Calcitonin A hypocalcaemia hormone Lecture NO 2 nd

















- Slides: 23

Calcitonin- A hypocalcaemia hormone Lecture NO: 2 nd MBBS Dr Muhammad Ramzan

Calcitonin – the definition • Calcitonin is the formal name of a protein hormone secreted by the Para follicular cells of Thyroid gland • Also called Thyrocalcitonin • Major action of the Calcitonin is to inhibit the bone resorption by the Osteoclasts.

Calcitonin – the background ↓ Ca++ level when it is high • Calcitonin reduces serum Ca++ and PO 4 level when it is high, opposite to the action of PTH • This action of Calcitonin is through Osteoblasts and Osteocytes that have Calcitonin receptors. • Osteoclasts do not have Calcitonin receptors and so is true about the PTH receptors

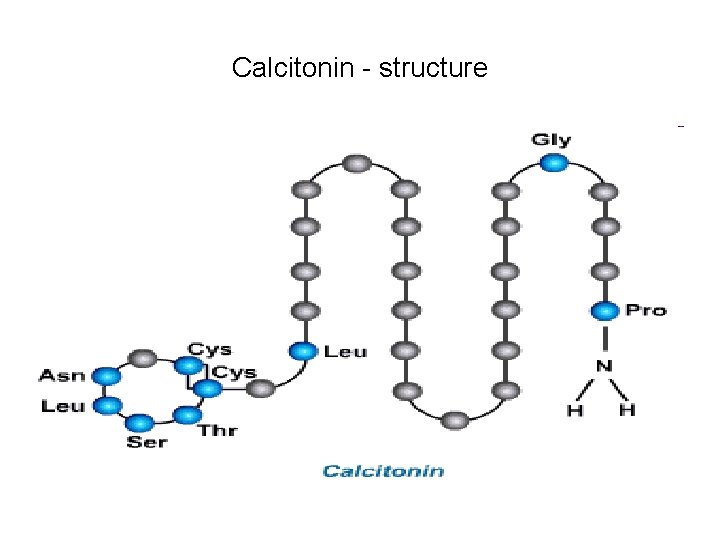
Calcitonin – Synthesis 32 AAs • Calcitonin is a single chain peptide of 32 AAs • Calcitonin is synthesized as a Prohormone having 115/142 AAs by the RER of : • Para follicular cells • It is cleaved to have 42/37/32 Amino acids after passing through Golgi Complex

Calcitonin – Synthesis cont. stored a vesicles • It is stored as secretary granules in the cytoplasm of the Para follicular cells • It Is released in response to an appropriate stimulus like high serum calcium level • Calcitonin has its own GPCR on the plasma membrane of the target organs

Calcitonin - structure

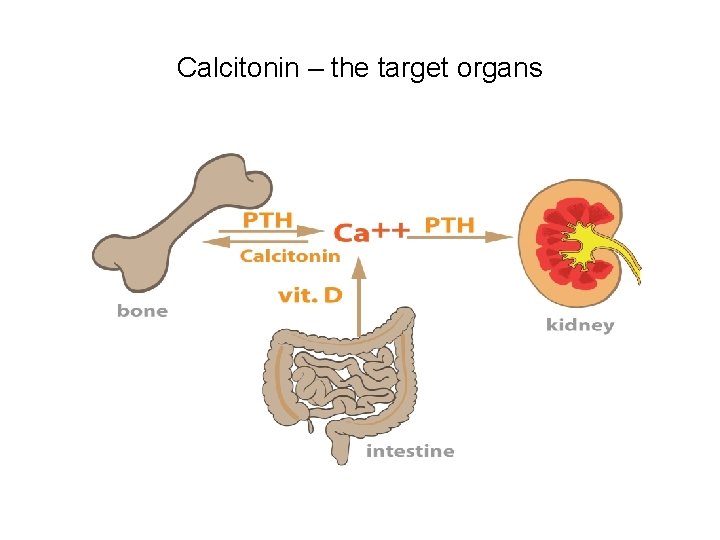
Calcitonin – Target tissues bone cells, renal tubules and GIT • Target tissues are the ones with Calcitonin receptors • The target organs for the Calcitonin are the : • Osteoblasts; Osteocytes, Renal tubular cells and GIT • Target tissues also bear PTH receptors and are also involved in binding Calcitonin • There are no Calcitonin receptors on Osteoclasts

