Respiratory Distress Syndrome By Nicole Stevens Neonates Respiratory

Respiratory Distress Syndrome By: Nicole Stevens

Neonates Respiratory System Differs from an older child/adult: • Number and development of alveoli • Structure of lung tissue and airways • Shape and composition of rib cage, diaphragm and musculature • O 2 consumption • Lung volumes • Pulmonary surfactant system • Respiratory control

Objectives • • • Define RDS Incidence of RDS Risk factors Factors that reduce risk Pathophysiology of RDS

Definition of RDS is a developmental disorder of the preterm lung, in which the primary defect appears to be the lack of surfactant • Also known as hyaline membrane disease (HMD) • Inversely related to gestational age • Onset shortly after birth, progresses in severity in first 24 – 48 hrs, most survivors show rapid improvement after 3 – 5 days, with a resolving of symptoms by 1 week. •

Incidence of RDS • • • The most significant disorder affecting newborn premature infants Affects about 14% of all low birth weight infants 60% of < 28 wks 30% of 28 – 34 wks 5% of 34 wks - term 10 – 20% mortality

Risk Factors • • Prematurity Low birth weight Caucasian Male babies (2: 1) Previous baby with RDS Perinatal asphyxia Cold stress Perinatal infection (chorioamnioitis)

Risk Factors • • • Multiple births (often premature, 2 nd twin greater risk) Patent ductus arteriosus Caesarean section (without labour) Secondary Surfactant Deficiency IDM Meconium aspiration syndrome Pulmonary Infections Asphyxia Pulmonary haemorrhage

Factors that decrease risk • • • Antenatal steroids: accelerate fetal lung maturity by increasing formation and release of surfactant Maternal hypertension Prolonged rupture of membranes Maternal narcotic abuse Placental insufficiency STRESSED BABIES RELEASE SURFACTANT

First Breath At birth, liquid is substited by gas to expand alveoli • Once the alveoli are open a film of surfactant stabilises the alveoli • First breath requires high opening pressures • Less pressure is required with subsequent breaths to achieve a similar volume (less effort is required) •

Pathophysiology of RDS • Stucturally immature lungs (less alveoli) • Decreased compliance • Decreased pulmonary vasculature • Inadequate surfactant

Pathophysiology of RDS A thin layer of water coats each of the alveoli and protects the living tissue underneath • This creates an extensive air-water interface within the lung cavity, and the surface tension of the water tends to collapse the lung if there is no surfactant present • Surfactants in general simply refer to molecules that preferentially migrate to an air-water interface (or surface) • Water wants to pull together and surfactant wants to disperse/ or push the walls apart •

Surfactant is produced by the type II pnuemocytes beginning at 24 -28 wks and continuing to term • These cells synthesize, store, secrete and recycle surfactant • When the lungs are inflated, receptors in the pnuemocytes mobilise surfactant into the air space • The slippery surfactant coats the lining of the alveoli and enables them to expand, contract and re-expand •

Pathophysiology • Collapse of small air sacks into large air sacks creating a mixture of: • Atelectasis and over distension • Poor alveolar stability • Surfactant deficiency decreases lung compliance • Increases work of breathing • Reduces functional residual capacity (FRC)

Pathophysiology • Surfactant defiency promotes collapse of terminal airways: Airways collapse results in poorly ventilated air sacs • Oxygen molecules continue to be extracted from air sacs in capillary network surrounding air sacs but are not replaced at normal rate • Pa. O 2 in air sac drops creating alveolar hypoxia •

Pathophysiology • Capillary network surrounding air sac sensitive to air sac PAO 2 • Capillary vasoconstriction Diversion of blood away from air sacs Right to left ‘shunt’ Tissue hypoxia • • •

Pathophysiology • Co 2 excretion dependent on the number of normally functioning air sacs available for gas exchange. Airway collapse results in poorly ventilated air sac • Reduced CO 2 exchange • CO 2 retention with hypercarbia •

Patholophysiology • RDS is an inflammatory disease • WBC migrate into airways and air sacs • Inflammatory mediators activated • Increased capillary permeability

Pathophysiology • Cells become more permeable, fluid leaks out of capillaries and into interstitial spaces leading to hypovolemia. • Hypovolemia leads to pulmonary constriction and hypo-perfusion which aids in diminishing surfactant. • Atelectasis causes V/Q mismatch and leads to hypo-ventilation and hypercapnia.

