Calcium Homeostasis By Dr Abdel Aziz M Hussein


Calcium Homeostasis By Dr. Abdel Aziz M. Hussein Assist Prof of Medical Physiology

Functional histology of bone
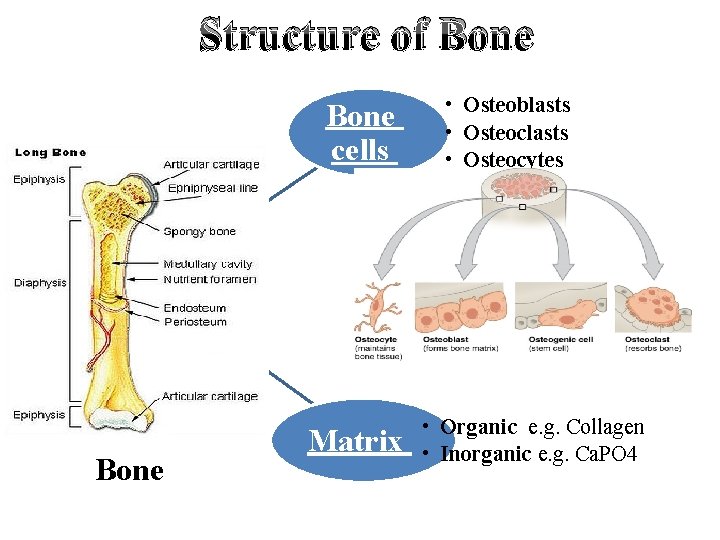
Structure of Bone cells Bone Matrix • Osteoblasts • Osteocytes • Organic e. g. Collagen • Inorganic e. g. Ca. PO 4

