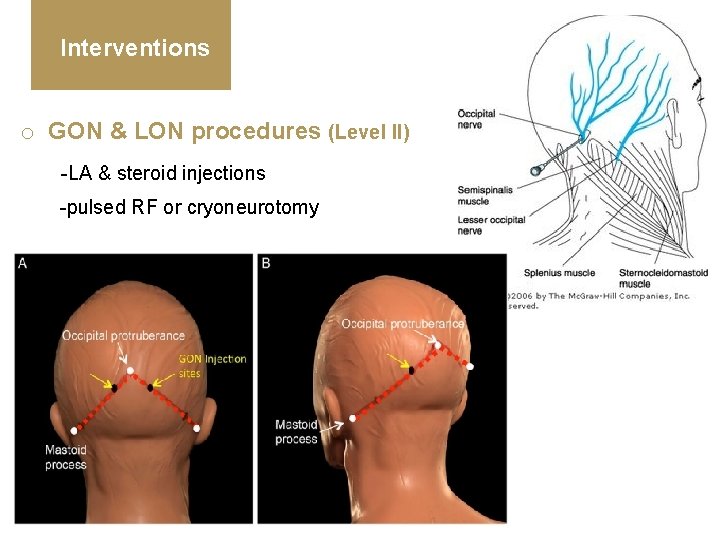
Interventions o GON & LON procedures (Level II) -LA & steroid injections -pulsed RF or cryoneurotomy
Interventions o Trigger point injections, dry needling o Acupuncture (Cochrane) -migraine -TTH
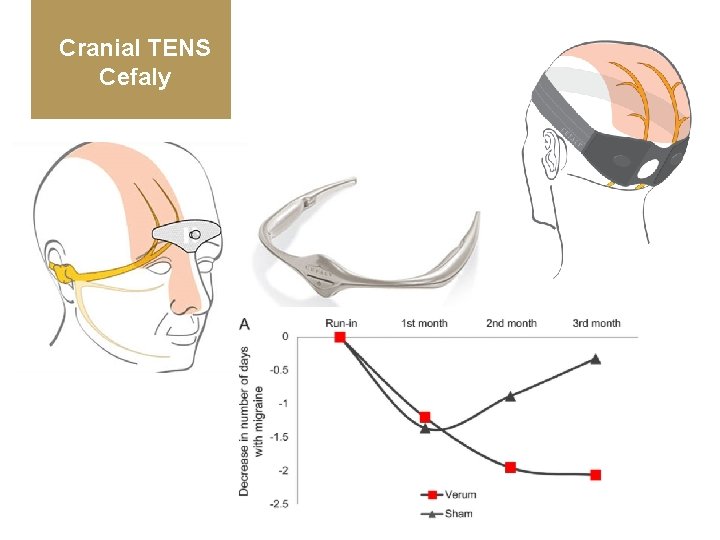
Cranial TENS Cefaly
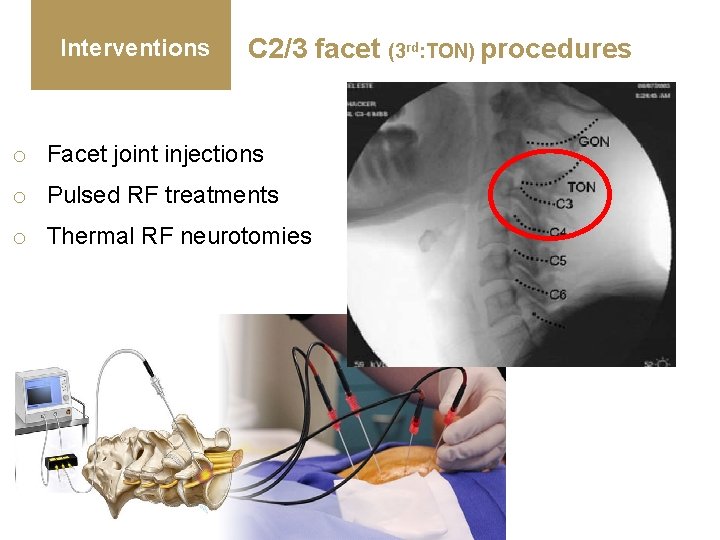
Interventions C 2/3 facet (3 rd: TON) procedures o Facet joint injections o Pulsed RF treatments o Thermal RF neurotomies
Interventions Neuromodulation o Cranial TENS (Cefaly) o Transcranial magnetic stimulation o Occipital nerve or field stimulator

