ACUTE INFLAMMATION ACUTE INFLAMMATION COMPONENT Definition Acute inflammation












- Slides: 39

ACUTE INFLAMMATION

ACUTE INFLAMMATION COMPONENT Definition: Acute inflammation is a rapid response to an injurious agent that serves to deliver mediators of host defense-leukocytes and plasma proteins-to the site of injury. Acute inflammation has three major components: (1) alterations in vascular caliber that lead to an increase in blood flow; (2) structural changes in the microvasculature that permit plasma proteins and leukocytes to leave the circulation; (3) emigration of the leukocytes from the microcirculation, their accumulation in the focus of injury, and their activation to eliminate the offending agent. (Robbins, 7 th ed. ) When a host encounters an injurious agent, such as an infectious microbe or dead cells, phagocytes that reside in all tissues try to get rid of these agents. At the same time, phagocytes and other host cells react to the presence of the foreign or abnormal substance by liberating cytokines, lipid messengers, and the various other mediators of inflammation.

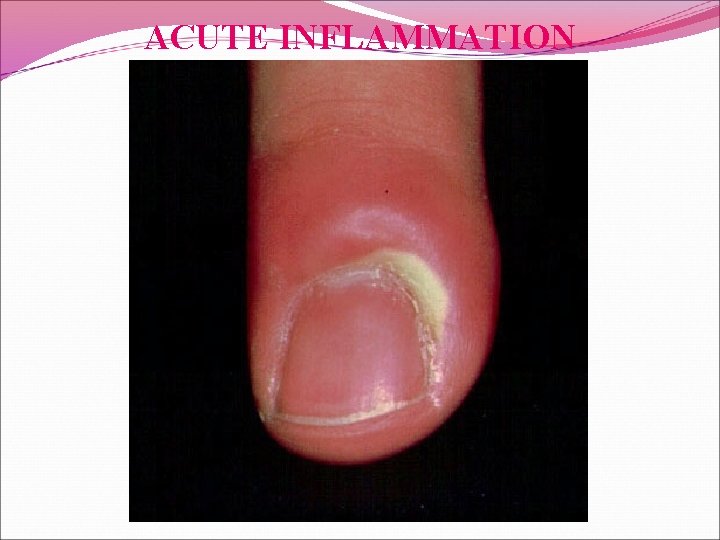
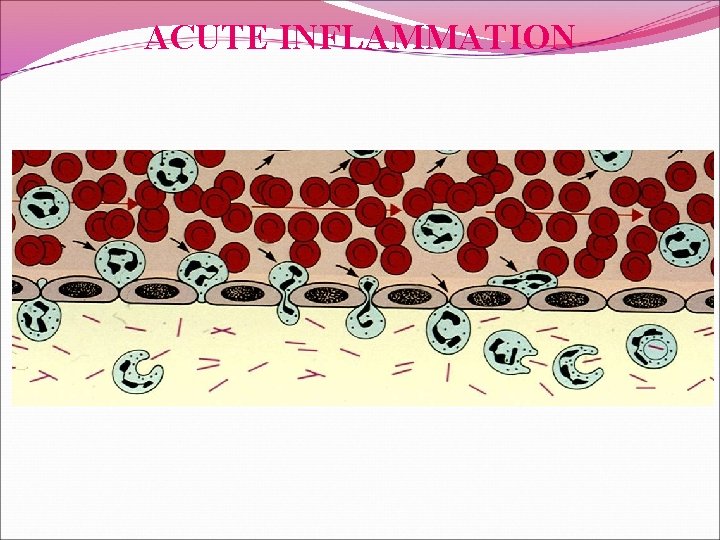
PLASMA PROTIEN & ACUTE INFLAMMATION Plasma proteins leave the vessels, most commonly through widened interendothelial cell junctions of the venules. The redness (rubor), warmth (calor), and swelling (tumor) of acute inflammation are caused by the increased blood flow and edema. Circulating leukocytes, initially predominantly neutrophils, adhere to the endothelium via adhesion molecules, transmigrate across the endothelium, and migrate to the site of injury under the influence of chemotactic agents. Leukocytes that are activated by the offending agent and by endogenous mediators may release toxic metabolites and proteases extracellularly, causing tissue damage. During the damage, and in part as a result of the liberation of prostaglandins, neuropeptides, and cytokines, one of the local symptoms is pain (dolor. (

Plasma proteins leave the vessels, most commonly through widened interendothelial cell junctions of the venules. The redness (rubor), warmth (calor), and swelling (tumor) of acute inflammation are caused by the increased blood flow and edema. Circulating leukocytes, initially predominantly neutrophils, adhere to the endothelium via adhesion molecules, transmigrate across the endothelium, and migrate to the site of injury under the influence of chemotactic agents. Leukocytes that are activated by the offending agent and by endogenous mediators may release toxic metabolites and proteases extracellularly, causing tissue damage. During the damage, and in part as a result of the liberation of prostaglandins, neuropeptides, and cytokines, one of the local symptoms is pain (dolor. (