Calcitonin – the target organs

Calcitonin - Regulation of secretion serum and ECF Ca++ • It is through negative feed back like PTH • Serum and extracellular calcium level is the major regulator of Calcitonin secretion • Serum Po 4 does not play an active role in human • There are 2 pathways for the regulation of Calcitonin • 1. Direct and 2. Indirect

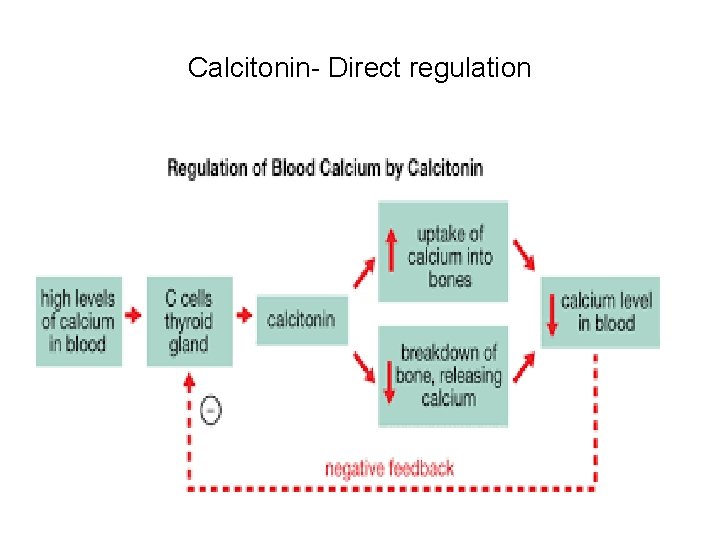
Calcitonin – Direct regulation interaction B/W Ca and Calcitonin • It is the interaction B/W serum Ca++ level and the Calcitonin • High Ca level stimulates Para follicular cells to ↑ synthesis of Calcitonin that lowers serum Ca++ level • It will also inhibit the Osteoclastic activity but promotes bone formation ( deposition of Ca) • There is no role of PTH

Calcitonin- Direct regulation

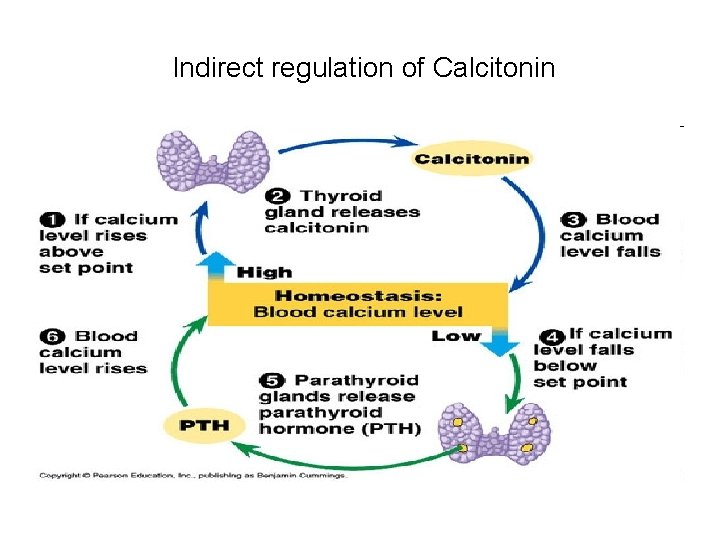
Calcitonin – Indirect regulation via PTH • Low serum Ca++, stimulates the Para thyroids to ↑ PTH secretion and Osteoclastic activity • This elevates serum Ca++ and inhibits Calcitonin synthesis by inhibiting Para follicular cells • Normal Ca level is 9 - 11 mg/100 ml