Bone Cells Osteoblast Bone forming cells Osteoclast Bone eating cells (Large multinucleated cells derived from monocytes) Secrete bone matrix or collagen Contain alkaline phosphatase (help Ca. PO 4 deposition) Help bone resorption and destruction Contain acid phosphatase which produce lactic and hyaluronic acid Osteocyte Mature bone cells Most numerous cells Cannot form collagen
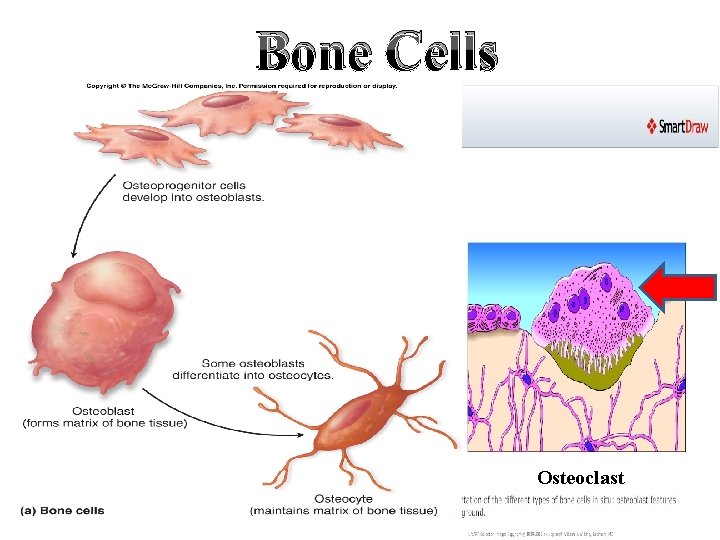
Bone Cells Osteoclast
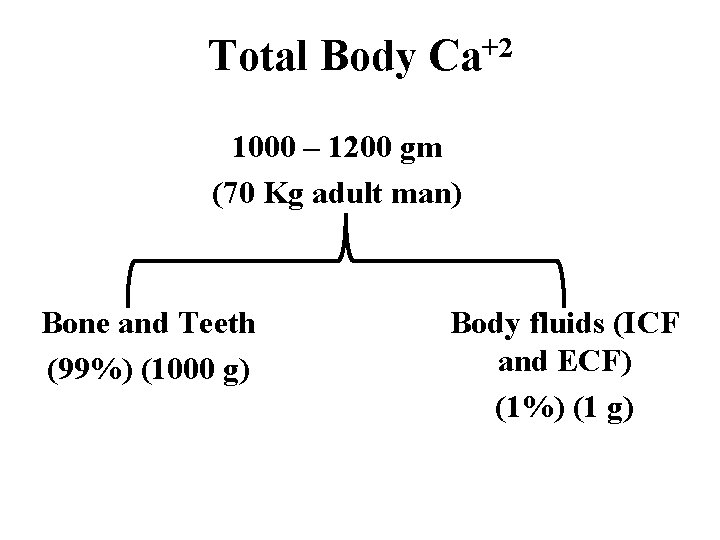
Total Body Ca+2 1000 – 1200 gm (70 Kg adult man) Bone and Teeth (99%) (1000 g) Body fluids (ICF and ECF) (1%) (1 g)
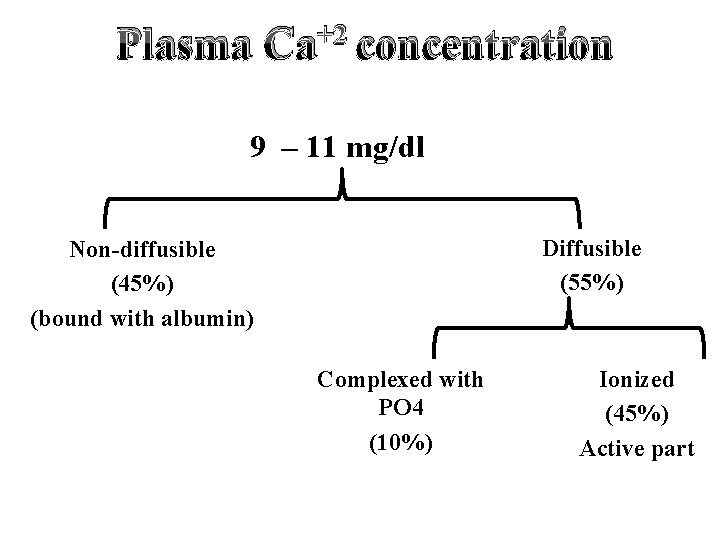
Plasma +2 Ca concentration 9 – 11 mg/dl Diffusible (55%) Non-diffusible (45%) (bound with albumin) Complexed with PO 4 (10%) Ionized (45%) Active part
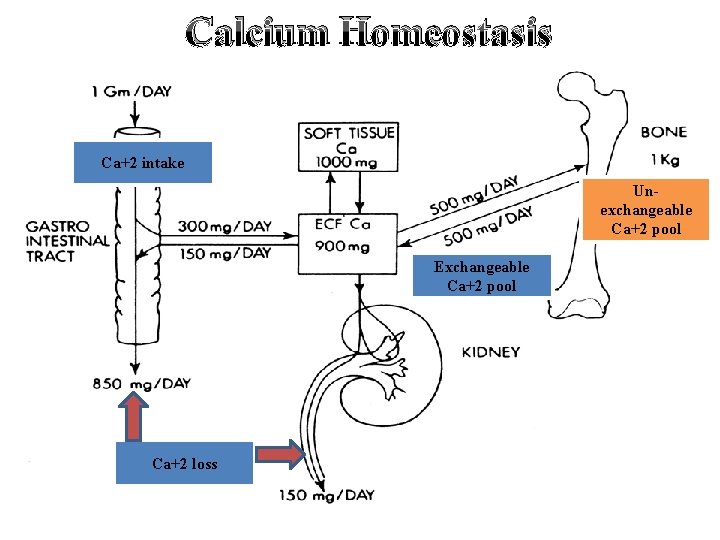
Calcium Homeostasis Ca+2 intake Unexchangeable Ca+2 pool Exchangeable Ca+2 pool Ca+2 loss

Physiological importance of Ca+2 • Ca+2 has fundamental importance to all biological systems. 1. Participates in numerous enzymatic reactions. 2. Important for hormone secretion. 3. Acts as a mediator of hormonal effects.

