Implementation Science for Health Disparities Research Melody Eide










































- Slides: 50

Implementation Science for Health Disparities Research Melody Eide, MD MPH December 8 th, 2015 1

Disclosure of Conflict of Interests I have no disclosures of relationships with industry 2

“A little knowledge that acts is worth infinitely more than much knowledge that is idle. ” - Kahlil Gibran 3

Objective To define the emerging field of Implementation Science and its application to health disparities research 4

Health Disparities § Health Disparities – Population-specific differences in the presence of disease, health outcomes or access to healthcare (HRSA) 5

Health Inequities-broadly defined 1. Race/ethnicity • Infant mortality • African Americans 2 x fold higher rate • Diabetes-related mortality • Hispanics and American Indians 2 x as likely to die • Cancer • Vietnamese women 5 x higher rate of cervical cancer 2. Socioeconomic Status, Income, Education - Highest poverty groups suffer poorest health status indicators - and lowest screening rates 3. 4. 5. 6. 7. Health literacy/numeracy and resources (computer) Immigration status By co-morbid conditions Geographical locations (e. g. , rural) Other 6

Health Disparities § These inequities have a wide source of origins and potential remedies § To begin to eliminate, we must address potential contributions from differences in Health care § Quality § Access § Costs § Outcomes & Satisfaction § Perceptions and Perspectives of care (cultural values) 7

Health Disparities § The status quo in areas of inequity must be challenged § Healthcare benchmarks in the US needs to reflect that equity is achievable Sickle cell survival to age 5 » US: >95% » Sub-Saharan Africa: 2% 8

Health Disparities § Health Disparities Research Collaborators: you have risen to the challenge of defining and addressing these inequities § Populations most in need may be harder to reach and require more thoughtful interventions to improve health outcomes/achieve equity § There is a gap between scientific discovery and population benefit - Gap is larger for medically underserved populations and can compound disparities - Implementation science can help bridge this gap 9

Implementation Science 10

Implementation Science is: § A systematic intervention process to adopt and integrate evidence-based healthcare innovations into usual care. Powell, Mc. Millen, Proctor et al. , Medical Care Research and Review, 2012 § The essential ingredient in the process of moving evidence-based medicine (EBM), empirically supported treatment (EST), quality initiatives (QI), health interventions and best practices into actual use. 11

Implementation “Strategies” … the ‘how to’ component of changing healthcare practice. … Key: How to make the “right thing to do” the “easy thing to do …Carolyn Clancy Canada: Referred to as “Knowledge Translation” 12

Definitions - D&I § Dissemination: An active approach of spreading evidence-based interventions to the target audience via determined channels using planned strategies. § Implementation: The process of putting to use or integrating evidence-based interventions within a specific setting. 13

Unraveling the “Black Box” Moving from passive to active D&I 14 Harris, Sidney. American Scientist, 1977

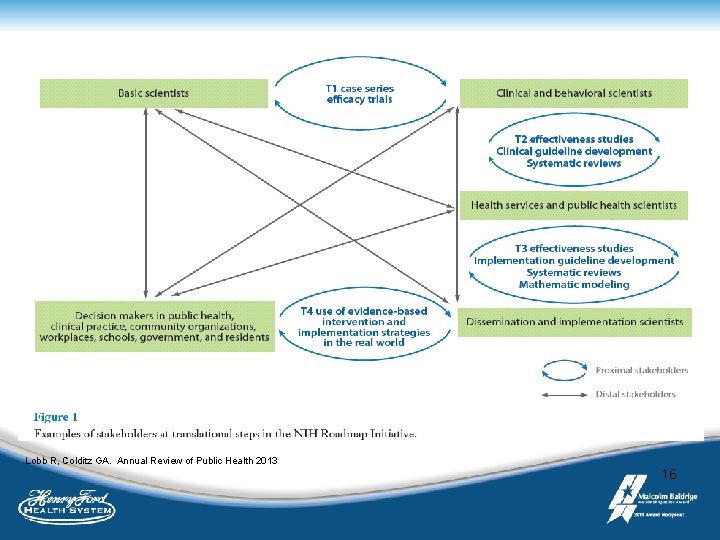
Phases of translational research T 1 studies: basic research science translated to humans T 2 studies: translate clinical application into evidence based guidelines T 2 research can do more to decrease morbidity and mortality than a new imaging device or a class of drugs Wolff, SH. The meaning of translational research and why it matters. 2008; JAMA, 299: 211 -213. T 3 studies: translate evidence-based guidelines into health and community practice ****Implementation Science**** T 4 studies: evaluate ‘real world’ health outcomes of a clinical application in practice Translational research is often depicted as linear but that may not be the best way to conceptualize 15