Pathophysiology • Generalised body disturbances occur: • Hypotension • General oedema • Renal insufficiency • Myocardial insuffiency

Recovery • Usually heralded by diuresis: • Usually starts after 48 hours of age Oxygen requirements decline rapidly after 72 hours Oxygen usually may be disconnected after 7 days In the VLBW / ELBW may be protracted course Can lead to CLD • •

Clinical Manifestations • Infants with RDS present with 5 cardinal signs: • Tachypnoea (>60/min, shallow, rapid) Nasal flarring (50% airway resist in nose and pharynx) Grunting (delayed expiration, maintains FRC) Retractions (subcostal, substernal, intercostal) Cyanosis accompanied by increasing oxygen requirements. • •

Investigations �Chest Xray �Blood Gases �Blood Cultures: FBE, U&E, TBG

Nursing Management �Resuscitation �Respiratory support �Surfactant Replacement therapy �Sweet (IVT 10%Dextrose) �Warm (Radiant heater/isolette) �Pink (Well oxygenated/Sa. O 2 monitoring) �Calm (Minimal Handling)

Management Monitoring (HR/RR/T/Sa. O 2/BP) Investigations (Bloods & CXR) Thermoregulation Fluids & Nutrition (IVT & Nil Orally) Oxygenation (Target Sa. O 2’s) Airway Management Correct biochemical imbalances Fluid Balance (wt nappies) Haematology Infection (IV Anti’s) Minimal Handling Positioning (Prone) Developmental Care Family Centred Care

CPAP �Prevents atelectasis �Reduces pulmonary Oedema �Shifts infant to breathe on more compliant portion of pressure volume curve

Mechanical Ventilation �Indications: �PCO@ >55 or rapidly increasing/ p. H <7. 25 �PO 2 <50 with Fi. O 2 >0. 6 -1. 0 (*Hospital Policy) �Impending Respiratory Failure �Risks of intubation and barotrauma considerable

Surfactant Replacement Therapy �Developed in the 1960’s �Derived from animal sources (survanta) or Artificial (Exosurf) �Prevents/treats a surfactant deficiency

When is Surfactant Used �Infants with RDS (clinical or radiological) �Infants requiring assisted ventilation �Infants requiring oxygen �Surfactant ONLY is delivered via the ETT

Actions of Surfactant Replacement Therapy � Decreases surface tension � Increases lung compliance � Prevents atelectasis � Decreases risk of death � Decreases risk of pulmonary air leak � *Surfactant has a dramatic response - within minutes with the need for oxygen & pressures to be weaned quickly

Risks of Surfactant Replacement Therapy �Can block ETT �Airleak Syndrome �Infection �Intracranial Haemorrhage (massive swings in BP) �Hypertension/hypotension �Hypercapnea / hypocapnea �Condition instability

Surfactant Replacement Therapy �When: Prophylaxis (prevention) V’s Treatment (rescue); Early V’s Late �What: Synthetic preparation (Exosurf) V’s Mixed Natural/Synthetic (Survanta) Curosurf �How: Administration ; indications, dosage, technique

