Chapter 7 Somatosensory System l Chris Rorden University
























- Slides: 45

Chapter 7 Somatosensory System l Chris Rorden University of South Carolina Norman J. Arnold School of Public Health Department of Communication Sciences and Disorders University of South Carolina 1

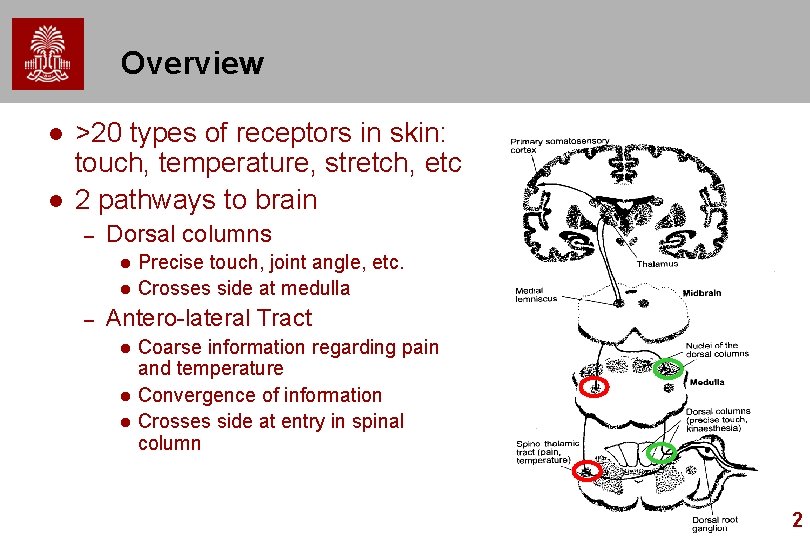
Overview l l >20 types of receptors in skin: touch, temperature, stretch, etc 2 pathways to brain – Dorsal columns l l – Precise touch, joint angle, etc. Crosses side at medulla Antero-lateral Tract l l l Coarse information regarding pain and temperature Convergence of information Crosses side at entry in spinal column 2

Early Somatosensation l PNS detection of – – l Pain Temperature Touch Conscious proprioception Transfer of information to CNS 3

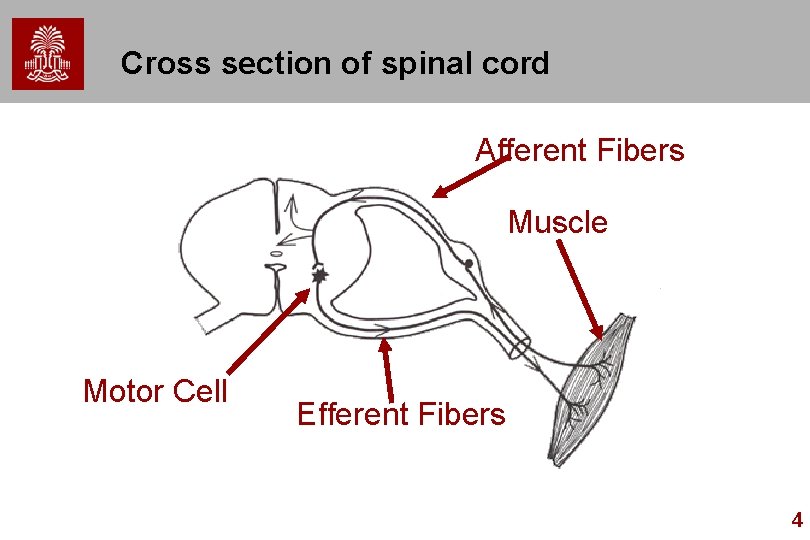
Cross section of spinal cord Afferent Fibers Muscle Motor Cell Efferent Fibers 4

Hierarchy of Sensory Fibers l l l l l Specialized Receptors (Stimuli to Neural Signal) Single Nerve Fiber Sensory Fiber Bundle Spinal Nerve Dorsal Root Ganglia Dorsal Column Nuclei Spinal Motorneurons or Reticular Formation Thalamus Primary and Association Cortex (Parietal Lobe) 5

Organization l Each tract mediates specific modalities of sensation, somatotopic organization in tracts and cortex – Mechanoreceptive l Mechanical displacement of nerve endings l Touch (fine and diffuse), pressure, vibration, kinesthesia – Thermoreceptive l Cold – and Heat Nociceptive l Pain 6

