Acute Mesenteric Ischemia Isaac George MD Resident in
































- Slides: 58

Acute Mesenteric Ischemia Isaac George, MD Resident in Surgery Department of Surgery Columbia University College of Physicians and Surgeons The PVD. org

Acute Mesenteric Ischemia • • • Incidence Pathophysiology Diagnosis Therapy Treatment Algorithm Objectives The PVD. org

Objectives • • • Understand pathophysiology Identify patients at high-risk for mesenteric ischemia Develop treatment plan for each patient/apply treatment algorithm The PVD. org

Introduction • Cokkinis (1921): “occlusion of the mesenteric vessels is regarded as one of those conditions of which the diagnosis is impossible, the prognosis hopeless, and the treatment almost useless. ” • Occlusive or non-occlusive mechanism leading to hypoperfusion of one or more mesenteric vessels The PVD. org

Rationale • Incidence – – • Mortality – – • 1960’s - 70 -100%2 1970’s - 60 -70%3 Morbidity – – • 1 -2/1000 hospital admissions 1% of GI admissions 1 Cardiopulmonary, MOSF Extended LOS, TPN dependence 4 Recurrence – The PVD. org Up to 60%4 Ann Surg 2001; 233(6): 801 -808 Ann Surg 1982; 195: 554 -565 3 Ann Surg 1978; 188; 721 -731 4 Ann Vasc Surg 2003; 17: 72 -9 1 2

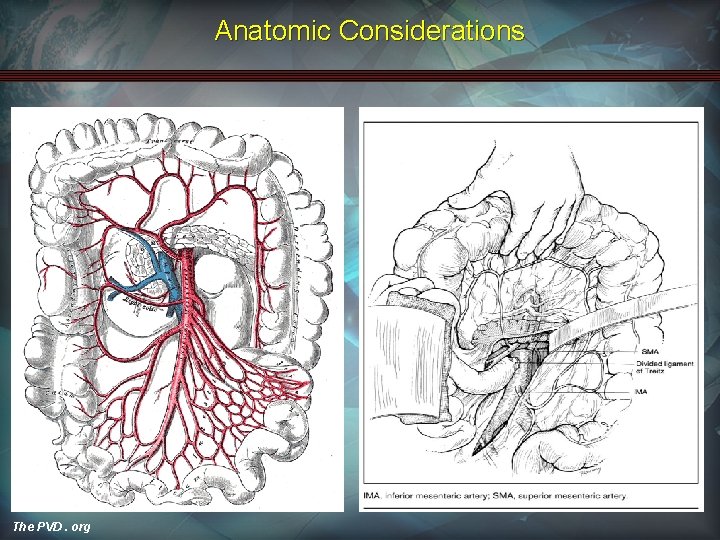
Anatomic Considerations The PVD. org

Pathophysiology: Etiology • Arterial Embolic Disease • Arterial Thrombotic Disease • Venous Thrombotic Disease • Non-occlusive Mesenteric Ischemia The PVD. org

Pathophysiology Arterial Embolism • • • Majority of cases (>50%): SMA occlusion Location: origin of middle colic artery (ischemia from proximal jejunem to splenic flexure) Embolic sources: cardiac (80%)1, aortic plaques Celiac and IMA occlusion usually tolerated SMA occlusion → death Most have underlying stenoses as well 1 The PVD. org Ann Vasc Surg 1990; 4: 112 -116

Pathophysiology Arterial Thrombotic Disease • • 15% of acute intestinal ischemia 1 Pre-existing atherosclerotic disease ― Worsening chronic mesenteric ischemia • Found at ostium of SMA • More delayed onset of symptoms 1 The PVD. org Vasc Surg 1996; 4 th ed.

Pathophysiology Venous Thrombotic disease • • • The PVD. org 5 -10% of intestinal ischemia Younger patient population 80% have hypercoaguable state Risk factors: oral contraceptives, previous DVT/PE, malignancy, portal HTN, nephrotic syndrome May limit arterial flow→edema, segmental infarction

Pathophysiology Non-Occlusive disease • • 20 -30% of acute intestinal ischemia Response to systemic hypoperfusion ― Sympathetic adrenergic system mediated • • Visceral vasoconstriction/shunting for cerebral protection Causes: any severe systemic illness, CHF, dehydration, drugs (cocaine, ergot alkaloids, digitalis, β-blockers, α-agonist, epo), hemodialysis The PVD. org

Clinical Presentation: Physical Examination Arterial Thromboembolic, Non-Occlusive • Severe abdominal pain • Sudden onset Venous Thrombotic • Less severe pain • Subacute • Symptoms variable • Abdominal pain-non-specific, crampy vs. steady, anterior • Gastric emptying/vomiting • Peritonitis late • Hypotension, tachycardia The PVD. org

Clinical Presentation: Laboratory Limited clinical utility • arterial lactate 1 • amylase 2 • CK, CK-BB 3 • Serum phosphate 4 • Other useless markers: LDH, PAF, TNF-α, AP, AST/ALT, αglutathione The PVD. org 1 Eur J Surg 1994; 160: 381 -4 2 Br J Surg 1986; 73: 219 -21 3 Dig Dis Sci 1991; 36: 1589 -93 4 Br J Surg 1982; 69: S 52 -3