ACUTE INFLAMMATION Mediators INJURY Acute inflammation

ACUTE INFLAMMATION

ACUTE INFLAMMATION

ACUTE INFLAMMATION SEQUENCE OF EVENTS Vasoconstriction Vasodilation Increased vascular permeability Hemoconcentration and stasis Leukocyte Adhesion Transmigration Chemotaxis Aggregation Phagocytosis

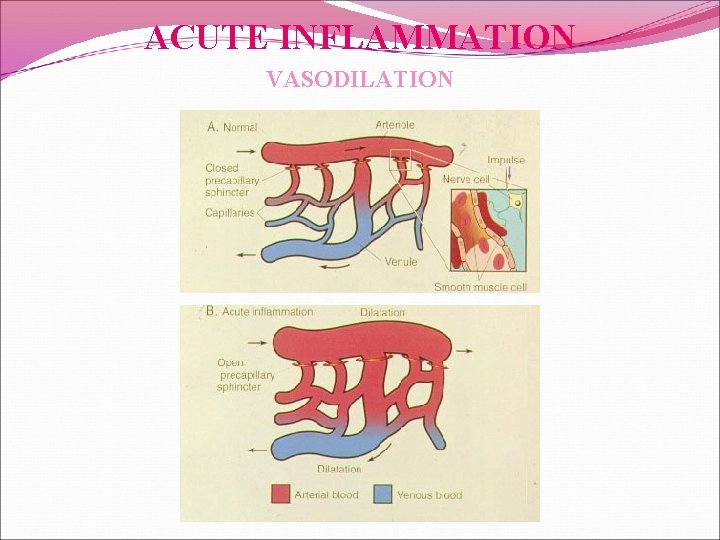
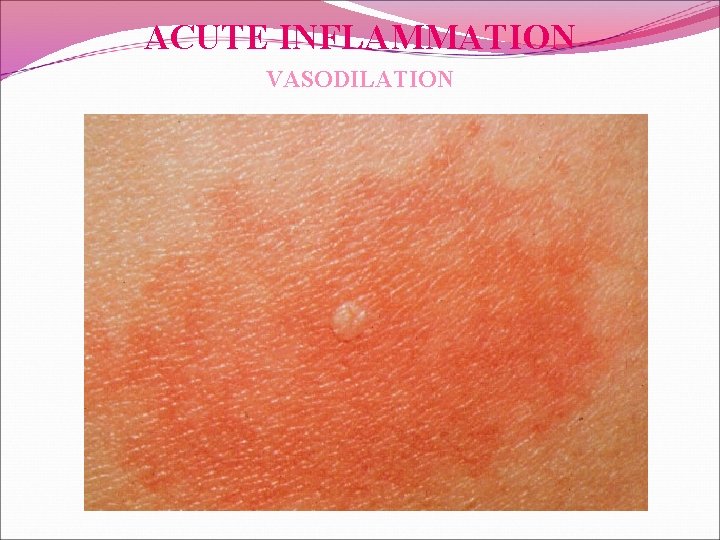
ACUTE INFLAMMATION VASODILATION

ACUTE INFLAMMATION VASODILATION

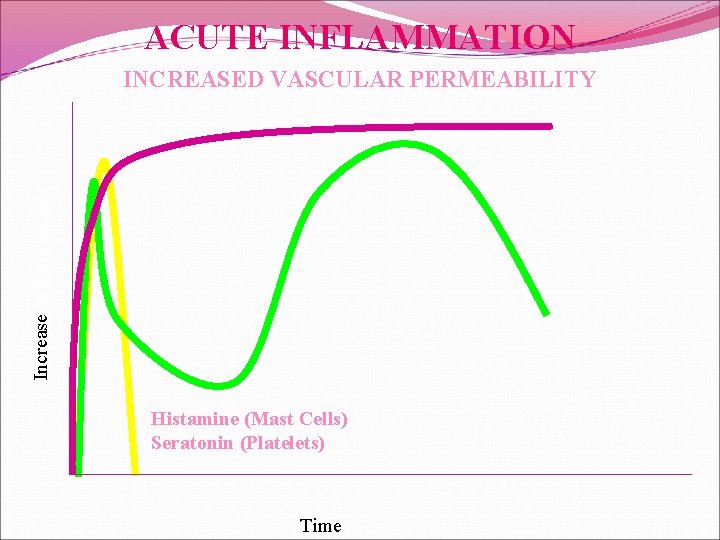
ACUTE INFLAMMATION Increase in Permeability INCREASED VASCULAR PERMEABILITY Histamine (Mast Cells) Seratonin (Platelets) Time

