Approach to patients with Dyspnea Dr Hadil Al



























- Slides: 42

Approach to patients with Dyspnea Dr. Hadil Al Otair MRCP, FCCP

Dyspnea • Definition: An unpleasant or uncomfortable awareness of breathing.

• Outline: - Control of breathing - Causes of acute dyspnea & their clinical features - Causes of chronic dyspnea - Investigations for chronic dyspnea

Dyspnoea An unpleasant or uncomfortable awareness of breathing Ability to breathing ↑Demand

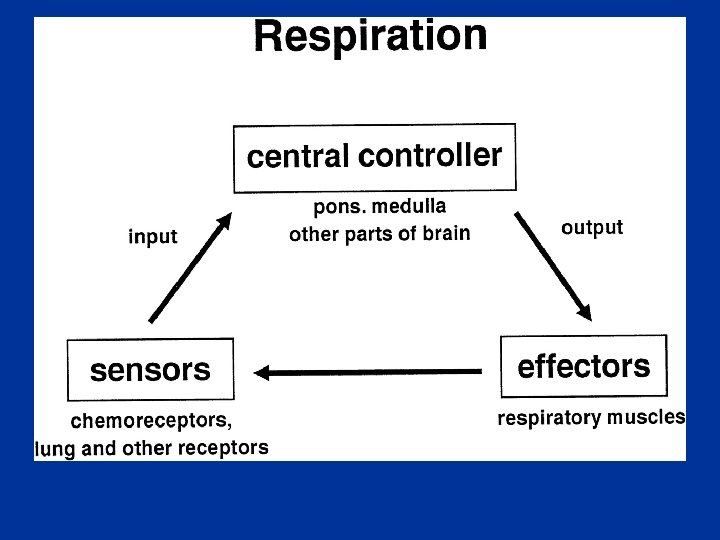
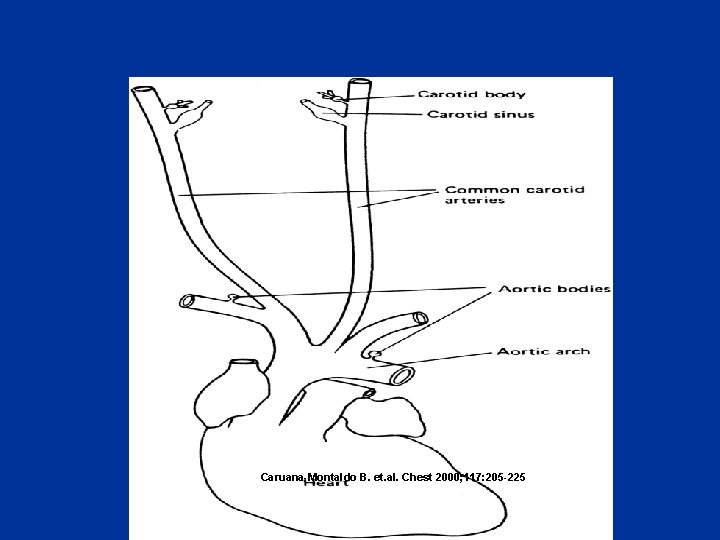
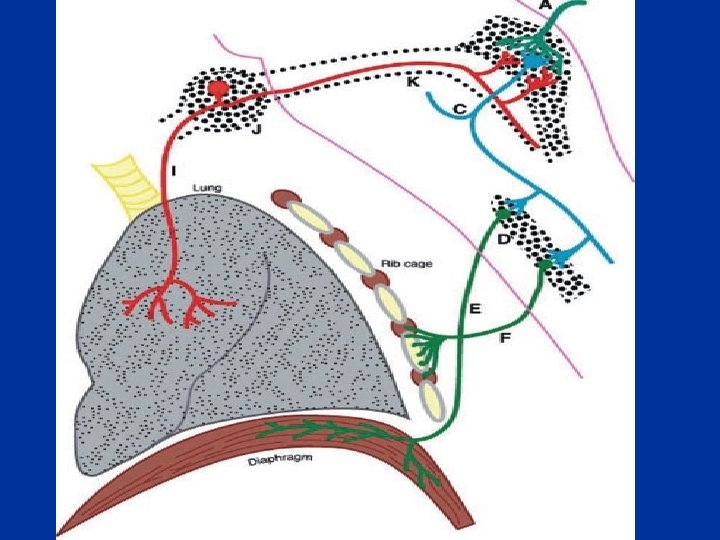
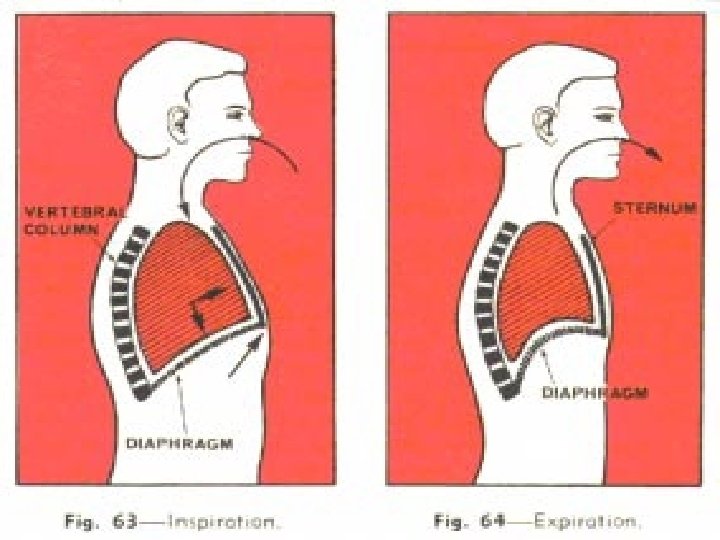
Control of breathing • Afferent (sensory ) information Chemoreceptors: Central (medulla) Peripheral (Carotid &Aortic bodies) Mechanoreceptors (Airways , lungs, chest wall) • Respiratory control system • Efferent respiratory discharges to ventilatory muscles