Medication overuse headache o o o o o Stopping medications is key Preparation is vital (work, lifestyle) Realistic expectations (it’s going to be hard) Psychologist (stress, pain) (key supporters) Exclude drug dependency or addiction Headache diary Optimise precursor headache (prophylaxis) Treat withdrawal & rebound headache Prevent relapse (30 -50%) Outpatient vs inpatient Evers & Jensen EJN 2011

Outpatient plan (4 weeks) o Optimise precursor headache -GON blocks, Cefaly, topiramate, Botox o Baseline treatment -amitriptyline, metoclopramide, prednisolone, lorazepam prn o Taper medications by 10% per week o Rescue plan -Cefaly, NSAIDs (indomethacin PR), clonidine, antiemetics, lorazepam prn -nasal oxytocin? o Frequent medical review

Key messages o o o o o CDH is common & crippling Precursor headache Medication overuse Stress Exclude red flags (MRI) Headache diary Optimise precursor headache Stop analgesics Multi disciplinary support Watch closely (relapse rate 30%)

Websites Churack-chair http: //www. nd. edu. au/churack/home Painchecker (coming soon)

Essential reading http: //www. racgp. org. au/afp/2014/march/chronic-headache/ http: //www. aafp. org/afp/2014/0415/p 642. pdf

Chronic Headaches Fremantle Broome Sydney

Primary Headaches o Tension-type (most common 80%) o Migraine (15%) -aura (15%) -without aura) (common migraine) (75%) o Vascular-autonomic (cluster headache) (rare <1%)

Secondary Headaches o Chronic daily headache (transformed) o Medication overuse headache o Cervicogenic headache o Whiplash-associated headache o Occipital neuralgia o Others (e. g. sinus headache) o Pathological ‘red flags’ (T. I. N. T)
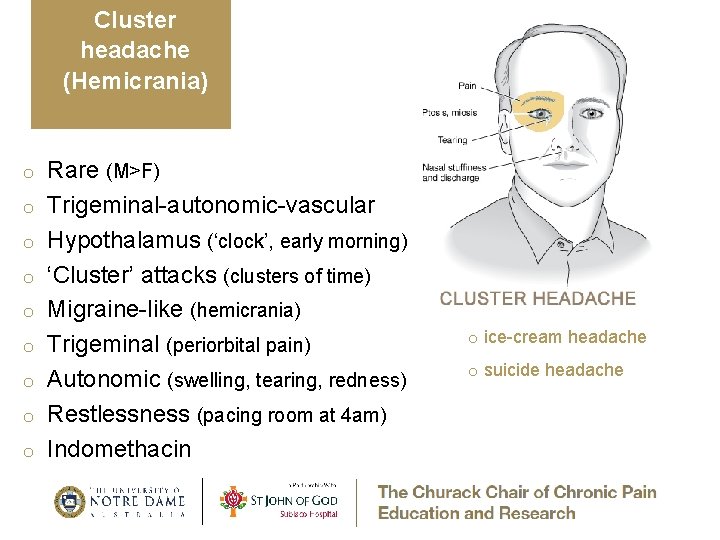
Cluster headache (Hemicrania) o o o o o Rare (M>F) Trigeminal-autonomic-vascular Hypothalamus (‘clock’, early morning) ‘Cluster’ attacks (clusters of time) Migraine-like (hemicrania) Trigeminal (periorbital pain) Autonomic (swelling, tearing, redness) Restlessness (pacing room at 4 am) Indomethacin o ice-cream headache o suicide headache

Inpatient plan (5 days) o As per outpatient plan o Abruptly cease headache medications o Baseline: IV low-dose ketamine, IV metoclopramide, IV dexamethasone o Rescue plan -Cefaly, IV antiemetics, parecoxib, clonidine, nasal oxytocin? -IV lignocaine

History o Character of headache -worsening, ‘thunderclap’, postural, neurological symptoms, vomiting, wakes at night o Triggers -injury, illness, whiplash, stress, medications, diet, sleep, menstrual o Personal & family -1⁰ family, head injury, sleep apnoea (OSA), patent ductus -childhood headache or pain, abdominal migraine o Medication & substance use


- Slides: 45