Complications of RDS �Acute (Complications of treatment) ◦ Pneumothorax ◦ Pulmonary interstitial emphysema ◦ Sepsis ◦ Tube incidence ◦ Ducts can open �Chronic ◦ Retinopathy of Prematurity (ROP) ◦ Chronic Lung Disease (CLD) ◦ Neurological Impairment ◦ Hearing / visual impairment
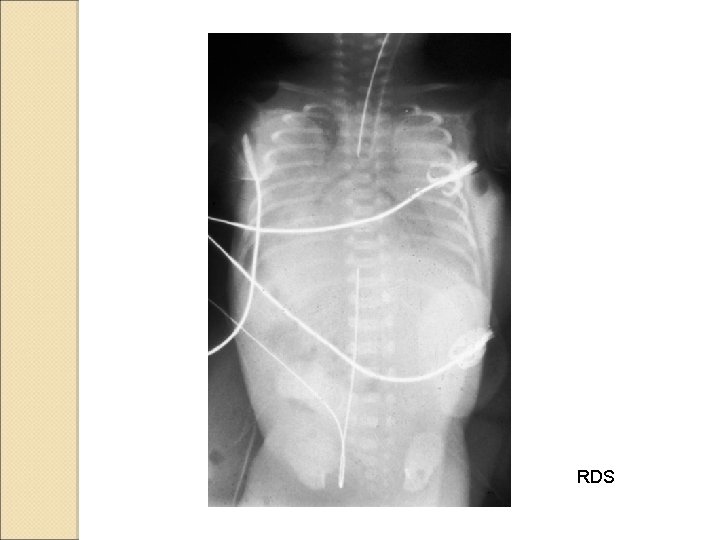
RDS
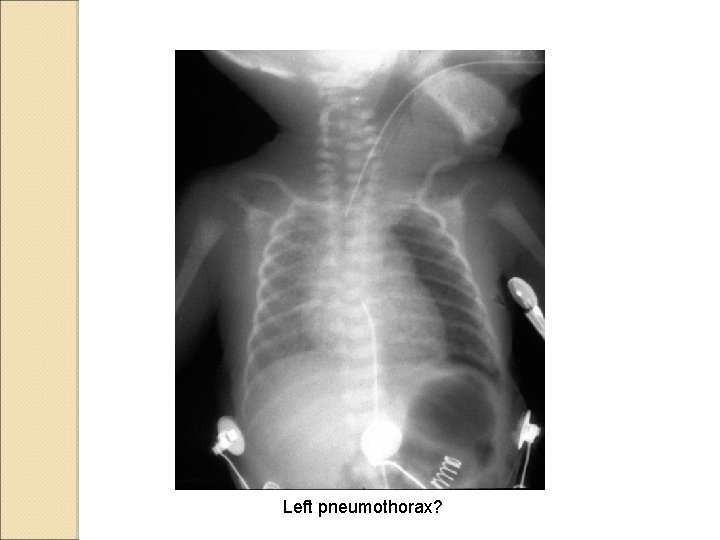
Left pneumothorax?
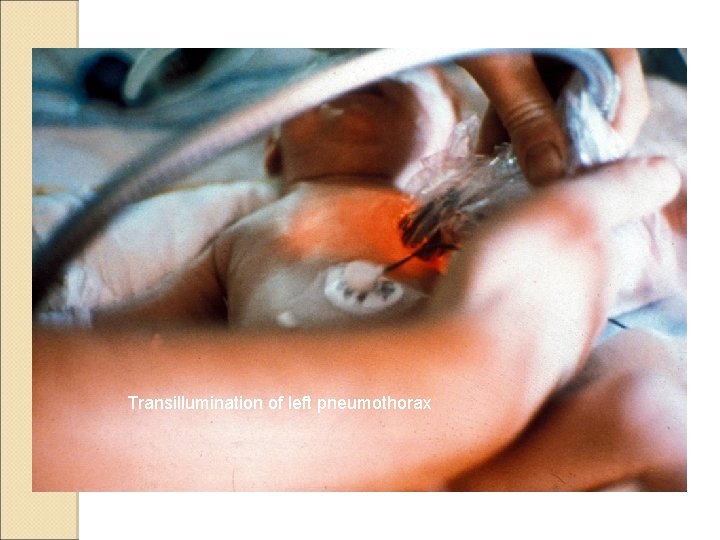
Transillumination of left pneumothorax
- Slides: 35