2016 AAFP Family Medicine Global Health Workshop 9816

2016 AAFP Family Medicine Global Health Workshop (9/8/16) Reimagining Global Health Engagement by the Do. D FBCH – HMC Partnership FBCH Family Medicine Residency Jaime Wong-Lopez, MD Andrew Baldwin, MD William Bynum, MD

Activity Disclaimer ACTIVITY DISCLAIMER It is the policy of the AAFP that all individuals in a position to control content disclose any relationships with commercial interests upon nomination/invitation of participation. Disclosure documents are reviewed for potential conflicts of interest (COI), and if identified, conflicts are resolved prior to confirmation of participation. Only those participants who had no conflict of interest or who agreed to an identified resolution process prior to their participation were involved in this CME activity. Jaime Wong-Lopez, MD Andrew Baldwin, MD William Bynum, MD have indicated they have no relevant financial relationships to disclose. 2

Disclaimer: “The views expressed in this presentation are those of the authors and do not reflect the official policy of the Department of the Army/Navy/Air Force, Department of Defense, or the U. S. Government. "

Academic Medicine. 2015 Dec 1.

Summary Guidelines for Implementing Short-Term Experience in Global Health (STEGH) Principles • Principle 1: Skills building in cross-cultural effectiveness and cultural humility are critical components of successful STEGHs • Principle 2: STEGHs must foster bidirectional participatory relationships • Principle 3: STEGHs should be part of longitudinal engagement that promotes sustainable local capacity building and health systems strengthening • Principle 4: STEGHs must be embedded within established, community-led efforts focused on sustainable development and measurable community health gains Academic Medicine. 2015 Dec 1.
El Salvador, Central America

San Salvador, El Salvador

Hospital Militar Central (HMC)

Hospital Militar Central (HMC) “Dios, Patria, Salud” (“God, Country, Health”)

2015 FBCH visit to HMC • Needs assessment by 2 faculty and 2 residents from FBCH • HMC requested: 1) med dispensing carts, 2) developing an adverse event reporting and safety program • Survey: HMC staff committed to patient safety but many barriers to error reporting

2015 observations of HMC assets: • • Excellent patient care (exam skills vs. studies) Comprehensive care: inpatient / outpatient Strong preventative & primary care medicine Adequate subspecialty support Basic electronic medical record (EMR) Strong desire to provide safe, competent care Strong commitment to continuous improvement

HMC Faculty, Residents, Nurses

May 2015 HMC visit to FBCH • Subject matter exchange: 1) patient safety 2) antibiotic stewardship 3) disaster preparedness 4) learning environment • Help getting med dispensing carts…

2015 HMC visit to FBCH http: //www. fbch. capmed. mil/News. Room/20150529_02. aspx

Jan 2016 FBCH visit to HMC FBCH Fam. Med Residency: Andy Baldwin, MD (Faculty) CDR MC USN Will Bynum, MD (Faculty) Capt USAF MC Brian Mc. Mullin, MD (PGY 3) Capt USAF MC Jaime Wong-Lopez, MD (PGY 2) LCDR MC USN 12 AF/SG, Monthan AFB International Health Specialist: Janet Cary, RN Maj USAF MSC

Purpose of 2016 visit (from 2015 needs assessment) Continue building bidirectional institutional relationship #1: Establish an adverse event reporting system #2: Encourage change towards culture of safety #3: Assess & optimize learning environment #4: Brainstorm future faculty development

Objective #1: Establish an Adverse Event Reporting System • Elicited electronic survey input from HMC nurses, residents, faculty • Developed an adverse event reporting tool, with HMC tech support to make electronic link on all hospital terminals • Identified a pilot group (Internal Medicine) • Proposed an Adverse Event Committee • Offered assistance with analyzing the data collected


Pre-trip electronic survey results • Adverse event reporting seen as important across all jobs • Significant barriers: 1) fear of punishment 2) effect on professional reputation 3) no standardized reporting system in place 4) lack of institutional response to prevent future events • Electronic tool preferred over paper-based • Great interest in tracking & prevention (eg, Committee)

“The beatings will continue, until morale improves” • HMC residents punished (extra work shifts), when blamed for errors: • “Samingo” = 48 -hr shift, Saturday-Sunday (“Sabado”-“Domingo”) • Stay on-duty until patient involved is discharged