Specialized Receptors l l Receptors specialize by type of stimulus Adaptiveness: Reduction of response to sustained stimuli Basic Types of Sensory Receptors Encapsulated Endings – Adapting (tactile) l l l Free Nerve Endings (pain, temp, some tactile) – l Pacinian corpuscle: deep pressure touch and high frequency vibration. Meissner’s corpuscle: light touch, such as the fingertips, palms, soles, lips, tongue, face Nonadapting Expanded Tip Endings (tactile, temp) – Moderately adapting 7

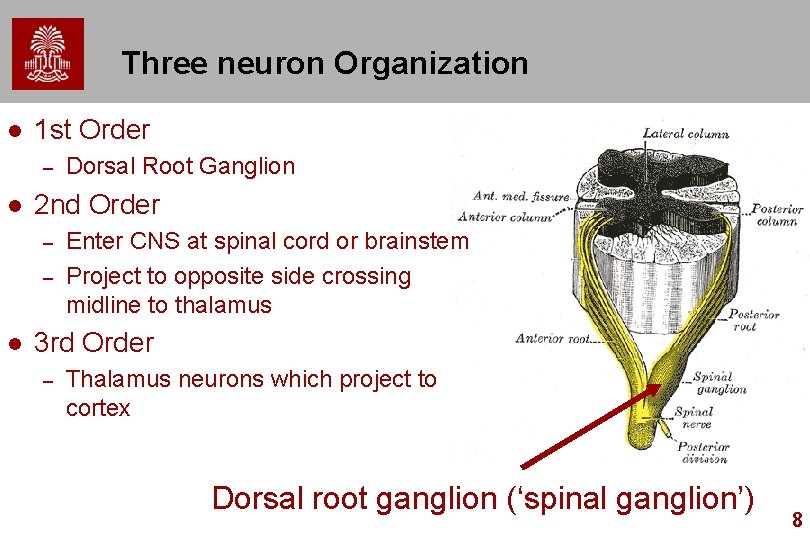
Three neuron Organization l 1 st Order – l 2 nd Order – – l Dorsal Root Ganglion Enter CNS at spinal cord or brainstem Project to opposite side crossing midline to thalamus 3 rd Order – Thalamus neurons which project to cortex Dorsal root ganglion (‘spinal ganglion’) 8

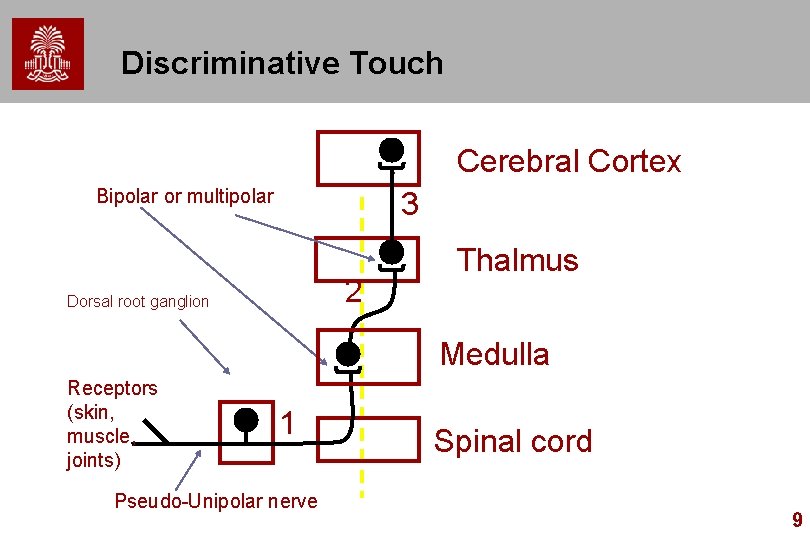
Discriminative Touch Cerebral Cortex Bipolar or multipolar 3 2 Dorsal root ganglion Thalmus Medulla Receptors (skin, muscle, joints) 1 Pseudo-Unipolar nerve Spinal cord 9

Anatomical Divisions l Dorsal Column-Medial Lemniscal (or Epicritic System) – – Fine discriminative touch, vibration, limb position, kinesthesia & deep pressure Position sense l l l Anterolateral (or Protopathic System) – Pain, temperature and diffuse touch l l l Proprioception - Awareness of limb position Kinesthesia - Awareness of limb movement Lateral spinothalamic tract Anterior spinothalamic tract Dorsal Column-Medial Lemniscal System 10

Dorsal Column-Medial Lemniscal System l Important for skilled movements – – l Stereognosis - Fine touch discrimination Graphesthesia - Recognizing numbers written on body Two and multiple point touch Deep touch Receptors – Meissner’s and Pacinian Corpuscles l l – Encapsulated end receptors Highly sensitive and adaptable Muscle Spindle Organs l l Kinesthesia Proprioception 11

