End of Life Care in the ICU Goals




























- Slides: 29

End of Life Care in the ICU

Goals in Critical Care and Medicine • Save the lives of salvageable patients, restore health, relieve suffering and offer the dying a peaceful and dignified death. • Patients should expect excellence in all treatments, humanity and compassion, respect for autonomy.

End-of-life in the ICU Use of intensive care at the end of life in the U. S. RWJ ICU End-of-Life Peer Group. Crit Care Med 2004 – Projection: 540, 000 people die after receiving ICU care each year. Of hospital deaths, half associated with ICU – 1 in 5 Americans die in/after ICU hospitalization • Deaths in ICU: majority of deaths expected – >70% are preceded by withholding or withdrawing of life support – Intensivists actively manage deaths in ICU • Institute of Medicine – national priority • Society of Critical Care Medicine supports palliative model

Palliative Care • Patient and family-centered • Alleviate suffering caused by illness - control symptoms • Communicate effectively about appropriate goals of treatment • Promote concordance of treatment with patient preferences • Promote quality of life – Quality of life as the outcome rather than morbidity/mortality – Does not hasten or prolong death, affirms life

Quality of ICU Dying Experience Fixed patient characteristics: Clinical status, demographics Modifiable dimensions: Symptoms (pain), social/family support, spiritual, moment of death/autonomy Care system interventions: Aggressiveness, palliative, communication, social – dignity/respect Mularski. Crit Care Med 2006

What are appropriate measures for quality in EOL Care? • Outcome: – Utilization of ICU • SUPPORT Study – ICU length of stay – Mortality • Holloway, Quill. JAMA 2007 – Scoring, symptoms • Quality of Death and Dying: Crit Care Med 2004, Chest 2005 – Family satisfaction • JAMA 2004 • Process quality indicators: – Decision-making, communication – Symptom management

End-of-life care for the critically ill: a national intensive care unit survey Nelson et al. Crit Care Med 2006 Survey of 428 ICUs, 590 ICU directors Greatest Barriers to EOL Care • Unrealistic patient/family expectation • Lack of advance directives • Insufficient physician training in communication • Competing demands on physicians’ time • Suboptimal space for family meeting • Unrealistic MD expectations • Lack of palliative care service

End-of-life care for the critically ill: a national intensive care unit survey Crit Care Med 2006 Strategies to improve EOL care • Role modeling by experienced clinicians • Training in communication • Training in symptom management • Regular family meetings • Bereavement programs • End-of-life care quality monitoring • Access to palliative care, ethics consultants • Regular pastoral care visits

Clinical practice guidelines for support of the family in the patient-centered ICU: American College of Critical Care Medicine Task Force Crit Care Med 2007 • Families support shared decision-making • Recommend: – Shared decision-making – ICU team informs about status and prognosis – ICU team strive to understand wishes about lifesustaining therapies – Family meetings – Training in communication

Decision making depends on communication • Goal is to use patient preferences in order to establish goals of care • The physician must provide information about the illness, treatments, and prognosis • Decisions depend on the patient’s values attached to life-prolongation, functioning, and comfort

Communication with Family • Communication with family: informal, family meetings • Provide information, understanding patient preferences, setting goals • Families: information, understanding – Crit Care Med 2000. over 50% of 102 ICU families failed to identify 1 failing organ, any treatment or prognosis – Chest 2006. 440 hospitalized patients, 160 caregivers. Poor knowledge of CPR – treatments and outcome

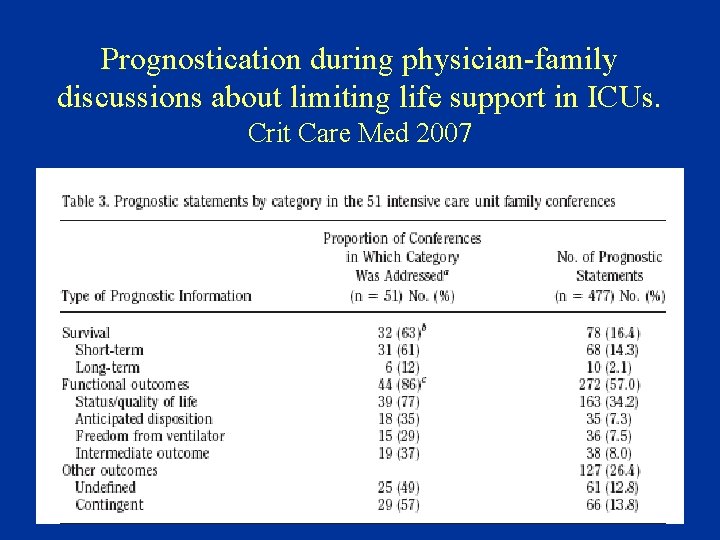
Communication - Family conferences • Study of family conferences, Seattle, 2000 -2002, Curtis et al – 51/111 eligible conferences- audiotaped, family questionnaire – Mainly white patient/family and physicians, Englishspeaking – 80% of patients died, WH/WDLS discussed in 86% of conferences • Family satisfaction with family conferences about end-of-life care in the ICU. Crit Care Med 2004 – Conference time 32 minutes, clinicians 70% of time talking. Increased proportion of family speech was associated with increased satisfaction