HMC Administrators & Faculty

Observed culture change • HMC briefly abolished punishment system after 2015 FBCH visit to HMC, and they received more error reports • Attributed to higher # of actual errors committed (instead of increased willingness to report), and punishment system restarted • Through discussion with us, they recognized this bias, and considered abolishing punishment system again

HMC Residents

Developing a Reporting Tool


Developing a Reporting Tool

Objective #2: Encourage change towards culture of safety • Analyzed electronic survey input from HMC nurses, residents, faculty • Conducted workshops (adapted each day): 1) Why reporting errors is important 2) The emotions associated with making errors 3) Systematic approach to analyzing errors • In mixed and separate groups, met with nurses, residents, and faculty to discuss culture of safety

Conducting Workshops

Incidentes y eventos adversos: la parte visible de la inseguridad del paciente 29
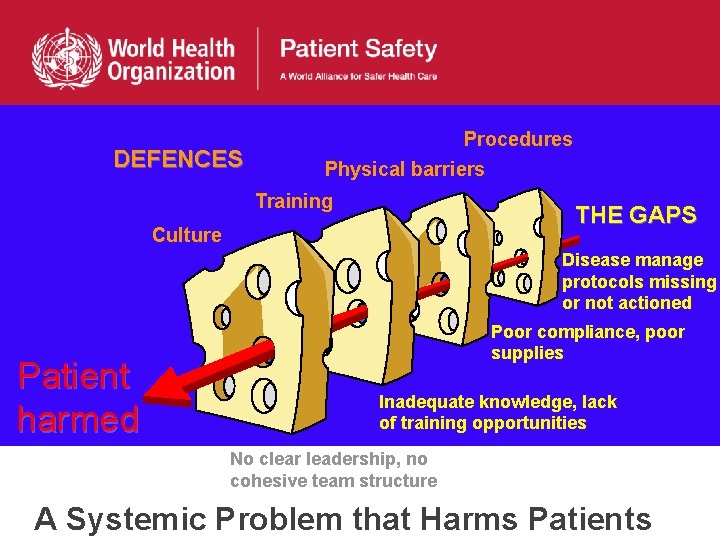
DEFENCES Procedures Physical barriers Training THE GAPS Culture Disease manage protocols missing or not actioned Patient harmed Poor compliance, poor supplies Inadequate knowledge, lack of training opportunities No clear leadership, no cohesive team structure A Systemic Problem that Harms Patients

Conducting Workshops
Escondite final Sitio de error Un Cuento Personal

Shame “I’m not ______ enough. ” The focus is on the self and not the behavior The person feels small, worthless, and exposed Stimulates a desire to hide and avoid responsibility Prevents engagement with the learning process Med Educ 2014; 48; 1045 -54

Guilt The focus is on the behavior and not the self “That thing I did was bad. But I am not bad. Most often stimulates reparative action Med Educ 2014; 48; 1045 -54

Small-group discussions, mixed staff

Objective #3: Assess & optimize learning environment • Observed two Morbidity & Mortality Conferences (M&Ms): 1) Surgery, 2) Internal Med • HMC staff applied principles learned during workshops to build M&Ms • Provided guidance for conducting and improving M&Ms • Workshop on root cause analysis of errors • Participated in inpatient rounds