Physiological importance of Ca+2 4. Essential for neurotransmission 5. Essential for ms contraction 6. Essential for blood clotting. 7. Essential formation of bone and teeth.
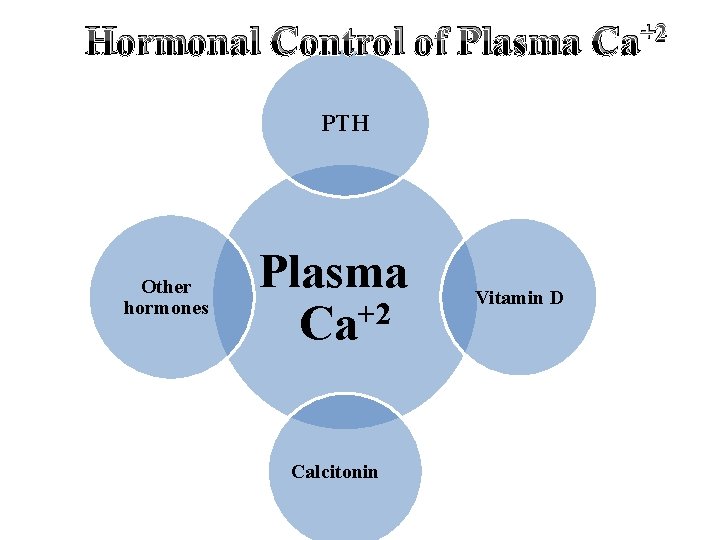
Hormonal Control of Plasma Ca+2 PTH Other hormones Plasma Ca+2 Calcitonin Vitamin D

Parathyroid Hormone
Parathyroid Hormone (PTH) Source: • Chief cells of parathyroid gland Chemistry: • Polypeptide hormone (84 aa)

Functions of PTH • The prime function of PTH is to keep a normal Ca+2 level in plasma (9 -11 mg %). • It also maintains a constant ratio between Ca+2 and inorganic phosphate PO 4 -, so that; • Solubility product = Ca x PO 4 = K (constant).
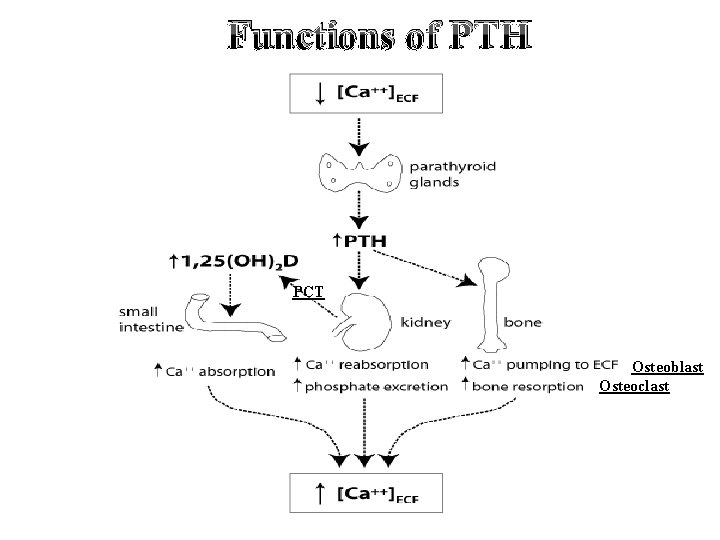
Functions of PTH PCT Osteoblast Osteoclast

Functions of PTH a) Kidney: 1. Increases reabsorption of Ca+2 and Mg+2 from DCT 2. Inhibits PO 4 reabsorption from PCT. 3. Activates Vit. D by 1 α hydroxylase enzyme in PCT b) Bone: 1. Increases number and level of activity of osteoclasts (bone destroying cells) in the skeleton →bone resorption 2. Increases pump of Ca+2 from bone matrix to ECF by osteoblast a) Small intestine : 1. Increases absorption of Ca+2 (mediated by active vitamin D (1, 25 DOH cholecalciferol)→ activated in the kidney by PTH. 2. Increases absorption of PO 4 and Mg+2.