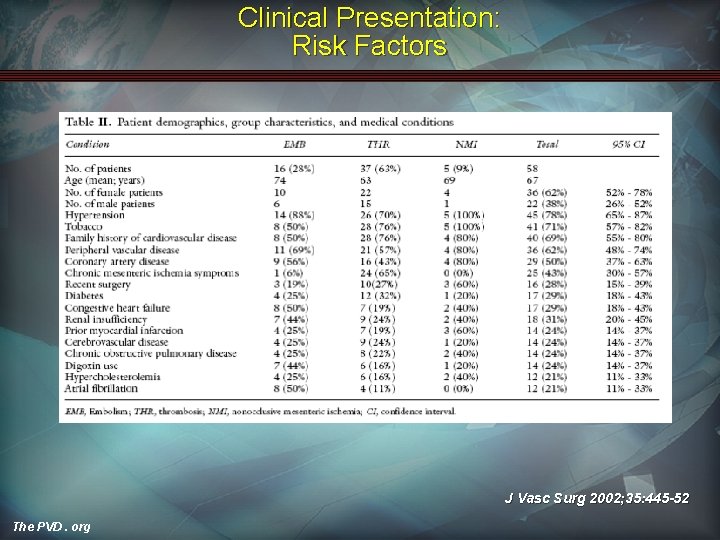
Clinical Presentation: Risk Factors J Vasc Surg 2002; 35: 445 -52 The PVD. org

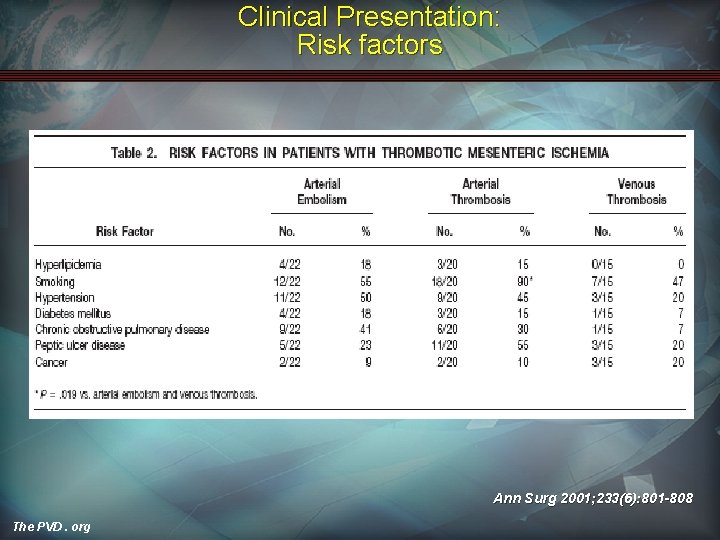
Clinical Presentation: Risk factors Ann Surg 2001; 233(6): 801 -808 The PVD. org

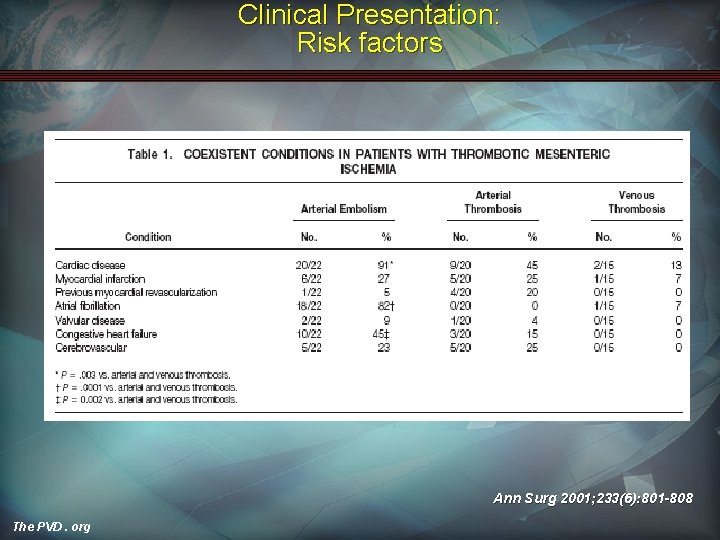
Clinical Presentation: Risk factors Ann Surg 2001; 233(6): 801 -808 The PVD. org

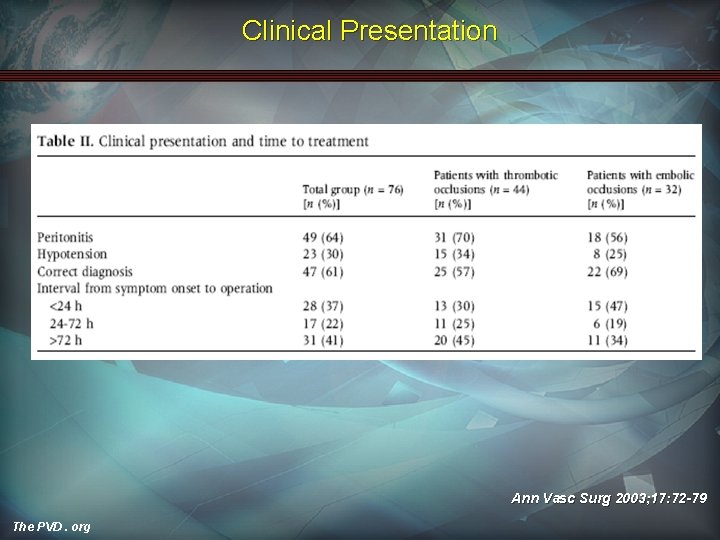
Clinical Presentation Ann Vasc Surg 2003; 17: 72 -79 The PVD. org