Lobb R, Colditz GA. Annual Review of Public Health 2013 16

Implementation Outcomes: Measure distinct from clinical outcomes Could have an effective intervention: Ø Not adopted Ø Poor penetration in health system Ø Implemented but with poor fidelity Ø Not sustained Implementation Science helps to ensure an effective intervention has its desired or intended result (efficacy) Adopted from Ross Brownson 17

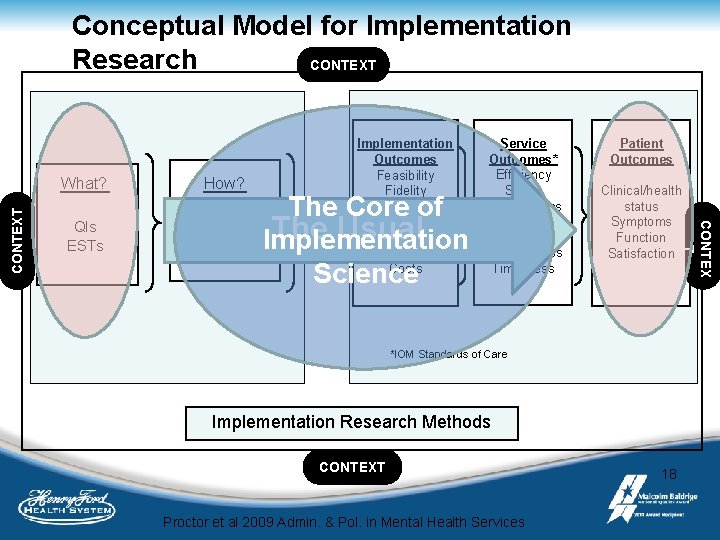
Conceptual Model for Implementation Research CONTEXT QIs ESTs How? The Core of Implementation. The Usual Strategies Implementation Science Service Outcomes* Efficiency Safety Effectiveness Equity Patientcenteredness Timeliness Patient Outcomes Clinical/health status Symptoms Function Satisfaction CONTEX T CONTEXT What? Implementation Outcomes Feasibility Fidelity Penetration Acceptability Sustainability Uptake Costs *IOM Standards of Care Implementation Research Methods CONTEXT Proctor et al 2009 Admin. & Pol. in Mental Health Services 18

Key Characteristics in Implementation Science Ø Ø Ø Ø Contextual Complex Multi-component programs and policies Non-linear Transdisciplinary Multi-level Addresses “wicked”, messy, important problems Glasgow RE, Steiner JF In: Brownson RC, Colditz G, Proctor E, eds. Dissemination and implementation research in health: Translating science and practice. New York: Oxford University Press, 2012: 72 -93 19

Key Characteristics of Implementation Science Glasgow, R. E. & Chambers, D. Clin Transl Sci 2012: 5, 48 -55 20