HMC Surgical Morbidity & Mortality Conference Focus of M&M was the error that occurred; not how to fix/avoid it
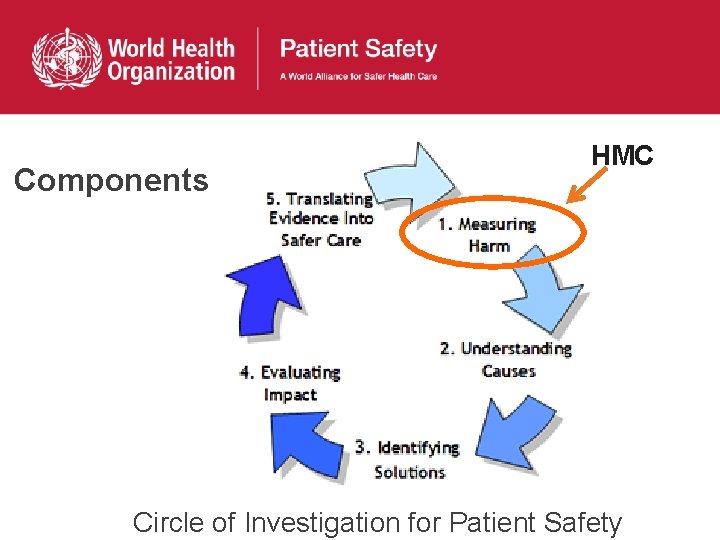
Components HMC Circle of Investigation for Patient Safety
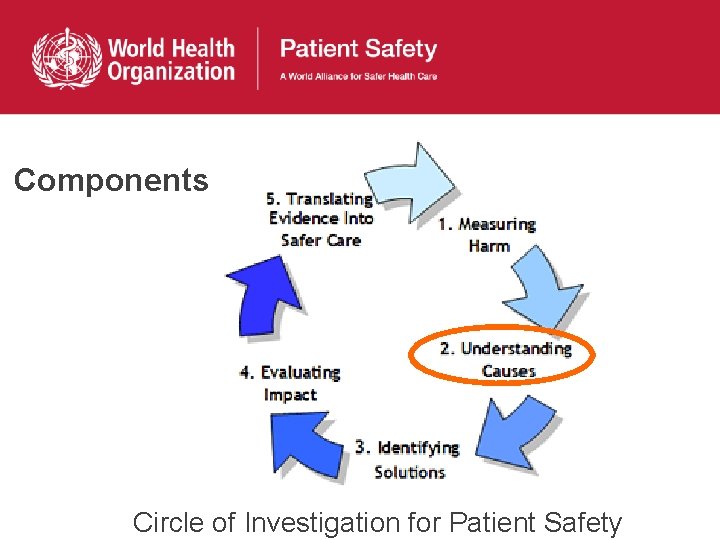
Components Circle of Investigation for Patient Safety
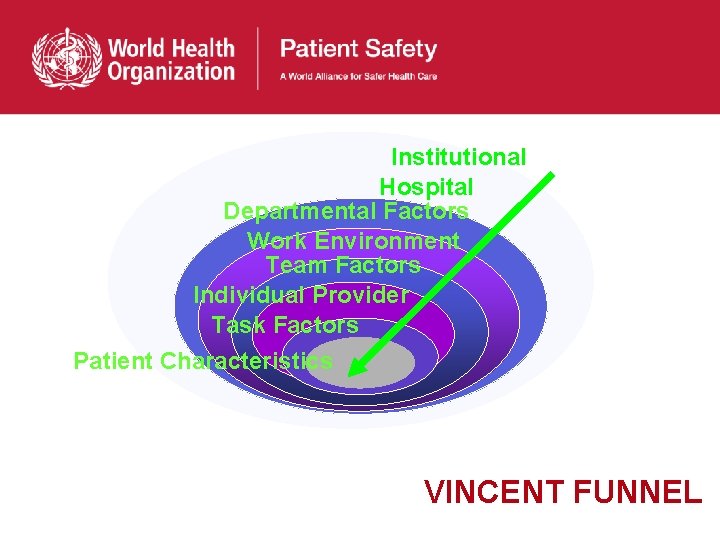
Institutional Hospital Departmental Factors Work Environment Team Factors Individual Provider Task Factors Patient Characteristics VINCENT FUNNEL

Head of Lab Services

HMC Ward Rounds: Learners

Observed culture change • Punishment system counterproductive: no lessons learned and/or more errors • Need better way to encourage reporting, address guilt/shame, and promote root cause analysis • After adverse events, residents could prepare an associated M&M, instead of made to work extra shifts

Objective #4: Brainstorm future faculty development • Met with residents and staff to discuss the learning environment and teaching at HMC (break -outs: nurses, residents, attendings) • Participated in inpatient rounds • Identified areas for future collaboration to enhance teaching and develop an optimal learning environment

HMC Faculty Development Faculty to Faculty

HMC Faculty Development

Observed culture change • “What do we do with a resident who keeps making the same mistake (besides extra work shifts)? ” • Introduced concepts of: 1) remediation 2) plan of supervision 3) delayed progression • Learn & improve instead of punish

HMC Ward Rounds: Teachers

Morale building with HMC faculty & residents

Morale building with HMC faculty & residents

Resident Collar Device Gifting

Final Brief for HMC Director

Next Steps: • Pilot the Reporting Tool and Committee • Collaborate on data analysis (remotely) • Expand adverse event system to other departments • Explore potential for Resident and Faculty rotations