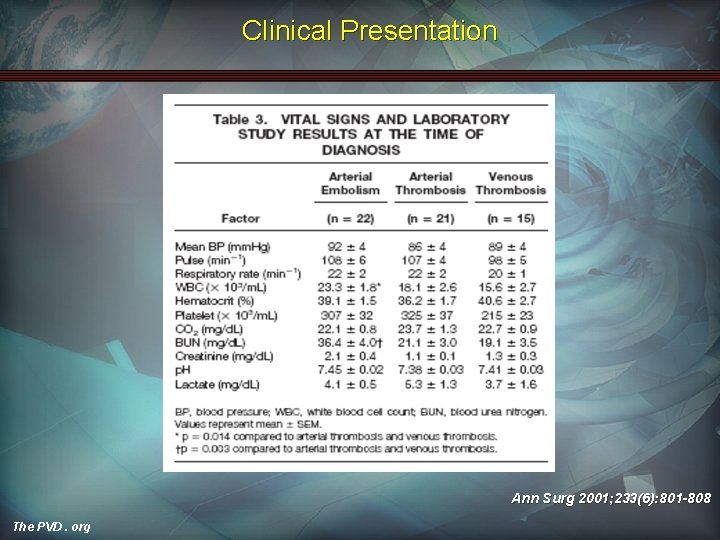
Clinical Presentation Ann Surg 2001; 233(6): 801 -808 The PVD. org

Diagnosis: Non-Invasive Imaging X-ray Computed Tomography (helical/angiography) Ultrasound MRI/MRA The PVD. org

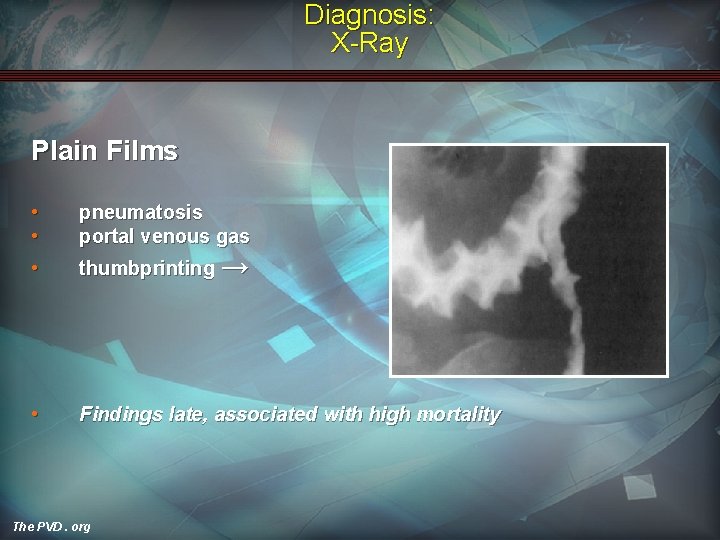
Diagnosis: X-Ray Plain Films • • pneumatosis portal venous gas • thumbprinting → • Findings late, associated with high mortality The PVD. org

Diagnosis: Computed Tomography Criteria • pneumatosis • venous gas • SMA/celiac/IMA occlusion w/distal disease • arterial embolism Sensitivity: 96% Specificity: 94% OR • bowel wall thickening + one of following: – – – lack of bowel wall enhancement solid organ infarction venous thrombosis 1 The PVD. org Radiol 2003; 229: 91 -98

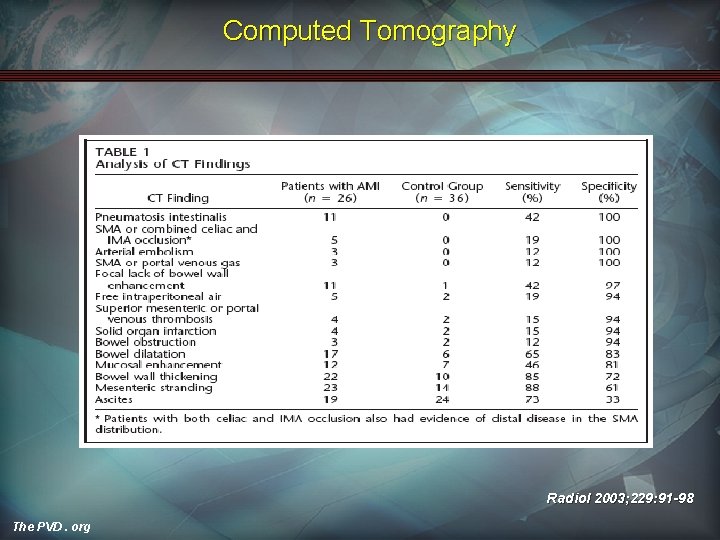
Computed Tomography Radiol 2003; 229: 91 -98 The PVD. org

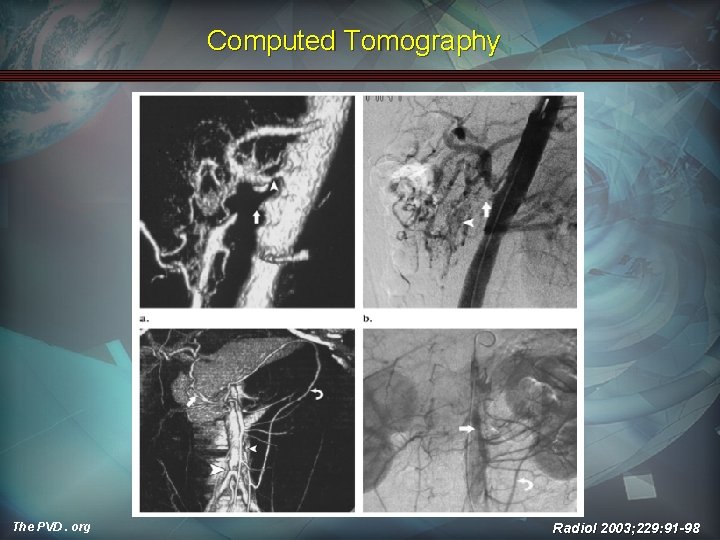
Computed Tomography The PVD. org Radiol 2003; 229: 91 -98

