Control of the cardiovascular system Reverend Dr David




















- Slides: 31

Control of the cardiovascular system Reverend Dr. David C. M. Taylor School of Medical Education dcmt@liverpool. ac. uk http: //pcwww. liv. ac. uk/~dcmt/cvs 09. ppt

What is the role of the cardiovascular system?

Blood Pressure Depends upon the amount of blood leaving the heart n cardiac output and the resistance of the vasculature n total peripheral resistance

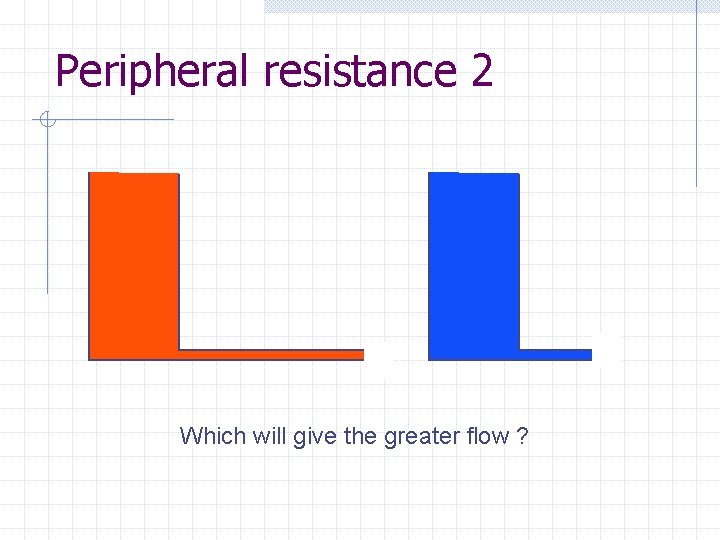
Peripheral Resistance Which will give the greater flow ?

Peripheral resistance 2 Which will give the greater flow ?

Cardiac Output Heart rate x stroke volume End diastolic volume - End systolic volume Stroke volume Cardiac output Heart rate

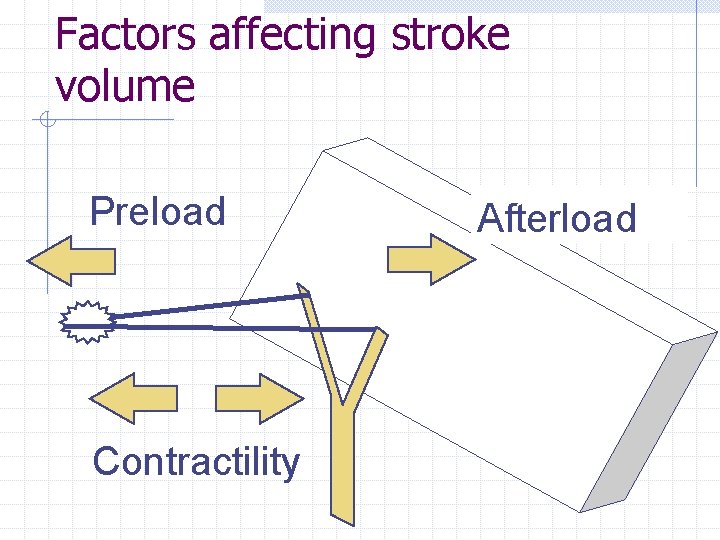
Factors affecting stroke volume Preload Contractility Afterload

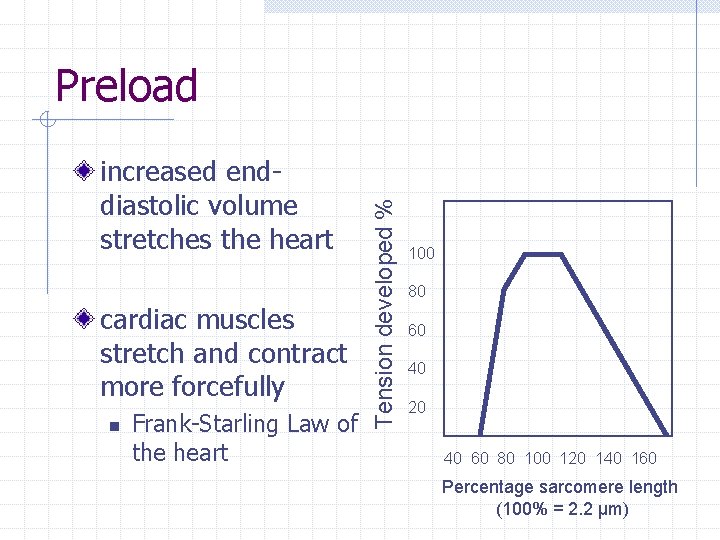
increased enddiastolic volume stretches the heart cardiac muscles stretch and contract more forcefully n Frank-Starling Law of the heart Tension developed % Preload 100 80 60 40 20 40 60 80 100 120 140 160 Percentage sarcomere length (100% = 2. 2 µm)

