Damage control surgery Prof Naeem Zia FCPS FACS





















- Slides: 25

Damage control surgery Prof Naeem Zia FCPS, FACS, FRCS


Definition �Damage control surgery (DCS) is a form of surgery typically by trauma surgeons utilized in severe unstable injuries �This form of surgery puts more emphasis on preventing the triad of death, rather than correcting the anatomy.

Technique of damage control surgery �Initial laparotomy �ICU resuscitation �Definitive Reconstruction

Initial laparotomy �Objectives � Control haemorrhage � Control contamination � Abdominal packing � Temporary abdominal closure

ICU resuscitation �Reverse the physiological insult �Lethal triad

Definitive reconstruction

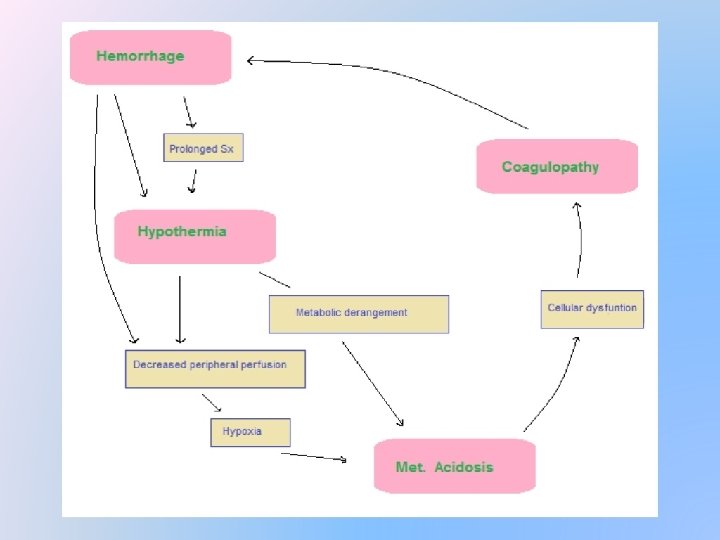
Trauma triad of death �Massive haemorrhage lead to � Hypothermia � Metabolic acidosis � Coagulopathy

Hypothermia �Heat loss by evaporationo and conduction of a �In ability to generate heat �Central cause of all derrangements

Metabolic acidosis �Massive transfusion �Vasopressors �Diminished cardiac function

Coagulopathy �Consumption dilution �Hypothermia �Acidosis


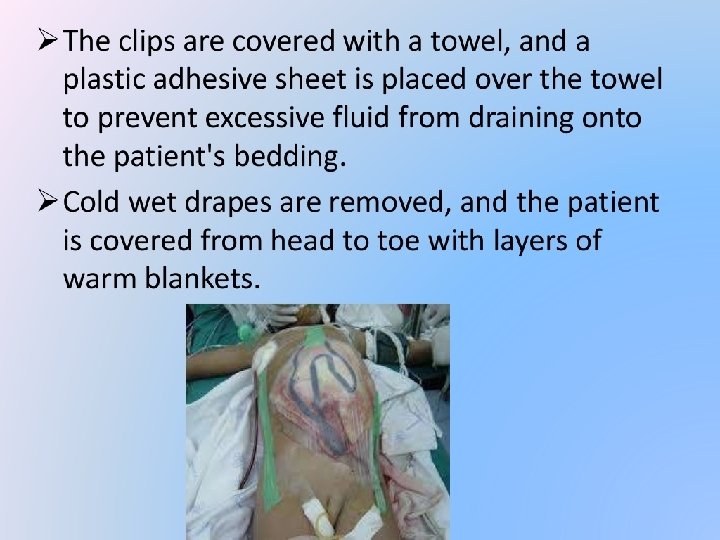
Principles of damage control Surgery �Rapid closure of abdomen �Opening abdomen for long period leads to loss of heat and fluid �Concomitant thoracic opening aggravates it �Break the viscous cycle of lethal triad and restore physiology

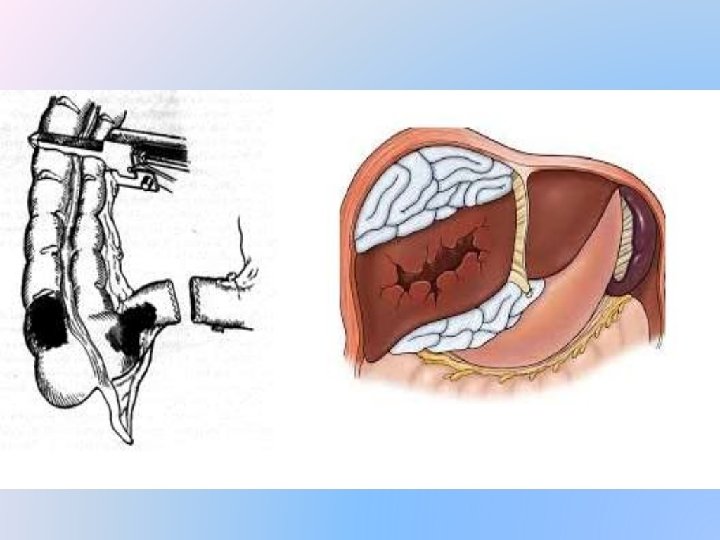
Steps in damage control Surgery �Bleeding raw surfaces , like that of the liver are packed with laparotomy pads �Small enteric injuries are closed with staples �Large ones are stapled on both sides with the GIA stapling device and damaged segment removed

�Injurs of the pancreas and kidneys are not treated if they are not bleeding �Clamps may be left on unrepaired vasculr injuries , or the vessels are ligated �Vessels which cannot be ligated without loss of life or limb can be treated with temporary indwelling shunts




Definitive surgery �Patient is taken for definitive surgery within 24 hours �If surgeons believes the metabolic derangemnts will improve within 2 hours patient can be kept in OT �If metabolic corrections will take a long time patient can be shifted to SICU

Indications for definitive surgery �Core temperature 36 F or above �Correction of acid base balance �Normalization of coagulation profile.

Disadvantages �Sepsis and multi organ failure �Pneumonia �Intrabdominal abscess �Enteric fistula �Compartment syndrome

Massive transfusion protocol �A massive transfusion protocol is used for massive trauma resuscitation, when more than ten units of blood are needed. Packed red blood cells, fresh frozen plasma, and platelets are administered in lieu of crystalloids or whole blood. Typically higher ratios of fresh frozen plasma and platelets are given relative to packed red blood cells.

�A massive transfusion protocol (MTP) is activated by a clinician in response to a patient that is experiencing massive bleeding. The responsible clinician activates the MTP either by phone or any other mechanism. Once a patient is in the protocol, the blood bank is able to insure rapid and timely availability of blood components to facilitate resuscitation

Permissive hypotension
Tranexamic acid