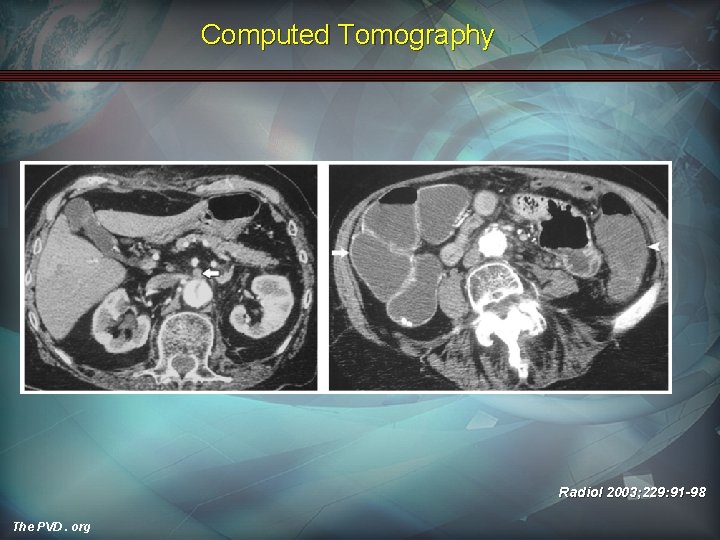
Computed Tomography Radiol 2003; 229: 91 -98 The PVD. org

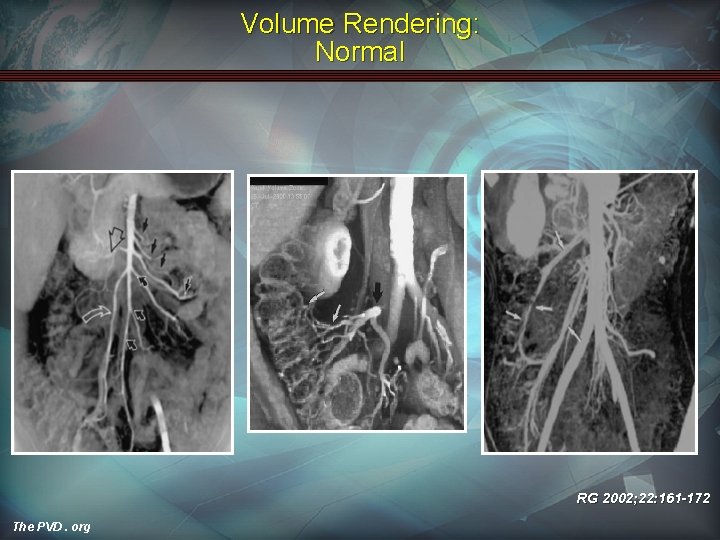
Volume Rendering: Normal RG 2002; 22: 161 -172 The PVD. org

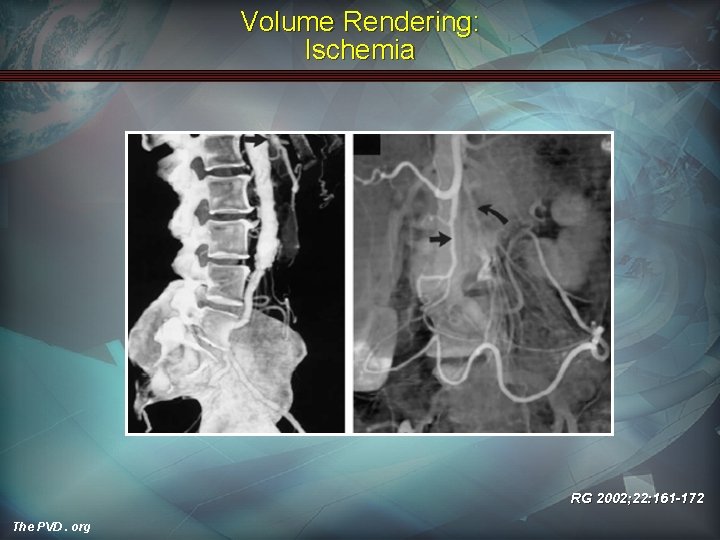
Volume Rendering: Ischemia RG 2002; 22: 161 -172 The PVD. org

Diagnosis: Ultrasound High-grade stenosis or occlusion of SMA • Sensitivity for SMA stenosis: 96% (1993) 1 – – • Prospective, n=100 Surgically confirmed embolism/thrombus Sensitivity for SMA stenosis/occlusion: 100% (1999)2 – – The PVD. org Specificity: 98% PPV: 93%, NPV: 100% N=82, prospective Confirmed with angiography 1 J Vasc Surg 1993; 17: 780 -788 2 Radiol 1999; 211: 405 -410

Diagnosis: MRI • • • Poor delineation of smaller vessels Limited clinical application Perfusion flow contrast studies show promise 1 1 The PVD. org Radiol 2004; 234: 569 -575