Caruana-Montaldo B. et. al. Chest 2000; 117: 205 -225




Factors Causing sensation of dyspnea • Chemicals: - Hypoxemia - Hypercapnea - Acidosis • Vascular: - Pulmonary Artery (PHT) - Ventricle Pressure (CHF) • Chest Wall & Neuro-muscular : - Guillen-Barre - Kyphoscoliosis • Inflation & Deflation receptors in Airways. - Asthma - COPD - IPF

CARDIAC • Pulmonary edema • Cardiac tamponade PULMONARY • Pulmonary embolism • Pneumothorax • Acute asthma • Aspiration syndrome • Fat embolism • Amniotic fluid embolism • Inhalation injury (co-poisoning) • Upper airway obstruction • Anaphylaxis • Traumatic


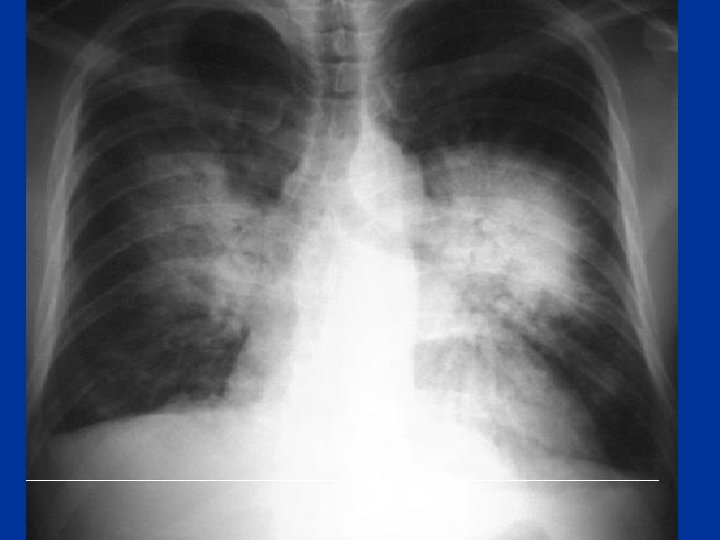
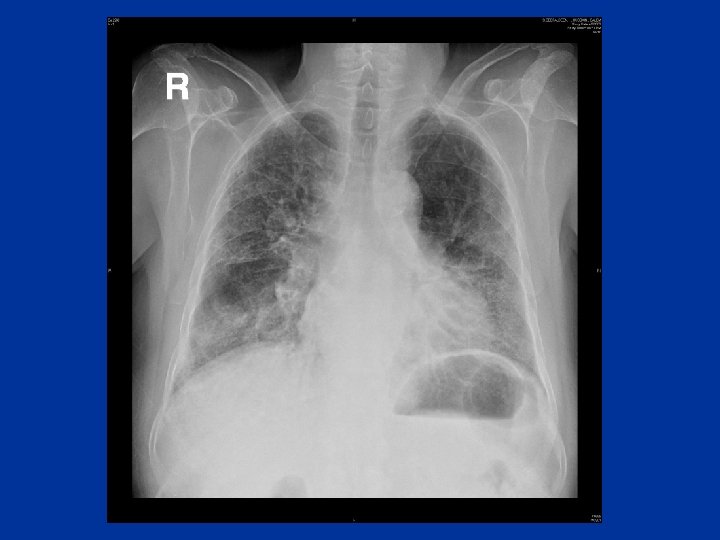
Pulmonary Edema Risk factors: • Smoking • HTN-DM, lipid • Gallop rhythm • ECG, CE • Murmur • Chest x-ray or prior H/O • heart cocaine • LL use • Edema • H/O rheumatic heart disease Symptoms: • Orthopnea, PND’s • Assoc. chest pain • Palpitations • Sweating JVP • Bibasilar crackles