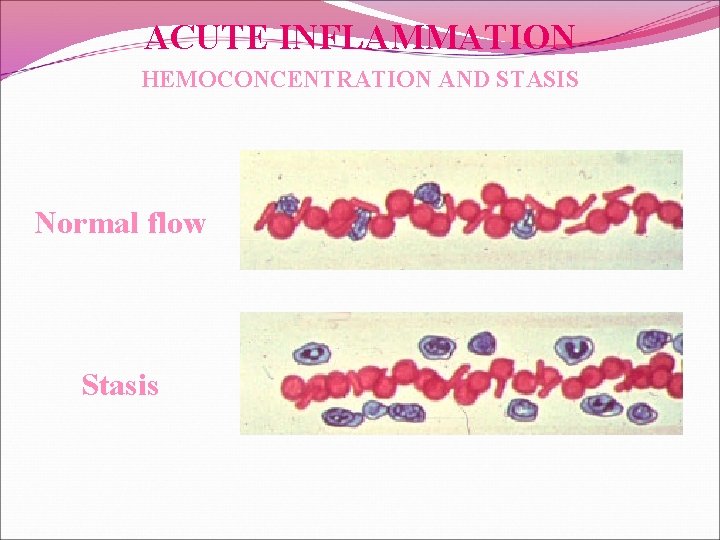
ACUTE INFLAMMATION HEMOCONCENTRATION AND STASIS Normal flow Stasis

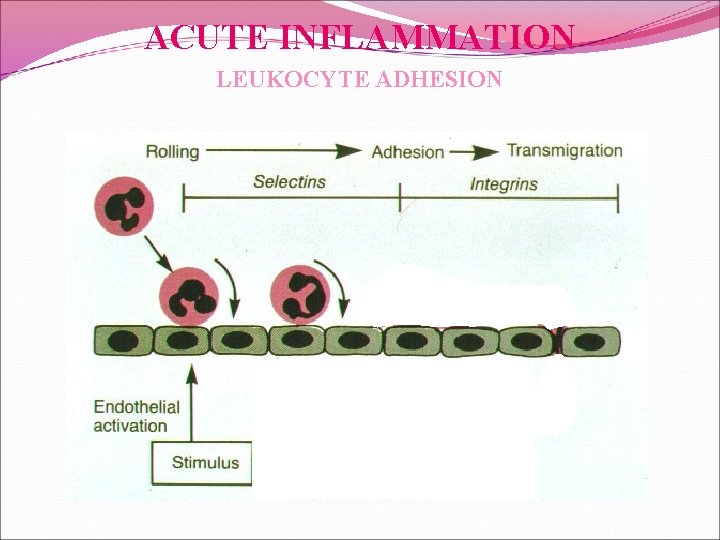
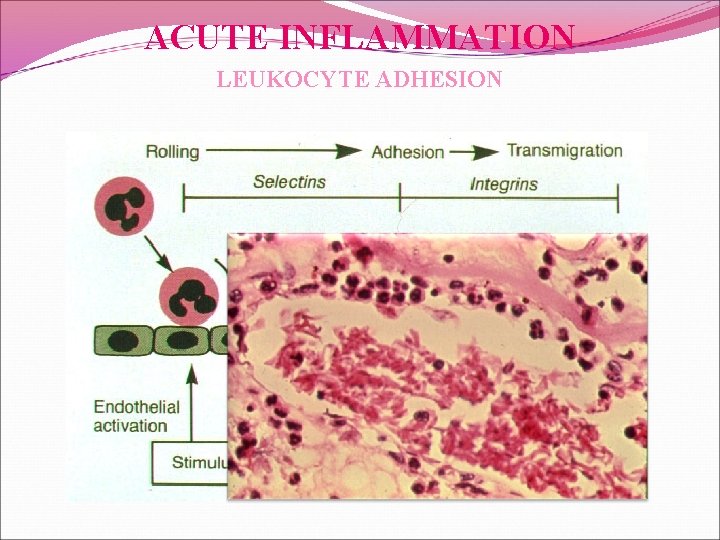
ACUTE INFLAMMATION LEUKOCYTE ADHESION

ACUTE INFLAMMATION LEUKOCYTE ADHESION

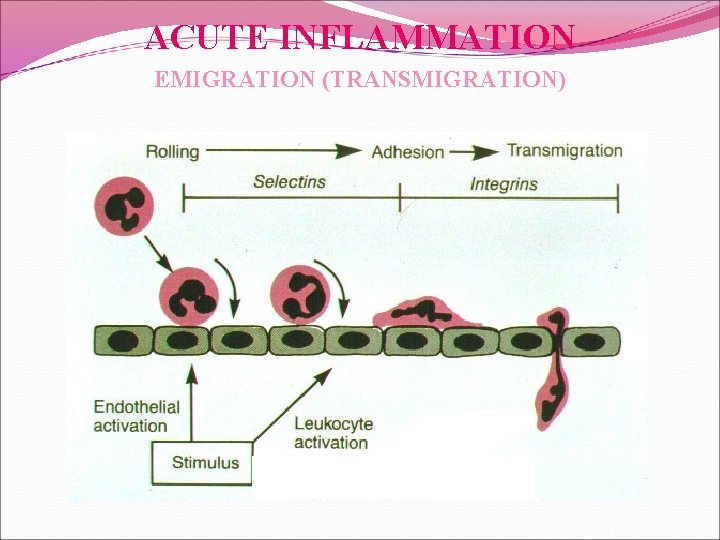
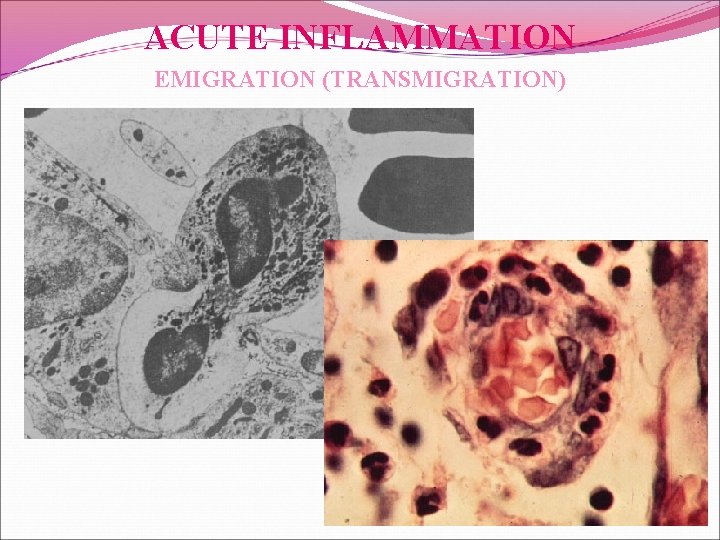
ACUTE INFLAMMATION EMIGRATION (TRANSMIGRATION)

