COPD Brandon Mickelsen DO Director ISU Family Medicine

COPD Brandon Mickelsen DO Director ISU Family Medicine Residency

DEFINITION • Chronic Obstructive Pulmonary Disease (COPD) is a common, preventable and treatable disease that is characterized by persistent respiratory symptoms and airflow limitation that is due to airway and/or alveolar abnormalities usually caused by significant exposure to noxious particles or gases.

DEFINITION • 2 categories • Emphysema • Chronic Bronchitis • What happens • • The airways and air sacs lose their elastic quality. The walls between many of the air sacs are destroyed. The walls of the airways become thick and inflamed. The airways make more mucus than usual and can become clogged.

EPIDEMIOLOGY • 85% from smoking • 15 -20% of smokers will develop • 4 th leading cause of death worldwide, in the next 5 years will likely become number 3

KNOWLEDGE CHECK • Which interventions decrease mortality in copd? • Which interventions decrease morbidity and improve symptoms? • How is copd diagnosed? • What is considered the gold standard source for information on COPD? • All patients with COPD, especially those younger than 45, should be considered for screening for what genetic disease? • The decisions to treat for copd is based upon which 3 factors?

DIAGNOSIS • Can the diagnosis be make clinically? • Spirometry fev 1/fvc ratio less than 70 • Draw a normal spirometry • Now draw a copd spirometry
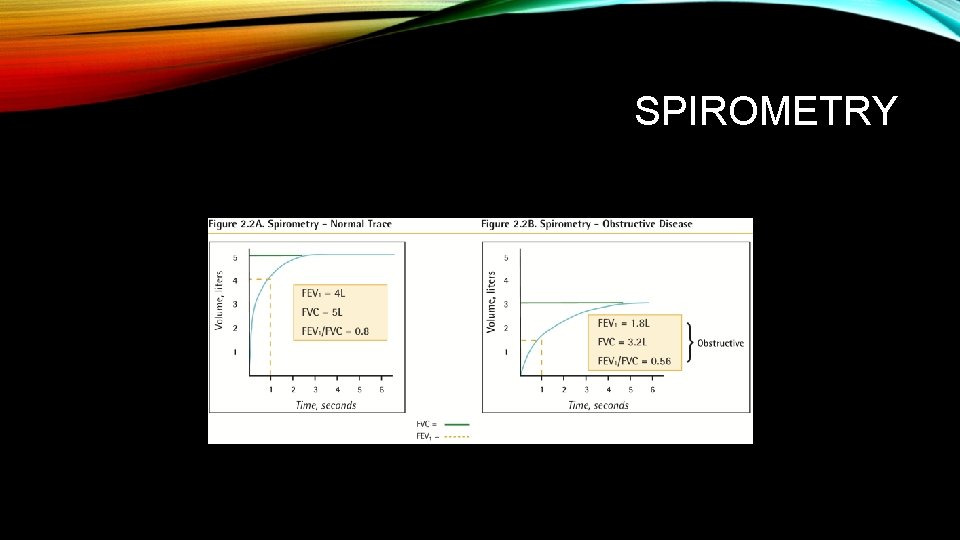
SPIROMETRY
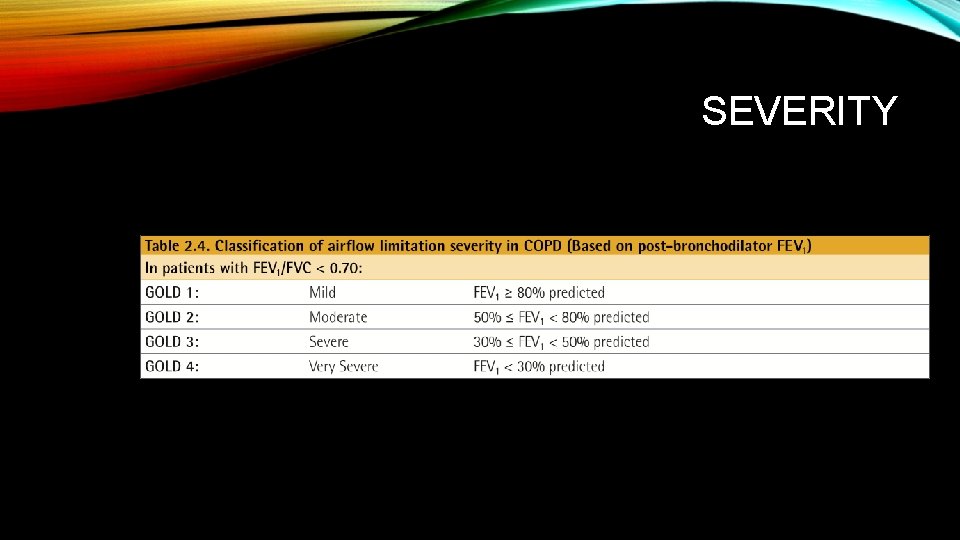