Acute Asthma • Known asthmatic • Tachypnea • CXR • H/O atopy • Tachycardia • PFT • Preceeding URTI • Wheezes • Symptoms: wheezes • Pulsus paradoxus

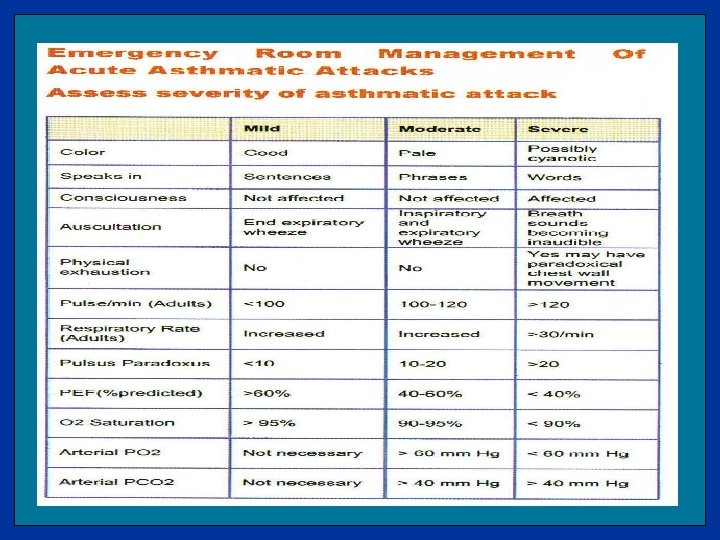
Management of Acute Asthma Assessment of attack severity. Clinical Findings. Peak Flow Measurement. Arterial Blood Gases EAR Early Asthmatic Response 30 min – 4 H LAR Late Asthmatic Response 3 H – 12 H




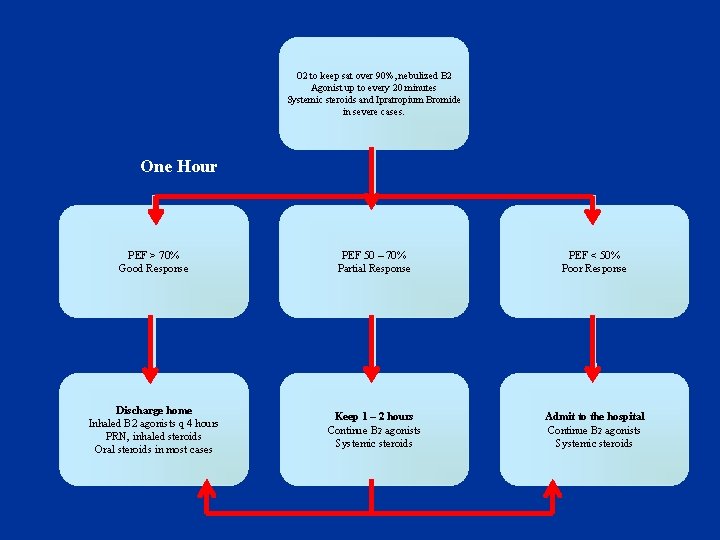
O 2 to keep sat over 90%, nebulized B 2 Agonist up to every 20 minutes Systemic steroids and Ipratropium Bromide in severe cases. One Hour PEF > 70% Good Response PEF 50 – 70% Partial Response PEF < 50% Poor Response Discharge home Inhaled B 2 agonists q 4 hours PRN, inhaled steroids Oral steroids in most cases Keep 1 – 2 hours Continue B 2 agonists Systemic steroids Admit to the hospital Continue B 2 agonists Systemic steroids

Patients at risk of developing severe or fatal asthma: . Previous life-threatening attacks Severe disease Hospital admission during the previous year One or more emergency room visits in the last year Patients’ noncompliance Psychosocial problems Three or more categories of antiasthmatic drugs prescribed Discontinuity of medical care

Life threatening Asthma Patterns of Fatal Asthma: 1) Acute on Chronic Asthma 2) Hyper Acute Asthma Clinical Findings: • Silent Chest • Cyanosis • Exhaustion • Bradycardia • Hypotension • PFR < 30%