Why do we need Implementation Science? 21

The Gap: Scurvy http: //greas. ca/publication/pdf/melaniebarwickenglish. pdf 22

23

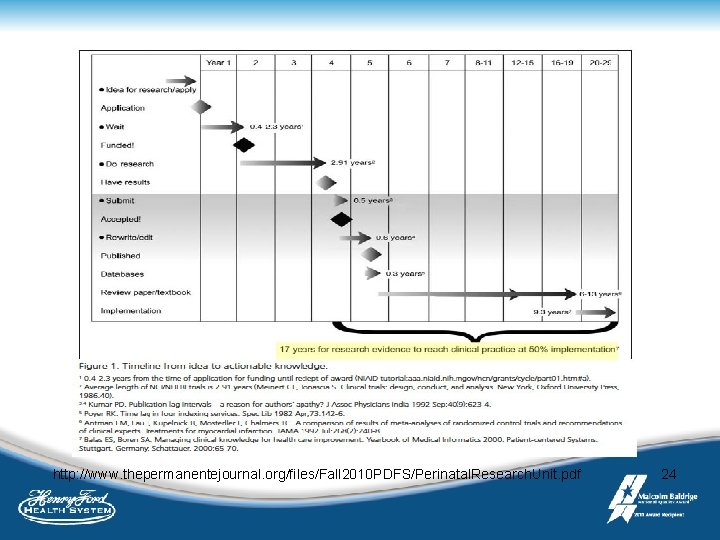
http: //www. thepermanentejournal. org/files/Fall 2010 PDFS/Perinatal. Research. Unit. pdf 24

Disparities in Healthcare § Evidence-based practices (EBP) frequently developed under traditional controlled, narrow conditions (efficacy focused rather than effectiveness). Traditionally… – – Differences in research participants minimized during sampling Participants with multiple health problems frequently excluded Cost of adopting a practice frequently not considered Language and culture may not be factored in § When the EBP gets to the real world, it may reach a very small proportion of those who need it. IMPLICATION: Using EBP’s without implementation science considerations frequently magnifies disparities 25

The promise of D&I research …there is still an enormous gap between what we know can maximize the quality of health care and what is currently being delivered in practice and community settings. …to optimize public health we must not only understand how to create the best interventions, but how to best ensure that they are effectively delivered within clinical and community practice. NIH, OBSSR 26

You have probably already used elements of Implementation Science in your Health Disparities Research. 27

Historical context (abbreviated) § Dissemination of innovation happens spontaneously, though not systematically, efficiently or equitably § Seminal article in 1943 on diffusion of hybrid seed corn in two Iowa communities – Key findings • Adoption as key dependent variable, change agents, importance of different communication channels 28

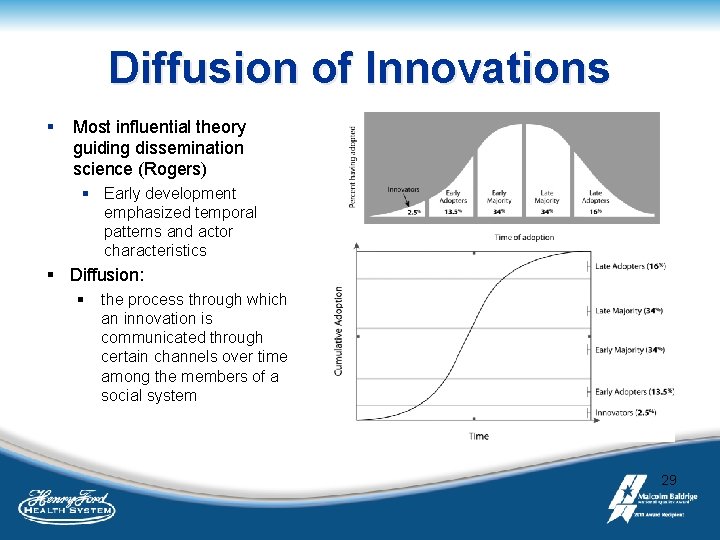
Diffusion of Innovations § Most influential theory guiding dissemination science (Rogers) § Early development emphasized temporal patterns and actor characteristics § Diffusion: § the process through which an innovation is communicated through certain channels over time among the members of a social system 29

