Making HIV Prevention Work Defining the Comprehensive HIV










- Slides: 19

Making HIV Prevention Work: Defining the Comprehensive HIV Prevention Package IAS Satellite Session 25 th July 2017 Daniel Were, Ph. D

Background § The basic premise of a comprehensive HIV prevention package is both epidemiological, behavioral, and sociocultural. § Knowledge on the drivers of the global, regional, and country-specific epidemics required. § A basic package must be designed around the target population and their specific needs. § Experience has shown that generic interventions are counterproductive.

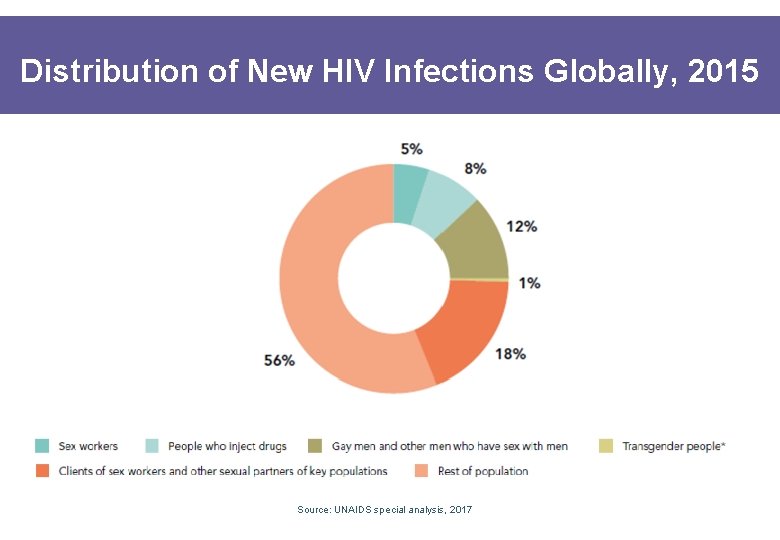
Distribution of New HIV Infections Globally, 2015 Source: UNAIDS special analysis, 2017

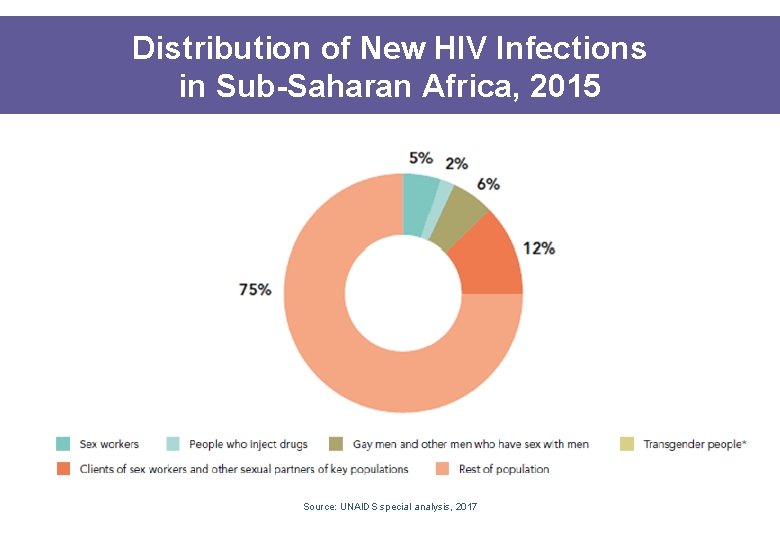
Distribution of New HIV Infections in Sub-Saharan Africa, 2015 Source: UNAIDS special analysis, 2017