SEVERITY

Choice of thresholds ► ► ► COPD Assessment Test (CAT TM ) Chronic Respiratory Questionnaire (CCQ® ) St George’s Respiratory Questionnaire (SGRQ) Chronic Respiratory Questionnaire (CRQ) Modified Medical Research Council (m. MRC) questionnaire © 2017 Global Initiative for Chronic Obstructive Lung Disease

ABCD Assessment Tool © 2017 Global Initiative for Chronic Obstructive Lung Disease

Treatment of Stable COPD © 2017 Global Initiative for Chronic Obstructive Lung Disease

IMMUNIZATIONS • Influenza • Pneumonia

NON DRUG INTERVENTIONS • The most important intervention is smoking cessation as it improves the quality of life, reduces the risk of declining lung function and reduces mortality. • Higher levels of physical activity even in moderate to severe disease are associated with substantially better outcomes in exacerbation risk, hospital admissions and mortality. • Pulmonary Rehab is associated with reduced hospital admissions and exacerbations, particularly when it is part of an integrated care approach, NNT 4 to prevent one hospitalization • Oxygen is associated with improved survival in patients with chronic hypoxia.

DRUG THERAPY • Apart from oxygen, no drug has been shown to reduce the increased risk of death in patients with COPD. For this reason drugs are prescribed predominantly to reduce symptoms, improve functional capacity, and prevent and treat exacerbations. • SABA/SAMA • LABA/LAMA • ICS

Bronchodilators in Stable COPD © 2017 Global Initiative for Chronic Obstructive Lung Disease

Anti-inflammatory Therapy in Stable COPD © 2017 Global Initiative for Chronic Obstructive Lung Disease
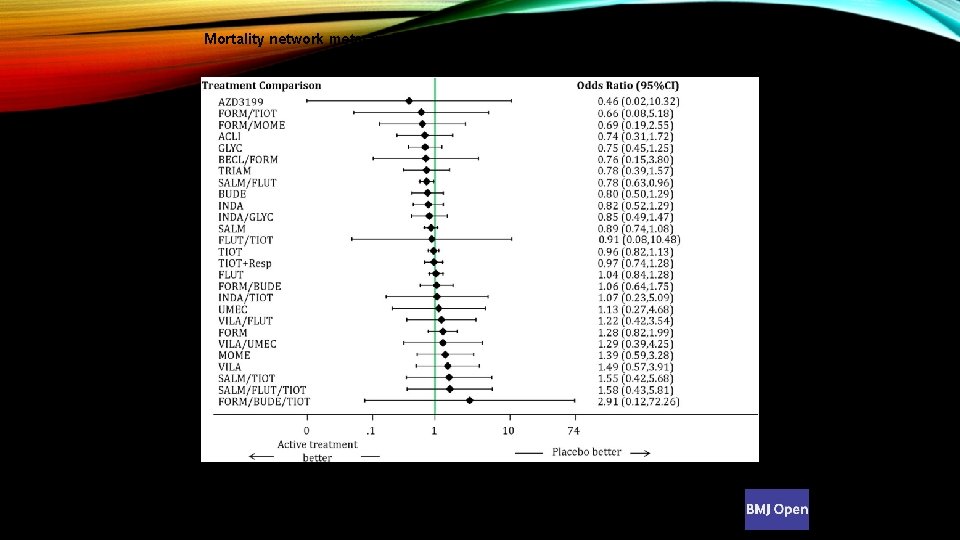
Mortality network meta-analysis forest plot for treatments compared to placebo. Andrea C Tricco et al. BMJ Open 2015; 5: e 009183 © 2015 by British Medical Journal Publishing Group