ACUTE INFLAMMATION EMIGRATION (TRANSMIGRATION)

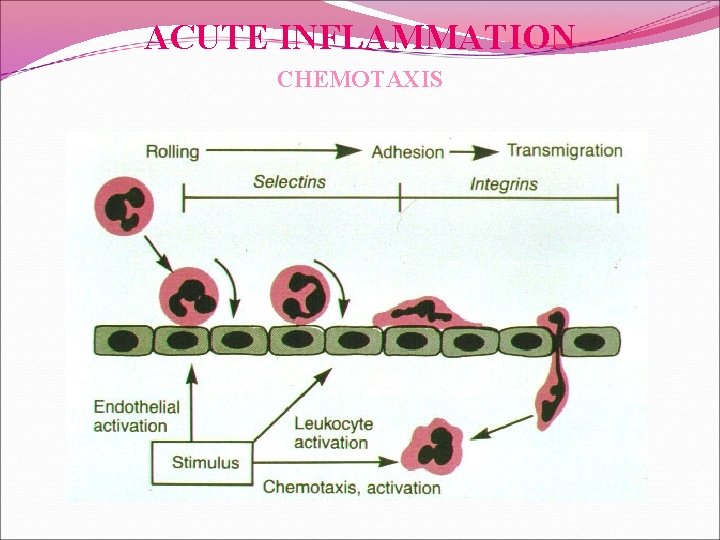
ACUTE INFLAMMATION CHEMOTAXIS

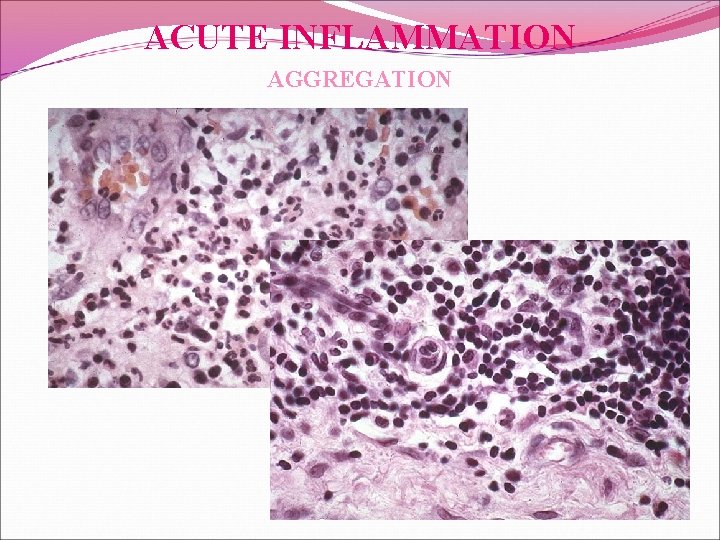
ACUTE INFLAMMATION AGGREGATION

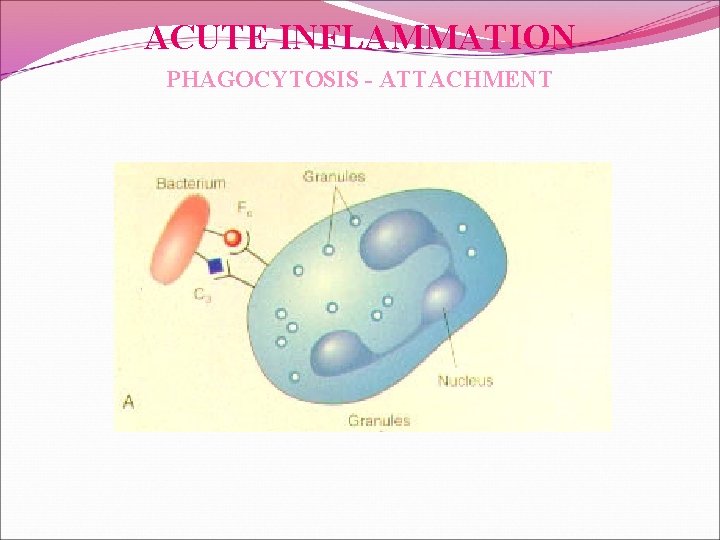
ACUTE INFLAMMATION PHAGOCYTOSIS - ATTACHMENT

