Cancer Pain Fremantle Broome Sydney 1 Cancer pain

Cancer Pain Fremantle Broome Sydney 1

Cancer pain o ‘Pain associated with cancer or its treatment’ o 30% of CA patients (40% have severe pain) o 70% at end-of-life o 50% following treatment (chronic) o prevalence of CA pain due to… o Aging population (more cases) o Treatments which cause pain (surgery, chemo-radiotherapy) o survival times (living w/- CA) o Shift in focus: end-of-life pain relief to chronic pain Mx 2

Types of cancer pain o Acute pain o Breakthrough pain o Incident pain o Chronic pain o Nociceptive pain o Neuropathic pain o Visceral pain o Neuroplastic pain (e. g. pathological fracture) (e. g. disease progression) (e. g. procedures, dressings, surgery, fractures) (e. g. post mastectomy) (e. g. fracture, dressings) (e. g. nerve plexus invasion, chemo neuropathy) (e. g. CA pancreas) (central sensitization) © Eric J. Visser 2017 UNDA. All rights reserved 3

Cancer pain: A brief history o Pre 1980 s: focus on end-of-life palliation o Pain control o Limited access to strong opioids, even for CA pain o Opioid stigma: fear of addiction, cultural & legal o 1986 -1990: WHO focus on CA pain management o WHO ladder & access to oral morphine resulted in… o Good CA pain control in 90% of cases (simple analgesics, opioid injections, nerve blocks) © Eric J. Visser 2017 UNDA. All rights reserved (narcotics treaties) 4

Cancer pain: A brief history o Palliative care movement in 1970 s o Advances in oncology, pain management, holistic care o Pain & palliative medicine specialities in 1990 s- o Changing CA patient profile (1990 s-) o Longer survival, remissions o Chronic pain due to CA treatments o 2000 s: living & functioning with CA pain (Dame Cicely Saunders, hospice) 5

Cancer pain management approach o pain & suffering o Qo. L & function o chronic pain o Mx other symptoms o Bio-medical-psycho-social approach o Team-based o Oncology o Pain medicine (in survivors) (multidisciplinary) (treat disease) (holistic) care & palliative medicine teams (acute, perioperative, chronic pain, ’blocks’ & pumps) © Eric J. Visser 2017 UNDA. All rights reserved 6

Opioid analgesia o Still mainstay of CA pain treatment o Severe pain, end-of-life, terminal sedation o Most commonly used opioids… o Morphine, hydromorphone, oxycodone, fentanyl, methadone o Codeine, tramadol, buprenorphine, tapentadol o Most common routes… o Oral, transdermal, transmucosal, subcutaneous © Eric J. Visser 2017 UNDA. All rights reserved 7

Opioids benefits o Cheap, available, familiar o Allows self-administration o Flexible dosing o Immediate & slow-release forms o Multiple routes of administration o Antitussive o Dyspnoea & diarrhoea (most countries) (oral, s/L buccal, PR) (titratable) (e. g. nil by mouth) © Eric J. Visser 2017 UNDA. All rights reserved 8

Opioids disadvantages o Classical ‘side effects’ o Neuro-cognitive o Myoclonus, seizures o Opioid metabolites o Endocrinopathy o Immunity? o Tolerance & opioid-induced hyperalgesia o Dependence (withdrawal) (sedation, confusion) ( doses) (M 3 G, nor-pethidine) (pituitary hormones, testosterone) © Eric J. Visser 2017 UNDA. All rights reserved 9

Opioids disadvantages o Dose escalation o Dose ceiling o Chemical coping o Addiction o Self harm & overdose o Opioid security o Legal issues (ONLY in 30% of patients) (don’t keep going up) (using opioids to cope with stress) (diversion) (Schedule 8) © Eric J. Visser 2017 UNDA. All rights reserved 10

WHO analgesia ladder o Global public health initiative o Opioids for CA pain o Stepwise in opioid potency for increasing pain o Dosing ‘by the mouth & by the clock’ o Simple, low cost, effective, useful in developing nations o May not reflect current practice (1986 -1990) (multimodal & ‘background’ analgesia) © Eric J. Visser 2017 UNDA. All rights reserved 11