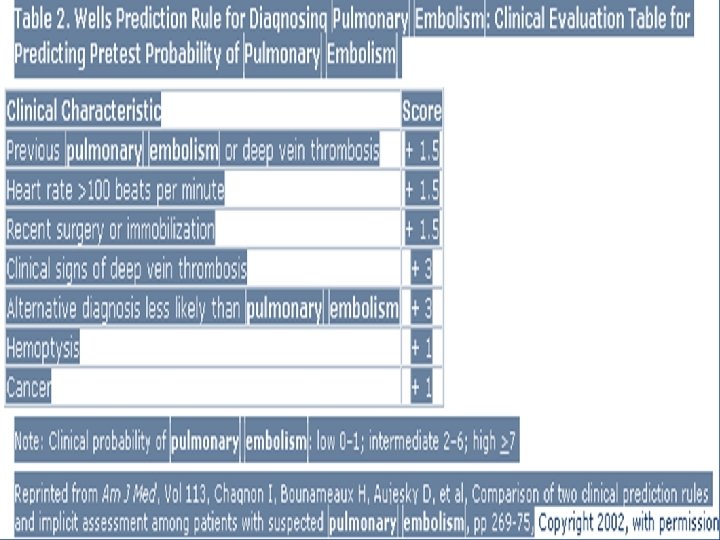
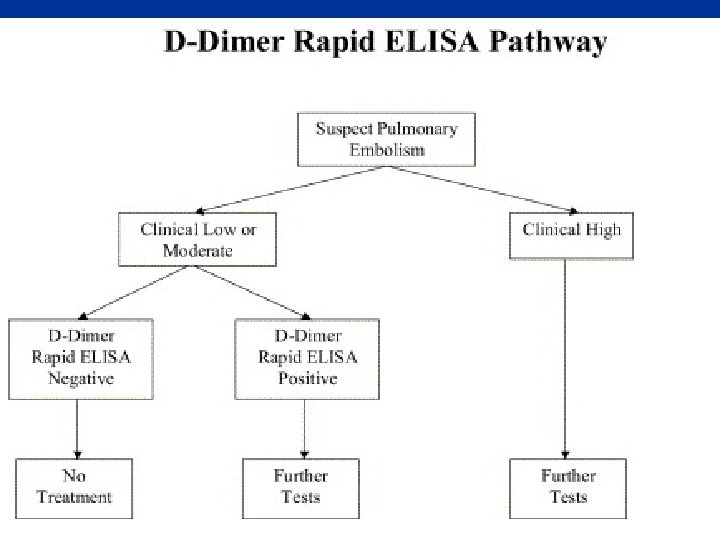
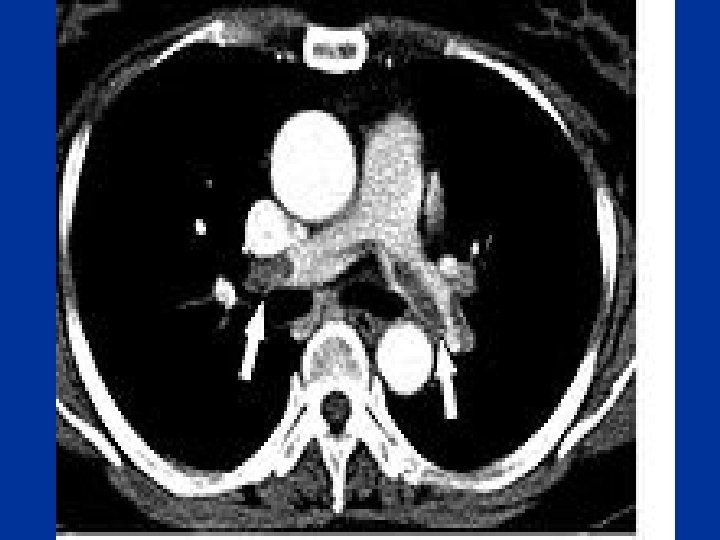
PULMONARY EMBOLISM • • • Risk factors Presenting Symptoms Physical Findings Investigations Therapy

Pulmonary Embolism Risk factors: • H/O hypercoagulable • tachycardia disorder, recent DVT • Tachypnea • Surgery, immobility • Loud P 2 • cancer • Pleural effusion • Symptoms: pleuritic • Acute Cor Pulmonale Chestpain, SOB • hypotension • hymoptysis • ABG • CXR • ECG • VQ • Spiral CT • Doppler LL