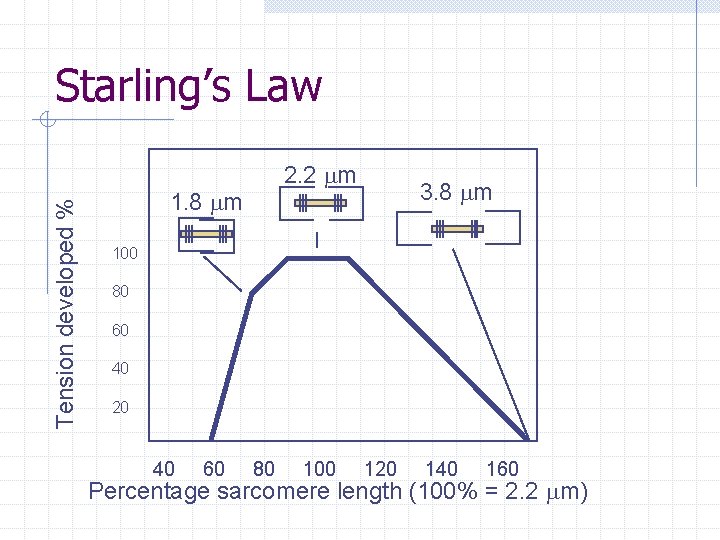
Tension developed % Starling’s Law 2. 2 m 1. 8 m 3. 8 m 100 80 60 40 20 40 60 80 100 120 140 160 Percentage sarcomere length (100% = 2. 2 m)

Contractility-”Inotropic effect” positive inotropic agents increase available intracellular Ca 2+ increase number of actinomyosin binding sites increase force of contraction positive inotropic agents n n n sympathetic stimulation catecholamines glucagon thyroid hormones increased extracellular Ca 2+

Afterload decreased arterial blood pressure during diastole decreased afterload semilunar valves open sooner when blood pressure in pulmonary artery & aorta is lower afterload n n n blood pressure viscosity of blood elasticity of arteries

Stroke Volume Cardiac Output Heart Rate

Heart Rate Nervous system n n increased sympathetic decreased parasympathetic Chemicals n n n catecholamines thyroid hormones moderate Ca 2+ increase

Heart Rate 2 Other factors n n age gender “fitness” body temperature

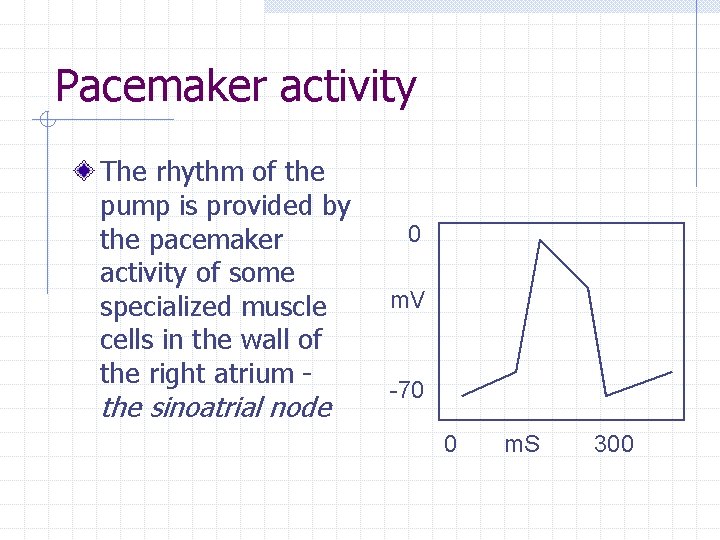
Pacemaker activity The rhythm of the pump is provided by the pacemaker activity of some specialized muscle cells in the wall of the right atrium - the sinoatrial node 0 m. V -70 0 m. S 300