Control of PTH secretion a) Plasma Ca level: • It the main regulator of PTH secretion. • ↓ Plasma Ca level → ↑ PTH secretion b) Plasma Mg level: as Ca c) Plasma PO 4 level: opposite to Ca d) Nervous factors: β-adrenergic receptors agonists as isoproterenol→↑ PTH secretion

Thyrocalcitonin
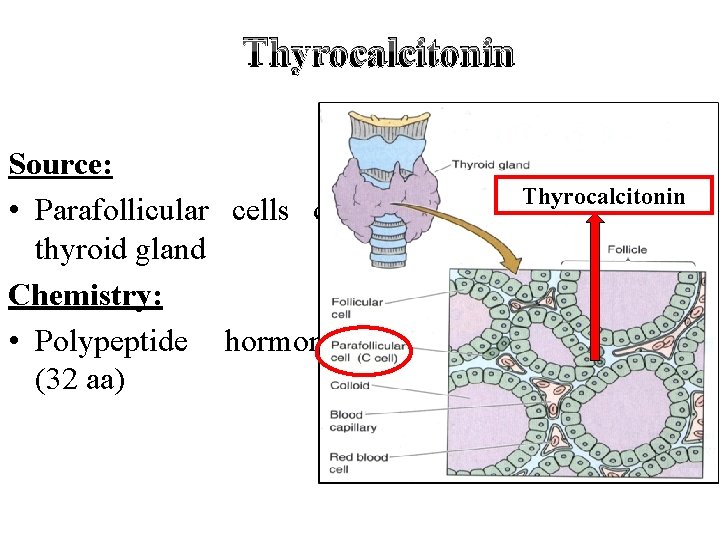
Thyrocalcitonin Source: • Parafollicular cells of thyroid gland Chemistry: • Polypeptide hormone (32 aa) Thyrocalcitonin
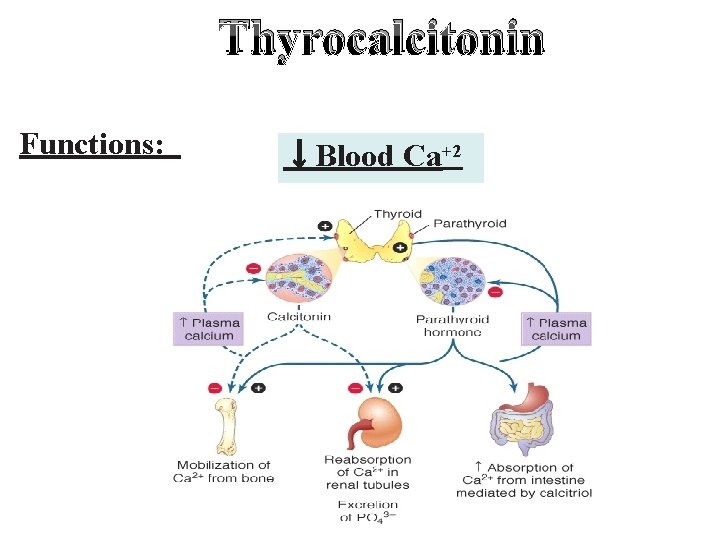
Thyrocalcitonin Functions: ↓Blood Ca+2
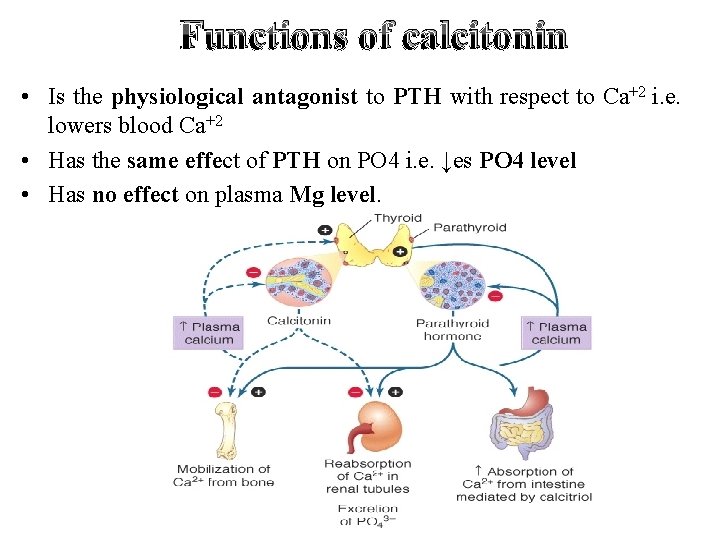
Functions of calcitonin • Is the physiological antagonist to PTH with respect to Ca+2 i. e. lowers blood Ca+2 • Has the same effect of PTH on PO 4 i. e. ↓es PO 4 level • Has no effect on plasma Mg level.