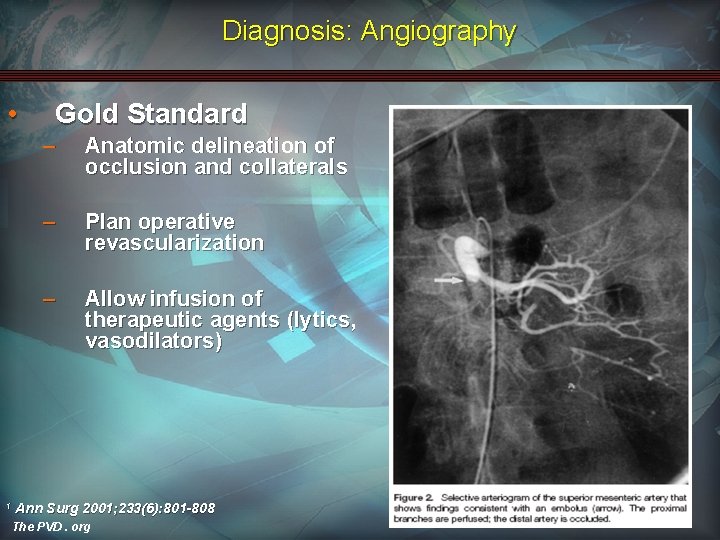
Diagnosis: Angiography • 1 Gold Standard – Anatomic delineation of occlusion and collaterals – Plan operative revascularization – Allow infusion of therapeutic agents (lytics, vasodilators) Ann Surg 2001; 233(6): 801 -808 The PVD. org

Principles of Treatment • Diagnose • Restore Flow • Resect non-viable tissue • Supportive Care • Second-Look The PVD. org

Therapy Supportive measures • IV resuscitation • Optimize cardiac status • Broad-spectrum antibiotics (no data) • Nasogastric decompression The PVD. org

Therapy: Pharmacologic Anticoagulation • Heparin IV – – – Prevents clot propagation Systemic vs. intra-arterial Timing of initiation • – • Immediately vs. 48 hr delay 1, 2 Restart 48 hrs after surgical intervention Warfarin – – The PVD. org Prevents clot propagation Give for 6 -12 mos if no clotting disorder (no data) 1 Surg Gynecol Obstet 1981; 153: 561 -569 2 Vascular Emergencies. 1982; 553 -561

Therapy: Pharmacologic Vasodilators • Papaverine (30 -60 mg/hr) – Increases c. AMP, relaxes smooth muscle – Primary indication: Non-occlusive arterial disease – Criterion for use: • • • The PVD. org Peritoneal signs absent Cannot undergo surgery Must have good distal perfusion bed

Therapy: Pharmacologic Vasodilators (cont. ) • Papaverine – Early SMA infusion reduces mortality to 40 -50%1 – Directed infusion via angiography – Rx: 24 -48 hrs • • Endpoints both clinical and angiographic Subsequent surgery 1 The PVD. org Surg 1977; 82: 848 -855

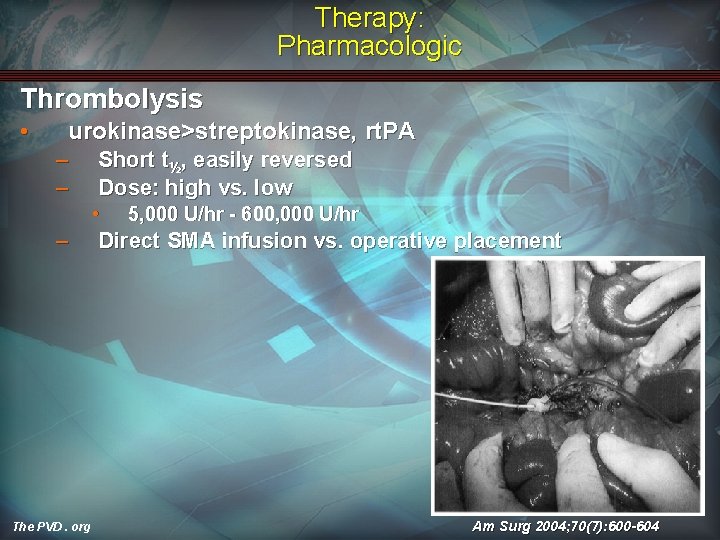
Therapy: Pharmacologic Thrombolysis • urokinase>streptokinase, rt. PA – – Short t½, easily reversed Dose: high vs. low • – The PVD. org 5, 000 U/hr - 600, 000 U/hr Direct SMA infusion vs. operative placement Am Surg 2004; 70(7): 600 -604

Therapy: Pharmacologic Thrombolysis • Duration: minutes – 48 hrs 1 – too long → risk of bowel necrosis – Treat to re-establish flow vs. complete dissolution – > 48 hrs • – Greater risk of bleeding Discontinue • • • Worsening abdominal symptoms without evidence of thrombolysis Bleeding No angiographic improvement 1 The PVD. org JVIR 2005; 16: 317 -329

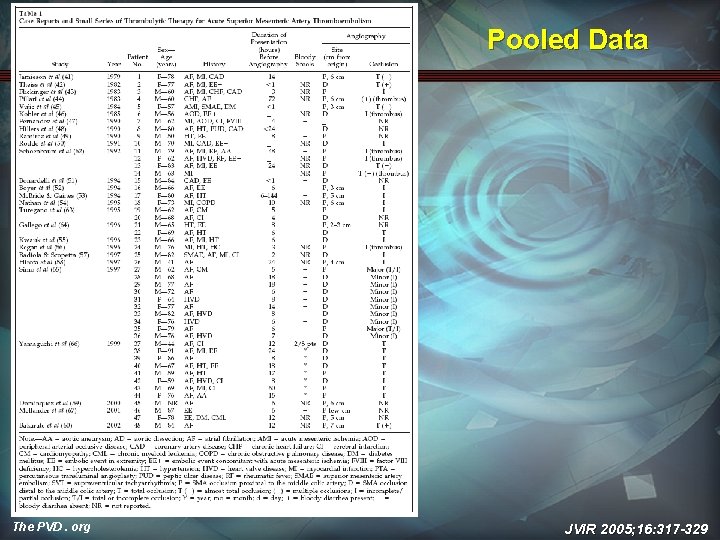
Pooled Data The PVD. org JVIR 2005; 16: 317 -329