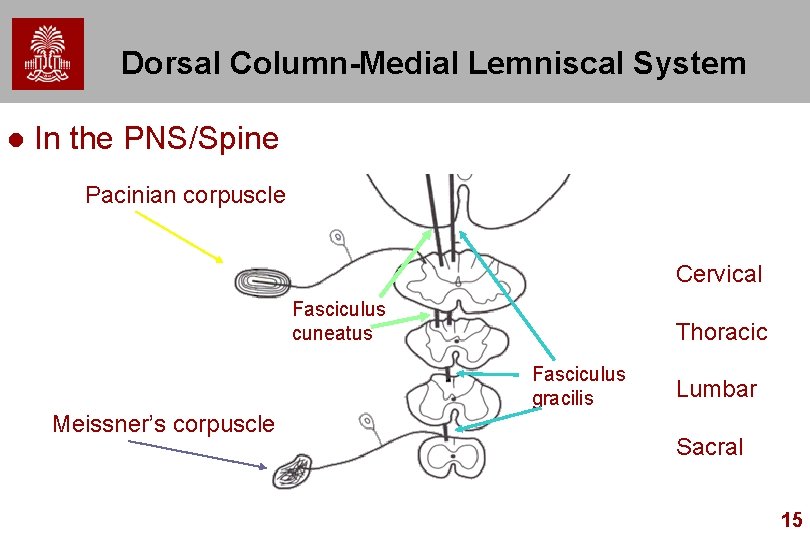
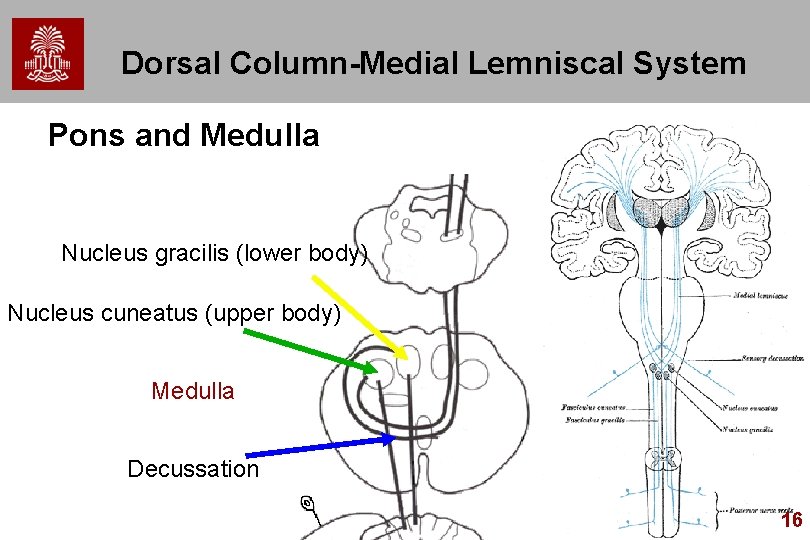
Neural Pathways l l l Fasciculus Gracilis (slender, graceful) Fasciculus Cuneatus (wedge-shaped – short) (think cuneiform writing) Path – – – Mediate discriminative Touch from different Body areas; follow three-neuron organization Spinal Ganglion (1) Fasciculus Gracilis/Cuneatus tracts (1) Gracilis or Cuneatus Nucleus (2) Through Medial Lemniscus to Thalamus (3) Thalamus to Cortex 12

Levels of Reception l Fasciculus Gracilis – – l Sacral to Midthoracic Level Lower Body Fasciculus Cuneatus – – Above Midthoracic Level Upper Body 13