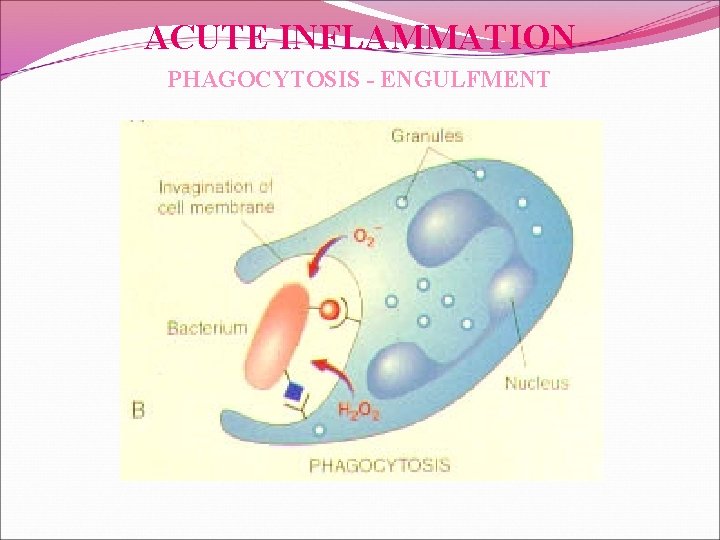
ACUTE INFLAMMATION PHAGOCYTOSIS - ENGULFMENT

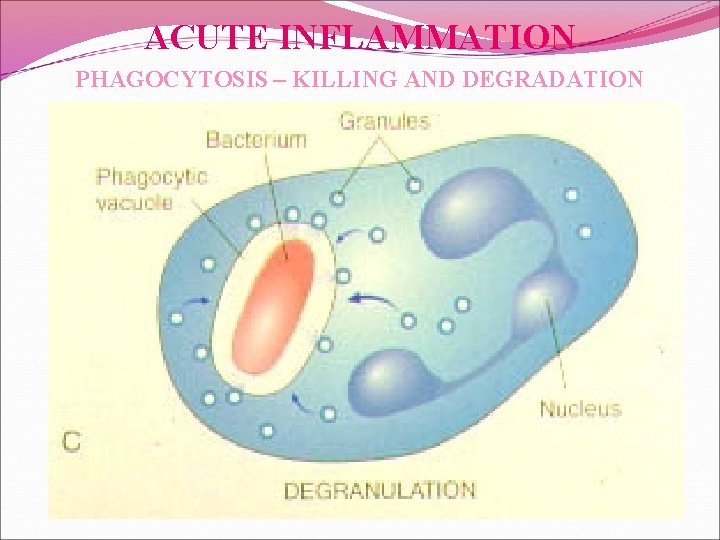
ACUTE INFLAMMATION PHAGOCYTOSIS – KILLING AND DEGRADATION

ACUTE INFLAMMATION

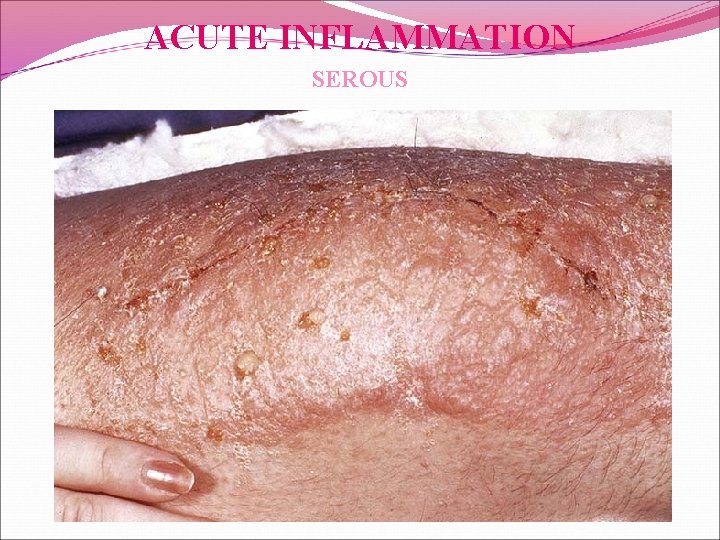
ACUTE INFLAMMATION PATTERNS Serous Catarrhal Fibrinous Hemorrhagic Suppurative Gangrenous Pseudomembranous