Communication - Family conferences • Missed opportunities during family conferences about end-of-life care in the ICU. Am J Respir Crit Care Med 2005 – 29% missed: listening/respond to question, inform about illness, ethics/palliative care, preferences, surrogate decision-making, nonabandonment, compassion • Clinician statements and family satisfaction with family conferences in the ICU. Crit Care Med 2006 • Increased family satisfaction - 3 types of clinician statements: – Assurances that patient will not be abandoned before death – Assurances that patient will be comfortable and will not suffer – Support for the family’s decision about EOL, including withdrawing or not withdrawing life support

Prognostication during physician-family discussions about limiting life support in ICUs. Crit Care Med 2007

• Understanding Cardiopulmonary Resuscitation Decision Making. Chest 2006 – Questionnaire to 440 patients with end-stage cancer and advanced diseases – Poor knowledge of CPR treatments (11% could identify 2 treatments) and outcome (2% thought success < 10%) – Many did not want to discuss preferences with doctor – Variable preferences for role in decision making. Most preferred including family member

Advance Directives • Health care proxy, living will • Permit patients to make informed decisions about their health care • Promote patient autonomy: patients have the right to make decisions and this right is protected when conscious capacity is lost. • The Patient Self-Determination Act of 1991 requires hospitals to ask patients whether they have an advance directive

• Patient with capacity to make health care decisions has the authority to decline life-sustaining treatment or ask that such treatment be withdrawn • Surrogate decision maker: patient’s representative to make decisions when the patient is incapable of making health care decisions • Substituted judgment: learn what the patient would have wanted if he or she had been able to understand participate in the decisions

Do Not Resuscitate Order • A “Do Not Resuscitate (DNR)” order is one advance directive that concerns interventions in the setting of a cardiopulmonary arrest • A DNR order means that if the patient suffers a cardiopulmonary arrest, the interventions of intubation, CPR and ACLS will be withheld

Decision to Withdraw Life Support • Patient’s expressed wishes • Health care proxy or living will • Oral advance directive – requires Ethics Consultation

Withholding and Withdrawing Life. Sustaining Treatments • Based on the individual patient’s goals of therapy, withholding an intervention may be appropriate • As well, a trial of therapy with clear goals may be undertaken. If the goals are not achieved, withdrawing an intervention is acceptable • The motivation must be respect for patient preferences and avoiding burdensome interventions

Withdrawal of Life Support • Majority of physicians withdraw/withhold life support Am J Respir Crit Care Med 1995 • Life-sustaining treatments: ventilation, vasopressors, dialysis, blood products, nutrition, hydration • >70% of ICU deaths are preceded by decision to WH/WD – Am J Respir Crit Care Med 1998

Withdrawal of Mechanical Ventilation in Anticipation of Death in the ICU Cook et al. N Engl J Med 2003 • 15 medical-surgical ICUs, 851 patients receiving mechanical ventilation • 63% weaned, 17% died while receiving MV • 19. 5% died after withdrawal of MV Determinants of withdrawal • Physicians’ perception of patient preference • Physician prediction of low likelihood of ICU survival and high likelihood of poor cognitive function • Dependency on inotropes and vasopressors

Symptoms in the Critically Ill • Patients die with treatable pain • The symptom burden of chronic critical illness. Crit Care Med 2004 – Patient report: 50 patients with tracheostomy – 40 -50% of patients experienced pain at the highest levels of intensity, 60% dyspnea – Studied communicative patients so likely underestimate symptoms and relief – Half of patients died by 3 months

Nursing - Front Line • Nurse is the main caregiver – ICU, Palliative unit • Improve EOL care – MD/RN Communication • Differences in ideas of EOL, processes, good death, predicting outcomes of critically ill patients – Crit Care Med 2003: 1900 judgments by MD and RNs, disagreements in 63% of dying patients • MD and RN: Different experiences and burdens

Factors associated with nurse assessment of the quality of dying and death in the intensive care unit. Crit Care Med 2004. • 178 patients • QODD: Control of pain, situation, breathing, dignity, time with family, spiritual/religious, someone present at death, on ventilator, proper amount of sedation • Independent predictors of QODD score: – CPR performed in last 8 hours of life – negative – Someone present at moment of death – positive

Quality of Dying in the ICU Chest 2005 • • Ratings by families of 38 decedents, QODD <50% had pain controlled 3% breathing comfortably 32% kept dignity and self-respect

Family Perspectives • Family perspectives on end-of-life care at the last place of care. JAMA 2004 • Family follow-up after 1578 deaths • 67% institution, 32% death at home • Unmet needs in institutions (more than 1/3 reported): inadequate treatment for pain or dyspnea, emotional support, respect, physician communication


How we can improve EOL care • Recognize end of life, preferences, goals of care for the patient • Process of ICU care: decision-making, communication, symptom management • Education, teaching communication skills • For ICU Nurses: involvement in EOL decisions • Communicate - MD, RN, family • Use resources: Nursing, Palliative, Critical Care, Geriatrics, Pastoral Care, Ethics, Social Work