Opportunities & Resources: Dissemination & Implementation Science to address Health Inequities 30

IS approaches § Models-lots! § Methods – Pragmatic studies – Practical measures & outcomes § Measures Evidence Integration Triangle 31

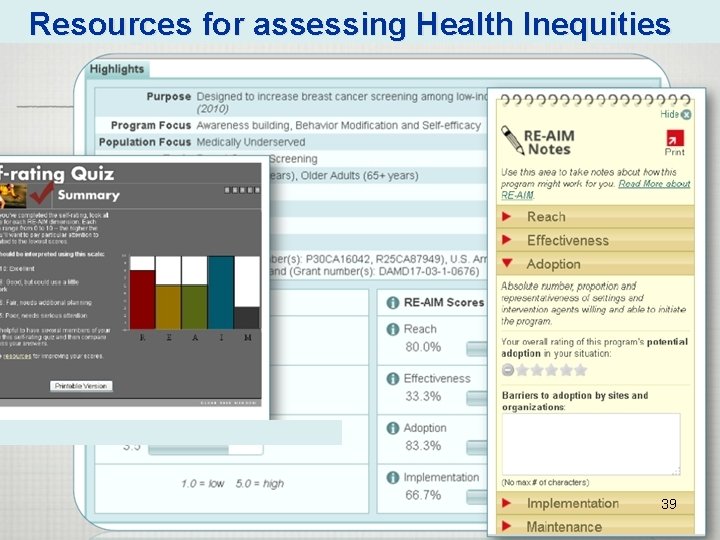
Resources for assessing Health Inequities 32

Resources for assessing Health Inequities 33

Considerations as you approach your next Grant or public health intervention 34

Make better use of models/frameworks § Outlined in Tabak et al. , proliferation of models: 61 reviewed ♦ Context is critical ♦ Begin with stakeholders—take their perspective ♦ Need balance between fidelity to EB program and adaptation to local setting ♦ Unlikely to need to create a new model 35

Well Recognized Models: RE-AIM To determine the characteristics of interventions that can: § Reach large numbers of people for most benefit & Effect § Be widely adopted by different settings § Be consistently implemented by staff members with moderate levels of training and expertise § Maintain: Produce replicable and long-lasting effects (and minimal negative impacts) at reasonable cost 36

RE-AIM: Disparities Implications RE-AIM ELEMENT Reach • • Characteristics of those who participate vs. decline Expand categories used for classification of potential disparities – e. g. , literacy, numeracy, address, geospatial Effectiveness • • • “Representative narrative” Impact of context Unanticipated consequences Adoption • • Engage stakeholders from low resource settings from outset Document and address reasons for non-participation Implementation • • • Monitor delivery Track costs of implementation Be transparent Maintenance • Assess long-term results of different subgroups… If inequities, find out why • Prepare delivery settings with tools to guide, monitor and adapt intervention • Support and study sustainability 37

The reality of translating an evidence-based (fill in blank) intervention ISSUE RE-AIM ELEMENT SUCCESS RATE POPULATIONWIDE IMPACT Settings that Participate ADOPTION 40% Patients Who Accept REACH 40% 16% Program Delivery IMPLEMENTATION 40% 6. 4% RCT Efficacy Results EFFECTIVENESS 40% 2. 6% Longer-term Effects MAINTENANCE (Individual Level) 40% 1. 0% www. re-aim. org Glasgow RE, et al. RE-AIMing Research for Application…J Am Bd Fam Phys 2006; 19(1): 11 -19 38