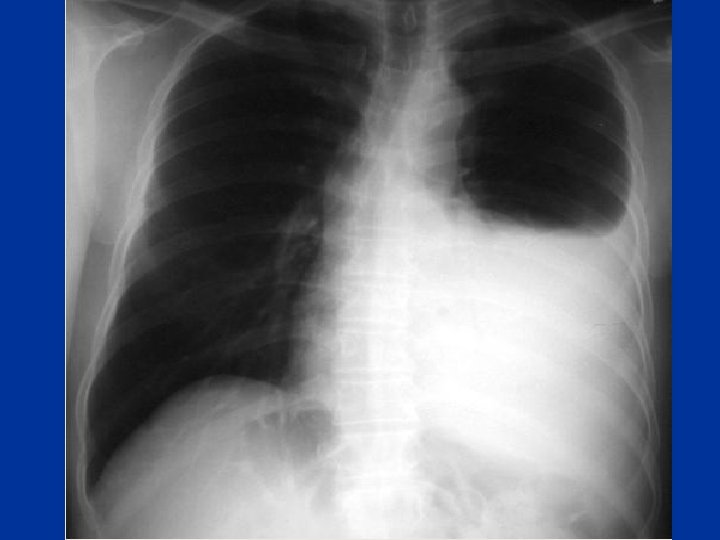
Pneumothorax • tall, thin, young patient. H/O pleural aspiration or biopsy • Symptoms: wheezes • one hemithorax • Hyperinflated • Hyperresonance • ↓ breath sounds • Trachea + mediastinal shift • CXR esp • exp. film


Pneumothorax • Major Types: • Spontaneous: Primary peak 20 -30 yrs, 4: 1 male : female • Tall thin , cigarette smokers, positive family history Secondary: Parenchymal lung disease e. g sarcoidosis, IPF, Emphysema, Necrotising pneumonia incl. Tb, PCP, • Iatrogenic: Pleural tap, transbronchial lung biopsy, positive pressure ventilation. • Traumatic: Rib fracture, bronchial rupture, esophageal rupture

Pneumothorax Mechanism • rupture of subpleural bleb or parenchymal process eroding visceral pleura this may also cause partial bronchial obstruction(check -valve mechanism) & hyperinflation

Complications • Tension Pneumothorax When significant positive pressure in the pleural space results in severe compression of ipsilateral lung, contralateral shift of the mediastinum • Results from one way valve mechanism • how to diagnose ? • What to do?

Pneumothorax management • Observation: in small pneumothorax(<15%) primary , spontaneuos or iatrogenic not ventilated • Oxygen; Increase the pressure gradient between pleural space&capillaries by decreasing partial pressure of nitrogen • chest tube • thoracotomy

• Recurrence: 10 -50% • 60% after the second recurrence • Sclerotherapy, Thoracotomy

Fat Embolism • Trauma • Long bone fracture Non-specific • ↓ level of consciousness • urine fat • petechial rash Amniotic Fluid Embolism • CXR • Prolonged labour • PROMAmniotic Fluid Assisted labour Non-specific • CXR

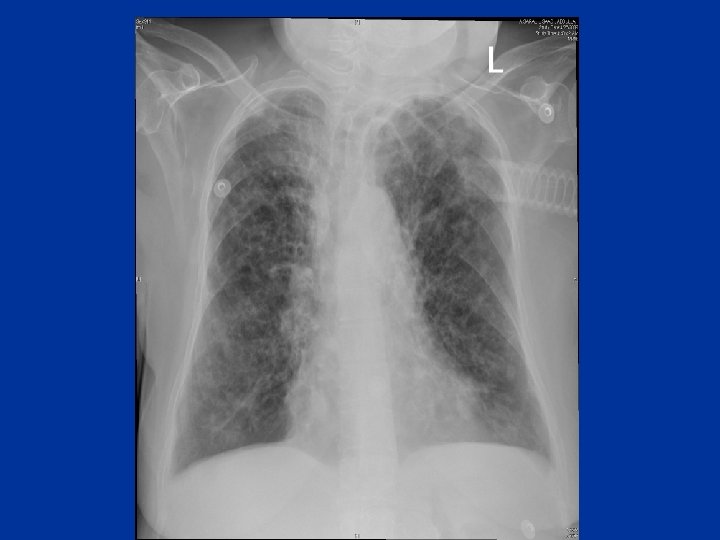
Chronic dyspnea • Major causes: Asthma COPD Bronchiectasis Interstitial lung disease Heart failure or cardiomyopathy

Evaluation • • • History& physical exam CXR PFTS Oximetry Echocardiogram CT-lungs - I. L. D _ Bronchiectasis - Occult emphysema - Chronic thromboembolic dis. • Cardiopulmonary exercise





THANK YOU