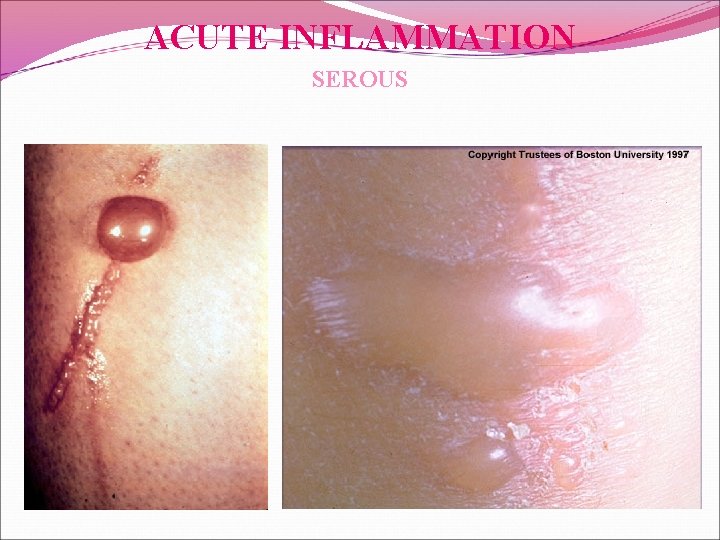
ACUTE INFLAMMATION SEROUS

ACUTE INFLAMMATION SEROUS

ACUTE INFLAMMATION CATARRHAL

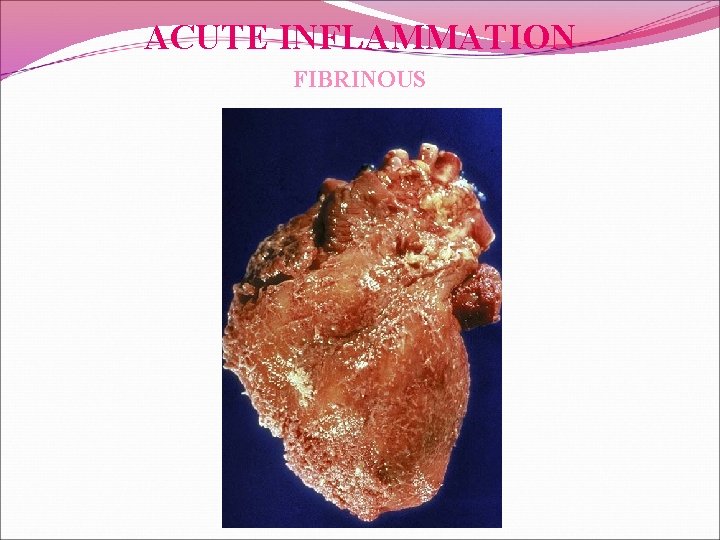
ACUTE INFLAMMATION FIBRINOUS

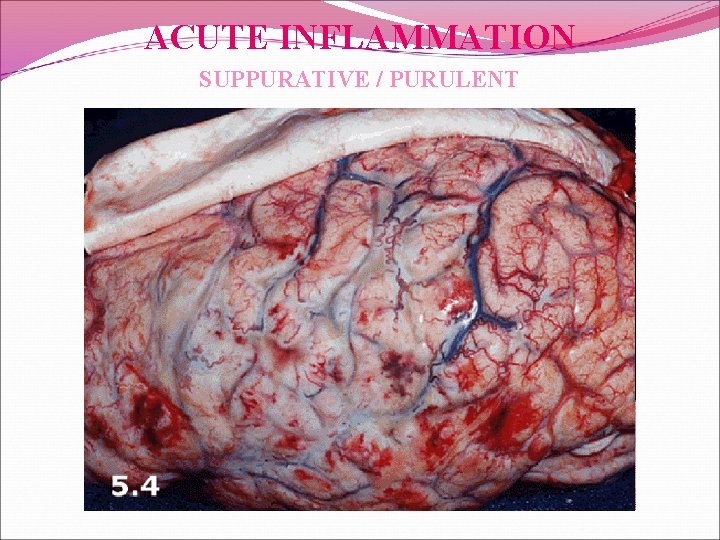
ACUTE INFLAMMATION SUPPURATIVE / PURULENT

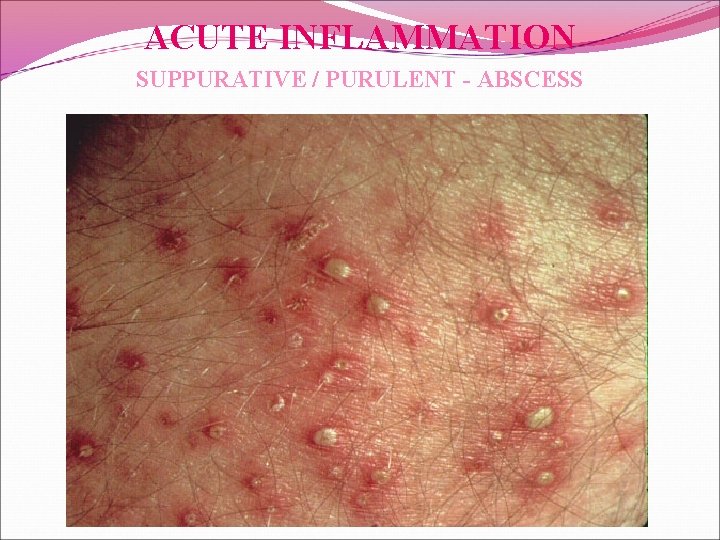
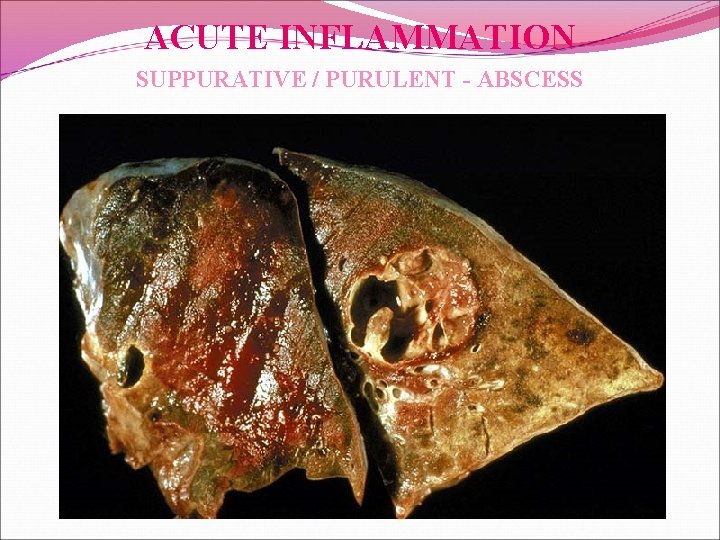
ACUTE INFLAMMATION SUPPURATIVE / PURULENT - ABSCESS