Morphine o ‘Gold standard’ for cancer pain o Multiple routes: o Renal excretion of active metabolites M 6 G & M 3 G o M 6 G: 100 x potency of morphine, longer t 1/2 (sedation) o M 3 G: neurotoxic in doses o M 3 G: tolerance & hyperalgesia oral (IR, CR), s/c, iv, intrathecal (confusion, myoclonus) © Eric J. Visser 2017 UNDA. All rights reserved 12
![Hydromorphone o ‘Cleaner’ morphine? o Water soluble o [ ] in high doses for Hydromorphone o ‘Cleaner’ morphine? o Water soluble o [ ] in high doses for](http://slidetodoc.com/presentation_image_h/0a7d55b0e0f203771d375d352407bd0a/image-13.jpg)
Hydromorphone o ‘Cleaner’ morphine? o Water soluble o [ ] in high doses for s/c pumps (palliative care) o H 6 G: less potent than M 6 G o H 3 G (renal): neurotoxic in doses (less sedation, confusion? ) (myoclonus) © Eric J. Visser 2017 UNDA. All rights reserved 13

Oxycodone o Fast o bioavailability & CNS penetrance o Effective for acute o Cleaner? (less cognitive side-effects? ) o Minimally active metabolites o Better for visceral & neuropathic pain? o Buccal wafer o Combined w/- naloxone CR (breakthrough) pain (CYP 2 D 6) (κ antagonist effect) (reduces opioid-induced constipation) © Eric J. Visser 2017 UNDA. All rights reserved 14
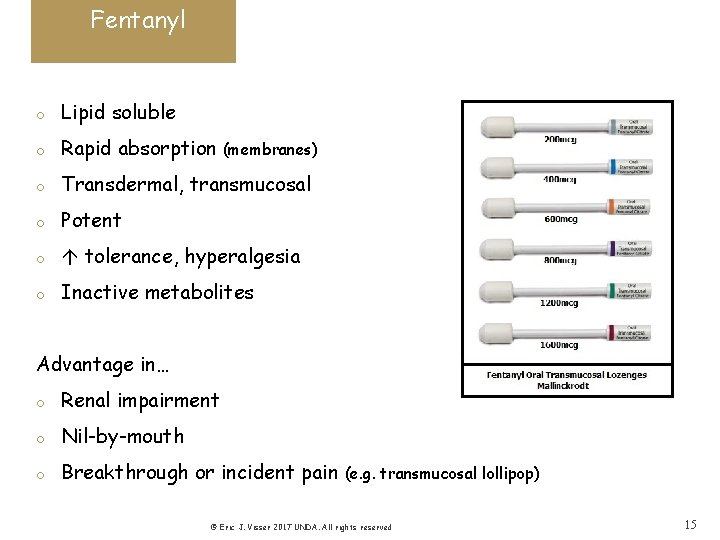
Fentanyl o Lipid soluble o Rapid absorption o Transdermal, transmucosal o Potent o tolerance, hyperalgesia o Inactive metabolites (membranes) Advantage in… o Renal impairment o Nil-by-mouth o Breakthrough or incident pain (e. g. transmucosal lollipop) © Eric J. Visser 2017 UNDA. All rights reserved 15

Opioid rotation ‘trouble shooting’ o Changing type or route of an opioid to improve analgesia and/or reduce side-effects o Route: oral to s/c or intrathecal o Fixes opioid problems 80% of the time o Good alternative to doses o analgesia; side effects o tolerance & hyperalgesia o Inter-individual variability in opioid response o Receptors, metabolites, clinical condition o ‘Personalised medicine’ (rotate before escalate) © Eric J. Visser 2017 UNDA. All rights reserved 16

Multimodal analgesia o The rational use of two-or-more analgesics to improve analgesia and/or reduce side effects o Usually by adding other analgesics to opioids o Opioid-sparing o Not well studied in RCTs for CA pain o Based on evidence from acute pain management © Eric J. Visser 2017 UNDA. All rights reserved 17