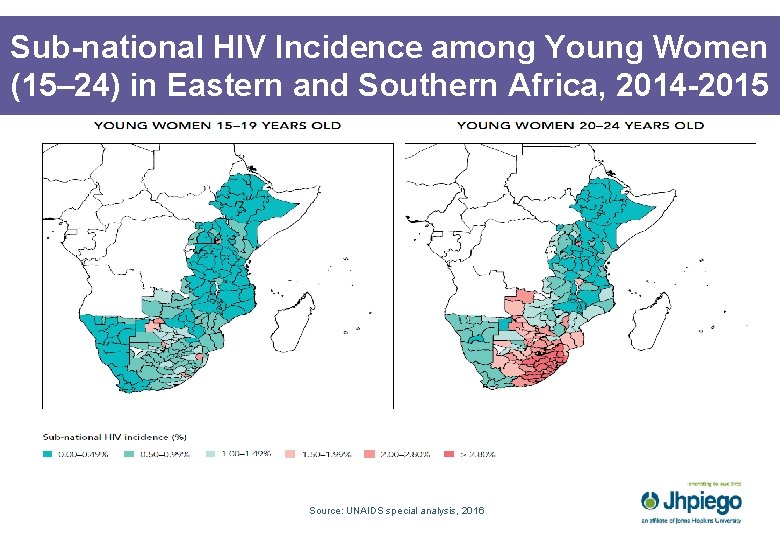
Sub-national HIV Incidence among Young Women (15– 24) in Eastern and Southern Africa, 2014 -2015 Source: UNAIDS special analysis, 2016

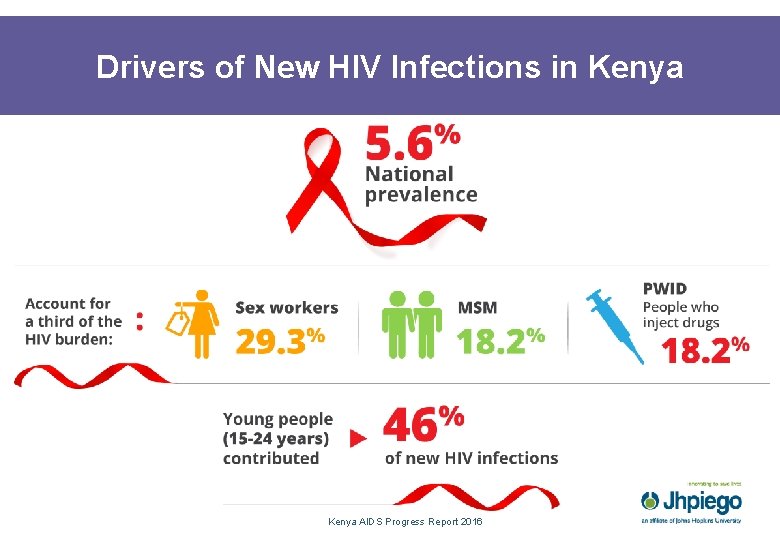
Drivers of New HIV Infections in Kenya AIDS Progress Report 2016

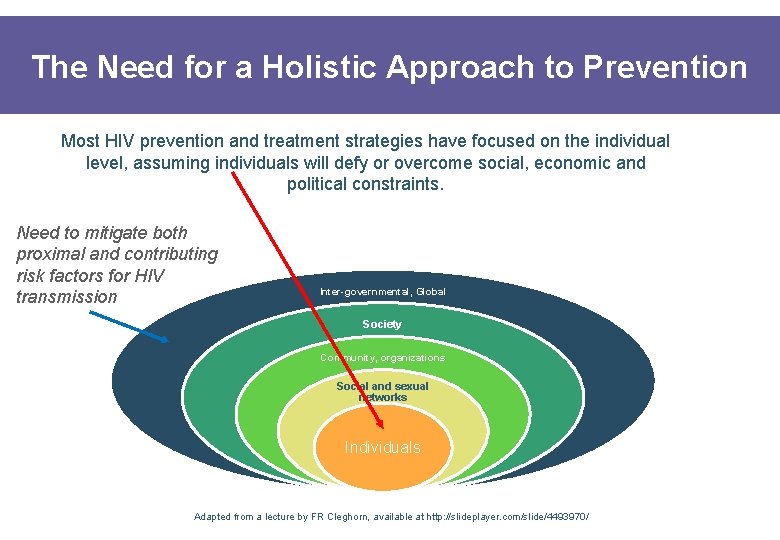
The Need for a Holistic Approach to Prevention Most HIV prevention and treatment strategies have focused on the individual level, assuming individuals will defy or overcome social, economic and political constraints. Need to mitigate both proximal and contributing risk factors for HIV transmission Inter-governmental, Global Society Community, organizations Social and sexual networks Individuals Adapted from a lecture by FR Cleghorn, available at http: //slideplayer. com/slide/4493970/