Functions of calcitonin a) Bones: 1. Inhibits osteolysis by osteocytes and reduces resorption by osteoclasts. 2. Decreases Ca+2 mobilization from bone to blood as it inhibits Ca+2 permeability of bone cells. b) Kidneys: 1. Increases urinary excretion of Ca+2 and PO 4. 2. Inhibits Vit. D activation in the kidney. c) Intestine: 1. Decreases Ca+2 absorption from the intestine. 2. Inhibits the gastric motility and gastrin secretion.

Control of Calcitonin secretion i)Plasma Ca+2: • The major stimulus to its secretion is a rise in serum Ca+2 • e. g. its plasma concentration ↑es 2 -10 times after acute rise of serum Ca+2 of as little as 1 mg%. ii) GIT hormones: • Several GIT hormones (gastrin is the most potent) stimulate calcitonin secretion during ingestion of food.

Vitamin d 3
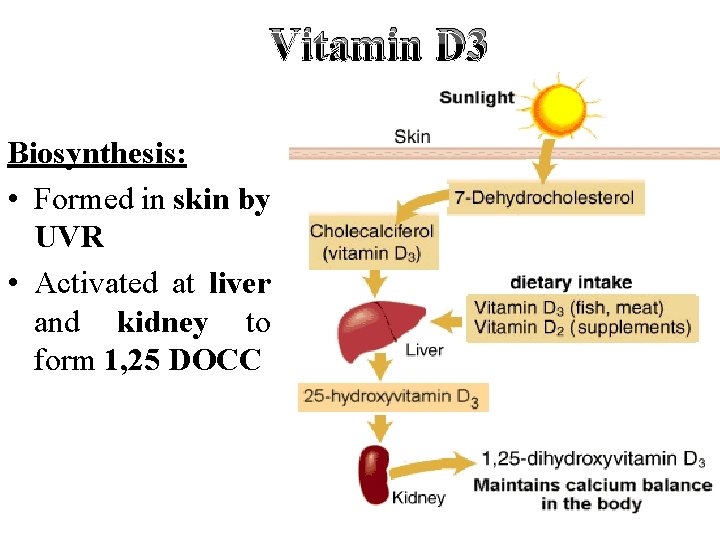
Vitamin D 3 Biosynthesis: • Formed in skin by UVR • Activated at liver and kidney to form 1, 25 DOCC

Action of Vitamin D • The intestine is the principal target of vitamin D a)On intestine: • Stimulates the absorption of both Ca+2 and PO 4 -. b)On bone: • Bone is the 2 nd major target of vitamin D. • Provides Ca+2 and PO 4 - to initiate the crystallization of bone osteoid at bone surfaces. c)On kidney: • Increases renal tubular reabsorption of both Ca+2 and PO 4 -.