Multimodal analgesia o Paracetamol, NSAIDs, COX-2 inhibitors (nociceptive pain) (I -? ) -e. g. metastatic bone pain o Anticonvulsants (pregabalin, gabapentin) (neuropathic pain) -e. g. radiculopathy, post-mastectomy, acute zoster pain -gabapentinoids added to opioids: no improvement in pain (I -) o Antidepressants (amitriptyline, duloxetine) (neuropathic pain) -e. g. polyneuropathy, post-herpetic neuralgia © Eric J. Visser 2017 UNDA. All rights reserved 18

Multimodal analgesia o Ketamine (opioid sparing, neuropathic pain) (I -) -modest analgesia & opioid sparing in CA pain? -no benefit from ‘pulse’ or rapid dose escalation (I -) o Corticosteroids (I -? ) o Antispasmodics -diazepam, baclofen for skeletal mm spasm -buscopan for smooth mm spasm o Cannabinoids (I -? ) © Eric J. Visser 2017 UNDA. All rights reserved 19
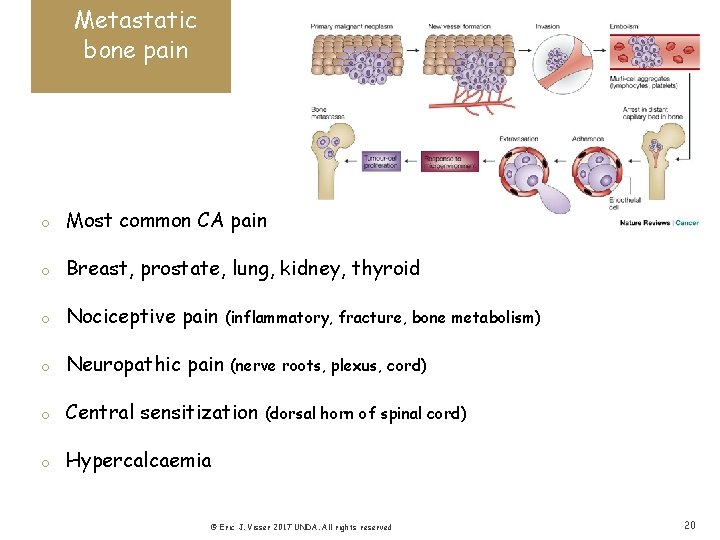
Metastatic bone pain o Most common CA pain o Breast, prostate, lung, kidney, thyroid o Nociceptive pain o Neuropathic pain o Central sensitization o Hypercalcaemia (inflammatory, fracture, bone metabolism) (nerve roots, plexus, cord) (dorsal horn of spinal cord) © Eric J. Visser 2017 UNDA. All rights reserved 20
Metastatic bone pain management o Cancer care o Multimodal analgesia o Opioids o Paracetamol o NSAIDs & COX-2 inhibitors o Bisphonates (calcitonin not effective) -first line, very effective (I+) - bone pain (days to weeks) - bone osteoclast activity ( fracture & Ca++) © Eric J. Visser 2017 UNDA. All rights reserved 21
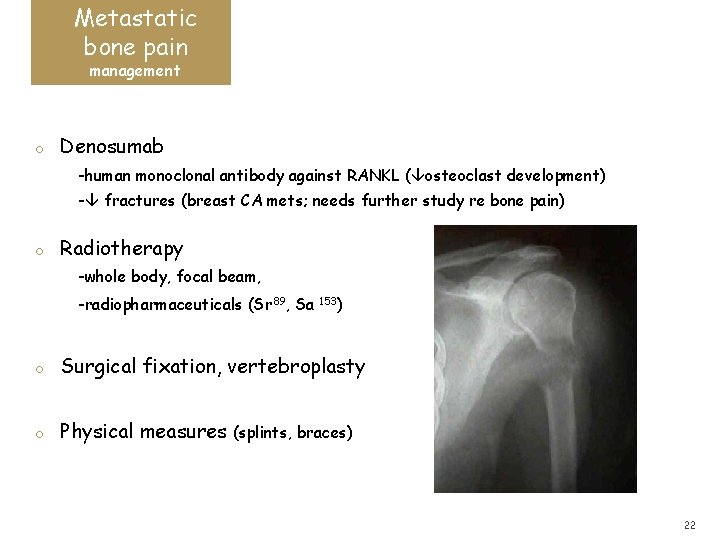
Metastatic bone pain management o Denosumab -human monoclonal antibody against RANKL ( osteoclast development) - fractures (breast CA mets; needs further study re bone pain) o Radiotherapy -whole body, focal beam, -radiopharmaceuticals (Sr 89, Sa 153) o Surgical fixation, vertebroplasty o Physical measures (splints, braces) 22
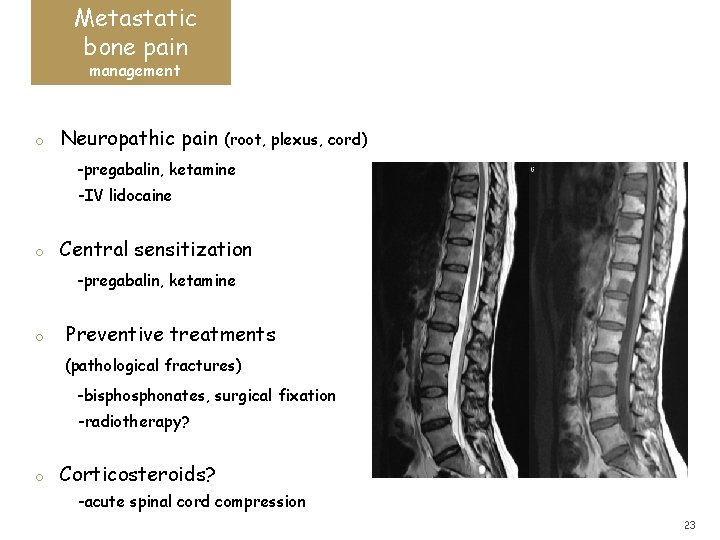
Metastatic bone pain management o Neuropathic pain (root, plexus, cord) -pregabalin, ketamine -IV lidocaine o Central sensitization -pregabalin, ketamine o Preventive treatments (pathological fractures) -bisphonates, surgical fixation -radiotherapy? o Corticosteroids? -acute spinal cord compression 23