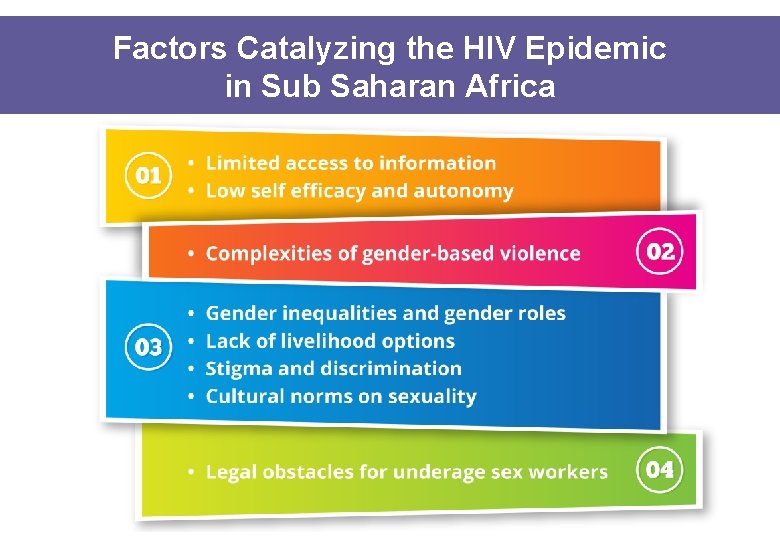
Factors Catalyzing the HIV Epidemic in Sub Saharan Africa

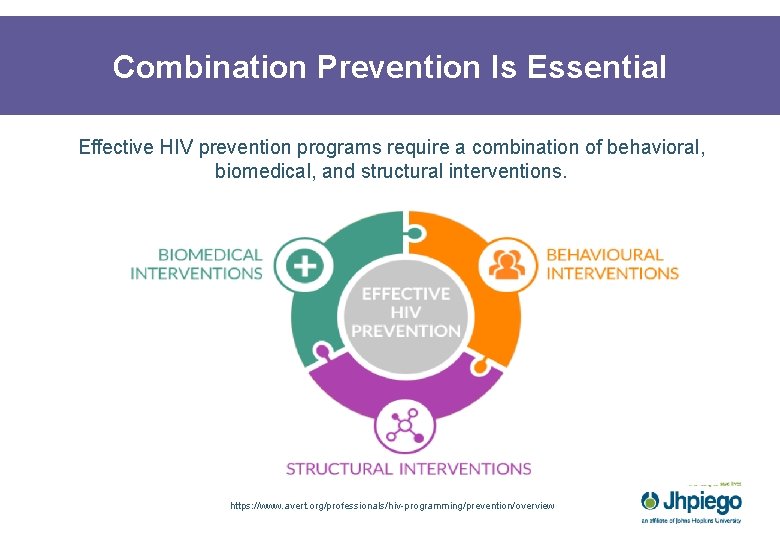
Combination Prevention Is Essential Effective HIV prevention programs require a combination of behavioral, biomedical, and structural interventions. https: //www. avert. org/professionals/hiv-programming/prevention/overview

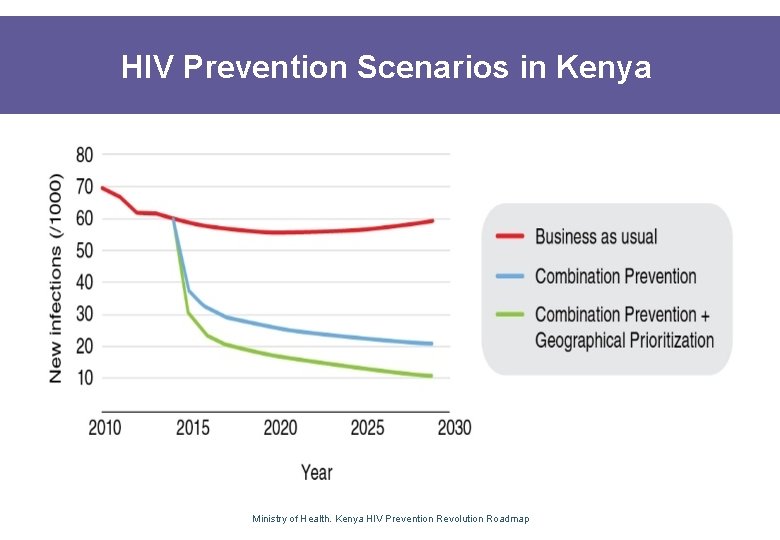
HIV Prevention Scenarios in Kenya Ministry of Health. Kenya HIV Prevention Revolution Roadmap

