CAESAREAN SECTION Dr Ifeyinwa Nwokoro Department of Obstetrics

CAESAREAN SECTION Dr. Ifeyinwa Nwokoro Department of Obstetrics and Gynaecology National Hospital Abuja © NITMED TUTORIALS

Definition Caesarean section is the delivery of a fetus through an abdominal and uterine incision after the age of viability (28 th weeks of gestation)

3 Historical Perspective • Origin controversial. • Hypothesised to be named after the manner of birth of Julius Caesar in 100 BC. • Originally used to deliver the baby of a mother who had died in ancient Egypt, Asia AND Europe. • First caesarean section on a live woman was that on the wife of Jacob Nufer in the 16 th century. • Earliest report of a child that survived C/S was the birth of Gorgias of Sicily in 508 BC. • The procedure was associated then with high mortality due to sepsis ( lack of antibiotics) and there was no anaesthesia. • Great improvement and survival from the 19 th century especially with the advent of the lower segment C/S BY Munro – Kerr.

4 Incidence • In west Africa 15 – 21 %.

Classification of Urgency of CS

6 Indication For C/S, • MATERNAL INDICATIONS • Severe pre- eclampsia with unfavourable cervix for vaginal delivery • Previous classical caesarean delivery (absolute) • 2 or more previous CS • Previous extensive uterine surgery with entry into the uterine cavity eg myomectomy. • Obstructive pelvic tumours eg fibroids, ovarian cysts, malignancies • Situations where the increasing intrathoracic pressure generated by Valsalva maneuvers could lead to maternal complications. These include, dilated aortic valve root and recent retinal detachment.

7 Maternal Indications for C/S contd. • Previous 30 perineal tears. • Previous successful VVF repair • Vulva herpes simplex.

8 Fetal Indications For C/S. • Fetal distress • Abnormal presentations – breech, brow (absolute), persistent occipito – posterior in labour, face with mento – posterior. • Abnormal lie – transverse, oblique, • Multiple pregnancies: the first twin in a nonvertex presentation, or higher order multiples (triplets or greater) • Fetal macrosomia – weight greater than 4500 g.

9 Fetal Indications for C/S contd. • Footling breech, • Very low birth weight – ( less than 1500 g). • Fetal abnormality –hydrocephalus, conjoint twins, spina bifida.

10 Maternal – Fetal Indications For C/S. • Cephalopelvic disproportion. • Dystocia –arrest of cervical dilatation or failure of descent of presenting part. • Major degree placenta praevia. • Placental abruption with a live fetus.

11 Preoperative Preparation. A full history and physical examination. Past medical and surgical history. Current medications. Hx of drug allergies. Indication for the C/S. Consent for the surgery. Laboratory investigations – Hb, PCV, Platelets, Urinalysis, EU/Cr. More extensive investigations in complicated cases like hypertension, cardiac diseases etc. patients are individualized in such cases. • Pass indwelling Foley urethral catheter into the bladder and retain. • During transfer to theatre, and during anaesthesia, patient should lie on her left lateral side with a wedge on her right buttocks to prevent supine hypotension. • •

12 Preoperative Preparation • Anaesthetic review • Pre – medication • Prophylatic antibiotics?

13 Anaesthesia For C/S. • General anaesthesia. • Regional anaesthesia. • Spinal. • Epidural AVOID FULL STOMACH ESPECIALLY IN LABOUR DURING ANY FORM OF ANAESTHESIA.

14 Skin Incisions For C/S • Skin incisions could be vertical or transverse. • Both have advantages and disadvantages.
15 Vertical Skin Incisions Vertical incisions • Midline sub – umbilical incision • Midline incision extending above the umbilicus. • Paramedian. Advantages • Less vascular, less haemorrhage. • Gives good exposure of both pelvic and abdominal organs. • Very useful in emergencies due to speed and ease of the procedure. Disadvantages • Prone to hernia formation

16 Transverse Skin Incisions • Pfannenstiel (most popular) Advantages: • Excellent cosmetic appearance. • Less risk of wound dehiscence. • Early ambulation. • Less risk of hernia formation. Disadvantages. • Takes longer time to perform. • May result in injury to ileo – inguinal and ileo – hypogastric nerves. • Increased blood loss.

17 Transverse Skin Incisions Joel Cohen incision • It is a straight transverse incision – anterior rectus sheath incised in the midline followed by blunt dissection. Maylard incision – (UNCOMMON) – transverse incision like the Pfannenstiel but the rectus is cut through at any level between the pubis and the umbilicus. Cherney incision – like Pfannenstiel but unlike the latter, the two recti muscles are pulled away from their insertion into the pubis.
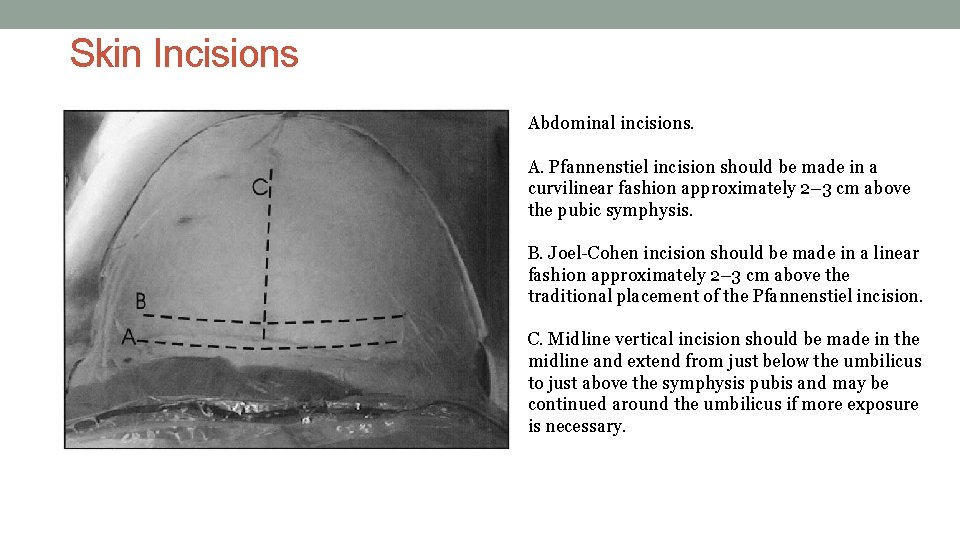
Skin Incisions Abdominal incisions. A. Pfannenstiel incision should be made in a curvilinear fashion approximately 2– 3 cm above the pubic symphysis. B. Joel-Cohen incision should be made in a linear fashion approximately 2– 3 cm above the traditional placement of the Pfannenstiel incision. C. Midline vertical incision should be made in the midline and extend from just below the umbilicus to just above the symphysis pubis and may be continued around the umbilicus if more exposure is necessary.