Mucositis pain o Painful inflammation & ulceration of (high cell-turnover) mucous membranes due to chemo or radiotherapy o Acute nociceptive & neuropathic pain o Lasting days to weeks o Extremely painful o Significant psychological distress o Children © Eric J. Visser 2017 UNDA. All rights reserved 24
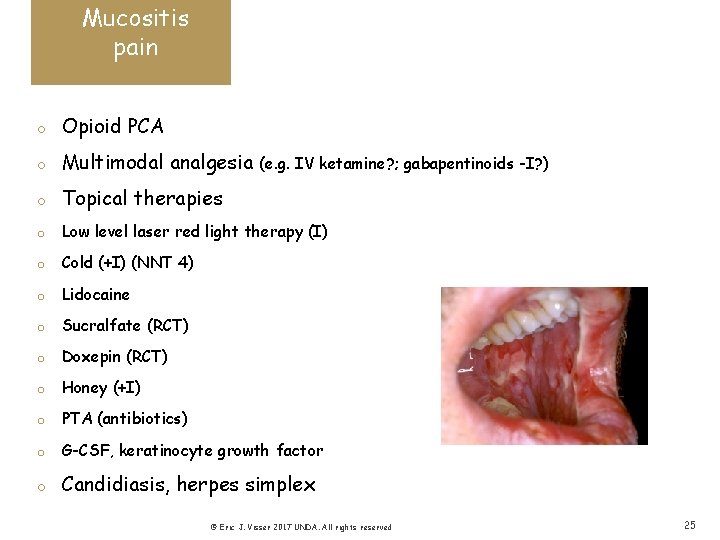
Mucositis pain o Opioid PCA o Multimodal analgesia o Topical therapies o Low level laser red light therapy (I) o Cold (+I) (NNT 4) o Lidocaine o Sucralfate (RCT) o Doxepin (RCT) o Honey (+I) o PTA (antibiotics) o G-CSF, keratinocyte growth factor o Candidiasis, herpes simplex (e. g. IV ketamine? ; gabapentinoids -I? ) © Eric J. Visser 2017 UNDA. All rights reserved 25
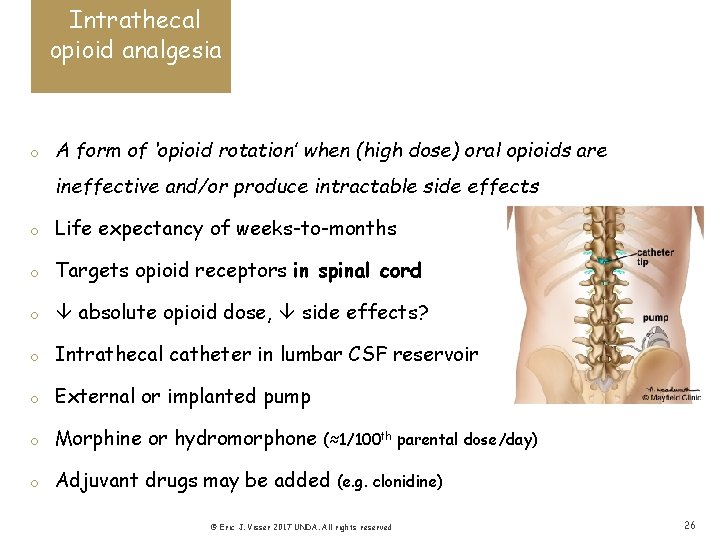
Intrathecal opioid analgesia o A form of ‘opioid rotation’ when (high dose) oral opioids are ineffective and/or produce intractable side effects o Life expectancy of weeks-to-months o Targets opioid receptors in spinal cord o absolute opioid dose, side effects? o Intrathecal catheter in lumbar CSF reservoir o External or