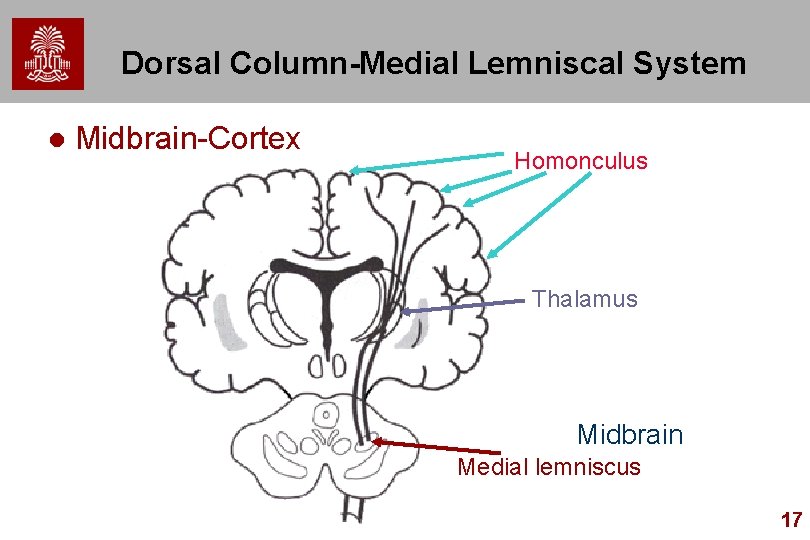
Pathway Spinal Cord l Brainstem Nuclei l Thalamus (N. Ventral Posterolateralis) l Thalamus through Internal Capsule to Primary Sensory Parietal Cortex l Primary to Association Cortex l – Mapped spatially (homunculus) 14

Dorsal Column-Medial Lemniscal System l In the PNS/Spine Pacinian corpuscle Cervical Fasciculus cuneatus Thoracic Fasciculus gracilis Meissner’s corpuscle Lumbar Sacral 15

Dorsal Column-Medial Lemniscal System Pons and Medulla Nucleus gracilis (lower body) Nucleus cuneatus (upper body) Medulla Decussation 16

Dorsal Column-Medial Lemniscal System l Midbrain-Cortex Homonculus Thalamus Midbrain Medial lemniscus 17

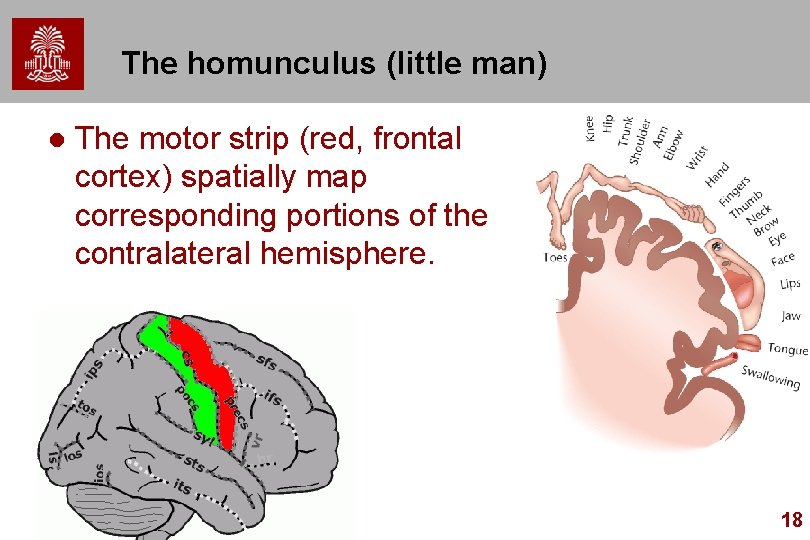
The homunculus (little man) l The motor strip (red, frontal cortex) spatially map corresponding portions of the contralateral hemisphere. 18

Clinical Considerations l l l If injury is inferior to decussation, deficit can be ipsilateral (same side) If injury is superior to decussation, deficit will be contralateral (opposite side) Tests – – – – Two Point Discrimination Stereognosis: ID object with eyes closed Graphesthesia: number or letter on skin Vibratory: Tuning fork on bony surface Romberg: standing with eyes closed Kinesthesia: movement identified Association: Identification of object 19

Anterolateral system l l Pain, Temperature, & Diffuse Touch Three-tier neuron organization system 1. 2. 3. l Enter at spinal ganglion (1 st) Cross in spinal tract (2 nd order) Ventral posterolateral n. of thalamus (3 rd) Two Tracts – – Lateral Spinothalamic Anterospinothalamic 20

Lateral Spinothalamic Tract l l Receptors - Free Nerve Endings Neural Pathway – – Nocioceptors (pain) Dorsolateral spinal cord (up or down several segments) l – Substantial Gelatinosa and Proprius l – – – spinal cord entrance Where 1 st order neurons connect with 2 nd order neurons Lateral Spinothalamic Tract Cross Midline (2 nd order) Spinal Lemniscus (brainstem) Thalamus (VPL) to Cortex Collaterals to Subcortical structures 21