Outcomes • Technical success: 43/48 • Technical failure: 5/48 • Outcome most dependent on age of thrombus/embolus • Improvement of abd pain in 1 st hour is a favorable prognostic sign • Technical success does not equal clinical success • Survival: 43/48 • Safety The PVD. org JVIR 2005; 16: 317 -329

Therapy: Pharmacologic Thrombolysis • Criterion for use: – – • Embolic/thrombotic disease Poor operative candidates No contraindications to fibrinolytics No bowel infarction (no peritonitis/acidosis) Expansion of use to all patients without bowel infarction The PVD. org

Therapy: Endovascular Angioplasty/Stenting • • • Long-term durability questioned vs. surgical repair Utility in acute ischemia setting Advantages: – Shorter duration of treatment than thrombolysis – Definitive treatment JVIR 1999; 10(7): 861 -867 The PVD. org

Therapy: Endovascular Angioplasty/Stenting • Ideal for thrombotic lesions – – – • Calcified ostial lesions Flow-limiting dissections Chronic occlusion Advanced techniques for embolic lesions – – The PVD. org Flow-limiting dissections Embolectomy w/distal protection

Therapy: Endovascular J Vasc Surg 2003; 38: 692 -8 The PVD. org

Therapy: Endovascular Stenting Outcomes (Chronic, SMA/Celiac) 1998: Primary patency 100% at 14 mos (n=3)1 0% mortality 1999: Primary patency 74% at 18 mos (n=12)2 8. 3% mortality <30 days 2003: Technical success 96% (n=26)3 Clinical success 88% Primary patency at 34 mos 65% Restenosis at 34 mos 12% Cardiovasc Int Radiol 1998; 21: 305 -313 2 JVIR 1999; 10(7): 861 -867 3 J Vasc Surg 2003; 38: 692 -8 I 1 The PVD. org

Therapy: Endovascular Stenting Indications • • • Simple stenotic lesions Complex lesions (long-segment, irregular, heavily calcified) Total occlusion Contraindications • • • Suspected bowel necrosis (peritonitis, acidosis, etc) diffuse distal disease Median arcuate ligament compression syndrome 1 The PVD. org J Vasc Surg 2003; 38(4): 692 -8

Surgery Anyone with peritonitis needs to be explored. • • • Midline incision Evaluate extent of ischemia Doppler of entire SMA Revascularization (embolectomy vs. bypass) Re-evaluate ischemia Lastly, non-viable bowel must be resected The PVD. org

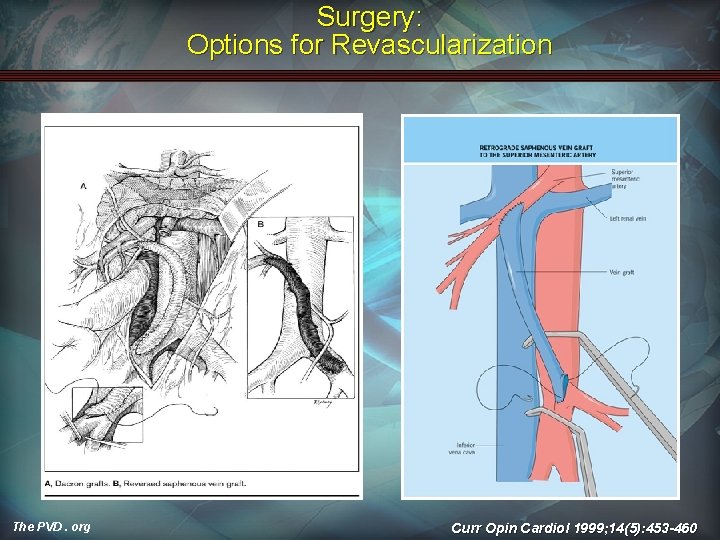
Surgery: Options for Revascularization Ann Vasc Surg 2003; 17: 72 -79 The PVD. org

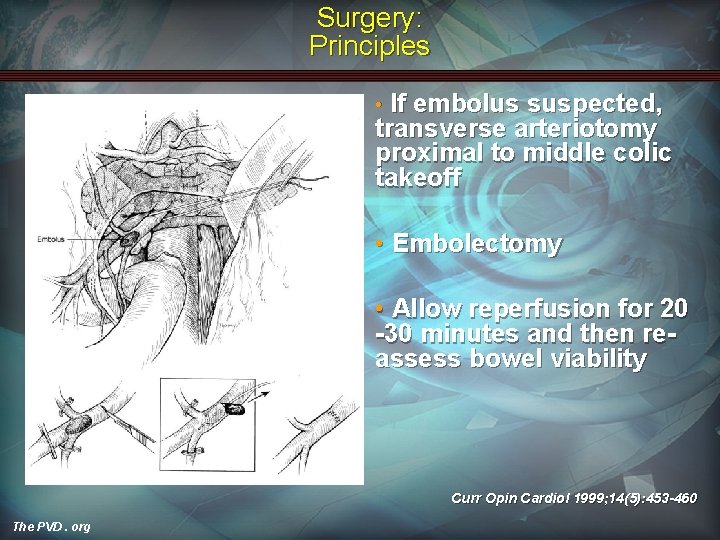
Surgery: Principles If embolus suspected, transverse arteriotomy proximal to middle colic takeoff • • Embolectomy • Allow reperfusion for 20 -30 minutes and then reassess bowel viability Curr Opin Cardiol 1999; 14(5): 453 -460 The PVD. org

