Meritus Health Family Medicine Residency Program Presentation to









- Slides: 11

Meritus Health Family Medicine Residency Program Presentation to IGME Workgroup September 10, 2015

Introduction Meritus believes that establishing a Primary Care Residency Program in Rural Maryland will assist the State in achieving the goals of the IGME Workgroup. • Focused on Triple Aim • Curricula addresses Population Health • Funded in Equitable and Efficient Manner • Augments what is Good about Residency Training Today If Primary Care Residency Programs were established, two key challenges should be addressed: • Evaluating the need of the Program • Determining the appropriate funding 1

Meritus Health Meritus Medical Center opened in December 2010 to replace the former Washington County Hospital in Hagerstown, MD – 243 licensed beds for acute and rehabilitation care – 41 nursery bassinets – Single patient rooms Services offered include: – – – Special care nursery Level III trauma program designated as an EMS base station by the state Certified primary stroke center Wound center re-accredited with distinction in hyperbaric medicine Award-winning cardiac catheterization laboratory Outpatient needs are met through: – – John R. Marsh Cancer Center for Breast Health Total Rehab Care 19 primary and specialty care practices that make up Meritus Medical Group 2

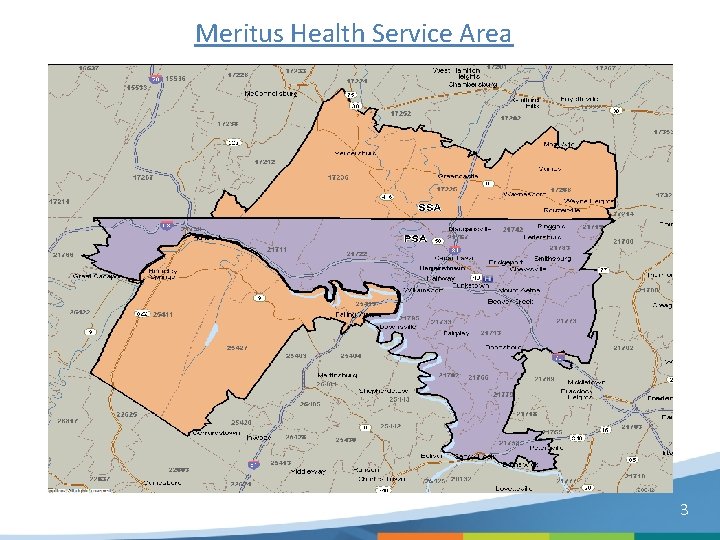
Meritus Health Service Area 3

Osteopathic Family Medicine Residency • Approval for an 18 resident program was received in June 2015 from the American Osteopathic Academy • Leadership for the new program includes Tom Gilbert, DO, Director of Medical Education • Widespread support from the medical staff • Core faculty include 6 primary care physicians, 1 hospitalist, and 1 pharmacist • Partnering with West Virginia School of Osteopathic Medicine and Mountain States OPTI 4

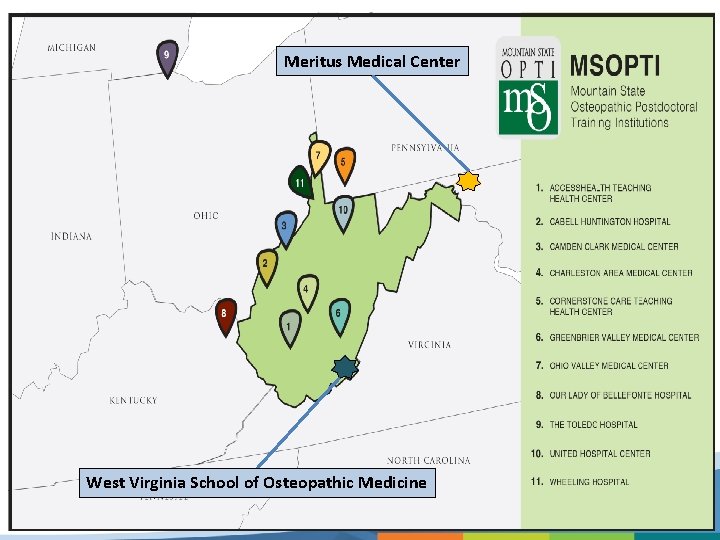
Meritus Medical Center West Virginia School of Osteopathic Medicine 5

HSCRC Existing Funding Mechanisms General Funding • Full Rate Application – – Review of total regulated costs of hospital Objective calculation based on approved methodology and efficiency standard Subjective analysis supporting hospital request above calculation Time consuming (~6 months from preparation to final approval), technical and costly • Partial Rate Application – Review of one specific aspect of hospital’s cost structure – Flexibility and variation in the structure and evaluation of the request Residency Funding • Included as part of a Full Rate Application for incremental funding • DME/IME credit in efficiency standard 6

Recommended Residency Funding Mechanism Partial Rate Application that meets Identified Criteria • Cost of Program – Comparison to Statewide Averages – Comparison to National / Regional Averages • How the Program meets the Triple Aim, for example: – Training that is primarily in the ambulatory setting focused on the patients in the community we serve – Training that emphasizes high quality and safe care with a curriculum that emphasizes reduction in harm measures such as the Maryland Hospital Acquired Conditions – Training that emphasizes cost conscious care such as reducing unnecessary utilization of resources and reductions in readmissions – Training that emphasizes team-based care and helps residents become effective team members and leaders 7

Recommended Residency Funding Mechanism (cont’d) • How the Program improves Population Health, for example: – Increased access to primary care through a resident clinic focused on meeting the needs of the chronically underserved / medically indigent patient – Starting a Family Medicine Residency will allow us to “grow our own” medical staff and assist with recruitment – Training a community of physicians that can assist other rural hospitals with meeting their unmet needs for access to primary care • Demonstrate Need for the Program – Through Community Needs Assessment – Shortage of Primary Care Physicians – National Comparisons 8

HSCRC Evaluation Process New Program or Expansion • New teaching hospital or teaching hospital expanding program Need Evaluation Funding Amount • Demonstrated support of • Direct triple-aim: experience - Actual budgeted costs across the continuum of - Statewide average (by care Specialty) • Adequate access to - Wage Adjusted Average • National particular sub-specialty • Regional within hospital’s service • Indirect area - Current Regression - Medical staff demand Model - Physicians per capita - Revised Regression for - Characteristics of IME population and - Resident / Bed community need Approach (Medicare) - Unemployment - Chronic disease 9

Partial Application for Residency Programs Template I. Amount of GME Request a) b) Direct Medical Education Indirect Medical Education Show calculations / support in appendix II. Overview of Program a) b) c) d) Type (Primary Care; Specialty) Number of Residents School Affiliation Timing III. Demonstration of Need for Program IV. Support for Program a) b) Address Three Part Aim Address Population Health 10