ACUTE INFLAMMATION SUPPURATIVE / PURULENT - ABSCESS

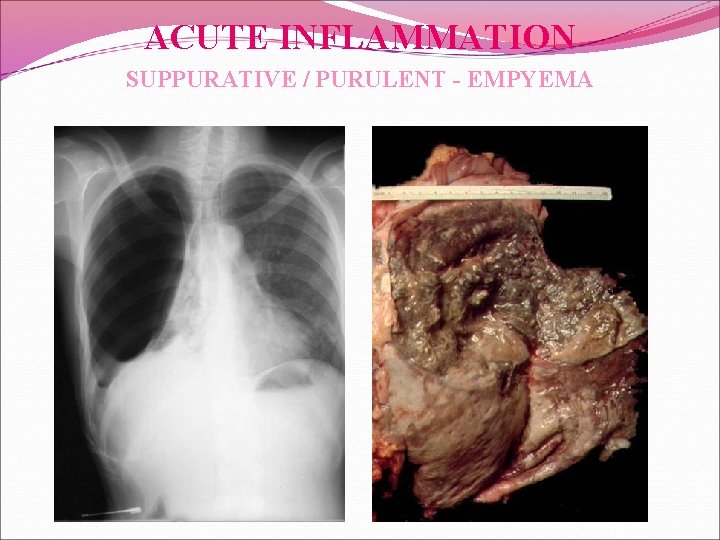
ACUTE INFLAMMATION SUPPURATIVE / PURULENT - EMPYEMA