implanted pump o Morphine or hydromorphone o Adjuvant drugs may be added (≈1/100 th parental dose/day) (e. g. clonidine) © Eric J. Visser 2017 UNDA. All rights reserved 26
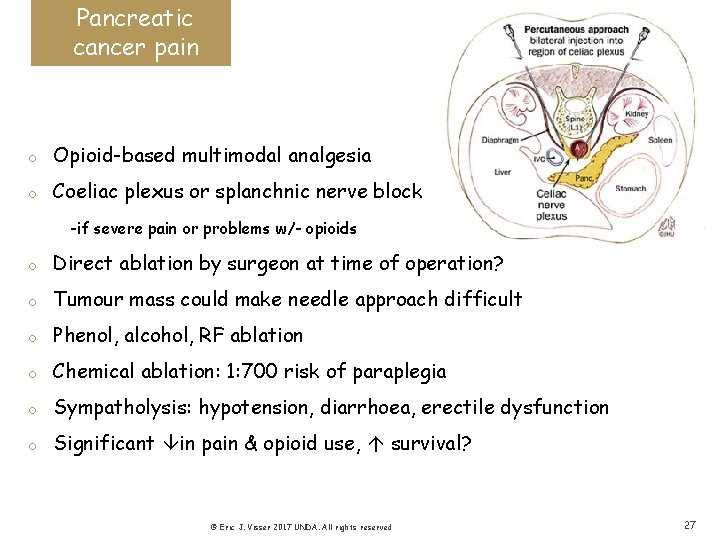
Pancreatic cancer pain o Opioid-based multimodal analgesia o Coeliac plexus or splanchnic nerve block -if severe pain or problems w/- opioids o Direct ablation by surgeon at time of operation? o Tumour mass could make needle approach difficult o Phenol, alcohol, RF ablation o Chemical ablation: 1: 700 risk of paraplegia o Sympatholysis: hypotension, diarrhoea, erectile dysfunction o Significant in pain & opioid use, survival? © Eric J. Visser 2017 UNDA. All rights reserved 27
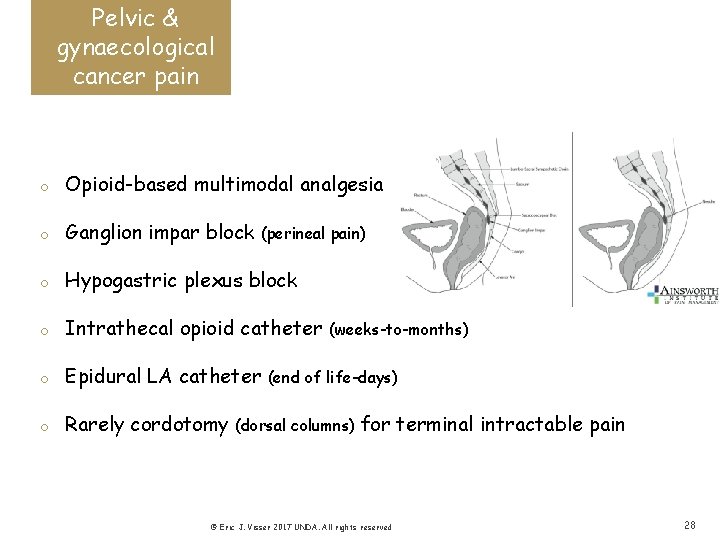
Pelvic & gynaecological cancer pain o Opioid-based multimodal analgesia o Ganglion impar block o Hypogastric plexus block o Intrathecal opioid catheter o Epidural LA catheter o Rarely cordotomy (perineal pain) (weeks-to-months) (end of life-days) (dorsal columns) for terminal intractable pain © Eric J. Visser 2017 UNDA. All rights reserved 28