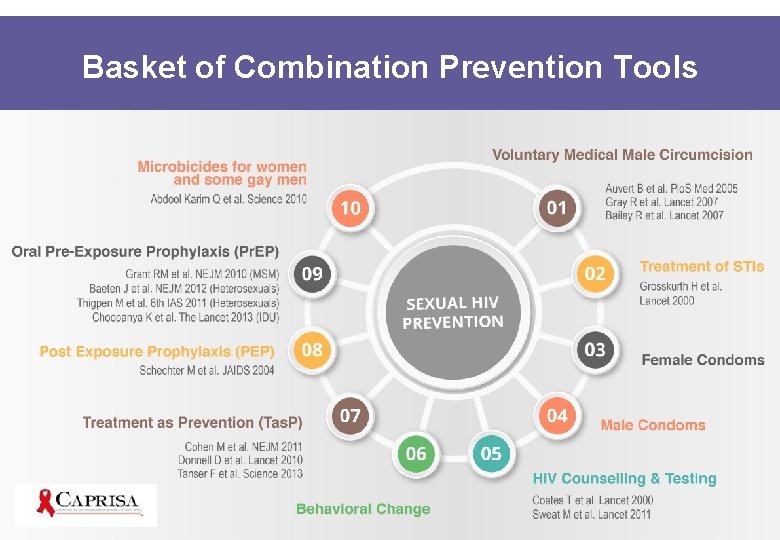
Basket of Combination Prevention Tools

Current Behavioral Interventions § Multiple evidence based behavioral interventions focused on; • • • Information and raising awareness Risk perception education Development of risk avoidance and risk reduction strategies Increasing self-efficacy Correct and consistent condom use skills Substance abuse mitigation

What to Prioritize in Behavioral Interventions § Address gaps in current behavioral interventions; • Basic awareness creation • Increase risk perception - risk avoidance and to develop a risk reduction strategy • Increase self-efficacy - to execute the risk reduction strategy through methods such as pre-exposure prophylaxis, correct condom use e. t. c.

Current Biomedical Interventions § § § § § HIV testing services Treatment as Prevention Voluntary medical male circumcision Pre-exposure prophylaxis Post-exposure prophylaxis Male and female condoms Methadone treatment and needle exchange Elimination of mother-to-child transmission Treatment of sexually transmitted infections

What to Prioritize in Biomedical Interventions § Focus on the gaps and optimize effective interventions; • HIV testing services - Men and youth • Treatment as Prevention - 90: 90 • Voluntary medical male circumcision - Age pivot • Pre-exposure prophylaxis - High risk populations • Male and female condoms • Methadone treatment and needle exchange - PWID • Treatment of sexually transmitted infections

Current and Priority Structural Interventions § Reducing vulnerability and victimization; • Social protection • Mitigating sexual and gender-based violence • Stigma reduction • Economic empowerment • Gender, social and cultural norms change • Human rights protection • Family and social support

Considerations for an Appropriate Combination of Prevention Interventions § Oral pre-exposure prophylaxis may be particularly imperative in settings where exposure to risk cannot be avoided. § Voluntary medical male circumcision is needed in generalized hyper endemic settings. § Behavioral interventions are pivotal to the uptake of biomedical interventions. § Mitigating vulnerability is key to sustaining optimal prevention outcomes.

Basic Package of Combination Prevention Interventions AGYW Awareness and risk reduction, HTS, Pr. EP, contraceptives, addressing (18 -24 years) vulnerability Female Sex Risk reduction counselling, Condoms, Pr. EP, STI treatment, Treatment as Workers Prevention, gender based violence Men who have Risk reduction counselling, Pr. EP, STI treatment, condoms, Treatment as sex with men Prevention, human rights protection Persons who Risk reduction counselling, Needle Inject Drugs exchange and Methadone treatment,

Conclusion § Each key and vulnerable population requires a unique basic package of interventions. § Geographic prioritization is essential. § We should offer population-specific choice and delivery of interventions. § Female-controlled methods should be a focal point.