Other hormones

Sex Hormones • Sex hormones are involved in the pubertal growth spurt and closure of the epiphyses a)Estrogens: • Protect female skeleton from the development of osteoporosis: 1. Inhibits PTH mediated bone resorption 2. ↓es the amount of bone-resorbing cytokines such as interleukin 1 and 6 in bone. 3. ↑es serum PTH due to the hypocalaemic effect of the inhibition of bone resorption. b)Androgens; • Protect men from the development of osteoporosis

Glucocorticoids A. At physiological levels, glucocorticoids are necessary for skeletal growth. B. Chronic excess have deleterious effects on Ca+2 homeostasis) 1. Decrease renal tubular Ca+2 absorption. 2. Inhibit intestinal Ca+2 absorption. 3. Inhibit osteoblastic bone formation.
Growth hormone 1. Stimulate bone growth 2. Stimulate Ca+2 and PO 4 absorption from intestine Thyroid hormone • Stimulate bone growth and ossification • Hypothyroidism delay bone growth and hyperthyroidism causes bone resorption

Disorders of ca+2 homeostasis
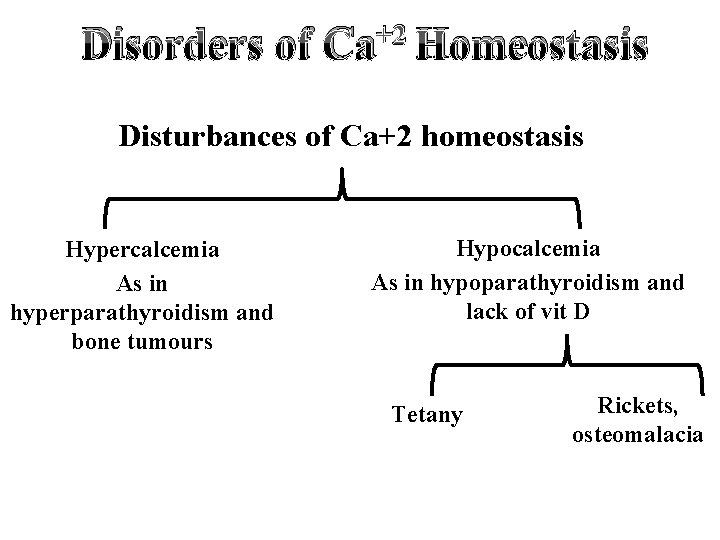
Disorders of +2 Ca Homeostasis Disturbances of Ca+2 homeostasis Hypercalcemia As in hyperparathyroidism and bone tumours Hypocalcemia As in hypoparathyroidism and lack of vit D Tetany Rickets, osteomalacia
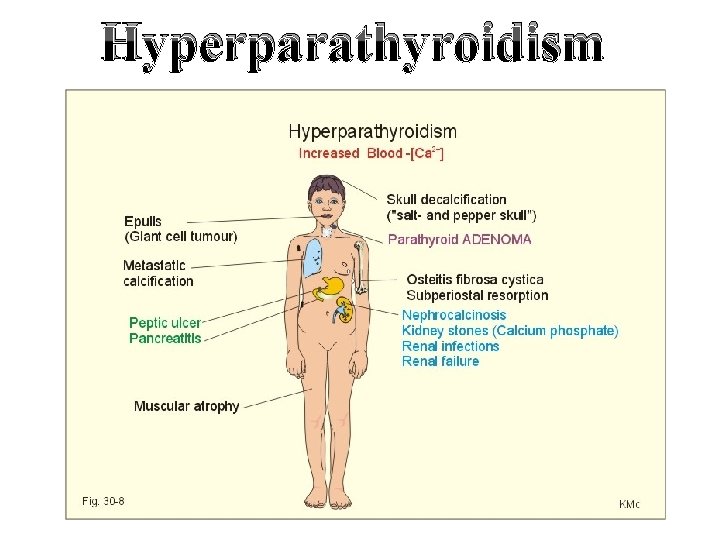
Hyperparathyroidism