Chronic pain after breast cancer o Mastectomy ~50% o Breast conserving surgery ~50% o Abnormal sensory (neuropathic) symptoms ~80% o Phantom breast pain ~5 -10% Meretoja, Tuomo J. , et al. "Pain at 12 months after surgery for breast cancer. " JAMA 311. 1 (2014): 90 -92; Gartner R et al. JAMA 2009.
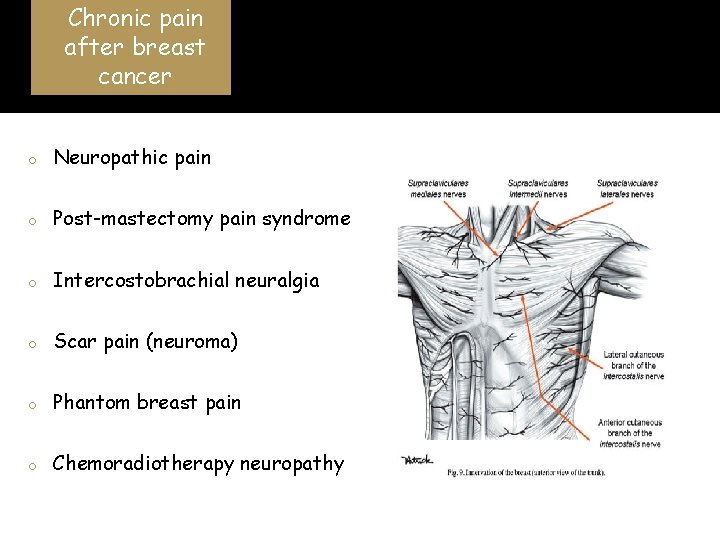
Chronic pain after breast cancer o Neuropathic pain o Post-mastectomy pain syndrome o Intercostobrachial neuralgia o Scar pain (neuroma) o Phantom breast pain o Chemoradiotherapy neuropathy
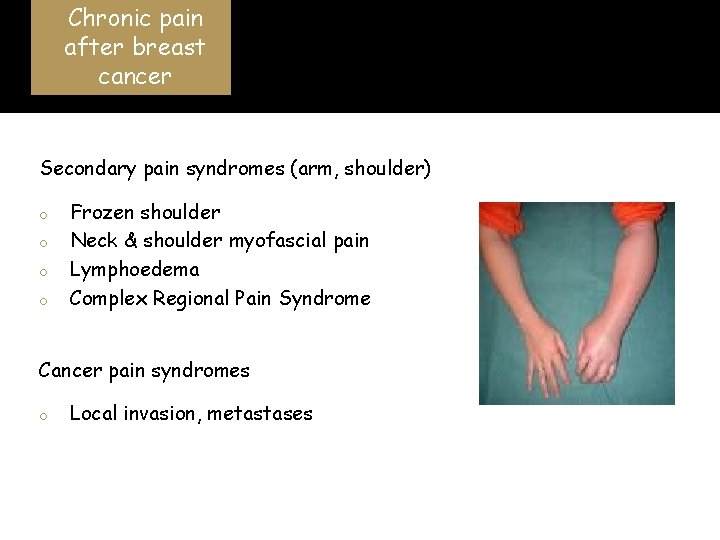
Chronic pain after breast cancer Secondary pain syndromes (arm, shoulder) o o Frozen shoulder Neck & shoulder myofascial pain Lymphoedema Complex Regional Pain Syndrome Cancer pain syndromes o Local invasion, metastases
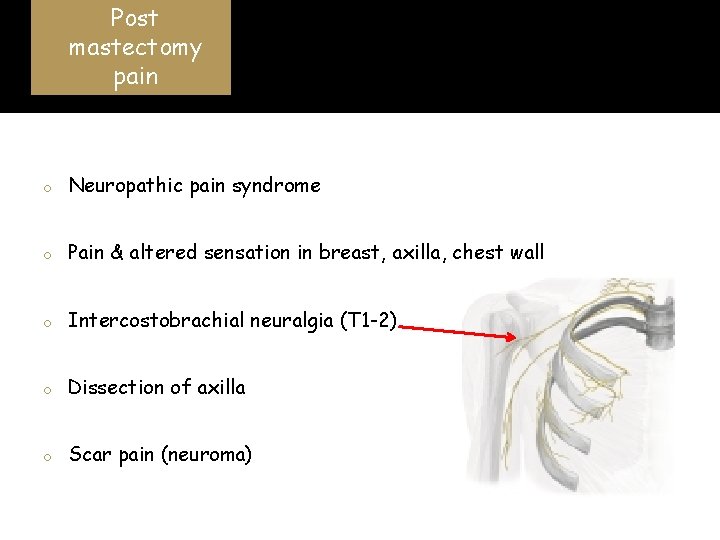
Post mastectomy pain Jung BF et al. Pain 2003 o Neuropathic pain syndrome o Pain & altered sensation in breast, axilla, chest wall o Intercostobrachial neuralgia (T 1 -2) o Dissection of axilla o Scar pain (neuroma)