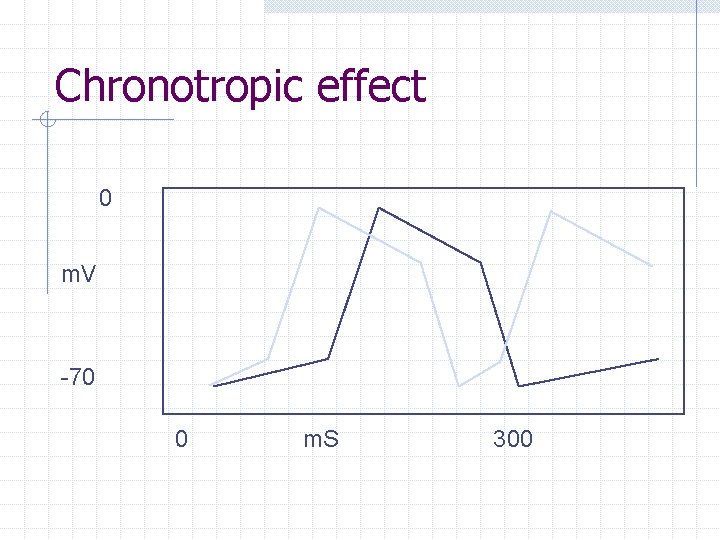
Chronotropic effect 0 m. V -70 0 m. S 300

Hypertension David Taylor School of Medical Education

Hypertension Excellent article: n ABC of Hypertension: The pathophysiology of hypertension, Beevers G, Lip GYH and O’Brien E (2001) BMJ, 322: 912 -916 Upto 5% of patients with hypertension have it as secondary to some other disease (e. g. renal disease) The rest have “essential hypertension”

The story so far. . . http: //pcwww. liv. ac. uk/~dcmt/cvs 09. ppt intrinsic (Starling’s Law) extrinsic (principally autonomic) Stroke volume Heart rate Cardiac output

Postulated mechanism Increased sympathetic activity n n Leads to increased cardiac output And peripheral vasoconstriction (to protect the capillary beds) Drop in blood flow n Triggers renin-angiotensin system

Evidence Cross transplantation studies show that essential hypertension has its origins in the kidneys. n Human and animal studies Little evidence that “stress” is involved n But, of course, drugs that decrease sympathetic activity lower blood pressure.

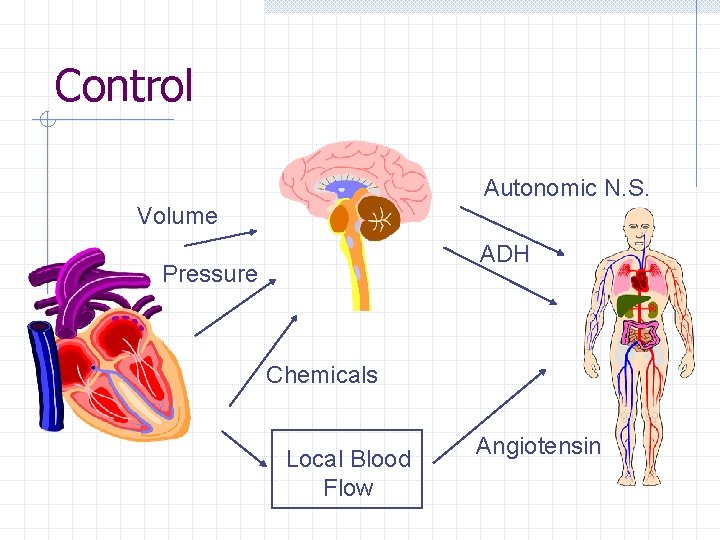
Control Autonomic N. S. Volume ADH Pressure Chemicals Local Blood Flow Angiotensin

Pressure Sensed by baroreceptors n in carotid arteries and aortic arch an increase in pressure causes a decrease in sympathetic activity a decrease in pressure causes an increase in sympathetic activity