Signs and symptoms Hypocalcaemia and Tetany
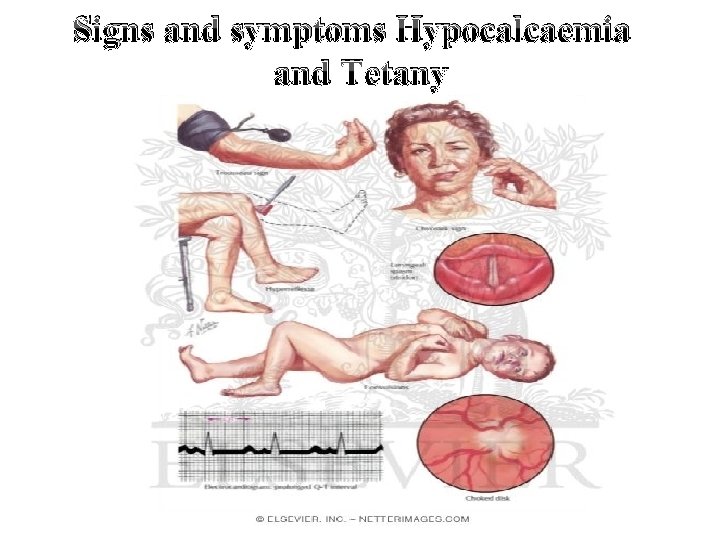
Signs and symptoms Hypocalcaemia and Tetany
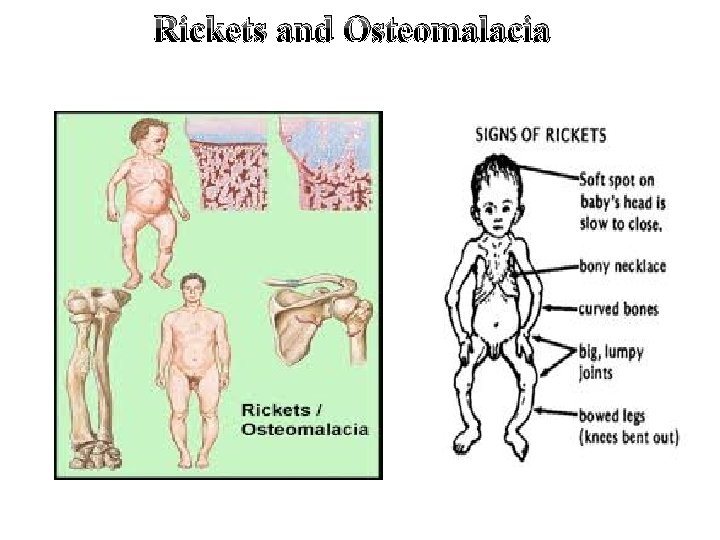
Rickets and Osteomalacia
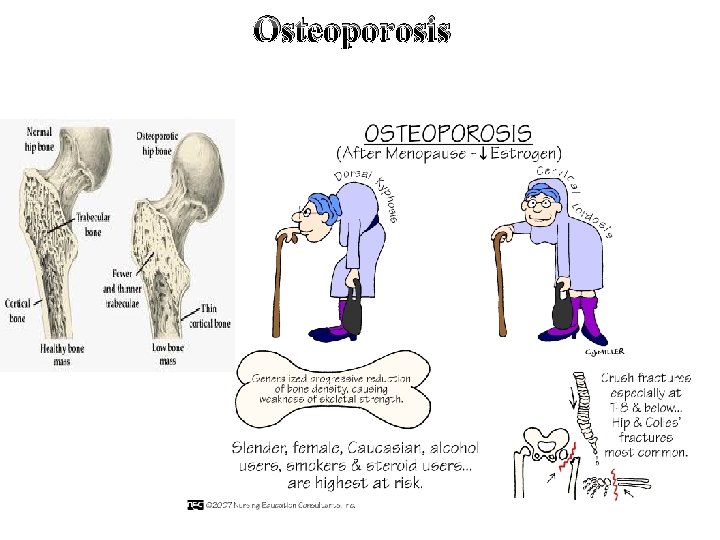
Osteoporosis

Thank You
- Slides: 39