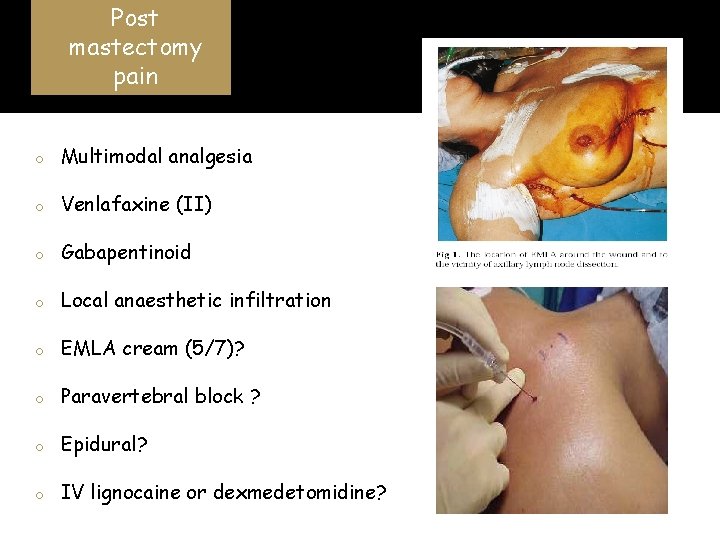
Post mastectomy pain o Multimodal analgesia o Venlafaxine (II) o Gabapentinoid o Local anaesthetic infiltration o EMLA cream (5/7)? o Paravertebral block ? o Epidural? o IV lignocaine or dexmedetomidine?

Other CA pain strategies o Physical o TENS (positioning, massage, TENS) Complementary o Aromatherapy o Acupuncture Psychosocial o Angst, depression o Relaxation, mindfulness o Sleep Spiritual © Eric J. Visser 2017 UNDA. All rights reserved 34

Pain & suffering in cancer o Pain is ‘an unpleasant sensory and emotional experience… …associated with perceived tissue damage’ o Suffering? o An overwhelming sense of helplessness & hopelessness o Pain in the context of cancer… o Seen as an existential threat from which there’s no escape o CA pain leads inevitably to suffering o Control, self determination, hope © Eric J. Visser 2017 UNDA. All rights reserved 35
- Slides: 35