Para saber más: http: //www. who. int/patientsafety/research/ methodological_guide/PSP_Meth. Guid. pdf
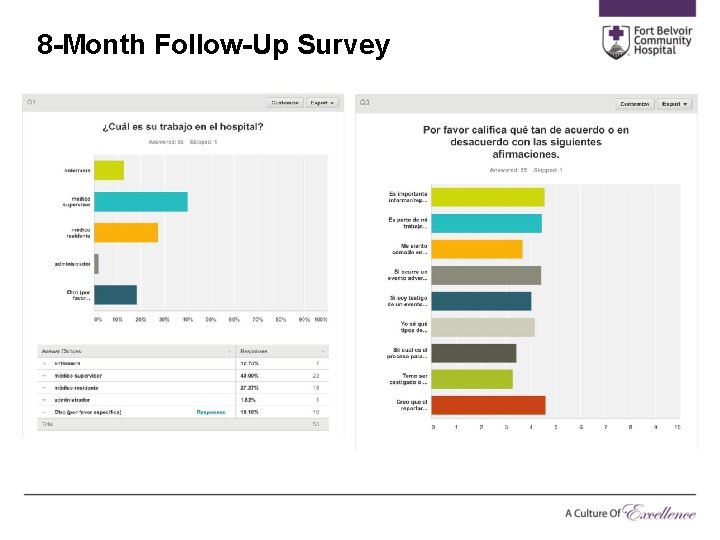
8 -Month Follow-Up Survey

8 -Month Follow-Up Survey
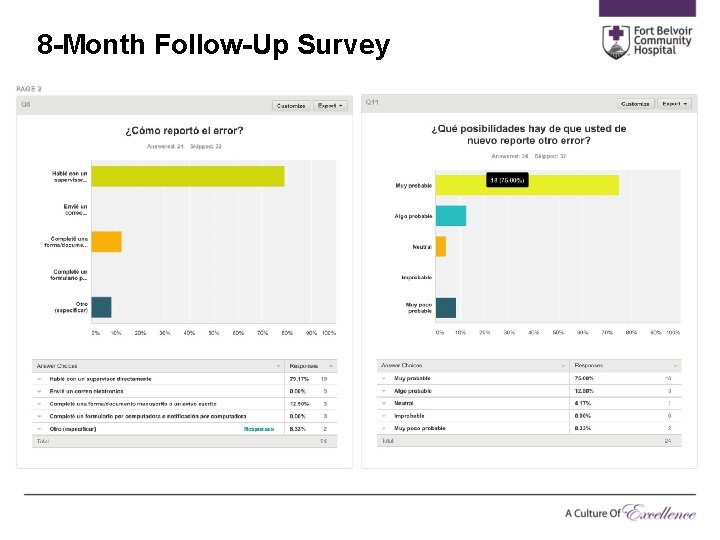
8 -Month Follow-Up Survey

Continuing the Partnership • HMC visit to FBCH (Aug 2016): 1) surgical Universal Protocol, time-out 2) M&M, PI/QI, PDSA 3) teaching/feedback by residents/faculty 4) HMC talks on their healthcare system, Zika • FBCH visit to HMC (Dec 2016): 1) updates on patient safety, learning environment, faculty development 2) new goals per HMC (eg, professionalism)

HMC visit to FBCH (Aug 2016)

Summary Guidelines for Implementing Short-Term Experience in Global Health (STEGH) Principles • Principle 1: Skills building in cross-cultural effectiveness and cultural humility are critical components of successful STEGHs • Principle 2: STEGHs must foster bidirectional participatory relationships • Principle 3: STEGHs should be part of longitudinal engagement that promotes sustainable local capacity building and health systems strengthening • Principle 4: STEGHs must be embedded within established, community-led efforts focused on sustainable development and measurable community health gains Academic Medicine. 2015 Dec 1.

Followed the 4 Principles 1) Cultural humility: our objectives met their goals; we shared stories about errors in our system, and our associated feelings; all discussions either in Spanish or with English-Spanish interpretation by our team 2) Bidirectional participation: trust relationship, built over time with multiple, short trips 3) Sustainable local capacity building: introduced WHO patient safety resources; adapted daily workshops to address their needs/ideas; encouraged non-hierarchical discussion b/w nurses, residents, faculty 4) Measurable community health gains: adverse event tracking/analysis system, standing Safety Committee, regular M&Ms, improved learning environment, new focus on faculty development

Got Coffee? Or Questions?
- Slides: 62



















































