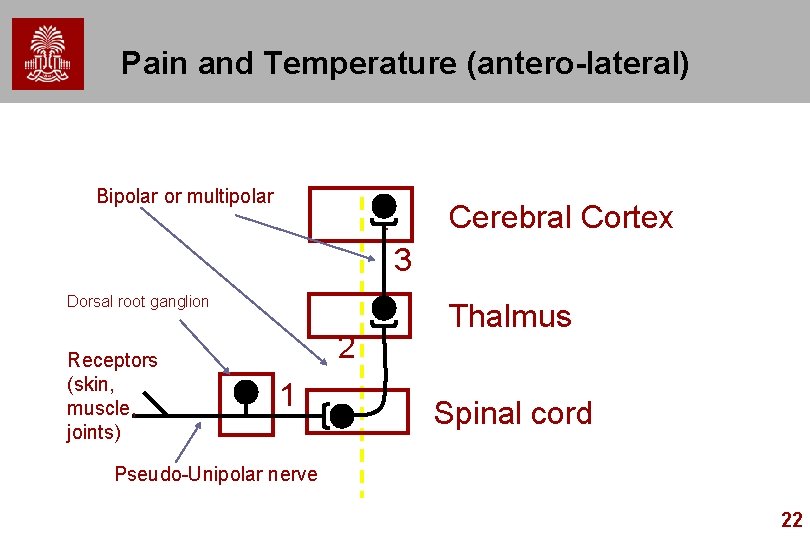
Pain and Temperature (antero-lateral) Bipolar or multipolar Cerebral Cortex 3 Dorsal root ganglion Receptors (skin, muscle, joints) 2 1 Thalmus Spinal cord Pseudo-Unipolar nerve 22

Clinical Considerations (lesion locations) PNS or spinal before midline cross results in problems ipsilaterally. l Spinal or Brainstem lesion results in problems contralaterally. l – l Chordotomy (surgical lesion) to reduce pain Dermatomes: Failure to perceive pain 23

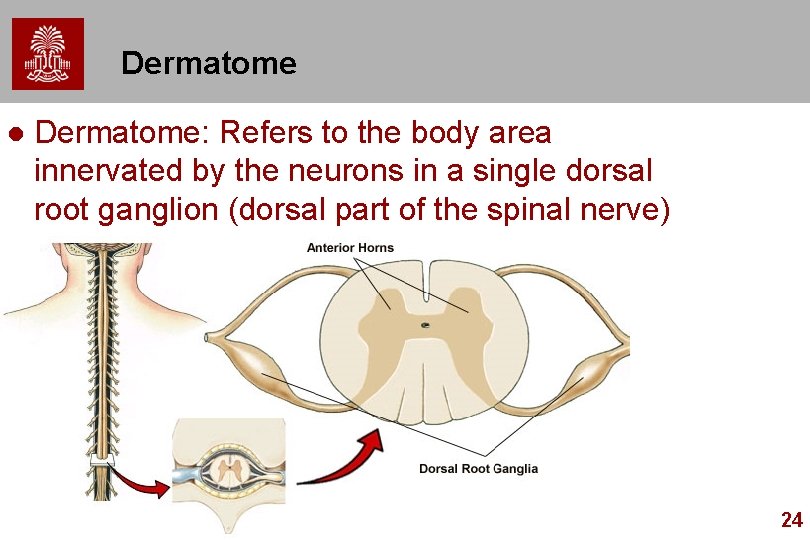
Dermatome l Dermatome: Refers to the body area innervated by the neurons in a single dorsal root ganglion (dorsal part of the spinal nerve) 24

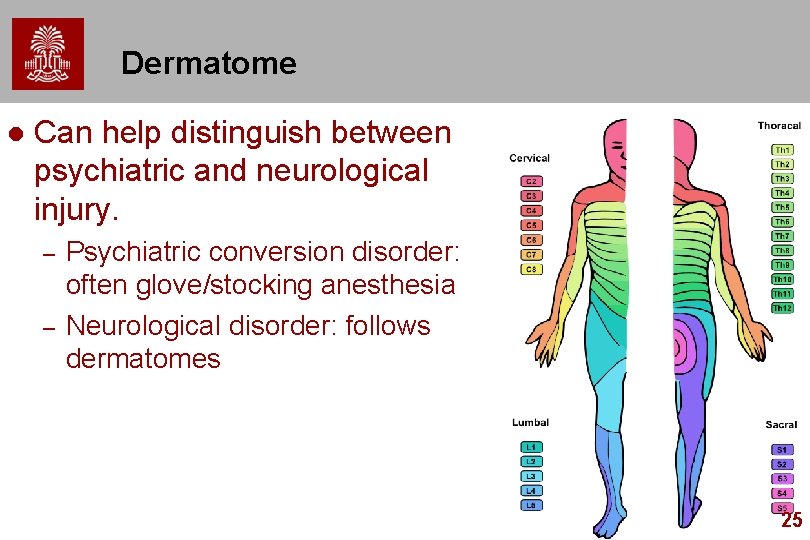
Dermatome l Can help distinguish between psychiatric and neurological injury. – – Psychiatric conversion disorder: often glove/stocking anesthesia Neurological disorder: follows dermatomes 25