19 Uterine Incisions • Lower segment transverse incision – 90 % of C/S. • Low vertical (De Lee) incision- made parallel to the longitudinal axis of the uterus in the midline but keeping mainly to the lower segment. • Classical incision – is made by incising the uterus parallel to the longitudinal axis of the uterus in the midline.
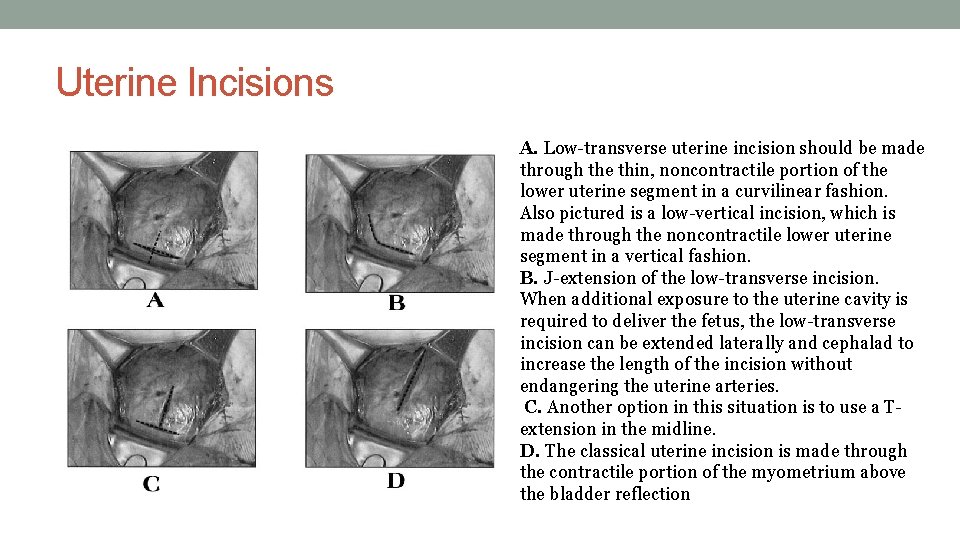
Uterine Incisions A. Low-transverse uterine incision should be made through the thin, noncontractile portion of the lower uterine segment in a curvilinear fashion. Also pictured is a low-vertical incision, which is made through the noncontractile lower uterine segment in a vertical fashion. B. J-extension of the low-transverse incision. When additional exposure to the uterine cavity is required to deliver the fetus, the low-transverse incision can be extended laterally and cephalad to increase the length of the incision without endangering the uterine arteries. C. Another option in this situation is to use a Textension in the midline. D. The classical uterine incision is made through the contractile portion of the myometrium above the bladder reflection

21 Classical incision • Indications • Preterm delivery with poorly formed lower segment. • Placenta praevia with large vessels in lower segment. • Transverse lie with back inferior. • Large cervical fibroid. • Postmortem C/S. • Caesarean hysterectomy

22 Advantages of transverse lower uterine incisions over classical incision • Less risk of entry into upper uterine segment • Great ease of entry • Less risk of adhesion formation to bowel or omentum • Less likelihood of uterine rupture in subsequent pregnancies. • VBAC is possible • Less intra- operative bleeding NOTE THAT CLASSICAL C/S ARE NOT ROUTINELY DONE.

23 Advantages of classical incision over lower segment incision. • Rapid entry into the uterus • No lateral extensions into the uterine vessels and broad ligament • If lower segment is poorly developed, delivery by classical C/S is advantageous without lateral extension • Easy entry into the uterus when there is fibroid in the lower segment.

Post operative care • IV Fluids • Antibiotics • Encourage early ambulation • Thromboprophylaxis • Oral intake • Length of hospital stay

25 Complications of c/s. • Haemorrhage which may lead to anaemia. • Injury to maternal organs – bladder, blood vessels, uterus, bowel. • Injury to neonate. • Wound infection. • Deep vein thrombosis. • Endometritis. • Maternal mortality. • Anaesthetic complications.


Conclusion • Incidence of caesarean delivery has increased dramatically • Although the operation continues to become safer, the incidence of maternal mortality and morbidity is still significant • Continued efforts on the part of the obstetrician must be made to ensure that caesarean deliveries are not performed for inappropriate indications and that each woman is counseled carefully according to her individual characteristics • When a cesarean section is indicated and embarked upon the preparation should be as carefully planned as time allows, and the surgical technique should adhere to good surgical principles.
- Slides: 27