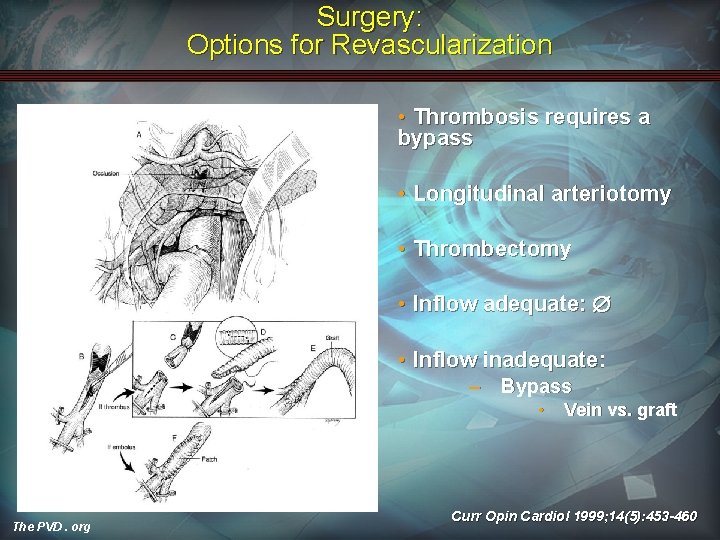
Surgery: Options for Revascularization • Thrombosis requires a bypass • Longitudinal arteriotomy • Thrombectomy • Inflow adequate: • Inflow inadequate: – Bypass • The PVD. org Vein vs. graft Curr Opin Cardiol 1999; 14(5): 453 -460

Surgery: Options for Revascularization The PVD. org Curr Opin Cardiol 1999; 14(5): 453 -460

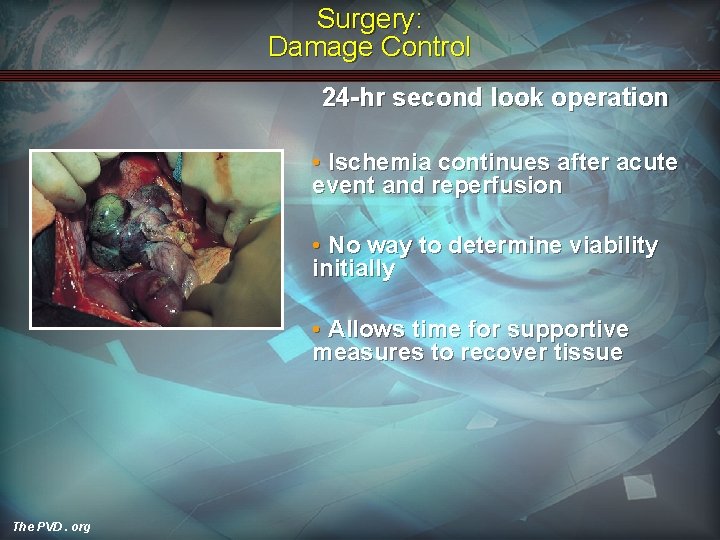
Surgery: Damage Control 24 -hr second look operation • Ischemia continues after acute event and reperfusion • No way to determine viability initially • Allows time for supportive measures to recover tissue The PVD. org

Surgery: Options Case Reports • Angiography + Laparoscopy The PVD. org

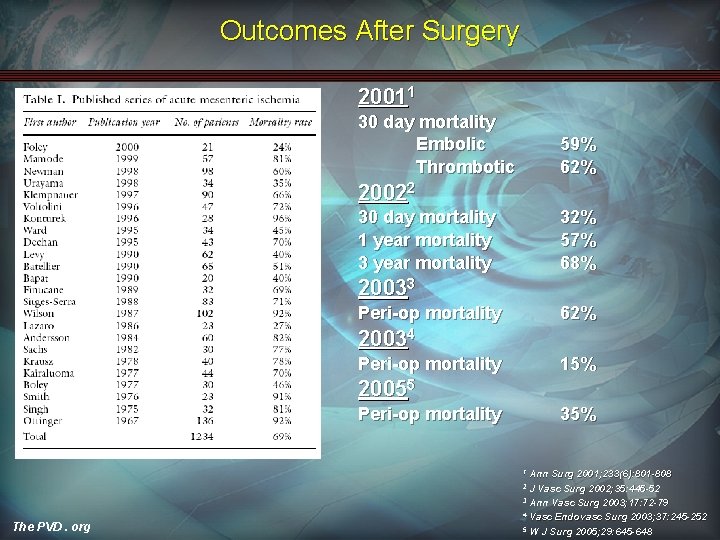
Outcomes After Surgery 20011 30 day mortality Embolic Thrombotic 59% 62% 20022 30 day mortality 1 year mortality 32% 57% 68% 20033 Peri-op mortality 62% 20034 Peri-op mortality 15% 20055 Peri-op mortality 35% Ann Surg 2001; 233(6): 801 -808 J Vasc Surg 2002; 35: 445 -52 3 Ann Vasc Surg 2003; 17: 72 -79 4 Vasc Endovasc Surg 2003; 37: 245 -252 5 W J Surg 2005; 29: 645 -648 1 2 The PVD. org