Other Considerations Referred pain: one site has pain but felt in another site l Drugs can suppress pain sensitivity or block pathway l Analgesia: No sensation l Hypalgesia: Decreased pain (higher threshold) l Hyperalgesia: Increased pain (lower threshold) l 26

Anterospinothalamic Tract l l Discrimination of Diffuse touch Receptors: All three types – – – l Neural Pathway – – – l Encapsulated endings Free nerve endings Expanded tip endings Skin to ganglia (1 st) Dorsolateral spinal cord (up and down seg) Proprius and Substantia Gelatinosa (2 nd) Go to spinothalamic tract to VPL (thalamus) to postcentral gyrus Collaterals to subcortical structures Clinically, interruption causes no obvious deficit 27

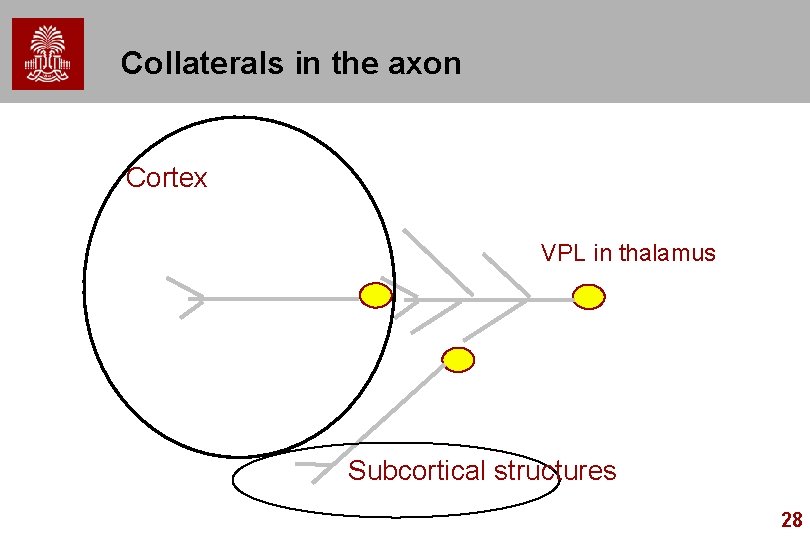
Collaterals in the axon Cortex VPL in thalamus Subcortical structures 28

Sensation from the head l Face and Head area – – – l face forehead anterior half of scalp dura mater orbital cavities nasal and oral cavities Epicritic (Dorsal) and Protopathic (Anterolateral) Systems 29

Facial sensation l Three Neuron Levels – – – 1 st order: Semilunar ganglion of Trigeminal Nerve 2 nd order: Principal sensory nucleus and trigeminal spinal tract nucleus 3 rd order: VPL in thalamus to lower third of postcentral gyrus 30

Fine Discriminative Touch l Neural Pathway – – – Encapsulated receptors in facial and head skin Semilunar ganglion and trigeminal nucleus Medial Lemniscus Thalamus to cortex 31

Cranial Proprioceptive and Kinesthetic Sensation Teeth, periodontium palate, TMJ, muscles of mastication l Involves mesencephalic N. and follows similar pattern l Mechanism for jaw reflex and bit control l 32

Cranial Sensation: Clinical Considerations l Lesions can affect only one branch – – l Ophthalmic Maxillary Mandibular Or one half of the face Tests the same for discrimination 33

Pain and Temperature from Face l Neural Pathway – – Nocioceptors Semilunar ganglion to l nucleus of spinal trigeminal tract (moves caudally) l chief sensory nucleus – – Cross midline to thalamus and some stay ipsilateral Postcentral Gyrus 34