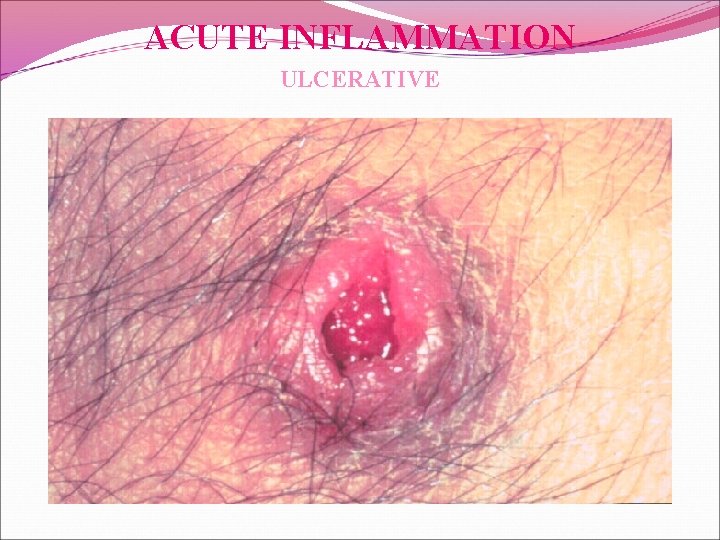
ACUTE INFLAMMATION ULCERATIVE

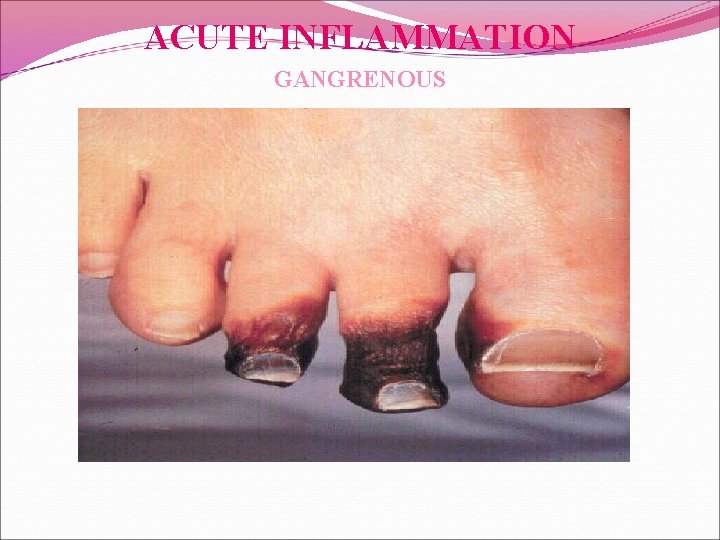
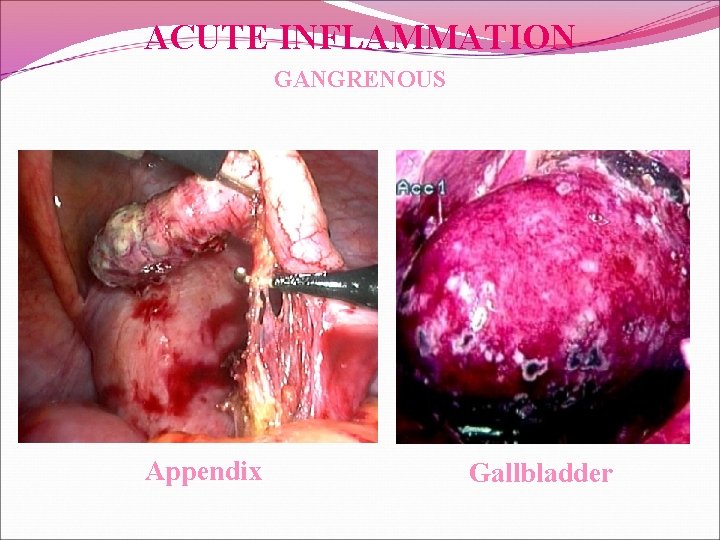
ACUTE INFLAMMATION GANGRENOUS

ACUTE INFLAMMATION GANGRENOUS Appendix Gallbladder

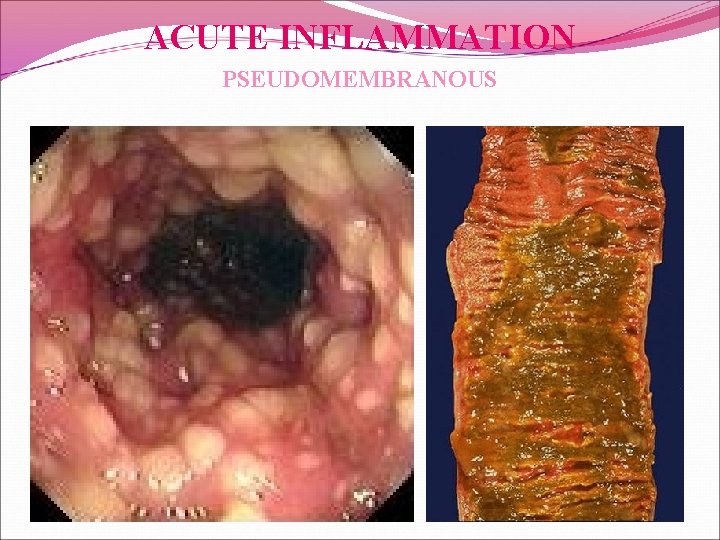
ACUTE INFLAMMATION PSEUDOMEMBRANOUS

ACUTE INFLAMMATION LOCAL MANIFESTATIONS Heat Redness Swelling Pain Loss of function

ACUTE INFLAMMATION SYSTEMIC MANIFESTATIONS Fever Chills Myalgia Discomfort

ACUTE INFLAMMATION LABORATORY MANIFESTATIONS Leukocytosis (granulocytosis vs. lymphocytosis) Elevated serum acute phase proteins (C-reactive protein, fibrinogen, etc) Increased ESR (erythrocyte sedimentation rate) Hypercoagulability

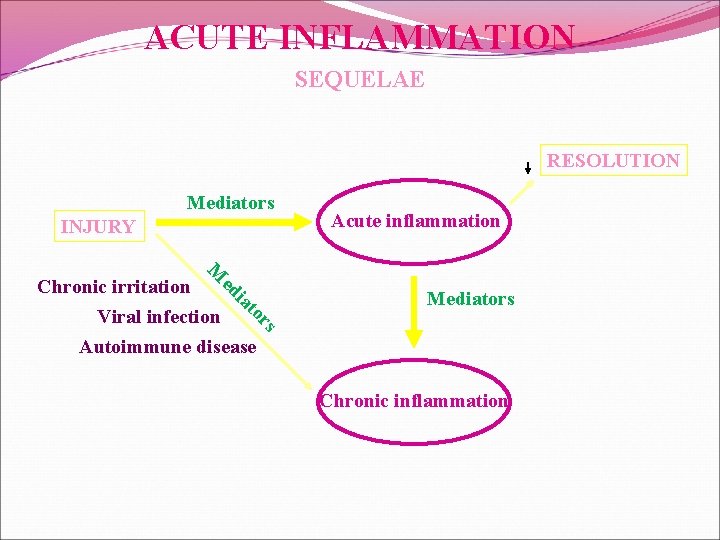
ACUTE INFLAMMATION SEQUELAE RESOLUTION Mediators INJURY Acute inflammation M Mediators rs o at i ed Chronic irritation Viral infection Autoimmune disease Chronic inflammation