The Inhaled Route © 2017 Global Initiative for Chronic Obstructive Lung Disease

LABA • All likely equivalent • Formoterol, indacaterol and vilanterol have a relatively fast onset of action, of 5– 10 minutes, while salmeterol has a 30 -minute onset. These differences may not be important once patients are taking long-acting bronchodilators regularly. • Salmeterol, formoterol, indacaterol, vilanterol and olodaterol have statistically and clinically significant effects on lung function, exercise tolerance, SABA use, dyspnoea, quality of life and exacerbations. • LABAs are well tolerated and there are negligible differences between them in relation to adverse effects. Tremor and tachycardia appear to occur less commonly with LABAs than SABAs.

NAC • 2015 metanlysis on the role of N-acetylcysteine (NAC) in the treatment of patients with chronic bronchitis and chronic obstructive pulmonary disease (COPD) included 13 studies with a total of 4 155 subjects. Patients treated with NAC had significantly and consistently fewer exacerbations (RR 0. 75, 95% CI 0. 66 to 0. 84). This protective effect was more apparent in patients without evidence of airway obstruction. However, high doses of NAC were also effective in patients suffering from COPD diagnosed using spirometric criteria (RR 0. 75, 95% CI 0. 68 to 0. 82). • The strong signal that comes from this meta-analysis leads us to state that if a patient suffering from chronic bronchitis presents a documented airway obstruction, NAC should be administered at a dose of ≥ 1200 mg per day to prevent exacerbations, while if a patient suffers from chronic bronchitis, but is without airway obstruction, a regular treatment of 600 mg per day seems to be sufficient.

SOURCES • Anthonisen NR, Connett JE, Murray RP. Smoking and lung function of Lung Health Study participants after 11 years. Am J Respir Crit Care Med 2002; 166: 675 -9. • Wu J, Sin DD. Improved patient outcome with smoking cessation: when is it too late? Int J Chron Obstruct Pulmon Dis 2011; 6: 259 -67. • Mc. Donough M. Update on medicines for smoking cessation. Aust Prescr 2015; 38: 106 -11. • Bourbeau J. Preventing hospitalization for COPD exacerbations. Semin Respir Crit Care Med 2010; 31: 313 -20. • Waschki B, Kirsten A, Holz O, Müller KC, Meyer T, Watz H, et al. Physical activity is the strongest predictor of all-cause mortality in patients with COPD: a prospective cohort study. Chest 2011; 140: 331 -42. • Benzo R. Activity monitoring in chronic obstructive pulmonary disease. J Cardiopulm Rehabil Prev 2009; 29: 341 -7.

SOURCES CONT. • Singh D. New combination bronchodilators for chronic obstructive pulmonary disease: current evidence and future perspectives. Br J Clin Pharmacol 2015; 79: 695 -708. • Rodrigo GJ, Neffen H. A systematic review of the efficacy and safety of a fixed-dose combination of umeclidinium and vilanterol for the treatment of COPD. Chest 2015; 148: 397 -407. • http: //goldcopd. org/gold-teaching-slide-set/ • https: //www. nhlbi. nih. gov/health-topics/copd • Cazzola M, Calzetta L, Page C et al. Influence of N-acetylcysteine on chronic bronchitis or COPD exacerbations: a meta-analysis. Eur Respir Rev 2015; 24(137): 451 -61
- Slides: 22