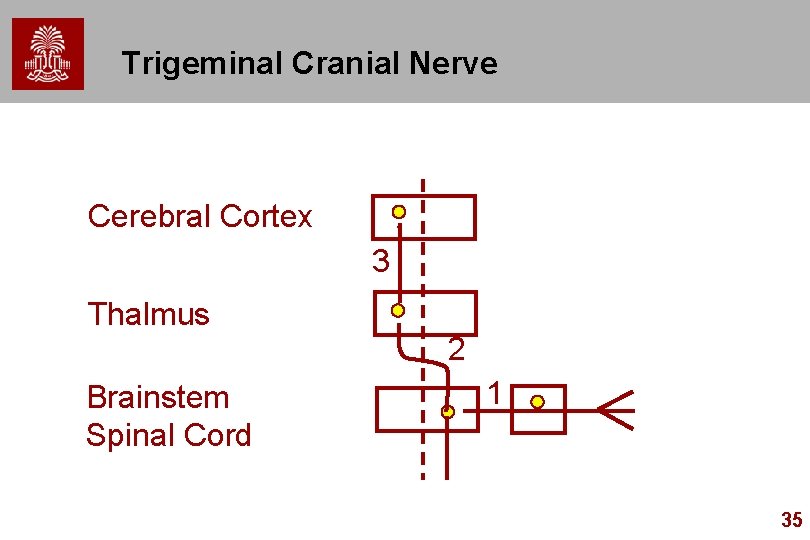
Trigeminal Cranial Nerve Cerebral Cortex 3 Thalmus 2 Brainstem Spinal Cord 1 35

Clinical Considerations Inflammation of semilunar ganglion causes severe pain l Tic douloureux - severe pain l Assessment of normal function l – – pinching to cause pain Quality assessment by patient 36

Diffuse Touch from Face l Neural Pathway – – – Dorsal and ventral secondary trigeminal tract Some to spinal trigeminal tract nucleus Some to chief sensory nucleus l To ventral posteromedial nucleus of thalamus l To sensory cortex 37

Unconscious Proprioception l l Conscious proprioception by dorsal column-medial lemniscal system Unconscious involved in walking, articulating, writing, swallowing, and eye movement. Two order neural system Tracts – – – l Dorsal Spinocerebellar Cuneocerebellar Ventral Spinocerebellar Receptors – Muscle spindles and Golgi tendon organs located in muscles and limb joints 38

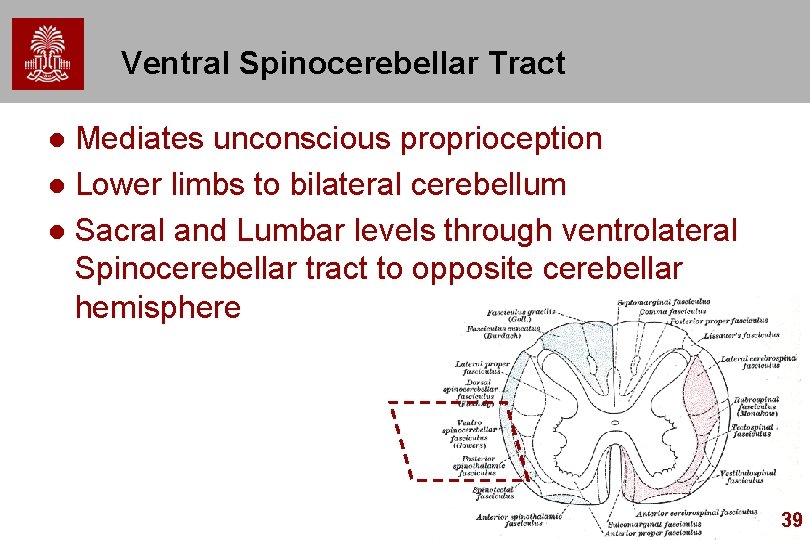
Ventral Spinocerebellar Tract Mediates unconscious proprioception l Lower limbs to bilateral cerebellum l Sacral and Lumbar levels through ventrolateral Spinocerebellar tract to opposite cerebellar hemisphere l 39

Dorsal Spinocerebellar Tract l l Mediates unconscious proprioception Lower limbs and middle regions of body to to bilateral cerebellum Spinal ganglion to nucleus dorsalis of Clark at third lumbar segment Do not cross and enter ipsilateral cerebellar hemisphere Dorsal spinocerebellar tract – information about movement (sensory feedback) Ventral spinocerebellar - internally generated information about the movement. 40

Cuneocerebellar Tract Mediates upper limbs and neck l Uncrossed fibers to ipsilateral external cuneate nucleus to cerebellum l Clinical Considerations l – – Romberg used to determine some function Difficult to test clinically Romberg Test Ask individual to stand straight with feet together and hands by the sides. Compare balance with eyes open versus eyes closed. If less steady with eyes closed (positive), ataxia is sensory – spinal injury. If there is no difference (negative) it suggests cerebellar problem. 41