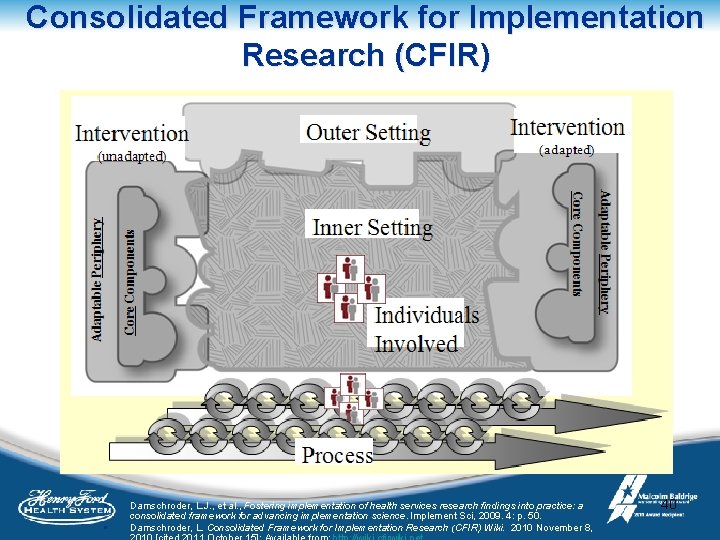
Resources for assessing Health Inequities 39

Consolidated Framework for Implementation Research (CFIR) § § Damschroder, L. J. , et al. , Fostering implementation of health services research findings into practice: a consolidated framework for advancing implementation science. Implement Sci, 2009. 4: p. 50. Damschroder, L. Consolidated Framework for Implementation Research (CFIR) Wiki. 2010 November 8, 40

Build more practice-based research “Where did the field get the idea that evidence of an intervention’s efficacy from carefully controlled trials could be generalized as THE best practice for widely varied populations and settings? ” --L. W. Green 41

Design for dissemination (D 4 D) § Some data from a national survey of 266 US researchers – 17% always/usually plan dissemination with some theory or framework – 32% always/usually provide shorter summaries – 34% always/usually involve stakeholders in D 4 D 42

Design for dissemination § Think about dissemination at the beginning of a research project – Systems changes • Shift funder, academic priorities/incentives – Processes • Engage stakeholders early and often – Products • Frame messages, develop brief summaries 43

Funding § Primary funders for D&I at NIH § § NCI NHLBI NIMH NIDDK § Grant trends § More applied research grants § PCORI influence? 44

NCI Implementation Science Studies 2002 -2012 Portfolio Analysis § 90 trans-NIH announcements § 67 funded grants (29 Trans-NIH PAR) § R 01= $89 M § Characteristics § Majority focused on prevention or screening § 26 - Tobacco § 20 – Colorectal cancer § IS Objectives § § 53 - implementation 31 - dissemination 26 - sustainability 20 - adoption 45 C. Vinson, NCI, June 2014

Areas Ripe for Exploration • Evidence-based Practice • Real-time feedback/monitoring • Sustainability in a Changing Context • Adaptability/Evolution over time • Impact of dissemination strategies on practice change • Scaling up practices across health plans, systems, and networks • De-Implementation/Exnovation • Adaptive designs (implementation as a step-wise approach) • Use of big data 46

Areas Ripe for Exploration § Studies needed which – Examine the utility of alternative dissemination strategies for service delivery systems targeting rural, minority, and/or other underserved populations – Explore methods for defining target audiences and packaging evidence for that specific population 47

Closing points 1. There are vast opportunities for D&I research in health disparities research. 2. Many theories/approaches are present with many overlapping constructs; utilize existing resources. 3. The messier the research topic, the lesser the amount of solid D&I research. The field is wide open 4. Design your studies with D&I in mind to stand out from the crowd 5. Let D&I guide you to your goal of making a difference 48

“To him/her who devotes his life to science, nothing can give more happiness than increasing the number of discoveries, but his/her cup of joy is full when the results of his/her studies immediately find practical applications. ” -- Louis Pasteur …. And overflowing, when those contributions level the playing field by improving health for all people regardless of starting point 49

Thank you Acknowledgements Enola Procter Ross Brownson Russ Glasgow Maria Hernandez Cynthia Vinson Fatima Ogaily MT-DIRC 50