Volume Sensed by atrial volume receptors A decrease in volume causes an increase in ADH secretion and a decrease in ANF secretion

Chemicals A decrease in O 2, or more usually an increase in CO 2 or H 2 causes an increase in chemoreceptor activity which increases sympathetic activity

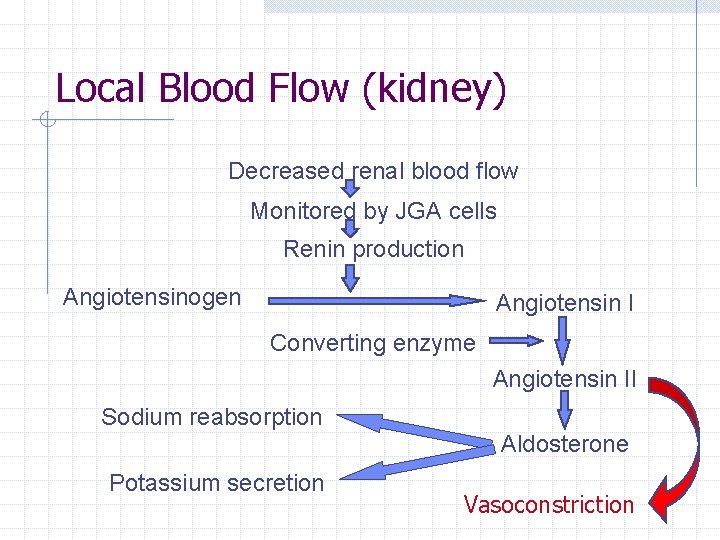
Local Blood Flow (kidney) Decreased renal blood flow Monitored by JGA cells Renin production Angiotensinogen Angiotensin I Converting enzyme Angiotensin II Sodium reabsorption Aldosterone Potassium secretion Vasoconstriction

Hormones Angiotensin II is a vasoconstrictor Aldosterone increases vascular sensitivity to Angiotensin II ADH (anti-diuretic hormone) increases water reabsorption ANF decreases sodium reabsorption

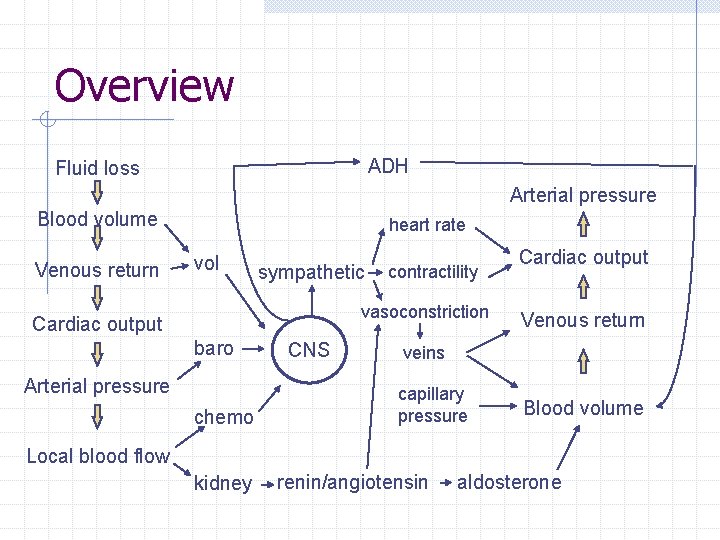
Overview ADH Fluid loss Arterial pressure Blood volume Venous return heart rate vol sympathetic contractility vasoconstriction Cardiac output baro Arterial pressure chemo CNS Cardiac output Venous return veins capillary pressure Blood volume Local blood flow kidney renin/angiotensin aldosterone

Shock David Taylor School of Medical Education

Shock Stage 1 Compensated/Nonprogressive n mechanisms work as planned Stage 2 Decompensation/Progressive n if blood volume drops more than 15 - 25% Stage 3 Irreversible

Progressive shock depression of cardiac activity n bp <60 mm. Hg poor flow through coronary arteries leads to ischemia depression of vasoconstriction n bp 40 - 50 mm. Hg increased capillary permeability n caused by hypoxia clotting, cell destruction, acidosis