42

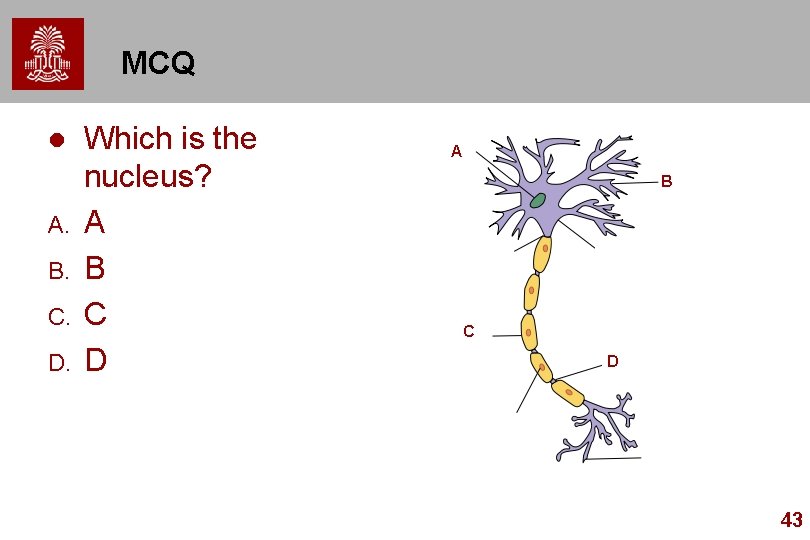
MCQ l A. B. C. D. Which is the nucleus? A B C D 43

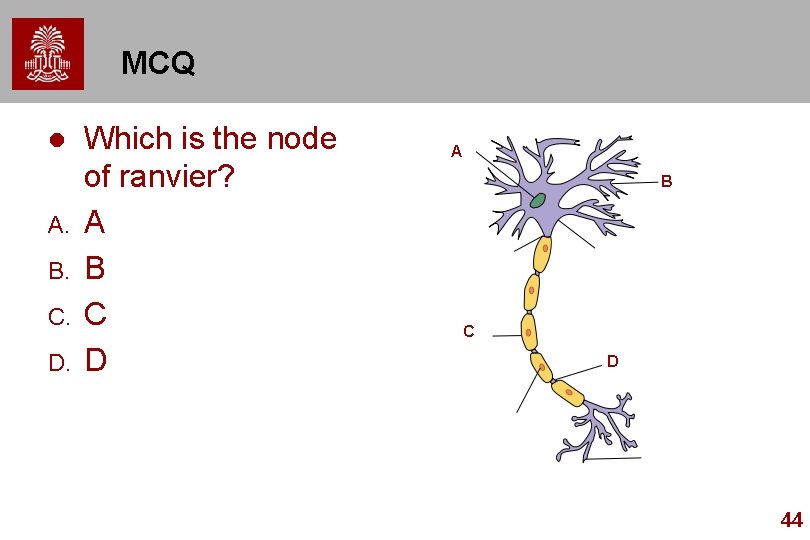
MCQ l A. B. C. D. Which is the node of ranvier? A B C D 44

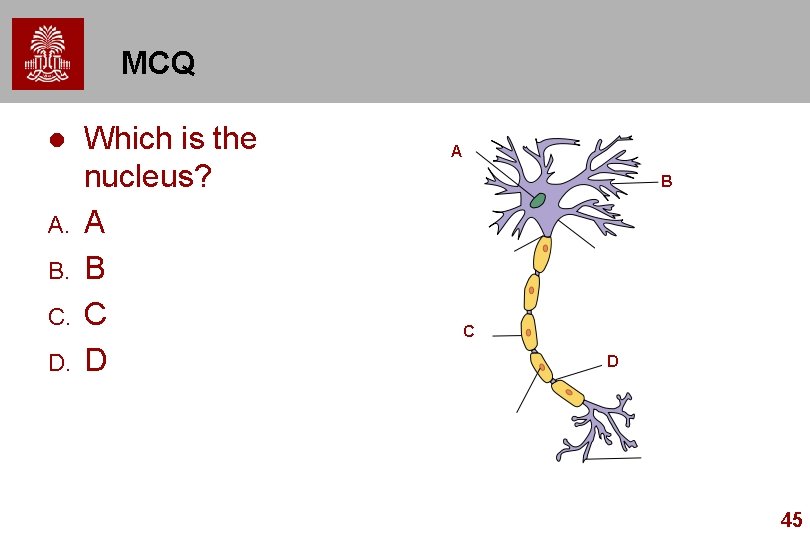
MCQ l A. B. C. D. Which is the nucleus? A B C D 45