Indirect regulation of Calcitonin

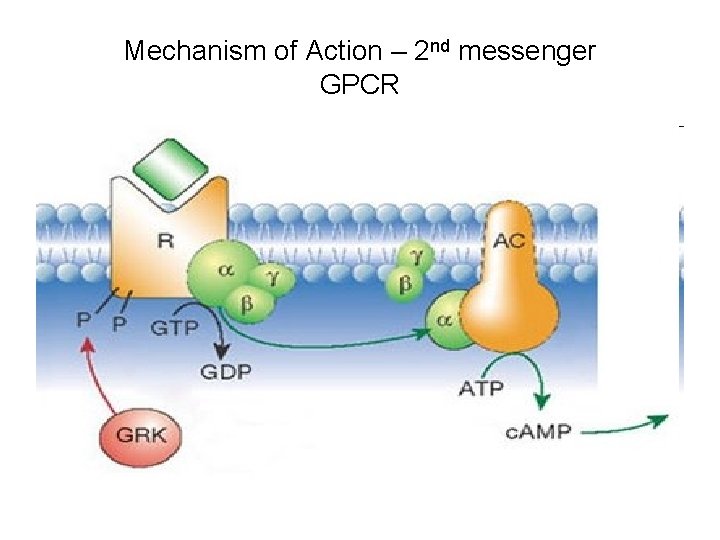
Calcitonin - Mechanism of action GPRC • Calcitonin is a peptide and its mechanism of action is like other peptides/proteins – 2 nd messenger • Calcitonin binds to the extra cellular domain of GPCR on Osteoblasts, Osteocytes and Renal tubules • Produces conformation changes in membranous subunit

Calcitonin – Mechanism of action cont. • It leads to the activation of G protein and binding of its α-subunit to the GDP in exchange for GTP • Membranous Adenylate Cyclase is stimulated by α-GTP and converts ATP to c. AMP – the 2 nd messenger • c. AMP activates Protein Kinase that Phosphorylates other proteins/enzymes to execute hormonal actions

Mechanism of Action – 2 nd messenger GPCR

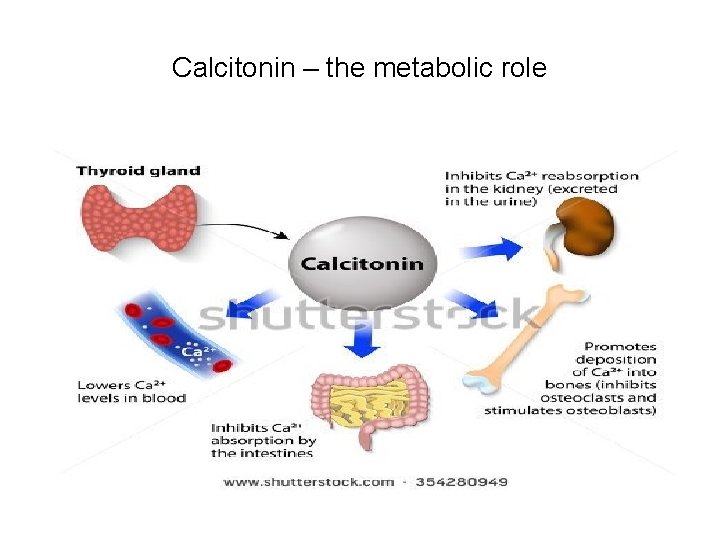
Metabolic role of Calcitonin • Depends upon its action on target organs • These include : • Bones • Kidneys • and Intestines

Calcitonin – the metabolic role

Effects on bone activity • Calc. inhibits Osteoclastic activity and bone resorption • Less Ca and PO 4 are mobilized from the bone to blood • Lowers serum and extracellular calcium ions • Calcitonin promotes Osteogenesis and Osteoblastic activity especially in children

Effects on Kidneys • It inhibits resorption of Ca and Po 4 from the distal tubule and ascending loop of Henley 1 • It promotes the renal excretion of Ca and PO 4 to reduce the blood calcium level 2 • Calcitonin inhibits the activation of Vitamin D in kidneys

Effects on intestine • Reduction in the activation of Vitamin D that reduces absorption of calcium from GIT • It lowers the blood calcium level

Calcitonin – Secretion abnormalities • A large no of diseases are associated with abnormally excess or deficiency of Calcitonin • However, the pathologic effects of abnormal Calcitonin secretion per se are not generally recognized.

Clinical significance of Calcitonin • Para follicular cells involved in thyroid malignancies • This results in ↑ Calcitonin with no significant hypocalcaemia • It is used for the treatment of osteoporosis after menopause and hysterectomy. • Further it is also used in the hypocalcaemia due to malignancies, hyperparathyroidism and VIT. D intoxication