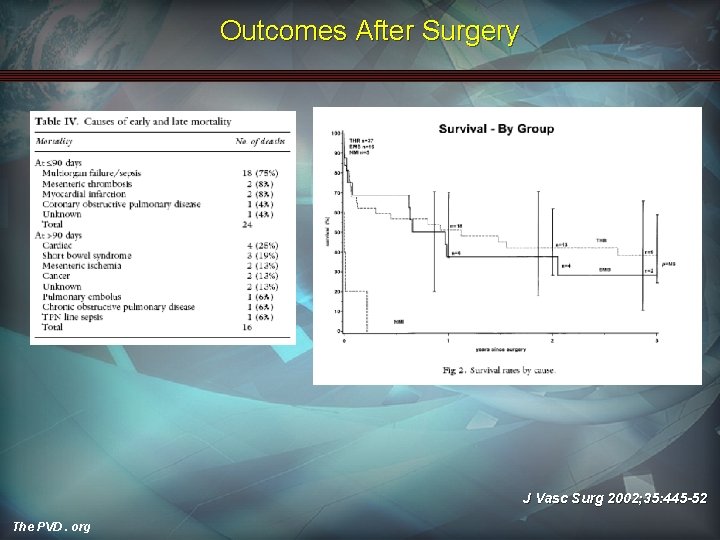
Outcomes After Surgery J Vasc Surg 2002; 35: 445 -52 The PVD. org

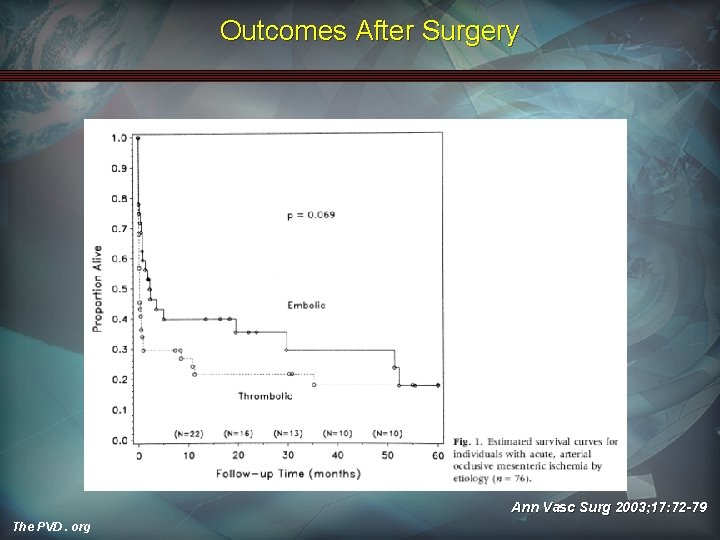
Outcomes After Surgery Ann Vasc Surg 2003; 17: 72 -79 The PVD. org

Outcomes • TPN dependence: – • • 8 -31%1, 2 Significant morbidity No studies comparing stenting vs. open surgery No studies comparing embolectomy vs. bypass Early intervention most important factor for survival 1 J 2 The PVD. org Vasc Surg 2002; 35: 445 -52 Ann Surg 2001; 233: 801 -808

Management of Mesenteric Vein Thrombosis • • • 5 -10% of mesenteric ischemia Subacute vs. chronic Better prognosis Diagnosis: CT scanning, venography Therapy: anticoagulation, thrombolysis – • • • surgery if bowel compromise suspected No role for venous thrombectomy Long-term anticoagulation Hypercoaguable workup 1 JVIR 2 The PVD. org 2005; 16: 317 -329 Surg Lap Endo Perc Tech 2003; 13(3): 215 -217

What Should You Do? Supportive • • • IV heparin Broad-spectrum antibiotics Hemodynamic optimization ― Volume status ― Cardiac function The PVD. org

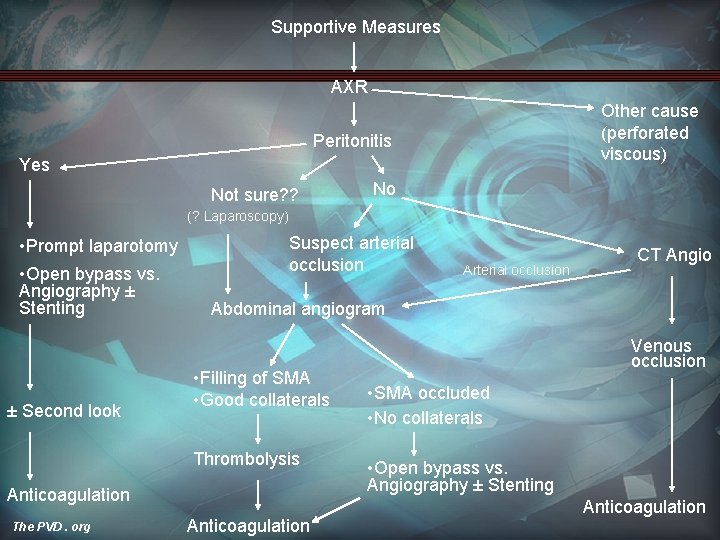
Supportive Measures AXR Other cause (perforated viscous) Peritonitis Yes Not sure? ? No (? Laparoscopy) • Prompt laparotomy • Open bypass vs. Angiography ± Stenting ± Second look Suspect arterial occlusion CT Angio Abdominal angiogram • Filling of SMA • Good collaterals Thrombolysis Anticoagulation The PVD. org Arterial occlusion Anticoagulation Venous occlusion • SMA occluded • No collaterals • Open bypass vs. Angiography ± Stenting Anticoagulation